A More Perfect Union Better Health Better Care

A More Perfect Union: Better Health; Better Care; Lower Costs through Improvement Jean D. Moody-Williams, RN, MPP Director, Quality Improvement Group

2

3

4

5

6

7

8

2012 Quote Collaboration is Hard Work! 9

Characteristics of a Learning Organization • It should review data and respond to it - with tests of new solutions and ideas - every week. • It should bring all participating sites together by phone, in person or webinar frequently • It should set one or two quantifiable, project-level goals, with a deadline, preferably defined in terms of outcomes, related to the project’s area of work. • It should invest more in learning than in teaching. 10

Characteristics of a Learning Organization • It should employ regional “innovator agents • It should celebrate success • It should use metrics to measure its success such as: – Rate of testing – Rate of spread – Time from idea to full implementation – Commitment rate (rate at which 50% of organizations take action for any specific request) – Number of questions asked per day – Network affinity/reported affection for the network – 11

Operating Values for Change • Rapid Cycle Improvement in Quality Improvement Activities and Outputs • Customer Focus and Value of the Quality Improvement Activities • Ability to Prepare the Field to Sustain the Improvements • Valuing Innovation • Commitment to “Boundarilessness” • Unconditional Teamwork • Commitments Secured/Participants Engaged/Results toward Achieving Targets 12

Measuring Progress Towards Goals 1. Track national progress towards the program goals; 2. Support local quality improvement measurement; 3. Obtain feedback on progress, in close to real time, so the project can be effectively managed; and 4. Evaluate the program’s impact on achieving stated goals. J Patient Saf - Volume 8, 2012: Hackbarth et. Andrew D. Hackbarth 1, MPhil, William B. Munier 2, MD, MBA, Noel Eldridge 2, MS, Jack Jordan 1, MS, Chesley Richards 3, MD, MPH, Niall J. Brennan 1, Ph. D , Dennis Wagner 1, MPA, Paul Mc. Gann 1, MD 13
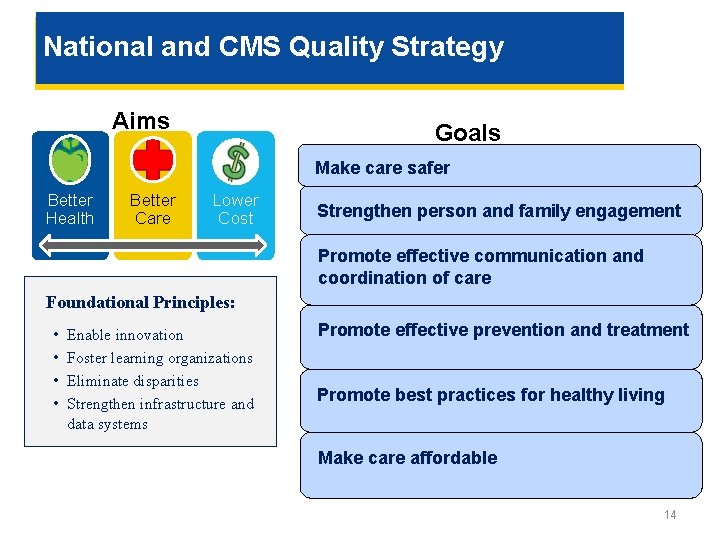
National and CMS Quality Strategy Aims Goals Make care safer Better Health Better Care Lower Cost Strengthen person and family engagement Promote effective communication and coordination of care Foundational Principles: • • Enable innovation Foster learning organizations Eliminate disparities Strengthen infrastructure and data systems Promote effective prevention and treatment Promote best practices for healthy living Make care affordable 14

15
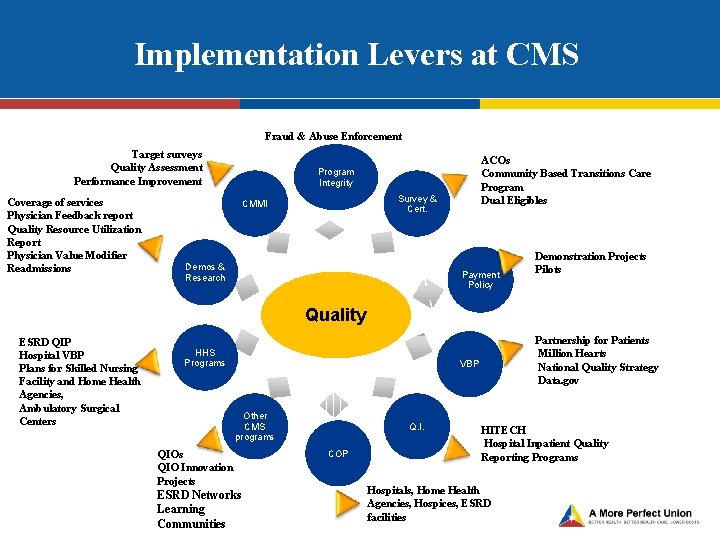
Implementation Levers at CMS Fraud & Abuse Enforcement Target surveys Quality Assessment Performance Improvement Coverage of services Physician Feedback report Quality Resource Utilization Report Physician Value Modifier Readmissions ACOs Community Based Transitions Care Program Dual Eligibles Program Integrity Survey & Cert. CMMI Demos & Research Payment Policy Demonstration Projects Pilots Quality ESRD QIP Hospital VBP Plans for Skilled Nursing Facility and Home Health Agencies, Ambulatory Surgical Centers HHS Programs Partnership for Patients Million Hearts National Quality Strategy Data. gov VBP Other CMS programs QIO Innovation Projects ESRD Networks Learning Communities Q. I. COP HITECH Hospital Inpatient Quality Reporting Programs Hospitals, Home Health Agencies, Hospices, ESRD facilities

Improving Individual Patient Care January 31, 2013
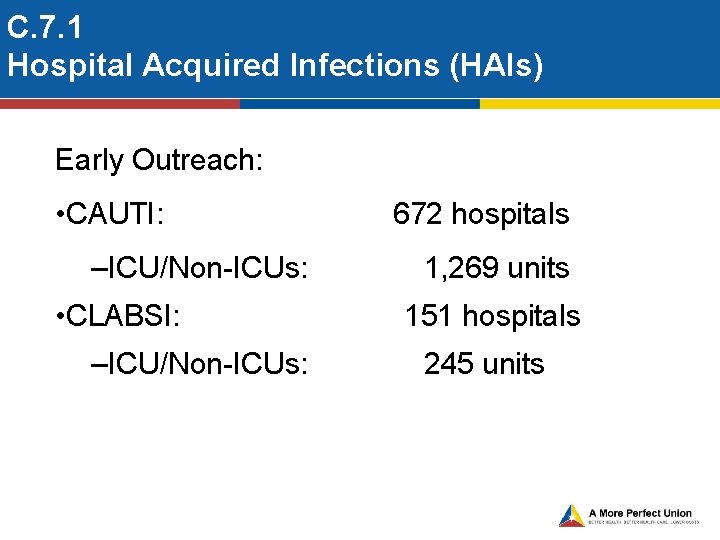
C. 7. 1 Hospital Acquired Infections (HAIs) Early Outreach: • CAUTI: –ICU/Non-ICUs: • CLABSI: 672 hospitals 1, 269 units 151 hospitals –ICU/Non-ICUs: 245 units
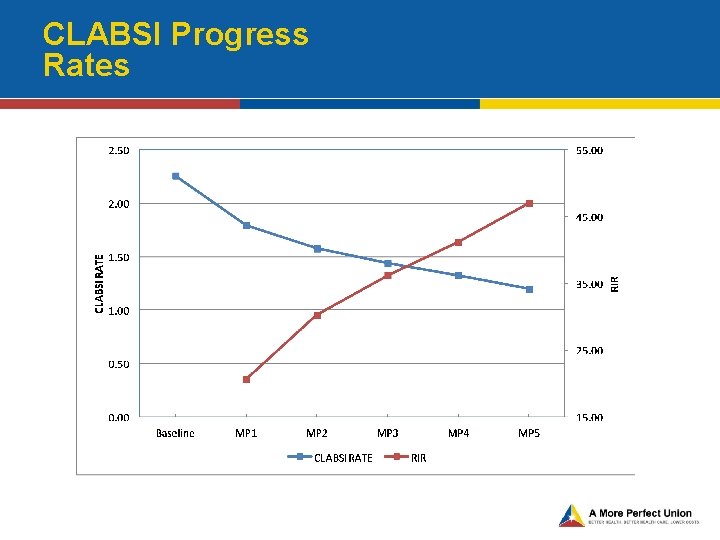
CLABSI Progress Rates
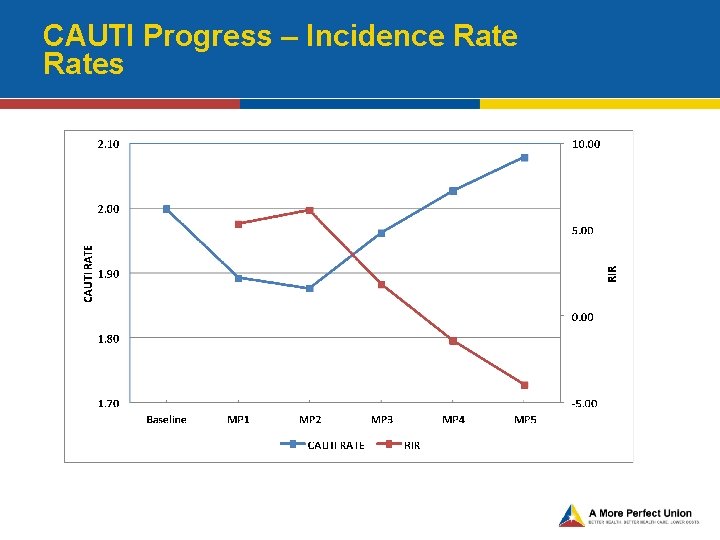
CAUTI Progress – Incidence Rates

Reason for Increased CAUTI rates • The reason behind the increase in national CAUTI SIR figures appears to be multifactorial: • New Reporters into NHSN: • The CMS IPPS rule in January 2012, which coincided with the first two quarters of this goal, added ~2, 000 new CAUTI reporters into NHSN. • Many of these hospitals had higher CAUTI SIRs increasing the aggregate SIR figure. • Better Reporters: • Widespread outreach and education efforts of CDC throughout 2012 to improve accuracy in reporting would reduce underreporting errors and contribute to increase in CAUTI figures. • Reducing Catheter Use: • Reducing urinary catheter use decreases the denominator in the SIR calculation making it more difficult to show reductions in the SIR. • The need for more aggressive implementation of infection prevention strategies: • Increased implementation of infection control and prevention methods consistently applied within a system that is dedicated to a culture of safety is needed to further impact CAUTI reductions on a wide scale.
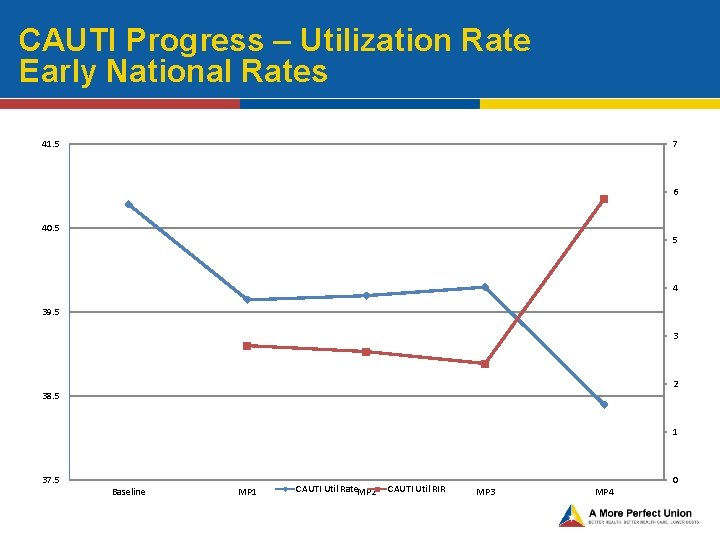
CAUTI Progress – Utilization Rate Early National Rates 41. 5 7 6 40. 5 5 4 39. 5 3 2 38. 5 1 37. 5 Baseline MP 1 CAUTI Util Rate. MP 2 CAUTI Util RIR 0 MP 3 MP 4
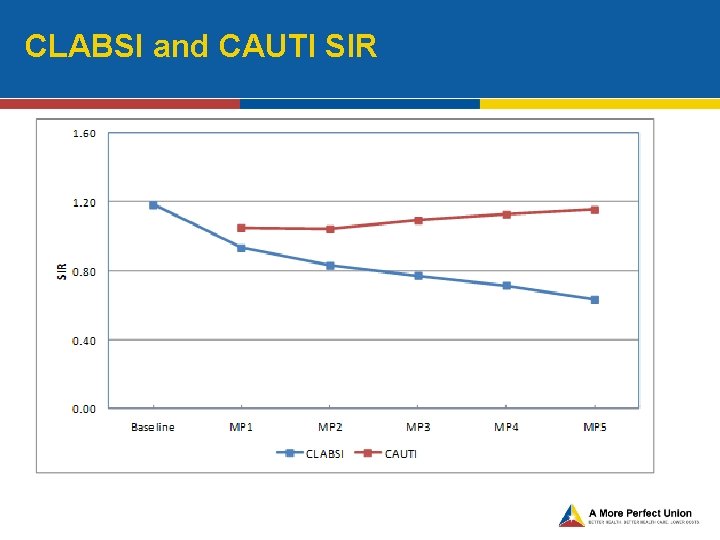
CLABSI and CAUTI SIR

Collaboration Example • COLLABORATION provides the opportunity to share both evidencebased infection prevention strategy and data-driven results on a broader scale. – CMS continues to lead regular interagency meetings to ensure continued knowledge and coordination between the 10 th SOW QIO and Pf. P’s HEN contractor efforts at the state, local and facility-level. – In working to promote CUSP principles nationwide, AHRQ’s contractor for the CUSP for CAUTI project, and QIOs are contractually obligated to work together to educate recruited facilities on principles of CUSP. – CDC continues to work closely with state HAI coordinators to accelerate prevention efforts at the state level. CDC’s most recent funding opportunity announcement sets forth that one of the primary responsibilities of an HAI coordinator is to ensure coordination of state-based prevention initiatives (e. g. CUSP, QIO, Partnership for Patients) and facilitate connections with leads of the various federally-supported prevention efforts. 24
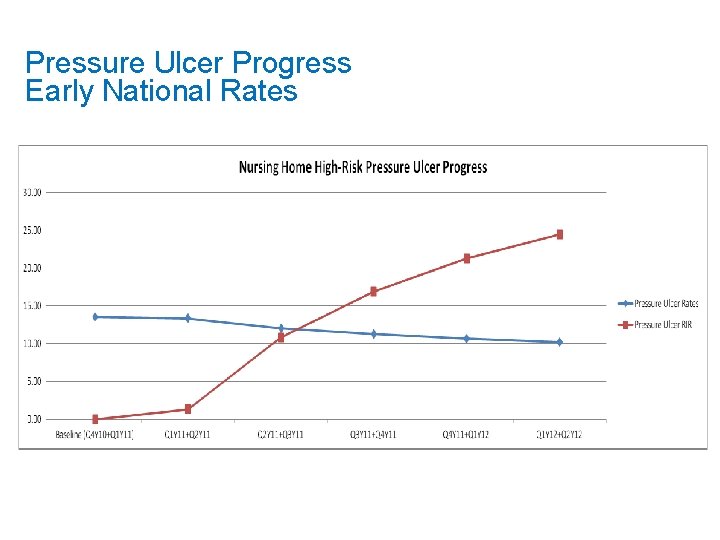
Pressure Ulcer Progress Early National Rates
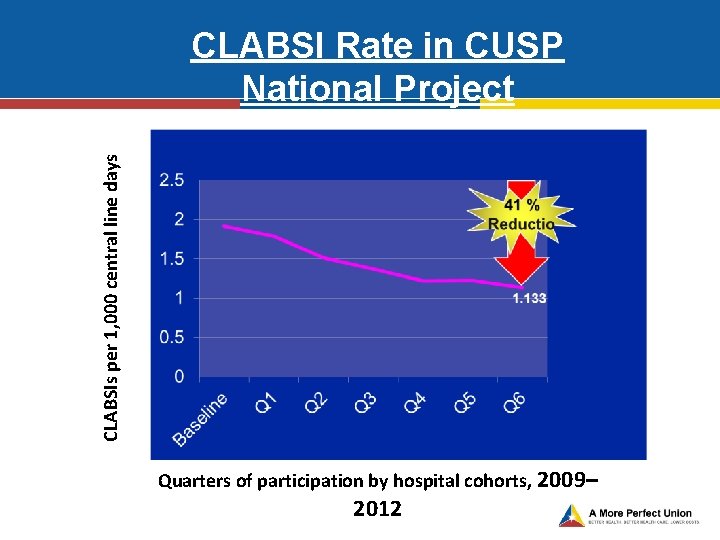
CLABSIs per 1, 000 central line days CLABSI Rate in CUSP National Project Quarters of participation by hospital cohorts, 2009– 2012
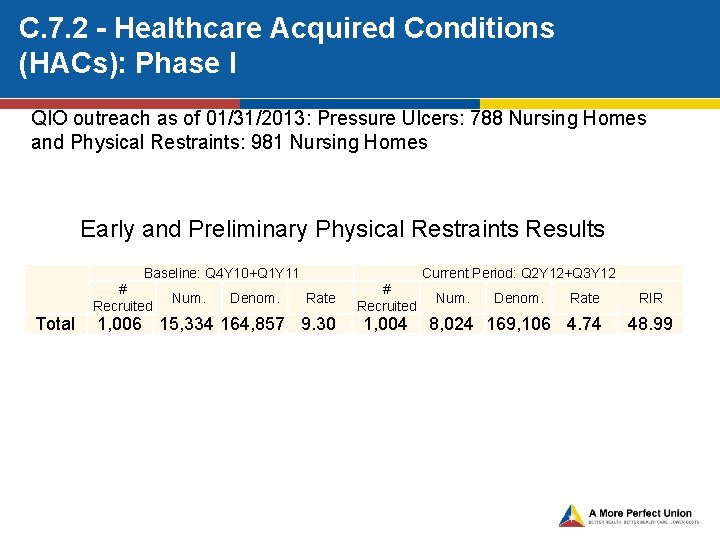
C. 7. 2 - Healthcare Acquired Conditions (HACs): Phase I QIO outreach as of 01/31/2013: Pressure Ulcers: 788 Nursing Homes and Physical Restraints: 981 Nursing Homes Early and Preliminary Physical Restraints Results Baseline: Q 4 Y 10+Q 1 Y 11 # Recruited Num. Denom. Current Period: Q 2 Y 12+Q 3 Y 12 Rate Total 1, 006 15, 334 164, 857 9. 30 # Recruited 1, 004 Num. Denom. Rate 8, 024 169, 106 4. 74 RIR 48. 99

National Nursing Home Quality of Care Collaborative (NNHQCC); Phase II High Performing Nursing Home site visits (10) completed by November 2012 Recruitment by January 31, 2013: Over 4, 208 nursing homes NNHQCC LAN Event activities start February 26, 2013 Change Package finalized and shared with QIOs and homes
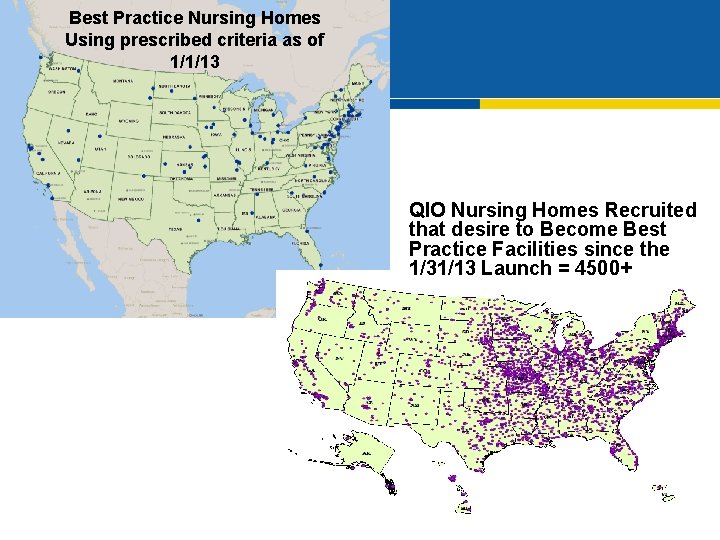
Best Practice Nursing Homes Using prescribed criteria as of 1/1/13 QIO Nursing Homes Recruited that desire to Become Best Practice Facilities since the 1/31/13 Launch = 4500+

Reducing Adverse Drug Events QIO/PSPC Teams on 01/31/2013: over 215 teams Anti-coagulant focus only: 36 teams Diabetic focus only: 43 teams Anti-psychotic focus: 42 teams Multi-focus: 62 teams
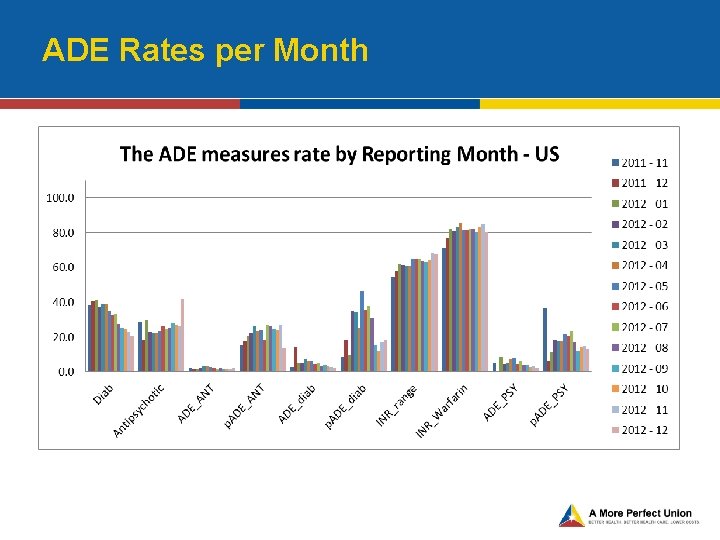
ADE Rates per Month

Quality Reporting and Incentives Highlights • 97% of hospitals successfully report data to the Hospital Inpatient Quality Reporting (IQR) Program • Intensive support to providers experiencing difficulty reporting new measures such as NHSN measures • Successful first year for the Hospital Value Based Purchasing (VBP) Program, with over $900 million redistributed based on quality based on IQR data
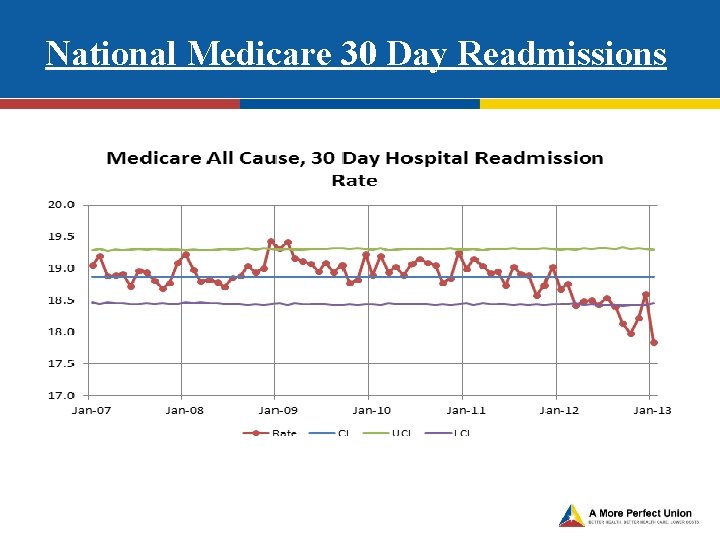
National Medicare 30 Day Readmissions

Innovation Center Initiatives Support Care Transformation • • • ACO Initiatives: Shared Savings Program, Pioneer, Advance Payment, Learning Sessions Bundled Payments for Care Improvement Innovation Advisors Program Multi-Payer Advanced Primary Care Practice Demonstration Comprehensive Primary Care Initiative Partnership for Patients Federally Qualified Health Center (FQHC) Advanced Primary Care Practice Demonstration Medicaid Health Home State Plan Option State Demonstrations to Integrate Care for Dual Eligible Individuals Demonstration to Improve Quality of Care for Nursing Facility Residents Financial Models to Support State Efforts to Coordinate Care for Medicare-Medicaid Enrollees 34

Hospital Readmissions from Post Acute Care (PAC) Settings CMS work in Progress for PAC settings, over Next Year: § Developing 30 -day Readmission Quality Measures for NHs, LTCHs, IRFs. § Key Considerations from Technical Expert Panels: § Risk Adjustment may need to vary by provider setting, population. Various models to consider. § Planned Readmissions exclusions? Reasons/diagnoses may vary by provider setting. § 30 -day Readmission Measurement Period: Could cover the 30 days after hospital discharge. Could have separate measure to cover the 30 days after PAC discharge. 35

PAC Readmission: Other CMS Targeting Strategies • CMS is currently updating the surveyor interpretive guidance for transfer and discharge planning regulations • New regulations are being developed to establish Quality Assurance and Performance Improvement (QAPI) programs in all CMS-certified nursing homes. 36

It Worked!! http: //jama network. com/arti cle. aspx? articlei d=1558278
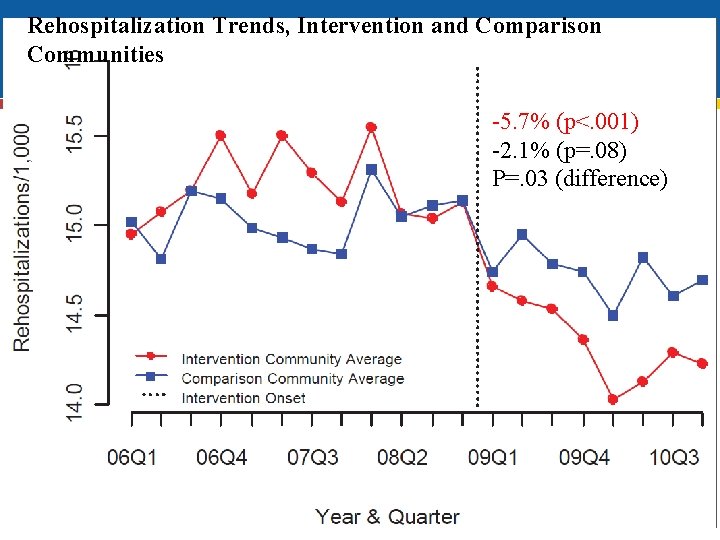
Rehospitalization Trends, Intervention and Comparison Communities -5. 7% (p<. 001) -2. 1% (p=. 08) P=. 03 (difference)
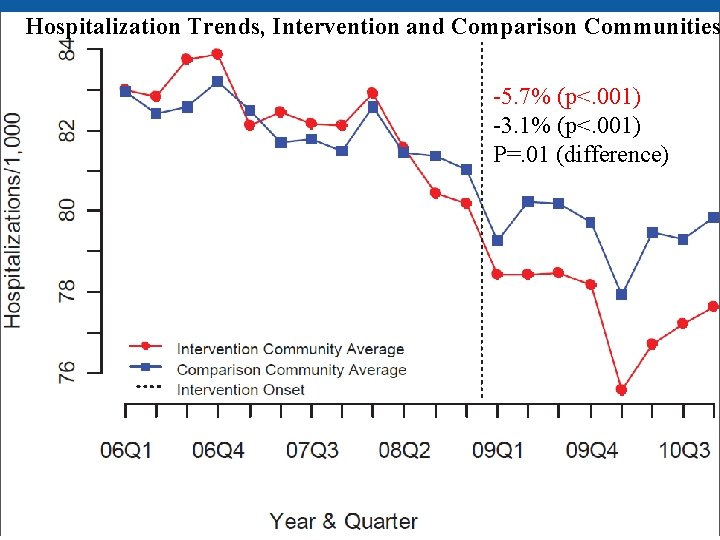
Hospitalization Trends, Intervention and Comparison Communities -5. 7% (p<. 001) -3. 1% (p<. 001) P=. 01 (difference)
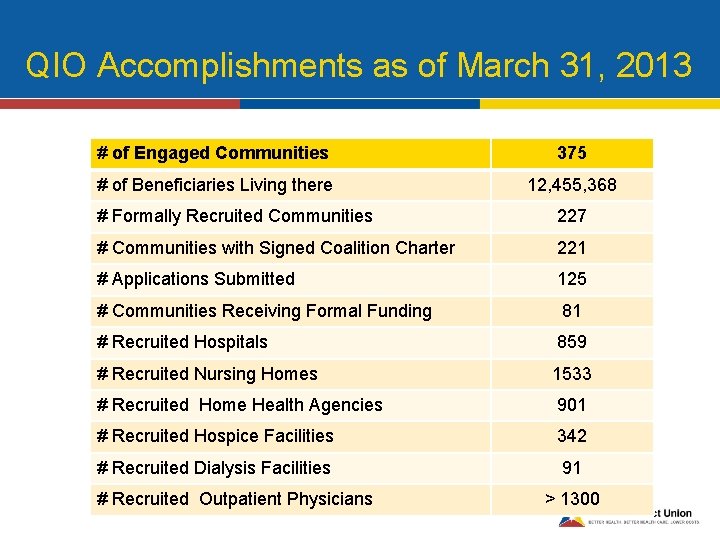
QIO Accomplishments as of March 31, 2013 # of Engaged Communities 375 # of Beneficiaries Living there 12, 455, 368 # Formally Recruited Communities 227 # Communities with Signed Coalition Charter 221 # Applications Submitted 125 # Communities Receiving Formal Funding 81 # Recruited Hospitals 859 # Recruited Nursing Homes 1533 # Recruited Home Health Agencies 901 # Recruited Hospice Facilities 342 # Recruited Dialysis Facilities 91 # Recruited Outpatient Physicians > 1300
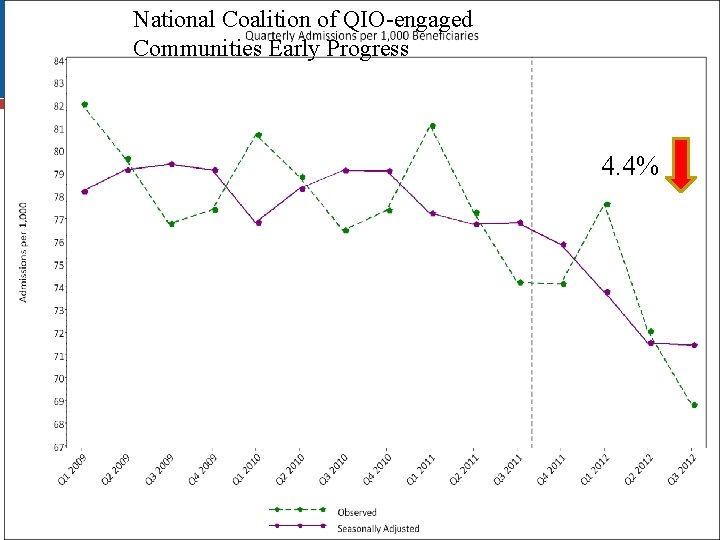
National Coalition of QIO-engaged Communities Early Progress 4. 4%
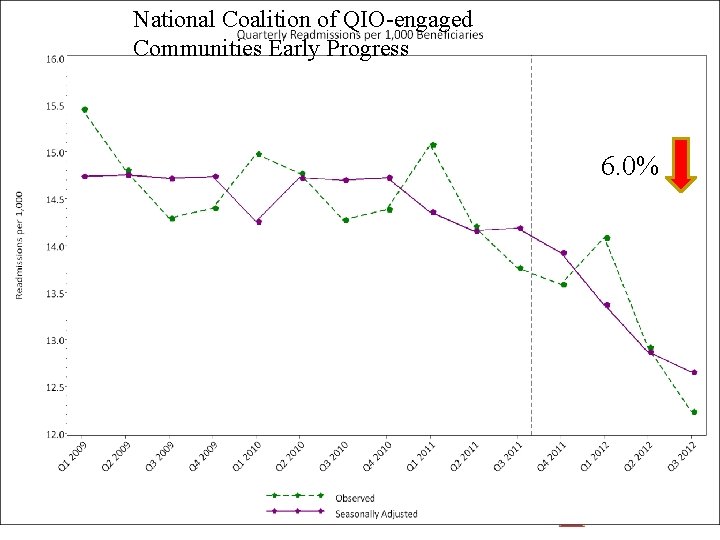
National Coalition of QIO-engaged Communities Early Progress 6. 0%
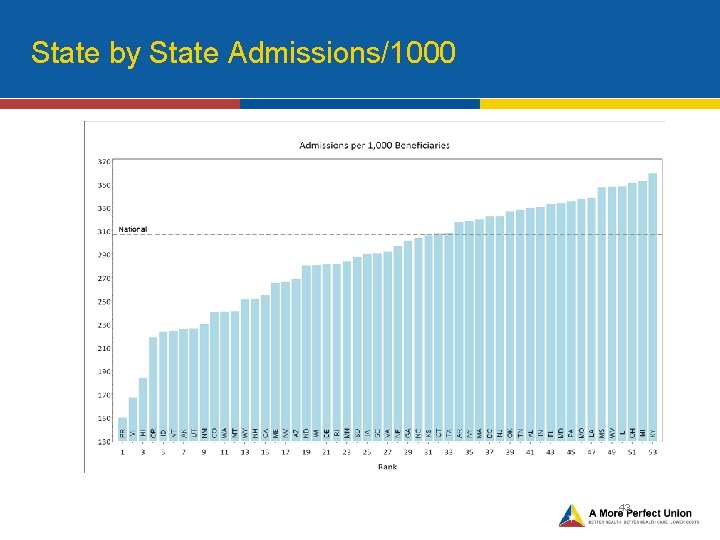
State by State Admissions/1000 43
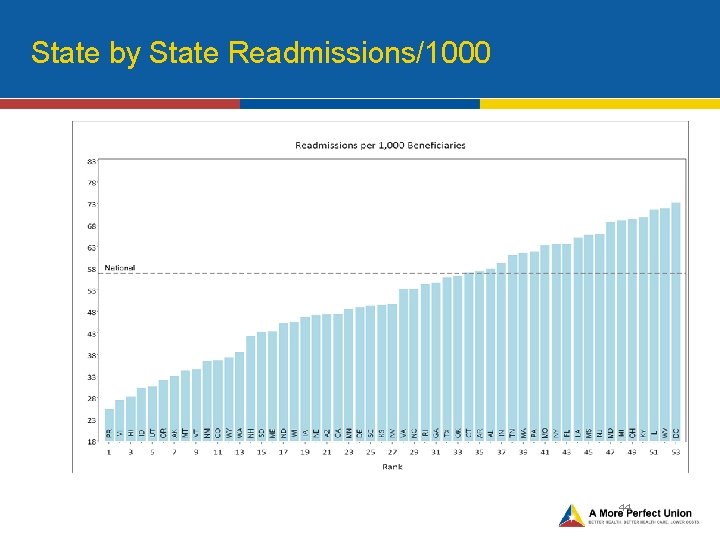
State by State Readmissions/1000 44
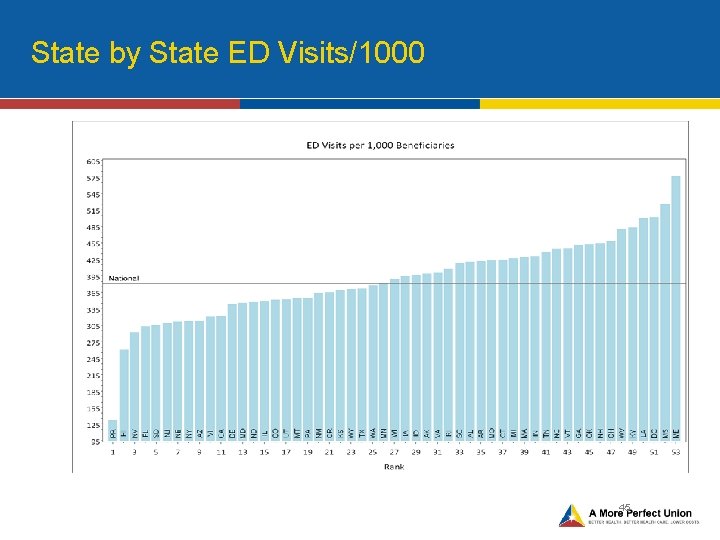
State by State ED Visits/1000 45
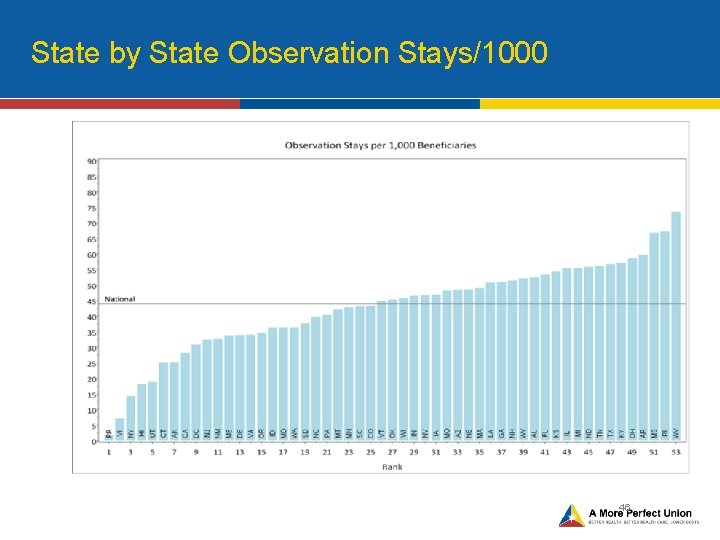
State by State Observation Stays/1000 46

ESRD Networks Continue to Make Progress Fistula First Catheter Last Graphs when necessary National AV Fistula Rate Reaches 60. 6% in April 2012 47

ESRD • Dialyisis Adequacy via URR – 96. 75% • Moving to Kt//V measuring hemodialysis, peritoneal dialysis and pediatric hemodialyis. • Working to develop better anemia management, bone and mineral metabolism, HAI measures and patient experience of care measures • Active involvement in care coordination to reduce hospital admissions • Exploring issues of volume, nutrition and quality of life • Beginning the second year of the ESRD QIP 48
Moving in the Right Direction Better Health 49 Better Care Lower Cost
- Slides: 49