Abdominal Pain II Lower abdominal and pelvic pain

Abdominal Pain II – Lower abdominal and pelvic pain EMC SDMH 2015

Objectives � Briefly revise patterns of pain radiation � Differentials of lower abdominal pain � Review assessment of appendicitis � Review assessment of diverticulitis � Review assessment of types of bowel obstruction � Discuss mesenteric ischaemia � Briefly review ovarian cyst accidents

Pain modalities in the abdomen � Visceral ‘aching, cramping, dull’ Poorly localised – typically midline ‘Colicky’ � Parietal Somatic, sharp, well localised ‘Peritonitic’ � Referred Ureteric teste/vulva Cardiac epigastrium, arm, back Diaphragmatic shoulder tip
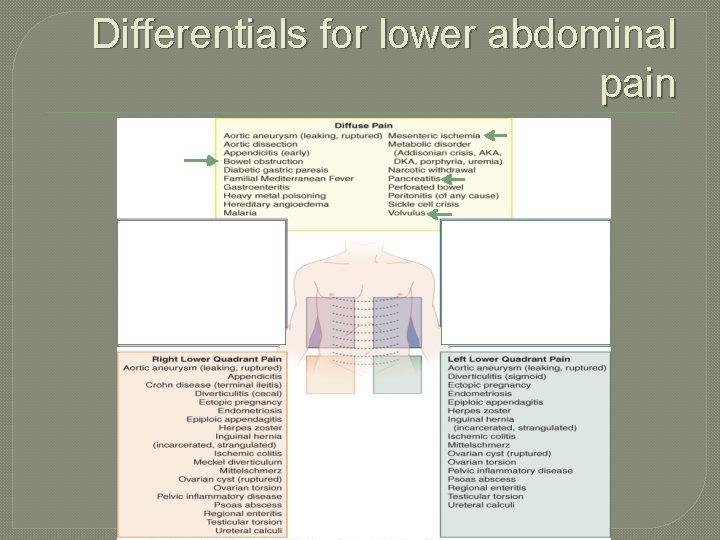
Differentials for lower abdominal pain
Appendicitis � Commonest surgical emergency � Typically younger adult � Peak in children 6 -9 yrs old � 10 % pts > 60 yrs age � 1: 1500 pregnancies � Initial diagnostic accuracy of ~ 85% � Often delayed diagnosis in children, elderly, pregnancy
Clinical features HISTORY (SPEC) � � � � Nausea Anorexia RLQ pain Migration Fever SENS EXAM 60 -90% (30%) 75% (35%) 80% (50%) 80% (80%) 50% (50%) Pain generally precedes nausea Elderly, paediatric more prone to atypical presentations � RLQ tenderness Guarding Fever � Rectal exam not helpful � Rovsings, Posas and Obturator signs may be specific, but insensitive � � 96% 25% 50%
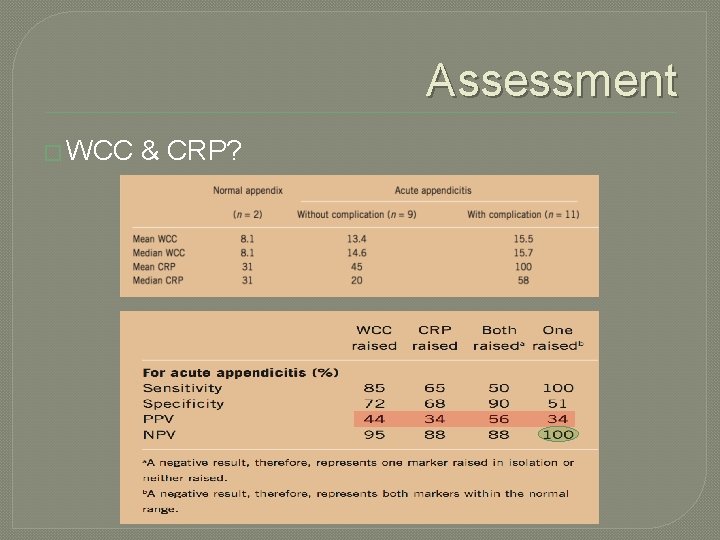
Assessment � WCC & CRP?

Decision rules u u u Alvarado Score Stratifies to high, intermediate and low risk appendicitis When compared to CT evidence Score 1 -4 4% Score 5 -6 32% Score 7 -10 - 78% u Prospective use of Alavarado <4 to exclude appendicitis ; 28% appendicitis! (Andrew et al 2013) u ~ Gestalt assessment 80 -85%
Imaging ULTRASOUND CT SCAN � Operator dependent � Generally accessible � Sensitivity 75 -90% � Sensitivity & specificity 98% � Specificity 86 -100% � Needs contrast � PPV and NPV 90 -95% � Radiation dose 8 -10 m. SV � Performs better in children

Management � Early surgical referral � May not require imaging to take to OT � IV Analgesia � IV Fluids � IV antibiotics – reduces peri-operative complication rate
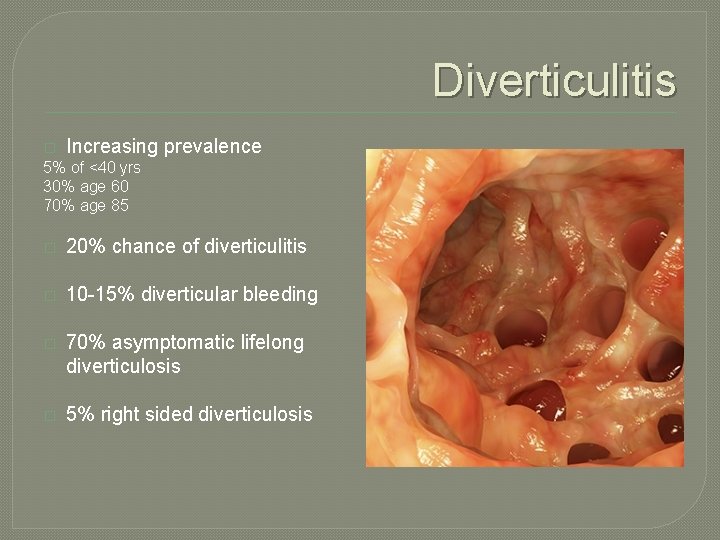
Diverticulitis � Increasing prevalence 5% of <40 yrs 30% age 60 70% age 85 � 20% chance of diverticulitis � 10 -15% diverticular bleeding � 70% asymptomatic lifelong diverticulosis � 5% right sided diverticulosis

Clinical features HISTORY � Left lower abdo pain (90%) � GI disturbance EXAM/LABS � Abdominal tenderness (90%) Fever (30%) � Leucocytosis (60%) � Clinical triad of LLQ pain, fever and leucocytosis ~25% � diarrhoea 30%, constipation 50% � Anorexia (~40%) � Nausea (~40%) � Dysuria/Frequency (10%) � Fever (30%)
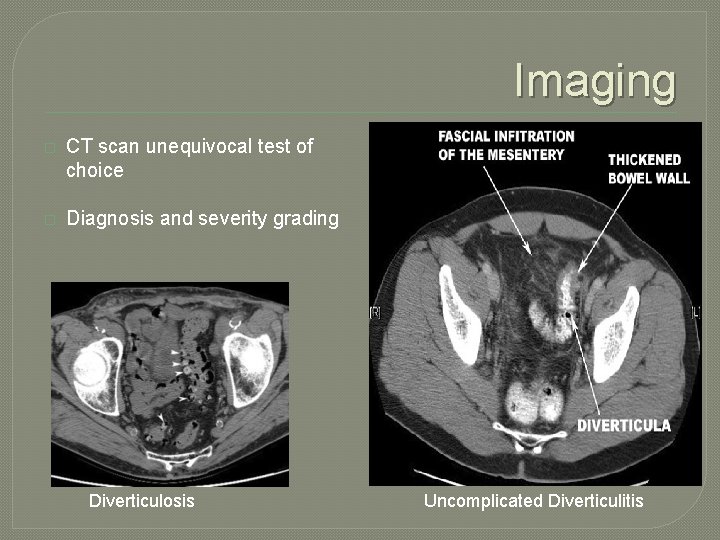
Imaging � CT scan unequivocal test of choice � Diagnosis and severity grading Diverticulosis Uncomplicated Diverticulitis
Management � Uncomplicated (75%) Inflammation simply confined to diverticulum/lumen wall � Complicated (25%) Inflammation and free fluid, abcess, collection, obstruction , perforation Depending upon institutional guidelines - NBM IV Fluids +/- resuscitation fluid Immunocompetent IV antibiotics – triple therapy Well appearing Pain controlled Targeted surgical treatment depending Self caring upon complication Clear fluid diet Oral antibiotics(Augmentin Duo) 5 -7 days(? ) Analgesia Outpatient colonoscopy 4 -6 weeks
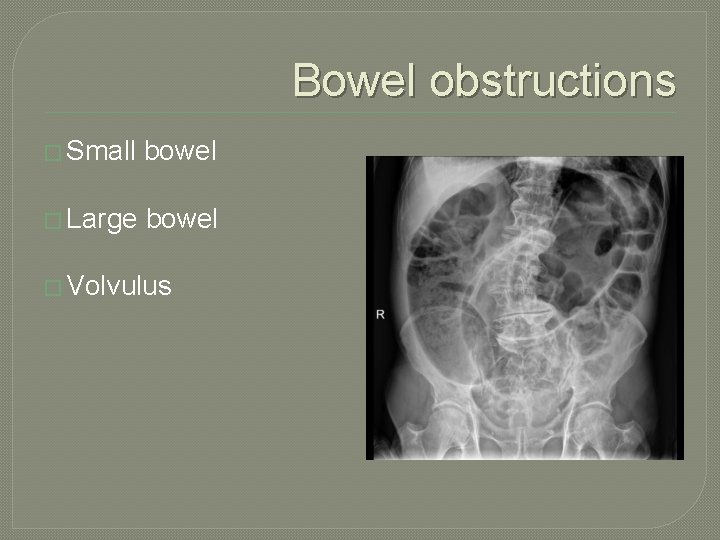
Bowel obstructions � Small bowel � Large bowel � Volvulus
Bowel obstruction HISTORY � Abdominal pain – cramping/colicky � Distension/bloating � ‘Constipation’/nil flatus � Vomiting – only if proximal EXAM / LABS � � � Abdominal distension Variable degree & nature of abdominal tenderness Bowel sounds variably present/absent Nil specific lab results – consistent with dehydration Acid base deficit/lactate elevation may suggest ischemia/sepsis – generally normal
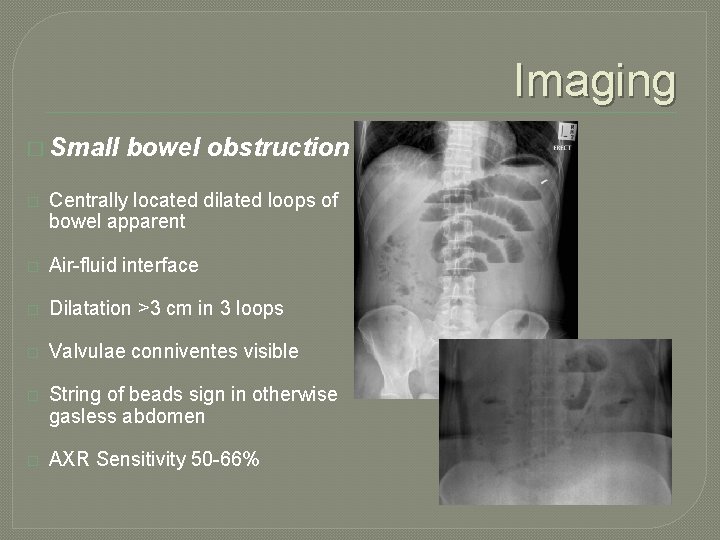
Imaging � Small bowel obstruction � Centrally located dilated loops of bowel apparent � Air-fluid interface � Dilatation >3 cm in 3 loops � Valvulae conniventes visible � String of beads sign in otherwise gasless abdomen � AXR Sensitivity 50 -66%
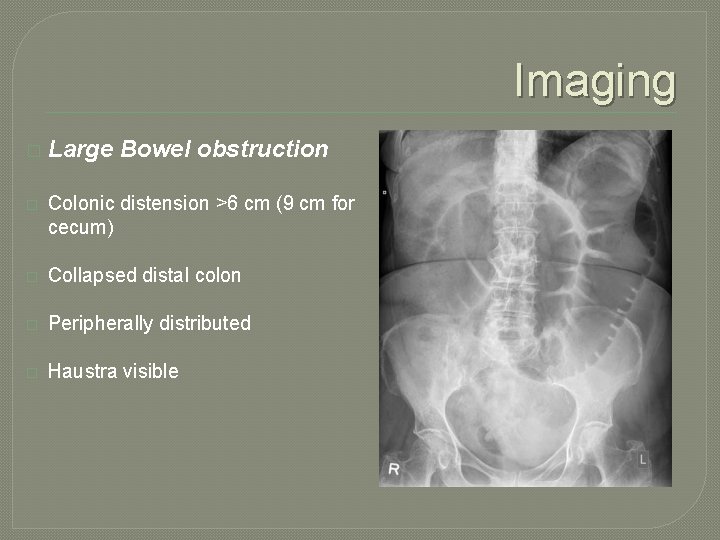
Imaging � Large Bowel obstruction � Colonic distension >6 cm (9 cm for cecum) � Collapsed distal colon � Peripherally distributed � Haustra visible
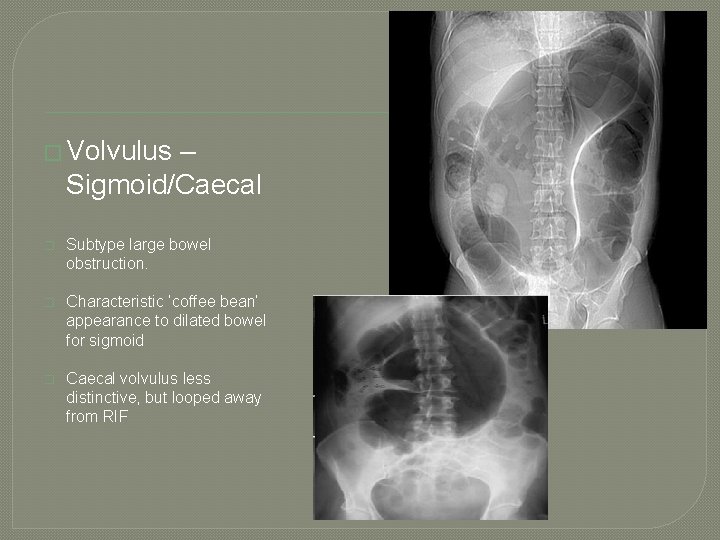
Imaging � Volvulus – Sigmoid/Caecal � Subtype large bowel obstruction. � Characteristic ‘coffee bean’ appearance to dilated bowel for sigmoid � Caecal volvulus less distinctive, but looped away from RIF

Management SMALL BOWEL (80%) LARGE BOWEL (20%) � Analgesia � NBM. � NGT optional � NGT not required � IV fluids to replace losses � CT scan to establish cause and exclude closed loop obstruction � CT scan to establish cause Adhesions/Herniae (internal/external)commonest causes Surgical consultation and admission Carcinoma/Diverticular stricture commonest reasons Sigmoid volvulus and caecal volvulus require urgent decompression to prevent bowel ischemia
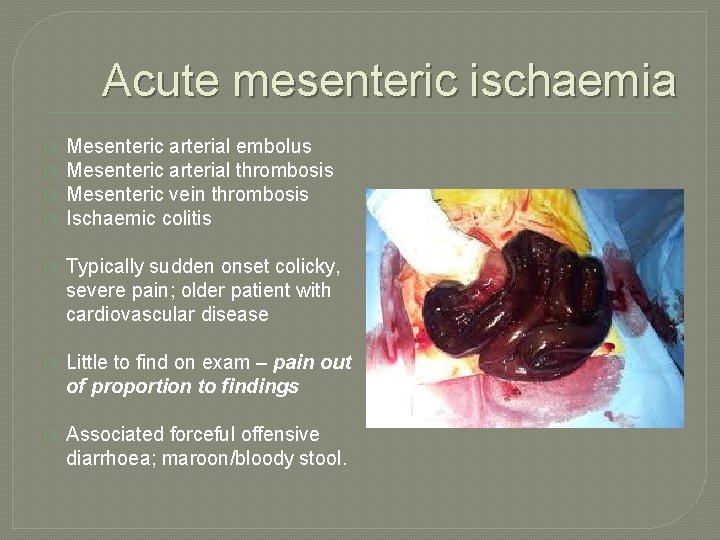
Acute mesenteric ischaemia � � Mesenteric arterial embolus Mesenteric arterial thrombosis Mesenteric vein thrombosis Ischaemic colitis � Typically sudden onset colicky, severe pain; older patient with cardiovascular disease � Little to find on exam – pain out of proportion to findings � Associated forceful offensive diarrhoea; maroon/bloody stool.
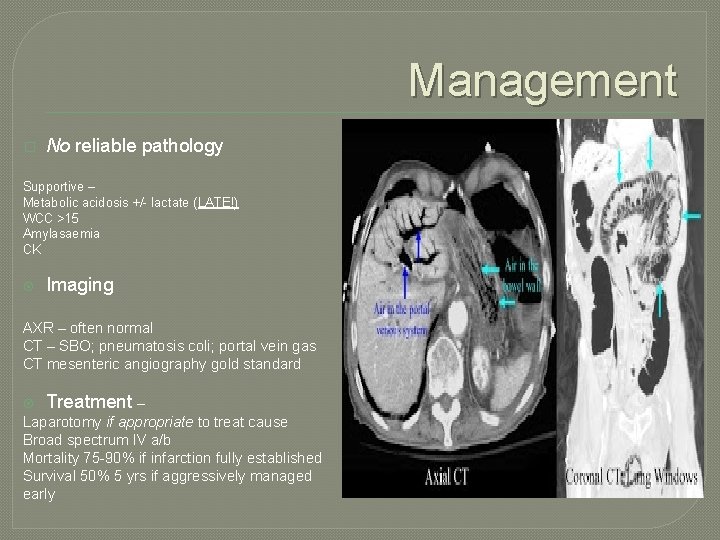
Management � No reliable pathology Supportive – Metabolic acidosis +/- lactate (LATE!) WCC >15 Amylasaemia CK Imaging AXR – often normal CT – SBO; pneumatosis coli; portal vein gas CT mesenteric angiography gold standard Treatment – Laparotomy if appropriate to treat cause Broad spectrum IV a/b Mortality 75 -90% if infarction fully established Survival 50% 5 yrs if aggressively managed early
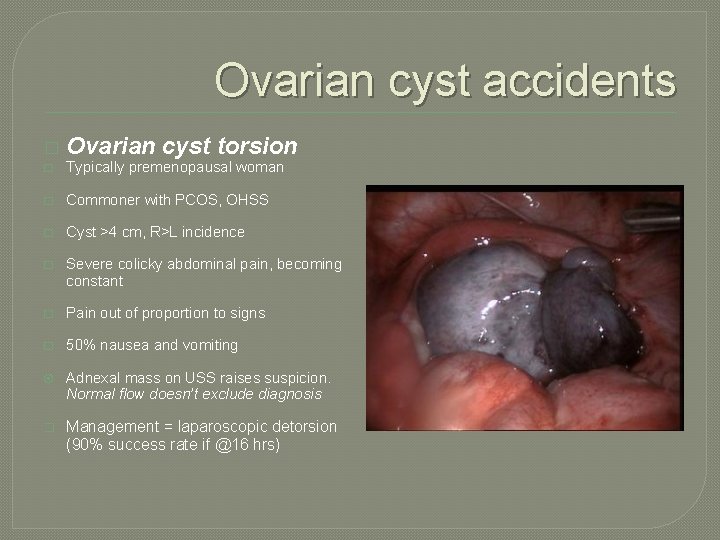
Ovarian cyst accidents � Ovarian cyst torsion � Typically premenopausal woman � Commoner with PCOS, OHSS � Cyst >4 cm, R>L incidence � Severe colicky abdominal pain, becoming constant � Pain out of proportion to signs � 50% nausea and vomiting Adnexal mass on USS raises suspicion. Normal flow doesn’t exclude diagnosis � Management = laparoscopic detorsion (90% success rate if @16 hrs)
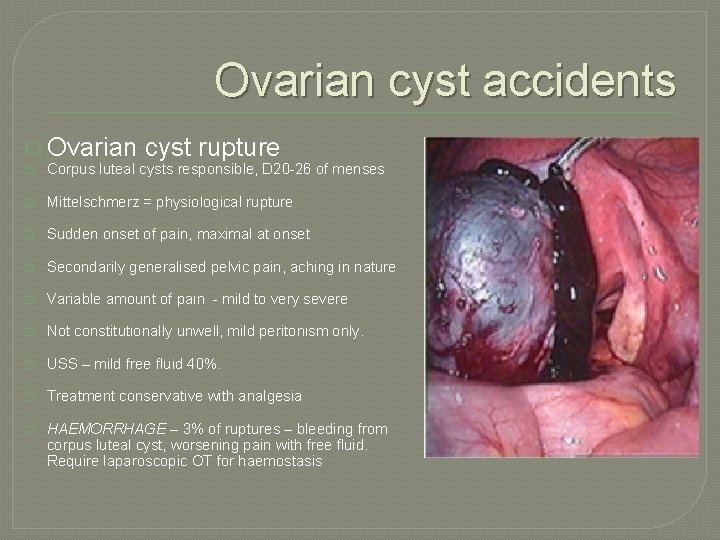
Ovarian cyst accidents � Ovarian cyst rupture � Corpus luteal cysts responsible, D 20 -26 of menses � Mittelschmerz = physiological rupture � Sudden onset of pain, maximal at onset � Secondarily generalised pelvic pain, aching in nature � Variable amount of pain - mild to very severe � Not constitutionally unwell, mild peritonism only. � USS – mild free fluid 40%. � Treatment conservative with analgesia � HAEMORRHAGE – 3% of ruptures – bleeding from corpus luteal cyst; worsening pain with free fluid. Require laparoscopic OT for haemostasis

Pelvic Inflammatory Disease � � Spectrum of illness from acute bilateral pelvic pain Tubo-ovarian abscess and sepsis � Bilateral crampy dull pain <7 days duration. Exacerbated by coitus � 75% associated with new PV discharge � Adnexal, uterine or cervical tenderness (95% sensitive). Cervicitis should be present � No pathology reliably rules in or out – inflammatory markers expected to be elevated however. Swabs for chlamydia, gonococcus � � USS demonstrates tubo-ovarian pathology in more unwell individuals (febrile), but often normal � Management � Mild infection – Ceftriaxone 500 mg + Azithromycin stat dose, metronidazole 14/7 Repeat dose azithromycin 7/7 Major infection – Ceftriaxone 2 g daily +azithromycin +metronidazole �

Questions?

Summary � History remains best predictor in appendicitis. � CRP, WCC may be more useful as rule-out tests � Outpatient treatment feasible for diverticulitis � Be mindful of possibility of closed loop obstruction in SBO and need for surgical intervention early � Acute mesenteric ischaemia – suspect early with pain out of proportion to signs � Ovarian cyst torsion – good prognosis with early OT � Ovarian cyst haemorrhage can complicate of cyst rupture, but requires OT � Don’t forget PID – although can be difficult to diagnose
- Slides: 27