Abnormal Uterine Bleeding District 1 ACOG Medical Student

Abnormal Uterine Bleeding District 1 ACOG Medical Student Education Module 2011

Disorders of the Menstrual Cycle • • Amenorrhea Dysmenorrhea Premenstrual Syndrome Abnormal Uterine Bleeding

Abnormal Uterine Bleeding: Definitions • Menorrhagia: Heavy or prolonged uterine bleeding that occurs at regular intervals. Some sources define further as the loss of ≥ 80 m. L blood per cycle or bleeding > 7 days. • Hypomenorrhea: Periods with unusually light flow, often associated with hypogonadotropic hypogonadism (athletes, anorexia). Also may be associated with Asherman’s syndrome • Metrorrhagia: Irregular menstrual bleeding or bleeding between periods • Menometrorrhagia: Metrorrhagia associated with > 80 m. L • Polymenorrhea: Frequent menstrual bleeding. Strictly, menses occur q 21 d or less • Oligomenorrhea: Menses are > 35 d apart. Most commonly caused by PCOS, pregnancy, and anovulation

Abnormal Uterine Bleeding: Differential Diagnosis • • Structural – Cervical or vaginal laceration – Uterine or cervical polyp – Uterine leiomyoma – Adenomyosis – Cervical stenosis/Asherman’s (hypomenorrhea) Hormonal – Anovulatory bleeding – Hypogonadotropic hypogonadism – Pregnancy – Hormonal Contraception (i. e. OCPs, Depo-Provera) – Thyroid disorders – Hyperprolactinemia Malignancy – Uterine or Cervical cancer – Endometrial hyperplasia (potentially pre-malignant) Bleeding disorders – von Willebrand’s Disease, Hemophilia/Factor deficiencies, platelet disorders

Abnormal Uterine Bleeding: Workup • History – Timing of bleeding, quantity of bleeding, menstrual hx including menarche and recent periods, associated sxs, family hx of bleeding disorders • Physical – R/o vaginal or cervical source of bleeding. Bimanual may reveal bulky uterus/discrete fibroids – Assess for obesity, hirsutism, stigmata of thyroid disease, signs of hyperprolactinemia (visual field testing, galactorrhea) – Pap smear – Endometrial biopsy, if appropriate • Pregnancy Test • Imaging – Pelvic ultrasound – Sonohystogram or hysterosalpingogram • Surgical – Hysteroscopy – D&C
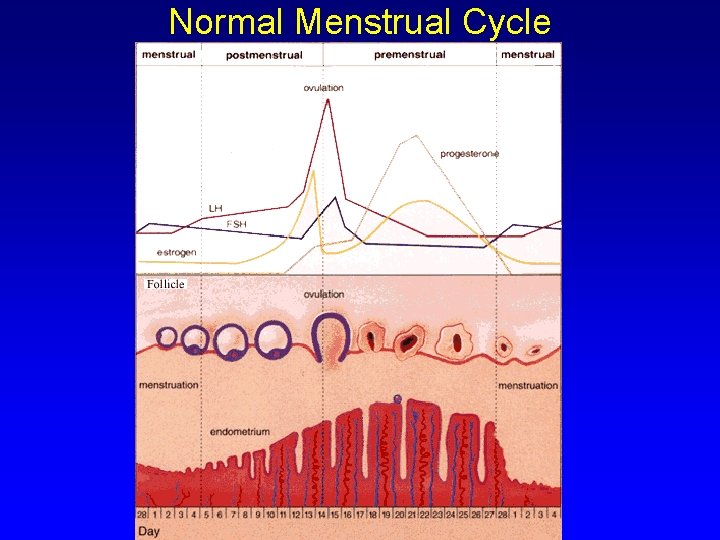
Normal Menstrual Cycle

Normal Ovulatory Cycle • Follicular development ovulation (d 14) corpus luteal function luteolysis • Endometrium is exposed to: – Ovarian production of estrogen (proliferation) – Combination of estrogen and progesterone (secretory phase) – Estrogen and progesterone withdrawal (desquamation and repair)

Anovulatory Bleeding • Corpus luteum is not produced – Ovary fails to secrete progesterone, although estrogen production continues – Result is continuous, unopposed E stimulation of endometrium: • Endometrial proliferation without P-induced differentiation / stabilization – Endometrium becomes excessively vascular without stromal support fragility and irregular endometrial bleeding

Anovulatory Bleeding: Etiologies • Hyperandrogenic anovulation (PCOS, CAH, androgen-producing tumors) • Hypothalamic dysfunction (stress, anorexia, exercise) • Hyperprolactinemia • Hypothyroidism • Primary pituitary disease • Premature ovarian failure • Iatrogenic (secondary to radiation or chemo)

Anovulatory Bleeding: Adolescents (13 -18 years) • Anovulatory bleeding may be normal physiologic process, with ovulatory cycles not established until 1 -2 yrs after menarche (immature HPG axis) • Screen for coagulation disorders (PT/PTT, plts) • May be caused by leukemia, ITP, hypersplenism • Consider endometrial bx in adolescents with 2 -3 year history of untreated anovulatory bleeding, especially if obese

Anovulatory Bleeding: Management in Adolescents • High dose estrogen therapy for acute bleeding episodes (promotes rapid endometrial growth to cover denuded endometrial surfaces): conjugated equine estrogens PO up to 10 mg/d in 4 divided doses or IV 25 mg q 4 hrs for 24 hrs • Treat pts with blood dyscrasias for their specific diseases, r/o leukemia • Prevent recurrent anovulatory bleeding with: • cyclic progestin (i. e. Provera) or • low dose (≤ 35 μg ethinyl estradiol) oral contraceptive – suppresses ovarian and adrenal androgen production and increases SHBG decreasing bioavailable androgens

Anovulatory Bleeding: Reproductive Age (19 -39 years) • Anovulatory bleeding not considered physiologic, evaluation required • 6 -10% of women have hyperandrogenic chronic anovulation (i. e. PCOS), characterized by noncyclic bleeding, hirsutism, obesity (BMI ≥ 25) – Underlying biochemical abnormalities: noncyclic estrogen production, elevated serum testosterone, hypersecretion of LH, hyperinsulinemia. – h/o rapidly progressing hirsutism with virilization suggests tumor • Lab testing: HCG, TSH, fasting serum prolactin – If androgen-producing tumor is suspected, serum DHEAS and testosterone levels – If POF suspected, serum FSH • Chronic anovulation resulting from hypothalamic dysfunction (dx’d by low FSH level) may be due to excessive psychologic stress, exercise, or weight loss

Anovulatory Bleeding: Reproductive Age (19 -39 yrs) When is endometrial evaluation indicated? • Sharp increase in incidence of endometrial CA from 2. 3/100, 000 ages 30 -34 yrs 6. 1/100, 000 ages 35 -39 yrs • Therefore, endometrial bx to exclude CA is indicated in any woman > 35 yrs old with suspected anovulatory bleeding • Pts 19 -35 who don’t respond to medical therapy or have prolonged periods of unopposed estrogen 2/2 anovulation merit endometrial bx

Anovulatory Bleeding: Reproductive Age (19 -39 yrs) Medical therapies • Can be treated safely with either cyclic progestin or OCPs, similar to adolescents. • Estrogen-containing OCPs – relatively contraindicated in women with HTN or DM – contraindicated for women > 35 who smoke or have h/o thromboembolic dz • If pregnancy is desired, ovulation induction with clomid is initial tx of choice – Can induce withdrawal bleed with progestin (i. e. provera), followed by initiation of therapy with Clomid, 50 mg/d for 5 days, starting b/t days 3 and 5 of menstrual cycle

Anovulatory Bleeding: Later Reproductive Age (40 -Menopause) • Incidence of anovulatory bleeding increases toward end of reproductive years • In perimenopausal women, onset of anovulatory cycles is due to declining ovarian function. • Can initiate hormone therapy for cycle control When is endometrial evaluation indicated? • Incidence of endometrial CA in women 40 -49 years: 36. 2/100, 000 • All women > 40 yrs who present with suspected anovulatory bleeding merit endometrial bx after excluding pregnancy

Anovulatory Bleeding: Later Reproductive Age (40 -Menopause) Medical therapy • Cyclic progestin, low-dose OCPs, or cyclic HRT are all options • Women with hot flashes secondary to decreased estrogen production can have symptomatic relief with ERT in combination with continuous or cyclic progestin

Anovulatory Bleeding: Later Reproductive Age (40 -Menopause) • • Surgical therapy Surgical options include: hysterectomy and endometrial ablation Surgical tx only indicated when medical mgmt has failed and childbearing complete Some studies suggest hysterectomy may have higher long-term satisfaction than ablation Endometrial ablation: Nova. Sure, thermal balloon – YAG laser and rollerball less widely-used currently – 45% of women achieve amenorrhea after YAG laser or resectoscope. 12 month post-op satisfaction is 90%. Only 15% of women achieve amenorrhea after thermal balloon ablation, and 1 yr satisfaction rate still 90% – Long-term satisfaction with ablation may be lower: • in 3 -year f/u study, 8. 5% of women who had undergone ablation were re-ablated, an additional 8. 5% had hyst • In a 5 -year follow up study, 34% of women who underwent ablation later had a hyst.
- Slides: 17