Abnormality Disorders Abnormality infrequent in population violates norms

Abnormality & Disorders • Abnormality: infrequent in population, violates norms, disability, distress

Abnormality & Disorders • Psychological Disorder: pattern of behavior that: • Causes significant distress • Causes harm to self or others • Interferes with ability to function

Models of Abnormality • Stress-Vulnerability Model: genetic predisposition to disorder; symptoms brought out during stress • Biological: neurotransmitter function • Evolutionary: exaggerated form of adaptive behavior • Cognitive: faulty thinking

Models of Abnormality • Learning/Behavioral: inappropriate conditioning or modeling • Humanistic: blocked personal growth; poor self-concept • Psychoanalytic/Psychodynamic: unconscious conflict (id, ego, superego) • Sociocultural: cultural beliefs or values
Control vs. Influence • • Emotion Memory Thinking Conditioning Neurotransmitters Nervous system Behavior? ?

Living with a disorder • 22% of people at any given time • Most can be treated successfully • Long-term prognosis: may see alternate periods of normal functioning with periods of disorder – or – management with proper treatment • Recovery?

Stress • Psychosomatic disorders: interruption to proper functioning because of overloaded nervous system • Prolonged stress creates physical problems • Stomach pain, asthma, eczema, hives, migraine headaches, rheumatoid arthritis, high blood pressure, colitis, heart disease, sore muscles (neck, back), indigestion, constipation, chronic diarrhea, fatigue, insomnia, sexual dysfunction • Prolonged stress triggers and/or worsens psychological symptoms • Related to increased symptoms for mood, anxiety, somatoform, eating, and schizophrenia disorders • Extreme stress or trauma can trigger initial symptoms, especially PTSD, dissociative disorders, bipolar disorder, and schizophrenia

Somatoform Disorders • Belief of physical illness without actual physical ailment • Hypochondiasis: constant worry about illness • Somatization Disorder: show of worry about specific symptoms for medical attention • Conversion Disorder: unexplained CNS disruption, e. g. , paralysis • Biological Factors: None • Environmental Factors: anxiety, reinforcement during illness, cognitive magnification of bodily changes

Schizophrenia • Thought disorder: Interruption to normal thinking / reasoning processes, usually with unexplainable auditory or visual experiences • The brain tries to fill in the gaps to make sense but the result does not reflect reality • Positive Symptoms (+): incoherence, loose associations, paranoia, clang associations, hallucinations (esp. auditory), delusions of: grandeur, persecution, reference • Negative Symptoms (-): loss of normal thought or behavior, catatonia, social withdrawal, inappropriate emotions/affect

Schizophrenia • Biological Factors (DP 14: 03 -15, 18: 18 -19: 50) • genetic predisposition (gene combination), disordered structures, NT imbalance much DA thinking areas, too DA & glutamate emotion areas) brain (too little • Environmental Factors • low support, stress, double-bind parenting, nutrition, drug use (during critical stages of development) • Treatment • Anti-psychotics for positive symptoms, stress management, social support, family therapy, social training (video)
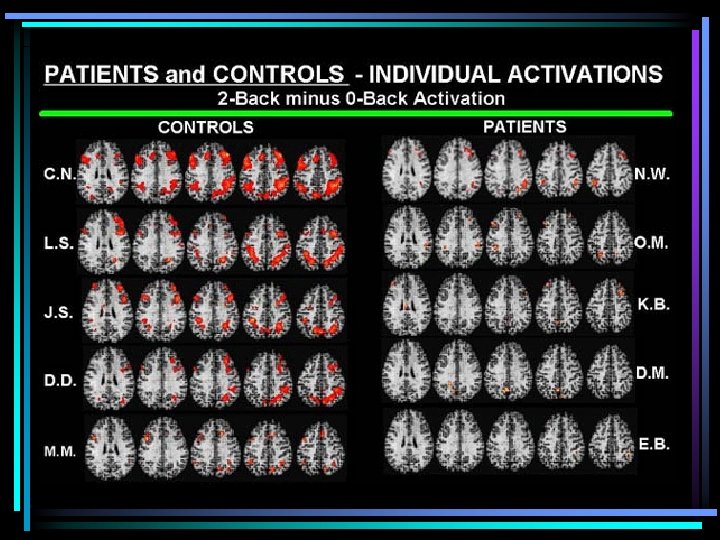

Prognosis • Schizophrenia • Maintenance drugs or symptoms for life • Psychotherapy to reduce episodes, severity, manage relationships, life skills

Dissociative Disorders • Dissociative Amnesia • can't recall information related to a traumatic or highly stressful event (selective to incident) • Dissociative Fugue State • sudden, unexpected travel from home, can't recall their past or personal identity

Dissociative Disorders • Dissociative Identity Disorder • 2 or more distinct personality states where different states recurrently take control of the host • The host’s memory of events experienced as other personalities is dependent on relationship with alters

Dissociative Disorders • Biological Factors • Not sure; can easily dissociate • Environmental Factors • High anxiety or traumatic experience • Prognosis • Amnesia and Fugue often spontaneously recover • Dissociative Identity Disorder rarely recover (integration usually unsuccessful) but can manage symptoms, relationships

Other Disorders • Impulse control: lacking inhibition of urges • Seasonal: related to sunlight, environ. • Comorbidity: presence of more than one disorder
- Slides: 16