A diagnostic checklist for HMB The HELP diagnostic

A diagnostic checklist for HMB

The HELP diagnostic checklist Practical guidance based on the FIGO recommendations 1 A step-by step guide to help: • Confirm presence and impact of HMB • Identify relevant medical history, physical symptoms and risk factors that may indicate a pathological cause • Guide the use of investigations and tests to exclude a pathological cause 1. Munro MG, et al. Int J Gynecol Obstet 2011; 113: 3– 13. 2

3 Using three key questions to help identify HMB 1 -3 Answering yes to one or more of these questions and experiencing symptoms for 3+ months indicates that HMB is a problem is impacting negatively on quality of life Further action is needed to identify cause and appropriate treatment 1. Philipp CS, et al. Am J Obstet Gynecol 2008; 198: 163. e 1 -163. e 8; 2. Bushnell, DM, et a. Curr Med Res Opin 2010; 26(12): 2745 -55; 3. Matteson KA, Clark MA. Women Health 2010; 50(2): 195 -211. HMB, heavy menstrual bleeding
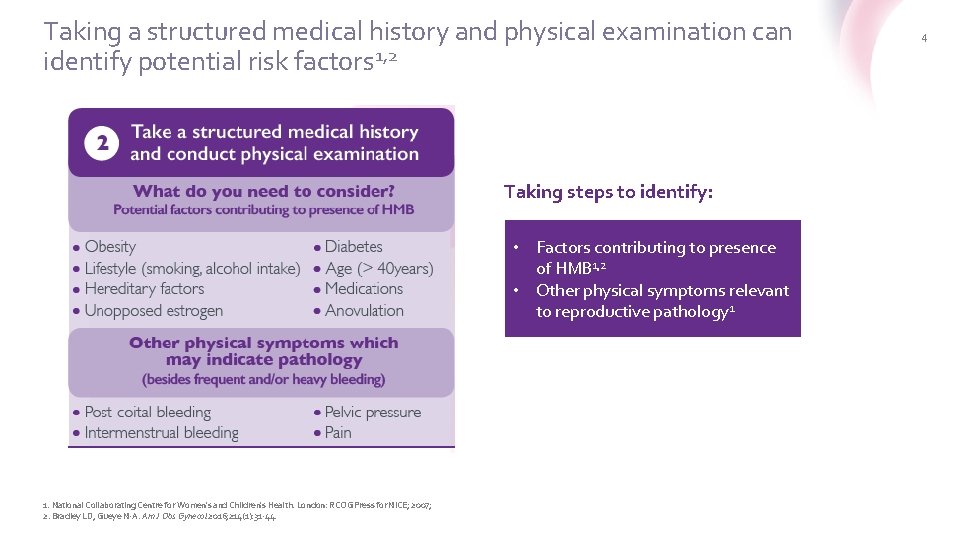
Taking a structured medical history and physical examination can identify potential risk factors 1, 2 Taking steps to identify: • Factors contributing to presence of HMB 1, 2 • Other physical symptoms relevant to reproductive pathology 1 1. National Collaborating Centre for Women's and Children's Health. London: RCOG Press for NICE; 2007; 2. Bradley LD, Gueye N-A. Am J Obs Gynecol 2016; 214(1): 31 -44. 4
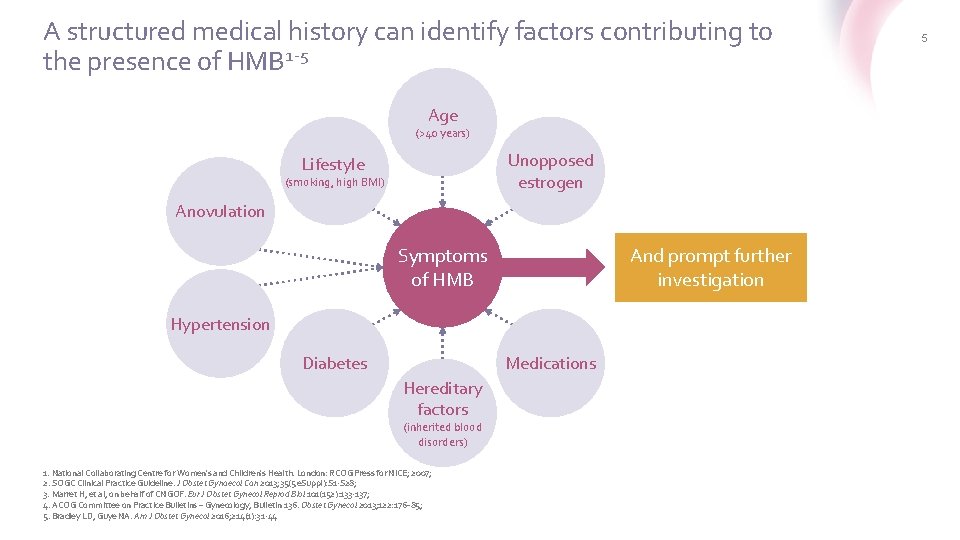
A structured medical history can identify factors contributing to the presence of HMB 1 -5 Age (>40 years) Unopposed estrogen Lifestyle (smoking, high BMI) Anovulation And prompt further investigation Symptoms of HMB Hypertension Diabetes Medications Hereditary factors (inherited blood disorders) 1. National Collaborating Centre for Women's and Children's Health. London: RCOG Press for NICE; 2007; 2. SOGC Clinical Practice Guideline. J Obstet Gynaecol Can 2013; 35(5 e. Suppl): S 1 -S 28; 3. Marret H, et al, on behalf of CNGOF. Eur J Obstet Gynecol Reprod Biol 101(152): 133 -137; 4. ACOG Committee on Practice Bulletins – Gynecology, Bulletin 136. Obstet Gynecol 2013; 122: 176– 85; 5. Bradley LD, Guye NA. Am J Obstet Gynecol 2016; 214(1): 31 -44 5
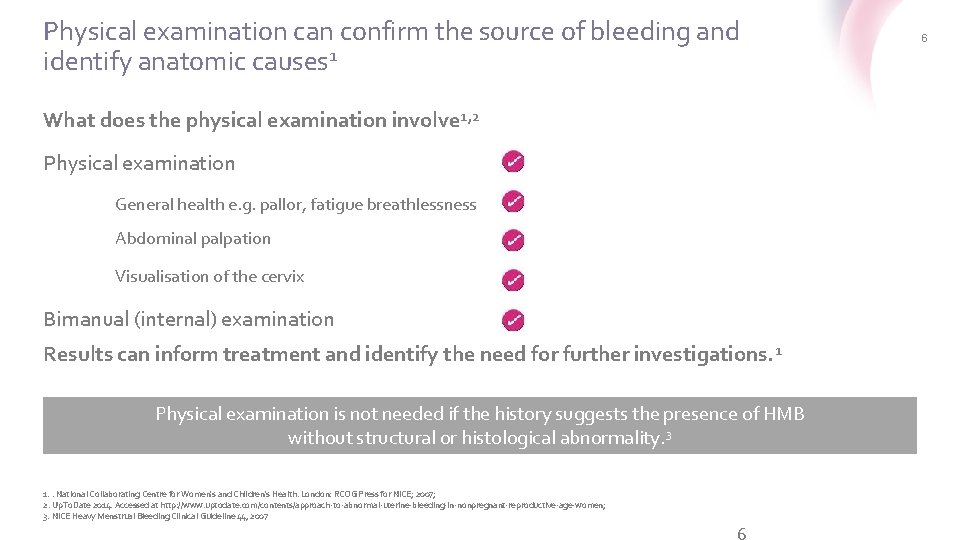
Physical examination can confirm the source of bleeding and identify anatomic causes 1 What does the physical examination involve 1, 2 Physical examination General health e. g. pallor, fatigue breathlessness Abdominal palpation Visualisation of the cervix Bimanual (internal) examination Results can inform treatment and identify the need for further investigations. 1 Physical examination is not needed if the history suggests the presence of HMB without structural or histological abnormality. 3 1. . National Collaborating Centre for Women's and Children's Health. London: RCOG Press for NICE; 2007; 2. Up. To. Date 2014. Accessed at http: //www. uptodate. com/contents/approach-to-abnormal-uterine-bleeding-in-nonpregnant-reproductive-age-women; 3. NICE Heavy Menstrual Bleeding Clinical Guideline 44, 2007 6
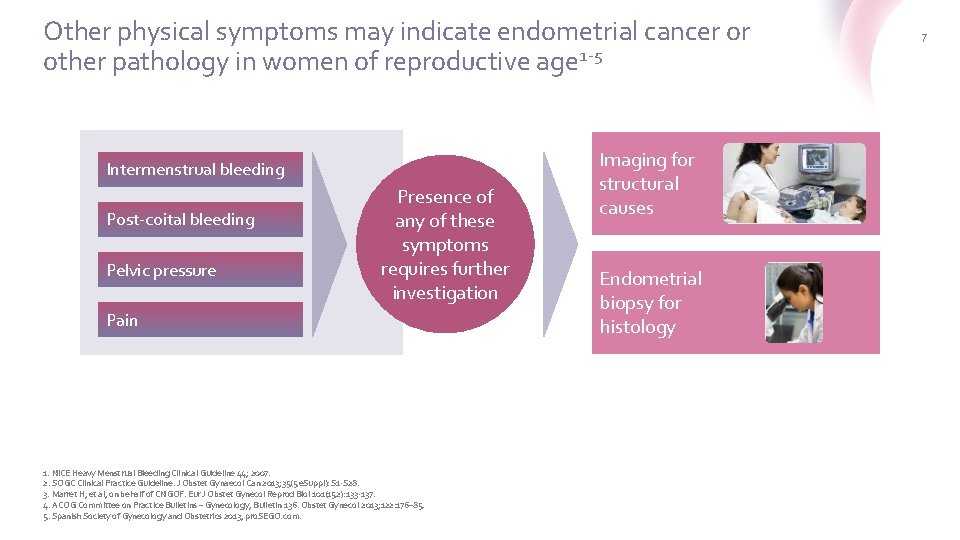
Other physical symptoms may indicate endometrial cancer or other pathology in women of reproductive age 1 -5 If. Evaluating suspected organic pathology the problem or risk factors present Intermenstrual bleeding Post-coital bleeding Pelvic pressure Presence of any of these symptoms requires further investigation Pain 1. NICE Heavy Menstrual Bleeding Clinical Guideline 44; 2007. 2. SOGC Clinical Practice Guideline. J Obstet Gynaecol Can 2013; 35(5 e. Suppl): S 1 -S 28. 3. Marret H, et al, on behalf of CNGOF. Eur J Obstet Gynecol Reprod Biol 101(152): 133 -137. 4. ACOG Committee on Practice Bulletins – Gynecology, Bulletin 136. Obstet Gynecol 2013; 122: 176– 85. 5. Spanish Society of Gynecology and Obstetrics 2013, pro. SEGO. com. Imaging for structural causes Endometrial biopsy for histology 7

HMB may result from structural and non-structural abnormalities FIGO has proposed a standard classification for abnormal uterine bleeding (AUB) to aid diagnosis 1 For the majority of women, there is no identifiable cause of HMB 2 1. Munro MG, et al. Int J Gynecol Obstet 2011; 113: 3 -13. 2. National Collaborating Centre for Women's and Children's Health. London: RCOG Press for NICE; 2007. 8

Further tests and investigations may help to exclude pathological cause of HMB These tests are ONLY needed if indicated by structured medical history or physical examination Remember, for the majority of women, there is no identifiable cause of HMB 1 1. National Collaborating Centre for Women's and Children's Health. London: RCOG Press for NICE; 2007. 9

Additional laboratory tests may be indicated 1 -3 If… • There are clinical findings suggestive of thyroid or pituitary dysfunction, or hyperandrogenism • There is a history of menstrual bleeding since menarche or a personal or family history of abnormal bleeding However, for all women with HMB… • a complete blood count is recommended 1 • the possibility of pregnancy should be ruled out 1. SOGC Clinical Practice Guideline. J Obstet Gynaecol Can 2013; 35(5 e. Suppl): S 1 -S 28. 2. Marret H, et al, on behalf of CNGOF. Eur J Obstet Gynecol Reprod Biol 101152): 133 -137. 3. National Collaborating Centre for Women's and Children's Health. London: RCOG Press for NICE; 2007. 10

Up to 20% of women with HMB have an inherited bleeding disorder 1 Bleeding symptoms indicative of an inherited bleeding disorder 1 Epistaxis (usually bilateral and lasting > 10 minutes duration) Notable bruising without injury (> 2 cm in diameter) Minor wound bleeding (i. e. from trivial cuts lasting longer than 5 minutes) Bleeding of the oral cavity or gastrointestinal tract without a lesion Excessive or prolonged bleeding following dental extraction Unexpected post-surgical bleeding Hemorrhage from ovarian cyst or corpus luteum Post-partum hemorrhage (especially delayed onset > 24 hours) It is important to have a high index of suspicion in adolescents, as coagulation disorders are a common cause of HMB in this age group 2 11

Imaging and endometrial assessment and biopsy is only indicated in specific circumstances 1, 2 • Examination suggests a structural cause of the bleeding • Pharmaceutical treatment has failed • Examination and/or symptoms suggest the risk of malignancy It is important to have a high index of suspicion in adolescents, as coagulation disorders are a common cause of HMB in this age group 2 Imaging can be carried out using ultrasound, hysteroscopy and/or Magnetic Resonance Imaging (MRI) 1. SOGC Clinical Practice Guideline. J Obstet Gynaecol Can 2013; 35(5 e. Suppl): S 1 -S 28. 2. National Collaborating Centre for Women's and Children's Health. London: RCOG Press for NICE; 2007. 12

Treatment can be offered even if further investigations are required 1 13

14 Treating symptoms of anemia • Fatigue and weakness are common symptoms of HMB that can help confirm diagnosis of iron deficiency 1 Age or gender group Hemoglobin (g/d. L) Children (0. 5 -4) < 11. 0 Children (5 -12) < 11. 5 Children (12 -15) < 12. 0 Adult men < 13. 0 Non-pregnant women < 12. 0 Pregnant women < 11. 0 Adapted from the WHO global database on anemia 2 Iron-deficiency affects >20% of women during their reproductive lives 3 • Iron supplementation corrects anemia and replenishes body stores 4 1. Fraser I, et al. . Int J Gynecol Obstetrics 2015: 128: 196– 200. 2. World Health Organization. Worldwide prevalence of anaemia 1993– 2005: WHO global database on anaemia, 2008. 3. Percy L, et al. Best Pract Res Clin Obstet Gynaecol 2017; 40: 55 -67. 4. Goddard A, et al. Gut 2011; 60: 1309 -1316.
- Slides: 14