Abdominal trauma penetrating trauma and ultrasound ST 3DREEM

Abdominal trauma, penetrating trauma and ultrasound ST 3/DRE-EM Regional Training Day Friday 13 th October 2017 Richard Kendall Consultant in emergency medicine

Patient 1 • 23 year old man • Pedestrian hit by car • On arrival P 110, BP 124/64, GCS 15 • Left lower chest and LUQ
What imaging do you arrange first? 1. 2. 3. 4. 5. CXR and pelvis AP Cervical spine FAST CT abdomen and CXR Whole Body CT (WBCT)
What imaging do you arrange first? 1. 2. 3. 4. 5. CXR and pelvis AP Cervical spine FAST CT abdomen and CXR Whole Body CT (WBCT)

Effect of whole-body CT during trauma resuscitation on survival: a retrospective, multicentre study The Lancet Huber-Wagner et al (the working group on polytrauma of the German Trauma Society) Volume 373, Issue 9673, Pages 1455 - 1461, 25 April 2009 – trauma registrar review – n = 4621 patients, 1491 underwent WBCT – WBCT increased probability of survival

But. . . . • WBCT – up to 30 m. Sv • Addenbrooke’s data: 10% show no radiological abnormality
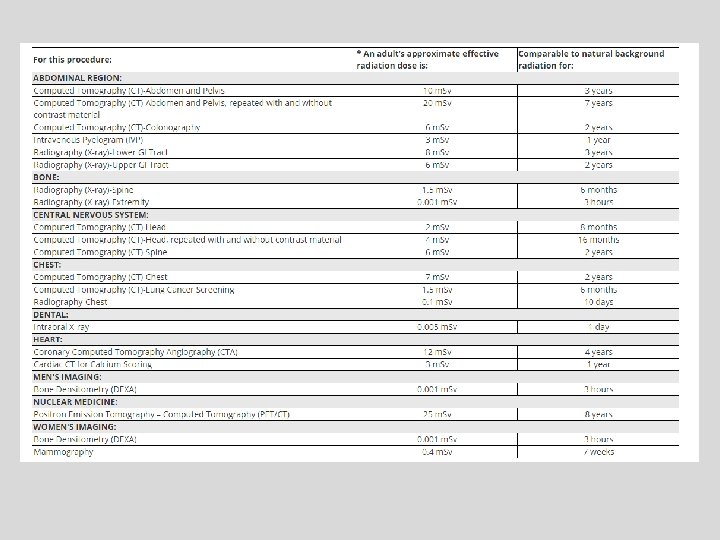
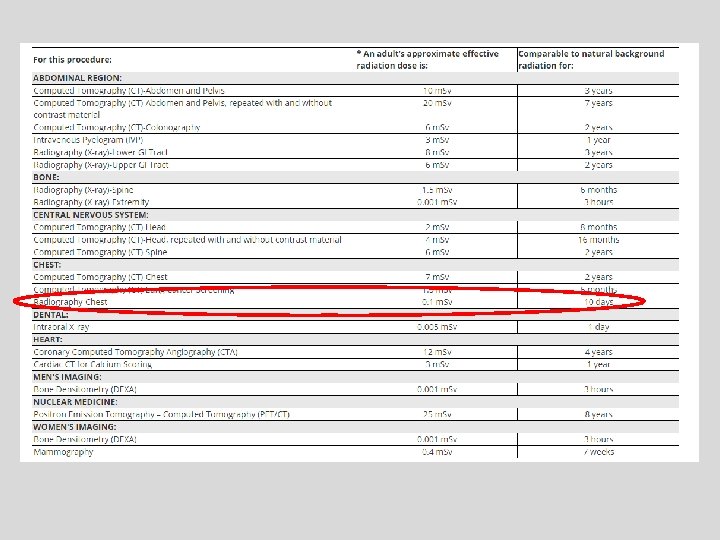
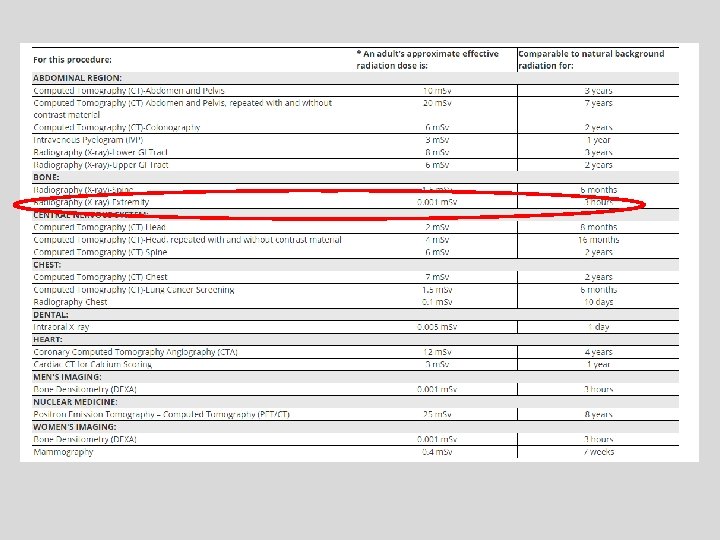
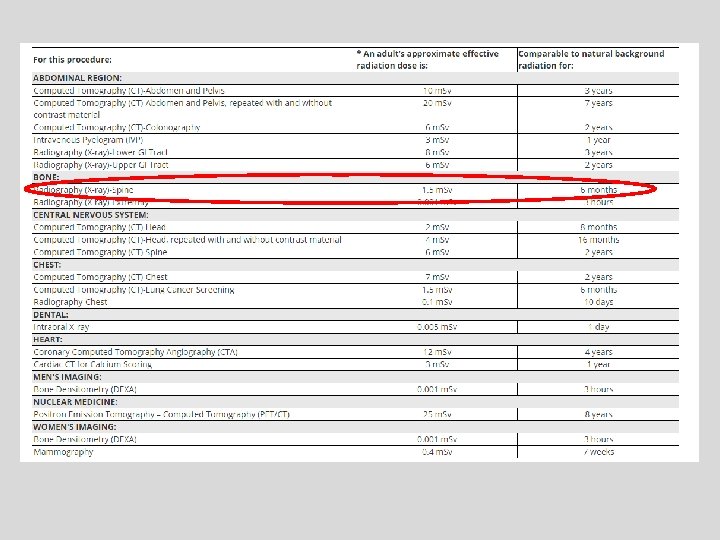
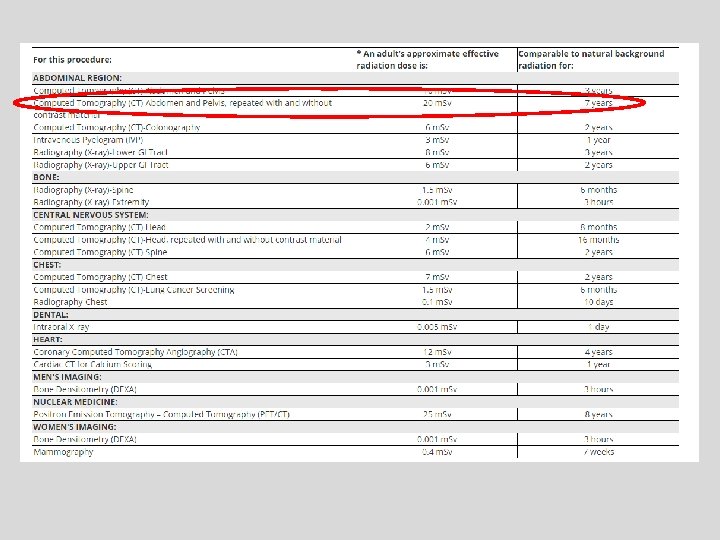

Computed Tomography — An Increasing Source of Radiation Exposure Brenner DJ and Hall EJ NEJM Volume 357: 2277 -2284 November 29, 2007 Number 22 A 10 m. Sv CT in a 25 year old is associated with an estimated : – Risk of induced cancer 1 in 900 – Risk of induced fatal cancer 1 in 1800

Patient 2 • 28 year old woman • Driver, frontal impact at 50 mph • On scene RSI (agitated, GCS 9 E 2 V 2 M 5) • Seat belt bruising to chest and abdomen • In resus P 136 BP 84/45
What imaging do you arrange first? 1. 2. 3. 4. 5. CXR, pelvis AP, lateral Cervical spine Pelvis AP and FAST WBCT
What imaging do you arrange first? 1. 2. 3. 4. 5. CXR, pelvis AP, lateral Cervical spine Pelvis AP and FAST WBCT

FAST • Focussed Assessment with Sonography in Trauma • Haemoperitoneum • Haemopericardium • e. FAST (extended FAST) – Pneumothorax – Haemothorax
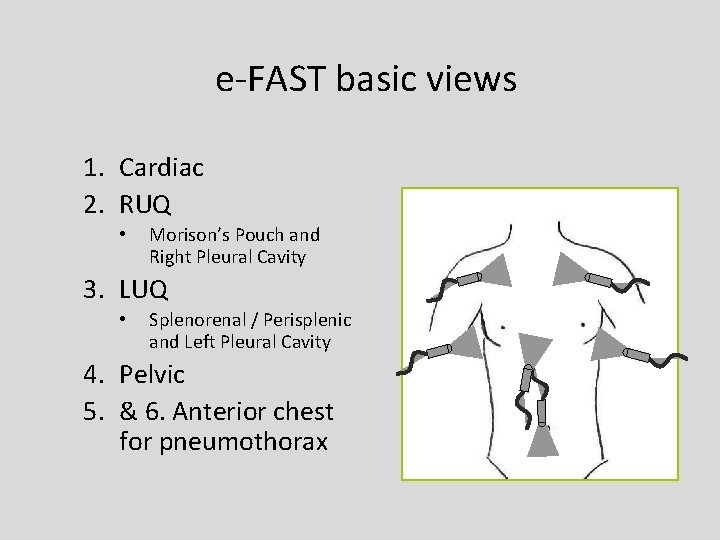
e-FAST basic views 1. Cardiac 2. RUQ • Morison’s Pouch and Right Pleural Cavity 3. LUQ • Splenorenal / Perisplenic and Left Pleural Cavity 4. Pelvic 5. & 6. Anterior chest for pneumothorax
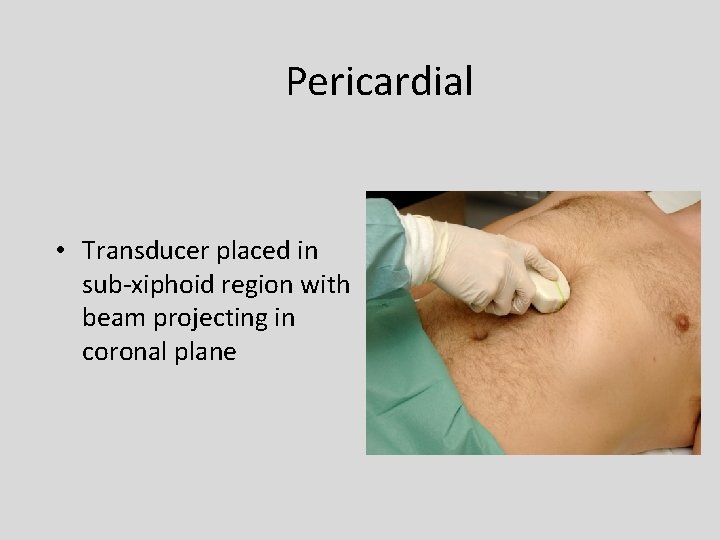
Pericardial • Transducer placed in sub-xiphoid region with beam projecting in coronal plane
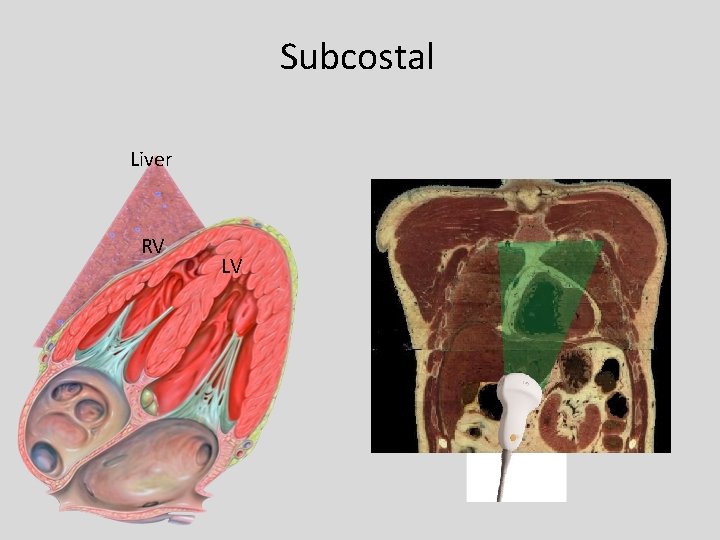
Subcostal Liver RV LV
l 20
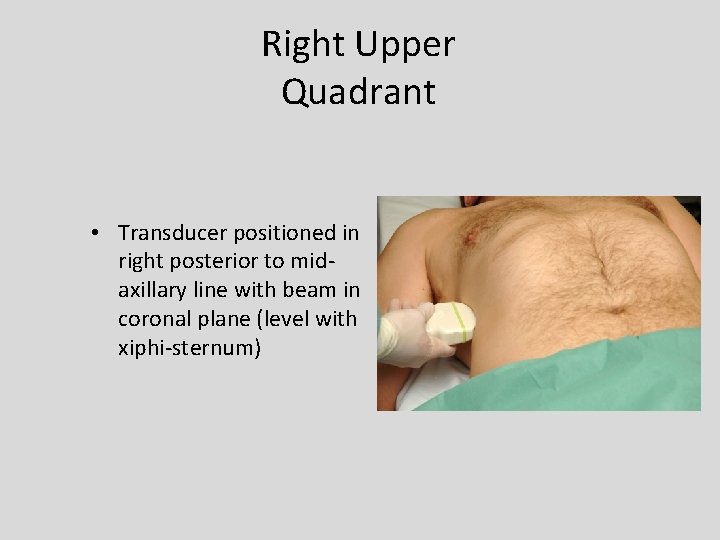
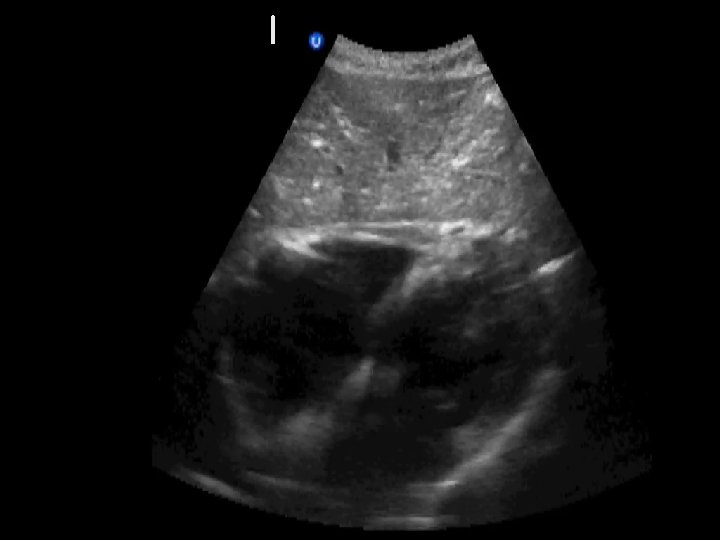
Right Upper Quadrant • Transducer positioned in right posterior to midaxillary line with beam in coronal plane (level with xiphi-sternum)
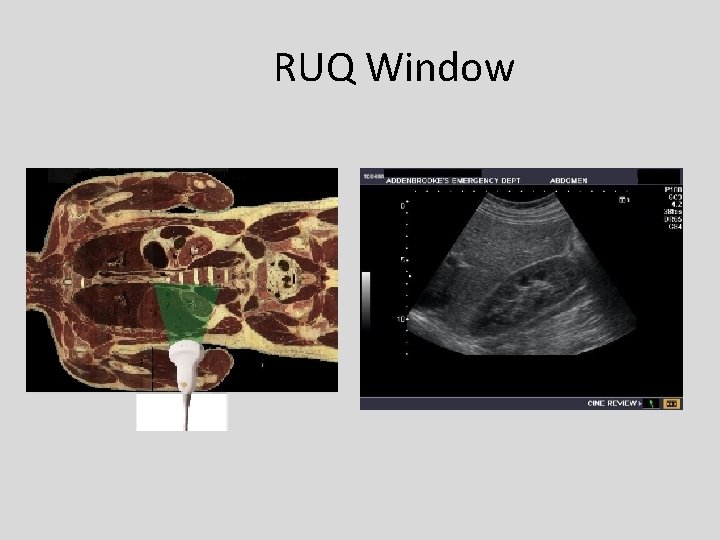
RUQ Window
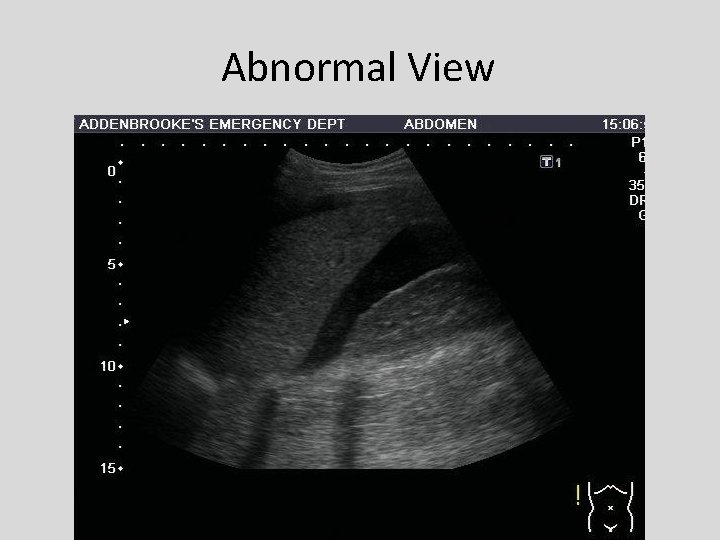
Abnormal View www. emergencyultrasound. org. uk 23

Left Upper Quadrant Window • Transducer positioned in left posterior axillary line with beam in coronal plane.
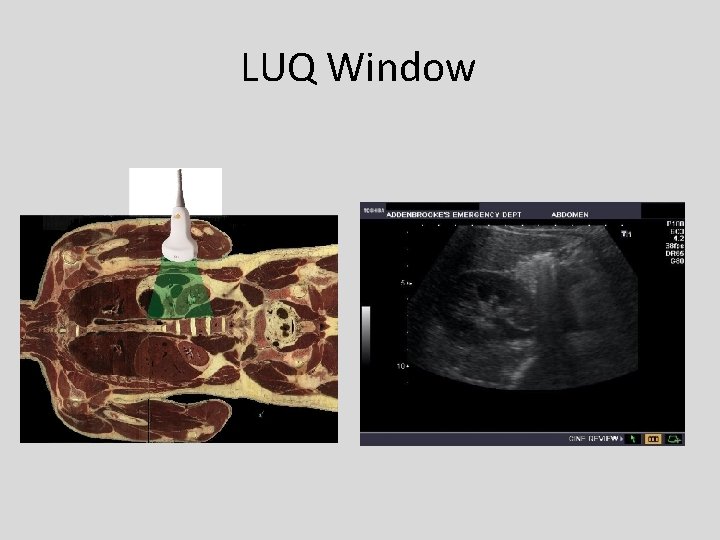
LUQ Window
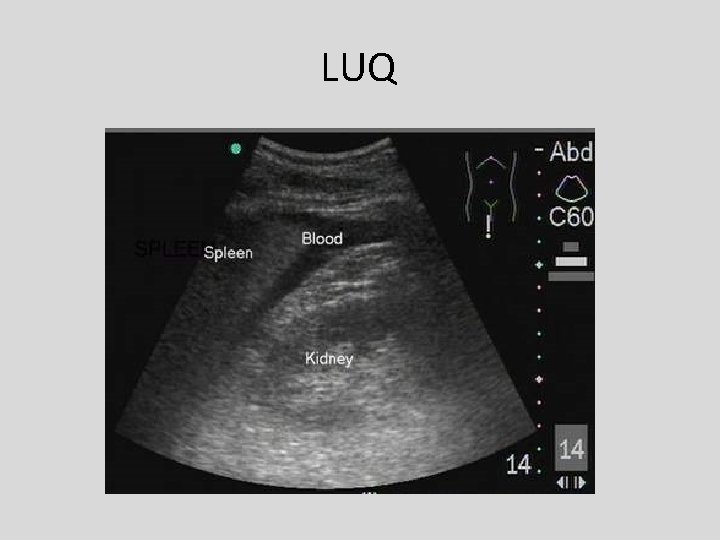
LUQ
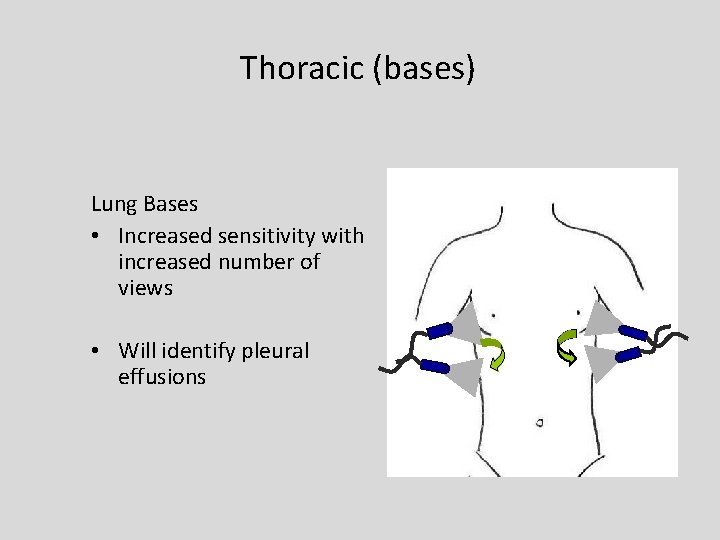
Thoracic (bases) Lung Bases • Increased sensitivity with increased number of views • Will identify pleural effusions
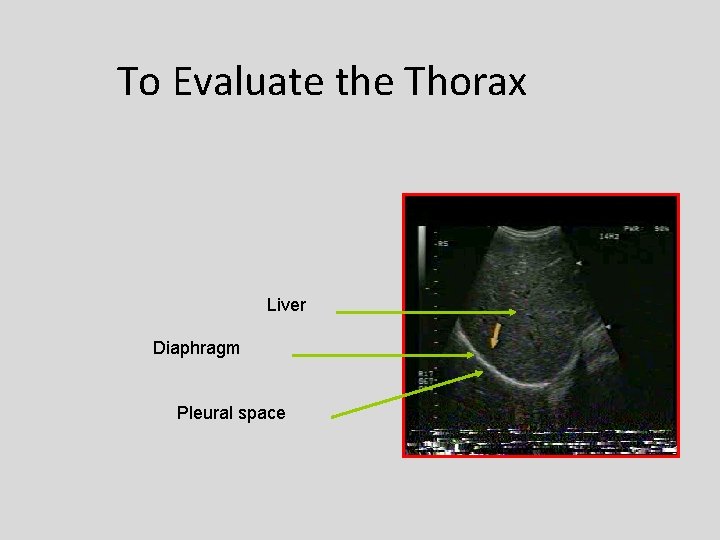
To Evaluate the Thorax Liver Diaphragm Pleural space
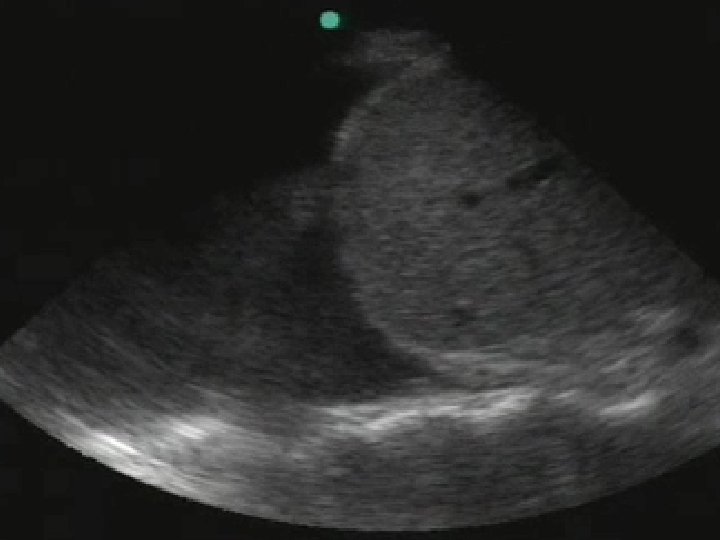
Haemothorax 29
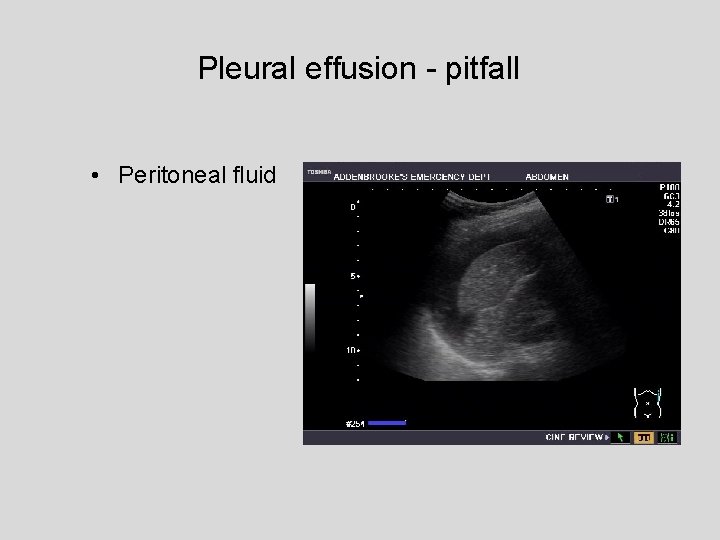
Pleural effusion - pitfall • Peritoneal fluid
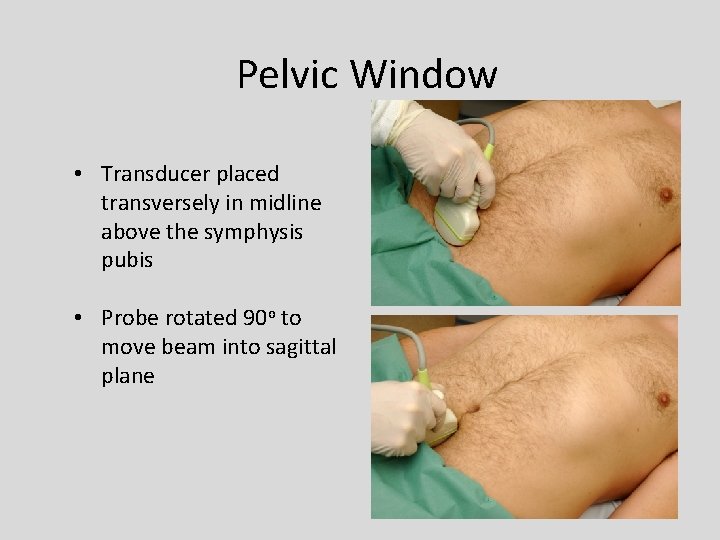
Pelvic Window • Transducer placed transversely in midline above the symphysis pubis • Probe rotated 90 o to move beam into sagittal plane

Patient 3 • 27 year old man • Altercation multiple stabbings to chest • Attended to by enhanced pre-hospital care team – RSI • Arrives with P 126 BP 63/42 • FAST shows pericardial effusion

When do you perform a thoracotomy? 1. Immediately 2. If loses output 3. Under no circumstances

When do you perform a thoracotomy? 1. Immediately 2. If loses output 3. Under no circumstances

Emergency Thoracotomy “how to do it” Wise et al Emerg Med J 2005; 22: 22 -24 • Within 10 minutes of cardiac arrest from penetrating trauma • Clam Shell thoracotomy • Bilateral 4 cm thoracostomies midaxillary line • Skin incision • Scissors (Gigli saw) – open ‘clam’, retractor • Incise pericardium
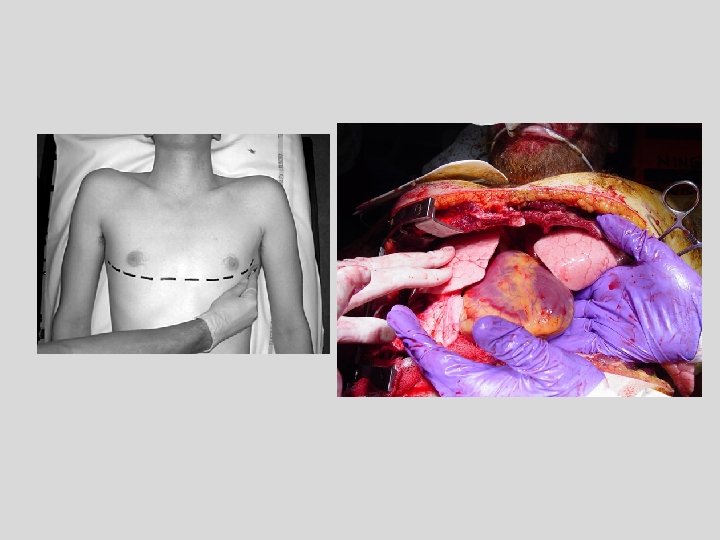

Patient 4 • • 46 year old man MVC – RSI on scene Brought be helicopter Bilateral thoracostomies prior to transfer

Where do we put the chest drains 1. Through the thoracostomy 2. Through a distant site 3. Through the thoracostomy and give IV antibiotics 4. Through a distant site and give IV antibiotics

Where do we put the chest drains 1. Through the thoracostomy 2. Through a distant site 3. Through the thoracostomy and give IV antibiotics 4. Through a distant site and give IV antibiotics

Patient 5 • • • 35 year old man Shotgun wound to right groin P 134 BP 90/46 GCS 14 (E 3 V 5 M 6) Bleeding profusely IV access and aggressive fluid resuscitation

How do we try and stop the bleeding? 1. 2. 3. 4. Firm pressure with gauze Firm pressure with CELOX Pack wound and firm pressure gauze Pack wound and firm pressure CELOX

How do we try and stop the bleeding? 1. 2. 3. 4. Firm pressure with gauze Firm pressure with CELOX Pack wound and firm pressure gauze Pack wound and firm pressure CELOX

CELOX • Haemostatic agent chitosan • Extracted from shrimp shells • Forms gel like clot once in contact with blood

Patient 6 • • • 24 year old man Jumped off roof of hospital Brought to ED within 15 minutes P 145 BP palpable carotid pulse Unable to obtain peripheral vascular access

Do you. . . 1. 2. 3. 4. Insert subclavian line Insert internal jugular line Insert intraosseous needle Insert femoral line

Do you. . . 1. 2. 3. 4. Insert subclavian line Insert internal jugular line Insert intraosseous needle Insert femoral line

EZ-IO

Summary • • • WBCT FAST Resuscitative Thoracotomy Thoracostomies CELOX EZ-IO
- Slides: 48