ABNORMAL PRESENTATION BREECH DEF In longitudinal lie when

ABNORMAL PRESENTATION— BREECH DEF: In longitudinal lie when the podalic pole of fetus is at pelvic brim. INCIDENCE: 20% at 28 weeks (9 times commoner compared to that at term) 5% at 34 weeks 3% at term 1
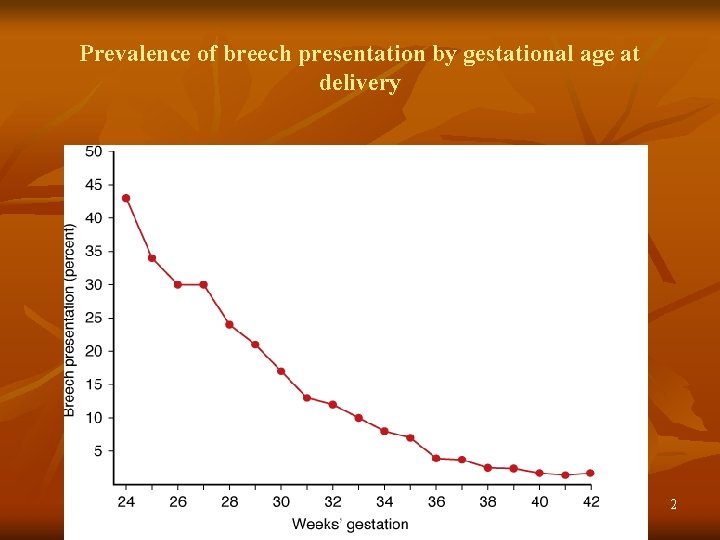
Prevalence of breech presentation by gestational age at delivery 2

TYPES n 1) Complete / Flexed Breech n 2) Incomplete n n n a) Breech with extended legs (frank breech) (>in primi) b) Knee presentation (>in multi) c) Footling presentation (>in multi) n Uncomplicated breech: no other obst. complication present except breech. n Complicated breech: complicating factors like PP, CPD, DM, TWINS. n Abnormal breech delivery: Extended legs, arms, nuchal displacement 3
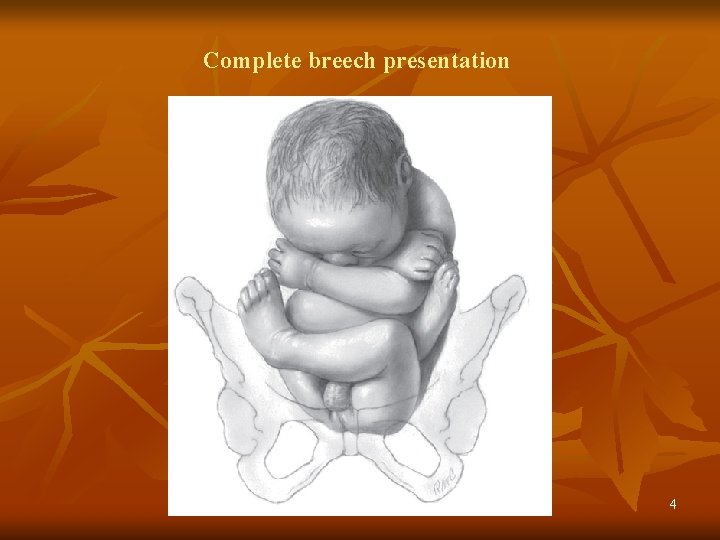
Complete breech presentation 4
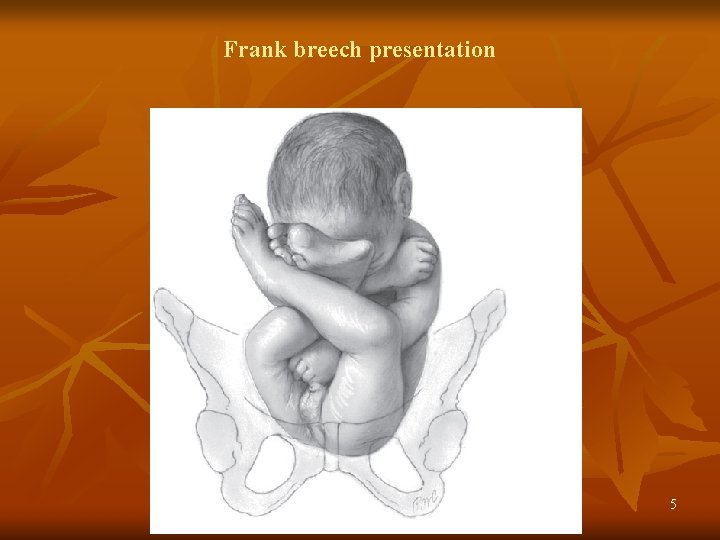
Frank breech presentation 5
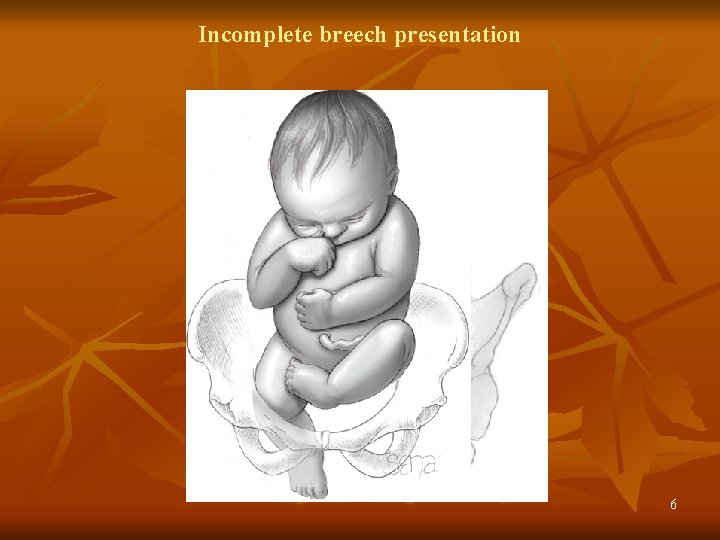
Incomplete breech presentation 6

BREECH PRESENTATION AETIOLOGY 1. Fetal Factors: Prematurity—At 28 weeks -- 9 times commoner compared to term Fetal death, Fetal deformity- hydrocephalus, anencephaly Breech with extended legs Short cord 7

BREECH PRESENTATION AETIOLOGY 2) Maternal factors: Uterine. & abdominal. muscle tone > in primi…. . breech with ext. legs occures < in multi…. . . complete breech Fundal Placental /cornual placenta smaller head occupies fundus Placenta praevia knee / footling /frank breech Hydramnios / olihydramnios 8 Vendittelli and colleagues (2008) recently described a twofold incidence of breech presentation and prior cesarean delivery.

BREECH PRESENTATION AETIOLOGY 3) Reccurent / Habitual breech: 40% of cases Malformations of uterus-like Septate uterus, Bicornuate uterus Unicornuate uterus 4) Idiopathic: 25% of cases 9

ABNORMAL PRESENTATION— BREECH DIAGNOSIS: (A) during ante-natal period H /O/: previous h/o breech h/o epigastric pain Signs: P /A Inspection- irregularity in upper part of ut. In thin lean pt. Palpation- F/H, Abd. Girth- corrospond to single foetus Fundal grip--head Lateral grip—back or limbs palpated ant. or post. Pelvic grip-----breech Auscultation- FHS higher in comp. breech, lower in frank breech P /V Non conclusive as cervix is not dilated 10

ABNORMAL PRESENTATION— BREECH D/D: 1) Comp. breech & Frank breech 2) breech from other presentations sacro-ant breech-----from OA sacro-post breech ------ from OP 11

DIAGNOSIS: (B) during labour H/O, P/A-inspection, palpation, auscultation, D/D: -same as ANC P/V: Cervical dilatation, effacement, bag of membrane, elongated in footling & knee presentations identify breech &D/D from face D/D frank& complete breech & knee & footling & figer & toes Pelvis assessment 12

Why feto pelvic evaluation? n n n Because most are preterm, in many fetuses, the breech is smaller than the aftercoming head. Moreover, unlike cephalic presentations, the head of a breech-presenting fetus is not permitted to undergo molding during labor. Thus to avoid trapping of the head following delivery of the breech, pelvic dimensions should be assessed prior to vaginal delivery. In addition, the type of breech and degree of neck flexion or extension should be identified. To evaluate these, there are several imaging techniques. 13

Sonography is the best confirmation of a suspected breech presentation It can provide information regarding the breech type and neck angle (Fontenot and associates, 1997; Rojansky and colleagues, 1994). The role of radiographic pelvimetry to help determine the mode of delivery for breech presentation is controversial Computed tomographic (CT) scanning also can be used and will also provide pelvic measurements and configuration with lower doses of radiation than standard radiographs Magnetic resonance (MR) imaging provides reliable information about pelvic capacity and architecture without ionizing radiation, but it is not always readily available (van Loon and colleagues, 1997). 14

ABNORMAL PRESENTATION— BREECH INVESTIGATIONS: A) For diagnosis : - USG B) For management: 1) Routine: - Hb. , Bl. Group&Rh , Urine ---Routine& micro 2) Specific as & when required IS BREECH DELIVERY SAFE: Maternal Risk: - > morbidity as LSCS are > : trauma , bleeding, infection Fetal Risk: -Perinatal mortality in uncomplicated breech 3 -10% Perinatal mortality in developing countries 5 -30% ( Intracranial haemorrhage, Asphyxia , Injuries of muscle, nerve , bone, viscera) 15

Maternal Morbidity how & why n n Because of the greater frequency of operative delivery, there is a higher rate of maternal morbidity for pregnancies complicated by persistent breech presentation. The most worrisome are genital tract lacerations. Intrauterine maneuvers, especially with a thinned lower uterine segment, or delivery of the aftercoming head through an incompletely dilated cervix, may cause rupture of the uterus, lacerations of the cervix and vaginal walls, or both. Such manipulations also may lead to extensions of the episiotomy and deep perineal tears. Anesthesia sufficient to induce appreciable uterine relaxation may cause uterine atony and in turn, postpartum hemorrhage. Finally, manual manipulations within the birth canal increase the risk of infection. The maternal mortality rate may even be increased. Schutte and colleagues (2007) reported the deaths of four women in the Netherlands from 2000 to 2002 as a result of elective cesarean delivery for breech presentation—a case fatality rate of 0. 47 maternal deaths per 1000 births. 16

ABNORMAL PRESENTATION— BREECH MANAGEMENT IN ANTE-NATAL PERIOD ECV: 1) Indications. 2) Contra-indications. 3) Time & place. 4) Explanation & consent. 5) Analgesia, anesthesia, uterine relaxants. 6) Principles of procedure. 7) Dangers. 8) Aetiology of failure. 9) Treatment of failure. 17
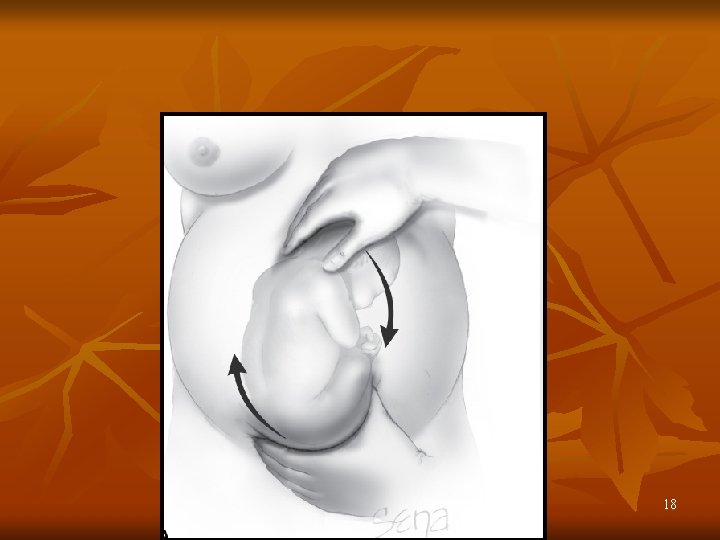
18
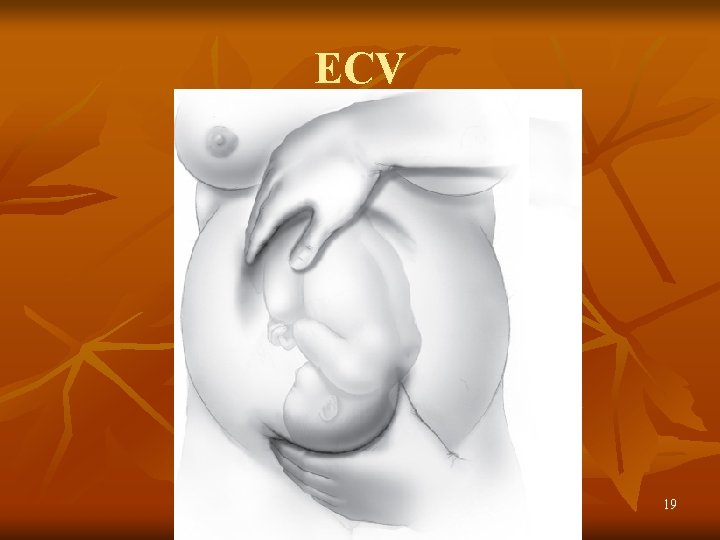
ECV 19

Current Status of Vaginal Breech Delivery The Randomised Multicentre Trial (Hannah and colleagues - 2000) The trial included -- 1041 women randomly assigned to planned cesarean -- 1042 to planned vaginal delivery. (In the planned vaginal delivery group, 57 percent were actually delivered vaginally. ) Overall, planned cesarean delivery compared with planned vaginal delivery— had Lower risk of perinatal mortality 3 per 1000 versus 13 per 1000. Lower risk of "serious" neonatal morbidity— 1. 4 versus 3. 8 percent. Maternal complications were similar between the groups. 20

American College of Obstetricians and Gynecologists published Committee Opinion in 2001 Women with persistent singleton breech presentation at term (Except in cases of "advanced labor" and "imminent delivery”) should undergo a planned cesarean delivery. 21

single-center studies that support a trial of vaginal delivery for selected breech-presenting term fetuses. Irion and associates (1998) fewer maternal complications, but no difference in corrected neonatal morbidity or mortality rates between 385 attempted vaginal breech deliveries— 70 percent of whom were delivered vaginally—and 320 planned cesarean deliveries. Giuliani and associates (2002) reported that in their institution, vaginal breech delivery was performed in half of 699 consecutive, term, breech-presenting fetuses. There were no short- or long-term differences in outcomes for fetuses delivered by either route. Alarab and associates (2004) reported no serious adverse neonatal outcomes in the fourth of 146 term breech fetuses delivered vaginally over a 31/2 -year period. Excellent outcomes for singleton breech fetuses after planned vaginal birth have 22 also been reported by Uotila (2005), Krupitz (2005), Pradhan (2005), and their colleagues.

large prospective European study were reported by Goffinet and co-workers (2006). Analyzed outcomes of 8105 term singleton breech-presenting fetuses from 174 French and Belgium hospitals. Vaginal delivery was planned with fairly stringent guidelines in about a third—(2526) of these women, (successful in 1796 of these— 71 percent. ) The perinatal mortality or serious neonatal morbidity rates were low. Importantly, they did not differ between the planned vaginal and planned cesarean group— 1. 6 versus 1. 5 percent, respectively. 23

Recommendations for Delivery I. III. IV. V. VIII. IX. X. XI. Cesarean delivery is commonly, but not exclusively, used in the following circumstances: A large fetus Fetopelvic disproportion A hyper extended head When delivery is indicated in the absence of spontaneous labor Uterine dysfunction—some would use oxytocin augmentation Incomplete or footling breech presentation An apparently healthy and viable preterm fetus with the mother in either active labor or in whom delivery is indicated Severe fetal-growth restriction Previous perinatal death or children suffering from birth trauma -- BOH A request for sterilization Lack of an experienced operator. 24

ABNORMAL PRESENTATION— BREECH MANAGEMENT IN LABOUR PATIENT COMES TO YOU D + D / D + INVESTIGATIONS + DECIDE FOR LSCS / VAGINAL DELIVERY VAGINAL…………………. . V / S……………. . . . …………. . LSCS H/O previous breech+ No disproportion No complicating factor + Spontaneous labor & progress+ Skill full obstetrician Anesthesia facility+ Disproportion Distress Precious preg. Prolonged labour with ut. dysfunction Scarred uterus Preterm, footling, hyper extended head 25

26

27

ABNORMAL PRESENTATION— BREECH FIRST STAGE: - Similar as normal labor except— 1) complete rest in bed to preserve membranes 2) Nil orally ----I / V drip 3) P/V ---a must to rule out feto- pelvic disproportion SECOND STAGE: Preparations to be made: - Doctors + Assistants + Instruments 28

THREE methods of vaginal breech delivery are 1. Spontaneous Br. delivery Mother does all efforts, doctor just supports 10% 2. Total breech extraction Doctor does all efforts Very rarely done 3. Assisted breech / Partial breech extraction - The fetus is delivered spontaneously as far as the umbilicus. Both do the efforts thereafter 29 Most commonly done

PRINCIPLES OF CONDUCTING SAFE BREECH DELIVERY General 1) Doctor must be calm & slow. 2) Mother must bear down hard. Apply fundal pressure during uterine. Contractionto assist bearing down efforts of mother. At delivry of buttocks 3) Give episiotomy when buttocks climb the perineum. Never pull breech , allow spontaneous delivery, hands get extended. wrap baby in wet warm towel. At delivery of shoulders 4) wait till shoulders make no attempts to deliver shoulder until one axilla is seen At delivery of head 5) For delivery of head , allow it to be fully flexed, never look for cord pulsations. they are bound to be slow. Hasty delivery of head may cause intracranial bld. 30

ABNORMAL PRESENTATION— BREECH n n n COMPLICATED BREECH DELIVERY……. . ie OBSTRUCTION OF Following at various levels like Pelvic floor Mid pelvis Pelvic inlet 1)Buttocks……………. . . 2)Shoulder…………… 3)Head Kristeller Classical Mauriceau-smellie-veit Groin traction Lovset Prague Groin hook Nuchal Killands Pinard LSCS 31
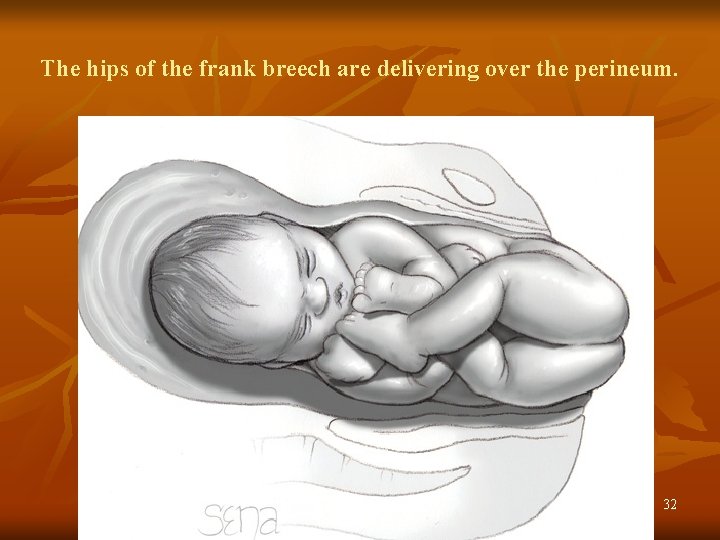
The hips of the frank breech are delivering over the perineum. 32

Hold fetus from pelvis & not abdomen and apply Gentle downward rotational traction 33
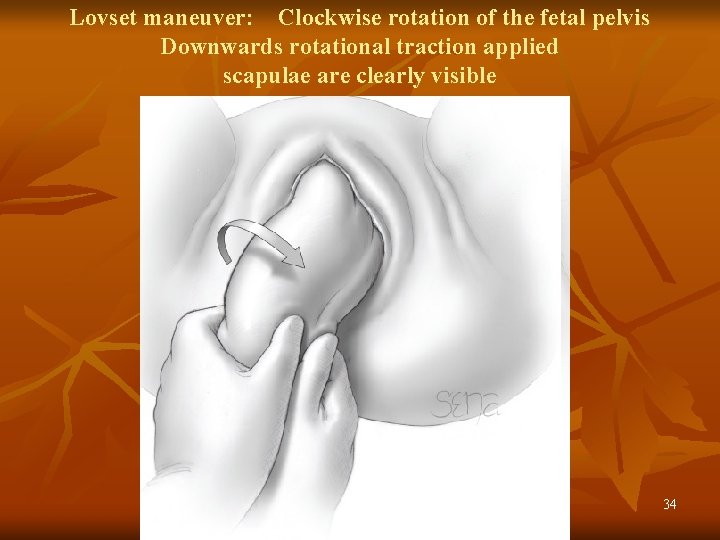
Lovset maneuver: Clockwise rotation of the fetal pelvis Downwards rotational traction applied scapulae are clearly visible 34
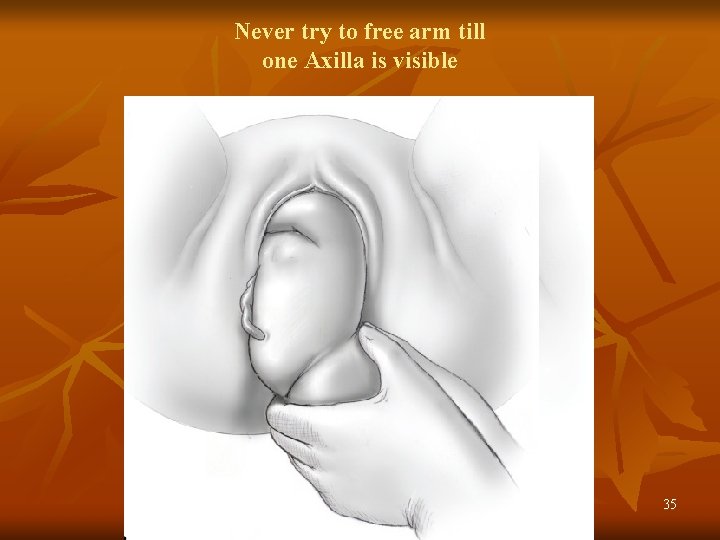
Never try to free arm till one Axilla is visible 35
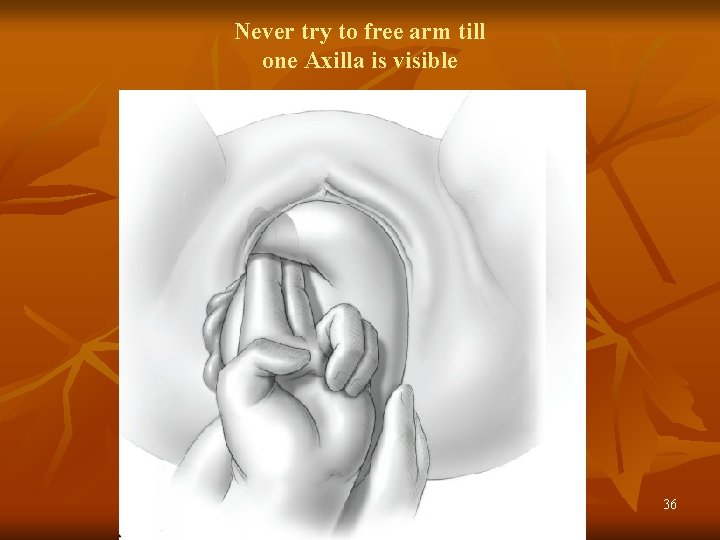
Never try to free arm till one Axilla is visible 36
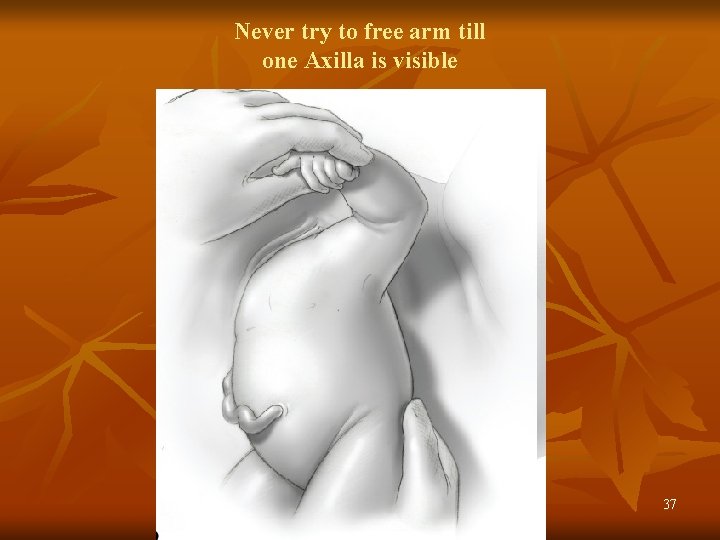
Never try to free arm till one Axilla is visible 37
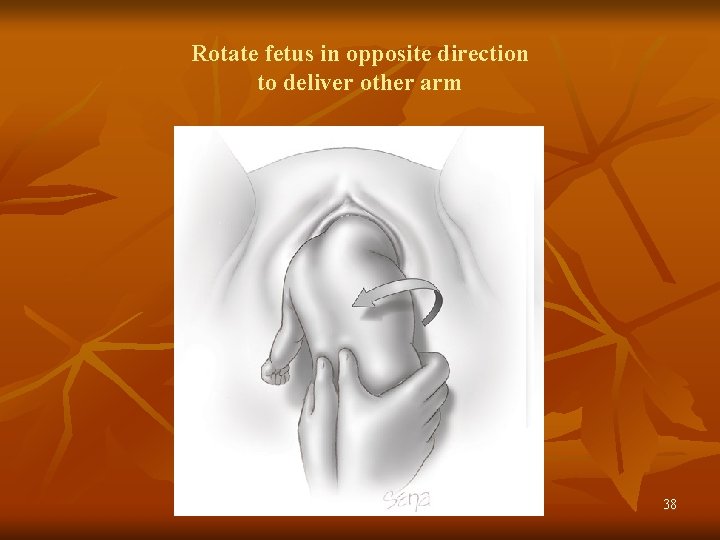
Rotate fetus in opposite direction to deliver other arm 38
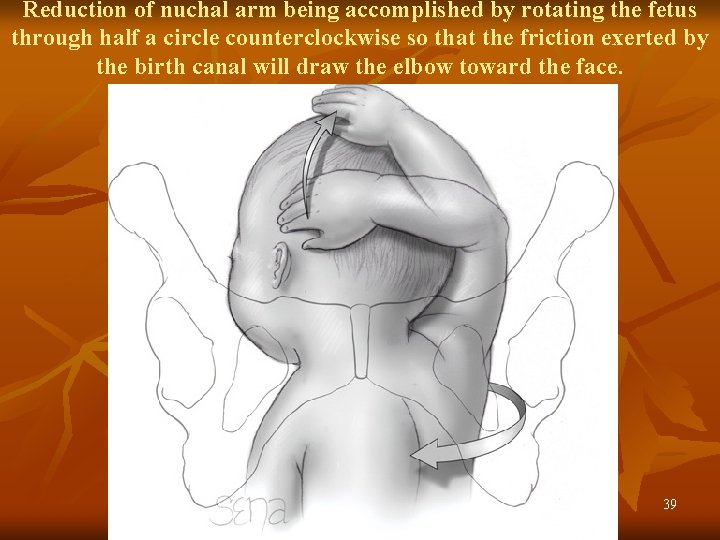
Reduction of nuchal arm being accomplished by rotating the fetus through half a circle counterclockwise so that the friction exerted by the birth canal will draw the elbow toward the face. 39
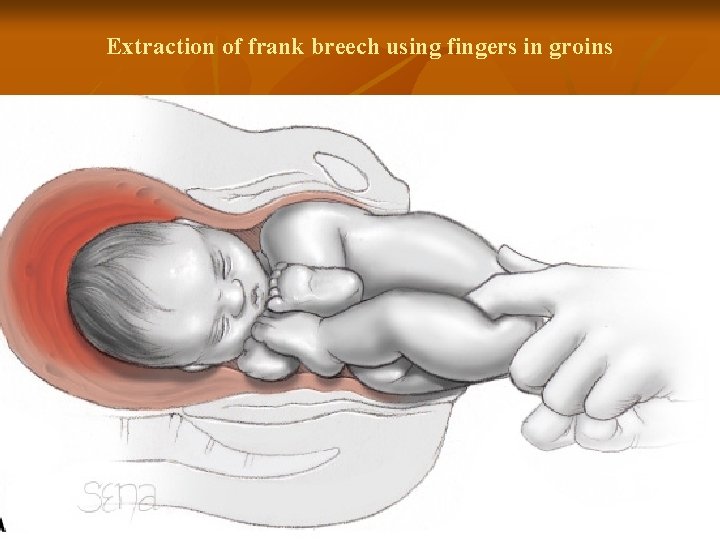
Extraction of frank breech using fingers in groins 40
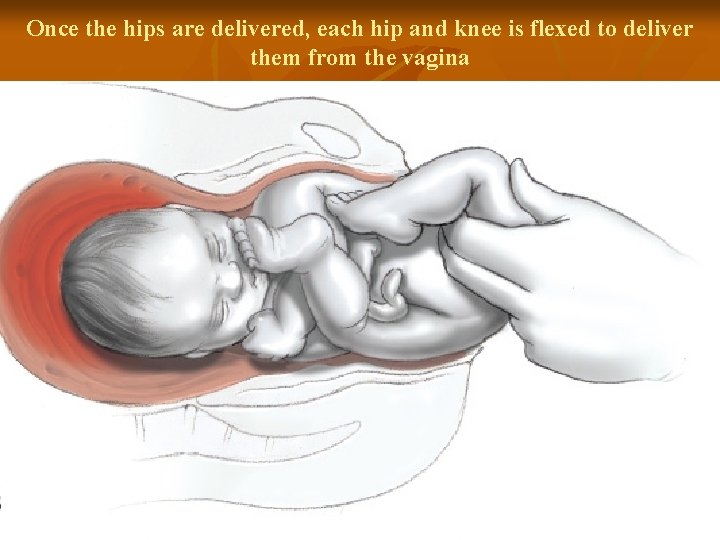
Once the hips are delivered, each hip and knee is flexed to deliver them from the vagina 41
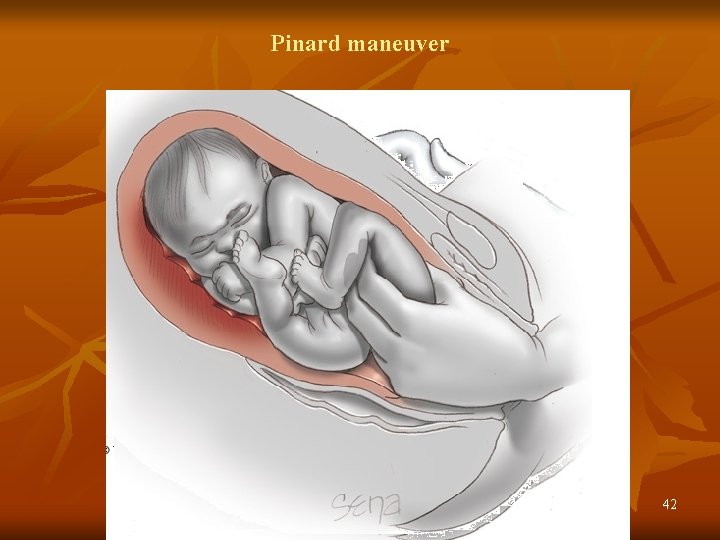
Pinard maneuver 42

Complete breech extraction begins with traction on the feet and ankles. 43
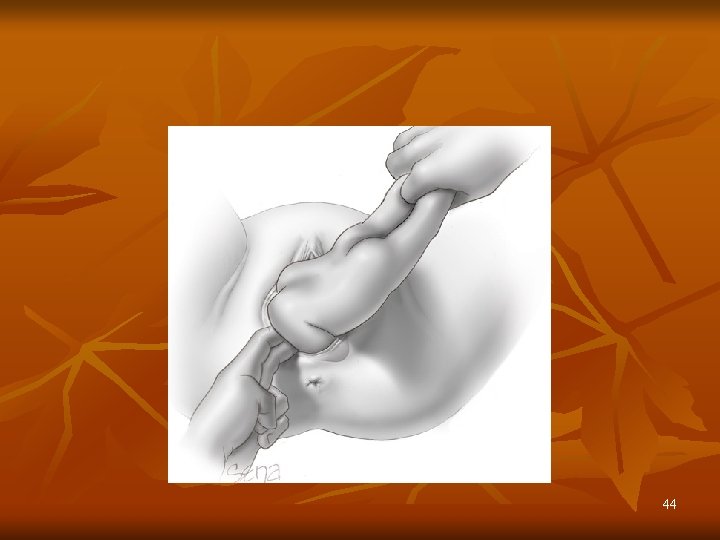
44
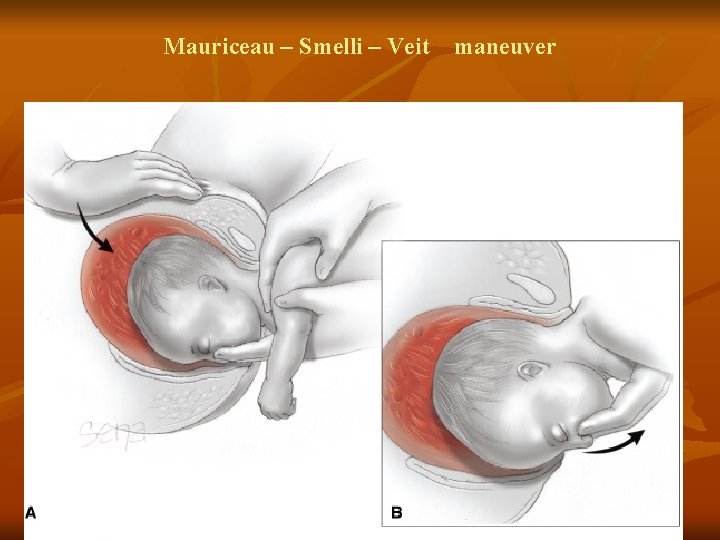
Mauriceau – Smelli – Veit maneuver 45
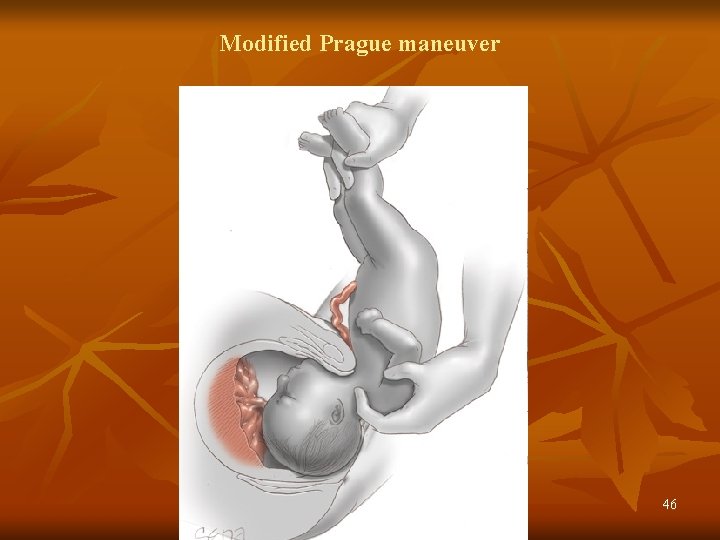
Modified Prague maneuver 46
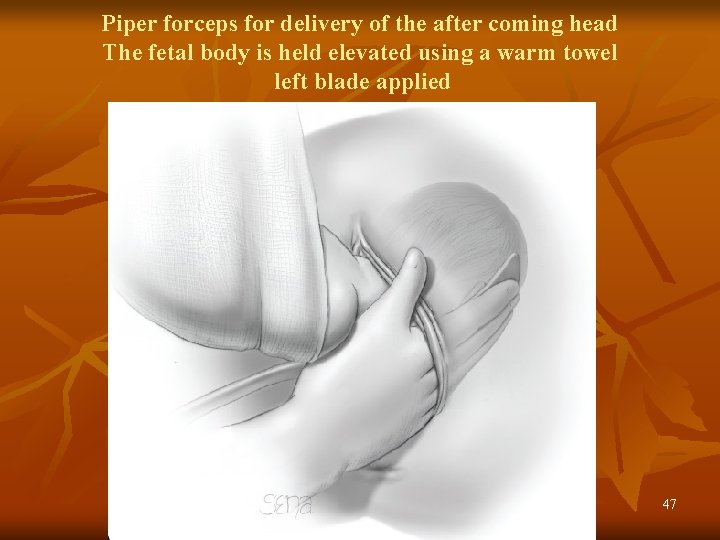
Piper forceps for delivery of the after coming head The fetal body is held elevated using a warm towel left blade applied 47

Piper forceps for delivery of the after coming head with the body still elevated The right blade applied 48
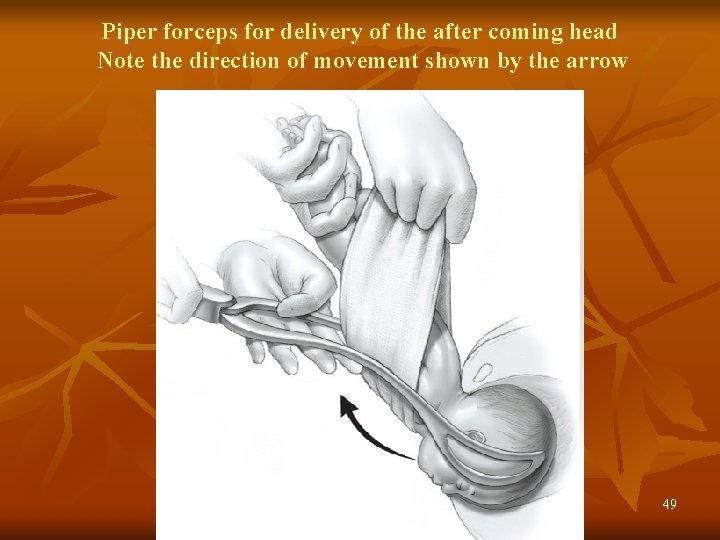
Piper forceps for delivery of the after coming head Note the direction of movement shown by the arrow 49
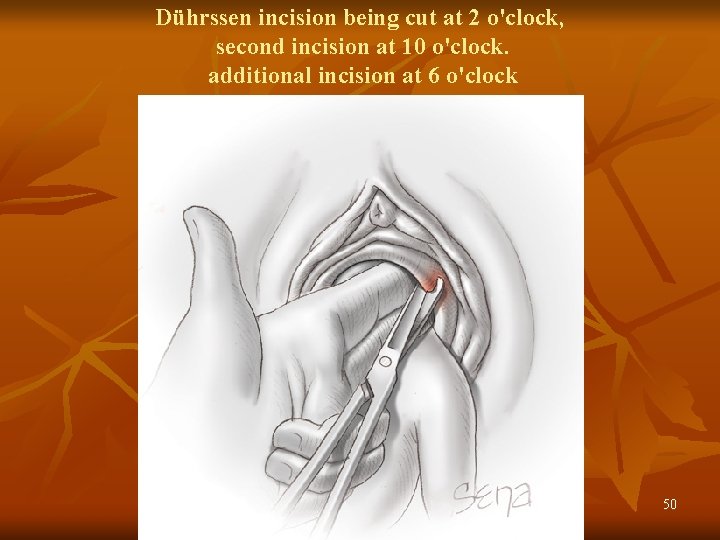
Dührssen incision being cut at 2 o'clock, second incision at 10 o'clock. additional incision at 6 o'clock 50

51
- Slides: 51