A practical approach to Peripheral Polyneuropathies Bashar Katirji

A practical approach to Peripheral Polyneuropathies Bashar Katirji, MD, FACP
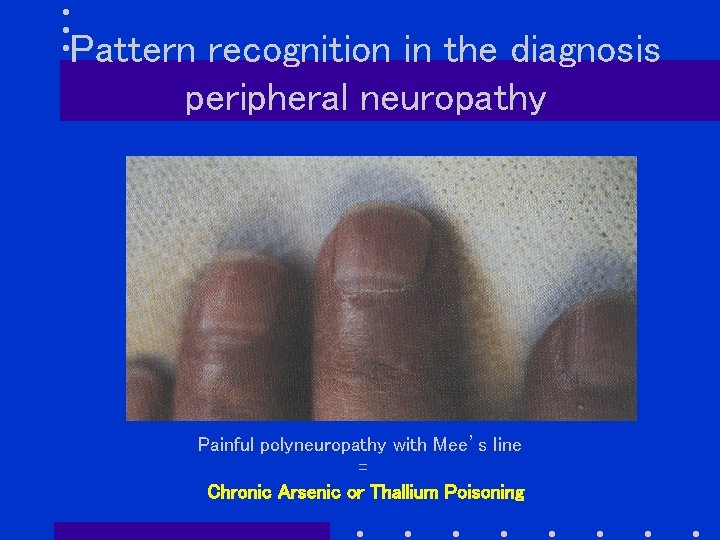
Pattern recognition in the diagnosis peripheral neuropathy Painful polyneuropathy with Mee’s line = Chronic Arsenic or Thallium Poisoning
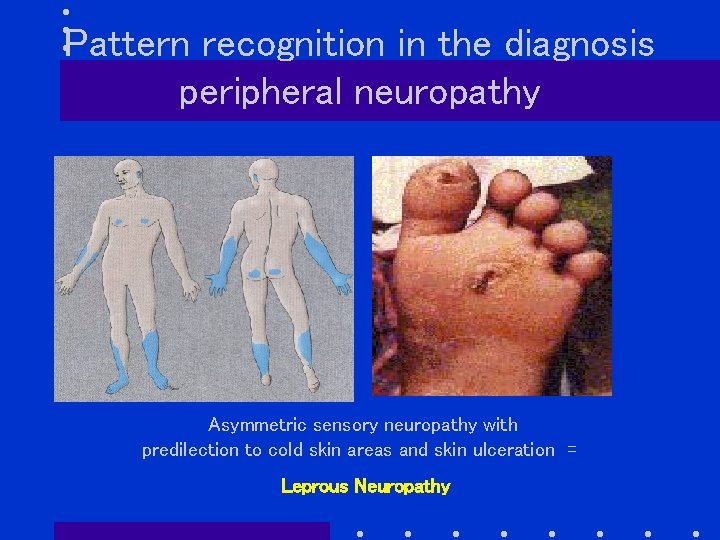
Pattern recognition in the diagnosis peripheral neuropathy Asymmetric sensory neuropathy with predilection to cold skin areas and skin ulceration = Leprous Neuropathy
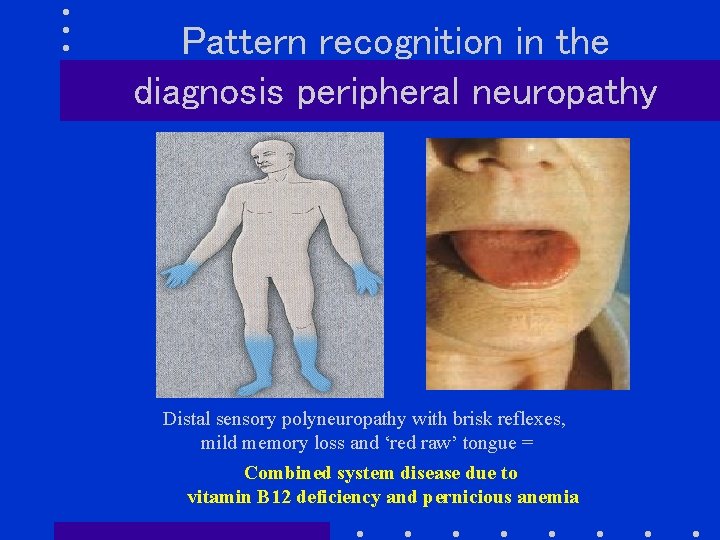
Pattern recognition in the diagnosis peripheral neuropathy Distal sensory polyneuropathy with brisk reflexes, mild memory loss and ‘red raw’ tongue = Combined system disease due to vitamin B 12 deficiency and pernicious anemia
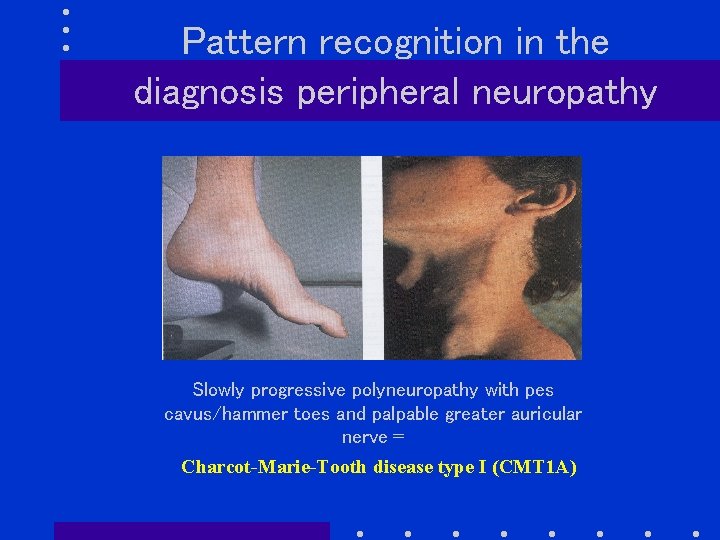
Pattern recognition in the diagnosis peripheral neuropathy Slowly progressive polyneuropathy with pes cavus/hammer toes and palpable greater auricular nerve = Charcot-Marie-Tooth disease type I (CMT 1 A)

Diagnosis of peripheral neuropathies • Pattern recognition – Requires vast experience and mostly accomplished by senior neurologists – Applies to a minority of patients – Is usually evident in advanced disease • Irrational approach – Order all tests to every patient with a neuropathy • Rational approach – A systematic approach that utilizes mainly the • Clinical findings • Electrodiagnostic studies

Classification of Peripheral Neuropathies Axonopathy Axonal degeneration Myelinopathy Segmental demyelination Neuronopathy Neuronal degeneration
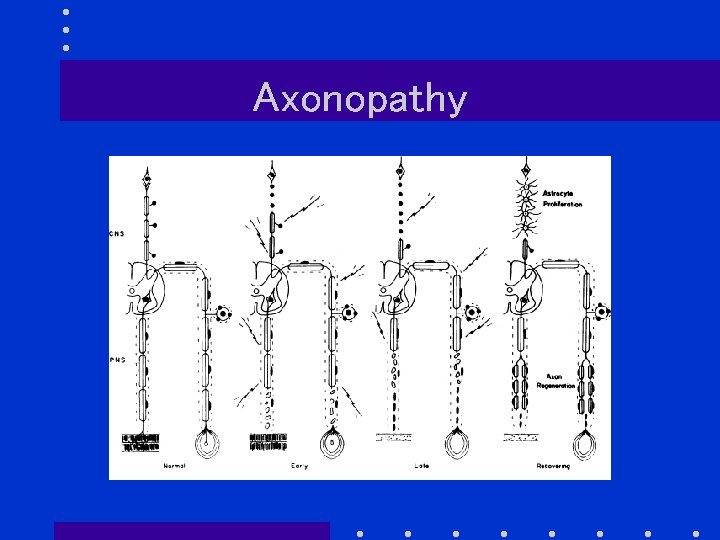
Axonopathy
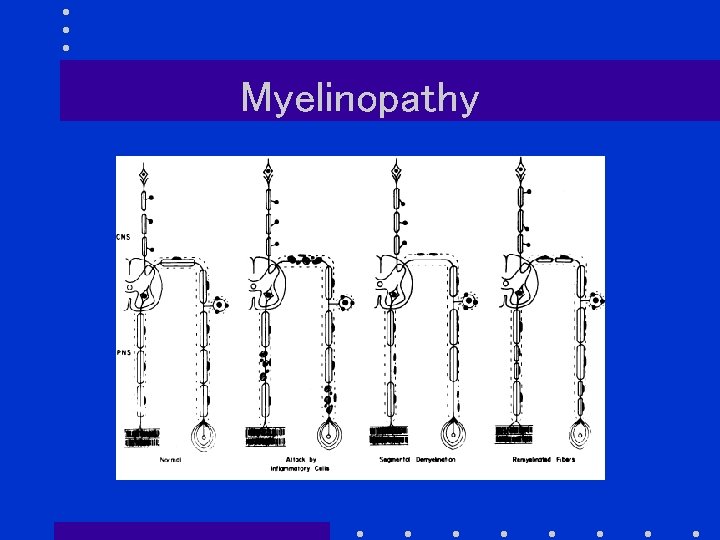
Myelinopathy
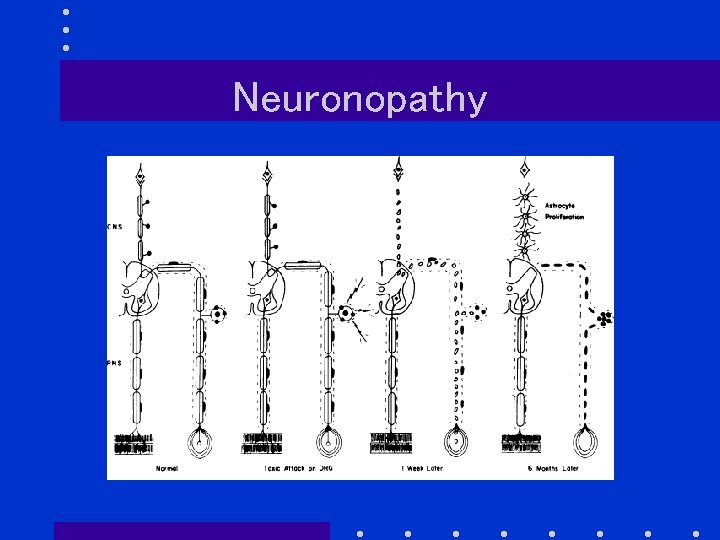
Neuronopathy

Systematic Approach to Peripheral Neuropathy • The history and physical examination is the starting point in the evaluation. • The electrodiagnostic evaluation is the next step in the accurate diagnosis. • Laboratory studies should be based on the differential diagnosis guided by the clinical evaluation and EDX studies • At times, other tests may be necessary – Autonomic testing (QSART), QST – Antibody testing – Nerve biopsy

The Value of the Electrodiagnostic Tests in Peripheral Neuropathies • EDX study provides unequivocal diagnosis of a neuropathy. • EDX study are very useful in confirming the anatomic distribution of a neuropathy. – A mononeuropathy – Multiple mononeuropathies – A peripheral polyneuropathy • The EDX excludes “mimickers” of polyneuropathies – – Bilateral carpal tunnel syndromes (e. g. in diabetics) Bilateral S 1/S 2 radiculopathies (e. g. in elderly) Bilateral tarsal tunnel syndromes Myopathy (e. g. distal)

The Value of the Electrodiagnostic Tests in Peripheral Neuropathies • Most importantly in polyneuropathy, the EDX study is essential in determining – The type(s) of fibers involved • Sensorimotor • Motor • Sensory – Underlying primary pathophysiology • Axonal • Demyelinating
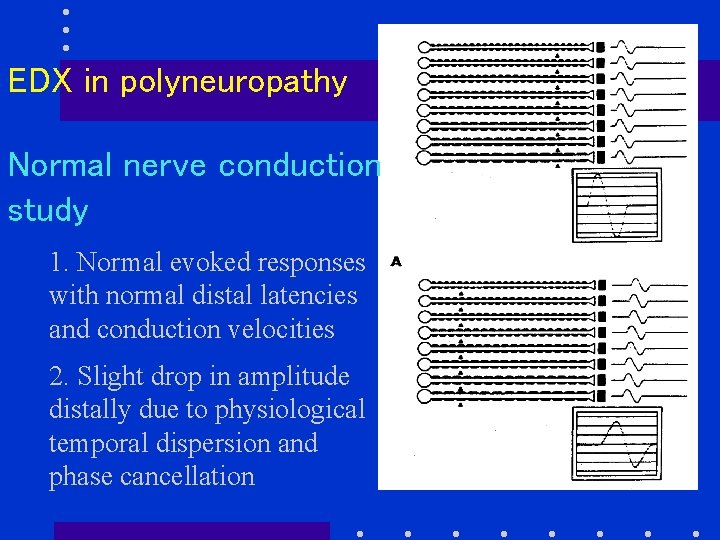
EDX in polyneuropathy Normal nerve conduction study 1. Normal evoked responses with normal distal latencies and conduction velocities 2. Slight drop in amplitude distally due to physiological temporal dispersion and phase cancellation
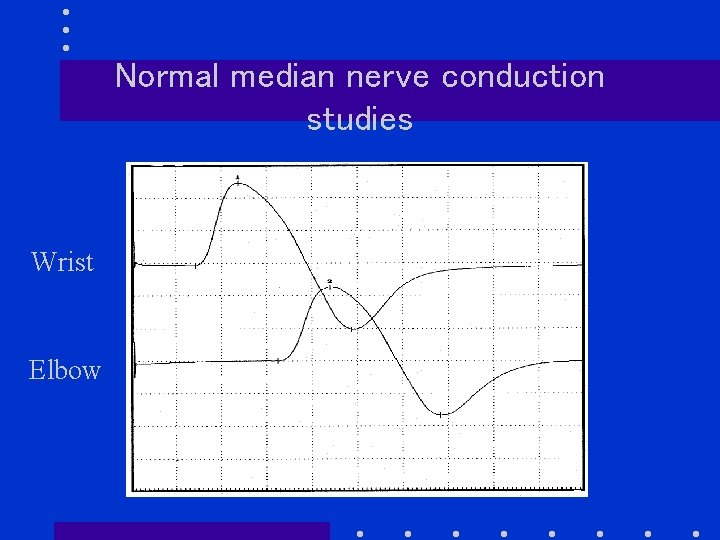
Normal median nerve conduction studies Wrist Elbow
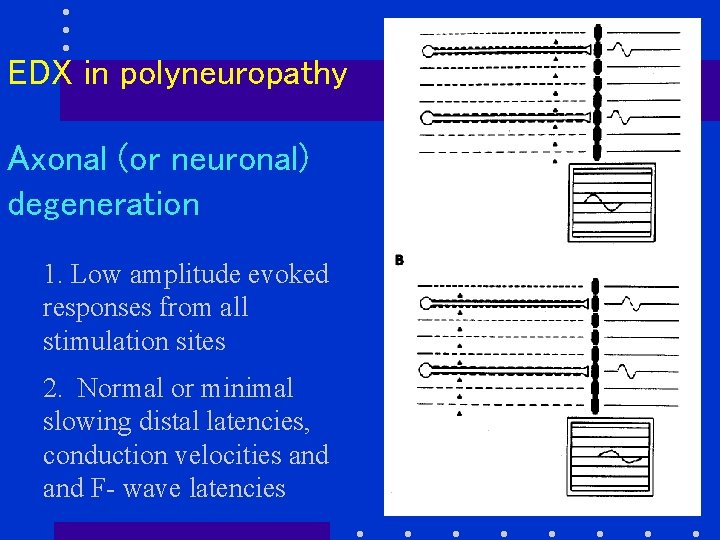
EDX in polyneuropathy Axonal (or neuronal) degeneration 1. Low amplitude evoked responses from all stimulation sites 2. Normal or minimal slowing distal latencies, conduction velocities and F- wave latencies
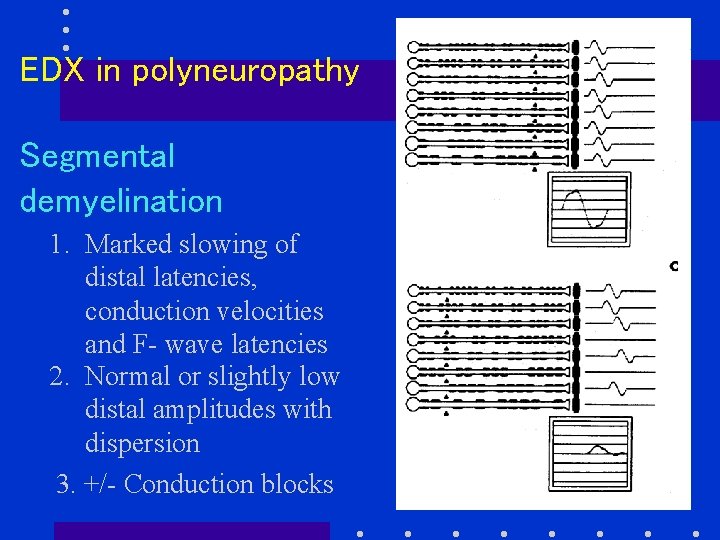
EDX in polyneuropathy Segmental demyelination 1. Marked slowing of distal latencies, conduction velocities and F- wave latencies 2. Normal or slightly low distal amplitudes with dispersion 3. +/- Conduction blocks

Identification of conduction block >50% loss of distal amplitude Abnormal amplitude reduction >15% of distal duration CMAP duration increased No Yes Area loss >50% Area loss <50% Area loss >50% Pure conduction block (CB) Temporal dispersion (TD) CB/TD
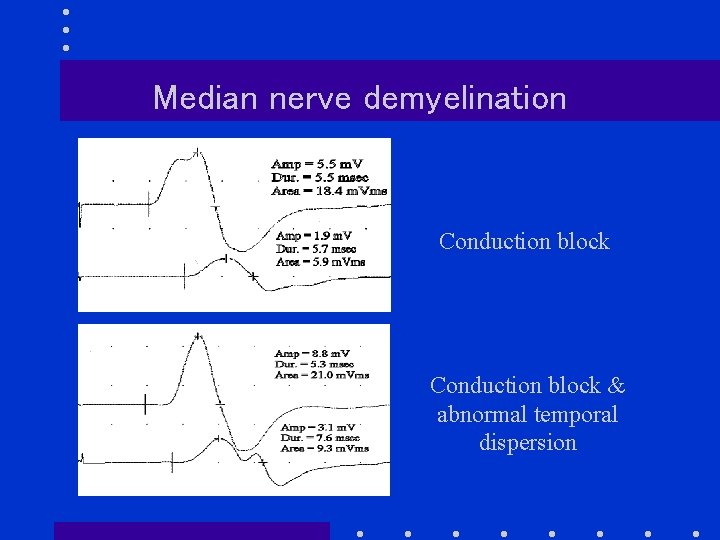
Median nerve demyelination Conduction block & abnormal temporal dispersion
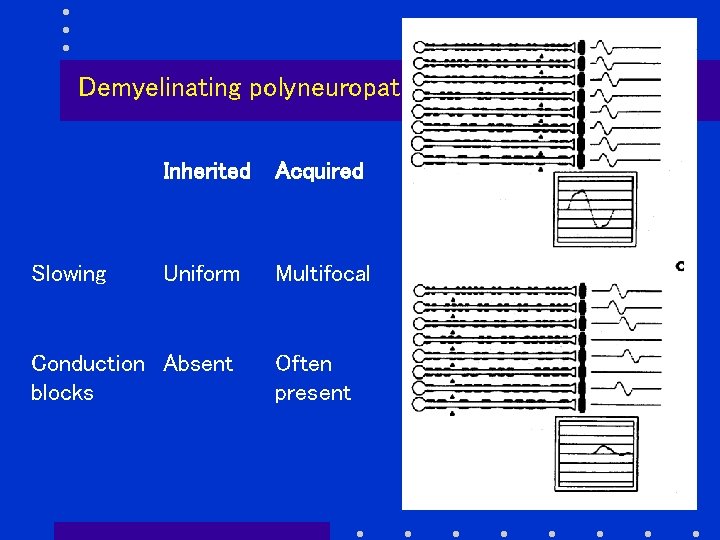
Demyelinating polyneuropathies Slowing Inherited Acquired Uniform Multifocal Conduction Absent blocks Often present
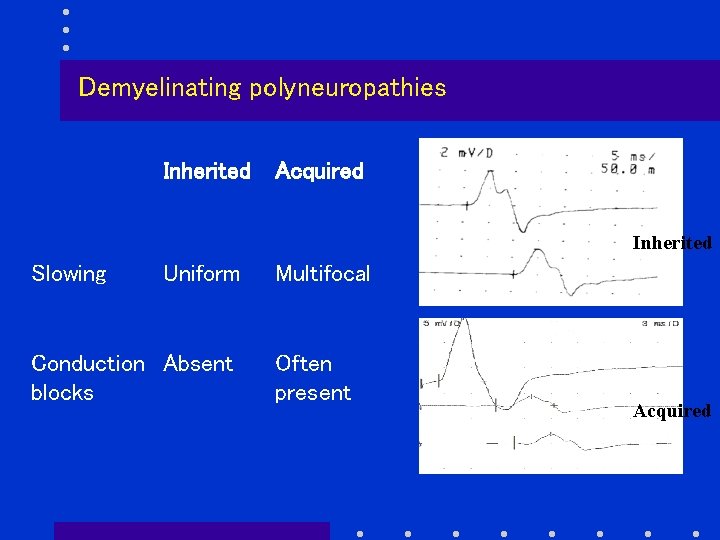
Demyelinating polyneuropathies Inherited Acquired Inherited Slowing Uniform Conduction Absent blocks Multifocal Often present Acquired
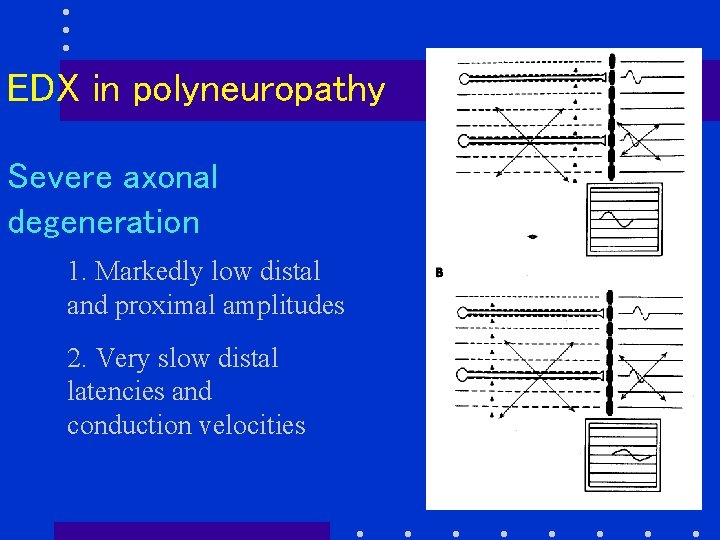
EDX in polyneuropathy Severe axonal degeneration 1. Markedly low distal and proximal amplitudes 2. Very slow distal latencies and conduction velocities
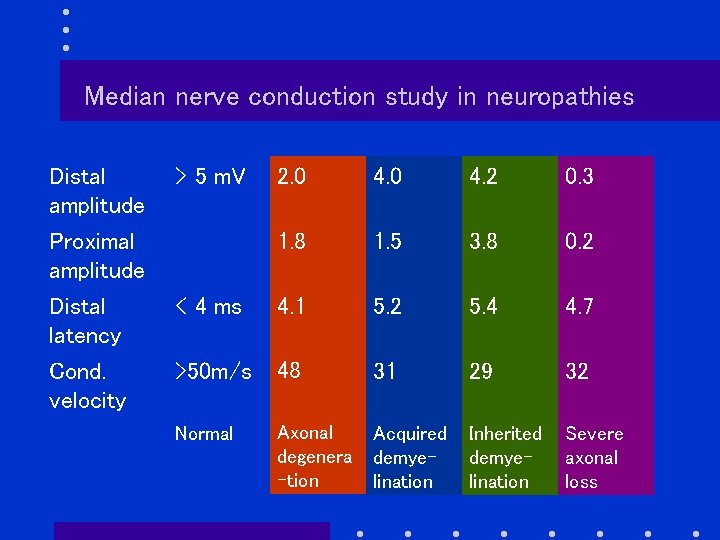
Median nerve conduction study in neuropathies Distal amplitude > 5 m. V Proximal amplitude 2. 0 4. 2 0. 3 1. 8 1. 5 3. 8 0. 2 Distal latency < 4 ms 4. 1 5. 2 5. 4 4. 7 Cond. velocity >50 m/s 48 31 29 32 Normal Axonal degenera -tion Acquired demyelination Inherited demyelination Severe axonal loss
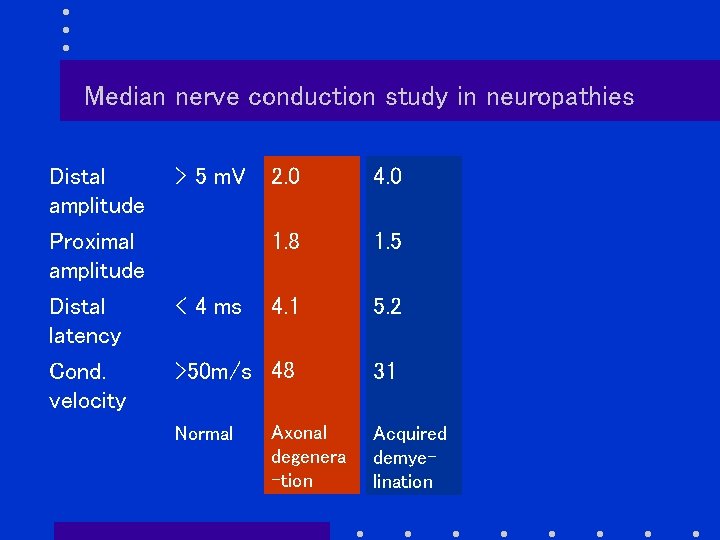
Median nerve conduction study in neuropathies Distal amplitude > 5 m. V Proximal amplitude 2. 0 4. 0 1. 8 1. 5 Distal latency < 4 ms 4. 1 5. 2 Cond. velocity >50 m/s 48 31 Normal Axonal degenera -tion Acquired demyelination
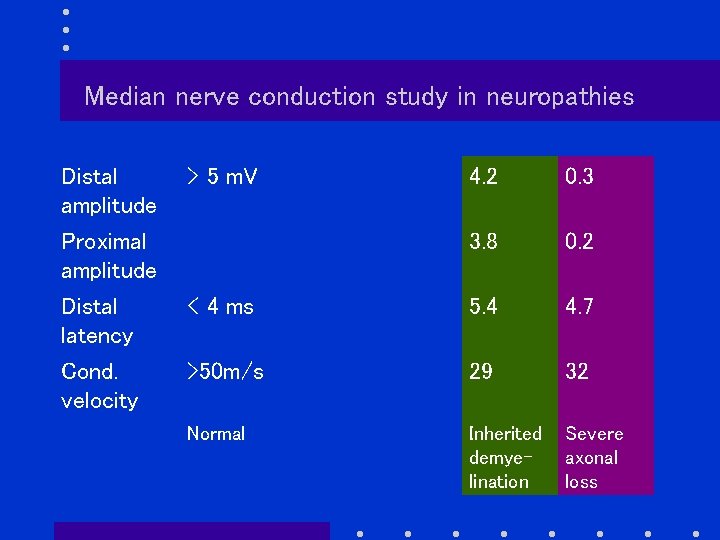
Median nerve conduction study in neuropathies Distal amplitude > 5 m. V Proximal amplitude 4. 2 0. 3 3. 8 0. 2 Distal latency < 4 ms 5. 4 4. 7 Cond. velocity >50 m/s 29 32 Normal Inherited demyelination Severe axonal loss

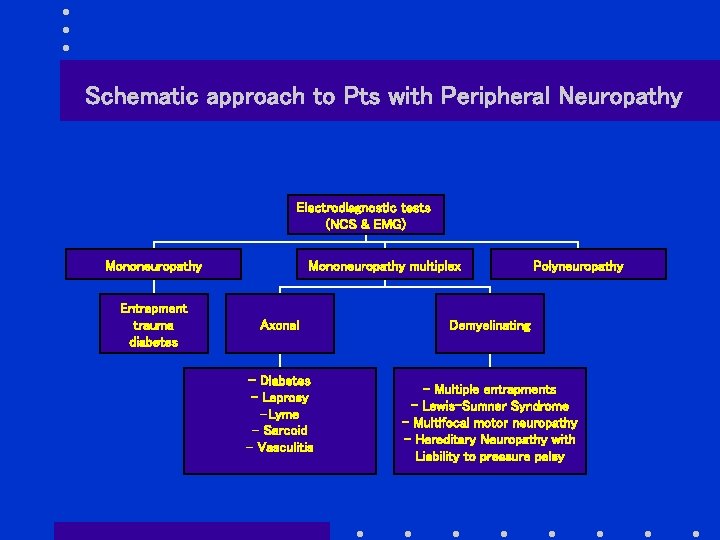
Schematic approach to Pts with Peripheral Neuropathy Electrodiagnostic tests (NCS & EMG) Mononeuropathy Entrapment trauma diabetes Mononeuropathy multiplex Axonal - Diabetes - Leprosy -Lyme - Sarcoid - Vasculitis Polyneuropathy Demyelinating - Multiple entrapments - Lewis-Sumner Syndrome - Multifocal motor neuropathy - Hereditary Neuropathy with Liability to pressure palsy
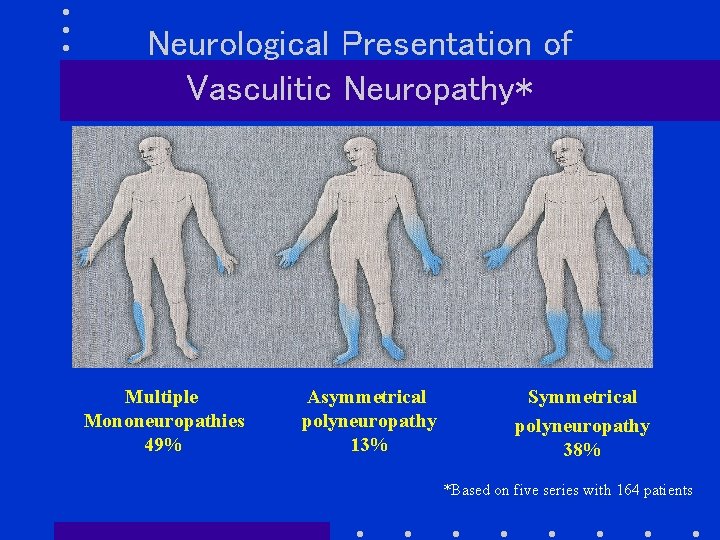
Neurological Presentation of Vasculitic Neuropathy* Multiple Mononeuropathies 49% Asymmetrical polyneuropathy 13% Symmetrical polyneuropathy 38% *Based on five series with 164 patients
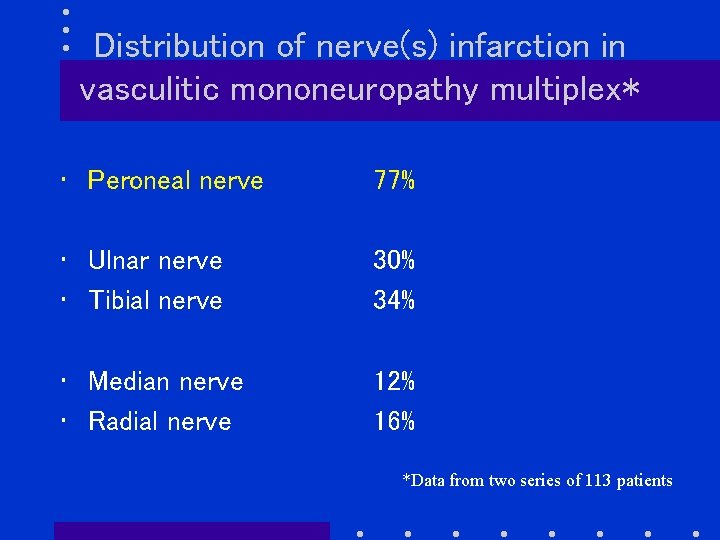
Distribution of nerve(s) infarction in vasculitic mononeuropathy multiplex* • Peroneal nerve 77% • Ulnar nerve • Tibial nerve 30% 34% • Median nerve • Radial nerve 12% 16% *Data from two series of 113 patients

Relative frequency of different disorders causing vasculitic neuropathy* • Polyarteritis nodosa group • Rheumatoid arthritis • Sjogren’s syndrome • SLE • Mixed CTD • Other systemic disease † • Nonsystemic vasculitis † including Wegener’s granulomatosus 18% 1% 1% 9% 13% 40% *Data compiled from three series with 149 patients
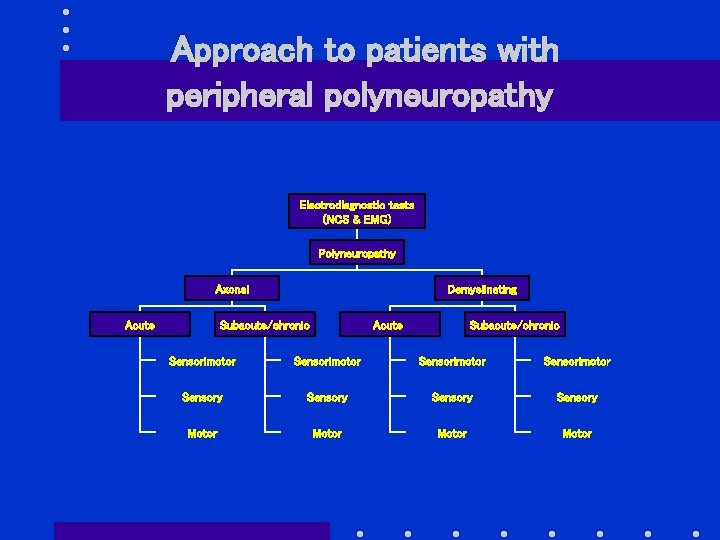
Approach to patients with peripheral polyneuropathy Electrodiagnostic tests (NCS & EMG) Polyneuropathy Axonal Acute Demyelinating Subacute/chronic Acute Subacute/chronic Sensorimotor Sensory Motor

Acute demyelinating polyneuropathies

Acute axonal polyneuropathies

Acute axonal polyneuropathies

Subacute/chronic demyelinating polyneuropathies

Subacute/chronic demyelinating polyneuropathies

Subacute/chronic axonal polyneuropathies

Subacute/chronic axonal polyneuropathies

Role of Autoantibody testing in peripheral polyneuropathy • Many antibodies are associated with clinical syndromes that are not unique to patients with the antibody • In most clinical conditions, the positive antibody is not sensitive enough to rely on solely fro the diagnosis. • The pathogenic role for the antibody in causing the clinical syndrome is uncertain.

Neuropathy syndromes associated with “anti-nerve” antibodies Neuropathy Antigen % positive Miller Fisher syndrome GQ 1 B 90% Subacute sensory neuropathy* Hu 90% Multifocal motor neuropathy GM 1 50 -60% Ig. M Neuropathy MAG 50 -60% Sensory neuropathy Sulfatide variable * Paraneoplastic, associated with SSLC
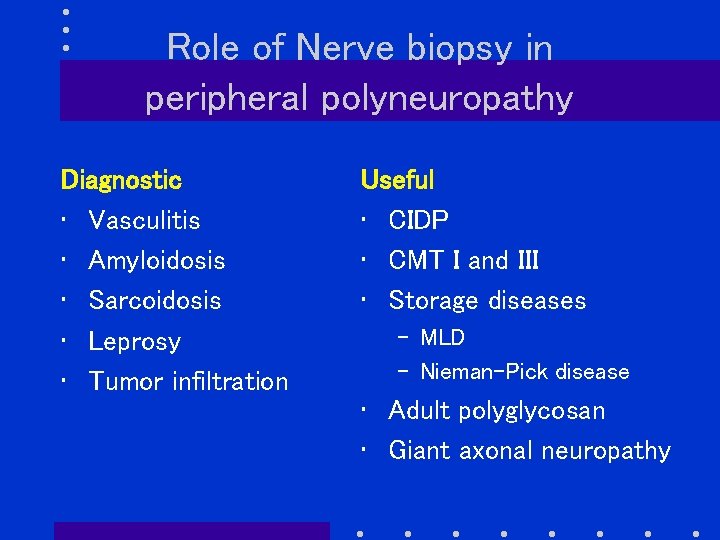
Role of Nerve biopsy in peripheral polyneuropathy Diagnostic • Vasculitis • Amyloidosis • Sarcoidosis • Leprosy • Tumor infiltration Useful • CIDP • CMT I and III • Storage diseases – MLD – Nieman-Pick disease • Adult polyglycosan • Giant axonal neuropathy
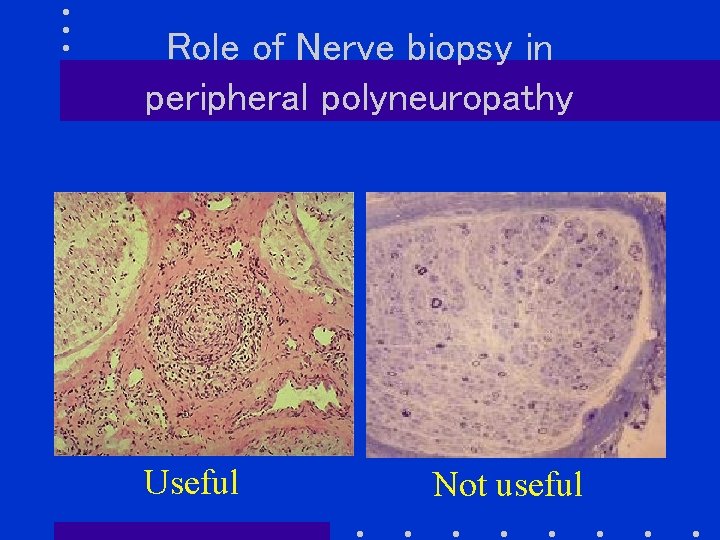
Role of Nerve biopsy in peripheral polyneuropathy Useful Not useful

- Slides: 43