8 Complement pathways of activation biological significance 9

8. Complement, pathways of activation, biological significance. 9. Alternative pathway of complement activation and its regulation. 10. Classical pathway of complement activation and its regulation. 11. The biological significance of complement and its mechanisms of regulation. 12. Basophils and mast cells and their role in the immune reactions. 13. Immune mechanisms of the inflammation (local and systemic reaction). 14. Physiological mechanisms of regulation of the immune system. Cytokines 15. Cytokines (overview, disposal according to their functions). 16. Antigen, hapten, epitope - basic characteristics. T-independent antigens, superantigens. Sequestered antigens - immunologically privileged tissue. 17. Chemical nature and molecular size of antigens. Degree of foreignness.

Complement system
Complement Humoral component of nonspecific immunity (over 30 serum and membrane proteins; C 1 –C 9, factor B, factor. D…) Removal microorganisms, own altered cells (apoptotic cells) and immune complexes Complement proteins are synthesized by the liver, less by tissue macrophages and fibroblasts Complement components circulate in the blood in inactive form Complement proteins activate in a cascade
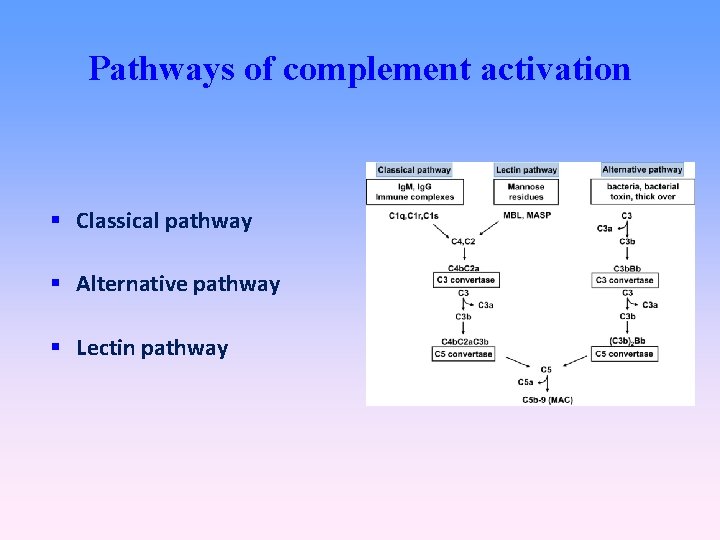
Pathways of complement activation Classical pathway Alternative pathway Lectin pathway
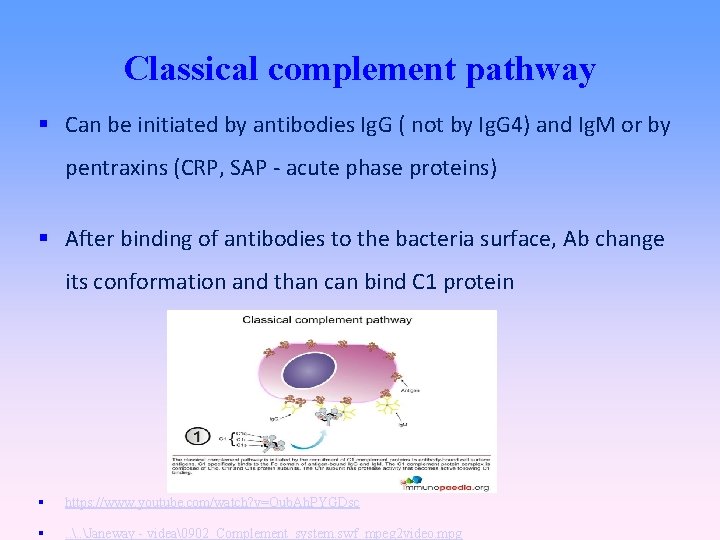
Classical complement pathway Can be initiated by antibodies Ig. G ( not by Ig. G 4) and Ig. M or by pentraxins (CRP, SAP - acute phase proteins) After binding of antibodies to the bacteria surface, Ab change its conformation and than can bind C 1 protein https: //www. youtube. com/watch? v=Oub. Ah. PYGDsc . . Janeway - videa�902_Complement_system. swf_mpeg 2 video. mpg

Alternative complement pathway C 3 component of complement rarely spontaneously breaks into C 3 b and C 3 a C 3 b can covalently bind on the surface of a particle (own cell, microorganism) or reacts with water, thereby inactivates https: //www. youtube. com/watch? v=qga 3 Wn 76 d 9 w

Lectin complement pathway Is initiated by serum mannose binding lectin (MBL) MBL binds to mannose residues on the surface of some microbes, after this binding starts cleave C 4 and C 2 This way is similar to the classical pathway https: //www. youtube. com/watch? v=ut. Qd. PPee. TLQ

Terminal (lytic) phase of the complement cascade C 5 b fragments creates a complex with C 6, C 7 and C 8, the complex dive into the lipid membrane of the cell and attache into a circle 13 -18 molecules of C 9 => MAC (membrane attack complex), forms a transmembrane channel, which causes osmotic lysis of the target cell (G-bacteria, protozoans, some viruses). Many microorganisms are resistant to this lytic effect of complement (protection by cell wall).
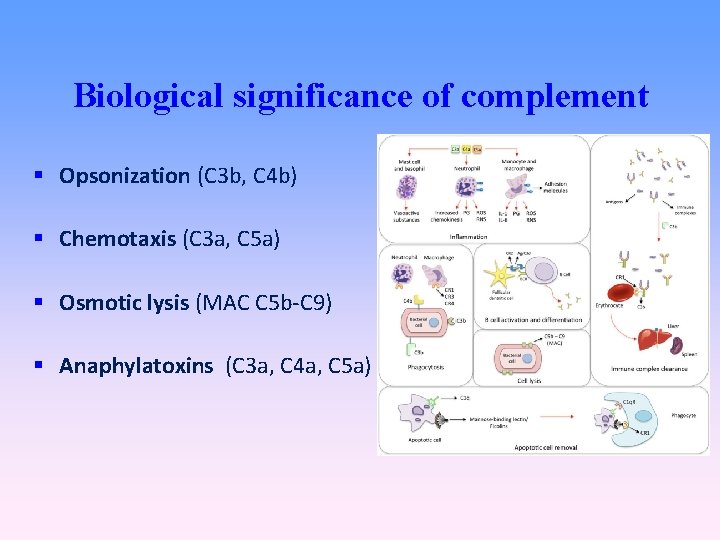
Biological significance of complement Opsonization (C 3 b, C 4 b) Chemotaxis (C 3 a, C 5 a) Osmotic lysis (MAC C 5 b-C 9) Anaphylatoxins (C 3 a, C 4 a, C 5 a)
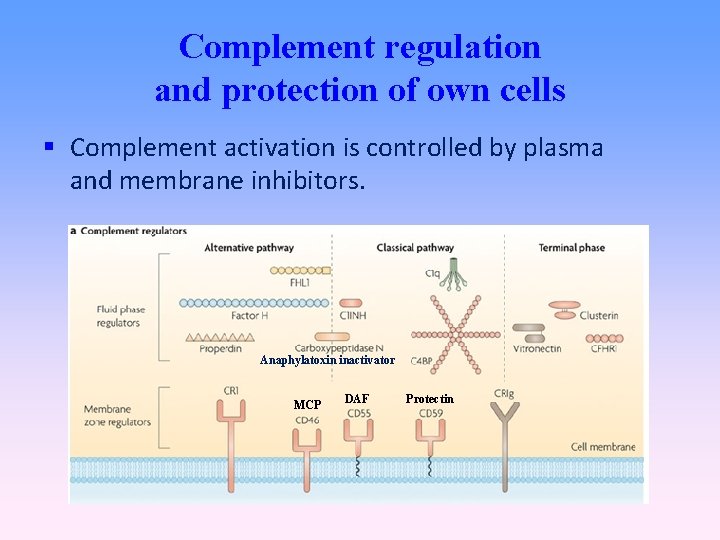
Complement regulation and protection of own cells Complement activation is controlled by plasma and membrane inhibitors. Anaphylatoxin inactivator MCP DAF Protectin
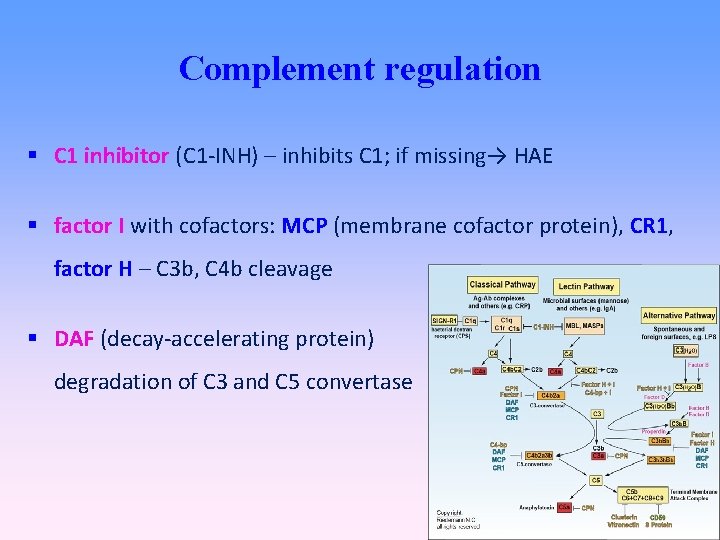
Complement regulation C 1 inhibitor (C 1 -INH) – inhibits C 1; if missing→ HAE factor I with cofactors: MCP (membrane cofactor protein), CR 1, factor H – C 3 b, C 4 b cleavage DAF (decay-accelerating protein) degradation of C 3 and C 5 convertase
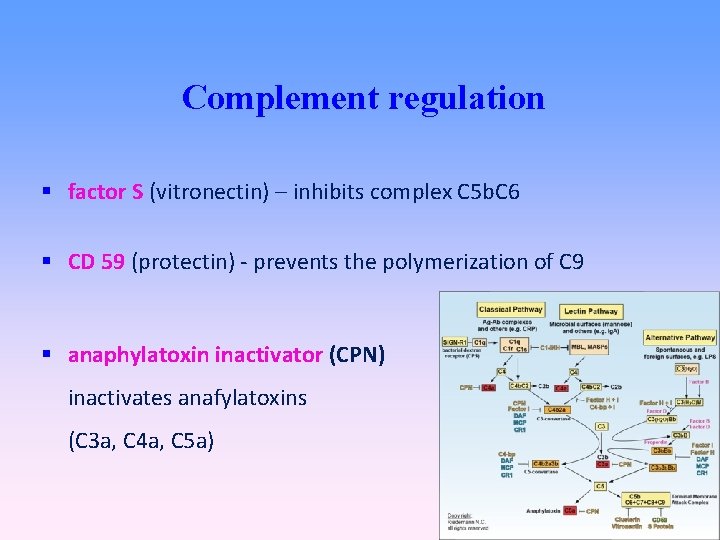
Complement regulation factor S (vitronectin) – inhibits complex C 5 b. C 6 CD 59 (protectin) - prevents the polymerization of C 9 anaphylatoxin inactivator (CPN) inactivates anafylatoxins (C 3 a, C 4 a, C 5 a)

Complement receptors Bind fragments of complement components (C 3 b, C 4 b) CR 1 - on various cells - promotes C 3 b, C 4 b decay - stimulate phagocytosis - erythrocyte transport of immune complexes CR 2 - on B lymphocytes and FDC - activation of B cells CR 3, CR 4 - on phagocytes - opsonization, adhesion
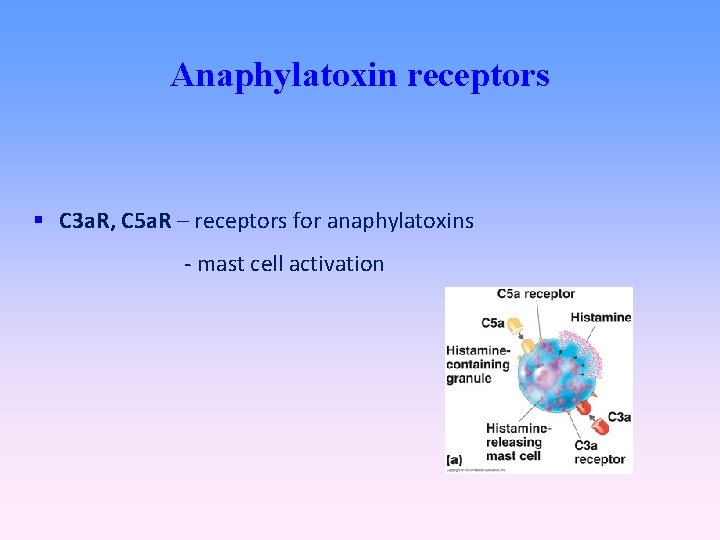
Anaphylatoxin receptors C 3 a. R, C 5 a. R – receptors for anaphylatoxins - mast cell activation

Basophils and mast cells and their importance in immune responses
Mast cells Mucosal mast cells Mucous membranes of respiratory and gastrointestinal tract Produce histamine, serotonin, heparin, tryptase, leukotriene C 4. . . Participate in parasitosis, allergy and inflammation Connective tissue mast cells Are not participating in parasitosis and allergy

Mast cell functions Apply during inflammation, in angiogenesis, in tissue remodeling Defense against parasitic infections In pathological circumstances, responsible for the allergic reactions (immunopathological reaction type I)
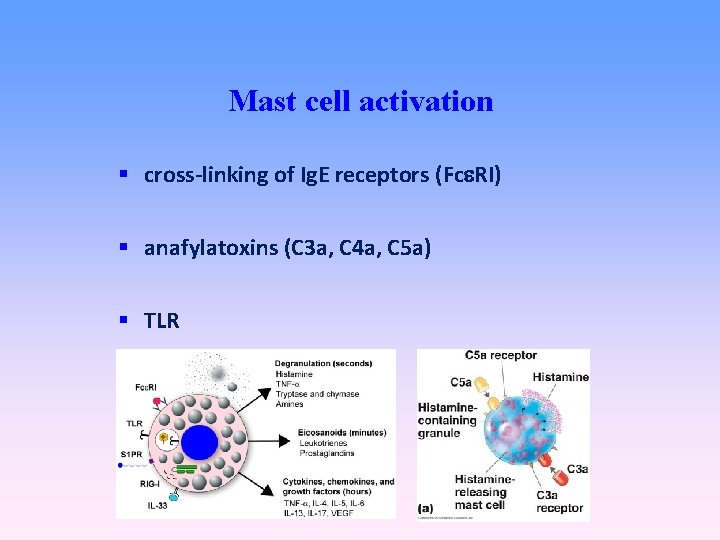
Mast cell activation cross-linking of Ig. E receptors (Fc RI) anafylatoxins (C 3 a, C 4 a, C 5 a) TLR
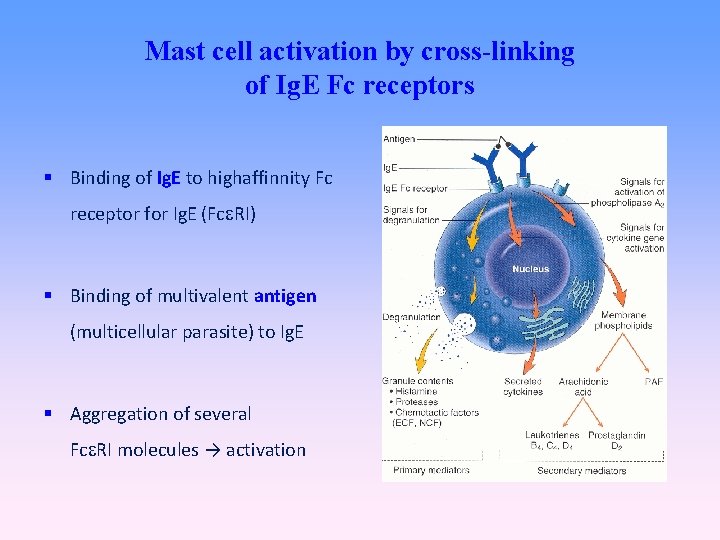
Mast cell activation by cross-linking of Ig. E Fc receptors Binding of Ig. E to highaffinnity Fc receptor for Ig. E (Fc RI) Binding of multivalent antigen (multicellular parasite) to Ig. E Aggregation of several Fc RI molecules → activation

Secretory products of mast cells Cytoplasmatic granules: hydrolytic enzymes, histamine, heparin, chondroitin sulphate, serotonin Histamine - vasodilation, ↑ vascular permeability (erythema, edema, itching), bronchoconstriction, ↑ intestinal peristalsis, ↑mucus secretion in the respiratory tract and GIT (helps eliminate the parasite) Arachidonic acid metabolites (leukotriene C 4, prostaglandin D 2) Cytokines (TNF, TGF , IL-4, 5, 6. . . ) https: //www. youtube. com/watch? v=Mo. M 5 JY_Ee. Ro
Basophils Differentiate from myeloid precursor Receptor equipment, content of granules, the mechanisms of stimulation and functions are very similar to mast cells Play a role in parasitic infections and allergies Basophil activation markers: CD 63, (CD 203)

Immune mechanisms of inflammation (Local and systemic reactions)

Inflammation Is a protective physiological response leading to protection against infection in damaged sites, localization of damage, elimination of necrotic cells and tissue repair.

Causes of inflammation Physical injury Infection by pathogens Damage caused by chemicals Cancer Alergic disease Autoimmune disease

Local body's response to inflammation Classical signs - pain (dolor), fever (calor), redness (rubor), swelling (tumor)
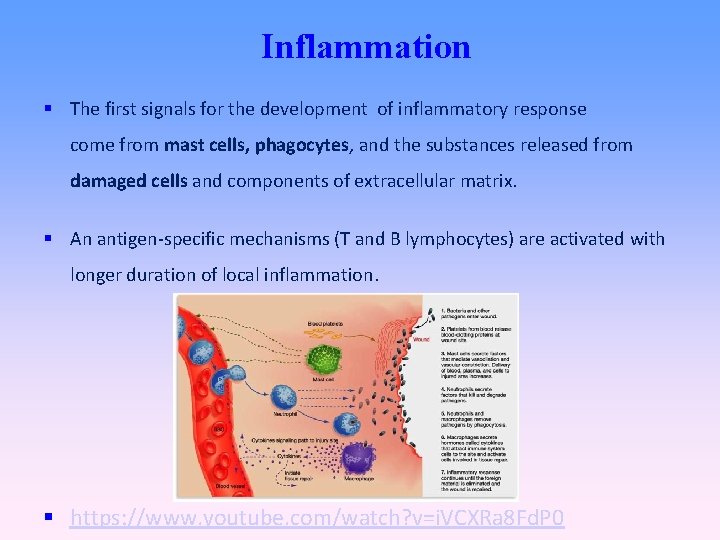
Inflammation The first signals for the development of inflammatory response come from mast cells, phagocytes, and the substances released from damaged cells and components of extracellular matrix. An antigen-specific mechanisms (T and B lymphocytes) are activated with longer duration of local inflammation. https: //www. youtube. com/watch? v=i. VCXRa 8 Fd. P 0

Inflammation – local reaction Vasodilation, ↑ vascular permeability (histamine, serotonin, bradykinin, complement components C 3 a, C 5 a, leukotrienes , prostaglandins, …) → rednes, swelling ↑expression of adhesion molecules on endothelia (TNF , IL-1) → leukocyte adhesion to the endothelium Influence of local nerve endings via prostaglandins → pain • Increased local temperature (IL-1, IL-6, TNF, prostaglandins)

Inflammation - systemic reaction Leukocytosis Fever (TNF, IL-1, IL-6, IFN ) ↑ tissue metabolism ↑ mobility of leukocytes ↑ formation of IFN, cytokines, Ig ↑ expression of Hsp Acute phase proteins (IL-6, TNF , IL-1) CRP, SAP - opsonization and complement activation
Tissue repair Elimination of damaged cells by phagocytes Activation of fibroplastic mechanisms Activation of angiogenesis Regeneration and tissue remodeling TGF

Physiological mechanisms of regulation of the immune system

Physiological mechanisms of regulation Regulation by antigen Regulation by antibodies Regulation by cytokines and cellular contact Negative regulation of efector cells Supression mediated by T cells Other factors
Cytokines (Tissue hormones)

Cytokines Regulatory proteins and glycoproteins produced by leukocytes and other cells Are known as interleukins (IL-1…IL-38) (except: TNF, lymphotoxin, TGF, interferons, CSF and growth factors) Essential regulators of the immune system Apply also in angiogenesis, tissue regeneration, carcinogenesis, treatment of many brain functions, embryonic development. . .
Cytokines Effects of cytokines- autocrine - paracrine - endocrine Cytokines - secreted - membrane (CD 80, CD 86, CD 40 L, Fas. L. . )
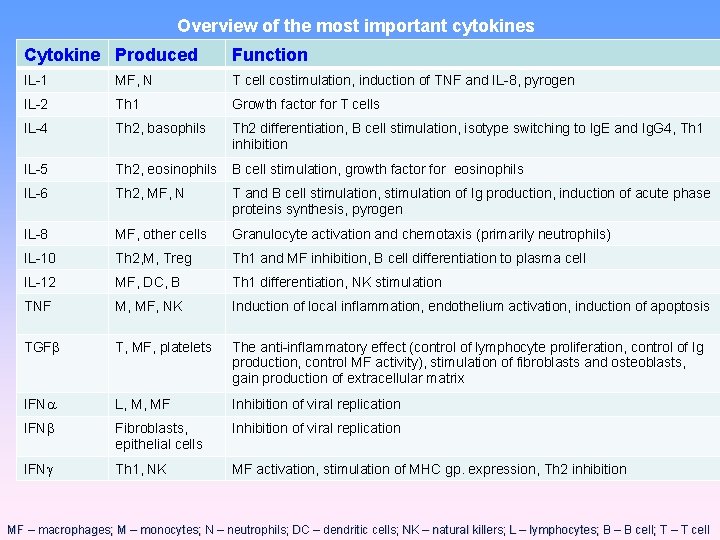
Overview of the most important cytokines Cytokine Produced Function IL-1 MF, N T cell costimulation, induction of TNF and IL-8, pyrogen IL-2 Th 1 Growth factor for T cells IL-4 Th 2, basophils Th 2 differentiation, B cell stimulation, isotype switching to Ig. E and Ig. G 4, Th 1 inhibition IL-5 Th 2, eosinophils B cell stimulation, growth factor for eosinophils IL-6 Th 2, MF, N T and B cell stimulation, stimulation of Ig production, induction of acute phase proteins synthesis, pyrogen IL-8 MF, other cells Granulocyte activation and chemotaxis (primarily neutrophils) IL-10 Th 2, M, Treg Th 1 and MF inhibition, B cell differentiation to plasma cell IL-12 MF, DC, B Th 1 differentiation, NK stimulation TNF M, MF, NK Induction of local inflammation, endothelium activation, induction of apoptosis TGF T, MF, platelets The anti-inflammatory effect (control of lymphocyte proliferation, control of Ig production, control MF activity), stimulation of fibroblasts and osteoblasts, gain production of extracellular matrix IFN L, M, MF Inhibition of viral replication IFN Fibroblasts, epithelial cells Inhibition of viral replication IFN Th 1, NK MF activation, stimulation of MHC gp. expression, Th 2 inhibition MF – macrophages; M – monocytes; N – neutrophils; DC – dendritic cells; NK – natural killers; L – lymphocytes; B – B cell; T – T cell

Clasification of cytokines by functions 1. Proinflammatory cytokines (IL-1, IL-6, IL- 8, IL- 12, IL- 18, TNF) 2. Antiinflammatory cytokines (IL-4, IL-10, TGF ) 3. Cytokines with the activity of hematopoietic cells growth factor (IL-2, 3, 4, 5, 6, 7, 9, 11, 14, 15, CSF, SCF, LIF, EPO) 4. Cytokines applying in TH 2 humoral immunity (IL-4, 5, 9, 13) 5. Cytokines applying in the cell-mediated immunity TH 1 (IL-2, 12, IFN , GM-CSF, lymphotoxin) 6. Cytokines with anti-viral effect (IFN- , IFN- )

Cytokine receptors Consist of 2 or 3 subunits One subunit binds cytokine, other are associated with cytoplasmic signaling molecules (protein kinases) Signaling subunit is shared by several different cytokine receptors - called receptor family Signaling through these receptors may lead to proliferation, differentiation, activation of effector mechanisms or blocking the cell cycle and induction of apoptosis https: //www. youtube. com/watch? v=9 wd. ZLv. NKy. QY

Antigens

Antigen (immunogen) Substance which provokes specific immune response Usually proteins or polysaccharides (lipids and nucleic acids only in the combination with proteins or polysaccharides) Molecules > 5 k. Da (optimal size of the antigen molecules is about 40 k. Da)
Hapten Small molecules, that are able to induce specific immune response only after the attachment to the macromolecular carrier Separate haptens are not immunogenic Typically drugs (eg penicillin antibiotics, hydralazin)

Epitope (antigenic determinant) Part of the antigen which is recognized by immune system (lymphocytes- BCR, TCR, Ig) Cross-reactive antigens - share one or more identical or similar epitopes

Antigen Endogenous antigens - autoantigens (self Ag) Exogenous antigens - foreign substances from the environment Allergen - exoantigen that in the susceptible individuals can cause allergic reaction

Antigen properties Immunogenicity proteins> carbohydrates> macromolecule complexes (glycoproteins, nucleoproteins, and glycolipids)> lipids Specificity

Factors affecting immunogenicity Physical: Solubility - insoluble Ag more immunogenic Molecular weight - ideal 5 -40 k. Da Chemical: Structure - the number of determinants Degradability - "ease" of uncovering the determinants in antigen presenting cells (APC cell) Biological: Biological foreignness Genetic and physiological disposition of the body

Degree of foreignness Autogeneic - antigens of the same individual Syngeneic - antigens of genetically identical individuals Allogeneic (alloantigens) - antigens genetically different individuals of the same species Xenogeneic (heterologous) - antigens derived from individuals of different species
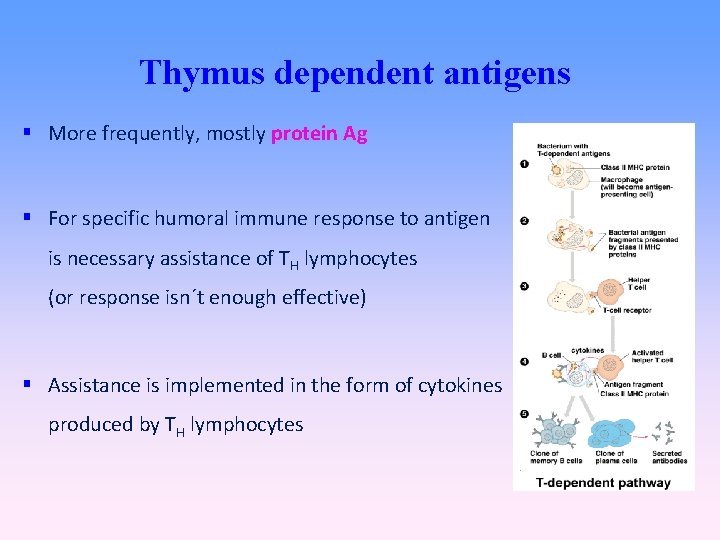
Thymus dependent antigens More frequently, mostly protein Ag For specific humoral immune response to antigen is necessary assistance of TH lymphocytes (or response isn´t enough effective) Assistance is implemented in the form of cytokines produced by TH lymphocytes
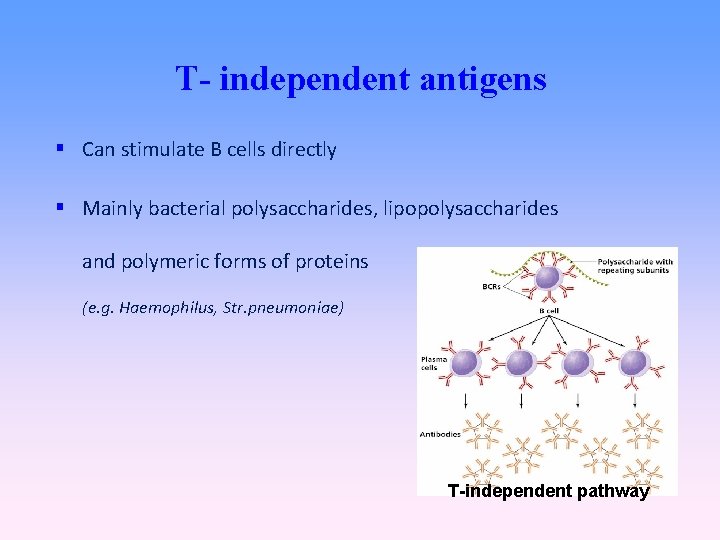
T- independent antigens Can stimulate B cells directly Mainly bacterial polysaccharides, lipopolysaccharides and polymeric forms of proteins (e. g. Haemophilus, Str. pneumoniae) T-independent pathway
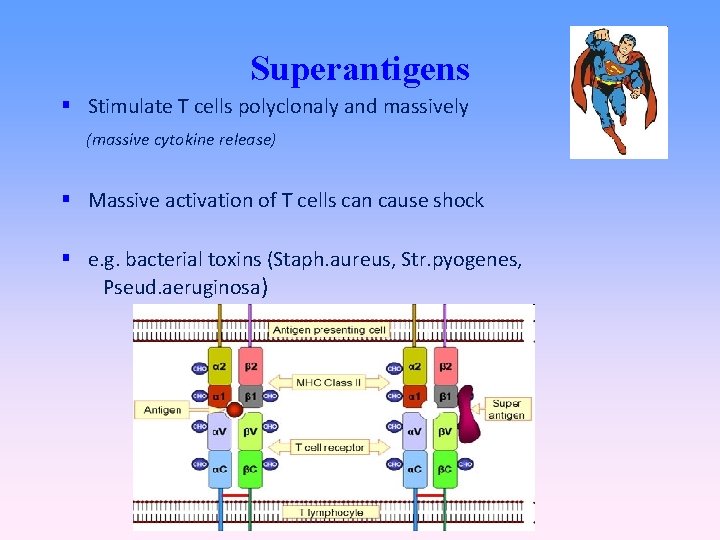
Superantigens Stimulate T cells polyclonaly and massively (massive cytokine release) Massive activation of T cells can cause shock e. g. bacterial toxins (Staph. aureus, Str. pyogenes, Pseud. aeruginosa)
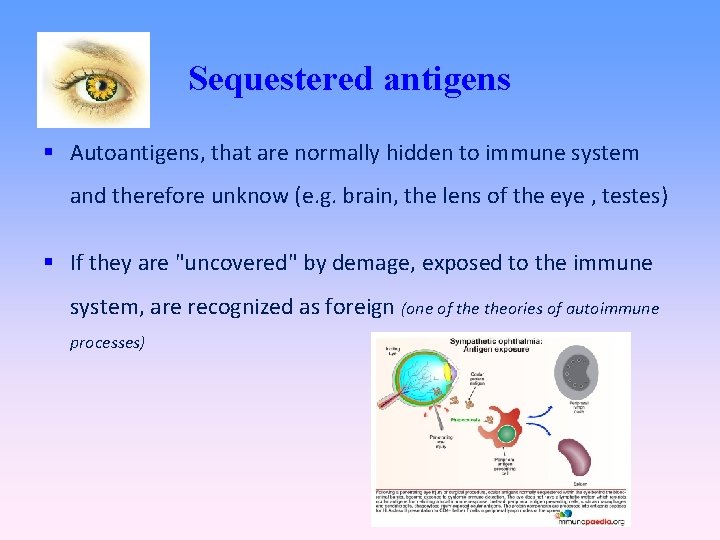
Sequestered antigens Autoantigens, that are normally hidden to immune system and therefore unknow (e. g. brain, the lens of the eye , testes) If they are "uncovered" by demage, exposed to the immune system, are recognized as foreign (one of theories of autoimmune processes)

Immunologically privileged sites CNS, eyes, gonads, placenta Are protected from potentially damaging inflammatory immune responses This tissues are far less rejected in allogeneic transplant This privileged position is not absolute

Immunologically privileged sites Protective mechanisms: Isolation from the immune system (blood-brain barrier) Preferences of Th 2 and suppression of Th 1 -response Production of immunosuppressive cytokines (TGFβ) Fas. L expression -active protection against effector T-lymphocytes Increased expression of membrane complement inhibitors

Thank you for your attention
- Slides: 52