A Plethora of Pills Reducing Medication Burden and

A Plethora of Pills: Reducing Medication Burden and Improving Adherence in Polypharmacy American College of Physicians - Maine Chapter Autumn Meeting in Bar Harbor September, 2014 Stephanie Nichols, Pharm. D. , BCPS, BCPP Associate Professor – Husson University School of Pharmacy Clinical Pharmacist – Psychiatry & Adult Inpatient Medicine Nicholss@Husson. edu

Objectives Define polypharmacy and recall it's prevalence Illustrate why recognition and management of polypharmacy is important Demonstrategies to avoid polypharmacy Assess high risk polypharmacy situations and formulate a plan to initiate pharmacological debridement Employ strategies to improve medication adherence in patients with a high pill burden

Define Polypharmacy and Recall it’s Prevalence

Polypharmacy is…. . X+ chronic daily medications? › OTCs/Herbals › Ex. HF or COPD “High Risk Polypharmacy” › Ex. 2+ narcotics, 2+ benzos, 3+ oral hypoglycemics 2+ drugs in the same class? More drugs prescribed than warranted clinically ? › “Prescribing cascade”

Polypharmacy?
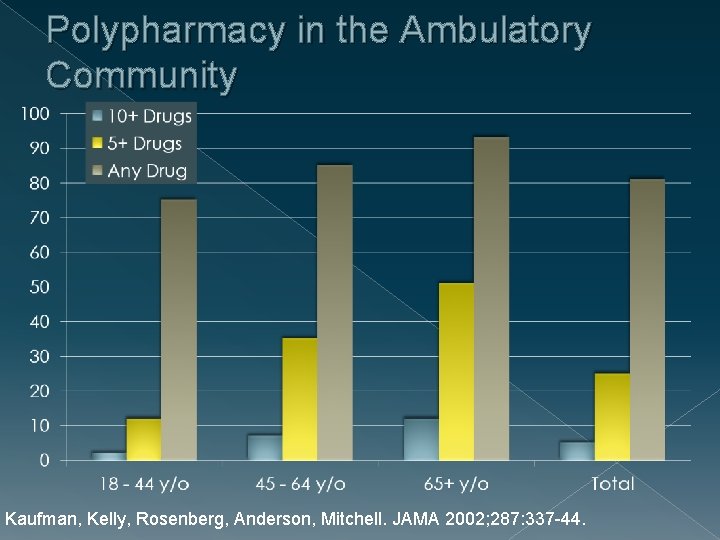
Polypharmacy in the Ambulatory Community Kaufman, Kelly, Rosenberg, Anderson, Mitchell. JAMA 2002; 287: 337 -44.

Post Discharge Medications in 65+ year olds Mean number of meds per patient = 13. 5 Nearly a quarter had >16 meds OR 4. 75 (95% CI: 1. 0 – 11. 2) for polypharmacy with 2+ high risk diagnoses › COPD, CA, DM, CHF, CAD Rohrer JE et al. J Prim Care Community Health. 2013 Apr 1; 4(2): 101 -5.
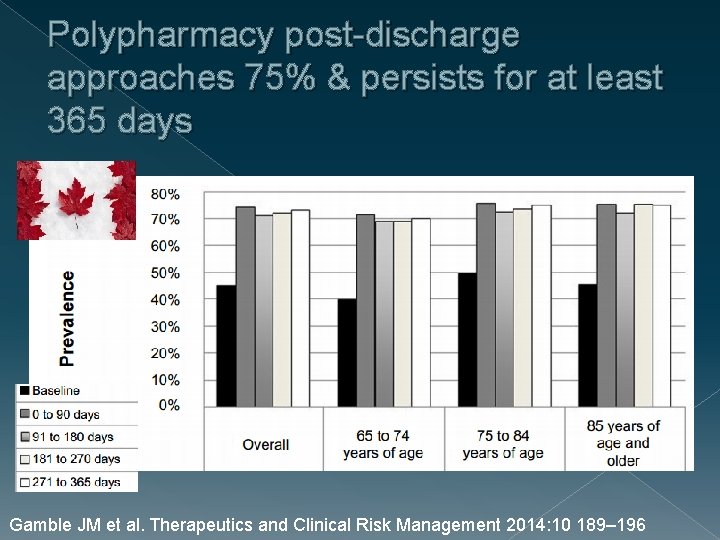
Polypharmacy post-discharge approaches 75% & persists for at least 365 days Gamble JM et al. Therapeutics and Clinical Risk Management 2014: 10 189– 196
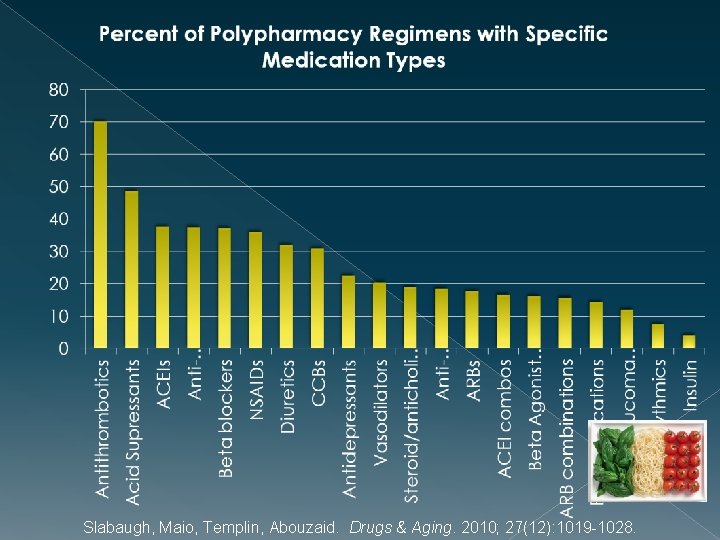
Slabaugh, Maio, Templin, Abouzaid. Drugs & Aging. 2010; 27(12): 1019 -1028.

Illustrate Why Recognition and Management of Polypharmacy is Important

drugs
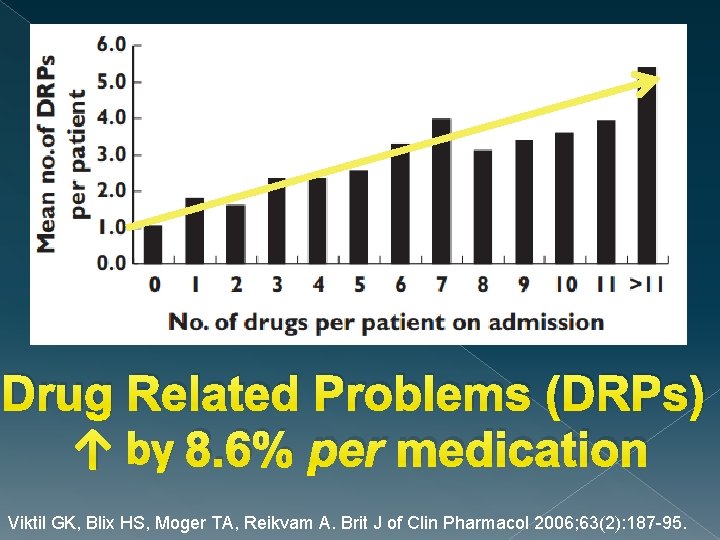
Drug Related Problems (DRPs) ↑ by 8. 6% per medication Viktil GK, Blix HS, Moger TA, Reikvam A. Brit J of Clin Pharmacol 2006; 63(2): 187 -95.

Examples of Drug Related Problems � Errors › Prescribing › Dispensing › Administration Adverse Reactions � Interactions � › Drug-Drug �Dynamic �Kinetic › Drug-Disease Order clarification necessary � Duplicate medication/class � Medication omission � Lack of dose adjustment with AKI or liver failure �
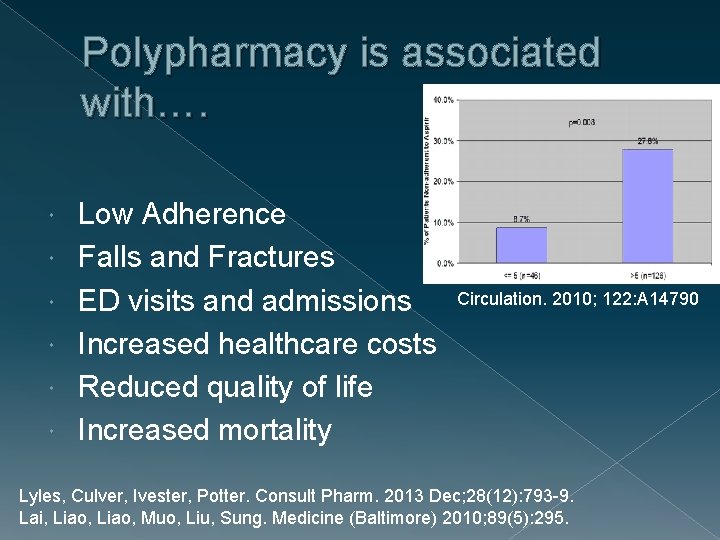
Polypharmacy is associated with…. Low Adherence Falls and Fractures ED visits and admissions Increased healthcare costs Reduced quality of life Increased mortality Circulation. 2010; 122: A 14790 Lyles, Culver, Ivester, Potter. Consult Pharm. 2013 Dec; 28(12): 793 -9. Lai, Liao, Muo, Liu, Sung. Medicine (Baltimore) 2010; 89(5): 295.
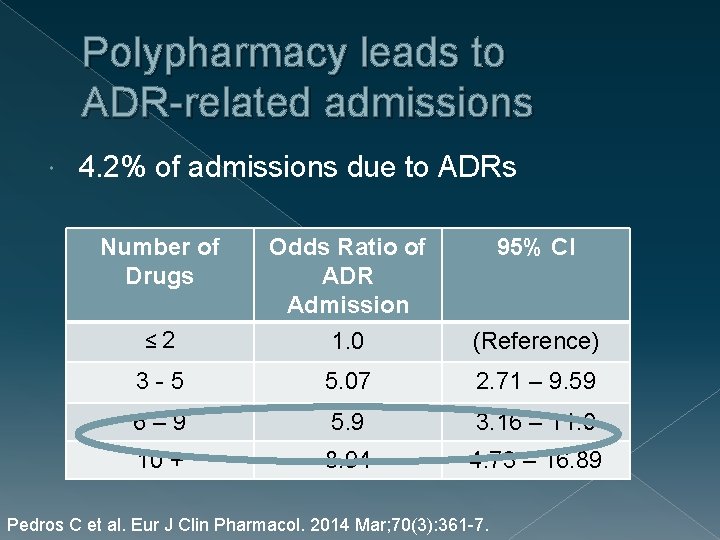
Polypharmacy leads to ADR-related admissions 4. 2% of admissions due to ADRs Number of Drugs Odds Ratio of ADR Admission 95% CI ≤ 2 1. 0 (Reference) 3 - 5 5. 07 2. 71 – 9. 59 6 – 9 5. 9 3. 16 – 11. 0 10 + 8. 94 4. 73 – 16. 89 Pedros C et al. Eur J Clin Pharmacol. 2014 Mar; 70(3): 361 -7.
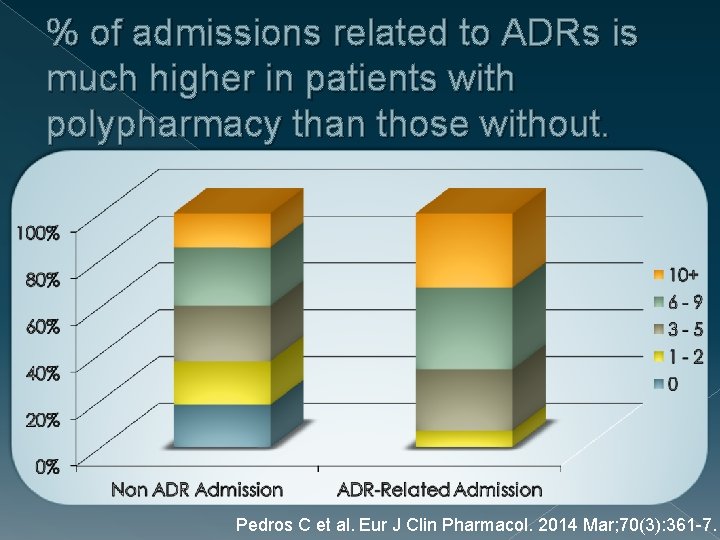
% of admissions related to ADRs is much higher in patients with polypharmacy than those without. Pedros C et al. Eur J Clin Pharmacol. 2014 Mar; 70(3): 361 -7.

Demonstrate Strategies to Avoid Polypharmacy

STEPS on the Path to Successful Pharmacotherapy Safety Tolerability Effectiveness Price Simplicity
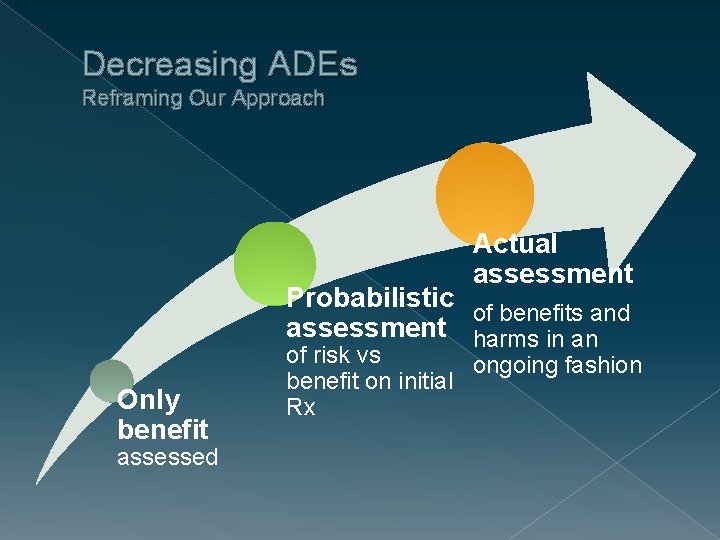
Decreasing ADEs Reframing Our Approach Actual assessment Probabilistic of benefits and assessment harms in an Only benefit assessed of risk vs ongoing fashion benefit on initial Rx
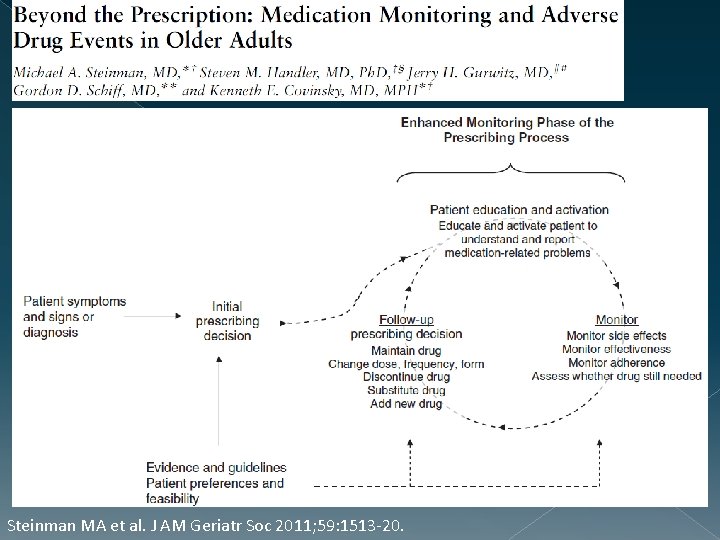
Steinman MA et al. J AM Geriatr Soc 2011; 59: 1513 -20.

Assess High Risk Polypharmacy Situations & Formulate a Plan to Initiate Pharmacological Debridement
2003 Pocket Card › http: //www. americangeriatrics. org/files/document s/beers/Printable. Beers. Pocket. Card. pdf AGS i. Geriatrics App - $2. 99

STOPP & START Criteria STOPP - Screening Tool of Older People’s potentially inappropriate Prescriptions › 65 recommendations START - Screening Tool to Alert doctors to the Right Treatment › 22 recommendations http: //www. ngna. org/_resources/documentation/chapter/ carolina_mountain/STARTand. STOPP. pdf Gallagher P, Ryan C, Byrne S, Kennedy J, O'Mahony D. Int J Clin Pharmacol Ther. 2008 Feb; 46(2): 72 -83.

Assess the Anticholinergic Burden • • Rudolph, Salow, Angelini, Mc. Glinchey. Arch Intern Med. 2008; 168(5): 508. Carnahan, Lund, Perry, Pollock, Culp. J Clin Pharmacol 2006; 46: 1481 -6. Boustani, Campbell, Munger, Maidment, Fox. Aging Health 2008; 4: 311 -20. http: //www. indydiscoverynetwork. org/resources/antichol_burden_scale. pdf

Match Drugs and Problems Find an indication for each drug › Goal of therapy? Are we using the best drug for each problem/disease/disorder in this patient? › Eg. HTN and beta blockers

Compare the Actual Medications to the Medication List Schedule a “brown bag” appointment periodically

Include the Pharmacist When switching from one agent to another, or stopping an agent completely… …ask the community pharmacy to d/c the old prescription Periodically compare medication lists with the pharmacist/pharmacy

New Symptoms or ADRs? When new symptoms emerge, particularly in geriatric patients, think about medication AEs

Employ Strategies to Improve Medication Adherence in Patients With a High Pill Burden
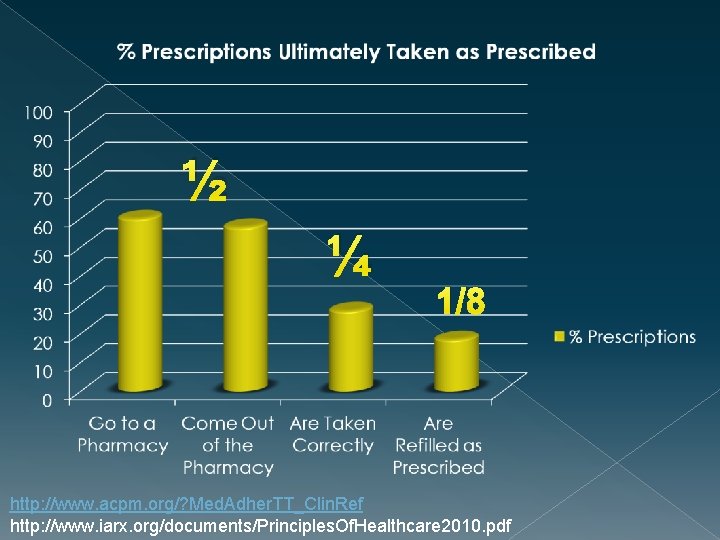
½ ¼ 1/8 http: //www. acpm. org/? Med. Adher. TT_Clin. Ref http: //www. iarx. org/documents/Principles. Of. Healthcare 2010. pdf

Keep it SIMPLE S implify regimen I mpart knowledge M odify patient beliefs and human behavior P rovide communication and trust L eave the bias E valuate adherence Atreja A, Bellam N, Levy S. Medacapt Gen Med. 2005: 7(1): 4.

Simplify the Regimen Daily or BID dosing › One-a-day formulations (incl. patches) › Match to ADLs (ex. breakfast) Combination products › Caution: loss of dosing flexibility Treat multiple conditions with one agent › Caution: commonly 2 agents are safer d/c extraneous or unnecessary medications

Impart Knowledge Focus on shared decision making Discuss purposes and side effects of medications Use the teach-back method Employ verbal and written instructions Give contact information for further questions

Gauge Health Literacy & Avoid Ambiguity REALM Assessment › http: //www. adultmeducation. com/downloads/REA LMR_INSTR. pdf “As Needed for Water Retention” “Take two every day”

Active and Ongoing Discussion About Pharmacotherapy Presentation of the advantages and disadvantages of each medication in a way that is understandable to your patient Discuss # of missed doses at each visit, nonpunitively Telephone counselling

Motivational Interviewing Empathy, supporting self-efficacy, avoiding argumentation, rolling with resistance, and developing discrepancy PSAPs VII; Book 8. Motivational Interviewing. Kavookjian J.

Modify Behaviors Empower patients to self-manage Ask about specific needs, fears, and concerns Identify perceived barriers (ex. financial) Ensure knowledge of the actual risks of missing medications

Provide Communication Confirm your patient’s message and paraphrase it Provide empathy and give feedback Involve your patient in decision making Use plain language and confirm understanding

Leaving the Bias Take the time to overcome cultural barriers Tailor education to the appropriate level of complexity for your patient’s optimal understanding

Evaluating Adherence Ask direct questions and ask them often › Every visit Identify adherence barriers Recognize lack of perceived benefit

Medication Possession Ratio � 30 day fills on Jan 1 st, Feb 7 th, Mar 18 th, Apr 26 th, & June 1 st 5 fills * 30 d each = 150 days supply Jan 1 st – Jun 1 st = 151 days + 30 days supply = 181 days 150/181 = 83% MPR

Adherence Tools and Tricks Wallet cards – medication lists Pill containers and counting Blister packs Pre-packed kits (ex. Medrol) Textured covers with vision impairment Alarms › On the bottle › Via email Team based care!

Polypharmacy and Adherence in Psychiatric Patients Consider Long-Acting Injectable Antipsychotics Engage the patient in the treatment decision when able, particularly regarding AEs Ask the pharmacist to partner with the treatment team to alert of non-timely filling

Psychiatric Patients and Adherence Depressed patients are 3 x more likely to be non-adherent with medical treatment regimens (non psychotropic) Di. Matteo MR, Lepper HS, Croghan TW. Arch Int Med. 2000; 160(14): 2101.

Take Home Points Polypharmacy is prevalent, particularly in those 65+ Polypharmacy increases morbidity, mortality, & healthcare costs, and decreases quality of life Perform ongoing medication assessment with tools, like STEPS, to avoid polypharmacy Use scores, scales, and lists to optimize medication regimens, avoid unnecessary medications, and/or reduce medication burden To improve medication adherence in polypharmacy, simplify the medication regimen and have ongoing dialogue with your patient about risks and benefits of each drug being used

Thank you!! Stephanie Nichols, Pharm. D. , BCPS, BCPP Associate Professor, Husson University School of Pharmacy Clinical Psychiatric Pharmacist, Maine Medical Center Nichols. S@Husson. edu
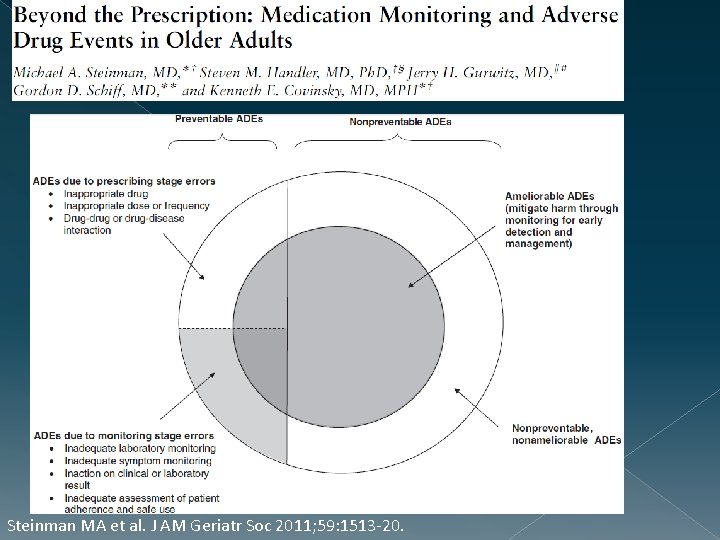
Steinman MA et al. J AM Geriatr Soc 2011; 59: 1513 -20.
- Slides: 47