ABDOMINAL COMPARTMENT SYNDROME AND OPEN ABDOMEN Abreviations IAP

ABDOMINAL COMPARTMENT SYNDROME AND OPEN ABDOMEN
Abreviations IAP = Intra-abdominal pressure IAH = Intra–abdominal hypertension APP = Abdominal perfusion pressure MAP = Mean arterial pressure ACS = Abdominal Compartment Syndrome

NORMAL INTRA-ABDOMINAL PRESSURE (IAP) ØThe pressure within the abdominal cavity ØNormal: 5 – 7 mm. Hg

Intra–Abdominal Hypertension (IAH) = sustained or repeatedly elevated IAP ≥ 12 mm. Hg

Grades of IAH Grade III Grade IV 12 – 15 mm. Hg 16 – 20 mm. Hg 21 – 25 mm. Hg >25 (ACS) ACS = Abdominal Compartment Syndrome

IAH Effects >12 mm. Hg IAP has significant effects on abd. organs and cardiac output with subsequent dysfunction of both abd. and extra-abd. organs

IAH Effects APP = MAP – IAP

Definition of ACS A sustained IAP > 25 mm. Hg, associated with new organ dysfunction Adverse physiological effects caused by massive interstitial and retroperitoneal swelling which lead to MOF (Multi Oran Failure)

ACS classification Primary ACS – associated with injury or disease in abdomen requiring early intervention Secondary ACS is from conditions not originating in the abdomen Recurrent ACS is the redevelopment of ACS following previous treatment of ACS
Primary causes of ACS Abdominal trauma with bleeding Pancreatitis Ruptured abdominal aortic aneurysm Retroperitoneal hematoma Obstructions/ileus Pneumoperitoneum Abscesses Visceral edema

Secondary Causes of ACS Acute respiratory distress syndrome Major trauma or burns Massive fluid resuscitation Hypothermia Acidosis Hypotension Massive blood transfusion Coagulopathy Sepsis

Chronic causes of ACS Obesity Liver failure with ascites Malignancies
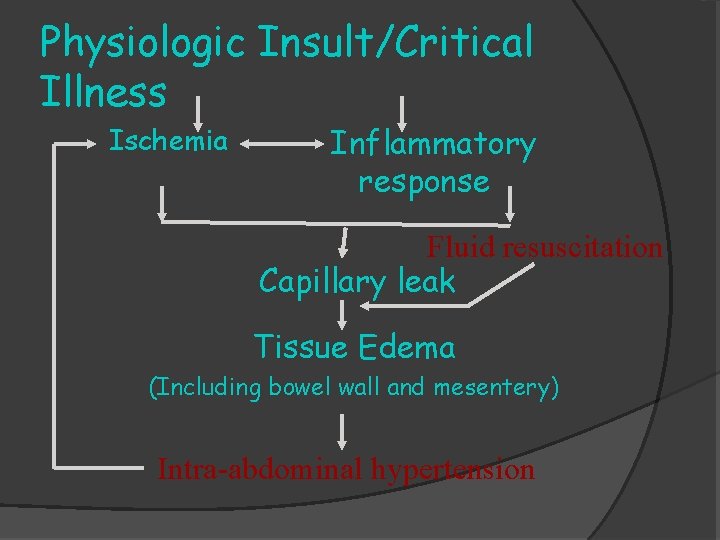
Physiologic Insult/Critical Illness Ischemia Inflammatory response Fluid resuscitation Capillary leak Tissue Edema (Including bowel wall and mesentery) Intra-abdominal hypertension

Pathophysiological Consequences of ACS Cardiovascular Reduced Cardiac Output Compression of the inferior vena cava and portal vein Reduced blood return to the heart Increased afterload from mechanical compression of vascular beds and vasoconstriction Tachycardia Increased pressure on great vessels making hemodynamic monitoring challenging with falsely elevated and misguiding pressures Increased risk for thromboembolic events secondary to venous stasis

Pathophysiological Consequences of ACS Respiratory/Pulmonary Reduced lung compliance secondary to diaphragmatic elevation → Increased peak airway → Increased risk of barotrauma Increased work of breathing → Hypoventilation and ventilation-perfusion mismatch→ Hypoxia and hypercarbia

Pathophysiological Consequences of ACS Renal decreased renal blood flow and glomerular filtration → Oliguria (IAP: 15 – 20) or Anuria (IAP: >30) Increase of antidiuretic hormone and activation of renin-angiotensin-aldosterone system (RAAS) → Increased water retention

Pathophysiological Consequences of ACS Gastrointestinal Reduced blood flow → Intestinal ischemia → Paralitic ileus

MEASURING INTRAABDOMINAL PRESSURE

Measuring IAP Physical examination yields low levels of detection of IAH/ACS Early detection and intervention reduces morbidity and mortality. Diagnosis is dependent on frequent and accurate measurement of IAP Cost effective, safe and accurate

Types of Measurements Direct pressure via intraperitoneal catheters Indirect pressure Gastric measure Rectal Urinary bladder pressure IVC

Urinary Bladder Pressure Reproducible and technically the most reliable Correlate closely with pressures measured directly in the abdominal cavity Transduced through a Foley catheter

Intermittent Monitoring Open Systems Closed Systems

Equipment needed for open measurement Disposable transducer 12” pressure monitoring tubing 4 -way stopcock Red dead-ender 60 cc, luer-lock syringe Sterile normal saline Clamp Disadvantages Risk of infection

Closed Monitoring Ab. Viser, Wolfe Tory Medical, SLC, UT Pre-assembled kit Adapts to Foley catheter and any transducer Reduces risk of infection Readily available, easily assessable data

Measuring Bladder Pressure Position patient flat & supine Read Mean pressure End Expiration

OPEN ABDOMEN

Abdominal Wall Closure Optimal closure technique based on 1. Amount of blood lost 2. Volume of fluid received 3. Degree of contamination present 4. Nutritional status 5. Overall stability

Standard Abdominal Wall Closure most common technique is continuous closure with monofilament suture single or multiple layers (peritoneum and fascia) continuous or interrupted Major benefit: relatively fast
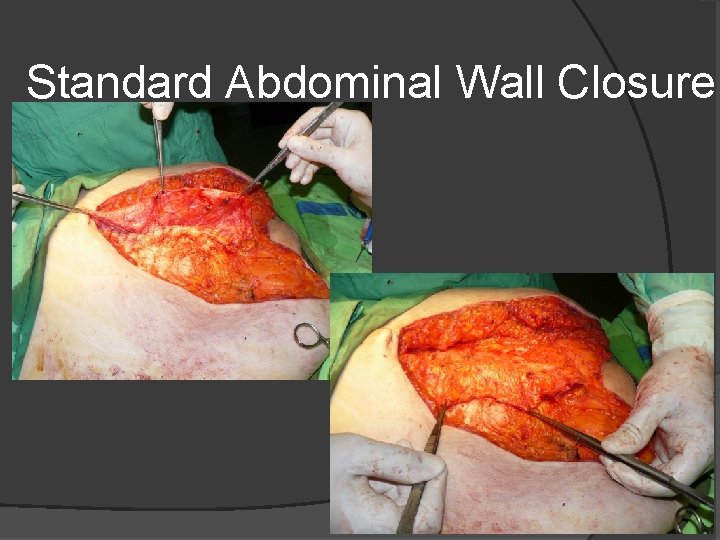
Standard Abdominal Wall Closure
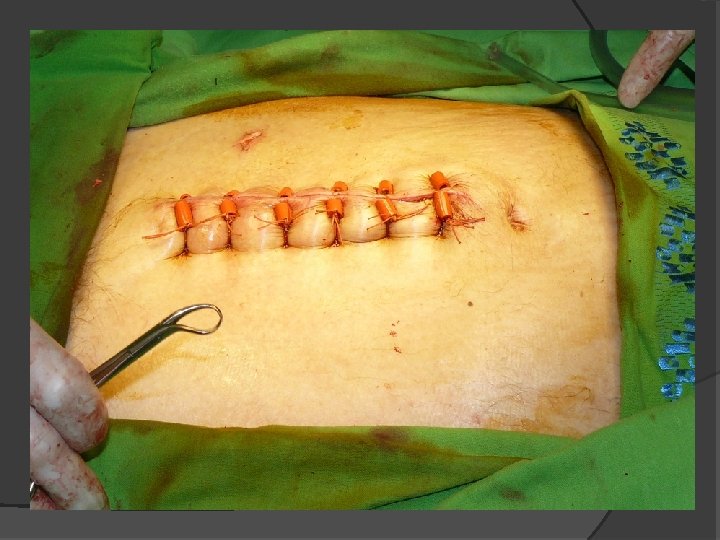
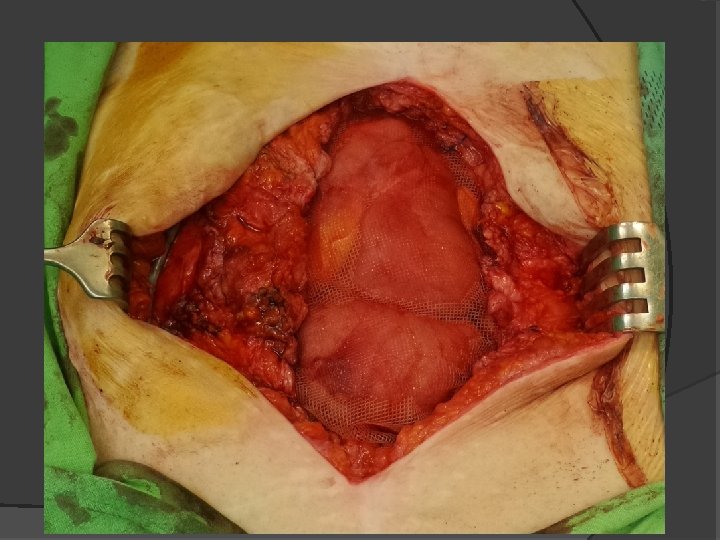
Indications for open technique Excessive visceral edema / bowel distentionfascial edges may not be brought together Post “damage control” laparotomy- gauze packs may displace abdominal contents Planned reexploration-closure damages fascia before the definitive repair Abdominal compartment syndrome (IAP > 25 mm. Hg)

Disadvantages of open abdomen Exposed intestines at increased risk for infection perforation subsequent „enteroatmospheric” fistulas frozen abdomen Definitive closure extremely difficult due to fascial retraction huge incisional hernias

Options for temporary closure Simple coverage with moist lap pads Towel clips “Bogota Bag” Repeated entry: zippers, velcro, slide fasteners Mesh

Simple coverage with moist lap pads perform only in extreme circumstances gauze adheres to bowel nonadherent material should be placed directly against abdominal viscera drain placed between nonadherent material and towel
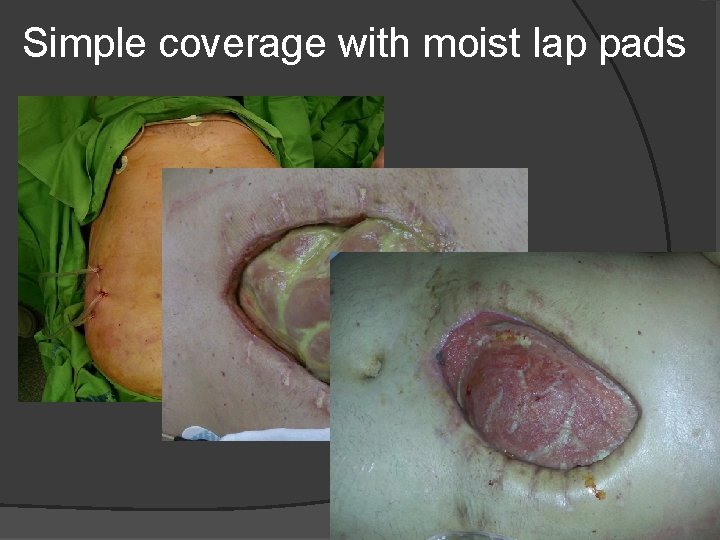
Simple coverage with moist lap pads
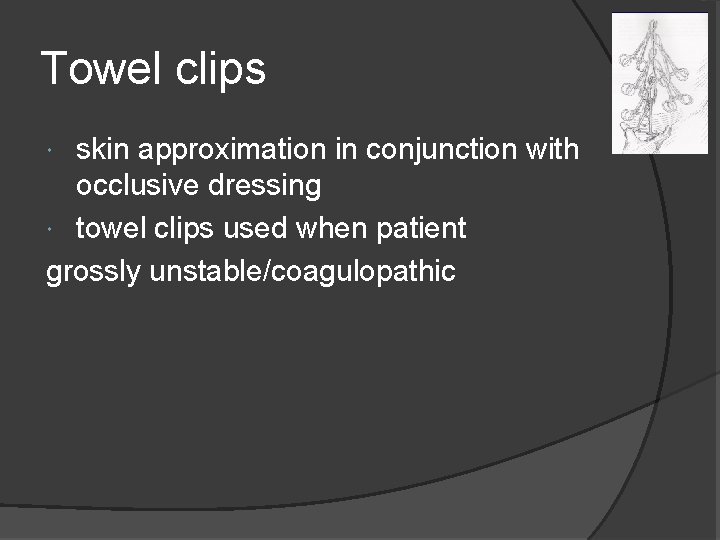
Towel clips skin approximation in conjunction with occlusive dressing towel clips used when patient grossly unstable/coagulopathic
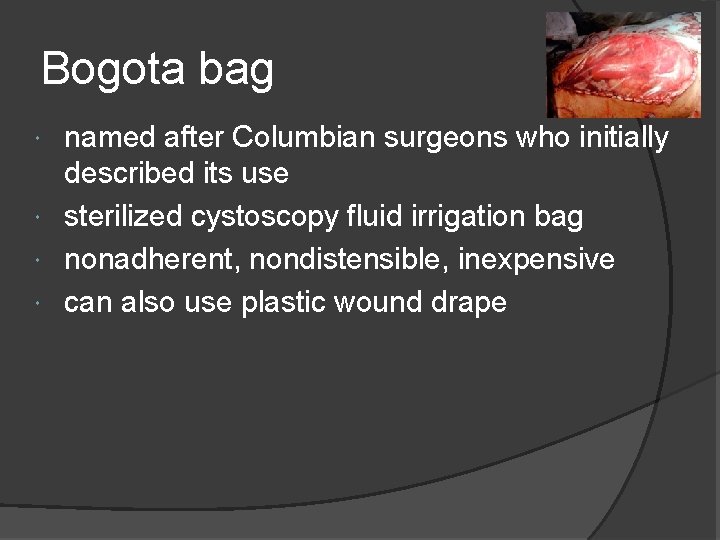
Bogota bag named after Columbian surgeons who initially described its use sterilized cystoscopy fluid irrigation bag nonadherent, nondistensible, inexpensive can also use plastic wound drape
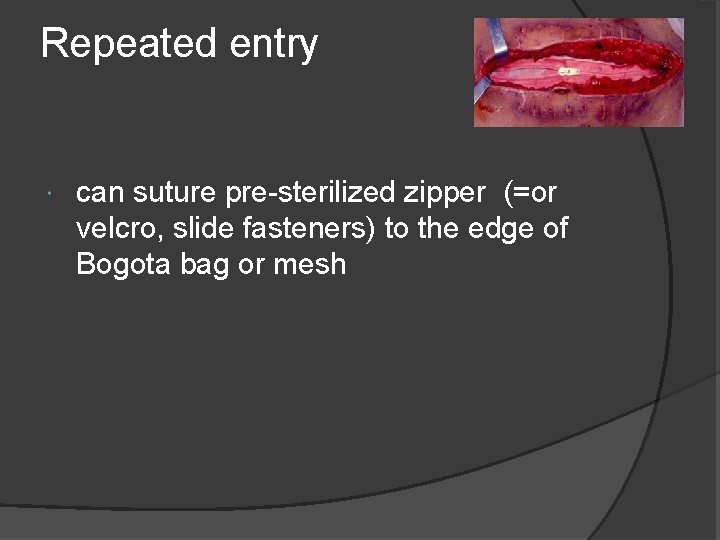
Repeated entry can suture pre-sterilized zipper (=or velcro, slide fasteners) to the edge of Bogota bag or mesh
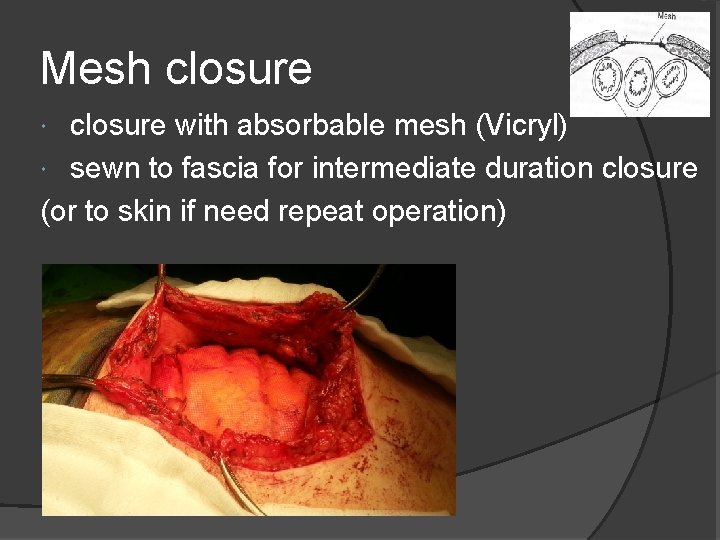
Mesh closure with absorbable mesh (Vicryl) sewn to fascia for intermediate duration closure (or to skin if need repeat operation)
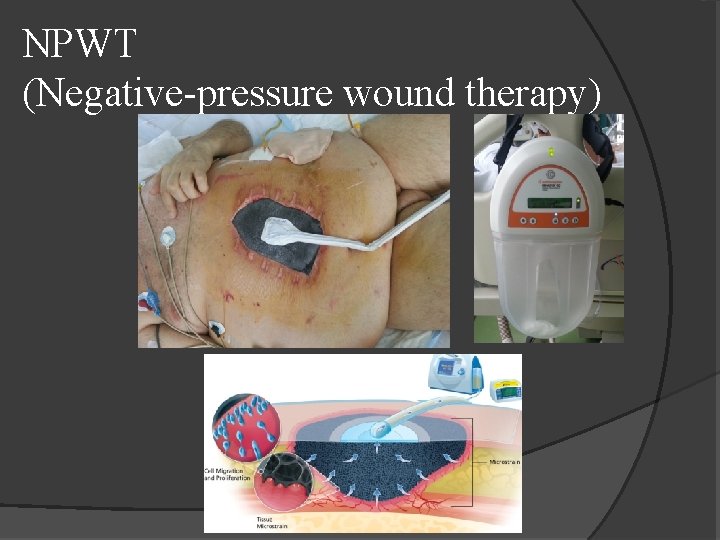
NPWT (Negative-pressure wound therapy)

Vacuum-assisted fascial closure VAC dressing placed when initial edema resolved and sponge can fit in wound nonadherent polyethylene sheet placed over bowel and under fascial edges to prevent adhesions VAC sponge held in place with adherent dressing vacuum allows for constant medial traction on fascia, preventing retraction and loss of domain dressing changed every 3 to 5 days in OR
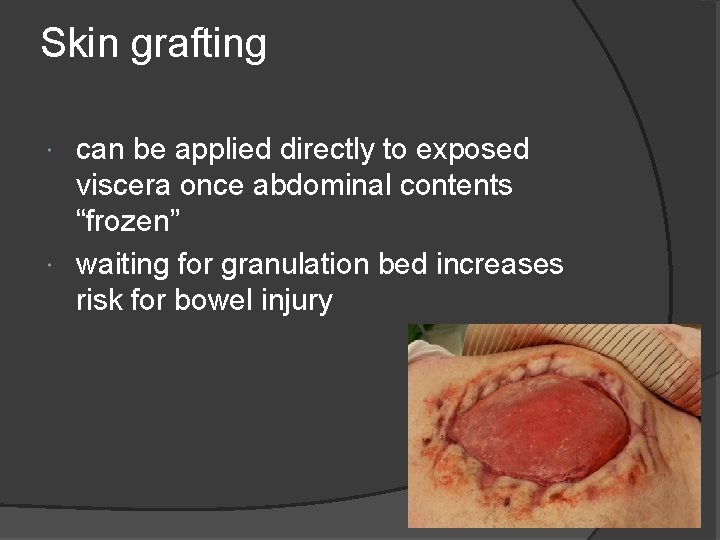
Skin grafting can be applied directly to exposed viscera once abdominal contents “frozen” waiting for granulation bed increases risk for bowel injury

Reconstruction tissue alone coverage may be achieved with skinflaps if fascia can close without tension, close primarily in standard manner if fascial defect remains: ◦ can place prosthetic mesh (eg. Composit mesh or biological) ◦ relaxing incisions in the external oblique aponeurosis lateral to rectus sheath
- Slides: 44