ABNORMAL LABOUR Dr Farzana Sabir MBBS FCPS Normal

ABNORMAL LABOUR Dr Farzana Sabir MBBS, FCPS.

Normal labour The onset of regular , painful uterine contractions that leads to effacement and dilatation of cervix with descent of fetus in vertex presentation.

Abnormal labour, dystocia, failure to progress Terms used to describe a difficult labour pattern, that deviates from that observed in majority of women who have spontaneous vaginal deliveries. Labour becomes abnormal when there is poor progress as evidenced by a delay in cervical dilatation or descent of the presenting part and/or the fetus shows signs of compromise.

Abnormal labour Failure to meet defined milestones & time limits for normal labour Another name is dystocia. Assessment of progress in labour • Progressive dilatation of cervix 1 cm / hr in primigravida 1. 5 – 2 cm / hr in multigravida • Progressive descent of head

Difinition “No change or minimal change in cervical dilatation in a 2 hour period during the latent or the active phase of labour, or no change or minimal change in descent of the presenting part in one hour during the second stage of labour”. Without timely intervention abnormal labour usually leads to prolonged labour. One of main objectives of labour monitoring is to detect abnormal progress of labour before it is prolonged.

Incidence of labor abnormalities Difficult to determine the exact incidence. In nulliparous patients, the incidence of labor disorders is ≈ 25% Dystocia is currently the most common (50 - 60%) indication for 1˚ C/S, ≈ 3 X more common than either NRFHRP or malpresentation.

Etiology The causes of abnormal labour generally fall into following I. Abnormal pattern of labour II. Abnormalities of passage III. Abnormalities of passenger IV. Abnormalities of the power

Abnormal Patterns of Labor Friedman described four abnormal patterns of labor 1. prolonged latent phase 2. protraction disorders (protracted active -phase dilatation and protracted descent) 3. arrest disorders (arrest of dilatation, arrest of descent, and failure of descent), and 4. precipitate labor disorders.
DISORDERS OF LABOUR

DISORDERS OF LATENT PHASE Prolonged latent phase: From the onset of regular uterine contractions to the beginning of the active phase of cervical dilatation The duration of latent phase is usually between 3 -8 hours in nulliparas and usually shorter in multiparas. Causes of prolonged latent phase include: use of general anesthesia before labor enters the active phase, labor beginning with an unfavorable cervix, irregular, uncoordinated, and ineffective uterine contractions, and fetopelvic disproportion.

Prolonged latent phase… Treatment options primarily consist of therapeutic rest regimens or active management of labor Adequate rest Rehydration Oxytocin stimulation OR cesarean delivery in case of fetal compromise. If immediate delivery is required for clinical reasons (eg, severe preeclampsia or amnionitis), oxytocin infusion is the treatment of choice.

Disorders of the Active Phase… Protraction Disorders May be divided into: q protracted active-phase dilatation and q protracted descent Ø Protracted active-phase dilatation: characterized by an abnormally slow rate of dilatation in the active phase, less than 1. 2 cm/h in nulliparas or less than 1. 5 cm/h in multiparas. Ø Protracted descent of the fetus: Characterized by a rate of descent; less than 1 cm/h in nulliparas or less than 2 cm/h in multiparas. Ø The second stage of labor is protracted when the stage exceeds: 2 hours in nulliparas or 1 hour in multiparas, or 3 and 2 hours, respectively, in the presence of conduction anesthesia

Protraction disorders Cause of a protraction disorder is probably multifactorial Inadequate uterine activity(the most common) Fetopelvic disproportion Abnormal positioning of the fetal presenting part improperly administered conduction anesthesia excessive sedation and, pelvic tumors obstructing the birth canal

Protraction disorders Management option of protraction disorders: Depends on the presence or absence of fetopelvic disproportion, and The adequacy of uterine contractions, Cesarean section is indicated in the presence of confirmed fetopelvic disproportion In the absence of fetopelvic disproportion, conservative management: consisting of support and close observation, and therapy with oxytocin augmentation both carry a good prognosis for vaginal delivery (approximately two-thirds of patients

Arrest Disorders The two patterns of arrest in labor can be characterized as follows: secondary arrest of dilatation ; with no progressive cervical dilatation in the active phase of labour for 2 hours or more between cervical dilatation of 7 -10 cm. Arrest of descent ; with descent failing to progress for 1 hour or more. Causative factors: o fetopelvic disproportion(in approximately 50%) o fetal malpositions, o inappropriately administered anesthesia, and o excessive sedation. Arrest disorders in the presence of adequate uterine contractions carry a poor prognosis for vaginal delivery. If allowed to continue, arrest disorders are associated with increased perinatal morbidity

Precipitate labor and delivery Expulsion of the fetus in less than 3 hours Ø cervical dilation ≥ 5 cm /hr in a primigravida Ø ≥ 10 cm /hr in a multipara. Causes : : abnormally low birth canal resistance , extremely strong uterine contractions , the absence of painful sensations.

Complications Maternal : uterine rupture , extensive lacerations of the cervix, vagina, vulva, or perineum , PPH from uterine atony Fetal : Perinatal mortality and morbidity , intracranial hemorrhage , risks associated with unattended delivery Management : stop any oxytocin if being administered , no significant use of analgesia , terbutaline or ritodrine intravenously Physical attempts to retard delivery are absolutely contraindicated

ABNORMALITY OF PASSAGE The passage relates to the uterus, cervix and the bony components of the pelvis CAUSES: • Malnourishment • previous fracture or metabolic bone diseases • Woman with paraplegia or spina bifida • Space occupying viscera in the pelvis Impacted rectum, Full bladder, Cervical fibroid, Ovarian cysts Cervical dystocia: noncompliant cervix which effaces but fails to dilate because of severe scarring which may be as a result of previous cone biopsy and also because of malpresentation and malposition • CPD cephalopelvic disproportion

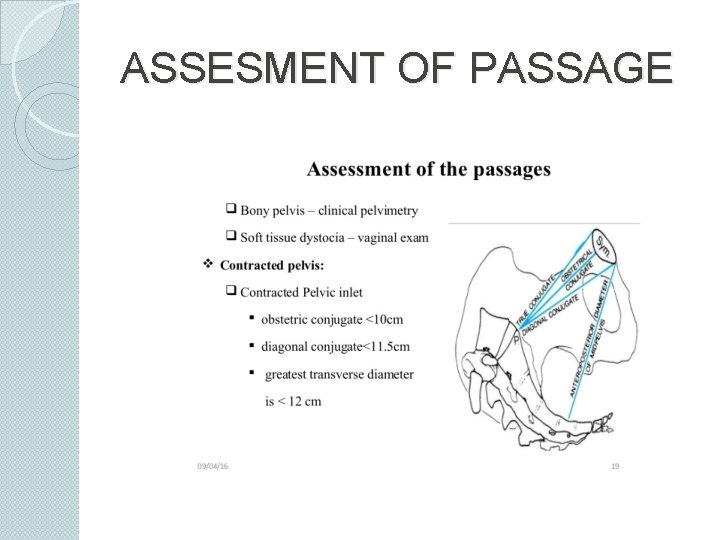
Cephalopelvic disproportion Contraced pelvis Ø Contracted inlet plane Ø Contracted midpelvis Ø Contracted outlet plane Pelvic malformation
ASSESMENT OF PASSAGE

ASSESMENT OF PASSAGE

ASSESMENT OF PASSAGE

Relative CPD Gross CPD Previous Estimated history of abnormal labour Primigravida of less than 16 yr of age Prominent ischial spines, flat sacrum True conjugate of 8 -10 cm fetal weight of >4 kg Hydrocephalus Gross traumatic, congenital pelvic abnormality True conjugate of<8 cm Diagnostic approach and risk assesment

Abnormalities of fetus (passenger) Ø Abnormalities of fetal: Position(OP, OT) Presentation(Face, brow, breech, shoulder) Lie(oblique, transverse) Attitude(extension) Ø Macrosomia Ø Fetal malformation(hydrocephaly, distended bladder, abdominal mass, ascites)

Abnormalities of fetus (passenger)… Diagnostic approach Clinical assessment is usually diagnostic especially in labor with dilated cervix through which Vaginal Exam. provides adequate information. Ultrasound is mainly used to: investigate predisposing factors (e. g. , placenta previa, fetal goiter) , assess fetal condition , assess attitude of the fetus especially in breech and to confirm clinical diagnosis.

Abnormalities of the powers… 2 categories Ø Hypotonic insufficient force, irregular or infrequent rhythm Cause: Sedation, over distension of the uterus, early administration of anesthesia Rx: -augmentation(ARM or oxytocin) Hypertonic Uncoordinated and frequent intense uterine contractions. Midsegment of uterus has more pressure power than the fundus Cause: over use of oxytocin. Rx: tocolysis, decrease in oxytocin infusion.

Abnormalities of the powers Assessment of powers of labor 3 ways: Palpation of uterine contractions External tocodynamometer Intrauterine pressure catheter monitoring Clinical presentation: : Abdominal palpation: uterine contraction is weak, and intervals is prolonged. Abnormal labor course: the most important clinical presentation.

Management The Vaginal examination: Rule out CPD To determine fetal presentation, position and station. To assess the cephalopelvic relation. To consider the route of delivery. The supportive management : Sufficient rest , To relieve anxiety and fear. Fluid and food intake.

Abnormalities of the powers Augmentation Increase the frequency and force of the existing uterine contractions. Methods: Amniotomy and oxytocin administration Amniotomy : If the fetal head is engaged, amniotomy is a choice to facilitate the uterine activity. After amniotomy the fetal head descends , pressing directly on cervix to enforce uterine contraction⇒ accelerating labor. Oxytocin infusion is started to augment uterine contraction. CI: CPD, severe fetal malposition, placenta previa, brow presentation, face , twin pregnancy, extensive genital wart, cervical cancer, uterine scar, NRFHR Secondary powers failure – Instrumental assistance

Management Assess fetomaternal well being Monitor uterine activity Bedside ultrasound to diagnose fetal malposition

CONT. . Emotional Support Hydration Reassurance Analgesia Mobilization One to one care A longer period of time to allow labour to progress Check for the cause

CONT. . Continued observation Augmentation of labour Attempt operative vaginal delivery(forceps, ventouse) Caeserian delivery
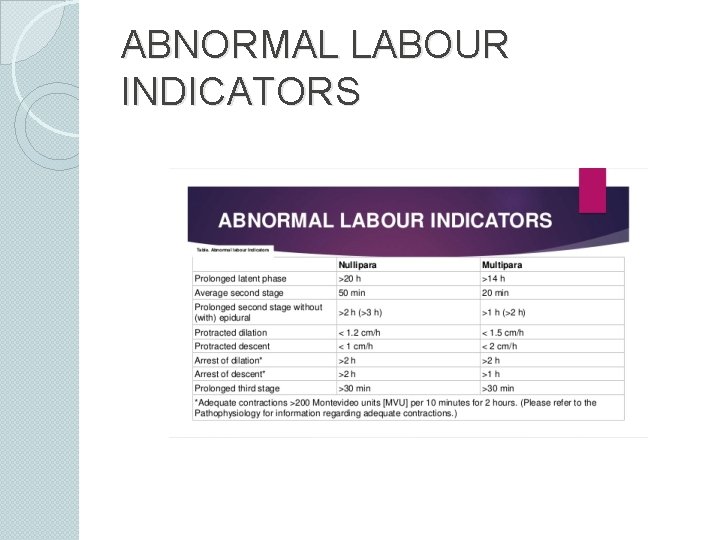

ABNORMAL LABOUR INDICATORS

Prognosis Good prognosis in multipara than primipara Poor prognosis when diagnosis is made in early phase of labour <6 cm Poor prognosis when there is high station

CONSEQUENCES OF ABNORMAL LABOUR Short Term On the Mother: Postpartum hemorrhage Increased rate of traumatic complications: Lacerations, injuries to adjacent organs Increased risk of infection (prolonged labour) Increased rate of difficult operative delivery

CONSEQUENCES OF ABNORMAL LABOUR Long Term Consequences: Psychological effects of a Traumatic Experience On the Fetus: Increased rate of perinatal morbidity and mortality Potential Complications of traumatic delivery Low Apgar score Neonatal complications (Birth Asphyxia, trauma )

THANKYOU…
- Slides: 37