Abstraction time per encounter decreases manual data abstraction

Abstraction time per encounter decreases manual data abstraction efficiency and limits timely registry submission A quantitative baseline prior to registry automation Kenneth E. Mah, MD, MS; Kelly R. Brown, MS, BSN, RN; John Butcher, BSN, RN; Allison J. Arand, BSN, RN; Karen A. Hendricks, MSN, RN, CPN; Matthew J. Brown; Mark A. Weber; Kelsey J. Hart, DNP, BSN, RN; James M. Brown, MS; and Nicolas L. Madsen, MD, MPH Kenneth. Mah@cchmc. org

Background • For an institution to participate in registries, data are manually abstracted from the electronic health record into the registry database and manually adjudicated at various institution dependent stages prior to submission. The goal of this process is to meet registry standards for time to submission and accuracy, which afford timerelevant quality science initiatives. • Currently, many institutions are not meeting Pediatric Cardiac Critical Care Consortium’s (PC 4) time to submission requirement (< 30 days from discharge to submission) and/or are facing financial challenges to support an abstraction staff to do so. • The factors contributing to untimely submission remain unclear. While granular aspects of abstraction workflow vary across institutions, the general process of data abstraction is shared yet has not been well cataloged with efficiency metrics.

Aims • Describe manual data abstraction in a time-based fashion • Identify factors contributing to inefficient or precluding efficient data abstraction • Identify etiologies of untimely registry submission

Methods – Study Design • Prospective observational study baseline prior to registry automation intervention • Dates: 1/19/20 -10/28/20 • Location: Cincinnati Children’s Hospital Medical Center (CCHMC) – CCHMC: 405 CPB operations and 745 total CICU encounters in 2019. 1. 5 -1. 75 PC 4 full-time equivalents (FTE) • Inclusion criteria: any CICU encounter • Exclusion criteria: none • Measures: – Primary: Time from hospital discharge to encounter submission to PC 4 – Secondary: Abstraction time per encounter – Secondary: Rate of submission (encounters abstracted per week) • Analysis – Statistical process control analysis – Descriptive statistics with variables expressed as the mean, median, or median with interquartile range (IQR)

Methods - Definitions • Long abstraction time encounter (LATE) = an encounter requiring > 160 minutes to abstract and fulfilling the following criteria: – Increases mean time from discharge to submission (1º measure) on the same or subsequent week of abstraction AND – Increases mean abstraction time per encounter (2º measure) on the week of abstraction above the system’s baseline average (centerline mean)
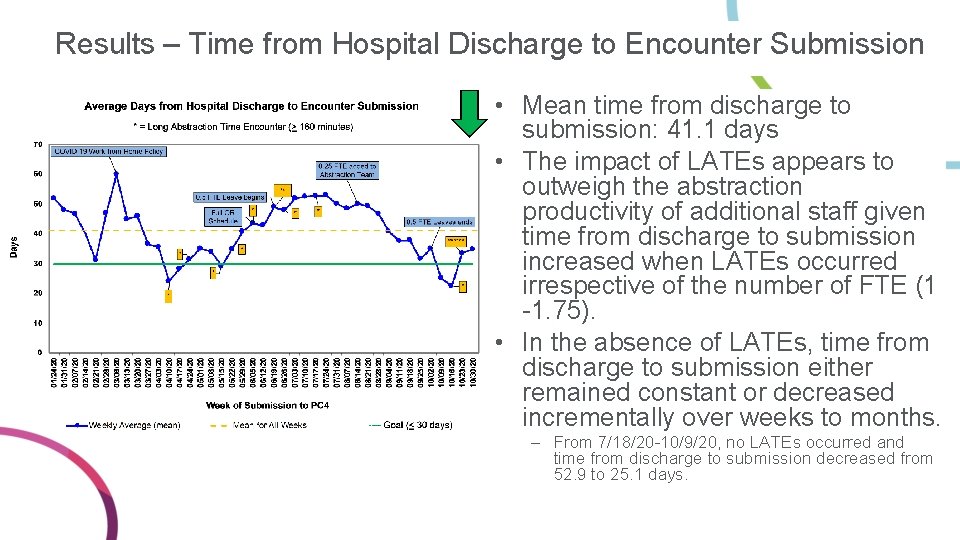
Results – Time from Hospital Discharge to Encounter Submission • Mean time from discharge to submission: 41. 1 days • The impact of LATEs appears to outweigh the abstraction productivity of additional staff given time from discharge to submission increased when LATEs occurred irrespective of the number of FTE (1 -1. 75). • In the absence of LATEs, time from discharge to submission either remained constant or decreased incrementally over weeks to months. – From 7/18/20 -10/9/20, no LATEs occurred and time from discharge to submission decreased from 52. 9 to 25. 1 days.
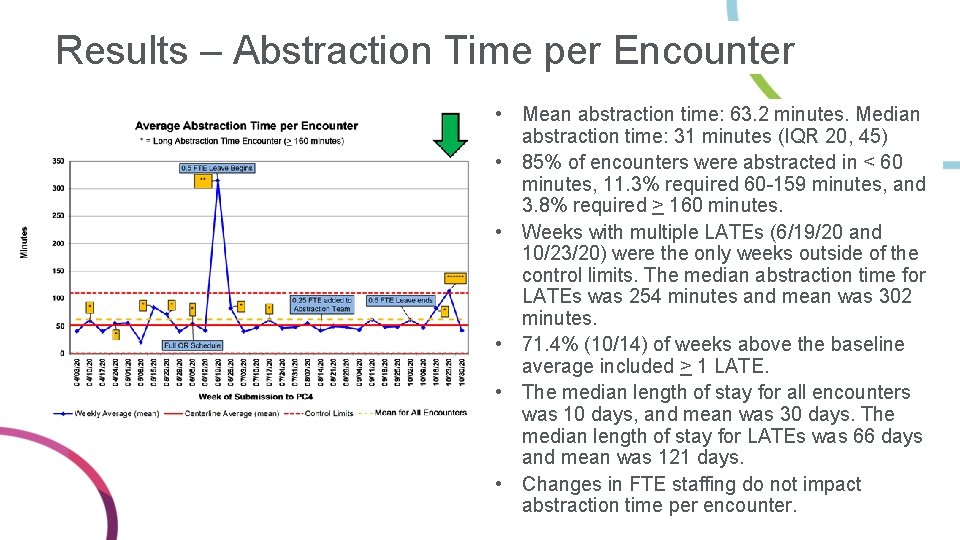
Results – Abstraction Time per Encounter • Mean abstraction time: 63. 2 minutes. Median abstraction time: 31 minutes (IQR 20, 45) • 85% of encounters were abstracted in < 60 minutes, 11. 3% required 60 -159 minutes, and 3. 8% required > 160 minutes. • Weeks with multiple LATEs (6/19/20 and 10/23/20) were the only weeks outside of the control limits. The median abstraction time for LATEs was 254 minutes and mean was 302 minutes. • 71. 4% (10/14) of weeks above the baseline average included > 1 LATE. • The median length of stay for all encounters was 10 days, and mean was 30 days. The median length of stay for LATEs was 66 days and mean was 121 days. • Changes in FTE staffing do not impact abstraction time per encounter.
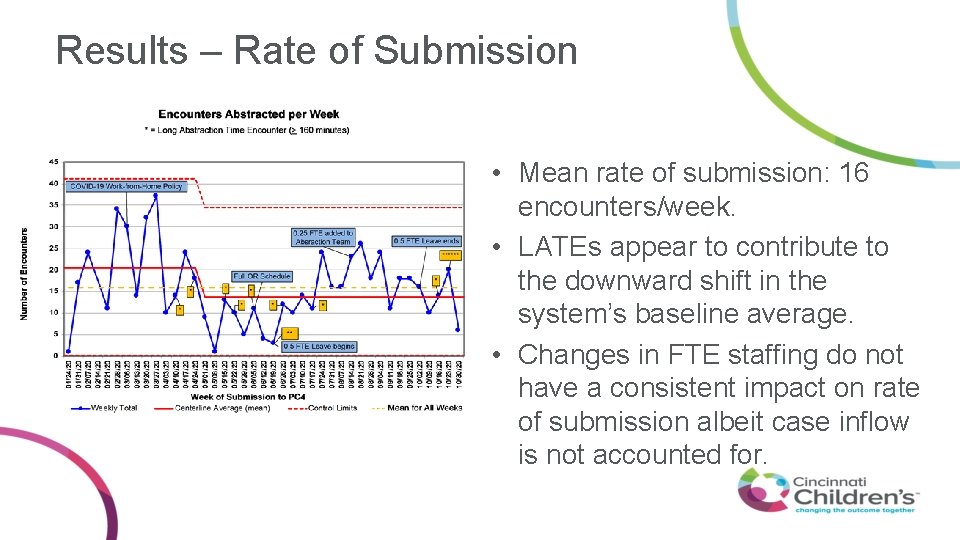
Results – Rate of Submission • Mean rate of submission: 16 encounters/week. • LATEs appear to contribute to the downward shift in the system’s baseline average. • Changes in FTE staffing do not have a consistent impact on rate of submission albeit case inflow is not accounted for.

Conclusions • Increased abstraction time per encounter decreases manual data abstraction efficiency and limits timely registry submission. • Long abstraction time encounters (LATEs) may be the primary etiology of untimely registry submission. • Sustainment or incremental reduction of an institution’s time to submission appears to be primarily offset by LATEs. This LATE impact appears to be independent of abstractor staffing. • In the absence of LATEs, additional abstractor staffing appears to increase the reduction rate of time from discharge to submission. • Data abstraction may experience efficiency gains by modifying the workflow to optimize abstraction time through such methods as registry data automation. • While encounter inflow is likely non-modifiable, targeted efficiency efforts may be successful by focusing on the early identification of LATEs and revision of LATE abstraction workflow.

Acknowledgements • PC 4 Abstraction Team – John Butcher (Abstractor) – Allison Arand (Abstractor) – Karen Hendricks (Abstractor) • James M. Anderson Center for Health Systems Excellence – Jim Brown (Senior Quality Improvement Specialist) – Kelsey Hart (Clinical Quality Specialist) • Safety, Quality, and Value Team of the Heart Institute – Kelly Brown (Program Manager, Informatics, Data & Analytics) – Matt Brown (Quality Analyst) • Information Services Team of the Heart Institute – Mark Weber (Technical Specialist)
- Slides: 10