ABNORMAL LFTS IS THERE REALLY SOMETHING WRONG WITH

ABNORMAL LFT’S: IS THERE REALLY SOMETHING WRONG WITH ME? Marilyn Zeman GI for GPs April 2019

FACULTY/PRESENTER DISCLOSURE • Faculty: University of Alberta • Relationships with financial sponsors: • none

OBJECTIVES • Appropriate investigations for abnormal liver enzymes • Determine which patient should have liver enzymes performed • Understand updates in HCV treatment
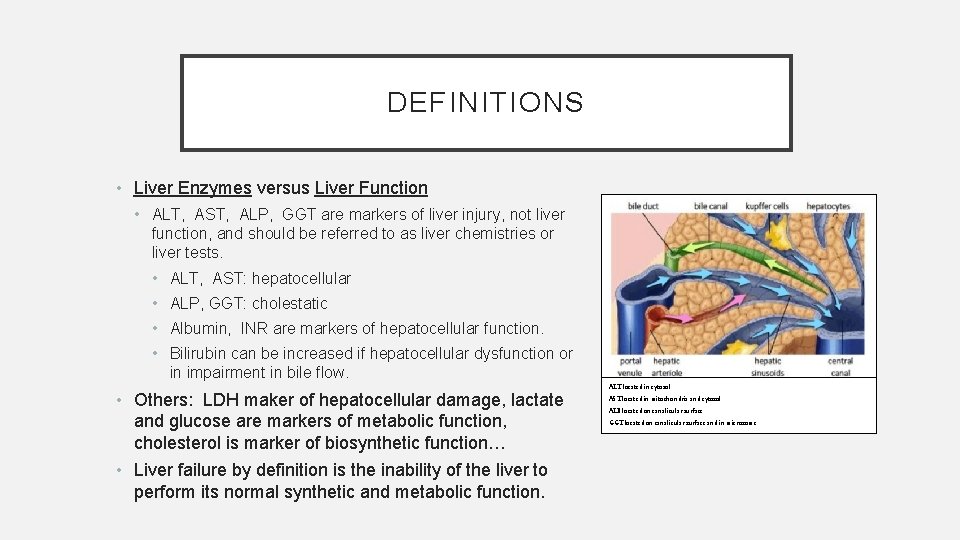
DEFINITIONS • Liver Enzymes versus Liver Function • ALT, AST, ALP, GGT are markers of liver injury, not liver function, and should be referred to as liver chemistries or liver tests. • ALT, AST: hepatocellular • ALP, GGT: cholestatic • Albumin, INR are markers of hepatocellular function. • Bilirubin can be increased if hepatocellular dysfunction or in impairment in bile flow. • Others: LDH maker of hepatocellular damage, lactate and glucose are markers of metabolic function, cholesterol is marker of biosynthetic function… • Liver failure by definition is the inability of the liver to perform its normal synthetic and metabolic function. ALT located in cytosol AST located in mitochondria and cytosol ALP located on canalicular surface GGT located on canalicular surface and in microsome
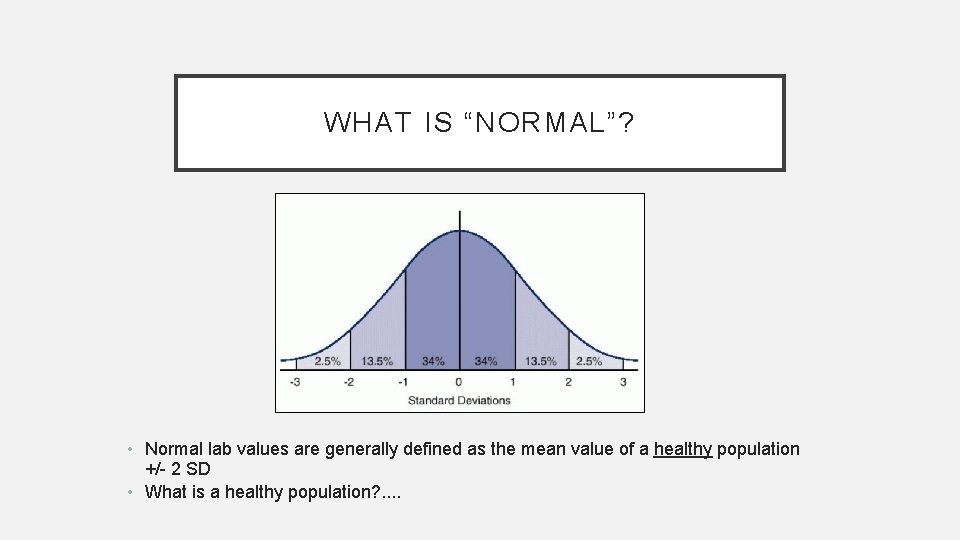
WHAT IS “NORMAL”? • Normal lab values are generally defined as the mean value of a healthy population +/- 2 SD • What is a healthy population? . .

OBJECTIVES • Appropriate investigations for abnormal liver enzymes • Determine which patient should have liver enzymes performed • Understand updates in HCV treatment

OBJECTIVES • Appropriate investigations for abnormal liver enzymes • Determine which patient should have liver enzymes performed • Understand updates in HCV treatment

DEFINITIONS IN EVALUATION OF ABNORMAL LIVER ENZYMES • Acute versus chronic • Defined as 6 months • Hepatic versus cholestatic • R ratio is calculated by formula R = (ALT value/ ALT ULN) � (ALP value/ ALP ULN) • R ratio < 2 is cholestatic, > 5 hepatocellular, 2 -5 is mixed • Severity of abnormality • “Borderline” ALT, AST < 2 ULN • “Mild” ALT, AST 2 -5 x ULN • “Moderate” ALT, AST 5 -15 x ULN • “Severe” ALT, AST > 15 x ULN • “Massive” ALT, AST > 10, 000 IU/L Kwo et al. ACG Practice Guidelines: Evaluation of Abnormal Liver Chemistries. Amer. J Gastro. 2016
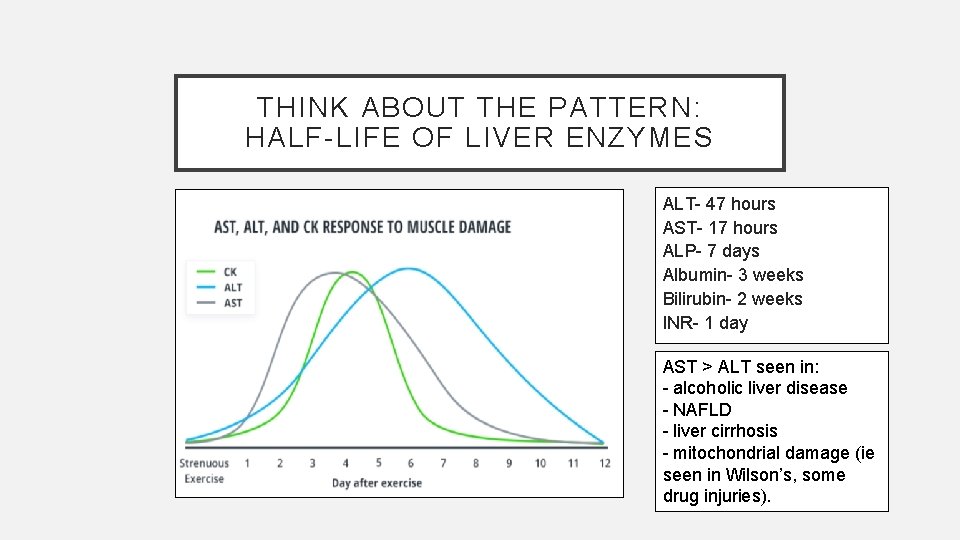
THINK ABOUT THE PATTERN: HALF-LIFE OF LIVER ENZYMES ALT- 47 hours AST- 17 hours ALP- 7 days Albumin- 3 weeks Bilirubin- 2 weeks INR- 1 day AST > ALT seen in: - alcoholic liver disease - NAFLD - liver cirrhosis - mitochondrial damage (ie seen in Wilson’s, some drug injuries).
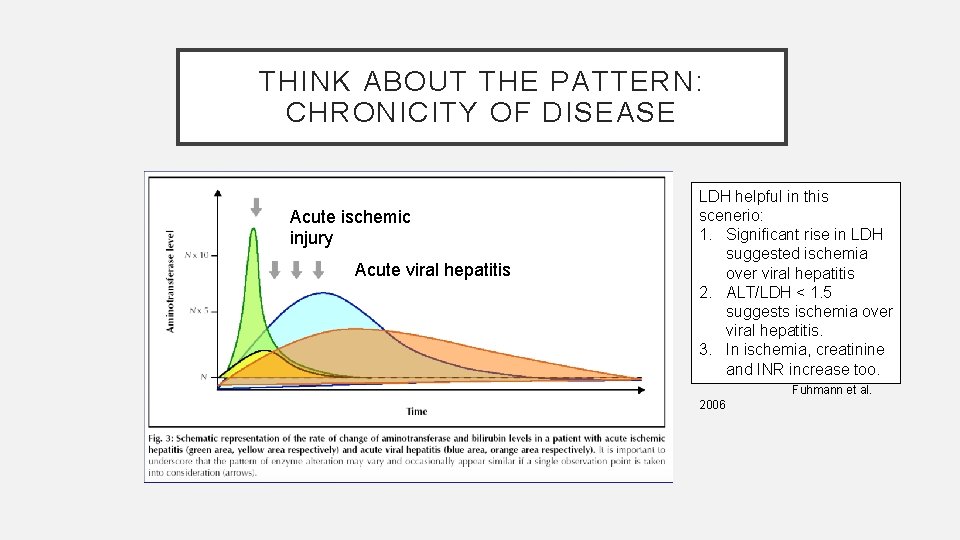
THINK ABOUT THE PATTERN: CHRONICITY OF DISEASE Acute ischemic injury Acute viral hepatitis LDH helpful in this scenerio: 1. Significant rise in LDH suggested ischemia over viral hepatitis 2. ALT/LDH < 1. 5 suggests ischemia over viral hepatitis. 3. In ischemia, creatinine and INR increase too. Fuhmann et al. 2006
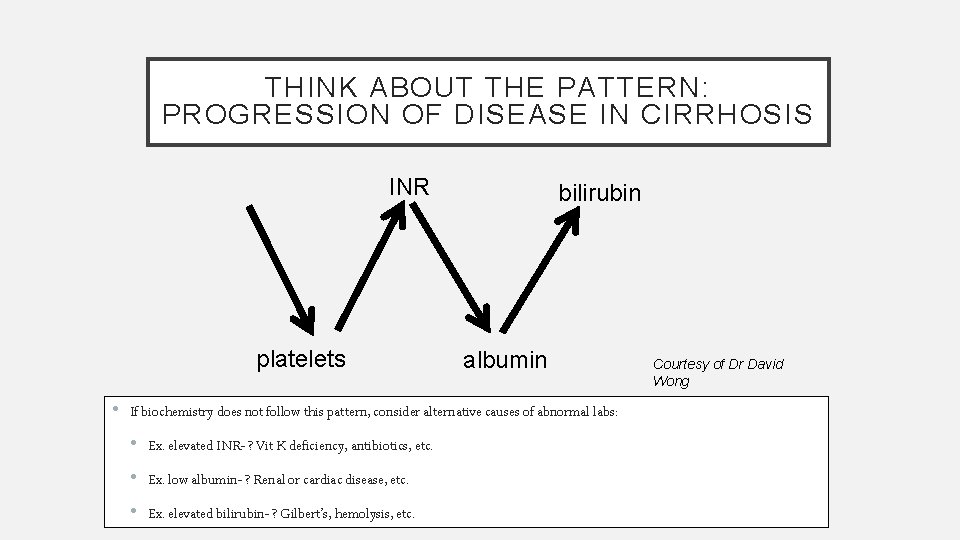
THINK ABOUT THE PATTERN: PROGRESSION OF DISEASE IN CIRRHOSIS INR platelets bilirubin albumin • If biochemistry does not follow this pattern, consider alternative causes of abnormal labs: • Ex. elevated INR- ? Vit K deficiency, antibiotics, etc. • Ex. low albumin- ? Renal or cardiac disease, etc. • Ex. elevated bilirubin- ? Gilbert’s, hemolysis, etc. Courtesy of Dr David Wong
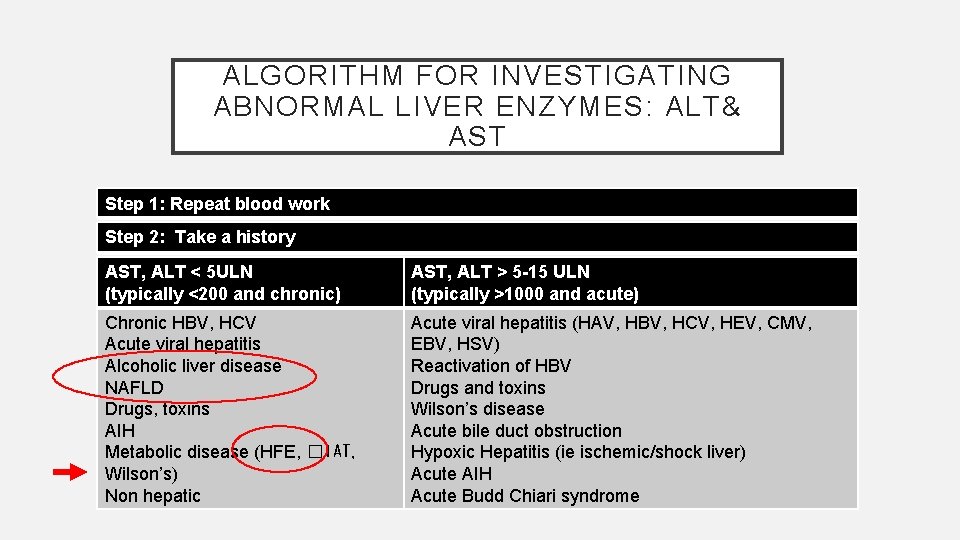
ALGORITHM FOR INVESTIGATING ABNORMAL LIVER ENZYMES: ALT& AST Step 1: Repeat blood work Step 2: Take a history AST, ALT < 5 ULN (typically <200 and chronic) AST, ALT > 5 -15 ULN (typically >1000 and acute) Chronic HBV, HCV Acute viral hepatitis Alcoholic liver disease NAFLD Drugs, toxins AIH Metabolic disease (HFE, � 1 AT, Wilson’s) Non hepatic Acute viral hepatitis (HAV, HBV, HCV, HEV, CMV, EBV, HSV) Reactivation of HBV Drugs and toxins Wilson’s disease Acute bile duct obstruction Hypoxic Hepatitis (ie ischemic/shock liver) Acute AIH Acute Budd Chiari syndrome
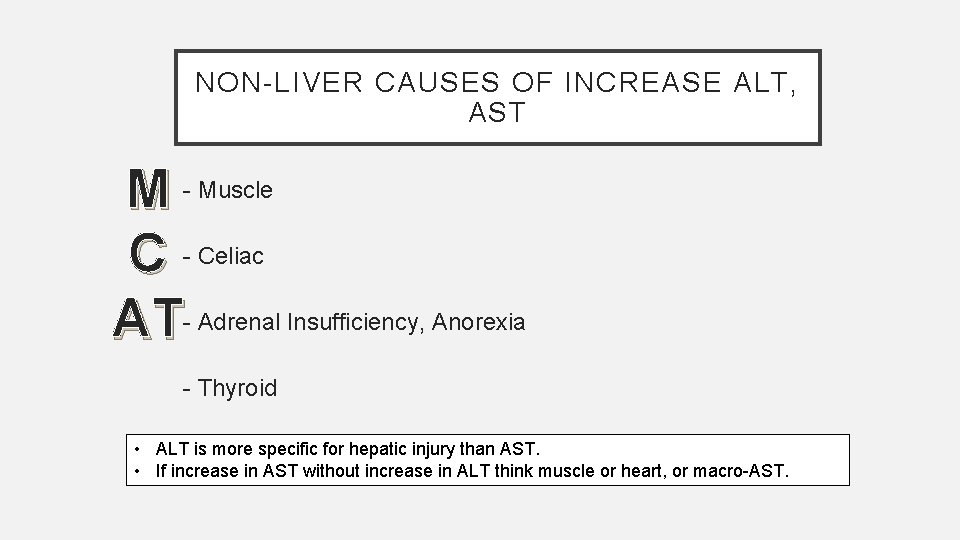
NON-LIVER CAUSES OF INCREASE ALT, AST M - Muscle C - Celiac AT- Adrenal Insufficiency, Anorexia - Thyroid • ALT is more specific for hepatic injury than AST. • If increase in AST without increase in ALT think muscle or heart, or macro-AST.
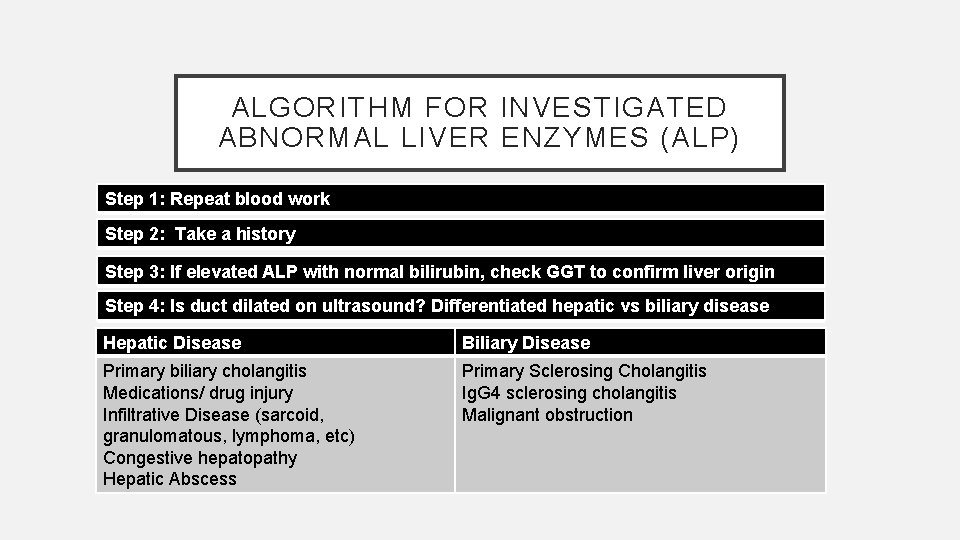
ALGORITHM FOR INVESTIGATED ABNORMAL LIVER ENZYMES (ALP) Step 1: Repeat blood work Step 2: Take a history Step 3: If elevated ALP with normal bilirubin, check GGT to confirm liver origin Step 4: Is duct dilated on ultrasound? Differentiated hepatic vs biliary disease Hepatic Disease Biliary Disease Primary biliary cholangitis Medications/ drug injury Infiltrative Disease (sarcoid, granulomatous, lymphoma, etc) Congestive hepatopathy Hepatic Abscess Primary Sclerosing Cholangitis Ig. G 4 sclerosing cholangitis Malignant obstruction
NON-LIVER CAUSES OF INCREASED ALP • Bone • Placenta • Intestine • Kidney

WHAT’S THE DEAL WITH GGT? • “Given its lack of specificity for liver disease, GGT should not be used as a screening test for underlying liver disease in the absence of other abnormal liver chemistries. ” • strong recommendations, very low level of evidence ACG practice guidelines. Kwo et al. Amer J Gastro 2016 • “GGT elevated in patients with pancreatic disease, myocardial infarction, renal failure, emphysema, diabetes, and in patients taking certain medications such as phenytoin and barbiturates. ” Lum et al. Clin. Chem. 1972 • GGT is associated with CVD and all cause mortality in multiple studies. Wannamwthee G et al. 1995; Kunutsor SK et al.
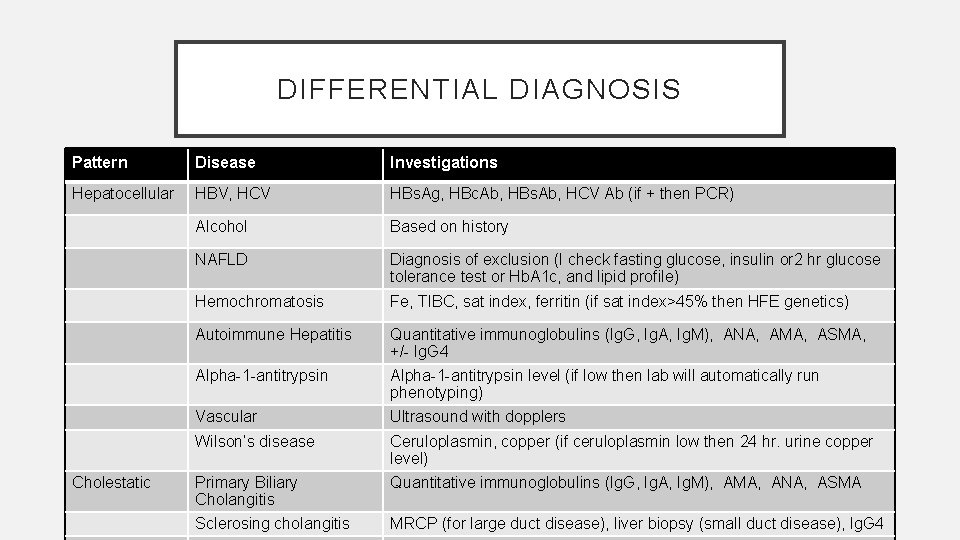
DIFFERENTIAL DIAGNOSIS Pattern Disease Investigations Hepatocellular HBV, HCV HBs. Ag, HBc. Ab, HBs. Ab, HCV Ab (if + then PCR) Alcohol Based on history NAFLD Diagnosis of exclusion (I check fasting glucose, insulin or 2 hr glucose tolerance test or Hb. A 1 c, and lipid profile) Hemochromatosis Fe, TIBC, sat index, ferritin (if sat index>45% then HFE genetics) Autoimmune Hepatitis Quantitative immunoglobulins (Ig. G, Ig. A, Ig. M), ANA, AMA, ASMA, +/- Ig. G 4 Alpha-1 -antitrypsin level (if low then lab will automatically run phenotyping) Vascular Ultrasound with dopplers Wilson’s disease Ceruloplasmin, copper (if ceruloplasmin low then 24 hr. urine copper level) Primary Biliary Cholangitis Quantitative immunoglobulins (Ig. G, Ig. A, Ig. M), AMA, ANA, ASMA Sclerosing cholangitis MRCP (for large duct disease), liver biopsy (small duct disease), Ig. G 4 Cholestatic

WHAT CAUSES FATTY LIVER ON ULTRASOUND? Liver diseases with fatty liver: Alcohol NAFLD HCV-3 Wilson’s Angulo. NEJM. 2002
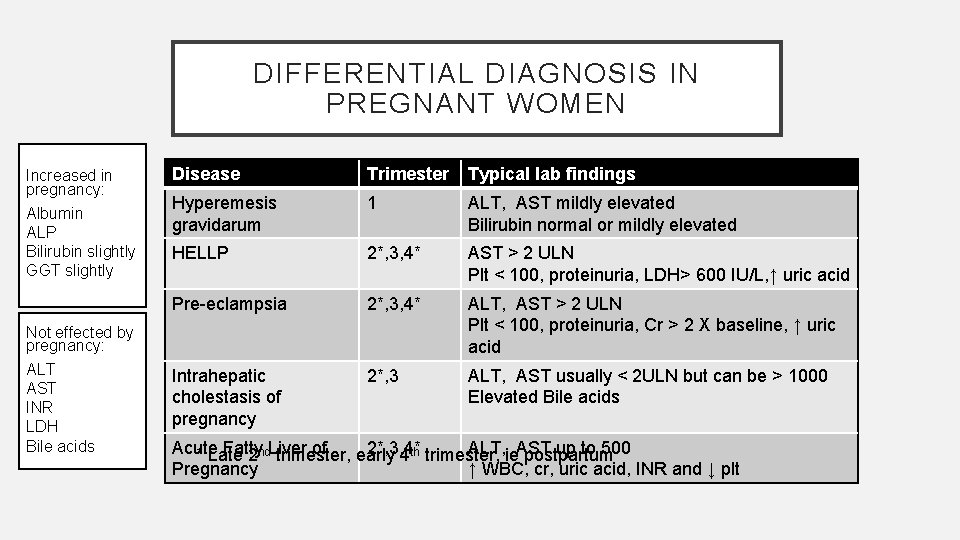
DIFFERENTIAL DIAGNOSIS IN PREGNANT WOMEN Increased in pregnancy: Albumin ALP Bilirubin slightly GGT slightly Disease Trimester Typical lab findings Hyperemesis gravidarum 1 ALT, AST mildly elevated Bilirubin normal or mildly elevated HELLP 2*, 3, 4* AST > 2 ULN Plt < 100, proteinuria, LDH> 600 IU/L, ↑ uric acid Pre-eclampsia 2*, 3, 4* ALT, AST > 2 ULN Plt < 100, proteinuria, Cr > 2 X baseline, ↑ uric acid Intrahepatic cholestasis of pregnancy 2*, 3 ALT, AST usually < 2 ULN but can be > 1000 Elevated Bile acids Not effected by pregnancy: ALT AST INR LDH Bile acids Acute Fatty of 2*, 3, 4* ALT, ie. AST up to 500 * Late 2 nd. Liver trimester, early 4 th trimester, postpartum Pregnancy ↑ WBC, cr, uric acid, INR and ↓ plt

CLUES ON HISTORY: MEDICATION • Consider all medications, even those discontinued in the last 3 months. • Most common drug classes include antibiotics, antiepileptics, NSAIDs, anti-TB drugs, anti-HIV drugs, biologics, chemotherapeutics. • Remember to ask about herbals. • Website livertox. nih. gov • N. B. statins may cause slight liver enzyme elevations which normalize on their own. • N. B. Tylenol does not cause liver damage unless in overdose.

OBJECTIVES • Appropriate investigations for abnormal liver enzymes • Determine which patient should have liver enzymes performed • Understand updates in HCV treatment
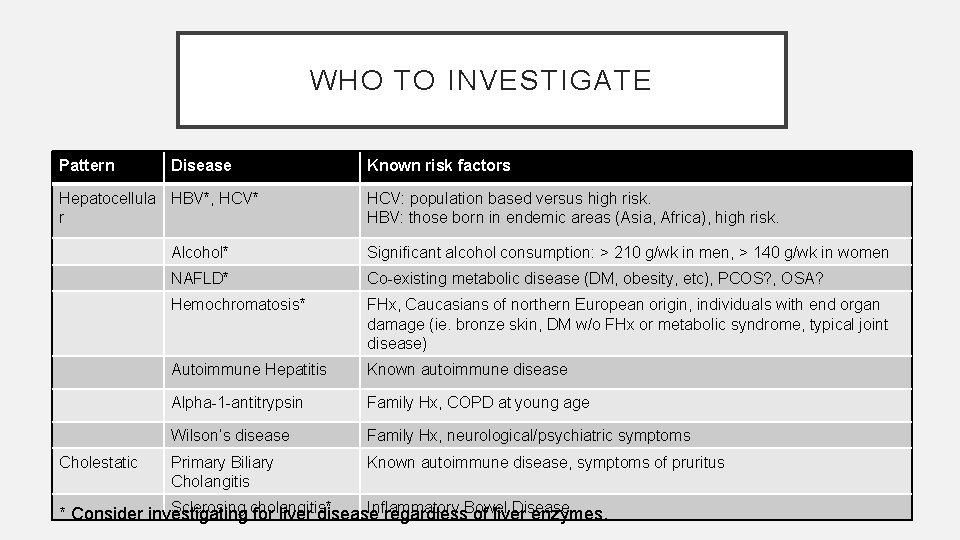
WHO TO INVESTIGATE Pattern Disease Hepatocellula HBV*, HCV* r Cholestatic Known risk factors HCV: population based versus high risk. HBV: those born in endemic areas (Asia, Africa), high risk. Alcohol* Significant alcohol consumption: > 210 g/wk in men, > 140 g/wk in women NAFLD* Co-existing metabolic disease (DM, obesity, etc), PCOS? , OSA? Hemochromatosis* FHx, Caucasians of northern European origin, individuals with end organ damage (ie. bronze skin, DM w/o FHx or metabolic syndrome, typical joint disease) Autoimmune Hepatitis Known autoimmune disease Alpha-1 -antitrypsin Family Hx, COPD at young age Wilson’s disease Family Hx, neurological/psychiatric symptoms Primary Biliary Cholangitis Known autoimmune disease, symptoms of pruritus Sclerosing cholangitis* Inflammatory Disease * Consider investigating for liver disease regardless. Bowel of liver enzymes.

CAN YOU HAVE LIVER DISEASE WITH NORMAL LIVER ENZYMES? YES • You can have HBV, HCV without “active disease”. • Many (10 -30%) with liver cirrhosis have normal ALT, AST. • Hereditary Hemochromatosis is more likely if you have an elevated ferritin and normal liver enzymes (saturation index, and not ferritin, is the screening test). • Can have the genotype without the phenotype… • It is estimated that about 10% of individuals with NAFLD have normal ALT, AST.
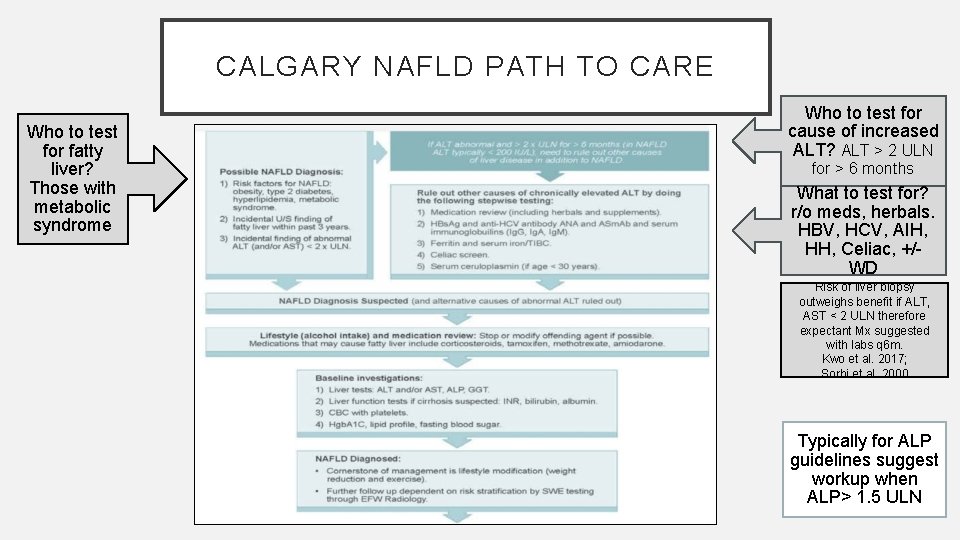
CALGARY NAFLD PATH TO CARE Who to test for fatty liver? Those with metabolic syndrome Who to test for cause of increased ALT? ALT > 2 ULN for > 6 months What to test for? r/o meds, herbals. HBV, HCV, AIH, HH, Celiac, +/WD Risk of liver biopsy outweighs benefit if ALT, AST < 2 ULN therefore expectant Mx suggested with labs q 6 m. Kwo et al. 2017; Sorbi et al. 2000 Typically for ALP guidelines suggest workup when ALP> 1. 5 ULN

WHAT IS THE ROLE OF FIBROSCAN? • Estimates the degree of liver fibrosis as a higher reading is associated with more liver scarring and fibrosis. • It does not directly measure fibrosis and therefore multiple conditions can overestimate liver fibrosis. • ex. acute inflammation, congestion, fatty infiltration, cholestasis, etc. or unreliable (ex. ascites, central obesity) • Liver stiffness needs to be interpreted in the appropriate clinical context. • Shear wave and strain imaging best studied in HBV, HCV. • Fibroscan studies suggest its use in NAFLD is to differentiates “low risk of advanced fibrosis” vs “high risk of advanced fibrosis”, not fibrosis (F) score and not to differentiate NAFLD vs NASH.

OBJECTIVES • Appropriate investigations for abnormal liver enzymes • Determine which patient should have liver enzymes performed • Understand updates in HCV treatment
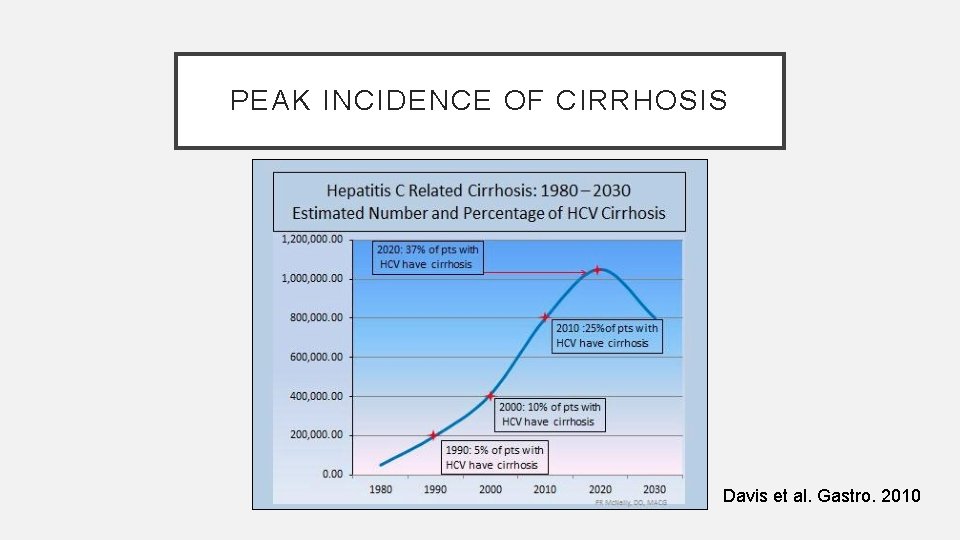
PEAK INCIDENCE OF CIRRHOSIS Davis et al. Gastro. 2010
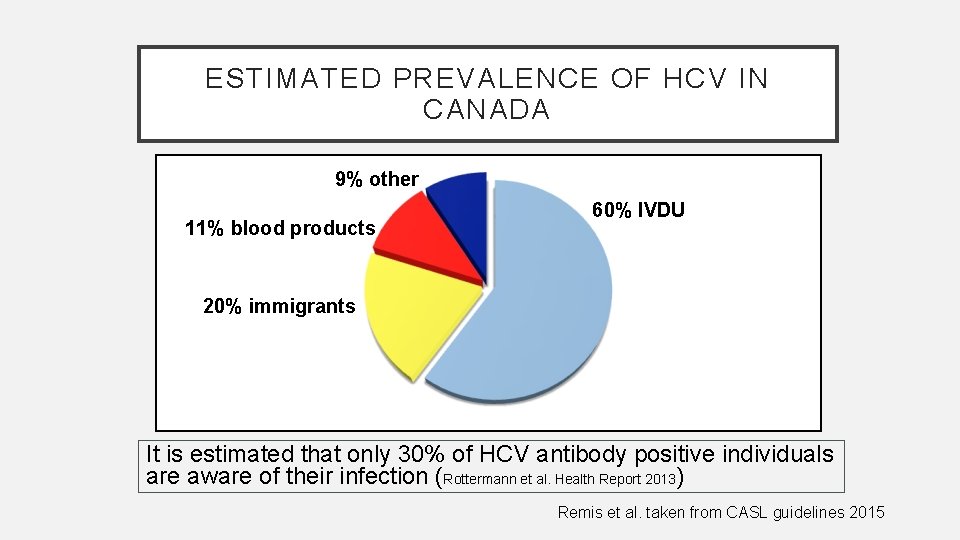
ESTIMATED PREVALENCE OF HCV IN CANADA 9% other 11% blood products 60% IVDU 20% immigrants It is estimated that only 30% of HCV antibody positive individuals are aware of their infection (Rottermann et al. Health Report 2013) Remis et al. taken from CASL guidelines 2015
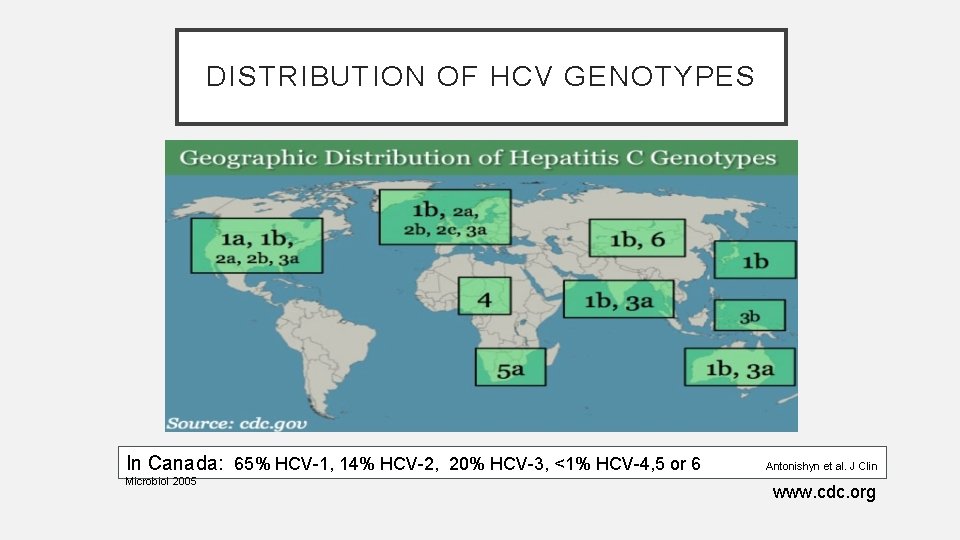
DISTRIBUTION OF HCV GENOTYPES In Canada: 65% HCV-1, 14% HCV-2, 20% HCV-3, <1% HCV-4, 5 or 6 Microbiol 2005 Antonishyn et al. J Clin www. cdc. org

WHO SHOULD BE TESTED? WHO SHOULD BE TREATED? • Alberta Blue Cross will allow all individuals regardless of fibrosis stage to be treated if chronic HCV. • Only reason not to treat is short life expectancy or severe comorbidities. • HCV Ab testing • Specificity greater than 99%. • Window period after exposure is 10 weeks. • Antibody suggests exposure and 25 -30% of individuals exposed to HCV clear the virus on their own, typically in first 6 months. • HCV RNA detection is necessary • HCV RNA qualitative assay no longer done. • HCV RNA quantitative assay. • Detection limit <12 IU/m. L. Hemant et al. The management of chronic hepatitis C: 2018 guideline update from the Canadian Association for the Study of the Liver. CMAJ, 2018.
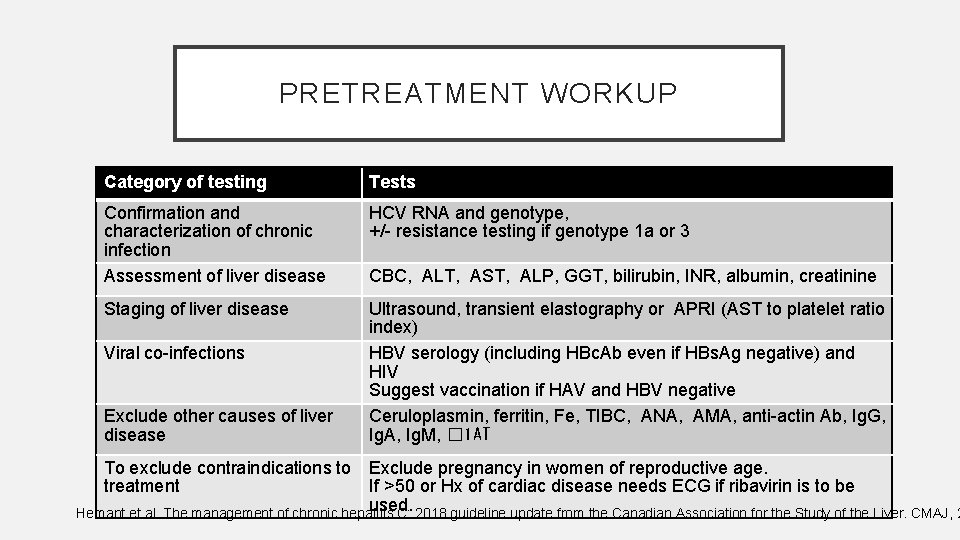
PRETREATMENT WORKUP Category of testing Tests Confirmation and characterization of chronic infection Assessment of liver disease HCV RNA and genotype, +/- resistance testing if genotype 1 a or 3 Staging of liver disease Ultrasound, transient elastography or APRI (AST to platelet ratio index) HBV serology (including HBc. Ab even if HBs. Ag negative) and HIV Suggest vaccination if HAV and HBV negative Ceruloplasmin, ferritin, Fe, TIBC, ANA, AMA, anti-actin Ab, Ig. G, Ig. A, Ig. M, � 1 AT Viral co-infections Exclude other causes of liver disease CBC, ALT, AST, ALP, GGT, bilirubin, INR, albumin, creatinine To exclude contraindications to Exclude pregnancy in women of reproductive age. treatment If >50 or Hx of cardiac disease needs ECG if ribavirin is to be used. Hemant et al. The management of chronic hepatitis C: 2018 guideline update from the Canadian Association for the Study of the Liver. CMAJ, 2

POST-TREATMENT FOLLOW-UP • Complete HCV eradication (ie. sustained virological response, SVR). • Defined as undetectable HCV PCR 12 weeks following end of treatment. • SVR is considered to be long term cure as late relapses are rare. • HCV Ab+ will remain positive after HCV viral eradication. • In those with ongoing risk of exposure, annual HCV PCR testing suggested to assess for reinfection. • After HCV eradication, liver cirrhosis and fibrosis can improve. • Surveillance for hepatocellular cancer (HCC) with q 6 m ultrasounds indefinitely even after SVR achieved in those with (1) cirrhosis, and also (2) in those who had “cirrhosis” at the beginning of treatment based on non invasive tests even if post-treatment testing no longer suggest cirrhosis. Hemant et al. The management of chronic hepatitis C: 2018 guideline update from the Canadian Association for the Study of the Liver. CMAJ, 20
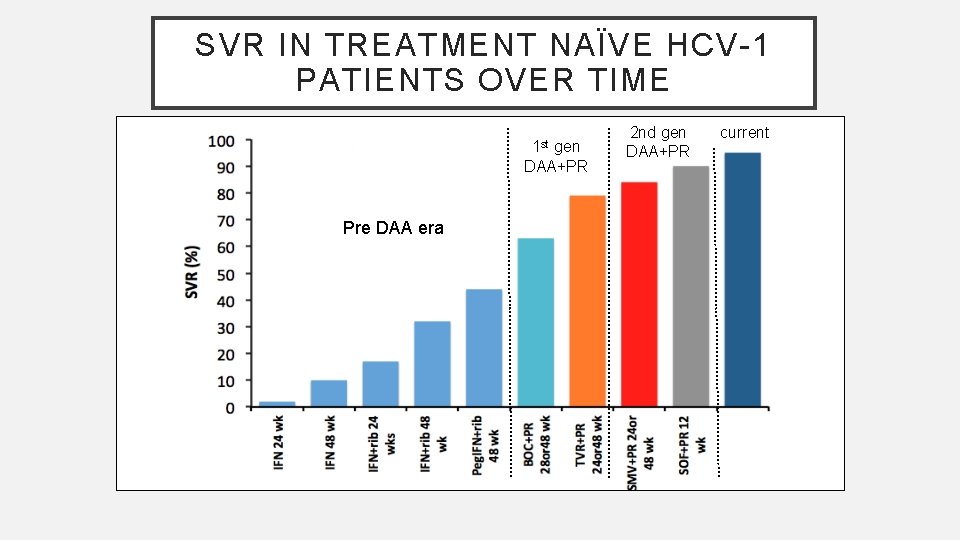
SVR IN TREATMENT NAÏVE HCV-1 PATIENTS OVER TIME 1 st gen DAA+PR 79 Pre DAA era 63 44 32 10 2 17 2 nd gen DAA+PR 90 84 current
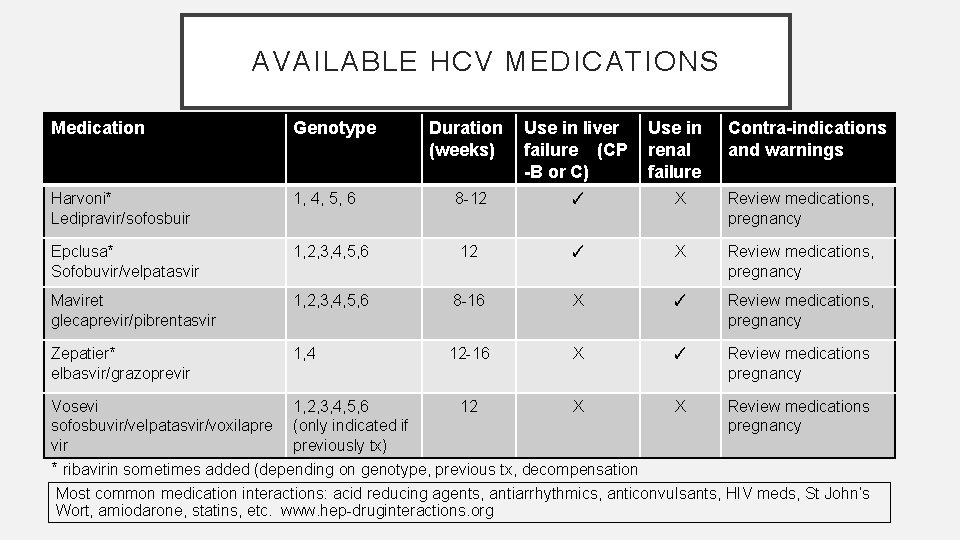
AVAILABLE HCV MEDICATIONS Medication Genotype Harvoni* Ledipravir/sofosbuir 1, 4, 5, 6 Epclusa* Sofobuvir/velpatasvir Duration (weeks) Use in liver failure (CP -B or C) Use in renal failure Contra-indications and warnings 8 -12 ✓ X Review medications, pregnancy 1, 2, 3, 4, 5, 6 12 ✓ X Review medications, pregnancy Maviret glecaprevir/pibrentasvir 1, 2, 3, 4, 5, 6 8 -16 X ✓ Review medications, pregnancy Zepatier* elbasvir/grazoprevir 1, 4 12 -16 X ✓ Review medications pregnancy Vosevi sofosbuvir/velpatasvir/voxilapre vir 1, 2, 3, 4, 5, 6 (only indicated if previously tx) 12 X X Review medications pregnancy * ribavirin sometimes added (depending on genotype, previous tx, decompensation Most common medication interactions: acid reducing agents, antiarrhythmics, anticonvulsants, HIV meds, St John’s Wort, amiodarone, statins, etc. www. hep-druginteractions. org

DIFFICULT TO TREAT POPULATIONS • Previously considered difficult to treat which are no longer considered such: • Post liver transplant • HCV/HIV • Currently considered difficult to treat: • HCV genotype 3 • Decompensated liver cirrhosis • Chronic Renal Insufficiency • Previous treatment failure/antiviral resistance

THANK YOU


WHO IS AT RISK OF NAFLD? 1. Chalasani. Hepatol. 2018; 2. EASL, EASD, EASO. J Hepatol. 2016 Slide credit: clinicaloptions. com
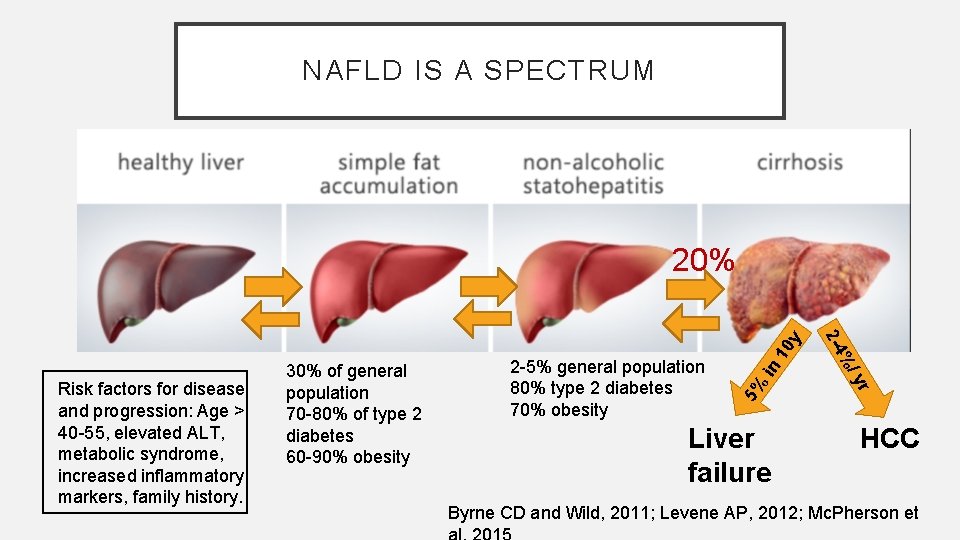
NAFLD IS A SPECTRUM in 5% yr Liver failure %/ 2 -5% general population 80% type 2 diabetes 70% obesity 2 -4 Risk factors for disease and progression: Age > 40 -55, elevated ALT, metabolic syndrome, increased inflammatory markers, family history. 30% of general population 70 -80% of type 2 diabetes 60 -90% obesity 10 y 20% HCC Byrne CD and Wild, 2011; Levene AP, 2012; Mc. Pherson et

☞ Angulo et al. 2007; Sterling et al. 2006; Mc. Pherson et al. 2010
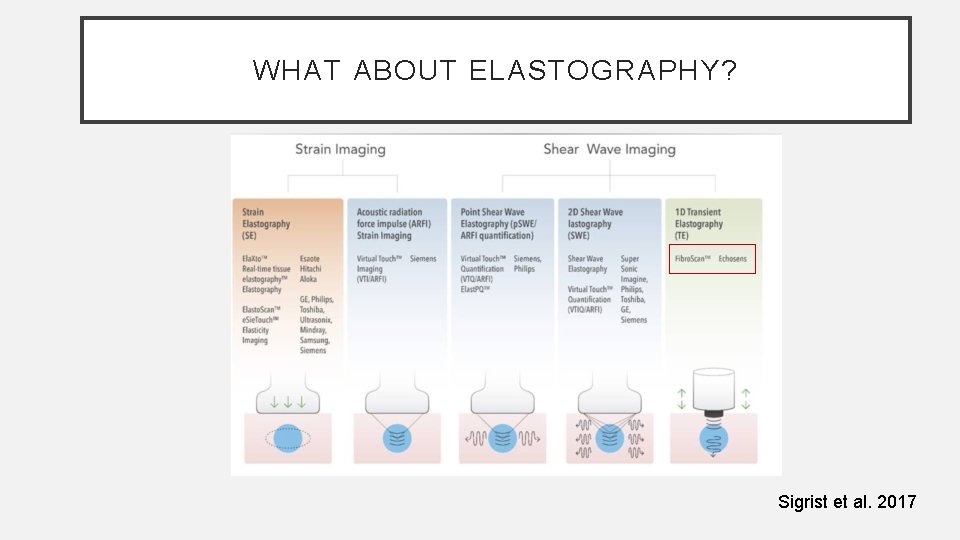
WHAT ABOUT ELASTOGRAPHY? Sigrist et al. 2017
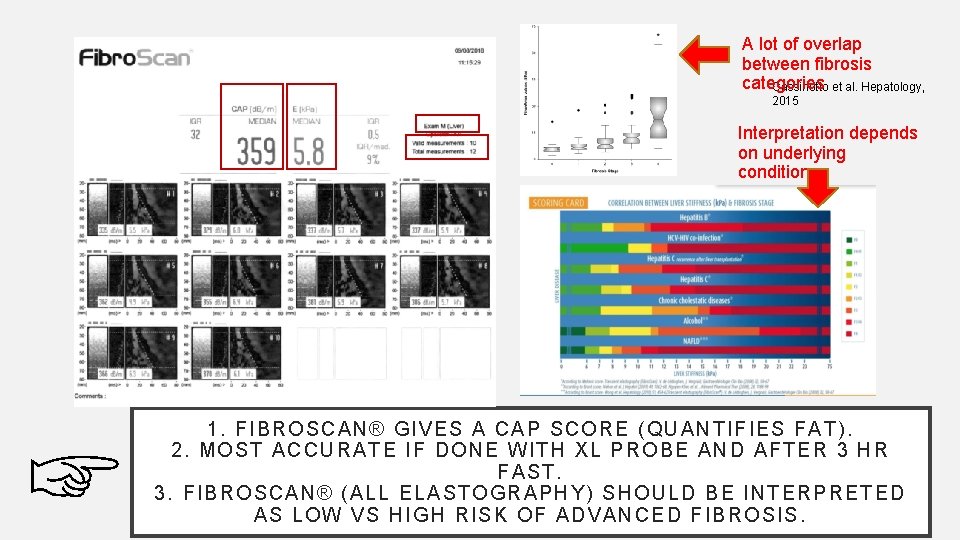
A lot of overlap between fibrosis categories Cassinotto et al. Hepatology, 2015 Interpretation depends on underlying condition ☞ 1. F IB ROSCAN® GIV ES A C AP SCO RE ( QUANTIFIES FAT). 2. MOST A CC UR AT E IF D ON E WITH XL PR OBE AND AFTER 3 HR FAST. 3. FIB ROSC AN ® (ALL ELA ST OG RAPH Y) SHO ULD BE IN TERPRETED A S LOW VS H IG H RI SK O F ADVANCED FIBROSIS.
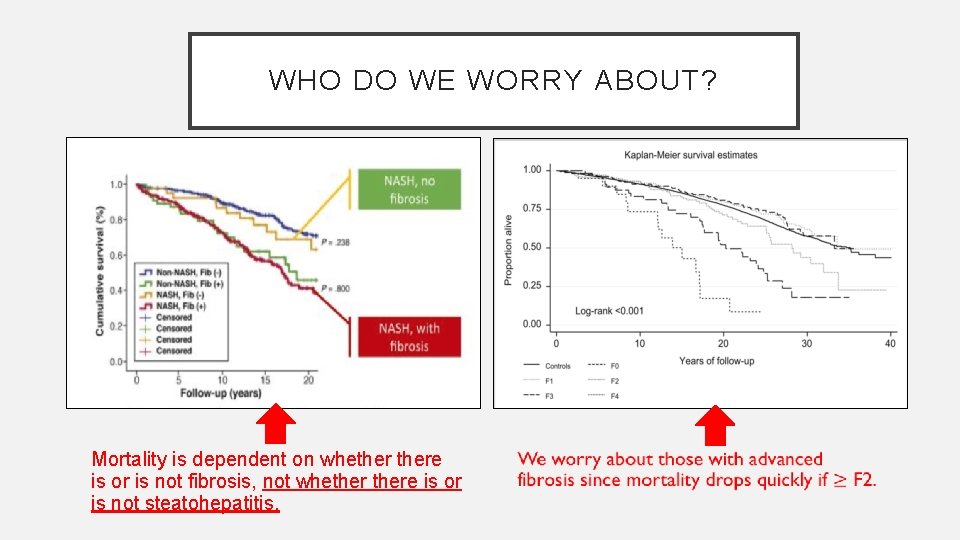
WHO DO WE WORRY ABOUT? Angulo et al, 2015 Mortality is dependent on whethere is or is not fibrosis, not whethere is or is not steatohepatitis. Hagstrom et al. 2016
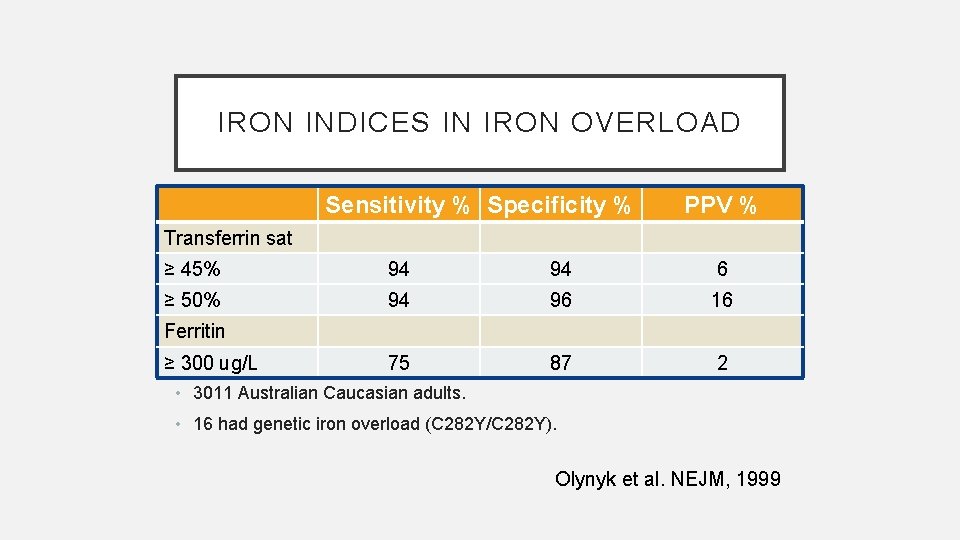
IRON INDICES IN IRON OVERLOAD Sensitivity % Specificity % PPV % Transferrin sat ≥ 45% 94 94 6 ≥ 50% 94 96 16 75 87 2 Ferritin ≥ 300 ug/L • 3011 Australian Caucasian adults. • 16 had genetic iron overload (C 282 Y/C 282 Y). Olynyk et al. NEJM, 1999
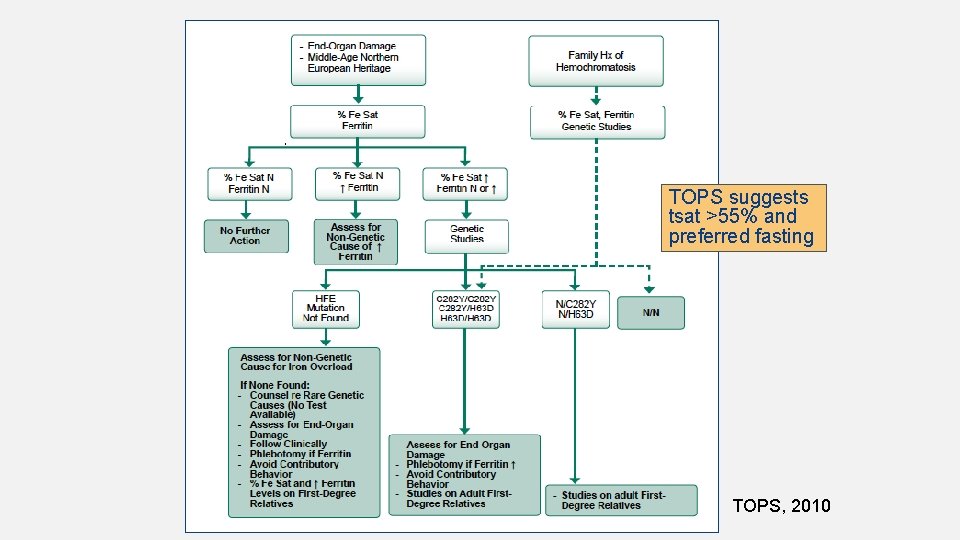
TOPS suggests tsat >55% and preferred fasting TOPS, 2010

HFE- HEREDITARY HEMOCHROMATOSIS • Autosomal Recessive trait. • HFE prevalence 1/150 - 1/200 of Northern European descent. 1 Genotype Phenotype C 282 Y/C 282 Y 1 -50% penetrance. 50% of women and 20% of men have normal ferritin and never require therapy. Disease rarely presents in people younger than 40 yr old. No way to predict who will develop clinical disease. C 282 Y/H 63 D <1% penetrance. Most have normal iron levels. Moderate iron overload can develop if other risks*. C 282 Y/normal 10% of Caucasians. Most have normal iron levels. Only develop iron overload when other risks*. H 63 D/H 63 D Most have normal iron. Mutation associated with increased t sat but not clinically sign iron overload. Iron overload depends on other risks*. H 63 D/normal 20% of Caucasians. Iron overload unlikely. If overload seen consider other risks*. *alcohol, viral hepatitis, obesity, etc. Having the genetics for HH (ex C 282 Y/C 282 Y) in the absence of elevated iron is not diagnostic for HH as a disease. It represents a genetic susceptibility to develop it in the future. • Individuals with asymptomatic HH and ferritin <1000 at low risk for developing signs and symptoms in the future. 2 • Ferritin >1000 predicts presence of cirrhosis (100% sensitivity and 70% specificity). 3 o Ferritin is considered the most useful prognostic indicator of disease activity. 1. Bacon. 2001; 2. Beutler et al. 2002; 3. Beaton et al. 2002. Gochee et al. 2002; Beutler et al. 2002; Kowdley et al. 2008
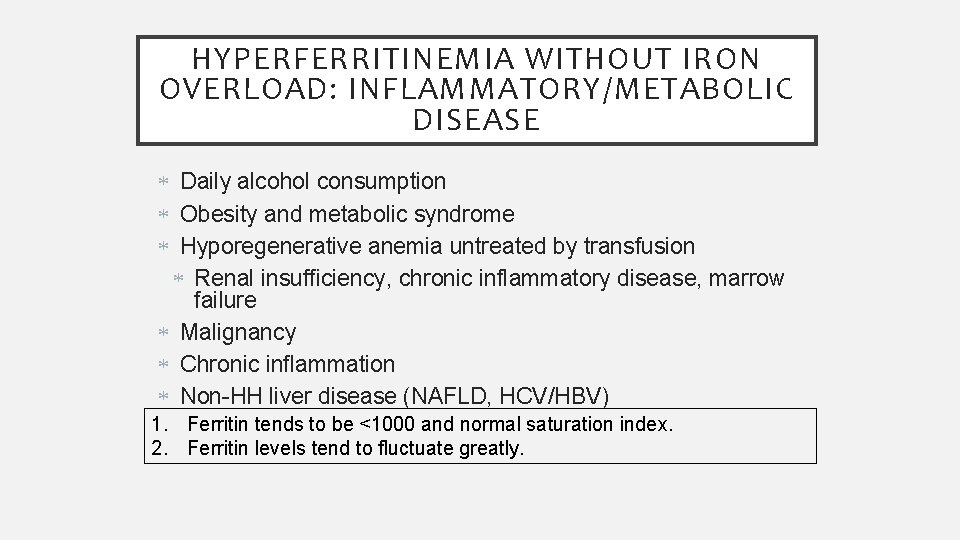

HYPERFERRITINEMIA WITHOUT IRON OVERLOAD: INFLAMMATORY/METABOLIC DISEASE Daily alcohol consumption Obesity and metabolic syndrome Hyporegenerative anemia untreated by transfusion Renal insufficiency, chronic inflammatory disease, marrow failure Malignancy Chronic inflammation Non-HH liver disease (NAFLD, HCV/HBV) 1. Ferritin tends to be <1000 and normal saturation index. 2. Ferritin levels tend to fluctuate greatly.
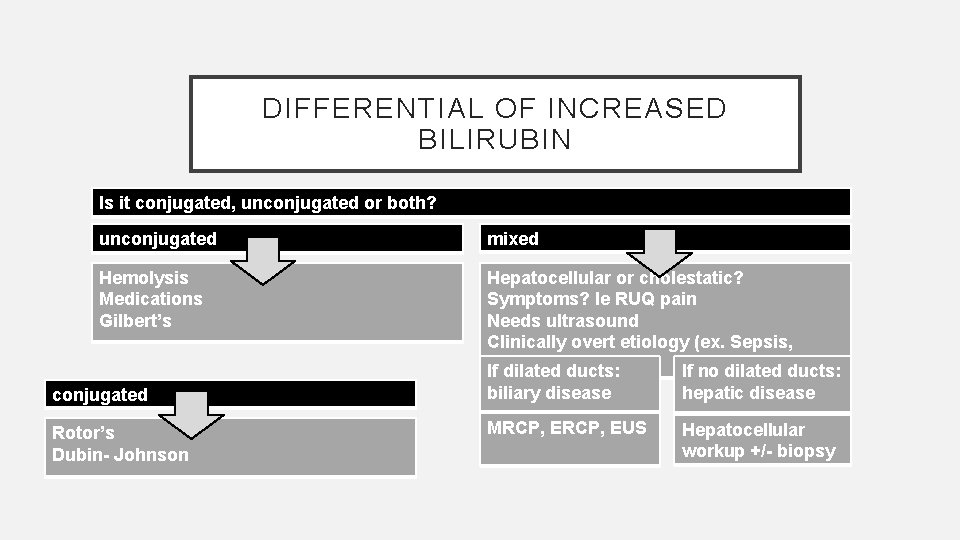
DIFFERENTIAL OF INCREASED BILIRUBIN Is it conjugated, unconjugated or both? unconjugated mixed Hemolysis Medications Gilbert’s Hepatocellular or cholestatic? Symptoms? Ie RUQ pain Needs ultrasound Clinically overt etiology (ex. Sepsis, TPN? ) If dilated ducts: If no dilated ducts: conjugated biliary disease hepatic disease Rotor’s Dubin- Johnson MRCP, EUS Hepatocellular workup +/- biopsy
- Slides: 48