Abnormalities Of The Testis And Scrotum Ahmed AlSayyad

Abnormalities Of The Testis And Scrotum Ahmed Al-Sayyad
Embryology Testicular differentiation is initiated in the 7 th week of gestation by the SRY gene n At 4 to 6 weeks’ gestation, the genital ridges organize. This is followed by migration of primordial germ cells n At 7 to 8 weeks’ both sertoli and leydig cells have developed n

Embryology During the 8 th week, the fetal testis begins to secrete testosterone and MIS independent of pituitary hormonal regulation n MIS is secreted by the Sertoli cells and causes degeneration of the müllerian structures after the 8 th week of gestation n The gubernaculum appears at the 7 th week of embryologic development where its cranial aspect envelops the cauda epididymis and lower pole of the testis and extends caudally into the inguinal canal, where it maintains a firm attachment n

Cryptorchidism 3% of full-term male newborns and 30. 3% incidence in premature infants n More prevalent among preterm, small-for-gestational-age, low-birth-weight, and twin neonates n Approximately 70% to 77% of cryptorchid testes will spontaneously descend by 3 months of age n By 1 year of age, the incidence of cryptorchidism declines to about 1% and remains constant throughout adulthood n

Descent Factors n n n Hormonal: androgens, MIS, estrogen, descendin Gubernaculum GFN and CGRP Epididymis Intra-abdominal pressure

Terminology n n n Undescended Ascended Gliding Retractile Ectopic

Nonpalpable testis n n n Intra-abdominal Vanishing Atrophic Missed on examination Bilateral nonpalpable work-up

Consequences of Cryptorchidism n n n Infertility Neoplasia Hernia Torsion Trauma Cosmetic

Work-UP Maternal history including the use of gestational steroids, Perinatal history, including documentation of a scrotal examination at birth, PMH, PSH, FH n Examine in a warm room, supine, squatting etc n Look for genital abnormalities, scrotal size, contralateral hypertrophy n

Investigations n n n Hormones US CT MRI Laparoscopy
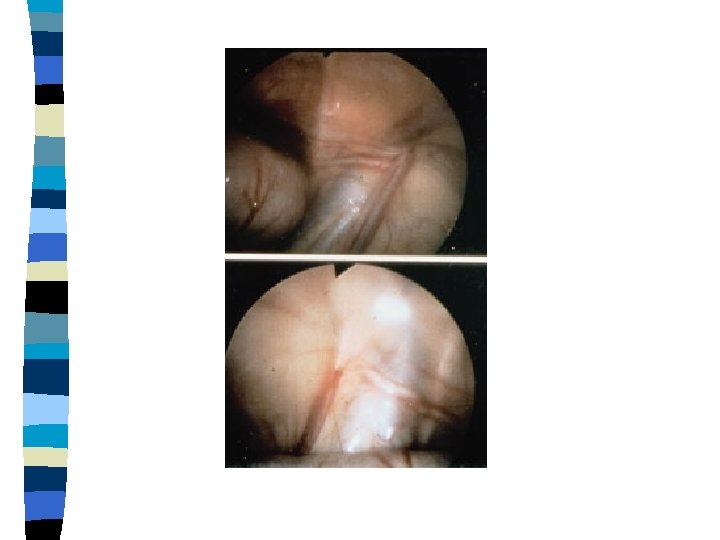
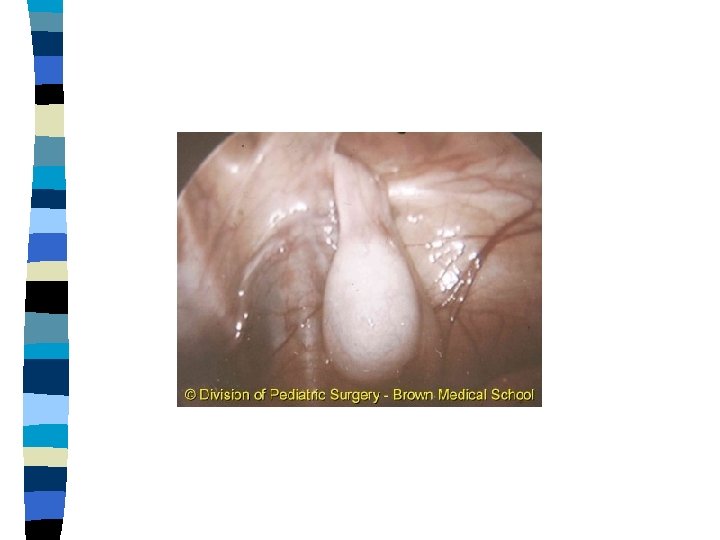

Hormonal Therapy n n n HCG or Gn. RH can be used The lower the pretreatment position the better the results Self limiting side effects Overall success rate < 20% Limited indications if any

Surgical Intervention n n n When Inguinal orchiopexy Laparoscopic orchiopexy Fowler-Stephens orchiopexy Staged orchiopexy Microvascular autotransplantation

Hydrocele Normally, the processus vaginalis is obliterated from the internal inguinal ring to the upper scrotum, leaving a small potential space in the scrotum that partially surrounds the testis n Embryologic misadventures may occur and results in (hydrocele, hydrocele of the cord, and communicating hydrocele). n

Simple Hydrocele n n n Simple (scrotal) hydrocele is an accumulation of fluid within the tunica vaginalis Results from persistence of or delayed closure of the processus vaginalis Commonly seen at birth, frequently bilateral, may be quite large. They transilluminate and may seem quite tense but not painful Most resolve during the first 2 years of life If surgical repair is elected, an inguinal approach should be used

Communicating Hydrocele n n n Persistence of the processus vaginalis which allows peritoneal fluid to communicate with the scrotum The classic description is that of a hydrocele that changes in size It can be compressible during examination All should be fixed using an inguinal approach Do it bilateral if patient got VP shunt or on peritoneal dialysis

Hydrocele of the cord Segmental closure of the processus, which leaves a loculated hydrocele of the cord n Presents as a painless groin mass which is mobile and transilluminates n Inguinal exploration and high ligation is curative n
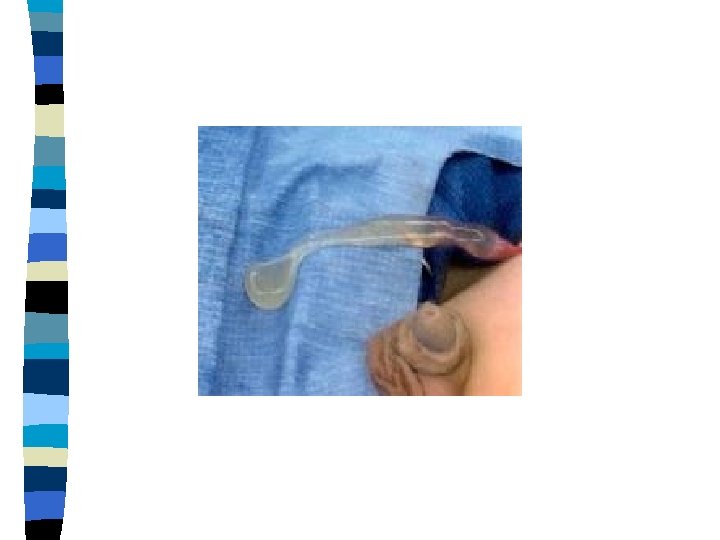

Acute Scrotum
Differential Diagnosis n n n n Torsion testis Torsion appendix epididymis Epididymo-orchitis Hernia Trauma Vasculitis Dermatological

Testicular Torsion True surgical emergency of the highest order n Irreversible ischemic injury may begin as soon as 4 hours after occlusion of the cord n Intravaginal torsion, result from lack of normal fixation of the testis and epididymis to the fascial and muscular coverings that surround the cord n This creates an abnormally mobile testis that hangs freely within the tunical space (a "bell-clapper deformity") n

Testicular Torsion Happens in any age but most commonly in prepubertal males n Presentation: Pain, NV, Poor appetite, previous episodes n Examination: Swelling, Tenderness, High riding, transverse orientation, Loss of cremasteric reflex n

Testicular Torsion n n Doppler US may help in the diagnosis Manual detorsion may be attempted in ER Scrotal exploration is mandatory Detorte the affected testis and pex the other side while waiting for the testis to pink up If the testis is still alive pex it , if not do an orchiectomy
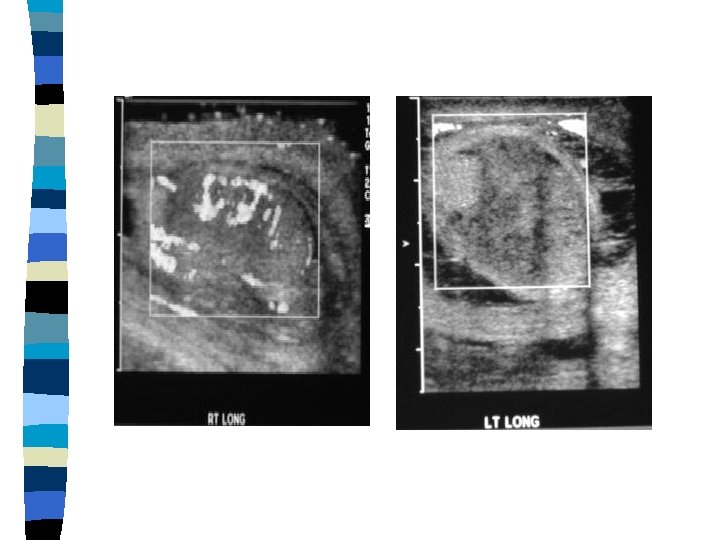
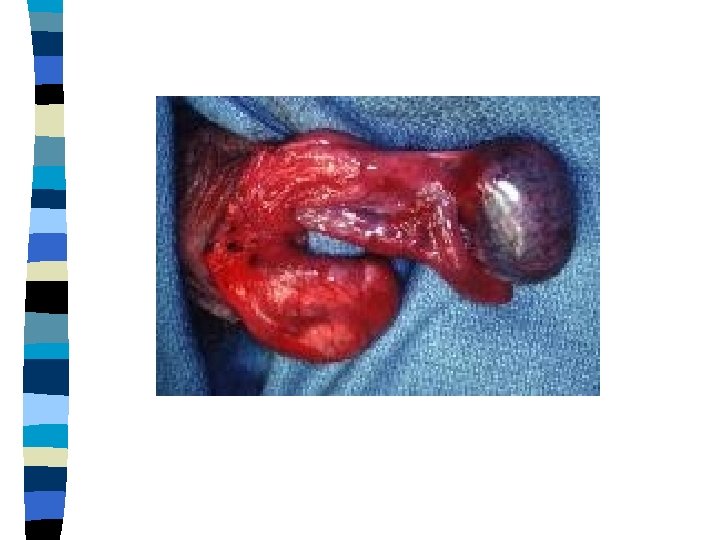

Intermittent Torsion Recurrent episodes of acute, self-limited scrotal pain n Normal physical examination will be found inbetween n If the suspicion is strong , elective scrotal exploration and bilateral orchiopexy should be performed n

Prenatal testicular torsion Extravaginal torsion n Presents at birth as a hard, nontender testis fixed to the scrotal skin which is usually discolored n Doppler US may help in the diagnosis n Management is controversial: observation Vs exploration n

Torsion Appendix Testis presentation is extremely variable, from an insidious onset of scrotal discomfort to an acute presentation identical to torsion testis n Exam: Tenderness or mass in the upper pole, Blue dot sign, cremasteric reflex usually present n Doppler US may help in diagnosis n Management: conservative, pain meds, limit activity n

Epididymitis n n n Rare in pediatrics Presentation: pain, swelling, erethyma, LUTS, fever, urethral discharge, STDs Investigations: pyuria, bacteriuria, positive urine culture, increased flow on doppler IV Abx given if systematically ill then oral for total of 10 -14 days Screening US usually indicated ? VCUG

Varicocele Dilated and tortuous veins of the pampiniform plexus n Found in approximately 15% of male adolescents, with a marked left-sided predominance n Etiology: increased venous pressure in the left renal vein, incompetent valves of the internal spermatic vein n

varicocele Unilateral varicocele may affect testicular function bilaterally n Toxic effect of varicocele may manifest as testicular growth failure, semen abnormalities, Leydig cell dysfunction, and histologic changes n n Possible mechanisms: reflux of adrenal metabolites, hyperthermia, hypoxia, local testicular hormonal imbalance, and intratesticular hyperperfusion injury

varicocele Presentation: asymptomatic, pain, scrotal mass, infertility, atrophy n Grading on physical examination n Obtain scrotal US n Treat if there is loss of volume (> 2 mls or > 20%) n

Treatment Alternatives Inguinal Ligation and Subinguinal Ligation n Retroperitoneal and Laparoscopic Ligation n Transvenous Occlusion n Complications: hydrocele, recurrence, testicular atrophy n
- Slides: 34