Abdominal pain Dyspepsia Pathophysiology Management approach Inoshi Atukorala

Abdominal pain & Dyspepsia Pathophysiology & Management approach Inoshi Atukorala 1

Learning outcomes At the end of this lecture you will be able to 1. Apply knowledge on anatomy & physiology to explain mechanisms of abdominal pain & dyspepsia 2. Reach a reasonable clinical diagnosis in a patient presenting with abdominal pain 2
Lecture Outline Why is abdominal pain important? Clinical approach Neuroanatomy & Neurophysiology Chronic abdominal pain Dyspepsia 3

Why is abdominal pain important? 4

Why is abdominal pain important? • Extremely common • Causes much human suffering • Costly: Ix, Rx, delayed diagnosis & Rx • Difficult to diagnose 5

What are the difficulties in diagnosis? I • Clinical features of pain alone => are not enough for evaluation • Special tests =>? expensive with limited availability • A subjective experience • great variability of presentation/ contributory factors: – Pathophysiological – Neuroanatomical Variability – Psychosocial 6

Clinical approach 7

The clinical approach Abdominal pain Clinical clues accurate pathophysiological diagnosis Ix & Rx 8

What do we need to know? • Neuroanatomy & neurophysiology of the GIT • Pathophysiology & natural history of diseases • Role of psychosocial factors in disease presentation • Therapeutic options available 9

Neuroanatomy & Neurophysiology 10

Neuroanatomy & neurophysiology-1 • Somatic pain vs visceral pain • Life-threatening visceral pathology can be entirely asymptomatic! Visceral pain Due to disease process or abnormal function of an internal organ or it’s covering Visceral pain 1. 2. 3. 4. True localized visceral pain Referred visceral pain Localized parietal pain Referred parietal pain 11
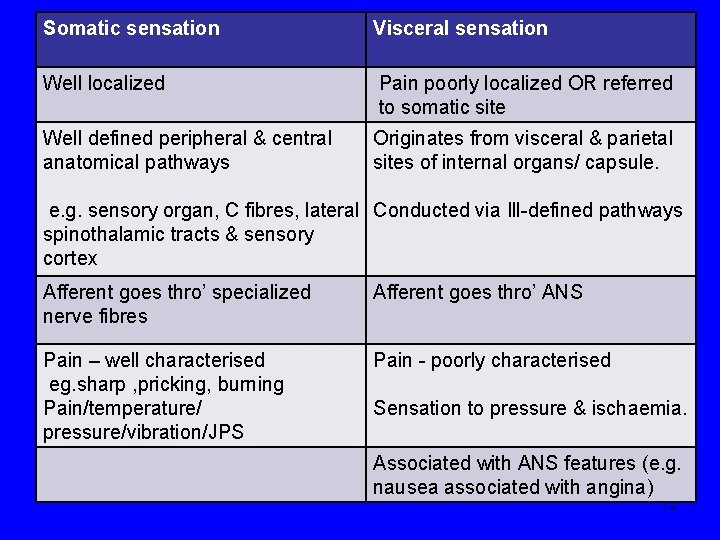
Somatic sensation Visceral sensation Well localized Pain poorly localized OR referred to somatic site Well defined peripheral & central anatomical pathways Originates from visceral & parietal sites of internal organs/ capsule. e. g. sensory organ, C fibres, lateral Conducted via Ill-defined pathways spinothalamic tracts & sensory cortex Afferent goes thro’ specialized nerve fibres Afferent goes thro’ ANS Pain – well characterised eg. sharp , pricking, burning Pain/temperature/ pressure/vibration/JPS Pain - poorly characterised Sensation to pressure & ischaemia. Associated with ANS features (e. g. nausea associated with angina) 12

Neuroanatomy & neurophysiology-4 Visceral pain mediation: – Mucosal receptors: chemical stimuli – Mural, serosal, mesenteric receptors: distension/contraction, traction/compression/torsion, stretch, chemical stimuli – Pain threshold increased by mucosal inflammation, smooth muscle tone Visceral nociceptors are of 3 functional types: 1. Low-threshold, intensity-coding afferents: activated by normal activity, graded response Regulatory reflexes non-painful sensations (e. g hunger, nausea) pain Common in the colon 13

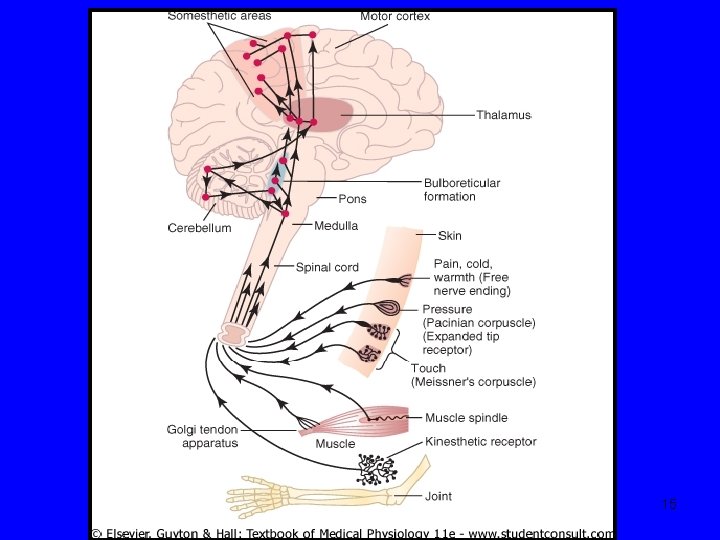
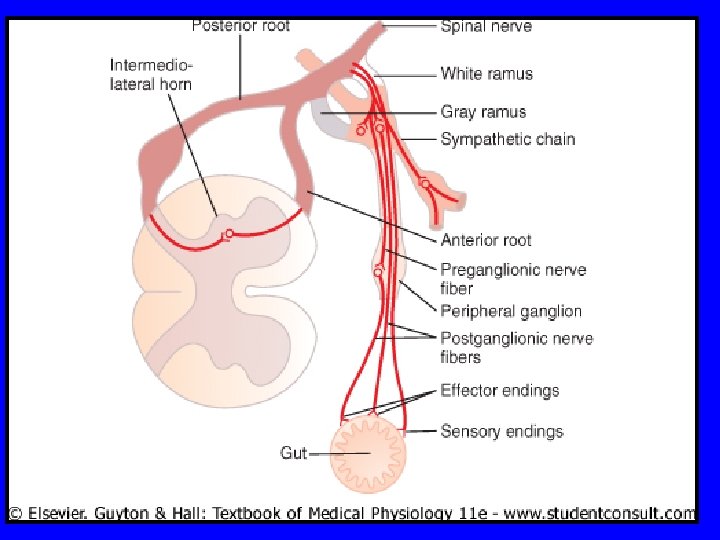
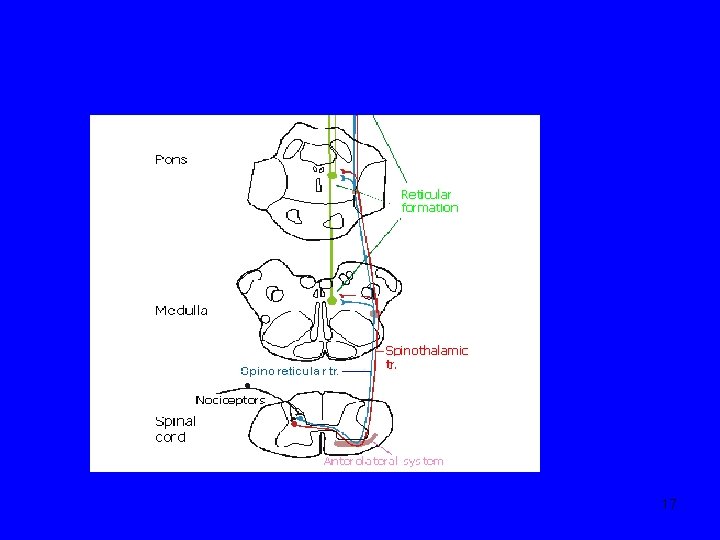
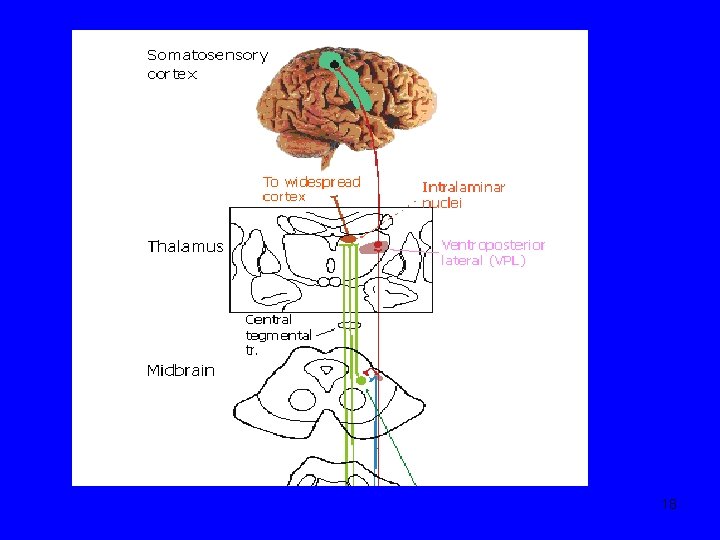
Neuroanatomy & neurophysiology-6 2 High-threshold, ‘dedicated’ nociceptors: mediates only pain (eg biliary tree) 3 ‘Silent’ nociceptors: activated by inflammation/injury or by normal triggers (Is this why patients with IBS experience pain at lower levels of stimulation? ) • • • 1 st order neurons go via arteries, plexuses to sympathetic ganglia 2 nd order neurons enter spinal cord spinothalamic, spinoreticular tracts thalamus & brain stem 3 rd order neurons reach somatosensory cortex & limbic system/frontal cortex 14
15
16
17
18

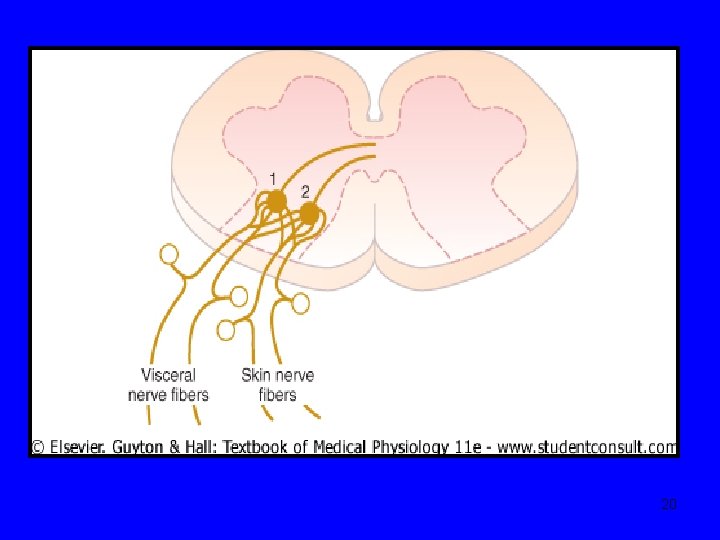
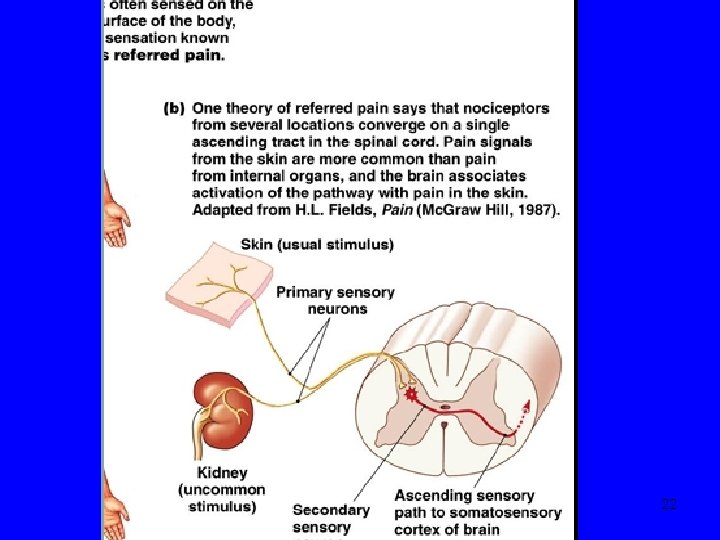
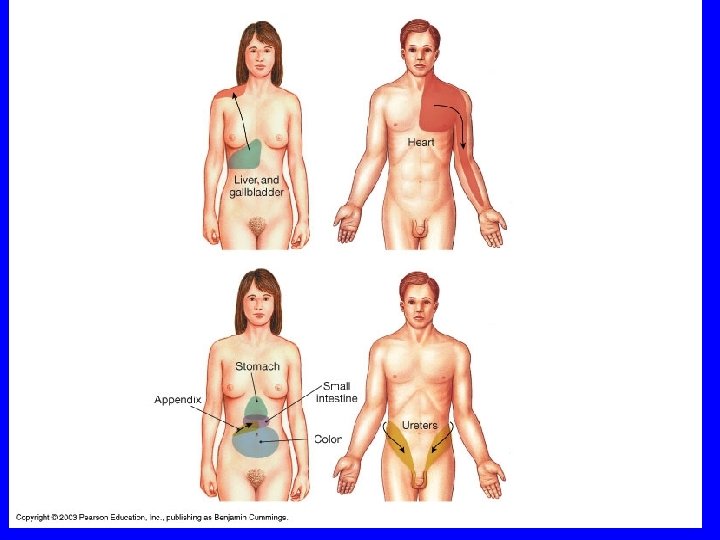
• • • Neuroanatomy & neurophysiology-9 Visceral pain from GIT usually poorly localized & in the midline ‘Foregut’: between xiphisternum & umbilicus (T 5 -T 9). Gallbladder pain may be lateralised ‘Midgut’: periumbilical (T 8 -T 11). Pain from ascending colon may be lateralised ‘Hindgut’: between umbilicus & pubis (T 11 -L 1). Pain from descending colon may be lateralized Pain will shift with visceral parietal involvement (eg gallbladder, appendix) Referred pain (e. g. gallbladder) 19
20
22
23

Neuroanatomy & neurophysiology-11 • Chronic pain may occur with or without continuing nociceptive input from the relevant organ (eg chronic pancreatitis) – like in the ‘phantom limb’ phenomenon 24

Chronic abdominal pain The clinical approach • Chronic abdominal pain – Intermittent – Chronic pain + established cause – Chronic pain without pathophysiological explanation 25
Chronic Abdominal Pain Chronic intermittent abdominal pain Chronic abdominal pain with cause Chronic abdominal pain without a cause 26

Chronic intermittent abdominal pain -1 • Recurrent episodes of pain lasting several hours to days, with NO PAIN in between episodes • A specific, treatable cause usually present • Careful clinical evaluation extremely useful • Physical – cholelithiasis, intermittent intestinal obstruction, peptic ulcer disease • Metabolic/genetic – acute intermittent porphyria • Neurological – diabetic radiculopathy, migraine, nerve entrapment syndromes, vertebral nerve root compression • Miscellaneous – Crohn’s disease, endometriosis, mesenteric ischaemia, ovulation, heavy metal poisoning, autoimmune disorders 27

Chronic intermittent abdominal pain ctd Occurrence and periodicity: – Monthly pain: ovulation, endometriosis – Drug-induced: AIP, pancreatitis (steroids, thiazides, tetracyclines) – Meal-related: mesenteric ischaemia, chronic pancreatitis – Posture-related: nerve root compression, entrapment syndromes Associated features: – Headache, visual aura: migraine – Jaundice, dark urine: cholelithiasis, gallstone pancreatitis – Anal fissure: Crohn’s disease – Abdominal signs of intestinal obstruction – Muscle spasm/rigidity: lead poisoning – Soft exudates, purpura: polyarteritis nodosa, SLE Co-morbidity: – Diabetes: neuropathy – Perianal disease: Crohn’s disease 28

Chronic pain with an identified cause- 1 • Once pain has been present for several months, associated features will point to the cause • The challenge is to use therapeutic options wisely • • Weight loss: malignancy, depression, chronic pancreatitis Pathological fractures: malignancy, osteoporosis Fever: intra-abdominal abscess, autoimmune disease, lymphoma The presence of jaundice, ascites or abdominal masses will help diagnosis Chronic pain with an identified cause- Rx • Drugs: – NSAIDs, opioids, antidepressants, anxiolytics • Nerve destruction or stimulation techniques: – Chemical /surgical nerve destruction (eg coeliac plexus blockade, sympathectomy, rhizotomy, cordotomy) – Transcutaneous electrical nerve stimulation (TENS) • Other methods: 29 – Relaxation therapy, hypnosis, psychotherapy

Chronic pain without a pathophysiological explanation -1 • Chronic intractable abdominal pain or chronic idiopathic abdominal pain (CIAP) • Definition: Abdominal pain present most of the time for > 6/12 without a diagnosis despite Ix • A bio-psychosocial approach is best Characteristic features: – Usually female (70%) – Pain - vague, bizzare, ‘idiosyncratic’ – Pain - “elsewhere in the body” – ‘Social’ or psychological precipitating factors c – Childhood pain, abuse – Globally disabled – Psychological problems common: depression, anxiety, withdrawal, loss of libido 30

Chronic pain without a pathophysiological explanation ctd • Establish rapport and trust – Acknowledge pain as real – Respectful, non-judgmental – Schedule brief, frequent visits – Reassurance • Set appropriate goals – Do not expect cure – Reduce impact on life – Complementary medicine • Shift emphasis from diagnosis to treatment – Reduce tests – Discuss treatment options • Focus on ‘adjustment’ rather than ‘cure’ – Coping. adaptation – Improved functionality • Maintain a ‘multidisciplinary’ approach – Referrals/Complementary medicine 31

The clinical approach Chronic abdominal pain Intermittent • Diagnose specific therapy Chronic pain + established cause • Therapeutic options to minimise pain Chronic pain without pathophysiological explanation • A bio-psychosocial approach used 32

Dyspepsia • • • A term that means different things to different people! – Upper abdominal/lower chest pain with or without relationship to food – Regurgitation, heartburn & waterbrash – Anorexia, nausea & vomiting – Bloating, belching, flatulence (Davidson’s Principle and Practice of Medicine, 18 th edition) Why use it at all? Used to indicate a non-specific symptom that is thought to arise from the upper GIT …but may in fact be due to GI disease in other parts or to non-GI disease Upper GI disease – Peptic ulcer disease, GI reflux disease, acute gastritis, cholelithiasis, GI motility disorders (oesophageal spasm), functional (non-ulcer) dyspepsia Other GI disorders – Irritable bowel syndrome, pancreatic disease (chronic pancreatitis, cancer), hepatic disease (hepatitis, metastasis), colonic cancer 33

• • Dyspepsia- GIT causes Gastro-oesophageal reflux disease Biliary pain Irritable bowel syndrome Aerophagia Dyspepsia- Non-GIT causes Systemic disease – IHD, renal failure, hypercalcaemia Drugs – NSAIDs, iron or K+ Rx, steroids, digoxin Other causes – Alcohol, pregnancy, psychological problems (e. g. anxiety, depression) 34

Dyspepsia: clinical approach • A thorough clinical evaluation to look for clues to the cause – ‘Alarm’ features: • Weight loss • Anaemia • Haematemesis or malaena • Dysphagia • Palpable abdominal mass • Lymphadenopathy • C/F of Chronic Liver/Kidney/ Heart Disease • Tests to confirm clinical suspicion treatment 35

Take home message • Abdominal pain is difficult to diagnose • Neurophysiology/neuroanatomy will help understand how abdominal pain occurs • Always check for “alarm signs” => sinister cause 36
- Slides: 35