A CASE SCENARIO by Dr Syed Hunain Riaz


A CASE SCENARIO by Dr. Syed Hunain Riaz P. G M 2 Slide 001

HISTORY

Case History • A 14 years old boy of very low socioeconomic background presented with 1. Shortness of breath----About 10 years 2. Generalized weakness-----About the same duration Slide 002

History of presenting illness • • • The boy was in his usual state of health when he was about 4 years old when he gradually developed shortness of breath. It was exertional in nature. He did not have orthopnea or PND. There is h/o palpitations associated with the dyspnea. No h/o chest discomfort, body swellings or hemoptysis. No h/o syncopal events. H/o yellowish discoloration of eyes for the last many years, no h/o abdominal distention, no h/o unconsciousness He started to develop generalized weakness and as such was unable to perform simple activities.

• No h/o blood in stools, no h/o alternating bowel habits or worms in stool. PAST HISTORY • Non/diabetic, non-asthmatic. Has had blood transfusions three times over period of 10 years. FAMILY HISTORY • No h/o diabetes, IHD, asthma or TB in the family, no h/o any disease in his siblings. Has 3 brothers, all older than him, all healthy.

• DRUG HISTORY No h/o any drug intake and no allergies to any medicine • SOCIOECONOMIC HISTORY Belongs to a lower class family who earn their bread by farming

EXAMINATION

General Physical exam • A young boy of average built with prominent facial bony features ( slightly protuding forhead, prominent zygomatic area ) well oriented, sitting comfortably in bed. • Vitals and Exam findings : BP: 90/50 mm. Hg Pulse: 90/min R/R: 18/min Temp: Afebrile Jaundice: ++(lime colored) Pallor: +++ Cyanosis: Clubbing: -

Lymph nodes: JVP: Not Raised Pedal edema: Palmar erythema: Neck veins: Not distended Koilonychia: - • 2 shallow ulcers(2 -3 cm each) with clean margins and yellowish discharge on dorsum of right foot.

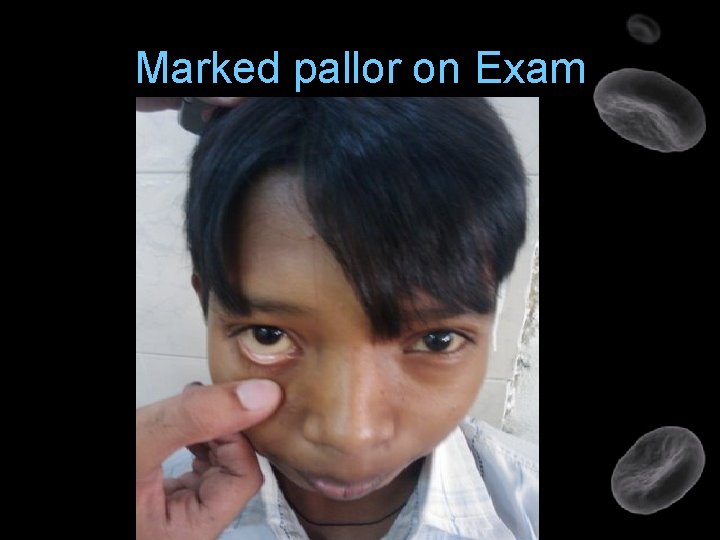
Marked pallor on Exam
Systemic Exam Cardiovascular: • Apex beat in left fifth ICS, normal in character • Soft S 1 and S 2, soft A 2 and loud P 2 • Pansystolic murmur heard in mitral area, radiating to axilla. • Pansystolic murmer heard in tricuspid area, increasing in intensity with inspiration

• Gastrointestinal: • Abdomen soft, non tender, no pulsations or veins visible • Upper border of liver in right 5 th ICS, lower edge palpated about 4 fingers below right hypochondrium, extending into the epigastrium, non-tender, and smooth surfaced. Liver span about 18 cm • Spleen palpated 2 fingers below left hypochondrium towards the umbilicus, non tender and smooth surfaced. • No free fluid on in abdomen on examination
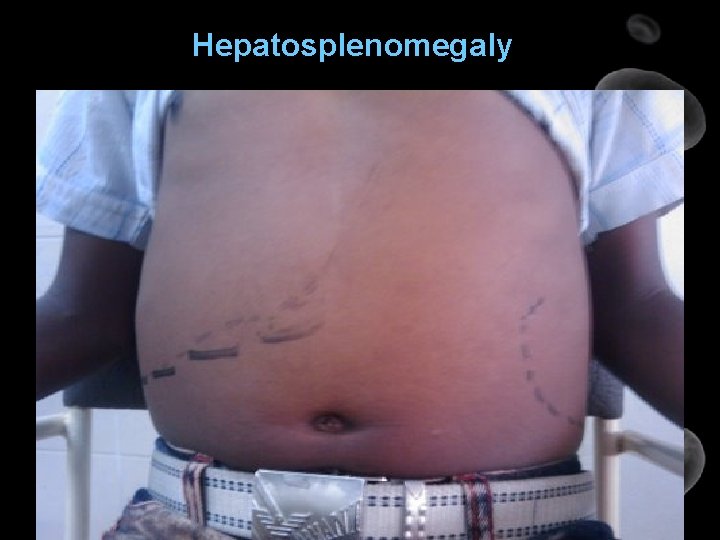
Hepatosplenomegaly
CNS: • Grossly intact Respiratory: • Normal chest shape and movements • Chest expansion normal • NVB with no added sounds Muskoloskeletal: • NAD

Differential Diagnosis based on HistoryExam • Anemia ( Iron deficiency? Hemolytic? ) • Lymphoproliferative disorder? • Valvular heart disease ( leading to long standing anemia )?

INVESTIGATIONS
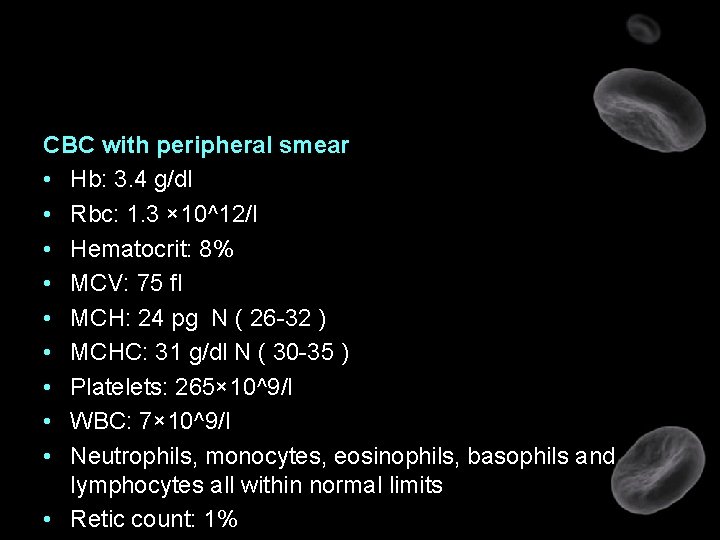
CBC with peripheral smear • Hb: 3. 4 g/dl • Rbc: 1. 3 × 10^12/l • Hematocrit: 8% • MCV: 75 fl • MCH: 24 pg N ( 26 -32 ) • MCHC: 31 g/dl N ( 30 -35 ) • Platelets: 265× 10^9/l • WBC: 7× 10^9/l • Neutrophils, monocytes, eosinophils, basophils and lymphocytes all within normal limits • Retic count: 1%
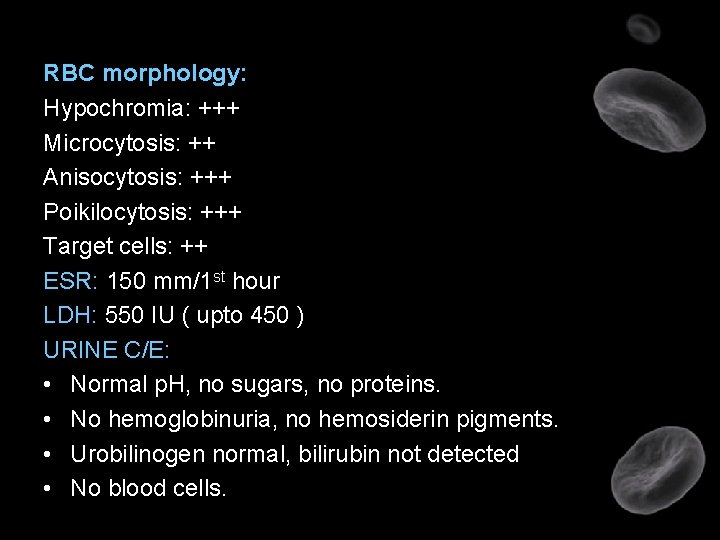
RBC morphology: Hypochromia: +++ Microcytosis: ++ Anisocytosis: +++ Poikilocytosis: +++ Target cells: ++ ESR: 150 mm/1 st hour LDH: 550 IU ( upto 450 ) URINE C/E: • Normal p. H, no sugars, no proteins. • No hemoglobinuria, no hemosiderin pigments. • Urobilinogen normal, bilirubin not detected • No blood cells.
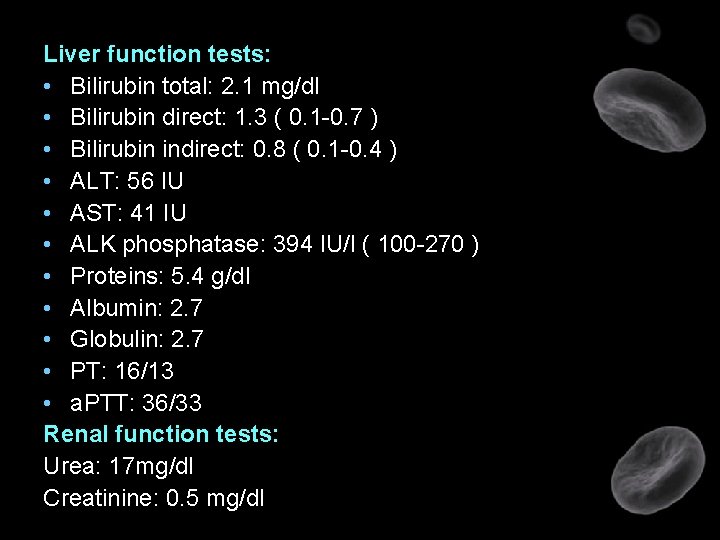
Liver function tests: • Bilirubin total: 2. 1 mg/dl • Bilirubin direct: 1. 3 ( 0. 1 -0. 7 ) • Bilirubin indirect: 0. 8 ( 0. 1 -0. 4 ) • ALT: 56 IU • AST: 41 IU • ALK phosphatase: 394 IU/l ( 100 -270 ) • Proteins: 5. 4 g/dl • Albumin: 2. 7 • Globulin: 2. 7 • PT: 16/13 • a. PTT: 36/33 Renal function tests: Urea: 17 mg/dl Creatinine: 0. 5 mg/dl
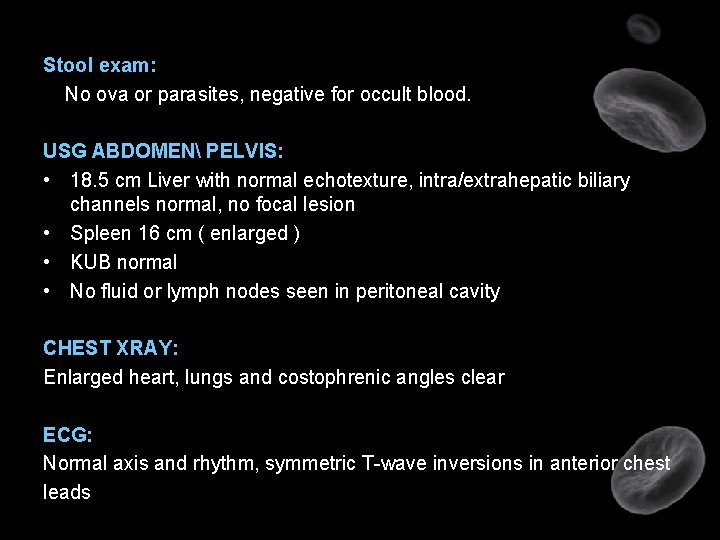
Stool exam: No ova or parasites, negative for occult blood. USG ABDOMEN PELVIS: • 18. 5 cm Liver with normal echotexture, intra/extrahepatic biliary channels normal, no focal lesion • Spleen 16 cm ( enlarged ) • KUB normal • No fluid or lymph nodes seen in peritoneal cavity CHEST XRAY: Enlarged heart, lungs and costophrenic angles clear ECG: Normal axis and rhythm, symmetric T-wave inversions in anterior chest leads
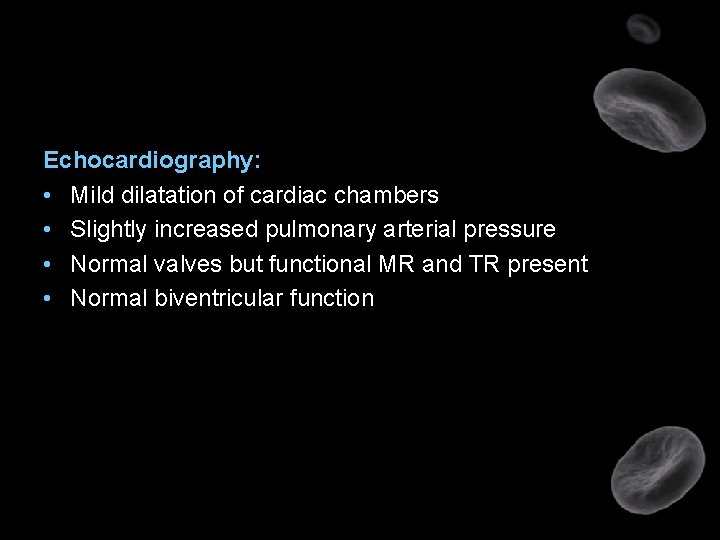
Echocardiography: • Mild dilatation of cardiac chambers • Slightly increased pulmonary arterial pressure • Normal valves but functional MR and TR present • Normal biventricular function

WHAT’S LIKELY AND WHAT TO DO?

Based on clinical and investigation data, there was a high suspicion of a long standing hemolytic anemia (extravascular hemolysis), specifically “ THALASSEMMIA”, so a hemoglobin electrophoresis was ordered…. .
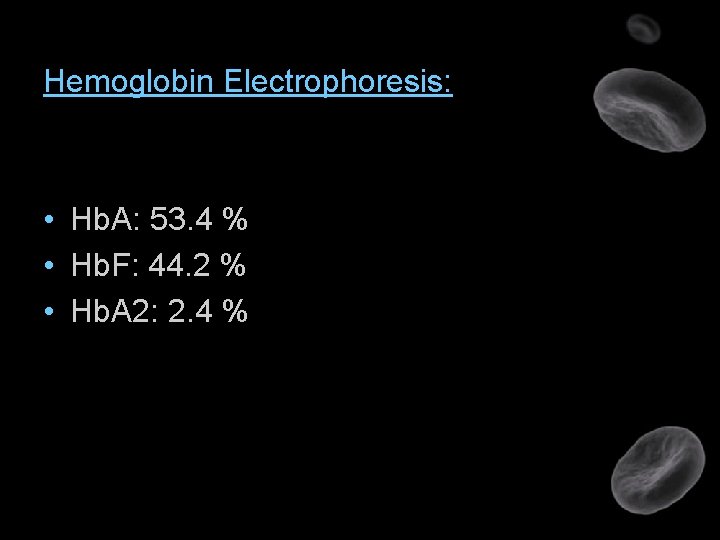
Hemoglobin Electrophoresis: • Hb. A: 53. 4 % • Hb. F: 44. 2 % • Hb. A 2: 2. 4 %
CONCLUSION The final diagnosis was: ß-THALASSEMIA INTERMEDIA/ MAJOR

Thalassemias • A heterogenous group of inherited disorders of hemoglobin synthesis resulting decreased or absent hemoglobin chains synthesis • Classified into alpha and beta thalassemias. • Varied pattern of inheritance • Decreased synthesis of ß-chains result in over production of alpha chains, and also gamma and delta chains leading to the finding of fetal and Hb. A 2 type of hemoglobin in ß-thalassemias

Treatment • Thalassemia major intermedia patients are treated on the following lines: • BLOOD TRANSFUSIONS • CHELATION THERAPY ( DESFERIOXAMINE ) • ALLOGENIC BONE MARROW TRANSPLANTATION Splenectomy may be needed if BMT is not feasible for reducing the RBC destruction in the spleen

Slide 004
- Slides: 30