A case of bilateral renal tumours Rajesh Batajoo

A case of bilateral renal tumours Rajesh Batajoo, Fellow Tata Medical Center

Clinical details 52 years/male, from Bangladesh Chief complaint - B/L loin pain L>R x 6 months History - Pain dull aching, - No h/o haematuria, no LUTS, no weight loss and fever Smoker No significant family history Comorbidity : Diabetic on regular treatment. No h/o

Clinical details O/E - ECOG 0 Thinly built, general condition fair, Vitals: Stable, no pallor, or lymphadenopahty P/A: Soft, non tender, no organomegaly External genitalia: Normal DRE: Small benign feeling prostate

Investigations • • CBC- Hb 13. 6 gm/dl, TC 11100, PLT 278000 S. Creat- 0. 83, Urea 28, Sodium 134, Potassium 4. 2 LFT normal Urine C/S: sterile • USG KUB: Left renal mass 6. 5 cmx 6. 4 cm at mid pole. (Done in Bangladesh)

Investigations cont. . • CT thorax and abdomen CT thorax: Normal. CT whole abdomen showed bilateral renal masses Ø Right superior and inferior polar lesions 4 cm, and 2. 1 cm Ø Left mid polar lesion 7. 5 x 7. 1 cm lesion
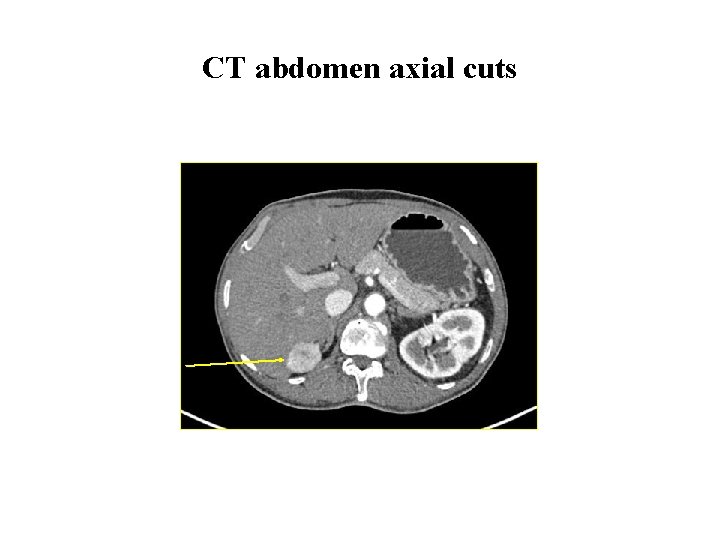
CT abdomen axial cuts
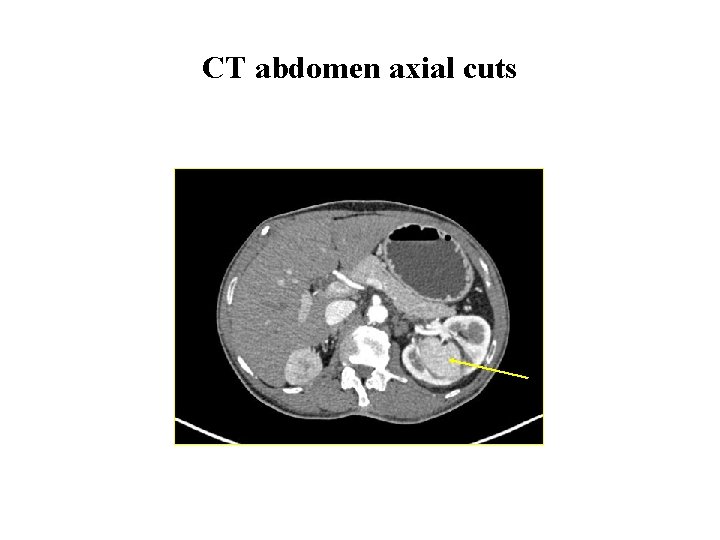
CT abdomen axial cuts
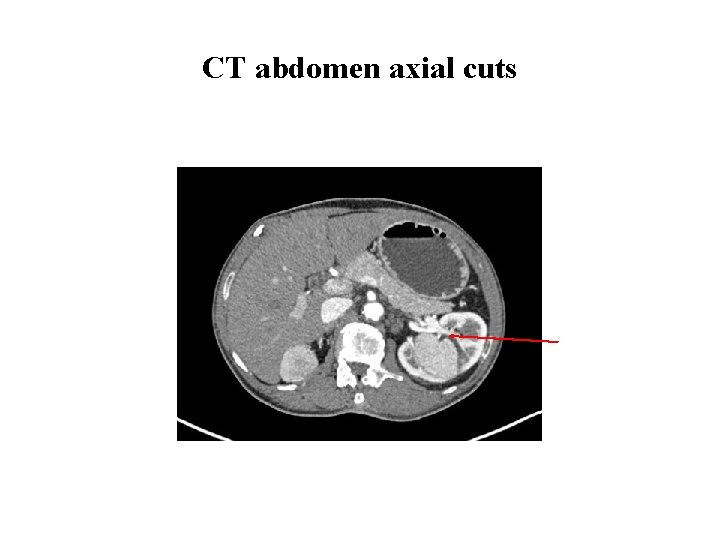
CT abdomen axial cuts
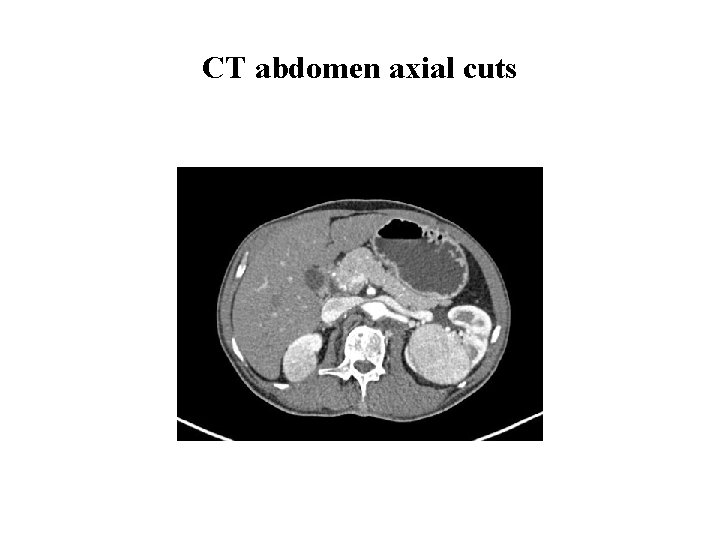
CT abdomen axial cuts
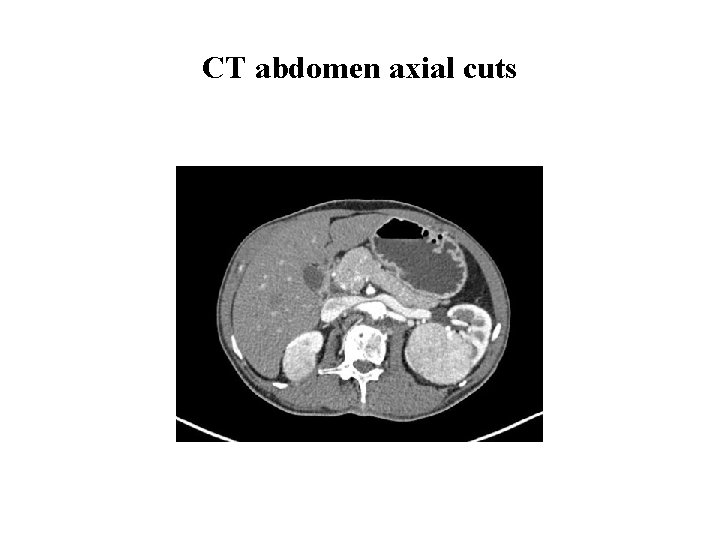
CT abdomen axial cuts
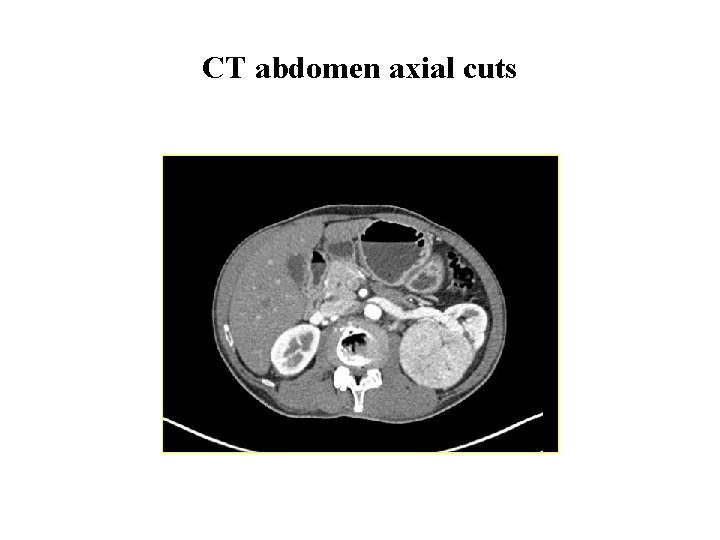
CT abdomen axial cuts
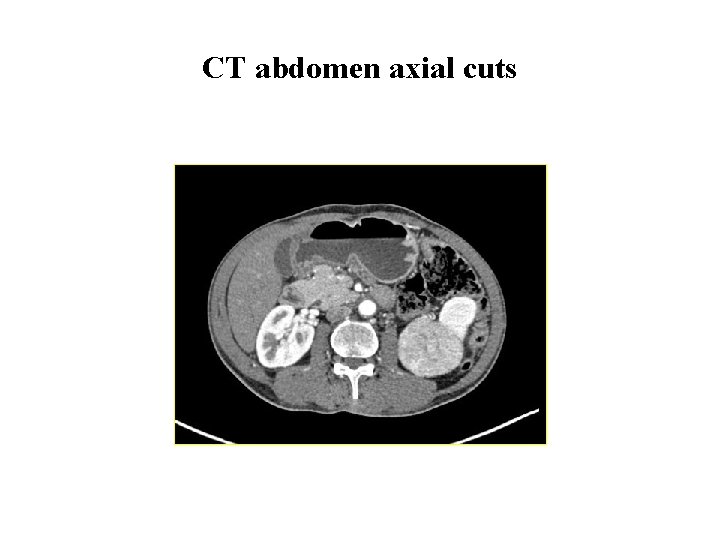
CT abdomen axial cuts
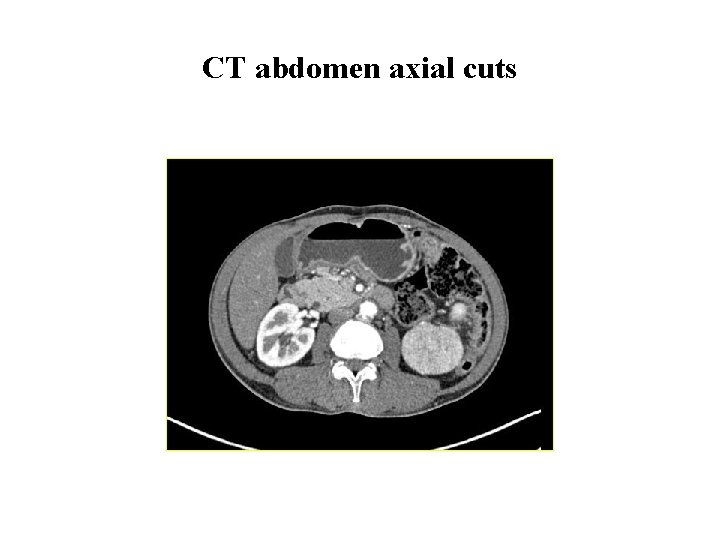
CT abdomen axial cuts
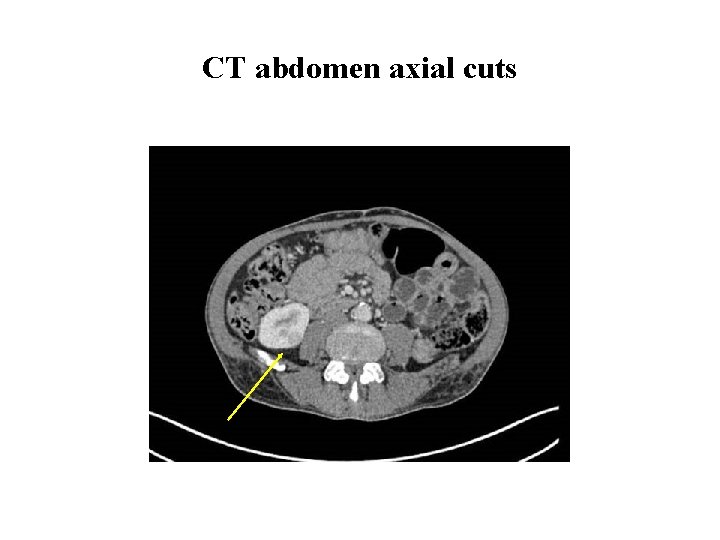
CT abdomen axial cuts
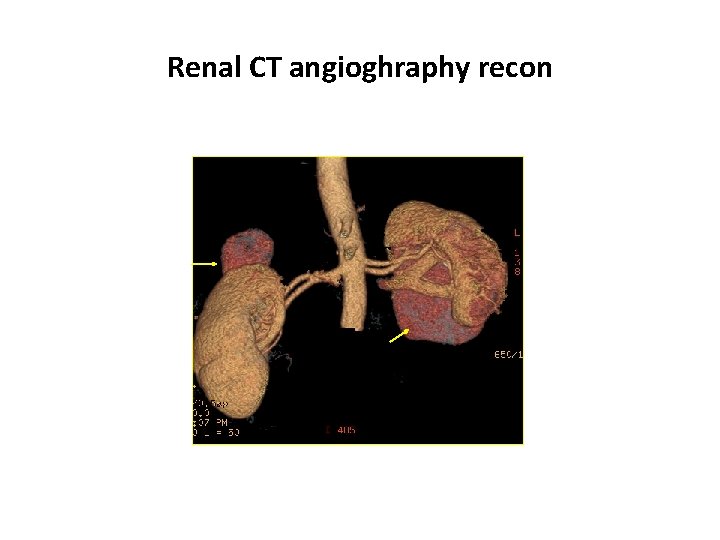
Renal CT angioghraphy recon

Planning - B/L renal SOLs, 2 SOLs in right kidney, large midpolar mass in left kidney MDT discussion Ø Surgery planned in two sessions Right side opted first ( Partial nephrectomy) (technically less challenging due to exophytic polar lesions) Left side planned radical/partial nephrectomy in second session

Right open partial nephrectomy (PN) Right loin incision, retroperitoneal approach (prior right ureteric stenting). Kidney mobilization and hilar control Renal artery clamped, excision of upper and lower pole lesions Frozen section of deep margins of both lesions: negative Cold ischaemia time 30 min

Right PN • Good post op recovery • S. cr. 0. 99 mg/dl and HB 13 gm/dl • Biopsy report: Chromophobe renal cell carcinoma, p. T 1 b(m)Nx Resection margin free, no LVI, no sarcomoid differentiation Sizes: 4. 2 cm upper pole lesion, 2 cm. lower pole lesion

Post right PN follow up Patient doing well No haematuria, wound healed well. RFT: Normal (s. creatinine 0. 8) DMSA scan (after 1 month of right PN) 1. Differential function: Rt. kidney - 63. 26% & Lt. kidney - 36. 74% 2. Large left parapelvic SOL photophenic area

Left partial nephrectomy (PN) • Left loin incision retroperitoneal approach (prior left ureteric stenting) • Kidney completely mobilized • Pelvis dissected from mass • Hilar dissection continued to segmental arteries, selective ligation of artery supplying renal mass Frozen section of deep cut margin: negative

Left PN • Post op period: good recovery • S. cr. 0. 8 mg/dl, HB 10. 6 gm/dl • Biopsy report: Chromophobe Renal cell Carcinoma, p. T 2 a Resection margin free, Size 8. 2 cm
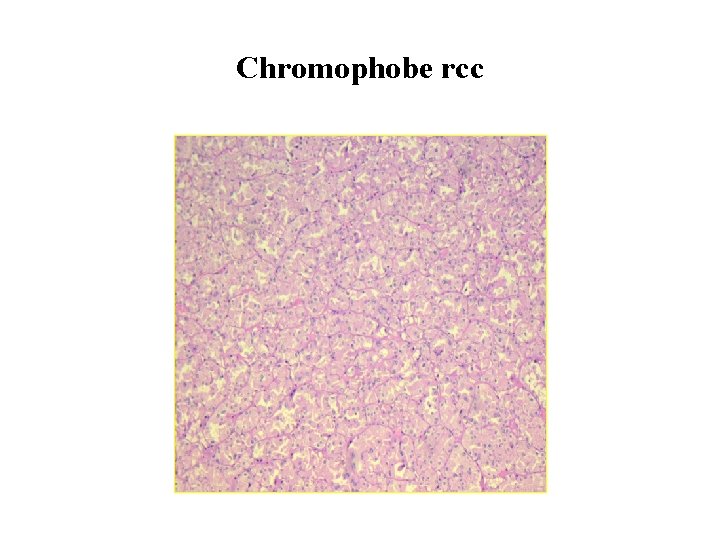
Chromophobe rcc
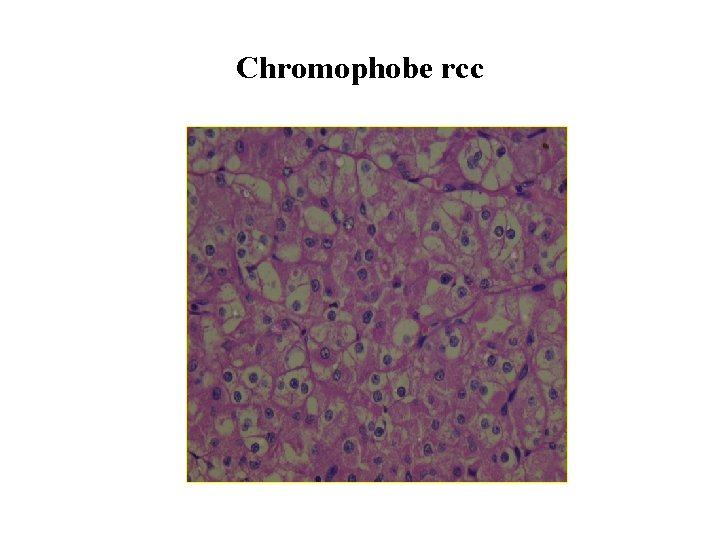
Chromophobe rcc

Follow up • Patient doing well, • CBC, RFT, LFT normal • CT abdomen: no local recurrance

Discussion 1 Chromophobe RCC

Chromophobe RCC • First described by Thoenes and colleagues in 1985, as a distinctive histologic subtype of RCC • Represents 5% of all RCCs • Derived from the cortical portion of the collecting duct (Algaba et al, 2011).

Chromophobe RCC • Commonly seen in the Birt-Hogg-Dubé syndrome ( associated with cutaneous benign lesions) • Most cases are sporadic (Linehan and Ricketts, 2013).

Chromophobe RCC Morphologically • Chromophobe RCC typically appears as a well circumscribed, homogeneous, tan tumor Microscopically • Chromophobe RCC include distinct cytoplasmic borders, perinuclear “halos, ” and nuclear “raisins. ”.

Chromophobe RCC • Most studies suggest a better prognosis for localized chromophobe RCC than for clear cell RCC • Poor outcome in the subset of patients with sarcomatoid features or metastatic disease (Renshaw et al, 1996; Klatte et al, 2008)

Chromophobe RCC • > 90% 5 years disease free survival for localised chromophobe rcc after treatment (Klatte et al, 2008; Deng and Melamed, 2012). • Limited data exist regarding treatment of metastatic chromophobe RCC (Tannir et al, 2012; Kroeger et al, 2013).

Discussion 2 Partial nephrectomy

Partial nephrectomy • Concept of PN – started when importance of preservation of renal parenchyma was realized. • 1890, Czerny performed partial nephrectomy.

Partial nephrectomy • Significant renal functional advantage • Incidence of Grade 3 CKD was more common with RN ( 65% v/s 20%) • More severe CKD (e. GFR < 60 m. L/min/1. 73 m 2 ) was also more common with RN ( 36% v/s 5%) (Huang et al, 2006; Russo and Huang, 2008 – Memorial Sloan Kettering Cancer Center)

Partial nephrectomy Ø Long term oncologic outcome equivalent to radical nephrectomy Curr Opin Urol 2015 Mar; 25(2): 95 -9. doi 0. 1097/MOU. 0000000140. Anatomic partial nephrectomy: technique evolution. Azhar RA Metcalfe C Gill I Ø T 1 a & T 1 b RCC with overall Cancer free survival rate over 90%. Uzzo and Novick, 2001; Campbell et al 2009

Indications of PN All patients with c. T 1 RCC whenever feasible Especially in Pts. with a solitary kidney Multiple small and/ or bilateral tumours Pts. with or at risk of chronic renal disease

• Guidelines recommend partial nephrectomy whenever technically feasible, independent of tumor size (Campbell 2009; Ljungberg 2015) • “is recommended in patients with clinical T 1 a tumours and should be favoured above radical nephrectomy in clinical T 1 b tumours whenever technically feasible” (Grade A and B recommendations EAU 2016)

Bilateral renal tumours • The simpler partial nephrectomy is performed first • MAG 3 renogram in the postoperative kidney. • Then more complicated partial or radical nephrectomy is performed on the contralateral kidney

Thank you.
- Slides: 38