ABALLA 1 embryonic phase n The embryonic phase

ABALLA 1

embryonic phase n The embryonic phase of development is complete by the end of the 10 th G. wk ABALLA 2

n Although a variety of terms are used to describe early pregnancy failure, in the presence of clear-cut sonographic evidence that a nonliving embryo is present, the term embryonic demise should apply ABALLA 3

Early pregnancy loss Only about 1/2 of zygotes persist as a clinical (symptomatic or noticeable) pregnancy. ABALLA 4

Anatomic Points n True gestational sacs implant into the endometrial lining, and are seen eccentric to the endometrial canal. Fluid collections within the canal are not true gestational sacs. ABALLA 5

Anatomic Points n The Gestational sac and yolk sac are seen beginning at 4. 5 -5 weeks, before a recognizable embryo is seen ABALLA 6

Anatomic Points n As the gestation enlarges into the endometrial cavity, only the early placenta need be in tight contact with the decidua. Small amounts of bleeding into the cavity are commonly seen, and may surround much of the gestational sac, but if the decidua basalis remains intact, the gestation can and usually does continue to develop normally. ABALLA 7

causes n Some causes of first trimester demise are well understood; however, in most instances, the etiology is unknown (Moore, 1998 ) ABALLA 8

causes n Chromosome abnormalities are the leading known cause of pregnancy loss. An estimated 6 -7% of zygotes have chromosome aberrations (Moore, 1998), n and more than 95% of chromosomally abnormal concepti die in utero ABALLA 9

causes n n cytogenic abnormalities in 20% in women who undergo in vitro fertilization (Bateman, 1992) and in 70% of women with spontaneous abortion (Ohno, 1991). many chromosome aberrations increase with advancing maternal age (Hook, 1981). This is particularly true for Down syndrome (trisomy 21) but is also evident with other less common trisomies ABALLA 10

environmental causes immunologic factors, n drugs, n infectious agents, n alcohol, n smoking, n environmental chemicals, n radiation n ABALLA 11

environmental causes Exposure before 5 weeks gestational age (GA), has an all-or-none result such that the embryo will either die or be unaffected (Moore, 1998). n (5 -10 wk) usually affects organ development and results in either demise or severe congenital abnormalities. n ABALLA 12

Luteal phase defect Once implantation has occurred, another cause of early pregnancy failure relates to an inability of the corpus luteum to adequately support the conceptus (Blumenfeld, 1992). n This condition, which tends to occur with maternal obesity and/or advancing maternal age, can be treated successfully during the embryonic phase of development by administrating human choriogonadotropin (h. CG). and /or progestrone. n ABALLA 13

Uterine causes n A developmental uterine anomaly such as a uterine septum or acquired uterine anomalies such as submucosal, large, or degenerating leiomyomas also can increase the incidence of embryonic demise ABALLA 14

Clinical Details ABALLA 15
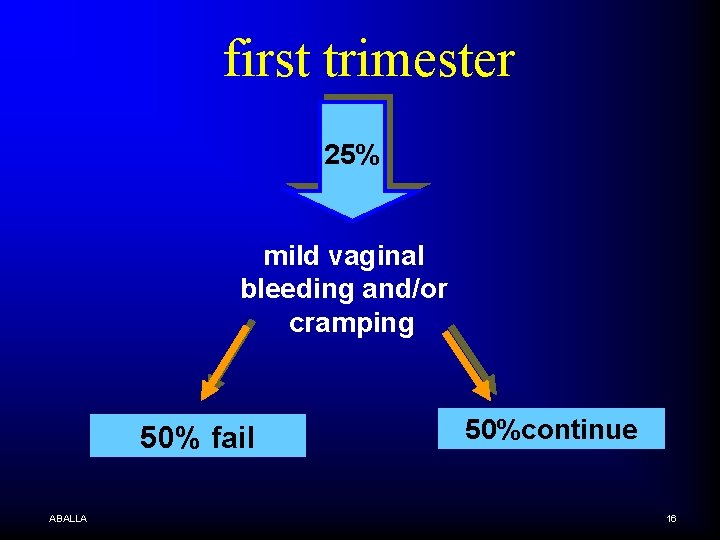
first trimester 25% mild vaginal bleeding and/or cramping 50% fail ABALLA 50%continue 16

Clinical Details n Some women with embryonic demise will be asymptomatic, and in these patients the diagnosis may be suggested based on subnormal uterine growth, ABALLA 17
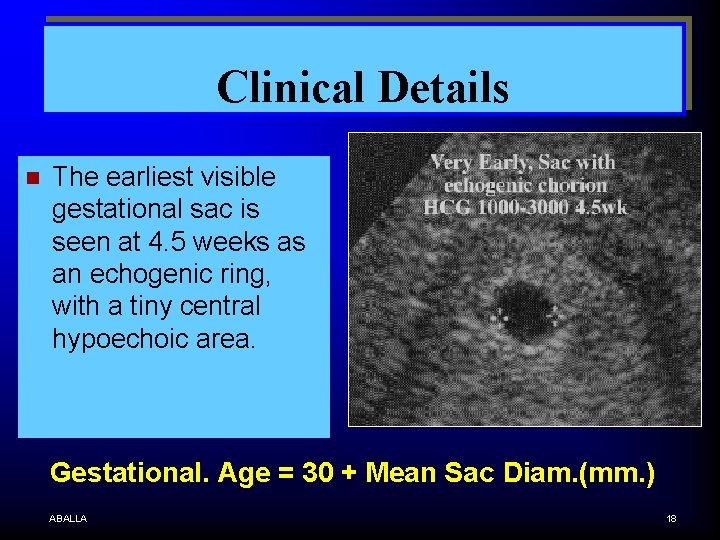
Clinical Details n The earliest visible gestational sac is seen at 4. 5 weeks as an echogenic ring, with a tiny central hypoechoic area. Gestational. Age = 30 + Mean Sac Diam. (mm. ) ABALLA 18

Clinical Details n To confidently diagnose an IUP, most sonographers rely on the double decidual sac (DDS) finding, which is not universally present until the MSD is 10 mm (40 days GA) (Nyberg, 1983). ABALLA 19
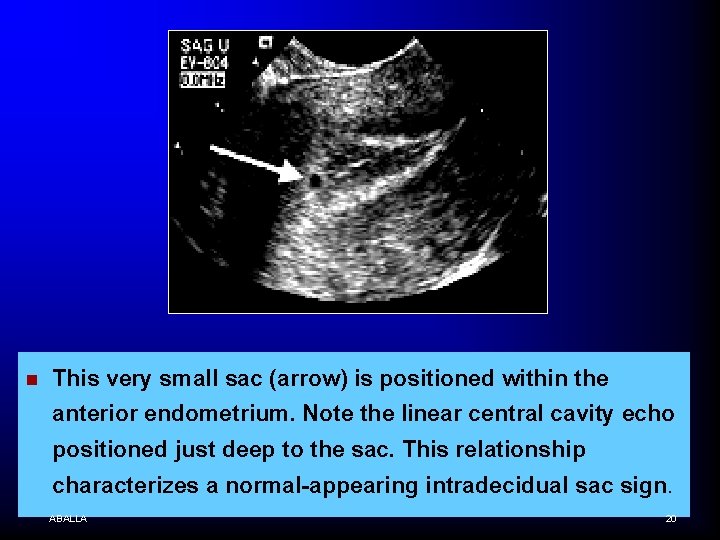
n This very small sac (arrow) is positioned within the anterior endometrium. Note the linear central cavity echo positioned just deep to the sac. This relationship characterizes a normal-appearing intradecidual sac sign. ABALLA 20

Clinical Details when using a transabdominal approach, cardiac activity should be visible by 8 weeks GA. , 9 mm should be considered the discriminatory embryonic length for detecting cardiac motion n with a transvaginal approach. can detect cardiac activity approximately 2 weeks earlier or by 6 weeks GA. 5 mm be considered the discriminatory embryonic length for detecting cardiac motion n ABALLA 21

the discriminatory value Cardiac activity n TAUS: 8 WK, 9 mm, CR 25 MSD ABALLA Cardiac activity n TVUS: 6 WK 5 mm, CR 18 MSD 22

Clinical Details n A limitation of the transvaginal approach is if a large pelvic mass is present. Most often, large or strategically placed calcified uterine fibroids cause this problem. Under these circumstances, an abdominal approach should be used in an effort to image the uterus and its contents. ABALLA 23
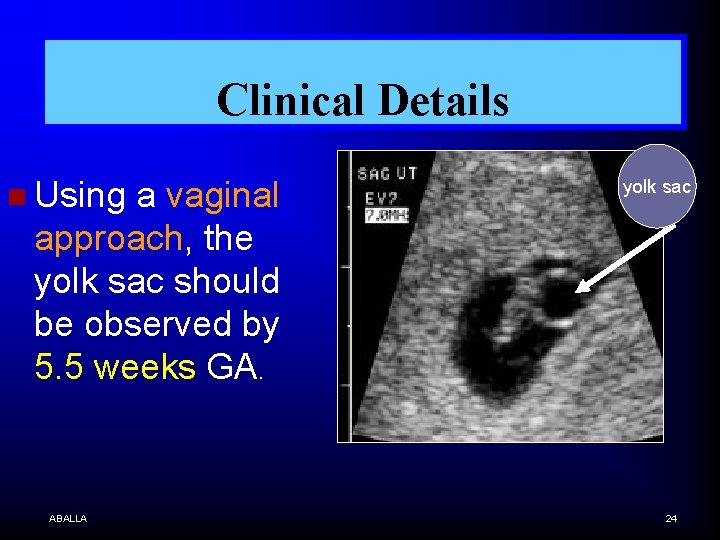
Clinical Details n Using a vaginal approach, the yolk sac should be observed by 5. 5 weeks GA. ABALLA yolk sac 24

Clinical Details n Yolk sac should be seen when sac is 10 mm. MSD by vaginal probe, or 20 mm. MSD by abdominal probe. ABALLA 25

NORMAL YOLK SAC TAUS TVUS (MSD) is 20 mm MSD is 10 mm 7 weeks 5. 5 weeks Yolk sac must be visible ABALLA 26
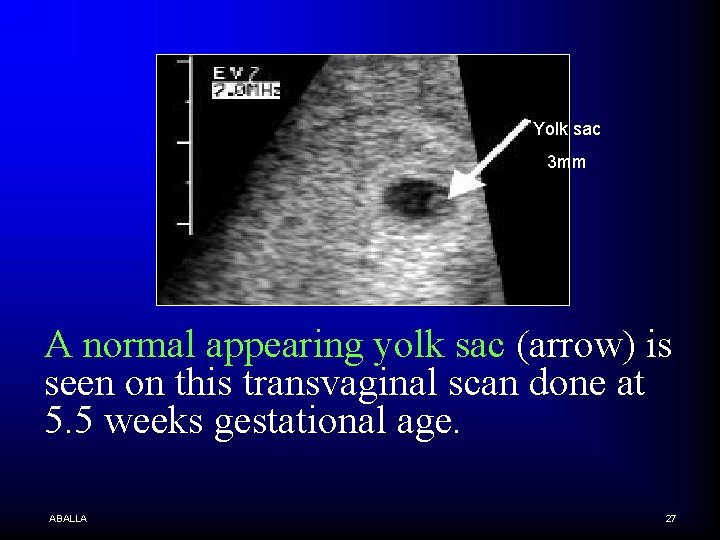
Yolk sac 3 mm A normal appearing yolk sac (arrow) is seen on this transvaginal scan done at 5. 5 weeks gestational age. ABALLA 27
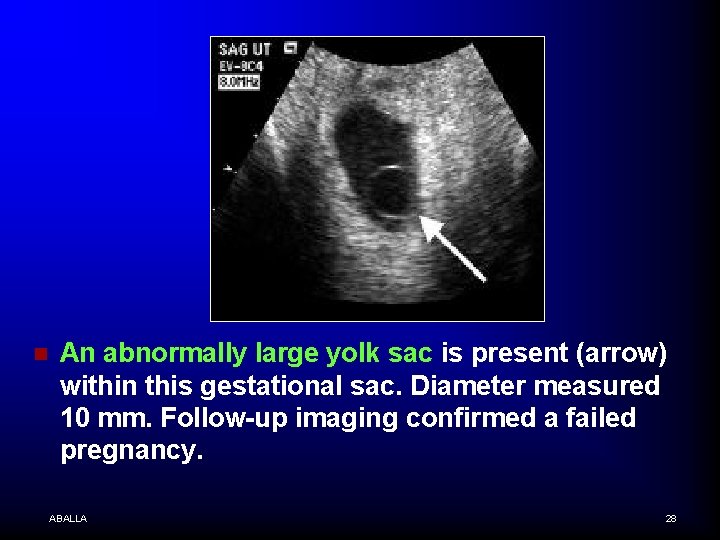
n An abnormally large yolk sac is present (arrow) within this gestational sac. Diameter measured 10 mm. Follow-up imaging confirmed a failed pregnancy. ABALLA 28

If no yolk sac n n If a small saclike structure is imaged but it does not contain a yolk sac, it is often not possible to determine if the intrauterine finding is the result of an early IUP or a pseudosac associated with an ectopic pregnancy. In these instances, careful evaluation of the adnexa may be helpful to detect an ectopic pregnancy. Occasionally, serial ultrasound and/or h. CG determinations may be required to determine the etiology for the intrauterine sac ABALLA 29

Visualizing a dead embryo ABALLA 30

Visualizing a dead embryo n using a transabdominal approach, 9 mm should be considered the discriminatory embryonic length for detecting cardiac motion. Used in this manner, ( the discriminatory level denotes the numeric value when a certain finding should always be present. ) ABALLA 31

Visualizing a dead embryo n when a transvaginal approach was used, 5 mm be considered the discriminatory embryonic length for detecting cardiac motion. ABALLA 32

the discriminatory value Cardiac activity n TAUS: 8 WK, 9 mm, CR 25 MSD ABALLA Cardiac activity n TVUS: 6 WK 5 mm, CR 18 MSD 33

Visualizing a dead embryo an embryo exceeds the discriminatory length and cardiac activity is absent, a nonviable gestation should be diagnosed. , n this observation should be made by two independent observers, and interpretive caution must be exercised in any questionable case. Documentation should be available by M mode imaging and/or by obtaining a videotape or video clip. n ABALLA 34
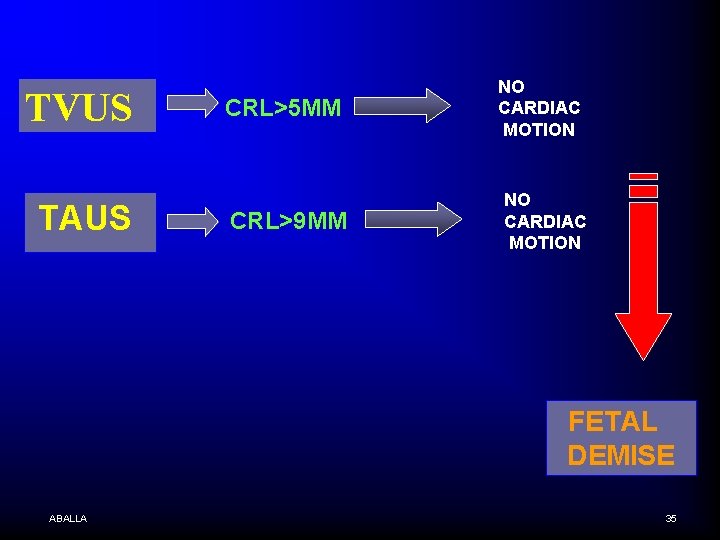
TVUS TAUS CRL>5 MM CRL>9 MM NO CARDIAC MOTION FETAL DEMISE ABALLA 35

Visualizing a dead embryo If the length of the embryo is less than the discriminatory value, the patient should be managed expectantly, n a repeat ultrasound examination should be performed when the expected embryonic CRL exceeds the discriminatory value. Alternatively, or additionally, the level of serum h. CG may be useful for determining whether a normal IUP is present. n ABALLA 36

Visualizing a living embryo Although seemingly a paradox, it is well known that detecting cardiac activity when using a vaginal transducer does not guarantee as favorable an outcome as detecting cardiac activity when using an abdominal transducer n the vaginal approach detects cardiac activity earlier when the incidence of pregnancy loss is relatively higher. n ABALLA 37

Predicting a poor outcome ABALLA 38

Predicting a poor outcome n a number of other important observations have been made, which, when observed with a living embryo, are predictive of a poor outcome (Falco 1996). ABALLA 39

Predicting a poor outcome mean embryonic heart rate (MEHR) mean gestational sac size (MSS) Abnormal yolk sac/amnion Subchorionic hemorrhage Abnormal sac criteria ABALLA Doppler findings 40

Predicting a poor outcome (MEHR) n At 5 -6 weeks GA, the mean embryonic heart rate is 101 beats per minute (bpm). n This rate increases to 143 bpm by 8 -9 weeks GA ABALLA 41

Predicting a poor outcome (MEHR) n it is not unusual for an initially detected embryonic heart rate to be somewhat slower than the fetal heart rate recorded later in pregnancy. An unusually slow heart rate is cause for concern. In one study, all embryos from 5+ to 8+ weeks GA in which the heart rate was less than 85 bpm resulted in spontaneous miscarriage (Benson, 1994 ABALLA 42
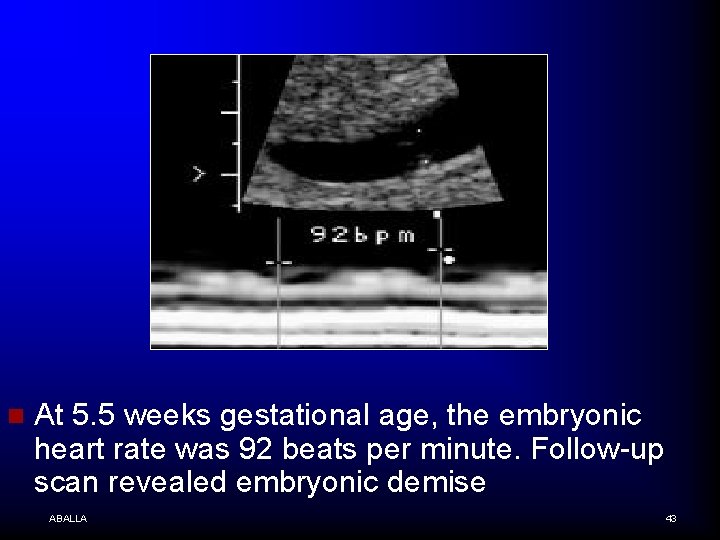
n At 5. 5 weeks gestational age, the embryonic heart rate was 92 beats per minute. Follow-up scan revealed embryonic demise ABALLA 43

Predicting a poor outcome (MSS) n Small sac size: From 5. 5 -9 weeks GA, the mean gestational sac size (MSS) is normally at least 5 mm greater than the CRL ABALLA 44

Predicting a poor outcome (MSS) n. When this difference is less than 5 mm, the subsequent spontaneous abortion rate exceeds 90% (Bromley, 1991) ABALLA 45
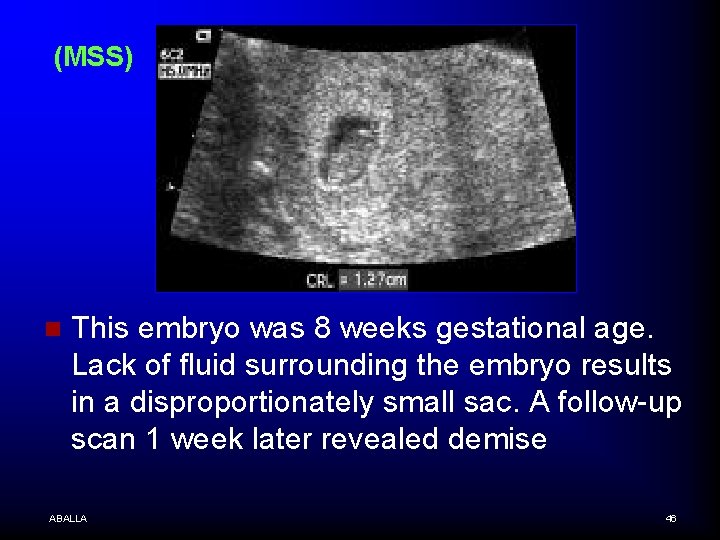
(MSS) n This embryo was 8 weeks gestational age. Lack of fluid surrounding the embryo results in a disproportionately small sac. A follow-up scan 1 week later revealed demise ABALLA 46

Predicting a poor outcome Subchorionic hemorrhage n Subchorionic hemorrhage: As many as 18% of women with vaginal bleeding during the first half of pregnancy have sonographic evidence for a Subchorionic hemorrhage as the etiology for their bleeding (Pederson, 1990). ABALLA 47

Early pregnancy bleeding 18% Subchorionic hemorrhage ABALLA 48

Predicting a poor outcome Subchorionic hemorrhage n Several authorities have suggested that the size of the blood clot can be used to predict the outcome (Abu-Yousef 1987); this has not been universally accepted (Dickey, 1992). ABALLA 49
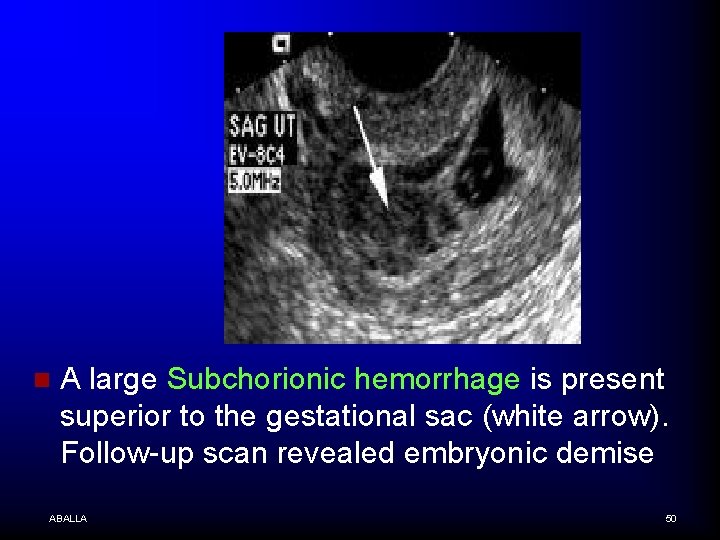
n A large Subchorionic hemorrhage is present superior to the gestational sac (white arrow). Follow-up scan revealed embryonic demise ABALLA 50

Predicting a poor outcome Subchorionic hemorrhage Hemorrhage volume (Estimated from formula Length (cm) X Height (cm) X Depth (cm) X 0. 52 = Volume ml), less then 75 -200 ml. is often associated with continued development ABALLA 51

Abnormal yolk sac/amnion ABALLA 52

NORMAL YOLK SAC TAUS TVUS (MSD) is 20 mm MSD is 8 mm GA of 7 weeks GA of 5. 5 weeks Yolk sac must be visible ABALLA 53

Abnormal yolk sac/amnion n The amnion develops somewhat earlier than the yolk sac, but because this membrane is so thin, it is more difficult to visualize than the yolk sac. Normally, the amnion is visible on transabdominal scans late in the embryonic period. If the amnion is easily seen, it is probably too thick and most likely is abnormal ABALLA 54

Abnormal yolk sac/amnion n Other features consistent with pregnancy failure include a visible amnion without a simultaneously visible yolk sac, embryo, or cardiac activity. An enlarged amniotic sac is another sonographic sign that predicts a failed pregnancy or embryonic death (Horrow, 1992). ABALLA 55
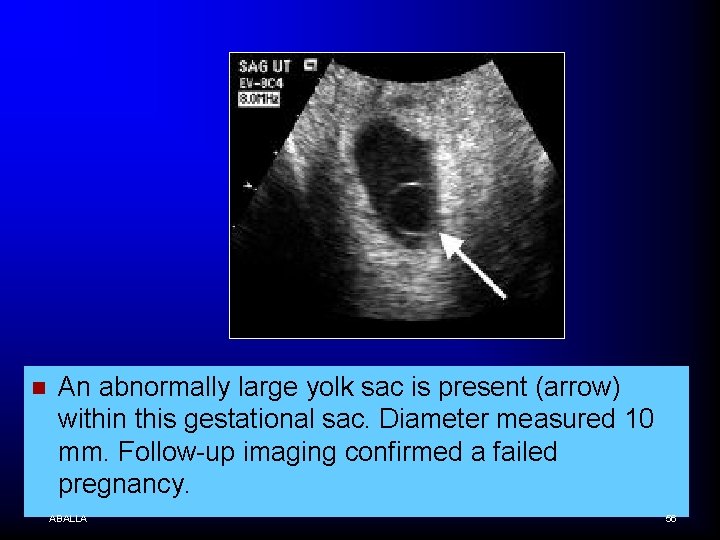
n An abnormally large yolk sac is present (arrow) within this gestational sac. Diameter measured 10 mm. Follow-up imaging confirmed a failed pregnancy. ABALLA 56

Doppler findings n conflicting reports exist with regard to the usefulness of first trimester Doppler for predicting pregnancy outcome. Some reports suggest if the resistive index is measured at the Subchorionic level and exceeds. 55, a high likelihood of spontaneous abortion exists (Jaffe, 1995); however, others claim that Doppler analysis of these vessels are not predictive of outcome (Frates 1996). ABALLA 57

Abnormal sac criteria ABALLA 58

Abnormal sac criteria n An early normal intrauterine gestational sac often can be identified transabdominally by 31 days GA and can consistently be identified by 35 days GA. To confidently diagnose an IUP, most sonographers rely on the double decidual sac (DDS) finding, which is not universally present until the MSD is 10 mm (40 days GA) (Nyberg, 1983). ABALLA 59

Abnormal sac criteria By transabdominal approach, size criteria that unequivocally suggest an abnormal sac include n failure to detect a DDS when the MSD is equal to or greater than 10 mm, n failure to detect a yolk sac when the MSD is equal to or greater than 20 mm, n failure to detect an embryo when the MSD is equal to or greater than 25 mm (Nyberg, 1986). ABALLA 60

Abnormal sac criteria Using vaginal ultrasound, a normal intrauterine gestational sac can be detected reliably at 4 -5 weeks GA, at which time the MSD approaches 5 mm. Using vaginal transducers, criteria that suggest an abnormal sac include n failure to detect a yolk sac when the MSD is 8 mm or greater, and n failure to detect cardiac activity when the MSD exceeds 16 mm (Levi, 1988) ABALLA 61

Visualizing an "empty " gestational sac n The earliest appearance for a normal sac is a small fluid collection surrounded by highamplitude echoes embedded in the decidualized endometrium. This appearance has been termed the “intradecidual sac sign” (IDSS)). ABALLA 62

Visualizing an "empty " gestational sac An "empty " gestational sac is the result of 1 of 3 entities: n 1) a normal early IUP, n 2) an abnormal IUP, or n 3) a pseudogestational sac in a patient with an ectopic pregnancy. ABALLA 63
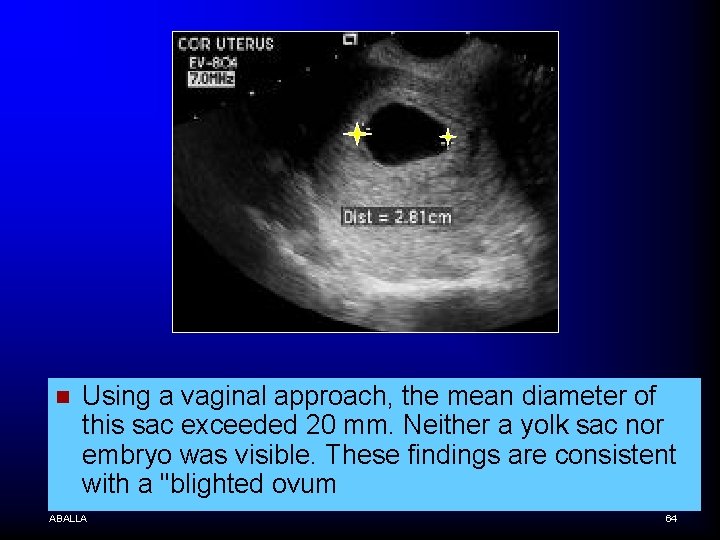
n Using a vaginal approach, the mean diameter of this sac exceeded 20 mm. Neither a yolk sac nor embryo was visible. These findings are consistent with a "blighted ovum ABALLA 64
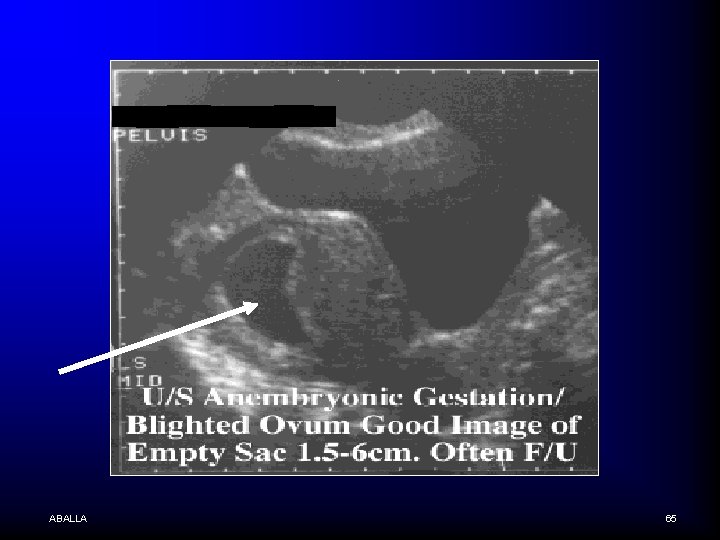
ABALLA 65
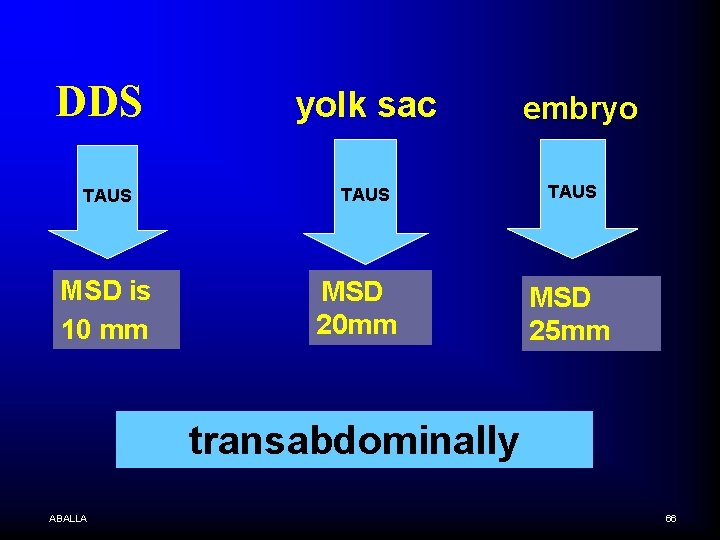
DDS TAUS MSD is 10 mm yolk sac TAUS MSD 20 mm embryo TAUS MSD 25 mm transabdominally ABALLA 66
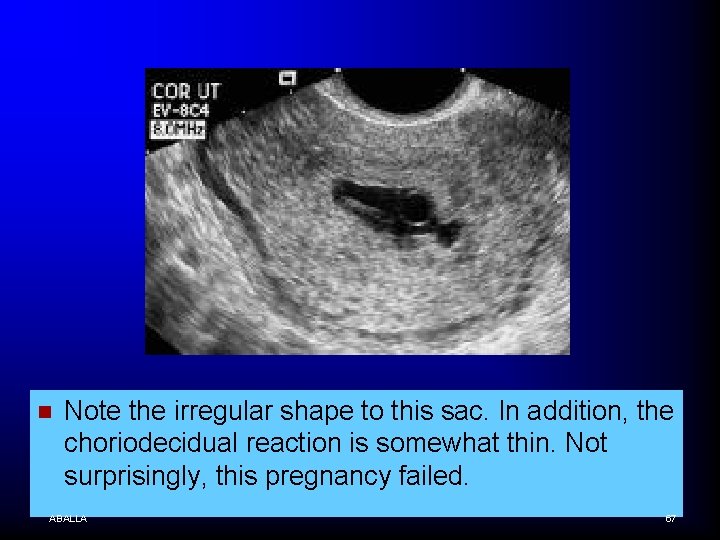
n Note the irregular shape to this sac. In addition, the choriodecidual reaction is somewhat thin. Not surprisingly, this pregnancy failed. ABALLA 67

Growth rate In normal gestation, mean sac growth is 1. 13 mm/day; in comparison, mean sac growth in an abnormal intrauterine gestation is 0. 70 mm/day (Nyberg, 1987). n Based on these observations, abnormal sac growth can be diagnosed confidently if the gestational sac fails to grow by at least 0. 6 mm/day. n ABALLA 68

Choriodecidual appearance This refers to the sonographic appearance of the echoes that surround an early intrauterine gestational sac. An abnormal appearance includes a distorted sac shape; n a thin (<2 mm), weakly echogenic, irregular choriodecidual reaction; n absence of the double decidual sac sign when the MSD exceeds 10 mm ABALLA 69

The Living Embryo and threatened abortion ABALLA 70

The Living Embryo and threatened abortion n The presence of an embryonic heartbeat is highly reassuring. When visualized by Low Resolution Abdominal sonography, more than 90% of pregnancies continue n Visualization by high resolution vaginal sonography is associated with a 70% continuance rate. ABALLA 71
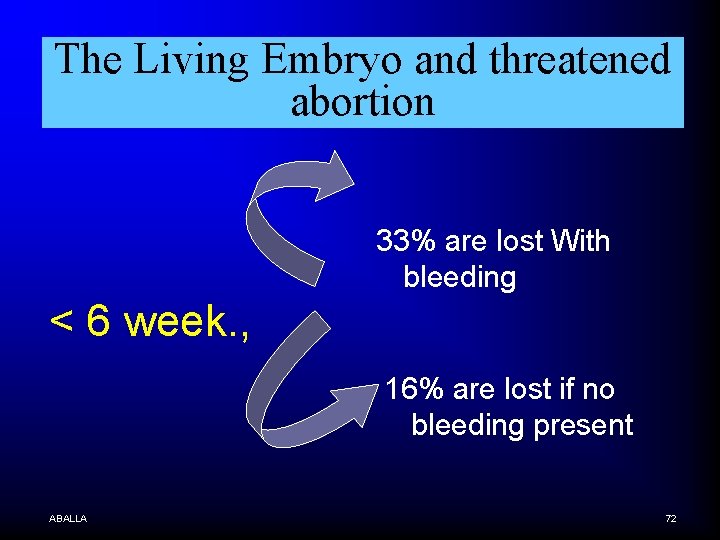
The Living Embryo and threatened abortion 33% are lost With bleeding < 6 week. , 16% are lost if no bleeding present ABALLA 72
The Living Embryo and threatened abortion 10% are lost With bleeding 7 -9 week 5 % are lost if no bleeding present ABALLA 73
The Living Embryo and threatened 4 % are lost With abortion bleeding 9 -11 week 2% are lost if no bleeding present ABALLA 74

conclusion The prognosis for the living embryo improves as gestation proceeds ABALLA 75
Visualizing a central cavity complex When the central cavity complex is abnormally thickened (and often irregularly echogenic), the differential diagnosis includes: n intrauterine blood, retained products following an spontaneous abortion, n decidual changes secondary to an early but not yet visible intrauterine pregnancy, n or a decidual reaction from an ectopic pregnancy. ABALLA 76

Degree of Confidence If certain findings are not observed at the appropriate time, if the ultrasound findings are equivocal, if the examination is technically difficult, or if the sonographer is inexperienced, caution is warranted. n The embryo always should be given the benefit of the doubt, and a follow-up ultrasound examination should be performed to obviate any risk of terminating a normal intrauterine pregnancy. n ABALLA 77

False Positives/Negatives n Prior to visualizing the yolk sac, it is often not possible to be certain if a small intrauterine saclike structure is due to an early intrauterine pregnancy (normal or abnormal), or a pseudosac associated with an ectopic pregnancy. This is because it may not be possible to clearly identify the DSS. Under these circumstances, a follow-up examination should be performed if clinically feasible. ABALLA 78

False Positives/Negatives n Occasionally, a subchorionic hemorrhage may resemble a second intrauterine sac. However, since most of these women are bleeding, with careful scanning, the correct diagnosis usually can be made. Whenever uncertainty exists, perform a short interval follow-up examination at 5 -7 days ABALLA 79

ABALLA 80
- Slides: 80