Abnormal Uterine Bleeding in Adolescents Maria C Monge

Abnormal Uterine Bleeding in Adolescents Maria C. Monge, MD Director of Adolescent Medicine Dell Children’s Medical Center UTSW-Austin Pediatrics Residency Program Lone Star Circle of Care

Disclosures • I have no relevant financial disclosures.

Objectives • 1. Define abnormal uterine bleeding (AUB) in an adolescent. • 2. Discuss possible etiologies of AUB in an adolescent and use these in consideration of the initial outpatient workup of AUB. • 3. Identify initial outpatient management strategies for adolescents with AUB.

CASE – MADELINE

Madeline • Madeline is a 12 year old who comes to your office after she felt lightheaded at school. – Mom called and triage nurse said to bring her in. – Mom told the nurse that Madeline has had menstrual bleeding for more than 1 week and has been feeling more tired than usual for the past month.

Madeline • Review of records before she arrives – Healthy, on no medications – Growth and development normal • 50% BMI • At last WCC had not started menstruating, but had SMR 3 breasts and pubic hair – Family history unremarkable

NORMAL MENSES

Normal Menses • Menarche: 2. 3 y after pubertal initiation – Range 1 -3 years • Cycle length: 21 -42 days (beginning to beginning) – Should be regular by 2 -2. 5 years – Cycles outside of 20 -45 days should be considered abnormal even in adolescents • Duration: 3 -7 days • Average blood loss: 30 m. L/cycle – Can be 20 -80 m. L
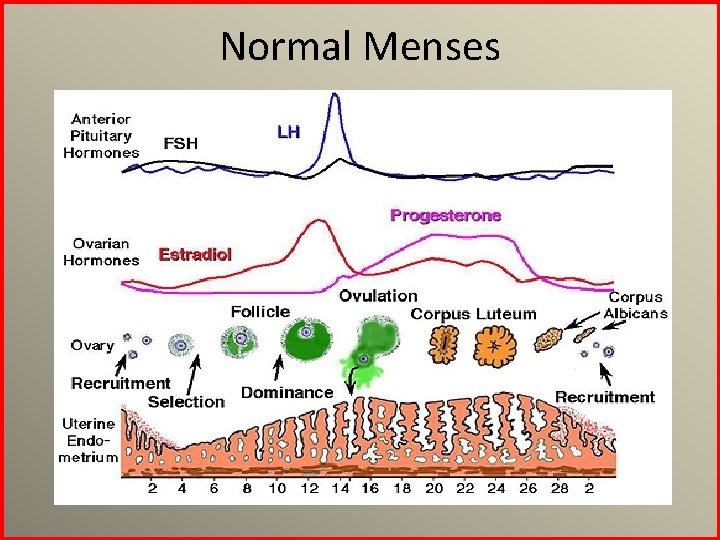
Normal Menses

Anovulatory Cycles • 55 -82% of adolescents take up to 24 months after menarche before having regular ovulatory cycles – Adolescents with later onset of menarche have longer intervals until cycles become ovulatory – Immaturity of HPO axis • Having an occasional ovulatory cycle stabilizes endometrial growth and allows for complete shedding

Madeline • On arrival to office -- History – In the midst of her 3 rd menstrual period • First one about 4 months ago and was light, lasted 5 days; Second one about 2 months ago and was moderate flow lasting 7 days – Started 8 days prior – Soaking pads every 1 -2 hours

How do you quantify bleeding? • Proposed screening questions – Period lasting > 7 days – Feeling of “flooding” or “gushing” most cycles – Activities limited by periods – Bleeding “problem” after dental extraction, surgery or delivery/miscarriage – Family history of bleeding disorder

Madeline – Additional details • ROS: feeling tired, maybe easy bruising but not sure, no acne or hirsuitism • Medications: None • Family History: Mom menarche age 13 and was irregular for 1 -2 years • Social history: Lives with Mom, in 6 th grade, has a boyfriend but no sex, no trauma, no foreign bodies in vagina

DIFFERENTIAL DIAGNOSIS

Differential for abnormal bleeding • Anovulatory uterine bleeding • Endocrine disorders • Bleeding disorders • Pregnancy-related complications • Infection • Hormonal contraception • Use of IUDs • Medications • Vaginal, cervical or uterine carcinoma, sarcoma, polyps • Cervical hemangioma • Congenital uterine abnormalities • Vaginal lacerations, trauma • Endometriosis • Foreign body

What is on our differential for Madeline? • Systematic approach • Consider pertinent history and physical
What is on our differential for Madeline? • Systematic approach – Prolactinoma – Thyroid Disease – Cushings, CAH – PCOS, Anovluation, Pregnancy, POI, Trauma, Infection, Polyp – Bleeding Disorder

EXAM CONSIDERATIONS

Exam • Key points – Vitals , Height, Weight, BMI – Features of endocrinopathies • Androgen excess • Cushingoid • Thyroid – Other signs of bleeding – GU exam • Minimum is external • Pelvic exam-most girls who have used tampons can tolerate a 1 finger digital exam to check foreign bodies

Madeline - Exam Vital Signs: BP 98/66 HR 72 T 98. 4 BMI 75 th% Gen: slightly pale and anxious-appearing Neck: no thyroid enlargement CV: soft SEM at RUSB Chest: SMR 4 breast Abd: soft, NT/ND, no striae GU: SMR 4 pubic hair, external exam without evidence of trauma, +bleeding from vagina • Skin: no hirsuitism, acne, acanthosis, petechiae, bruising • •

Any changes to the differential? • Anything move up or down the list?

LABORATORY EVALUATION

Laboratory Evaluation • • CBC with differential B-hcg (sensitive urine or serum) TSH, free T 4 Type and Screen FSH, LH, prolactin, free/total T, DHEA-S PT/PTT, von Willebrand panel GC/CT testing

Madeline - Results • CBC: Hemoglobin 10. 4 g/d. L, remainder normal • Urine hcg: negative • TSH: 255 m. IU/L, T 4 0. 5 mcg/L • Von Willebrand Panel: – VW Factor 90% (50 -160 normal) – Factor XIII 142% (70 -170 normal)

A note about VWF screening • Many factors impact VWF levels – Ideal to test off of hormones or on Day 7 of placebos • VWD <30% activity now considered diagnostic – 30 -50% is “low von Willebrand factor” • Consider screening as not uncommon in adolescents with menorrhagia – Estimates vary widely in literature with many suffering from selection bias

Role of imaging? • Consider if: – Unable to do pelvic exam – Prolonged bleeding despite treatment – Pelvic mass or uterine anomaly suspected

Next steps? • Stop bleeding • Treat underlying condition (if applicable)
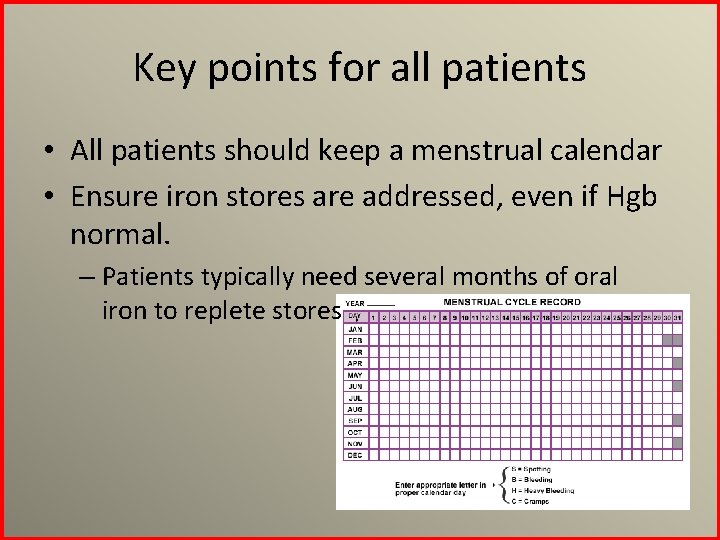
Key points for all patients • All patients should keep a menstrual calendar • Ensure iron stores are addressed, even if Hgb normal. – Patients typically need several months of oral iron to replete stores

HORMONAL TREATMENT OF BLEEDING

Recommended choice of OCPs • Off-label use • Monophasic • Potent progestin – Norgestrel (0. 3 mg) • Ex. Lo/Ovral, Low-Ogestrel, Cryselle – Levonorgestrel (0. 15 mg) • Ex. Nordette, Levlen, Levora, Portia Note: Naming brand names does not imply endorsement of a particular product

Treatment depends on current bleeding and Hgb • Mild – Menses slightly prolonged or cycle slightly more frequent – Normal hemoglobin • This can be distressing to patients and families • May observe for several cycles – Iron supplementation – Naproxen or Ibuprofen • Anti-prostaglandins have been reported to decrease blood loss • May consider treatment with OCP or progestin

Treatment depends on current bleeding and Hgb • Moderate – Menses >7 d or cycle frequency <3 weeks and mild anemia (Hgb 10 -11 g/d. L) • If patient not bleeding significantly at time of visit and is not already on hormonal therapy can start with 1 pill daily • If patient with moderate bleeding at time of visit, 1 pill BID until bleeding stops, then daily for total of 21 days – Continue cyclic pills or may do continuous • Follow Hgb as needed – Consider continuing pills at least until Hgb normal (min 3 -6 months)
Treatment depends on current bleeding and Hgb • Severe – Ongoing heavy bleeding with moderate anemia (Hgb 8 -10 g/d. L) • If bleeding is slowing and Hgb >9 g/d. L – Can start with BID pills (see moderate) • If bleeding not slowing – 1 pill q 6 h for 2 -4 days • prn anti-emetic 2 h before pill – 1 pill q 8 hx 3 days – 1 pill q 12 h for at least 2 weeks • Follow serial Hgb closely • Consider inpatient admission if concern for patient/family reliability

Treatment depends on current bleeding and Hgb • Severe – Ongoing heavy bleeding, Hgb ≤ 7 g/d. L, Orthostatic vital signs – Admit for inpatient management – Notes • Decision to transfuse not based solely on number • Most patients can be managed with OCPs • D&C rarely indicated

What if patient has contraindication to estrogen? • Medroxyprogesterone – Short courses in mild bleeding – Cyclic therapy if need ongoing • Norethindrone acetate – Short courses in mild bleeding – Cyclic therapy – Continuous menstrual suppression • LNG-IUS

INDICATIONS FOR REFERRAL

When should referral be considered? • To ER – Symptomatic anemia – Vital sign abnormalities • To Adolescent Medicine/Reproductive Endocrinology – OCP complications or decisions – Bleeding difficult to control (breaking through) – Secondary cause identified

TAKE HOME POINTS

Conclusions • Remember what is “normal” • Differential broad • History is important – Menstrual history as a “vital sign” • CBC to guide treatment • Different treatment options exist

Thank you! Contact information: Maria C. Monge, MD Director of Adolescent Medicine UTSW-Austin Pediatrics Residency Program 312 -498 -3470 mcmonge@hotmail. com
- Slides: 40