A NOVEL SUBSPECIALTY MEDICAL HOME PROGRAM FOR INDIVIDUALS

A NOVEL SUBSPECIALTY MEDICAL HOME PROGRAM FOR INDIVIDUALS WITH NEURODEVELOPMENTAL DISABILITIES: PART 1: STRUCTURE AND OUTCOMES BY DEBORAH BILDER, MD. ASSOCIATE PROFESSOR, DEPARTMENT OF PSYCHIATRY, DIVISION OF CHILD & ADOLESCENT PSYCHIATRY ADJUNCT ASSOCIATE PROFESSOR, DEPARTMENTS OF PEDIATRICS AND EDUCATIONAL PSYCHOLOGY MEDICAL DIRECTOR, NEUROBEHAVIOR HOME PROGRAM MEDICAL DIRECTOR, AUTISM SPECTRUM DISORDER CLINIC UNIVERSITY OF UTAH ©UNIVERSITY OF UTAH HEALTH,

DISCLOSURES • Consultant, advisory board and steering committee member for Bio. Marin Pharmaceuticals • Consultant and scientific and clinical advisors board member for Audentes Therapeutics

OVERVIEW • Intro to HOME • Role of a subspecialty medical home • Advancing clinical care through research

NEUROBEHAVIOR HOME PROGRAM • A novel, Medicaid-funded medical home model for patients with developmental disabilities throughout their lifespan • provides primary care and behavioral health care in one setting • A financially viable University-based multidisciplinary clinic • Over 1100 enrollees • Created by Josette Dorius, RN, MPH and Scott Stiefel, MD in 2000.

THE MEDICAL HOME • An approach to providing comprehensive primary care • Defined as primary care is: – Continuous --Accessible – Culturally effective --Coordinate -- Compassionate --Comprehensive -- Family-centered • Improves patient outcomes

FISCALLY VIABLE FUNDING IN A NUTSHELL • Combine capitated medical and behavior health funds from Medicaid • Co-locate medical and behavior health outpatient services • Serve Medicaid’s most expensive patient population • Provide preventative and proactive outpatient care to reduce one of the most costly components of care for this population – psychiatric hospitalizations

MANAGING OUTBURSTS • By recognizing agitation as a final common final pathway for many underlying causes rather than the treatment target itself, HOME provides a fiscal viability way of optimizing health and functioning, living in the community ©UNIVERSITY OF UTAH HEALTH,

PERSON-CENTERED APPROACH • Design of services for individuals with diverse needs and desires. • Each person, regardless of ability, is worthy of respect. • Our clients with developmental disabilities have the right to set their own goals and objectives to the best of their ability.

HOME STRUCTURE • • Case Management: communication facilitators – with families, within clinic, with outside specialists, hospitals, community agencies Medical: pediatrics, family medicine, nurse practitioners, nutritionist – Outpatient visits, immunizations, phlebotomy, EKG, nutrition group • Behavioral health services: triple board/psychiatrists, nurse practitioners, therapists, behaviorists, – Individual/group sessions, feeding clinic, in-home intensive support • “Sister” program – Autism Spectrum Disorder Clinic – Specialty psychological evaluations, early intervention, social skills group • 60 employees

INDIVIDUAL THERAPY

IDENTIFYING COMORBID CONDITIONS • Physical discomfort (pain) • Medical condition (metabolic disorder, endocrine, seizure disorder, sleep disorder) • Medication side effect • Functional Behaviors (behaviors which “work” for the child) • Social stressors • Psychiatric disorder
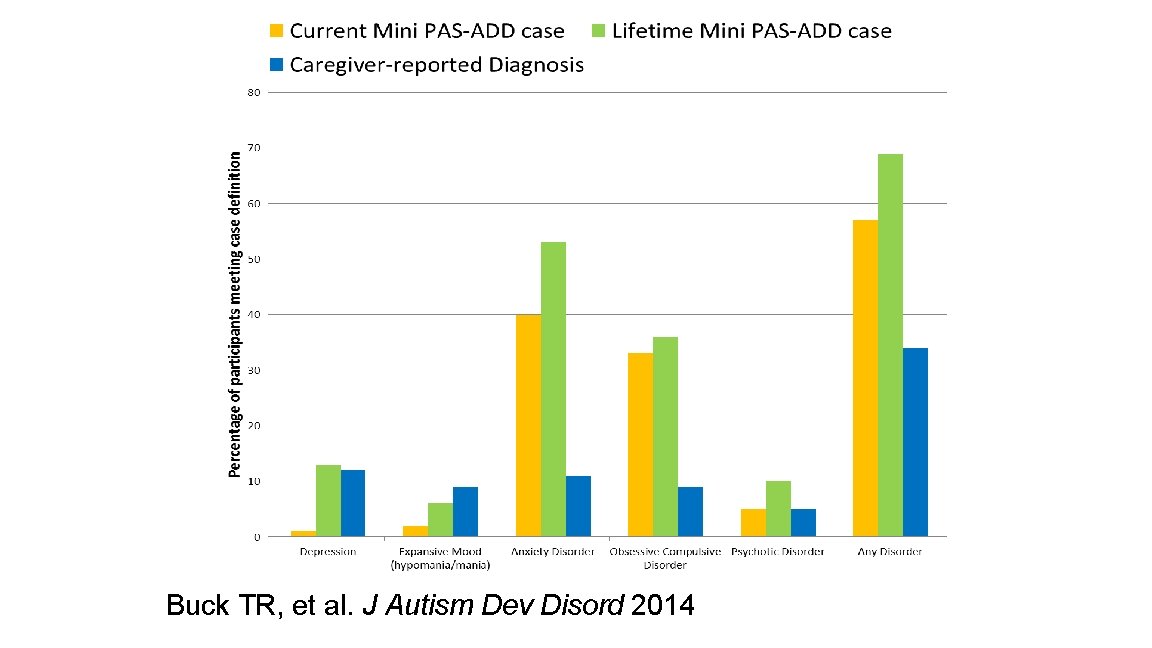
Buck TR, et al. J Autism Dev Disord 2014

TEAM APPROACH • One-hour visits with clients, their caregivers, and their providers to get to the source of our client’s distress.

MORTALITY IN AUTISM SPECTRUM DISORDER • N=305 Utah adults with ASD, 73% with co-occurring ID • 9. 5% (n=29) died during follow-up period • 9. 9 (CI 5. 7 -17. 2) Hazard rate ratio U N I V E RDev S I T Y Disord O F U T A 2012 H HEALTH, Bilder, et al. J©Autism

RESEARCH ©UNIVERSITY OF UTAH HEALTH,

ANTIPSYCHOTIC USE IN HOME • 60. 4% taking antipsychotic medication – More likely to be taking medication • Males • Intellectual disabilities • Co-occurring intellectual disabilities and ASD – Less likely to be taking medication • Ages 4 -14 years • Ages >60 years • Triple insurance coverage
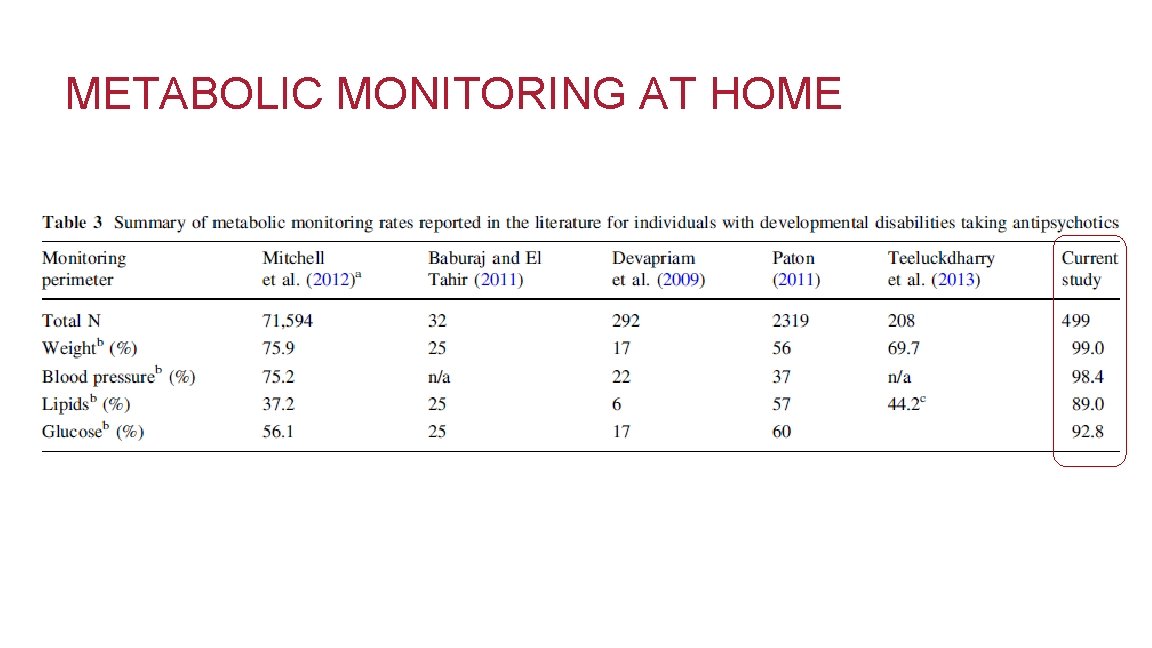
METABOLIC MONITORING AT HOME

BIG PICTURE • Subspecialty HOME Program provides a fiscally viable means of taking good care of medically and behaviorally challenging patients • Person-centered approach is a respectful and effective means of reducing disruptive behavior • Blending research and clinical care allows us to share what our clients teach us with our collective community of providers, caregivers, and individuals with neurodevelopmental disabilities

ACKNOWLEDGEMENTS • HOME Program Team • Our enrollees and their families ©UNIVERSITY OF UTAH HEALTH,

PSYCHIATRIC COMORBIDITY IN ASD Without ID With ID • • • Any diagnosis 80 -99% Anxiety 50 -56% Depression 45 -70% Bipolar 8 -9% Psychotic Disorder 412% Substance dependence 7 -16% OCD 24% • • Any diagnosis 35 -48% Anxiety 4 -8% Depression 6 -20% Bipolar 11% Psychotic Disorder 618% Tourette 2 -4% Catatonia 12% Lugnegard 2011, Hofvander 2009, Morgan 2003, Billstedt 2005, Melville 2008
- Slides: 20