A brief introduction to Recommended Summary Plan for

A brief introduction to Recommended Summary Plan for Emergency Care and Treatment Alison Richardson Member of Re. SPECT Working Group Professor of Cancer Nursing & End of Life Care University of Southampton & University Hospital Southampton Re. SPECT

Re. SPECT • Background to Re. SPECT • What Re. SPECT is (and what it isn’t) • Aims of Re. SPECT • Key parts of the Re. SPECT process • Implementing Re. SPECT

Background — the evidence October 2014 DNACPR from best evidence to best policy and practice http: //www. journalslibrary. nihr. ac. uk/ hsdr/volume-4/issue-11#abstract Re. SPECT

Background DNACPR decisions and discussions have led to: • Negative patient/public perceptions • Negative clinicians’ perceptions • Complaints • Litigation • Negative media reports Re. SPECT

Background Common themes • Poor or absent communication • Bad decision-making • Poor or absent documentation Re. SPECT

Background Court of Appeal 2014 DNACPR decisions “… presumption in favour of patient involvement. . . ” Re. SPECT

How could we do better? • Discuss CPR in the context of broader care plans • Discuss treatment to be given • More frequent (routine) conversations • National documentation Re. SPECT

Re. SPECT was created by…

What is Re. SPECT? Re. SPECT – an alternative process for discussing, making and recording recommendations about future emergency care and treatment, including CPR Re. SPECT – developed by many stakeholders including patients, doctors, nurses and ambulance clinicians, to try to achieve a process that will be adopted nationally Re. SPECT records treatments to be considered as well as those that are not wanted or would not work Re. SPECT encourages people to plan ahead for their care and treatment in a future emergency in which they are unable to make decisions Re. SPECT

Re. SPECT – what it isn’t! • not another DNACPR form • not specifically for end-of-life care • not a substitute for an advance care plan • not an ‘order’ Re. SPECT

Re. SPECT – Aims • More conversations between people and clinicians • More planning in advance • Good communication • Good decision-making • Shared decision-making whenever possible • Good documentation • Cross-boundary recognition • Better care Re. SPECT

Re. SPECT – what’s needed? A change of culture involving: • • health and care professionals members of the public Re. SPECT

Re. SPECT – who is it for? • Anyone, but especially people: ▫ with particular healthcare needs ▫ nearing the end of their lives or at risk of cardiac arrest ▫ who want to record their preferences for any reason • Re. SPECT is best completed when a person is relatively well, so that their preferences and agreed clinical recommendations are known if a crisis occurs • If someone with no Re. SPECT form has an acute illness, consider discussing and completing Re. SPECT as soon as possible Re. SPECT

Re. SPECT – other features • Re. SPECT can be used for people of any age • When used for a child or young person must be appropriate parental involvement • Re. SPECT can complement other documents such as advance care plans but does not replace them • If a person has a completed Re. SPECT form there should be no need for a separate CPR decision form or TEP Re. SPECT
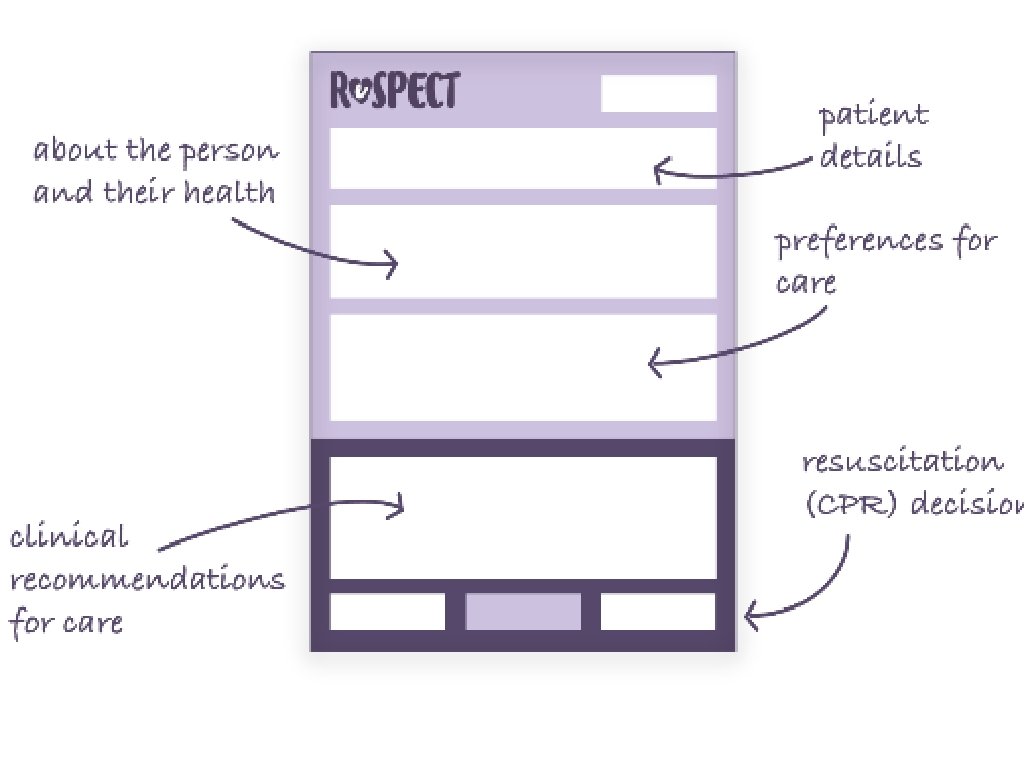
Key parts of the process Re. SPECT

Introducing & Using Re. SPECT • • • Re. SPECT made available for adoption by health and care communities in February 2017. Introduced in some localities as part of a 3 year NIHR funded research evaluation Moving to next phase where health and care communities wishing to adopt Re. SPECT offered access to materials needed to plan implementation. Interested organisations should join the Implementation Network. Implementation of Re. SPECT will be a gradual process, different health communities adopting and implementing using different timeframes, according to local or regional circumstances Health communities adopting Re. SPECT are directly responsible for establishing an implementation group and developing implementation plan (e. g. training, resources, risks, interdependencies and audit). Re. SPECT

Where to find out more… • On the Re. SPECT process and implementation network http: //www. respectprocess. org. uk/ • Review the website and materials - specimen Re. SPECT form, the FAQs, the Implementation Roadmap and ‘Act and Adopt’ documents • Feedback is welcomed. Re. SPECT aims to be a dynamic process that responds to, and develops further from, feedback • BMJ articles accessible via the website: Analysis: Resuscitation policy should focus on the patient, not the decision Practice Pointer: Emergency care and resuscitation plans • BMJ Talk Medicine podcast on emergency care plans at end of life http: //www. bmj. com/archive/podcasts Re. SPECT

A word from patients “Let's face it - no-one really wants to think about what might happen if they were to become critically ill! But of course the best way to do that is by planning ahead and doing the thinking while there's no crisis to deal with. That way you have time to think clearly, take advice, and share your thoughts and wishes with the people who might have to care for you. The Re. SPECT process provides this opportunity in a clear, straightforward way. It will hopefully make it much easier for everyone, both inside and outside the healthcare professions, to make these challenging decisions together. ” Viv Cummin, Patient Representative, Re. SPECT Working Group Re. SPECT
- Slides: 18