A GUIDE TO OUTPATIENT MANAGEMENT OF VENOUS THROMBOEMBOLISM

A GUIDE TO OUTPATIENT MANAGEMENT OF VENOUS THROMBOEMBOLISM GAIL POKORNEY MD APRIL 2017

NO DISCLOSURES

LEARNING OBJECTIVES Review the initial treatment of venous thromboembolism (VTE) Duration of anticoagulation Choice of anticoagulant Use of additional devices, including IVC filters and compression stockings Provide guidance on long-term management of VTE Duration of anticoagulation Choice of anticoagulant Role of additional testing, including thrombophilia work-up and D-dimer

PATHOPHYSIOLOGY OF THROMBOSIS: VIRCHOW’S TRIAD Endothelial Injury Smoking Trauma Inflammatory disorders Surgery Catheters Thrombosis Immobility Abnormal Blood Flow Pregnancy & Hormones Hereditary thrombophilia APLS Cancer & Chemotherapy Hypercoagulability Streiff et al. J Thrombolysis. 2016; 41: 32 -67

SAMPLE VTE CASES Case 1: 50 y. M with DVT after orthopedic surgery Case 2: 50 y. M with unprovoked PE Case 3: 50 y. F with DVT in the setting of pancreatic cancer Case 4: 40 y. M with DVT in the setting of an IBD flare Case 5: 30 y. F with PE on OCPs

VTE MANAGEMENT OVERVIEW Initial treatment Long-term treatment Re-evaluation

CASE 1: POST-OPERATIVE DVT 50 y. M presents to the ER with RLE pain, swelling, erythema R total knee replacement 4 weeks ago U/S reveals a large proximal DVT Questions regarding initial treatment: Duration Choice of anticoagulant IVC filter Catheter-directed therapy Compression stockings

INITIAL TREATMENT: DURATION OF ANTICOAGULATION Initial length of treatment (months) 1. 0 or 1. 5 Bottom line: Treat for 3 months and then stop, unless indefinite anticoagulation is justified Probability of VTE compared with 3 months once therapy is stopped 12 to 27 15 4 -6 weeks is insufficient 6 -12 months does not lower recurrence rates 6 3 12 9 6 3 0 0 6 12 18 Months since stopping treatment Boutitie et al. BMJ. 2011; 342: d 3036 Kearon and Akl. Blood. 2014; 123(12): 1794 -1801 24

INITIAL TREATMENT: CHOICE OF ANTICOAGULANT DOAC First choice except in select populations Rivaroxaban and apixaban can be started immediately Dabigatran and edoxaban require 5 -10 day heparin lead-in Warfarin Requires heparin for 5 days or until INR is 2 -3, whichever is longer LMWH Gold standard in cancer-associated VTE Streiff et al. J Thrombolysis. 2016; 41: 32 -67
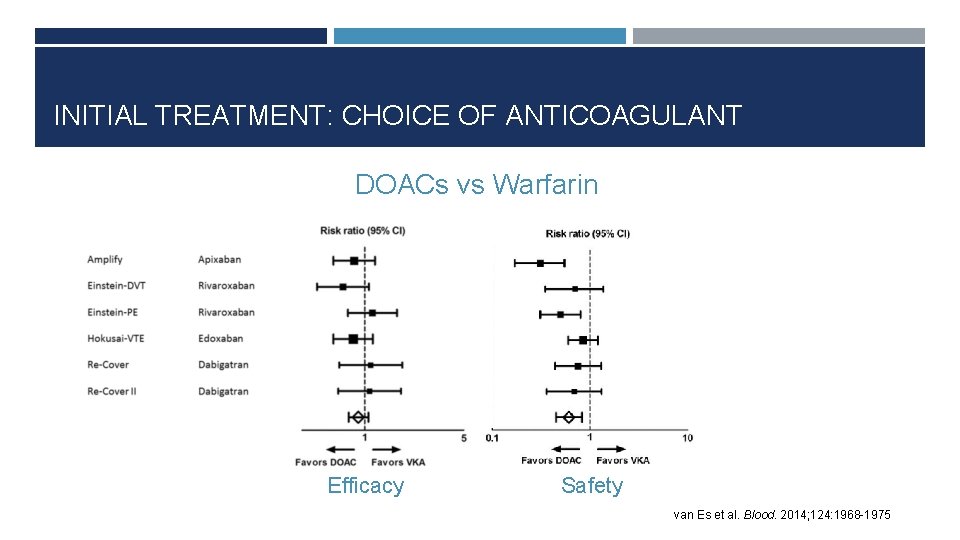
INITIAL TREATMENT: CHOICE OF ANTICOAGULANT DOACs vs Warfarin Efficacy Safety van Es et al. Blood. 2014; 124: 1968 -1975

INITIAL TREATMENT: ANTICOAGULANT OF CHOICE Avoid DOACs in the following patient groups: Active cancer Severe renal insufficiency End-stage liver disease Weight <50 kg or >120 -kg Gastric bypass surgery High-risk thrombophilic conditions (e. g. APLS, HIT) Pregnancy Breastfeeding Await solid evidence of efficacy and safety before recommending DOACs in unstudied or understudied scenarios Burnett et al. J Thrombolysis. 2016; 41: 206 -232 Yeh et al. Blood. 2014; 124(7): 1020 -1028

IVC FILTERS Goal: prevention of potentially fatal PE from a lower extremity DVT Unlike the benefit of anticoagulant therapy, the benefit derived from IVC filters remains unproven Randomized trial data is very limited Risks include thrombosis, filter migration, inability or failure to remove filter Rajasekhar. J Thrombolysis. 2015; 39: 315– 327

IVC FILTERS Key Study: PREPIC 2 (2015) Efficacy and safety of retrievable IVC filter to prevent recurrent PE 399 patients with acute symptomatic PE plus LE DVT randomized to receive or not receive a retrievable IVC filter in addition to therapeutic anticoagulation No difference in symptomatic recurrent PE at 3 or 6 months, no mortality benefit Mismetti et al. JAMA. 2015; 313(16): 1627 -1635

IVC FILTERS Indication for placement: Acute DVT (within 4 weeks) in the presence of a contraindication to anticoagulation Filter should be retrieved once anticoagulation can be initiated Other indications are controversial and of unproven clinical benefit or frankly harmful Rely on therapeutic or prophylactic anticoagulation whenever possible Streiff et al. J Thrombolysis. 2016; 41: 32 -67

CATHETER-DIRECTED THERAPIES Goal: prevention of post-thrombotic syndrome (PTS) PTS develops in 20 -50% of patients with DVT, even with appropriate anticoagulant therapy Key studies: Ca. Ven. T (2012) → CDT decreased PTS at the expense of major bleeding ATTRACT (2017) → CDT did not prevent PTS but decreased its severity Consider referral on a case-by-case basis: Common femoral or iliofemoral vein involvement, low bleeding risk, life expectancy >1 yr Start LMWH and discuss case ASAP with PAMC IR on-call doc Enden et al. Lancet. 2012; 379(9810): 31 -38 Kahn. Hematology 2016; 2016(1): 413 - 418

ELASTIC COMPRESSION STOCKINGS Goal: prevention of PTS Key study: SOX (2014) Multicenter placebo-controlled RCT of 803 patients with proximal DVT No evidence of benefit of ECS, worn for 2 years, to prevent PTS, reduce risk of recurrent VTE, or improve quality of life Do NOT routinely prescribe for PTS prevention Consider 20 -30 mm. Hg below-knee ECS for patients with DVT symptoms who can tolerate compression and derive benefit Enden et al. Lancet. 2014; 383(9920): 880 -888 Kahn. Hematology 2016; 2016(1): 413 - 418

INITIAL TREATMENT: AMERICAN COLLEGE OF CHEST PHYSICIANS 2016 GUIDELINES For acute PE or DVT of leg (no cancer): suggest dabigatran, rivaroxaban, apixaban, or edoxaban over vitamin K antagonist therapy For acute PE or DVT of leg (associated with cancer): suggest LMWH over DOACs or VKA therapy For acute DVT or PE treated with anticoagulants: recommend against the use of an IVC filter For acute proximal DVT of the leg: suggest anticoagulant therapy alone over CDT For acute DVT of the leg: suggest not using compression stockings routinely to prevent post- thrombotic syndrome Kearon et al. Chest. 2016; 149(2): 315 -352

BREAK FOR QUESTIONS

CASE 1: POST-OPERATIVE DVT 50 y. M with DVT after orthopedic surgery Patient returns for re-evaluation after 3 months of therapeutic anticoagulation with rivaroxaban He is wondering if he can stop anticoagulation

DURATION OF ANTICOAGULATION Decisions about whether to recommend long-term treatment will depend on: Risk of recurrence Risk of bleeding Patient preference 1. Risk factors for recurrent VTE (a) …, (b) …, (c) … 2. Risk factors for bleeding (a) …, (b) …, (c) … 3. Patient preference “Warfarin hate factor” “DOAC dislike factor” Moll. J Thrombolysis (2015) 39: 367– 378
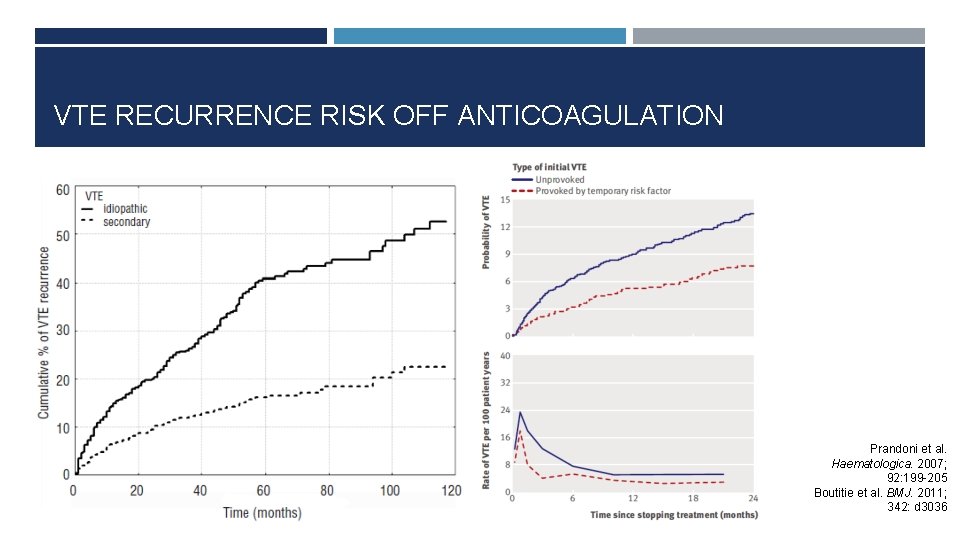
VTE RECURRENCE RISK OFF ANTICOAGULATION Prandoni et al. Haematologica. 2007; 92: 199 -205 Boutitie et al. BMJ. 2011; 342: d 3036

VTE RECURRENCE RISK OFF ANTICOAGULATION Not all provoking risk factors are created equal Rate of recurrence off anticoagulation after index VTE provoked by a transient risk factor: 3. 3% during the first year Surgical provoking risk factor: 0. 7% per patient-year Non-surgical provoking risk factor: 4. 2% per patient-year Rate of recurrence off anticoagulation after unprovoked index VTE event: 7. 4% per patient-year (Iorio et al) 10% at 1 year, 40% at 5 years (Prandoni et al) Iorio et al. Arch Intern Med. 2010; 170(19): 1710 -1716 Prandoni et al. Haematologica. 2007; 92: 199 -205

SAMPLE VTE CASES Case 1: Post-operative DVT → 3 months Case 2: Unprovoked PE Case 3: Cancer-associated DVT Case 4: PE in setting of a systemic inflammatory state Case 5: DVT in setting of OCPs

SAMPLE VTE CASES Case 1: Post-operative DVT → 3 months Case 2: Unprovoked PE → Extended Case 3: Cancer-associated DVT Case 4: PE in setting of a systemic inflammatory state Case 5: DVT in setting of OCPs

CASE 2: UNPROVOKED PE 50 y. M with PE but without medical illness or recent surgery Patient returns for re-evaluation after 3 months of therapeutic anticoagulation with rivaroxaban without bleeding complications He is reluctant to continue anticoagulation despite your recommendation based on recurrence risk He asks about additional testing that could impact his risk and possibly modify your recommendation Thrombophilia work-up Screening for occult malignancy D-dimer Residual vein thrombosis
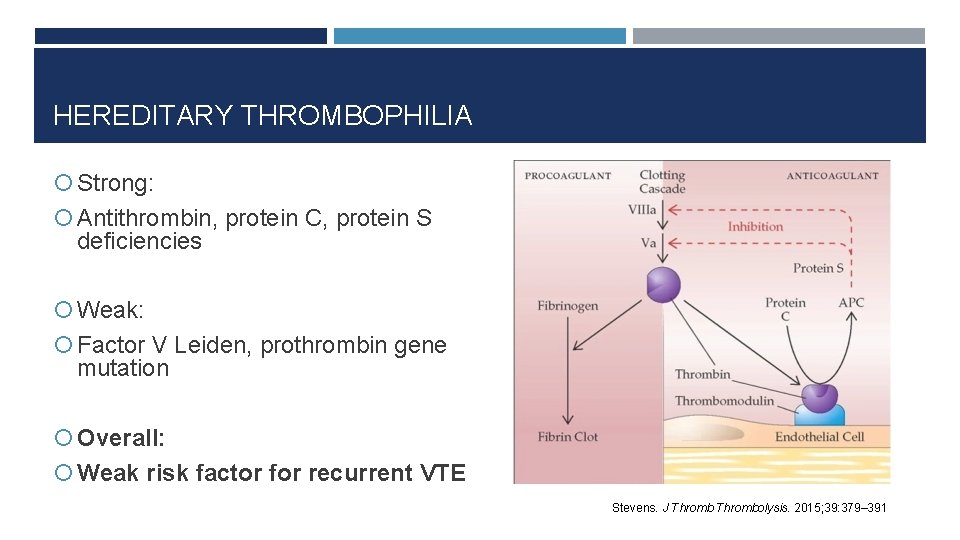
HEREDITARY THROMBOPHILIA Strong: Antithrombin, protein C, protein S deficiencies Weak: Factor V Leiden, prothrombin gene mutation Overall: Weak risk factor for recurrent VTE Stevens. J Thrombolysis. 2015; 39: 379– 391

HEREDITARY THROMBOPHILIA TESTING Evidence is lacking that management based on thrombophilia impacts outcomes No utility for testing in provoked VTE Risk: benefit balance favoring time-limited anticoagulation remains the same Little utility for testing in unprovoked VTE Risk for recurrent thrombosis is substantial and warrants indefinite anticoagulation regardless of thrombophilia testing results Cons include cost, insurance issues, anxiety, incorrect decisions Stevens. J Thrombolysis. 2015; 39: 379– 391

HEREDITARY THROMBOPHILIA TESTING: GUIDANCE Do not perform thrombophilia testing: Following an episode of provoked VTE (ASH Choosing Wisely) Following an episode of unprovoked VTE At the time of diagnosis and/or when the patient is on anticoagulation Perform thrombophilia testing only: If you can interpret the results If results will change management After anticoagulation has been stopped for one month Stevens et al. J Thrombolysis. 2016; 41: 154– 164

ACQUIRED THROMBOPHILIA TESTING Antiphospholipid Antibody Syndrome (APLS) Check lupus anticoagulant if initial PTT is prolonged Consider full APLS testing in younger patients with unprovoked VTE, stroke, recurrent early miscarriages, autoimmune disease since this would change management Myeloproliferative Neoplasms (e. g. PV, ET) Check JAK-2 mutation if splanchnic vein thrombosis or suspicious CBC findings

SCREENING FOR OCCULT MALIGNANCY Methods: multicenter, open-label, RCT involving 854 patients assigned to undergo limited occult-cancer screening or limited occultcancer screening in combination with CT A/P Results: no significant difference between the two study groups in the mean time to a cancer diagnosis or in cancer-related mortality Conclusion: routine screening with CT of the abdomen and pelvis did not provide a clinically significant benefit Bottom Line: Perform ageappropriate cancer screening

D-DIMER AND RECURRENT VTE Key study: Objective: assess prognostic value for VTE recurrence of elevated D-dimer levels 1 month after discontinuation of oral anticoagulation for idiopathic VTE Methods: meta-analysis of 4 studies involving 1539 patients Results: elevated D-dimer levels were significantly associated with recurrent VTE (OR 2. 36; 95% CI: 1. 65 to 3. 36) Conclusion: elevated D-dimer levels measured 1 month after d/c of anticoagulation identify patients with idiopathic VTE at higher risk of recurrence Bruinstroop et al. J Thromb Haemost. 2009; 7: 611– 8

ULTRASOUND AND RECURRENT DVT Key study: Objective: determine if residual vein obstruction (RVO) is a valid predictor of recurrent VTE in patients with a first unprovoked DVT who had received at least three months of anticoagulant Methods: meta-analysis of 10 prospective studies involving 2, 527 patients Results: RVO was independently but weakly associated with recurrent VTE (HR = 1. 32, 95% CL: 1. 06 -1. 65) Conclusions: Residual clot not clinically helpful, U/S not recommended by most experts Donadini et al. Thromb Haemost. 2014; 111(1): 172 -9

CASE 2: UNPROVOKED PE Summary of recommendations: Extended anticoagulation* Age-appropriate cancer screening Hereditary thrombophilia testing D-dimer testing Only if results will change management! No ultrasound to check for RVO v The only exception is distal (calf vein) DVT for which only 3 months of anticoagulation is recommended even if unprovoked

CASE 3: CANCER-ASSOCIATED THROMBOSIS 50 y. F with DVT in the setting of pancreatic cancer Patient returns for re-evaluation after 3 months of therapeutic anticoagulation with LMHW Patient wonders how long she needs to stay on anticoagulation and if injection therapy is required

CANCER-ASSOCIATED THROMBOSIS Cancer type Cancer stage All influence VTE risk: 4 -7 x Cancer treatment Continue anticoagulation as long as there is evidence of disease or ongoing cancer therapy LMWH remains the agent of choice per ACCP and ASCO guidelines Trials of DOACs vs LMWH are ongoing Rivaroxaban and edoxaban trials completed enrollment 12/2016 Streiff. Hematology 2016; 2016(1): 196 -205

SAMPLE VTE CASES Case 1: Post-operative DVT → 3 months Case 2: Unprovoked PE → Extended Case 3: Cancer-associated DVT → Extended with LMWH Case 4: PE in setting of a systemic inflammatory state Case 5: DVT in setting of OCPs

CASE 4: INFLAMMATION-ASSOCIATED VTE 40 y. M with DVT in the setting of an IBD flare Patient returns for re-evaluation after 3 months of therapeutic anticoagulation with rivaroxaban He will be starting infliximab soon and for cost reasons does not want to continue a DOAC unless necessary
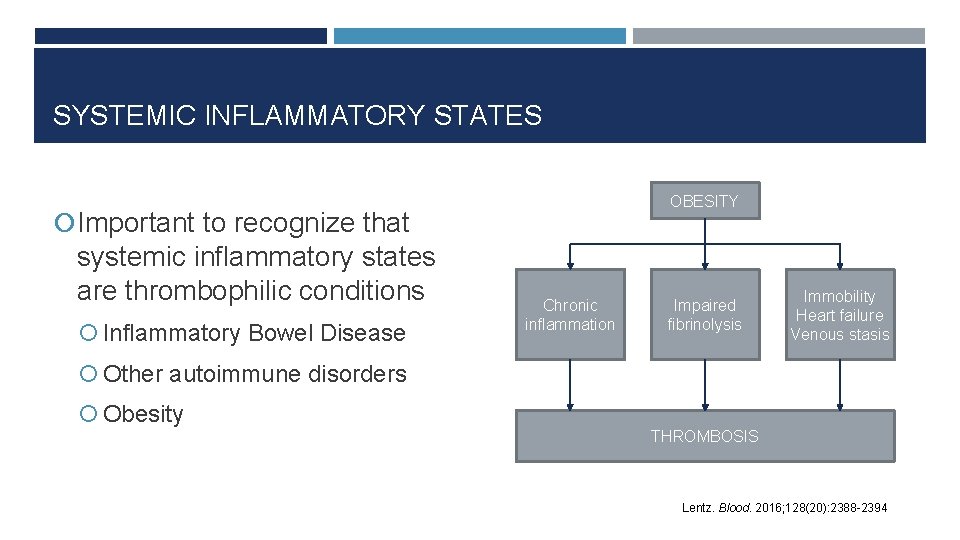
SYSTEMIC INFLAMMATORY STATES OBESITY Important to recognize that systemic inflammatory states are thrombophilic conditions Inflammatory Bowel Disease Chronic inflammation Impaired fibrinolysis Immobility Heart failure Venous stasis Other autoimmune disorders Obesity THROMBOSIS Lentz. Blood. 2016; 128(20): 2388 -2394

SYSTEMIC INFLAMMATORY STATES Obesity Weight loss reverses many of the pro-thrombotic metabolic effects of obesity No other obesity-specific therapeutic approaches to prevent and treat thrombosis are available Inflammatory Bowel Disease VTE event in setting of IBD flare → anticoagulate until IBD remission x 3 months VTE event provoked by a factor other than IBD → 3 months Unprovoked VTE event with IBD in clinical remission → indefinite Lentz. Blood. 2016; 128(20): 2388 -2394

SAMPLE VTE CASES Case 1: Post-operative DVT → 3 months Case 2: Unprovoked PE → Extended Case 3: Cancer-associated DVT → Extended with LMWH Case 4: PE in setting of a systemic inflammatory state → 3+ months Case 5: DVT in setting of OCPs

CASE 5: HORMONE-ASSOCIATED VTE 30 y. F with PE on a combined oral contraceptive pill Patient returns for re-evaluation after 3 months of therapeutic anticoagulation with rivaroxaban She is wondering if she can stop anticoagulation if she stays away from hormones

ORAL CONTRACEPTIVES Key Study: Results: risk of VTE recurrence 9. 7 per 1000 patient-years among patients who completed at least 3 months of anticoagulation and discontinued hormonal therapy Conclusion: OCPs can be approached as a provoking risk factor Key Study: Results: hormonal therapy not associated with increased recurrent VTE risk in women on anticoagulant therapy Conclusion: OK to continue OCPs while on anticoagulants if hormonal therapy is medically necessary Martinelli et al. Blood. 2016; 127(11): 1417 -25

SAMPLE VTE CASES Case 1: Post-operative DVT → 3 months Case 2: Unprovoked PE → Extended Case 3: Cancer-associated DVT → Extended with LMWH Case 4: PE in setting of a systemic inflammatory state → 3+ months Case 5: DVT in setting of OCPs → 3 months unless OCP use continues
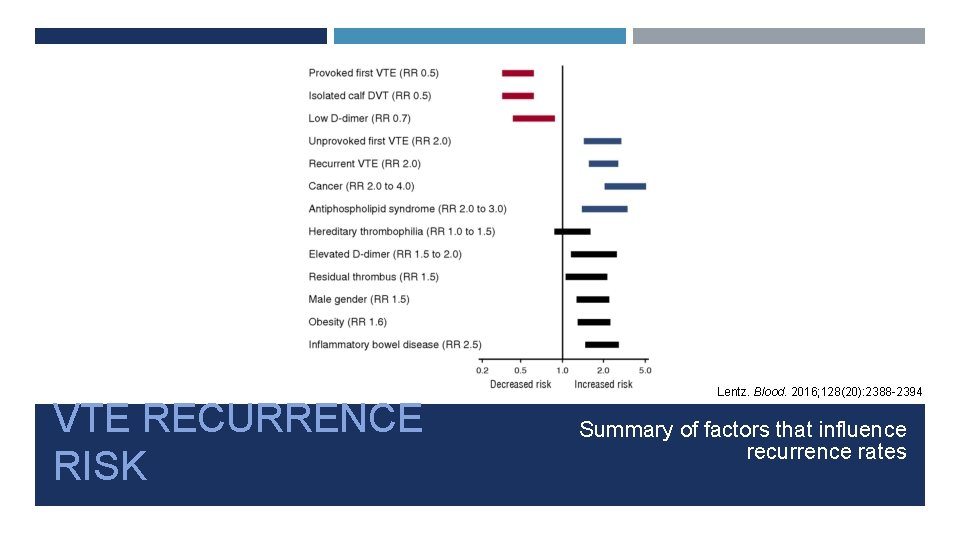
VTE RECURRENCE RISK Lentz. Blood. 2016; 128(20): 2388 -2394 Summary of factors that influence recurrence rates

DURATION OF ANTICOAGULATION: GENERAL GUIDELINES Potent pro-thrombotic reversible risk factor (e. g. surgery, trauma) Discontinue therapy after three months Non-surgical provoking factor (e. g. IBD, cancer, hormones, immobility) Continue therapy as long as underlying trigger remains Unprovoked VTE Reassess after three months of therapy High bleeding risk OR Isolated distal DVT Discontinue therapy All others Continue therapy indefinitely

REAL-LIFE CASE 52 y. M in good health presenting with DVT/PE two days after arthroscopic knee surgery Anticoagulation started with apixaban Platelet count noted to be in 600 s Work-up with JAK 2 and BMBx returned consistent with ET Plan: anticoagulation x 3 months for post-op VTE, then additional OAC until platelet count controlled to <400 with hydroxyurea

LONG-TERM TREATMENT: CHOICE OF ANTICOAGULANT Warfarin and DOACs reduce recurrent VTE risk by 80 -90% compared with placebo Warfarin is associated with a 2. 6 -fold increase in major bleeding Dabigatran is as effective as warfarin but with similar major bleeding Rivaroxaban and apixaban have been compared to placebo only Edoxaban has not been studied for extended treatment Aspirin 100 mg daily reduces recurrent VTE risk by 34% vs placebo with similar risk of major bleeding Streiff et al. J Thrombolysis. 2016; 41: 32 -67
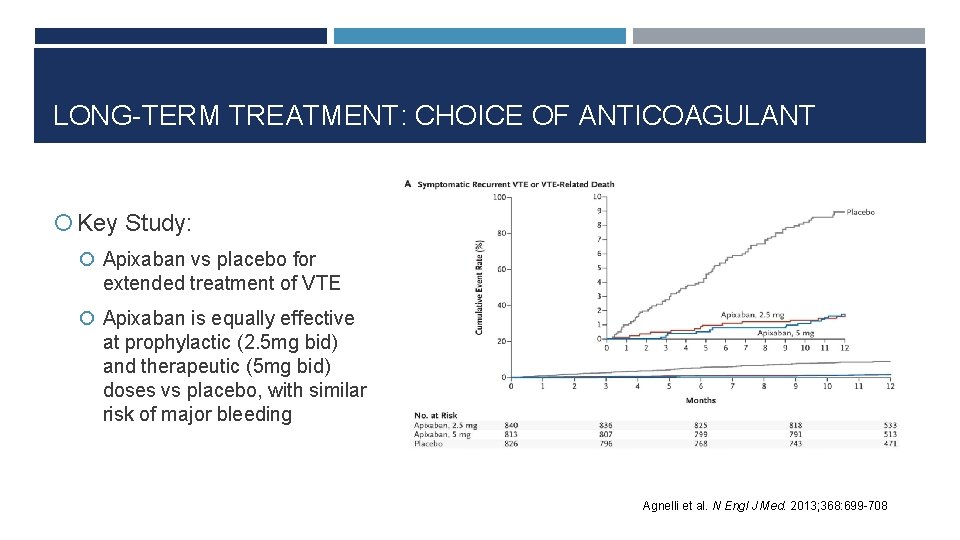
LONG-TERM TREATMENT: CHOICE OF ANTICOAGULANT Key Study: Apixaban vs placebo for extended treatment of VTE Apixaban is equally effective at prophylactic (2. 5 mg bid) and therapeutic (5 mg bid) doses vs placebo, with similar risk of major bleeding Agnelli et al. N Engl J Med. 2013; 368: 699 -708
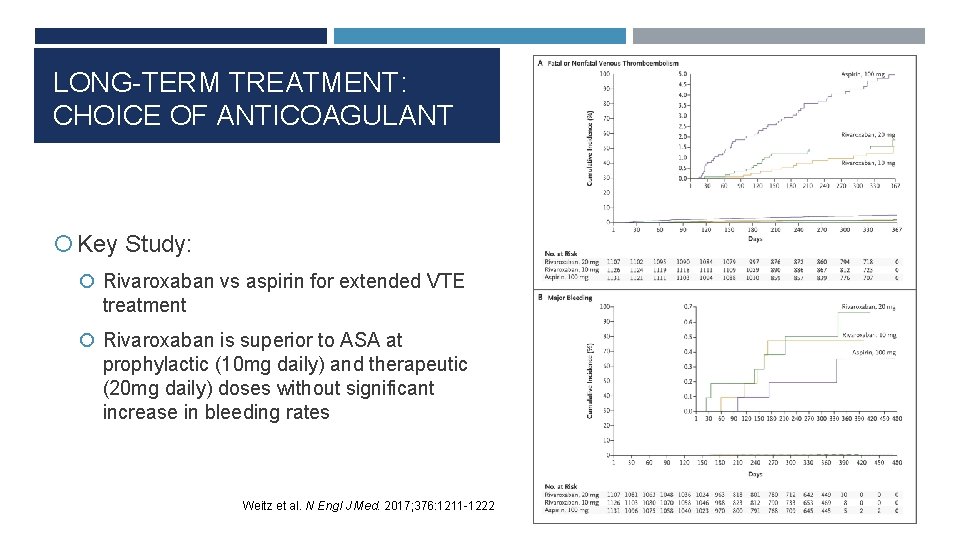
LONG-TERM TREATMENT: CHOICE OF ANTICOAGULANT Key Study: Rivaroxaban vs aspirin for extended VTE treatment Rivaroxaban is superior to ASA at prophylactic (10 mg daily) and therapeutic (20 mg daily) doses without significant increase in bleeding rates Weitz et al. N Engl J Med. 2017; 376: 1211 -1222

LONG-TERM TREATMENT: CHOICE OF ANTICOAGULANT ACCP 2016 Guidelines: For patients with DVT of the leg or PE who receive extended therapy, suggest that there is no need to change the choice of anticoagulant after the first 3 months If switching to prophylactic dosing of apixaban or rivaroxaban, treat with therapeutic dosing for at least 6 months Data on DOACs for extended VTE treatment remains limited compared to warfarin

CONCLUSIONS Anticoagulation is the gold standard for VTE treatment DOACs are the preferred agents for initial and long-term anticoagulation except in cancer Duration of anticoagulation is typically either 3 months or indefinite For provoked events, continue so long as the trigger is present Perform additional testing only if it will change management
- Slides: 51