A Revisit to Anorectal Malignant Melanoma ARMM Joint




























- Slides: 37

A Revisit to Anorectal Malignant Melanoma (ARMM) Joint Hospital Surgical Grand Round 8 Nov 2014 Dr Jessie Chan Pamela Youde Nethersole Eastern Hospital

Outline Introduction Epidemiology Presentation Investigations Staging Prognosis Treatment Surgery Adjuvant therapy

Introduction Rare neoplasm First reported by Moore in 1857 Distinct biological and clinical entity from cutaneous melanoma with worse prognosis No clear etiology elucidated Arised from melanocytes distal to dentate line and extend proximally to rectum Arised directly from melanocytes which present rarely in the mucosal epithelium of proximal anus or distal rectum

ARMM <1% of all malignant melanomas <4% of anal canal malignancies Primary Secondary Metastasis from cutaneous melanoma (2%)

Epidemiology Median age at presentation: 55 (range 29 -92) Reported incidence: 0. 04 – 1. 19% No adequate population-based studies to draw definite conclusions for racial and gender difference

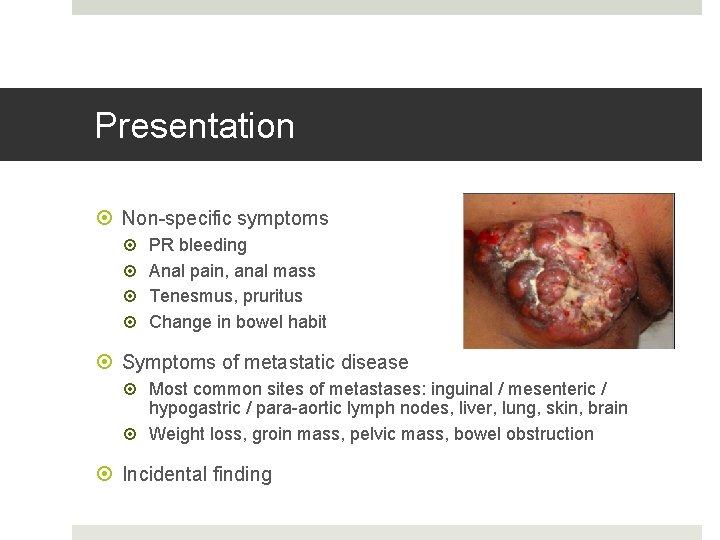
Presentation Non-specific symptoms PR bleeding Anal pain, anal mass Tenesmus, pruritus Change in bowel habit Symptoms of metastatic disease Most common sites of metastases: inguinal / mesenteric / hypogastric / para-aortic lymph nodes, liver, lung, skin, brain Weight loss, groin mass, pelvic mass, bowel obstruction Incidental finding

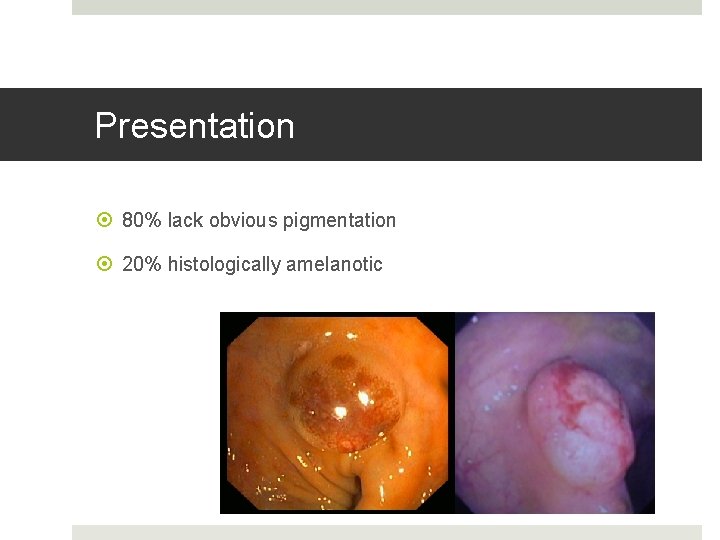
Presentation 80% lack obvious pigmentation 20% histologically amelanotic

Presentation Up to 60% with locoregional lymphatic spread (mesorectal, pelvic side wall, inguinal lymph nodes) Up to 40% with distant metastasis

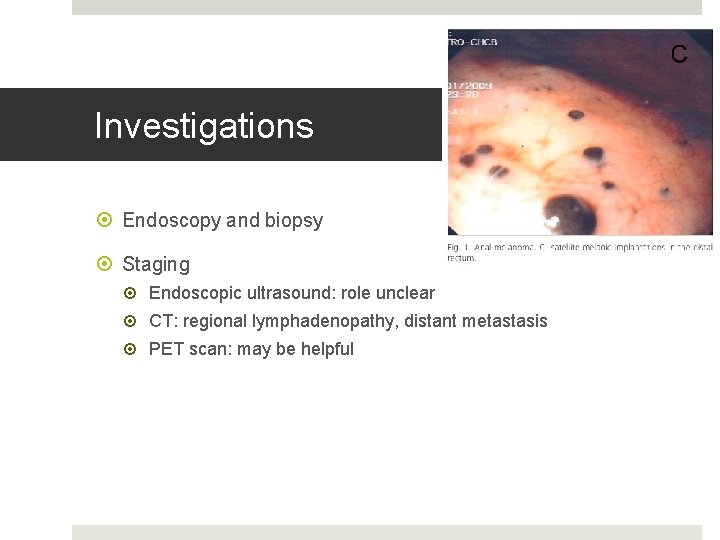
Investigations Endoscopy and biopsy Staging Endoscopic ultrasound: role unclear CT: regional lymphadenopathy, distant metastasis PET scan: may be helpful

Staging Cutaneous melanoma: AJCC TNM system ARMM Clinical staging Stage I: local disease Stage II: local disease with regional lymph nodes Stage III: distant metastatic disease

Prognosis Poor prognosis Overall 5 -year survival 3 -22% Survival <10 months with recurrent or metastatic disease

Prognosis Good prognostic factors Tumour thickness <2 mm Poor prognostic factors Tumour thickness >3 mm Tumour site above dentate line Lymphovascular / perineural invasion Necrosis Wanebo HJ, Woodruff JM, Farr GH, et al. Anorectal melanoma. Cancer. 1981 Apr 1; 47(7): 1891 -900. Brady MS, Kavolius JP, Quan SH. Anorectal melanoma. A 64 -year experience at Memorial Sloan. Kettering Cancer Center. Dis Colon Rectum. 1995 Feb; 38(2): 146 -51. Perez DR, Trakarnsanga A, Shia J, et al. Locoregional lymphadenectomy in the surgical management of anorectal melanoma. Ann Surg Oncol. 2013; 20: 2339 -2344.

Treatment

Treatment Surgery Wide local excision (WLE) Abdominoperineal resection (APR) Regional lymph node Sentinel lymph node biopsy Lymphadenectomy

Treatment Adjuvant therapy Systemic Chemotherapy Biochemotherapy Interferon Vaccine / immunotherapy Local Radiation therapy Electrochemotherapy

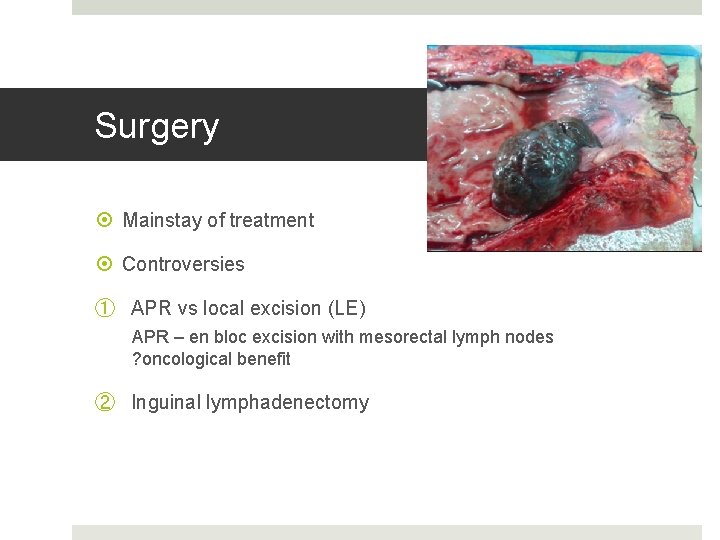
Surgery Mainstay of treatment Controversies ① APR vs local excision (LE) APR – en bloc excision with mesorectal lymph nodes ? oncological benefit ② Inguinal lymphadenectomy

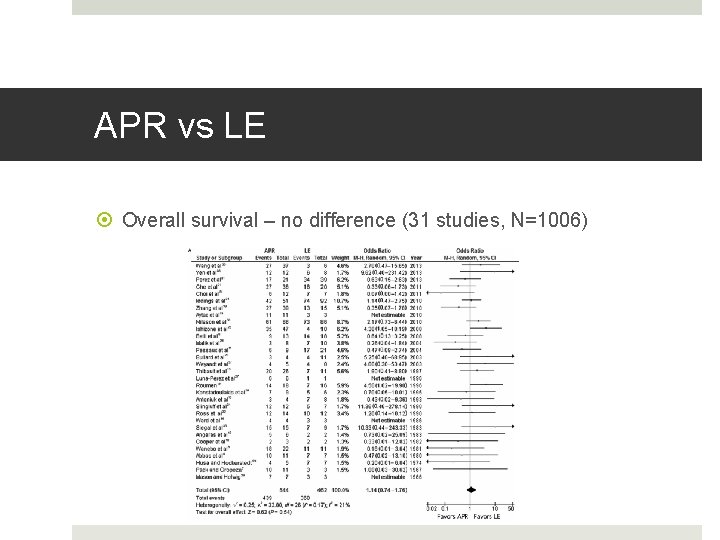
Surgery Meta-analysis by Akihisa Matsuda et al in Annals of Surgery 2014 31 studies 1006 patients APR vs LE Overall survival Relapse-free survival Local recurrence rate Akihisa Matsuda, Masao Miyashita, Satoshi Matsumoto, et al. Abdominoperineal Resection Provides Better Local Control But Equivalent Overall Survival to Local Excision of Anorectal Malignant Melanoma – A Systemic Review. Ann Surg. 2014; 00: 1 -8.

APR vs LE Overall survival – no difference (31 studies, N=1006)

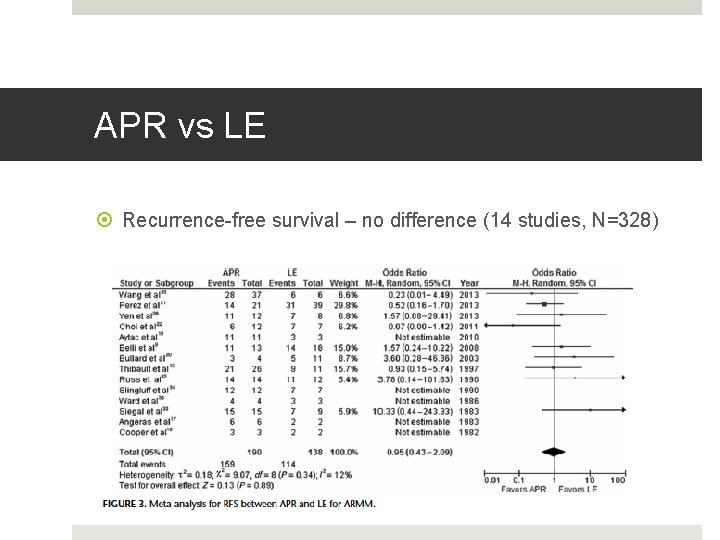
APR vs LE Recurrence-free survival – no difference (14 studies, N=328)

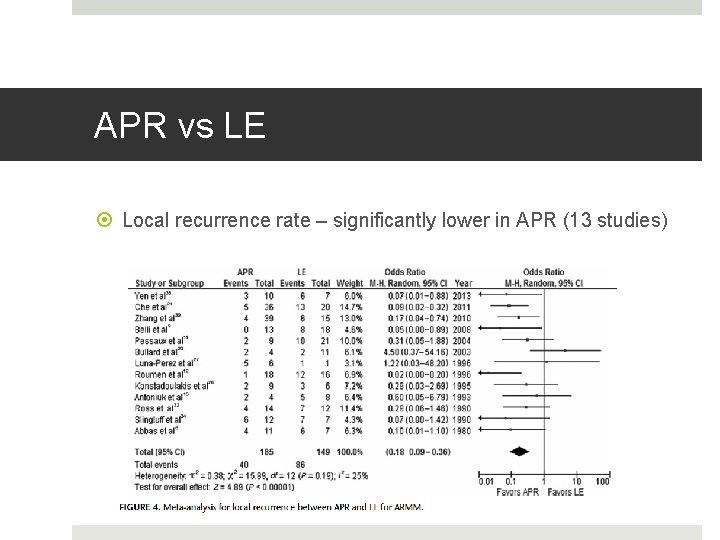
APR vs LE Local recurrence rate – significantly lower in APR (13 studies)

Surgery No survival benefit from APR over LE Higher local recurrence from LE which could be managed by salvage surgery Less complications and morbidities with LE Better body image Better urinary and sexual function Minimal impact on bowel function Minimizing morbidities and maximizing quality of life merits consideration in such an aggressive disease

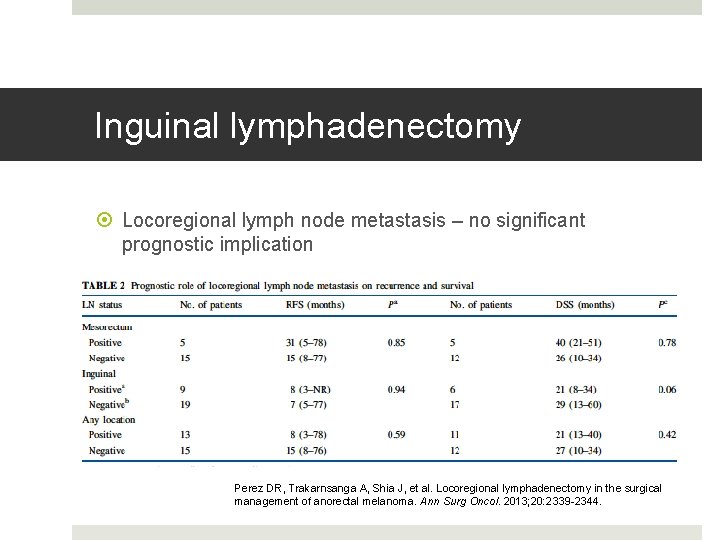
Inguinal lymphadenectomy Locoregional lymph node metastasis – no significant prognostic implication Perez DR, Trakarnsanga A, Shia J, et al. Locoregional lymphadenectomy in the surgical management of anorectal melanoma. Ann Surg Oncol. 2013; 20: 2339 -2344.

Inguinal lymphadenectomy Systemic dissemination with micrometastasis in distant organs occurs early with unfavourable prognosis Prophylactic – no improvement in survival, increased risk of complications Therapeutic – seems not to contribute to improvement of survival Perez DR, Trakarnsanga A, Shia J, et al. Locoregional lymphadenectomy in the surgical management of anorectal melanoma. Ann Surg Oncol. 2013; 20: 2339 -2344.

Adjuvant Therapy

Chemotherapy Role remains unclear ? Adjuvant ? Palliative Dacarbazine, cisplatin, vinblastine, vincristine, nimustine, bacillus Calmette-Guérin, levamisole, temozolomide Single or combination – poor results

Interferon alpha Combination of direct activities and indirect immune-mediated effects Parenteral route / intratumoural injection No standard regimen established Insufficient data

Biochemotherapy Biologic agent (interferon, interleukin) + traditional cytotoxic chemotherapeutic agent Longer disease-free and median survival in metastatic ARMM when compared with chemotherapy alone Kim K B, Sanguino A M, Hodges C, et al. Biochemotherapy in patients with metastatic anorectal mucosal melanoma. Cancer. 2004; 100: 1478– 1483. Atkins MB, Lotze MT, Dutcher JP, et al. High-dose recombinant interleukin 2 therapy for patients with metastatic melanoma: analysis of 270 patients treated between 1985 and 1993. J Clin Oncol. 1999 Jul; 17(7): 2105 -16.

Biochemotherapy Role Best available adjuvant therapy after surgery Considered in advanced or metastatic ARMM

Vaccine / Immunotherapy Immunize against melanoma cell antigen BRAF and c. KIT mutations Insufficient data Area of significant research effort and may play an important part of the non-operative treatment of melanoma in the future

Radiation Therapy Locoregional disease control Primary lesion, inguinal and pericolic lymph nodes Utility unclear, evidence conflicting

Radiation Therapy Ballo et al Local excision + post-op RT Local control rate comparable with APR 5 -year local control rate: 74% Ballo MT, Gershenwald JE, Zagars GK, et al. Sphincter-sparing local excision and adjuvant No improvement in survival radiation for anal-rectal melanoma. J Clin Oncol. 2002 Dec 1; 20(23): 4555 -8. Moozar et al Pre-op RT little effect on tumour burden Post-op RT did not change local recurrence No survival benefit Moozar KL, Wong CS, Couture J. Anorectal malignant melanoma: treatment with surgery or radiation therapy, or both. Can J Surg. 2003 Oct; 46(5): 345 -9.

Electrochemotherapy Injection of chemotherapy directly into the lesions, followed by application of electric pulses using a needle electrode Electrical stimulation to the tissues creating a transient permeabilization of the plasma membrane Allows direct access of the chemotherapeutic agents into the cytosol of tumor cells Known to provide effective local control for cutaneous melanoma

Electrochemotherapy Convert APR to sphincter-preserving local excision Snoj M, Rudolf Z, Cemazar M, et al. Successful sphincter-saving treatment of anorectal malignant melanoma with electrochemotherapy, local excision and adjuvant brachytherapy. Anticancer Drugs. 2005 Mar; 16(3): 345 -8. Overall success rate unclear

Summary ARMM is a rare and highly malignant disease Survival predicted by status of regional and distant metastasis but not method of surgery for local control Minimizing surgical morbidities and maximizing quality of life should be the major consideration in formulating the treatment plan Role of all adjuvant therapies is still unclear

References P Carcoforo, M. T Raiji, G. M Palini, et al. Primary Anorectal Melanoma: An Update. J Cancer. 2012; 3: 449 -453. doi: 10. 7150/jca. 5187. Marc Singer and Matthew G. Mutch. Anal Melanoma. Clin Colon Rectal Surg. May 2006; 19(2): 78– 87. Akihisa Matsuda, Masao Miyashita, Satoshi Matsumoto, et al. Abdominoperineal Resection Provides Better Local Control But Equivalent Overall Survival to Local Excision of Anorectal Malignant Melanoma – A Systemic Review. Ann Surg. 2014; 00: 1 -8. Perez DR, Trakarnsanga A, Shia J, et al. Locoregional lymphadenectomy in the surgical management of anorectal melanoma. Ann Surg Oncol. 2013; 20: 2339 -2344. Wanebo HJ, Woodruff JM, Farr GH, et al. Anorectal melanoma. Cancer. 1981 Apr 1; 47(7): 1891900. Brady MS, Kavolius JP, Quan SH. Anorectal melanoma. A 64 -year experience at Memorial Sloan -Kettering Cancer Center. Dis Colon Rectum. 1995 Feb; 38(2): 146 -51.

References Kim K B, Sanguino A M, Hodges C, et al. Biochemotherapy in patients with metastatic anorectal mucosal melanoma. Cancer. 2004; 100: 1478– 1483. Ulmer A, Metzger S, Fierlbeck G. Successful palliation of stenosing anorectal melanoma by intratumoral injections with natural interferon-β. Melanoma Res. 2002; 12: 395– 398. Atkins MB, Lotze MT, Dutcher JP, et al. High-dose recombinant interleukin 2 therapy for patients with metastatic melanoma: analysis of 270 patients treated between 1985 and 1993. J Clin Oncol. 1999 Jul; 17(7): 2105 -16. Snoj M, Rudolf Z, Cemazar M, et al. Successful sphincter-saving treatment of anorectal malignant melanoma with electrochemotherapy, local excision and adjuvant brachytherapy. Anticancer Drugs. 2005 Mar; 16(3): 345 -8. Ballo MT, Gershenwald JE, Zagars GK, et al. Sphincter-sparing local excision and adjuvant radiation for anal-rectal melanoma. J Clin Oncol. 2002 Dec 1; 20(23): 4555 -8. Moozar KL, Wong CS, Couture J. Anorectal malignant melanoma: treatment with surgery or radiation therapy, or both. Can J Surg. 2003 Oct; 46(5): 345 -9.

Thank You