AAC and Autism Spectrum Disorder ASD Blair Ridgley

AAC and Autism Spectrum Disorder (ASD) Blair Ridgley Michelle Neumann Bianca Havel

Autism Spectrum Disorder (ASD) A developmental disability Children with autism, also known as autism spectrum disorder or ASD, have deficits in: Social Skills Communication Language They also have restricted and repetitive patterns of behavior, interests, or activities, such as flipping objects, echolalia, or excessive smelling or touching of objects. ASD may be mild or severe. All children with autism don't have the exact same problems.

Social Deficits in ASD Sharing a common focus with another person about the same object or event-known as joint attention Playing with others and sharing toys Empathy Difficulties in conversation: Turn-taking, Understanding social cues, Sensing the feelings or reactions of others, Interpreting another’s perspective. , Reduced sharing of interests Deficits in nonverbal communication Absence of interest in peers Difficulty adjusting behavior to suit various social contexts Difficulty with imaginative play Difficulty making inferences and nonliteral or ambiguous meaning of language making and keeping friends.

Communication Deficits in ASD Children with ASD may have trouble with communication skills like understanding, talking with others, reading or writing. Sometimes, he or she might lose words or other skills that they used before. Children may have problems: Understanding and using gestures, like pointing, waving, or showing objects to others Following directions Understanding and using words Developing language skills Communicating nonverbally Using spoken language Learning to read or write. Or she/he may read early but without understanding the meaning—called hyperlexia.

Communication Deficits in ASD Trouble understanding that words relate to objects and activities Abstract words are challenging Often self-absorbed* Unable to successfully communicate and interact with those around them

Communication Disorders Associated with ASD Not every child with ASD will have a language problem… Varies depending on intellectual and social development Some may be nonverbal Some may have rich vocabularies Most have little or no problem pronouncing words The majority has difficulty using language effectively May have problems with the meaning and rhythm of words and sentences May be unable to understand body language and vocal tones

Nonverbal Communication • • They do not learn to use facial expressions to convey a message Often have blank expressions/inappropriate expressions Do not instinctively know that a smile communicates pleasure and a frown represents displeasure or sadness – In a normally developing child, they pick up meanings of facial expression spontaneously For kids with ASD, any recognition of the meaning of nonverbal expressions must be explicitly taught

Repetitive or Restrictive Behaviors and Special Interests …As manifested by at least 2 of the following: 1. Repetitive motor movements, use of objects, or speech Hand flapping, toe walking Lining up objects Watching the same scene of a movie 2. Insist on sameness Extreme distress at small changes; Difficulty with transitions 3. Highly restricted, fixated interests Strong attachment with unusual objects 4. Hyper or hypo- reactivity to sensory input Pain/temperature Specific sounds or textures Visual fascination with lights or movements

Other Deficits in ASD Children may also: Repeat words just heard or words heard days or weeks earlier-called echolalia Talk with little expression or use a sing-song voice Use tantrums to tell you what he does or does not want. Get upset by certain sounds Like only a few foods

Diagnosis of Autism Parents typically first notice unusual behaviors Medical diagnosis made by physician, according to the DSM 5 Guides physicians according to a specific number of symptoms Failure to make eye contact, repetitive behaviors, not responding to his/her name Problems in at least one of the areas of communication, socialization, or restricted behavior must be present before the age of three Behavioral assessments conducted Some characteristic behaviors apparent in first few months or early years of the child’s life

Diagnosis (continued) 2 stages of the diagnosis: 1. A developmental screening during the child’s regular “checkups” 2. A comprehensive evaluation by a multidisciplinary team Pediatrician Psychologist Speech-language pathologist Occupational therapist

Criteria to be met for diagnosis of ASD 1. Deficits in social communication and interaction 2. Repetitive or restrictive behaviors and special interests 3. Language delays occurring in beginning stages of language development as well as in interactive conversation 4. Symptoms must be present in early childhood

Possible Causes of ASD? ASD is a lifelong problem with a number of possible genetic and/or environmental causes, including but not limited to: Genetic problems or syndromes Severe infections that affect the brain (meningitis, celiac disease, encephalitis, etc. ) Exposure to toxins or illness during pregnancy (rubella, chemicals, etc. )

How can ASD be treated? Behavior and development programs Education and learning programs Medications Other treatment and therapies

Behavior and Development Programs Applied Behavior Analysis (ABA): Focuses on the principles that explain how learning takes place When a behavior is followed by a reward, the behavior is more likely to be repeated By assessing the relationship between a targeted behavior and the environment, ABA can be used to change that behavior UCLA/Lovaas: Utilizes the principles of ABA Typical therapy session: Two or three hour sessions Short periods of structured time devoted to a task (3 -5 minutes) are followed by an equal amount of free play for the child Longer breaks at the end of every hour (10 -15 minutes) Free play and breaks are used for incidental teaching or practicing learned skills in new environments

Education and Learning Programs These programs are offered in schools or other learning centers. They focus on learning and reasoning skills and “whole life” approaches. TEACCH Autism Program (University of North Carolina) is based on understanding the “culture of autism” Framework includes: Physical organization Individualized schedules Activity systems Visual structure of materials in tasks and activities

Education and Learning Programs Social Skills Development Interventions The primary focus of Social Skills Development Programs is to help children with ASD develop improved awareness and understanding of other perspectives in order to improve conversation skills, develop relationships with peers, play cooperatively, mediate conflict, develop self regulation skills, and problem-solve. The social skills sessions are highly structured and begin with an assessment and conclude with brief progress reports. Methods such as role-playing and simulation are also used. Activity-based lessons are often incorporated in order to focus on the teachable moments when real-life dilemmas occur.

Medications Antipsychotic drugs: resperidone (Risperdal) and Aripirazole (Abilify) can help reduce emotional distress, aggression, hyperactivity, and self-injury. Ø Side effects include weight gain, sleepiness, tremors, and abnormal movements Serotonin-reuptake inhibitors (antidepressants) and hyperactivity medicines (Ritalin) have not been studied enough to know if it can help treat ASD symptoms

Other Treatment and Therapies • • Speech and Language Therapy Dietary interventions Music Therapy Occupational Therapy Acupuncture Sensory Integration Therapy AAC

Autism and Augmentative and Alternative Communication (AAC) Augmentative and alternative communication (AAC) strategies were first explored for individuals with autism spectrum disorders (ASD) in the 1980 s and early 1990 s. Since that time, developments in technology have played a crucial role in improving the quality, affordability and accessibility of AAC strategies for members of this population. As the use of AAC for persons with ASD became more widespread, it expanded beyond its traditional use for expressive communication alone, and was used to augment comprehension and to provide organization of time and sequences AAC Systems (no tech, low tech and high tech)

No Tech and Low Tech Systems No Tech – – Gestures Signs Low Tech – Visual Aids • • – Calendars Schedule Boards Reminder Strips Communication Boards PECS

High Tech AAC i. Pad Nova. Chat 5, 7, & 10 Accent 800, 1000, & 1200

Using Visual Strategies to Improve Behavior for Children with ASD It is important to recognize that students have different learning styles and that many students are VISUAL learners The issue causing the behavior problem should first be recognized then strategies can be developed to prevent or lessen the behavior. Many behavior situations and problems are related to communication; relating to understanding, expression, or other learning skills such as establishing attention and memory

Using Visual Strategies to Improve Behavior-Communication-Visual Strategies Framework Causes of behavior differences are frequently related to communication difficulties; problems in understanding and/or difficulty with expression The remedy to improving behavior is improving communication The method is using visual strategies to support communication

Using Visual Strategies to Improve Behavior Managing behavior for any student requires • insight, keen observation, patience, and lots of wisdom Communication emerges as an integral part of the problem, or it evolves as an essential part of the solution.
Visuals Schedules Reminder Strips

Visuals Calendar Emotions Self Regulation

The SCERTS Model A comprehensive, multidisciplinary approach to enhance communication and socialemotional abilities of individuals with ASD Primary Developmental Dimensions • • • Social Communication Emotional Regulation Transactional Support

The SCERTS Model Disciplines involved in team General and Special Education Speech-Language Pathologist Occupational Therapist Child Psychologist and Psychiatrist Social Worker

The SCERTS Model Social Communication • Addresses overriding goals of helping a child to be an increasingly competent, confident, and active participant in social activities. – To do so, children must acquire capacities in 2 major areas of functioning » » Joint attention Symbol use

The SCERTS Model Social Communication Joint Attention Children must learn to share attention and emotion with a partner as well as to express intentions across communicative partners Symbol Use One aspect is communication means Communication means may be presymbolic or symbolic

The SCERTS Model Social Communication Ultimate Goal: Support children in developing the foundational abilities in joint attention and symbol use that support communicative and social competence Research as well as clinical experience has demonstrated that with increased social communicative abilities, behavioral difficulties may be prevented or lessened.

The SCERTS Model – Emotional Regulation • For a child to be optimally available, he or she must have the emotional regulatory capacities and skills to: – – – Seek assistance and/or respond to other’s attempts to provide support for emotional regulation when faced with stressful, overly stimulating, or emotionally dysregulating circumstances Remain organized and well-regulated in the face of potentially stressful circumstances Recover from being “pushed over the edge” into states extreme emotional dysregulation or shutdown, through mutual- and/or self regulatory strategies

The SCERTS Model Emotional Regulation • Helping a child more effectively maintain optimal arousal, or at the very least, a well-regulated state • Frequent high states of arousal: anxiety, fear, distress, dysregulating positive emotional states of elation and giddiness – • The child may also withdraw or shutdown Low state of arousal: appear passive, disengaged, and inattentive Ultimate goal: To support a child in adapting to and coping with the inevitable and uniquely individual daily challenges that he or she will face in maintaining a well-regulated state of arousal most conducive to learning and relating to others

The SCERTS Model Transactional Supports Interpersonal Supports Learning Supports Support to Families Support among Professionals and Other Service Providers

The SCERTS Model Transactional Support Interpersonal Supports Adjustments made by communication partners in language use, emotional expression, and interactive style that are effective in helping a child with ASD process language, participate in social interaction, experience social activities as emotionally satisfying, and maintaining well-regulated states. Also includes Peer Support

The SCERTS Model Transactional Support Learning Supports Environmental arrangement, or the ways typical settings and activities are set up or modified to foster communication and emotional regulation, visual supports for social communication and emotional regulation, which may be implemented in various settings

The SCERTS Model Transactional Support to Families Mainly educational support: sharing helpful information and resources or direct instruction in facilitating a child’s social communication, emotional regulation, and daily living skills and implementations of learning supports for the child. Emotional support is used necessary

The SCERTS Model Transactional Support among Professionals and Other Service Providers Informal and planned opportunities for enhancing educational and therapeutic skills and for providing emotional support , whenever necessary, to cope with the challenges of working with children with ASD and to prevent burnout

The SCERTS Model When a child’s development in social communication and emotional regulation is supported, with strategic implementation of transactional support, there is great potential for comprehensive, long term positive effects on a child’s development in educational and everyday activities.

What is the Picture Exchange Communication System Low tech form of AAC Originally designed for young children with autism in the late 1980 s Children are taught to approach a communication partner with a picture of a desired item in exchange for that item The PECS protocol and training sequence (six phases) are based on the operants defined by Skinner’s work Verbal Behavior (1957)-mand, tact, and intraverbal Each phase targets a different communication goal

How Does PECS Work? The 6 phases of PECS: I. Teaches the child how to make a request II. Requires the child to travel to their communicative partner (communication book + increased distance between child and communicative partner) III. The child must chose between 2 items (highly desired vs. nondesired item to gradually multiple desired items) IV. Sentence structure is developed (A sentence starter “I want” + picture symbol) V. Teaches the child how to answer “What do you want? ” (verbal prompt, delay, and gestural prompt) VI. Child is taught to comment in response to their partner’s communication question (I. e. What do you see? )

Advantages of PECS • Children with relatively limited prerequisite skills (e. g. eye contact, gestures, and verbal imitation) can utilize PECS • Training for PECS is short, typically a 2 -day workshop • It is motivating for children since they are immediately rewarded • Cost

Disadvantages of PECS Restricted range of communicative functions: • Phases I-V all target requests (no protests or refusals) • Phase VI targets comments • Comments are not spontaneous since they are responses to adult prompts • • • No opportunity to indicate that an item is not wanted Preparation can be labor intensive for clinicians Vocabulary is limited

Is PECS Effective? Research has shown that PECS is a promising, but not yet established evidence-based intervention for facilitating communication in children with ASD, but not for facilitating speech. Ø Ø Ø Small to moderate effects were demonstrated for the shortterm efficacy of PECS in improving communicative outcomes for young children with ASD PECS may also decrease problems behaviors (e. g. tantrums grabbing, etc. ) in some children Evidence for maintenance and generalization of communicative gains is limited and future research is needed

Language Acquisition through Motor Planning (LAMP) LAMP was developed by utilizing motor learning principles along with the Unity language system for treatment of individuals who are nonverbal and use AAC to communicate.

Studies in AAC and Autism: The Impact of LAMP as a Therapy Intervention LAMP • • • A therapeutic approach based on neurological and motor learning principles. The goal is to give individuals who are nonverbal or have limited verbal abilities a method of independently and spontaneously expressing themselves in any setting. It focuses on giving the individual independent access to vocabulary on voice output AAC devices that use consistent motor plans for accessing vocabulary. Teaching of the vocabulary happens across environments, with multisensory input to enhance meaning. The child's interests and desires help determine the vocabulary to be taught.

Studies in AAC and Autism: The Impact of LAMP as a Therapy Intervention The LAMP approach includes 5 components Readiness to learn Shared Engagement Consistent Motor Patterns Auditory Signals Natural Consequences

Studies in AAC and Autism: The Impact of LAMP as a Therapy Intervention Methods – – – 7 children involved in study Ranged from age 3 to 7 Diagnosis of ASD or pervasive developmental disorder- not otherwise specified and complex communication needs • – – All 7 diagnosed with expressive-receptive language disorder Each obtained a speech generating device (SGD) and received LAMP intervention Each child was a patient of a private practice

Studies in AAC and Autism: The Impact of LAMP as a Therapy Intervention Methods It was clear from both baseline data and observation that each participant had complex communication needs Limited Vocalizations Low intelligibility Severely limited expressive vocabulary Difficult behaviors Inability to maintain attention to tasks

Studies in AAC and Autism: The Impact of LAMP as a Therapy Intervention Methods The SLP believed AAC intervention was warranted in each case Each child was given an AAC evaluation and trialed multiple devices Therapy with LAMP was identified as the best approach for these subjects Device used: Vantage Lite Therapy involved one to three sessions per week

Studies in AAC and Autism: The Impact of LAMP as a Therapy Intervention Methods Primary measure of gains in communication Mean Length of Utterance (MLU) The Systematic Analysis of Language Transcripts (SALT) was applied to language samples and data was matched to Brown’s Stages to provide a frame of reference for therapy and help track progress. Along with this data, other data from sources such as the Preschool Language Scale, Type Token Ratio, and parent reports were noted.
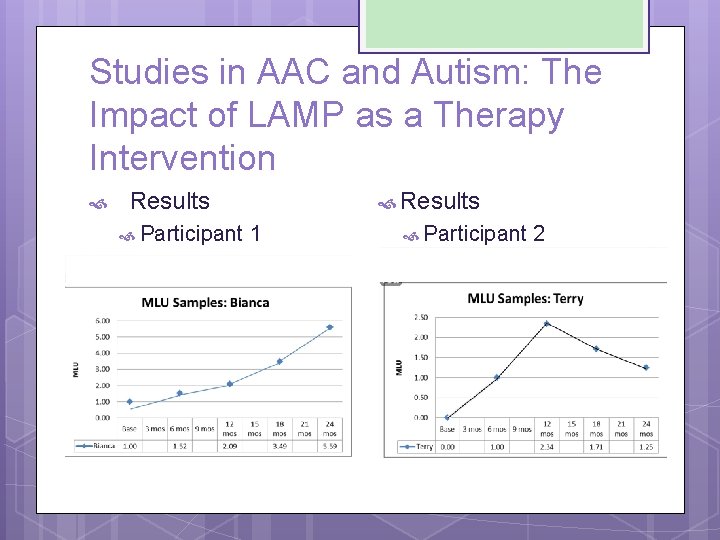
Studies in AAC and Autism: The Impact of LAMP as a Therapy Intervention Results Participant 1 Results Participant 2

Studies in AAC and Autism: The Impact of LAMP as a Therapy Intervention Results Participant 3 Results Participant 4
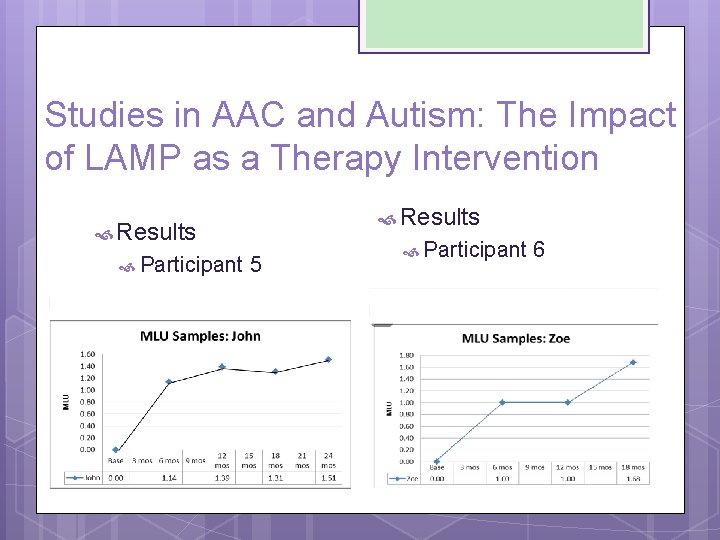
Studies in AAC and Autism: The Impact of LAMP as a Therapy Intervention Results Participant 5 Results Participant 6

Evaluation: TD INTRODUCTION • • Evaluated to determine a suitable AAC device Received a medical diagnosis of Autism, which accounted for her speech delay and behavioral problems: – – • • • Tantrums Self-abusive behaviors such as hair pulling, scratching, and biting Also diagnosed with a profound to severe communication and developmental delay. Essentially nonverbal Difficult to communicate with family, teachers, schoolmates, and her therapists.

Evaluation: June 23, 2014 Medical History: u. REMOVED FOR CONFIDENTIALITY

Medical History cont. Hospitalizations: u. REMOVED FOR CONFIDENTIALITY Current Medications: u. REMOVED FOR CONFIDENTIALITY

Motor Development TD’s motor development was severely delayed: She never crawled Started rolling at one year Was able to sit alone without support at two years Walked at five years with 100% assistance Required complete assistance for self-help skills including: feeding, dressing, and using the toilet utilizes the following adaptive equipment: walker, stroller, wheelchair, and communication switches at school She has been receiving intermittent physical therapy services since 2006 and occupational therapy since 2007

Speech Development TD’s speech development was delayed: started babbling at the age of one, but has not spoken her first word yet. She uses gestures, eye pointing, and vocalizations to communicate. has trouble following directions, but understands single words. The self-abusive behaviors have gotten progressively worse this past year has received speech-language therapy in the past, but it currently on a waiting list current methods for communication are not adequate at the present time nor will they be sufficient to meet daily communication needs in the near future without the use of a device to expand expressive language skills.

Comprehensive Analysis • Vision: – – • Hearing: – – • Most recent vision test was conducted six months prior to the evaluation Results revealed one dimensional vision and poor peripheral vision No difficulty with hearing She exhibited hypersensitivity to sound (above conversational level) during the assessment Physical: – – Gross motor: Restricted mobility, used wheelchair or 100% assistance to walk Fine motor: difficulty using an isolated finger, often mis-selected icons

Comprehensive Analysis • Oral Mechanism – – – • Lips symmetrical and of normal length Vertical jaw movement (munching pattern) to chew snack • Rotary jaw movement ideal • Limited muscle and jaw control Adequately created a seal with her lips when using sippy cup Unable to sip liquid from a straw • Indicates low muscle tone and limited muscle coordination No nasal obstructions Speech and Language – – Speech and language skills severely limited Essentially nonverbal; uses some vocalizations, eye gaze, and pointing

Devices Used During the Evaluation Nova. Chat 7 has a variety of vocabulary configurations and synthesized voices The device uses Symbol. Stixtm as the standard symbols and PCStm symbols can be added as an alternative. Offers the Multi. Chat software on an Android platform The device has a battery life of about 10 hours Touchscreen is accessible by direct selection or an included stylus. Nova. Chat 7 offers Ivona voices that include a child’s voice, teen’s voice, and numerous American, British English, and Australian adult options.

Devices Used/Recommended i. Pad with Touch. Chat *Recommended Offers a word, phrase and message system Over 10, 000 Symbol. Stix symbols included Buttons may be programmed to speak a message, navigate to new page, change volume, or clear the display Users can subscribe to i. Share and store files for safekeeping Can share customized pages with an online community Words, phrases or messages spoken with either the built-in voice synthesizer or by playing recorded messages Can also upload your own image or take a photo with the built-in camera 5 US English and 2 British English voices are available This device chosen because… Family already owns an i. Pad Large icons Keyguard can be used Cheaper

Additional Recommendations Use of actual objects or signs around the house i. e. dressing area, in the bathroom, kitchen etc. Mounting: Requires a mount on her wheelchair to carry the device. Device to be placed directly in front of her due to poor peripheral vision Carrying Case: for safe transport; i. Adapter 4 c Keyguard: To assist in appropriate activation of icons. Number of Symbols: Device should have an overlay of 15 locations with every other location programmed Large icons because of fine motor skills (1. 75 x 1. 5 inches) Type of Symbols: Start with pictures

ADDITIONAL RECOMMENDATIONS Sound: Make sure volume is not too high because of her hypersensitivity to sound Vocabulary: Mixture of fringe and core vocabulary Core • I want to eat • I don’t want to play • I need to color • More to drink • I like to listen to • Chat to read • Finished/all done Fringe • Chips Puzzle • Pudding Bowling • Oranges Bubbles • Goldfish Color • Ball Playdoh • School

ADDITIONAL RECOMMENDATIONS • Mother, sister, grandparents and teachers should all be trained on how to program and use the device, how to get her to use it. • A combination of high and low tech is ideal for TD High tech • – • i. Pad Touch. Chat app Low tech – Visuals

Treatment Plan Upon receiving an AAC device, it is recommended that she receive speech therapy to address goals listed below: Goal 1: Use an AAC device to increase pragmatic skills to an age-appropriate level Objective 1: She will use an AAC device to initiate an activity while communicating with a variety of communication partners within six months. Objective 2: She will use an AAC device to take turns interacting with a variety of communication partners by combining two symbols on her device within six months. Objective 3: She will terminate an activity using an AAC device within six months.

Treatment Plan Goal 2: Use an AAC device to express medical emergency situations or health related information independently to an unfamiliar listener within six months. Objective 1: She will use an AAC device to indicate wants and needs independently to an unfamiliar listener within six months. Objective 2: She will use an AAC device to express emotions independently to familiar and unfamiliar listeners within the next six months.
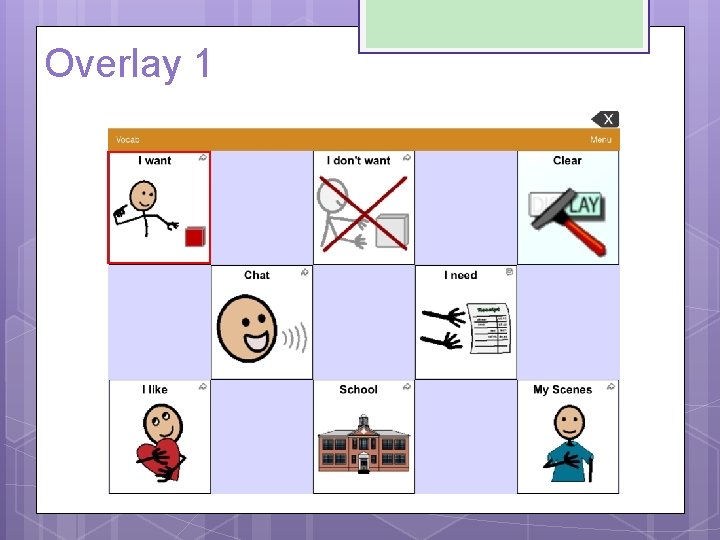
Overlay 1
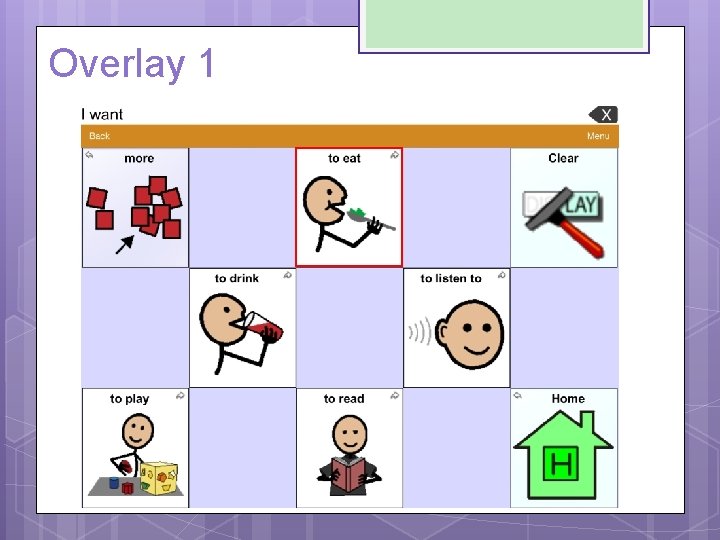
Overlay 1

Overlay 1

Overlay 1

Overlay 2

Overlay 2
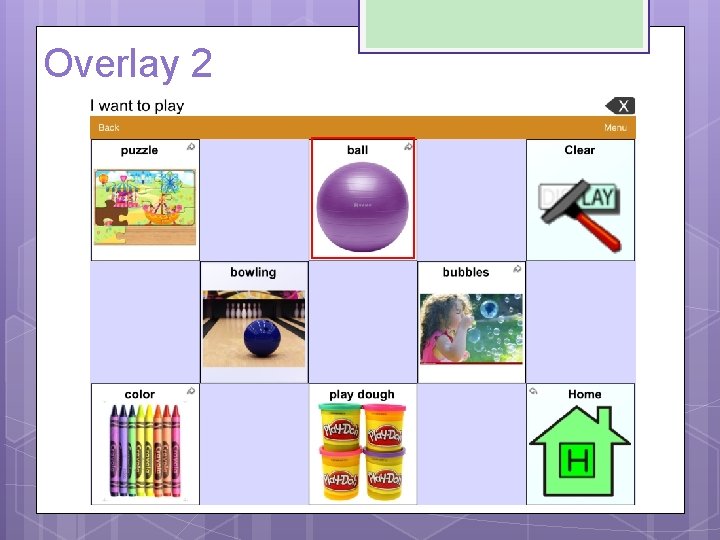
Overlay 2
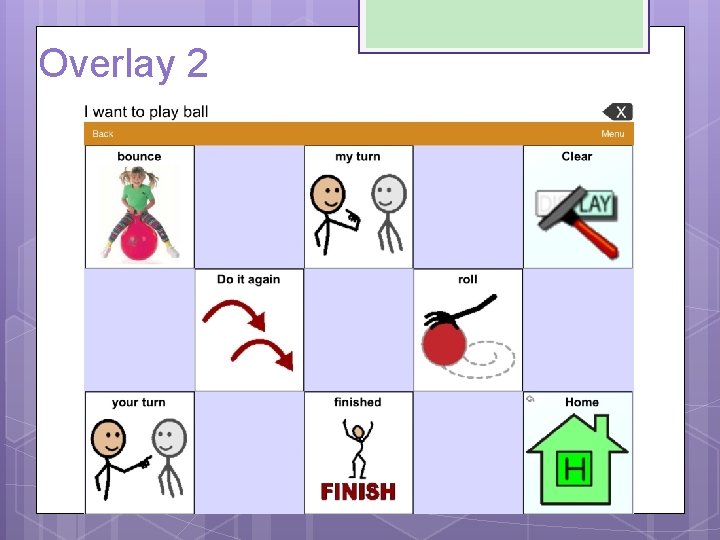
Overlay 2

References Abramson, J. , Flynn S. , Howard, S. , Laubscher, E. , Schlosser, R. , Sorce, J. (2011). Applying Technology to Visually Support Language and Communication in Individuals with Autism Spectrum Disorders. Journal of Autism Developmental Disorders, 42, 1228 -1235. Retrieved July 3, 2014 from Pub. Med. American Speech-Language Hearing Association. (2014). Autism (Autism Spectrum Disorder). Retrieved from http: //www. asha. org/public/speech/disorders/autism/. Autism (Autism Spectrum Disorder). Retrieved July 1, 2014, from http: //www. asha. org/public/speech/disorders/autism/. Autism Speaks. (2014). How is Autism Diagnosed? . Retrieved July 2, 2014, from http: //www. autismspeaks. org/what-autism/diagnosis. DSM-5 Diagnostic Criteria. (2013). Retrieved July 5, 1014, from http: //www. autismspeaks. org/.

References Flippin, M. , Reszka, S. , Watson, L. (2010). Effectiveness of the Picture Exchange Communication System (PECS) on Communication and Speech for Children with Autism Spectrum Disorders: A Meta-Analysis. American Journal of Speech-Language Pathology, 19, 178 -195. Retrieved July 1, 2014 from Pub. Med. Hawkins. (n. d. ). About Autism: Diagnosis. Retrieved July 5 2014, from http: //www. autismsociety. org/. Hodgdon, L. A. (1999). Solving Behavior Problems in Autism: Improving Communication with Visual Strategies. (pp. 1 -4). Troy, MI: Quirk. Roberts Publishing. Laurent, A. C. , Prizant, B. M. , Rubin, E. , Rydell, P. J. , & Wetherby, A. M. (2006). The SCERTS Model: A Comprehensive Educational Approach for Children With Autism Spectrum Disorders. (Vol. 1, pp. 1 -18). Baltimore, MD: Paul H. Brookes Publishing Co. Lovaas Institute. Retrieved July 3 2014, from http: //www. lovaas. com/approachdifferentiate. php.

References Mental Health, N. (2010). How Autism is Diagnosed. Psych Central. Retrieved July 7, 2014, from http: //psychcentral. com/. NIDCD Information Clearinghouse. (2012, July 19). Communication problems in children with autism spectrum disorder. Retrieved from http: //www. nidcd. nih. gov/. Potts, M. , & Satterfield, B. (2013). Studies in AAC and Autism: The Impact of LAMP as a Therapy Intervention. Prentke Romich Company, 1 -22. Retrieved from http: //www. liberator. co. uk/. Reynolds, T. (n. d. ). Deficits Associated with Autism. Retrieved from http: // communitycounselingservices. org/.

References TEACCH Approach. Retrieved July 5, 2014, from http: //teacch. com/aboutus/what-is-teacch. Therapies for Children with Autism Spectrum Disorders: A Review of the Research for Parents and Caregivers. (June 30, 2011). Retrieved July 1, 2014, from http: //effectivehealthcare. ahrq. gov/index. cfm/.
- Slides: 81