Abdomen Pelvis and Perineum ANA 301 Course Outline

Abdomen, Pelvis and Perineum ANA 301

Course Outline • Anterior abdominal wall (femoral and inguinal hernias) • Peritoneal reflections and mesenteries • Esophagus and stomach • Small intestine • Colon, cecum, appendix, and anal canal • Liver, gallbladder, biliary tracts • Vasculature of the abdomen (portocaval system) • Pancreas and spleen • Posterior abdominal wall – kidney and adrenal gland • Lumbar plexus • Osteology of the pelvis (sex differences / clinical importance) • Pelvis and perineum • Sacral plexus • Levator ani muscles • Male internal and external genitalia • Female internal and external genitalia 2

Abdomen • Part of the trunk between the thorax and the pelvis. • Houses organs of the alimentary system and part of the urogenital system. • Containment of these organs and their contents is provided by musculo-aponeurotic walls anterolaterally, the diaphragm superiorly, and the muscles of the pelvis inferiorly. • Anterolateral musculo-aponeurotic walls are suspended by the inferior margin of the thoracic skeleton superiorly and the pelvic girdle inferiorly and lumbar vertebral column in the posterior abdominal wall. 3
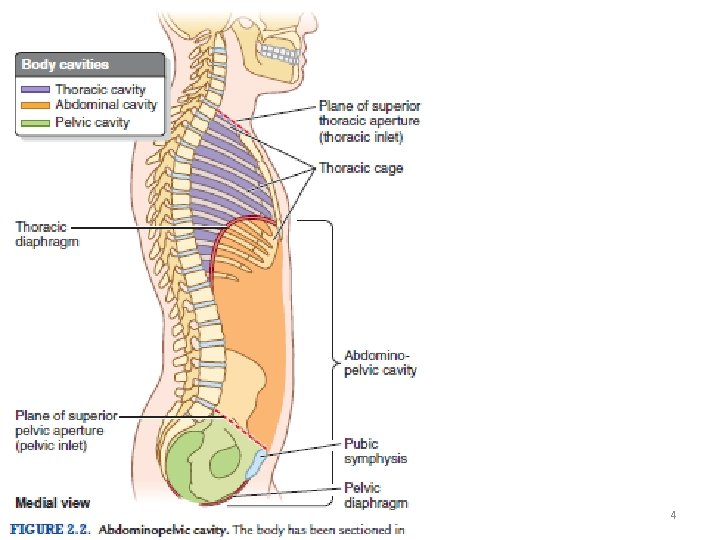
4
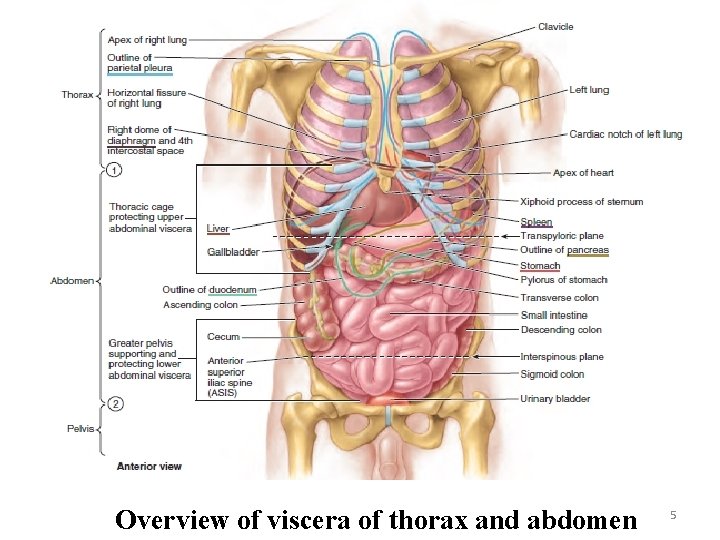
Overview of viscera of thorax and abdomen 5

• Musculo-aponeurotic abdominal walls contract to increase intra-abdominal pressure and distend to accommodate expansions • Anterolateral abdominal wall (AAW) and several organs lying against the posterior wall are covered on their internal aspects with serosa that reflects onto the abdominal viscera. • Peritoneal cavity is formed between the walls and the viscera • Double-layered reflections of peritoneum provide passage for the blood vessels, lymphatics, fat and nerves. 6

Abdominal cavity • Forms the superior and major part of the abdominopelvic cavity • Extends between the thoracic diaphragm and pelvic diaphragm. • Continuous with the pelvic cavity. • Plane of the pelvic inlet (superior pelvic aperture) separates the abdominal and the pelvic cavities. • Extends superiorly to the thoracic cage to the 4 th intercostal space. • Superiorly placed abdominal organs (spleen, liver, part of the kidneys, and stomach) are protected by the thoracic cage. • Greater pelvis (expanded part of the pelvis superior to the pelvic inlet) supports and partly protects the lower abdominal viscera (part of the ileum, cecum, appendix, and sigmoid colon). • Location of most digestive organs, parts of the urogenital system (kidneys and most of the ureters), and the spleen. 7

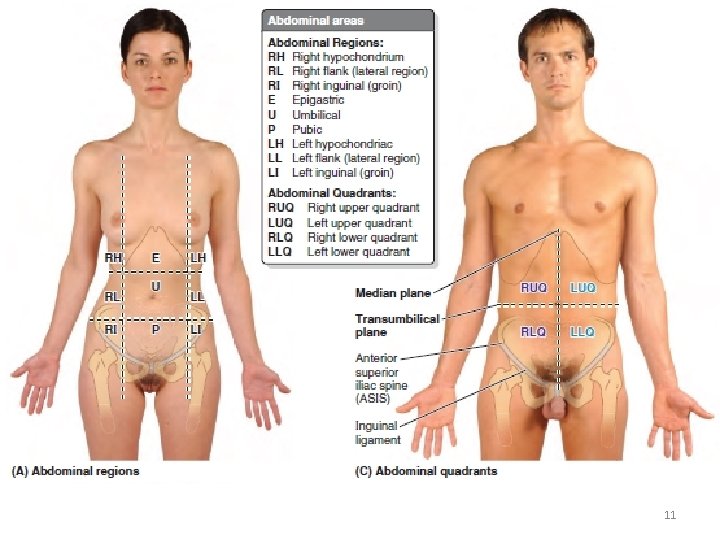
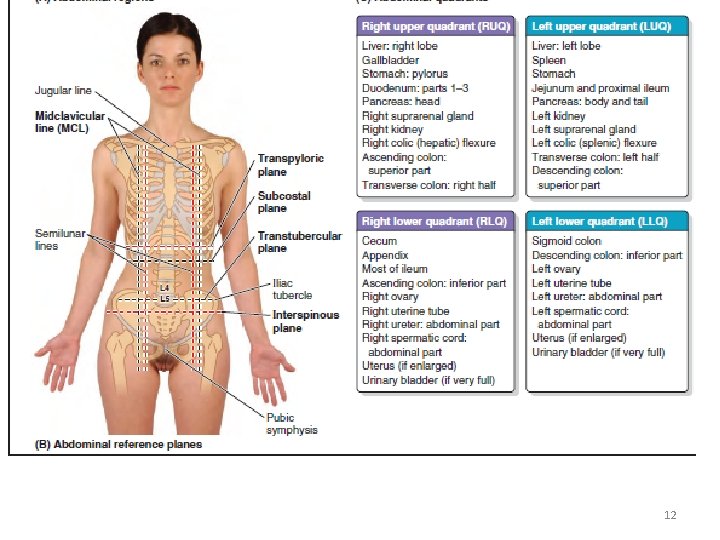
9 Regions • Four planes: two sagittal and two transverse planes. • Two sagittal planes are the midclavicular planes that pass from the midpoint of the clavicles to the midinguinal points, midpoints of the lines joining the anterior superior iliac spine (ASIS) and the pubic tubercles on each side. • Two transverse planes are the subcostal plane, passing through the inferior border of the 10 th costal cartilage on each side, and the transtubercular plane, passing through the iliac tubercles and the body of the L 5 vertebra. • Transpyloric plane, extrapolated midway between the superior borders of the manubrium of the sternum and the pubic symphysis (L 1 vertebral level), transects the pylorus, fundus of the gallbladder, neck of the pancreas, origins of the superior mesenteric artery (SMA) and hepatic portal vein, root of the transverse mesocolon, duodenojejunal junction, and hila of the kidneys • Interspinous plane passes through the ASIS on each side. 8

Four quadrants of the abdominal cavity defined by two readily defined planes: • Transumbilical plane, passing through the umbilicus (and the intervertebral [IV] disc between the L 3 and L 4 vertebrae), dividing it into upper and lower halves • Median plane, passing longitudinally through the body, dividing it into right and left halves. 9

• Abdominal wall is subdivided into the anterior wall, right and left lateral walls, and posterior wall • Boundary between the anterior and lateral walls is indefinite, therefore the term anterolateral abdominal wall. - Bounded superiorly by the cartilages of the 7 th– 10 th ribs and the xiphoid process of the sternum - Bounded inferiorly by the inguinal ligament and the superior margins of the anterolateral aspects of the pelvic girdle (iliac crests, pubic crests, and pubic symphysis). - Consists of skin and subcutaneous tissue composed of fat, muscles and their aponeuroses and deep fascia, extraperitoneal fat, and parietal peritoneum. - Three musculotendinous layers; the fiber bundles of each layer run in different directions. 10
11
12
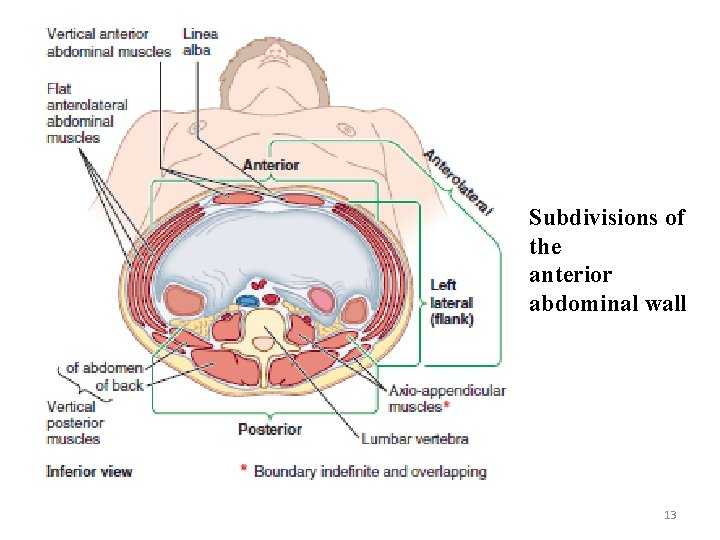
Subdivisions of the anterior abdominal wall 13

Superficial Fascia of the Anterolateral Abdominal Wall • Major site of fat storage, fat forms sagging folds (panniculi). • 2 layers inferior to the umbilicus: - Superficial fatty layer (Camper fascia) - Deep membranous layer (Scarpa fascia). • Membranous layer continues into the perineal region as the superficial perineal fascia (Colles fascia) • Investing fascia cover the external aspects of the three muscle layers • Internal aspect of AAW constitute endoabdominal fascia. • Transversalis fascia lines transversus abdominis muscle and its aponeurosis • Parietal peritoneum formed by a single layer of epithelial 14 cells and supporting connective tissue.

Muscles of Anterolateral Abdominal Wall • Five (bilaterally paired) muscles in the AAW: three flat muscles and two vertical muscles. • Flat muscles are the external oblique, internal oblique, and transversus abdominis. • Fibers of the outer two layers runs diagonally and perpendicular to each other, and the fibers of the deep layer runs transversely. • Between the midclavicular line (MCL) and the midline, the aponeuroses form the rectus sheath enclosing the rectus abdominis muscle. • Aponeuroses interweave with their fellows of the opposite side, forming midline raphe - the linea alba extends from the xiphoid process to the pubic symphysis. • Contained within the rectus sheath, are rectus abdominis and the pyramidalis. 15

EXTERNAL OBLIQUE MUSCLE • Largest and most superficial of the three flat AAW muscles. • Fibers run inferomedially, approaching a horizontal course. • Muscle fibers become aponeurotic at the MCL medially and at the spino-umbilical line inferiorly decussating at the linea alba • Contralateral external and internal oblique muscles form a “digastric muscle” • Inferiorly, it attaches to the pubic crest medial to the pubic tubercle. • Inferior margin is thickened and spans between the ASIS and the pubic tubercle as the inguinal ligament (Poupart ligament). 16

Internal oblique • A thin muscular sheet that fans out anteromedially. • Fibers run perpendicular to those of the external oblique, running superomedially • Fibers also become aponeurotic at the MCL and participate in the formation of the rectus sheath. 17

TRANSVERSUS ABDOMINIS MUSCLE • Innermost of the three flat abdominal muscles • Runs more or less transversally • Fibers end in an aponeurosis, which contributes to the formation of the rectus sheath. • Between the internal oblique and the transversus abdominis muscles is a neurovascular plane • Neurovascular plane contains the nerves and arteries supplying the AAW. 18

RECTUS ABDOMINIS MUSCLE • A long, broad, strap-like muscle • principal vertical muscle of the anterior abdominal wall • Paired rectus muscles, separated by the linea alba, lie close together inferiorly. • Three times as wide superiorly as inferiorly; it is broad and thin superiorly and narrow and thick inferiorly. • Most of the rectus abdominis is enclosed in the rectus sheath. 19

PYRAMIDALIS • Small, triangular muscle that is absent in approximately 20% of people. • Lies anterior to the inferior part of the rectus abdominis and attaches to the anterior surface of the pubis and the anterior pubic ligament. • Ends in the linea alba • Tenses the linea alba. When present, surgeons use the attachment of the pyramidalis to the linea alba as a landmark for median abdominal incision. 20

RECTUS SHEATH, LINEA ALBA, AND UMBILICAL RING • Rectus sheath is the strong, fibrous compartment of the rectus abdominis and pyramidalis muscles. • Found in the rectus sheath are the superior and inferior epigastric arteries and veins, lymphatic vessels, and distal portions of the thoraco-abdominal nerves (abdominal portions of the anterior rami of spinal nerves T 7–T 12). • Formed by the decussation and interweaving of the aponeuroses of the flat abdominal muscles. • External oblique aponeurosis contributes to the anterior wall. • Arcuate line demarcates the transition between the posterior wall of the sheath covering the superior three quarters of the rectus and the transversalis fascia covering 21 the inferior quarter.

FUNCTIONS OF ANTEROLATERAL ABDOMINAL MUSCLES • Support for the anterolateral abdominal wall. • Support the abdominal viscera and protect them from most injuries. • Compress the abdominal contents to maintain or increase the intra-abdominal pressure • Move the trunk and help to maintain posture. • Muscles form a muscular girdle that exerts pressure on the abdominal viscera. • Movements of the trunk at the lumbar vertebrae. 22
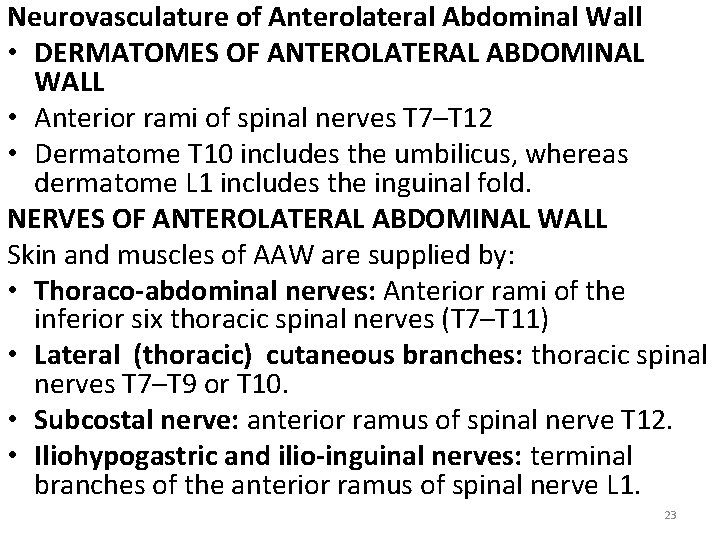
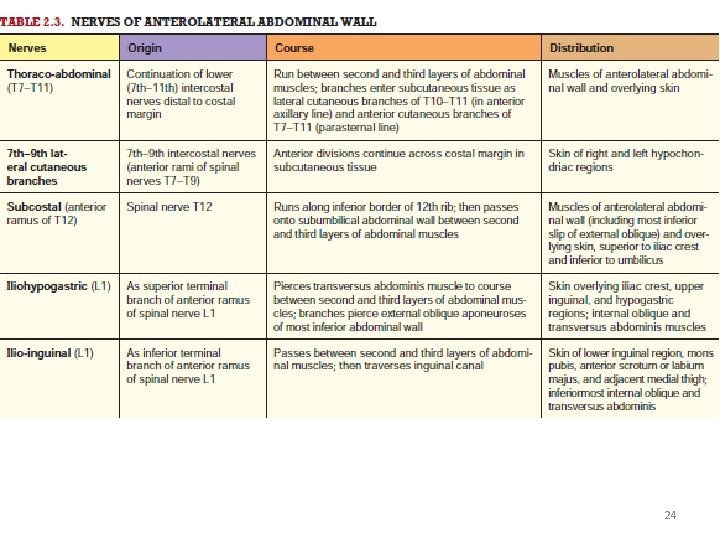
Neurovasculature of Anterolateral Abdominal Wall • DERMATOMES OF ANTEROLATERAL ABDOMINAL WALL • Anterior rami of spinal nerves T 7–T 12 • Dermatome T 10 includes the umbilicus, whereas dermatome L 1 includes the inguinal fold. NERVES OF ANTEROLATERAL ABDOMINAL WALL Skin and muscles of AAW are supplied by: • Thoraco-abdominal nerves: Anterior rami of the inferior six thoracic spinal nerves (T 7–T 11) • Lateral (thoracic) cutaneous branches: thoracic spinal nerves T 7–T 9 or T 10. • Subcostal nerve: anterior ramus of spinal nerve T 12. • Iliohypogastric and ilio-inguinal nerves: terminal branches of the anterior ramus of spinal nerve L 1. 23
24

• T 7–T 9 supply the skin superior to the umbilicus. • T 10 supplies the skin around the umbilicus. • T 11, plus the cutaneous branches of the subcostal (T 12), iliohypogastric, and ilio-inguinal (L 1), supply the skin inferior to the umbilicus. • Thoraco-abdominal, subcostal, and iliohypogastric nerves communicate with each other. 25

VESSELS OF ANTEROLATERAL ABDOMINAL WALL • Drains superiorly to the internal thoracic vein medially and the lateral thoracic vein laterally and inferiorly to the superficial and inferior epigastric veins, tributaries of the femoral and external iliac veins. • Cutaneous veins surrounding the umbilicus anastomose with para-umbilical veins and tributaries of the hepatic portal vein. • Thoraco -epigastric vein between the superficial epigastric vein (a femoral vein tributary) and the lateral thoracic vein (an axillary vein tributary). • Anastomosis between the inferior epigastric vein (from external iliac vein) and the superior epigastric/internal thoracic veins (subclavian vein tributaries) afford collateral 26 circulation during blockage of either vena cava.

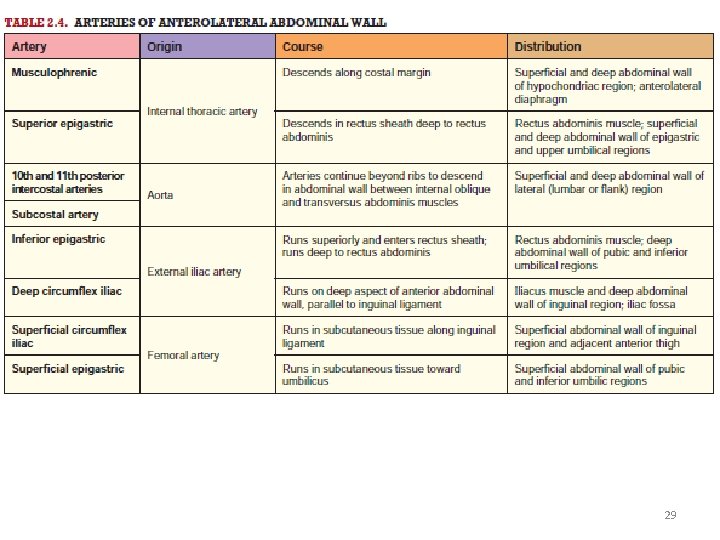
• Blood vessels of the AAW are the superior epigastric vessels and branches of the musculophrenic vessels from the internal thoracic vessels. • Inferior epigastric and deep circumflex iliac vessels from the external iliac vessels. • Superficial circumflex iliac and superficial epigastric vessels from the femoral artery and greater saphenous vein, respectively. • Posterior intercostal vessels of the 11 th intercostal space and the anterior branches of subcostal vessels. • Superior epigastric artery is the continuation of the internal thoracic artery and anastomoses with the inferior epigastric artery approximately in the umbilical region. • Inferior epigastric artery arises from the external iliac artery just superior to the inguinal ligament and anastomoses with the superior epigastric artery. 27

Lymphatic drainage • Superficial lymphatic vessels accompany the subcutaneous veins - Those superior to the transumbilical plane drain to the axillary lymph nodes - A few drain to the parasternal lymph nodes. - Superficial lymphatic vessels inferior to the transumbilical plane drain to the superficial inguinal lymph nodes. • Deep lymphatic vessels accompany the deep veins of the abdominal wall - Drain to the external iliac, common iliac, and right and left lumbar (caval and aortic) lymph nodes. 28
29

Abdominal Hernias • AAW may be the site of abdominal hernias Umbilical hernias • Common in neonates because the anterior abdominal wall is weak in the umbilical ring. • Small • Result from increased intra-abdominal pressure in the presence of weakness and incomplete closure of the anterior abdominal wall after ligation of the umbilical cord at birth. Acquired umbilical hernias • Occur most commonly in women and obese people. • Extraperitoneal fat and/or peritoneum protrude into the hernial sac. 30

Injury to Nerves of Anterolateral Abdominal Wall • Inferior thoracic spinal nerves (T 7–T 12) and the iliohypogastric and ilio-inguinal nerves (L 1) • Susceptible to injury in surgical incisions or from trauma at any level of the abdominal wall. • Injury to nerves of the anterolateral abdominal wall may result in weakening of the muscles predisposing to development of an inguinal hernia. 31

Abdominal Surgical Incisions • Allows access to the abdominal cavity. • Follow the cleavage lines (Langer lines) in the skin. • Allows adequate exposure, and the best possible cosmetic effect, is chosen. • Surgeon avoids injury to motor nerves, maintenance of blood supply, and minimizes injury to muscles and fascia of the abdominal wall while aiming for favorable healing. • Surgeon considers the direction of the muscle fibers and the location of the aponeuroses and nerves. • Muscles and viscera are retracted toward, not away from, their neurovascular supply. • Cutting a motor nerve paralyzes the muscle fibers supplied by it, thereby weakening the anterolateral abdominal wall. 32

LONGITUDINAL INCISIONS • Median and paramedian incisions offer good exposure and access to the viscera • Median incisions can be made along any part or the length of the linea alba from the xiphoid process to pubic symphysis. • Linea alba transmits only small vessels and nerves to the skin, a midline incision is relatively bloodless, and avoids major nerves. • Paramedian incisions (lateral to the median plane) are made in a sagittal plane and may extend from the costal margin to the pubic hairline. 33

OBLIQUE AND TRANSVERSE INCISIONS • Direction of oblique and transverse incisions is related to muscle fiber orientation and minimizes nerve damage. • Gridiron (muscle-splitting) incisions are often used for an appendectomy. • Oblique Mc. Burney incision is made at the Mc. Burney point, approximately 2. 5 cm superomedial to the ASIS on the spino-umbilical line. • Muscles are incised in the direction of their fibers and retracted; iliohypogastric nerve, running deep to the internal oblique, is identified and preserved. 34

• Suprapubic (Pfannenstiel) incisions (“bikini” incisions) are made at the pubic hairline. These incisions—horizontal with a slight convexity—are used for most gynecological and obstetrical operations (e. g. , for cesarean section). - The iliohypogastric and ilio-inguinal nerves are identified and preserved. 35

• Transverse incisions through the anterior layer of the rectus sheath and rectus abdominis provide good access and cause the least possible damage to the nerve supply of the rectus abdominis. • Subcostal incisions provide access to the gallbladder and biliary ducts on the right side and the spleen on the left. The incision is made parallel but at least 2. 5 cm inferior to the costal margin to avoid the 7 th and 8 th thoracic spinal nerves. 36

HIGH-RISK INCISIONS • Pararectus incisions along the lateral border of the rectus sheath are undesirable because they may cut the nerve supply to the rectus abdominis. • Inguinal incisions for repairing hernias may injure the ilio-inguinal nerve. INCISIONAL HERNIA • A protrusion of omentum or an organ through a surgical incision. • If the muscular and aponeurotic layers of the abdomen do not heal properly, an incisional hernia can result. 37
- Slides: 37