56 Year Old Male with Familial Hypertriglyceridemia and














- Slides: 37

56 Year Old Male with Familial Hypertriglyceridemia and Hypertension Case Category: Primary Prevention, Familial Hypertriglyceridemia History of present illness: 56 year old male with extended history of high triglycerides (>1000 less than 6 months ago) and pancreatitis requiring hospitalization in past. Treatment with Tricor and Lovaza has had little effect. Has also tried Lipitor, Zeita, Niaspan and metformin but all with side effects. On a high carb, low fat diet.

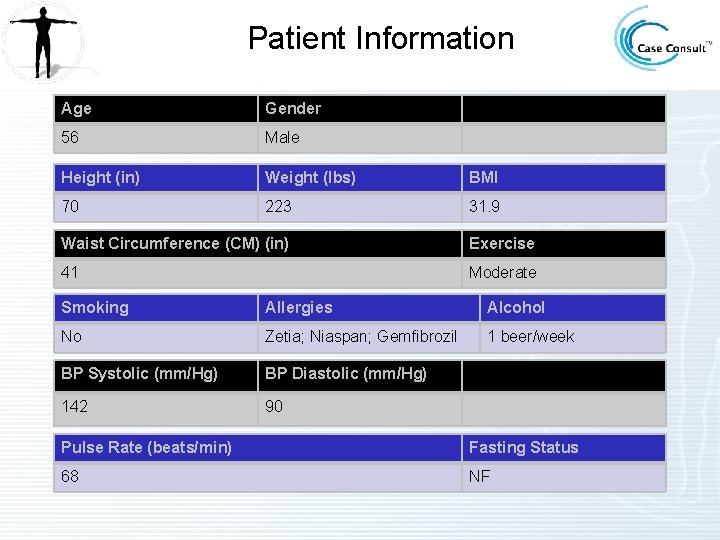
Patient Information Age Gender 56 Male Height (in) Weight (lbs) BMI 70 223 31. 9 Waist Circumference (CM) (in) Exercise 41 Moderate Smoking Allergies Alcohol No Zetia; Niaspan; Gemfibrozil 1 beer/week BP Systolic (mm/Hg) BP Diastolic (mm/Hg) 142 90 Pulse Rate (beats/min) Fasting Status 68 NF

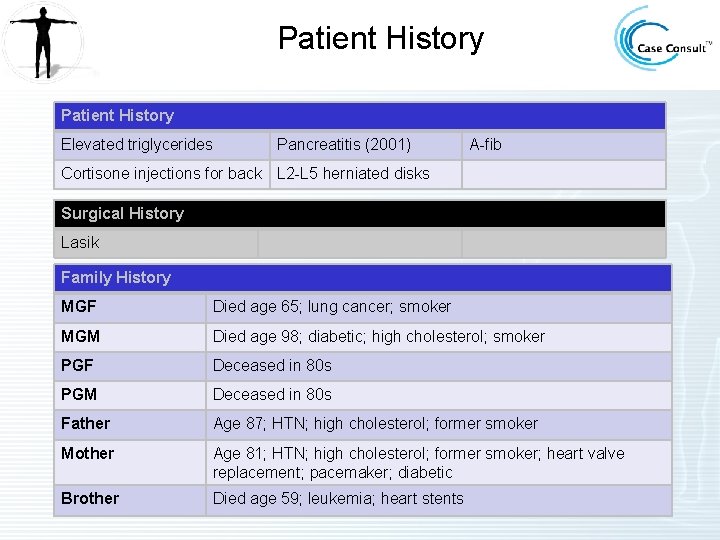
Patient History Elevated triglycerides Pancreatitis (2001) A-fib Cortisone injections for back L 2 -L 5 herniated disks Surgical History Lasik Family History MGF Died age 65; lung cancer; smoker MGM Died age 98; diabetic; high cholesterol; smoker PGF Deceased in 80 s PGM Deceased in 80 s Father Age 87; HTN; high cholesterol; former smoker Mother Age 81; HTN; high cholesterol; former smoker; heart valve replacement; pacemaker; diabetic Brother Died age 59; leukemia; heart stents

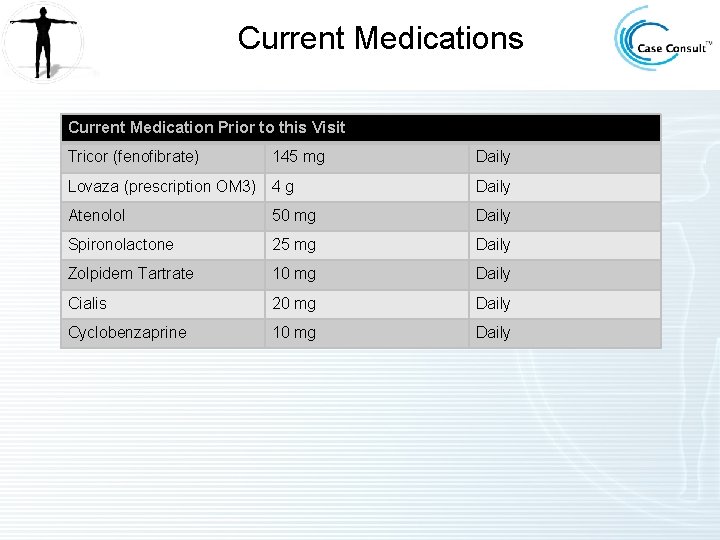
Current Medications Current Medication Prior to this Visit Tricor (fenofibrate) 145 mg Daily Lovaza (prescription OM 3) 4 g Daily Atenolol 50 mg Daily Spironolactone 25 mg Daily Zolpidem Tartrate 10 mg Daily Cialis 20 mg Daily Cyclobenzaprine 10 mg Daily

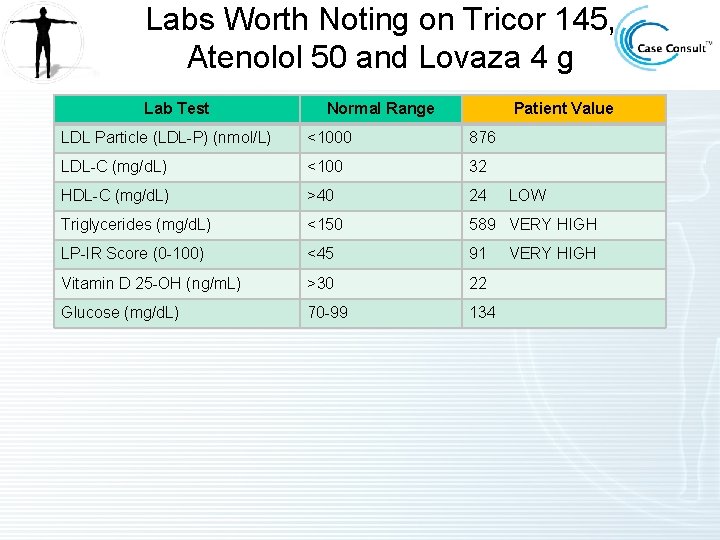
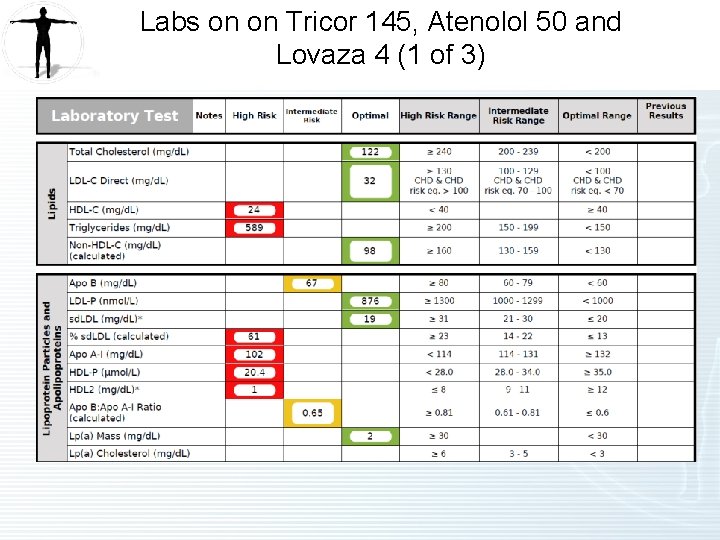
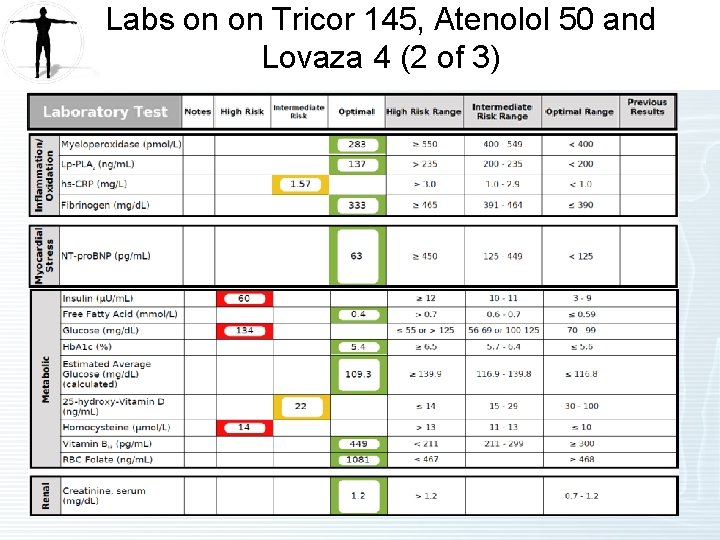
Labs Worth Noting on Tricor 145, Atenolol 50 and Lovaza 4 g Lab Test Normal Range Patient Value LDL Particle (LDL-P) (nmol/L) <1000 876 LDL-C (mg/d. L) <100 32 HDL-C (mg/d. L) >40 24 Triglycerides (mg/d. L) <150 589 VERY HIGH LP-IR Score (0 -100) <45 91 Vitamin D 25 -OH (ng/m. L) >30 22 Glucose (mg/d. L) 70 -99 134 LOW VERY HIGH

Questions to Consider • Question 1: Always need to rule out secondary causes of high triglycerides, including current medications (Atenolol). Insulin resistance, diabetes, hypothyroidism? High carb diet? Alcohol use? • Question 2: Assess medication compliance. Call pharmacy to make sure medications are filled monthly, etc. • Question 3: What were the specific issues with previous drug therapies? Which statin and which dose? How severe were the side effects? Regarding Niaspan, was it taken with aspirin, food, etc. ?

Labs on on Tricor 145, Atenolol 50 and Lovaza 4 (1 of 3)

Labs on on Tricor 145, Atenolol 50 and Lovaza 4 (2 of 3)

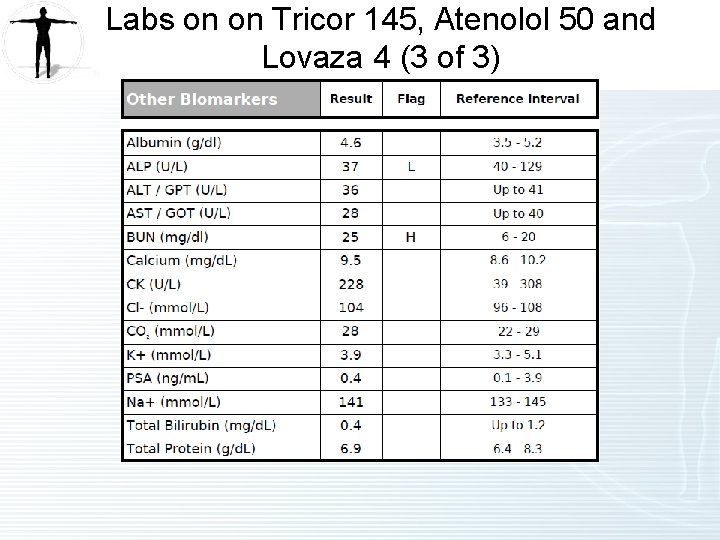
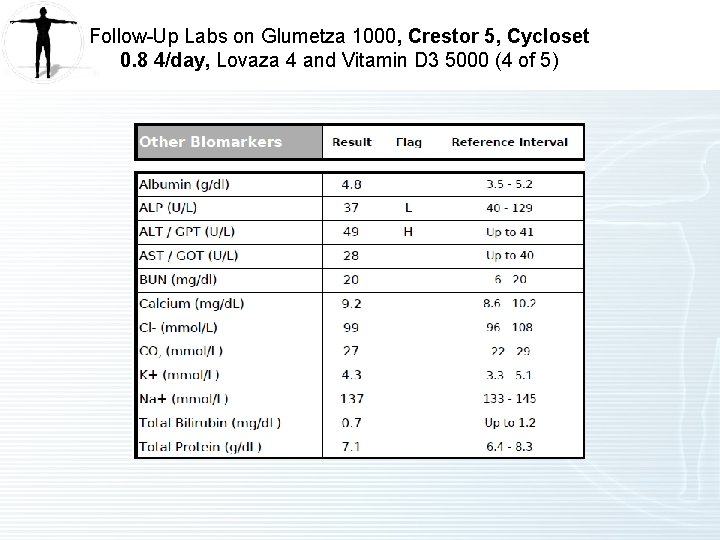
Labs on on Tricor 145, Atenolol 50 and Lovaza 4 (3 of 3)

NMR Lipo. Profile • Insert NMR Lipoprofile 06152011 MC 54 Insert

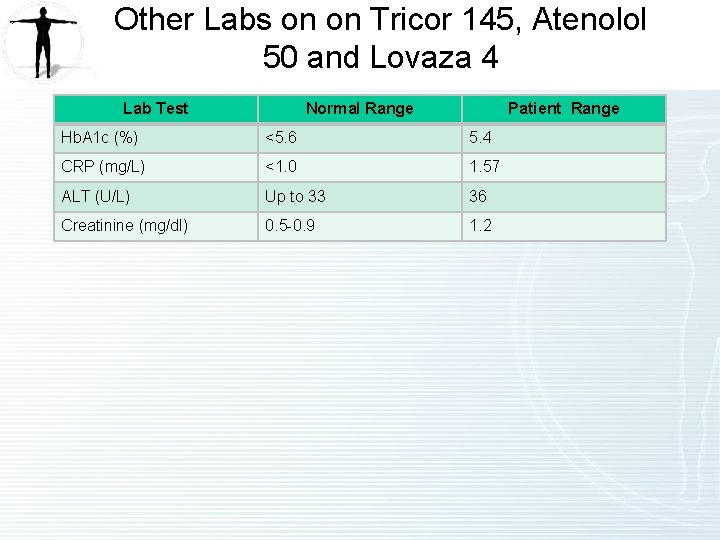
Other Labs on on Tricor 145, Atenolol 50 and Lovaza 4 Lab Test Normal Range Patient Range Hb. A 1 c (%) <5. 6 5. 4 CRP (mg/L) <1. 0 1. 57 ALT (U/L) Up to 33 36 Creatinine (mg/dl) 0. 5 -0. 9 1. 2

Initial Treatment & Management • • Advise low carb diet, increased exercise and to specifically avoid sugary beverages and alcohol. Consider stopping fenofibrate due to apparent lack of efficacy, borderline high creatinine and low HDL. For now continue. Continue Lovaza 4 g/day. Start Glumetza (metformin ER 500 mg) 2 -3 tablets daily with slow titration as tolerated. Brand name is better tolerated and he is concerned about GI side effects. Consider switching from Atenolol to Carvedilol (generic BID or Coreg CR once daily). Carvedilol a is beta blocker that is lipid neutral. Advise home blood pressure meter and switching to a beta blocker that does not affect lipids. Treat secondary causes for myalgia (vitamin D deficiency). Also consider CO Q 10 supplement with ubiquinol; Effective dose is 300 -600 mg/day in capsules with oil. This is in anticipation we may need to add statin. Start Vitamin D 3 5000 IU for 8 weeks and Vitamin D 2 50000 IU/week. Addressing deficiency will help muscle aching if a statin is needed for hypertriglyceridemia.

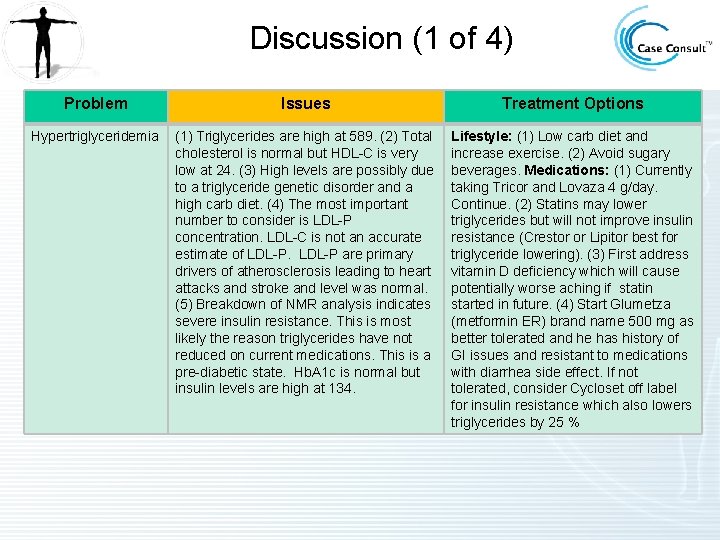
Discussion (1 of 4) Problem Issues Treatment Options Hypertriglyceridemia (1) Triglycerides are high at 589. (2) Total cholesterol is normal but HDL-C is very low at 24. (3) High levels are possibly due to a triglyceride genetic disorder and a high carb diet. (4) The most important number to consider is LDL-P concentration. LDL-C is not an accurate estimate of LDL-P are primary drivers of atherosclerosis leading to heart attacks and stroke and level was normal. (5) Breakdown of NMR analysis indicates severe insulin resistance. This is most likely the reason triglycerides have not reduced on current medications. This is a pre-diabetic state. Hb. A 1 c is normal but insulin levels are high at 134. Lifestyle: (1) Low carb diet and increase exercise. (2) Avoid sugary beverages. Medications: (1) Currently taking Tricor and Lovaza 4 g/day. Continue. (2) Statins may lower triglycerides but will not improve insulin resistance (Crestor or Lipitor best for triglyceride lowering). (3) First address vitamin D deficiency which will cause potentially worse aching if statin started in future. (4) Start Glumetza (metformin ER) brand name 500 mg as better tolerated and he has history of GI issues and resistant to medications with diarrhea side effect. If not tolerated, consider Cycloset off label for insulin resistance which also lowers triglycerides by 25 %

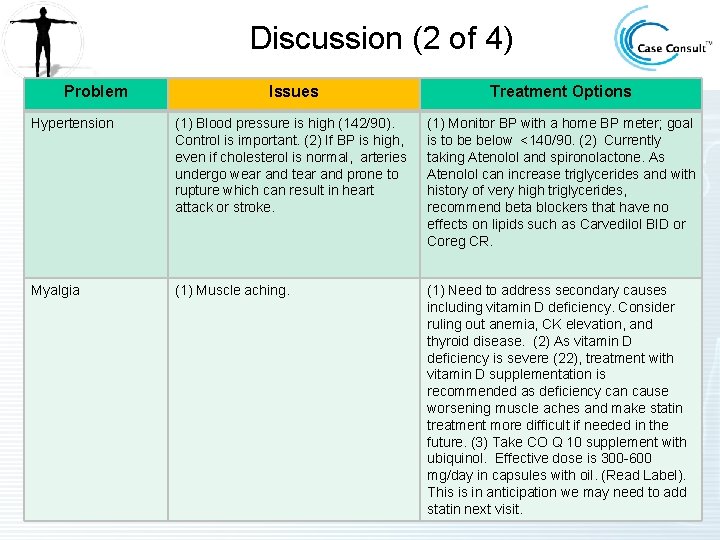
Discussion (2 of 4) Problem Issues Treatment Options Hypertension (1) Blood pressure is high (142/90). Control is important. (2) If BP is high, even if cholesterol is normal, arteries undergo wear and tear and prone to rupture which can result in heart attack or stroke. (1) Monitor BP with a home BP meter; goal is to be below <140/90. (2) Currently taking Atenolol and spironolactone. As Atenolol can increase triglycerides and with history of very high triglycerides, recommend beta blockers that have no effects on lipids such as Carvedilol BID or Coreg CR. Myalgia (1) Muscle aching. (1) Need to address secondary causes including vitamin D deficiency. Consider ruling out anemia, CK elevation, and thyroid disease. (2) As vitamin D deficiency is severe (22), treatment with vitamin D supplementation is recommended as deficiency can cause worsening muscle aches and make statin treatment more difficult if needed in the future. (3) Take CO Q 10 supplement with ubiquinol. Effective dose is 300 -600 mg/day in capsules with oil. (Read Label). This is in anticipation we may need to add statin next visit.

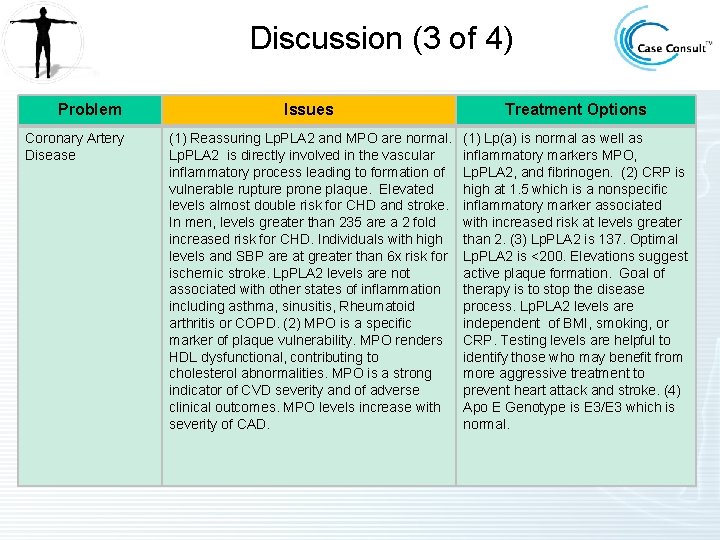
Discussion (3 of 4) Problem Coronary Artery Disease Issues Treatment Options (1) Reassuring Lp. PLA 2 and MPO are normal. Lp. PLA 2 is directly involved in the vascular inflammatory process leading to formation of vulnerable rupture prone plaque. Elevated levels almost double risk for CHD and stroke. In men, levels greater than 235 are a 2 fold increased risk for CHD. Individuals with high levels and SBP are at greater than 6 x risk for ischemic stroke. Lp. PLA 2 levels are not associated with other states of inflammation including asthma, sinusitis, Rheumatoid arthritis or COPD. (2) MPO is a specific marker of plaque vulnerability. MPO renders HDL dysfunctional, contributing to cholesterol abnormalities. MPO is a strong indicator of CVD severity and of adverse clinical outcomes. MPO levels increase with severity of CAD. (1) Lp(a) is normal as well as inflammatory markers MPO, Lp. PLA 2, and fibrinogen. (2) CRP is high at 1. 5 which is a nonspecific inflammatory marker associated with increased risk at levels greater than 2. (3) Lp. PLA 2 is 137. Optimal Lp. PLA 2 is <200. Elevations suggest active plaque formation. Goal of therapy is to stop the disease process. Lp. PLA 2 levels are independent of BMI, smoking, or CRP. Testing levels are helpful to identify those who may benefit from more aggressive treatment to prevent heart attack and stroke. (4) Apo E Genotype is E 3/E 3 which is normal.

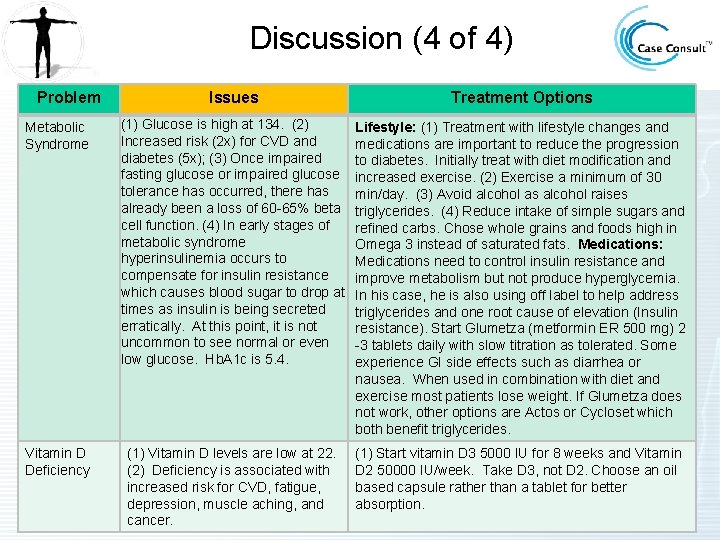
Discussion (4 of 4) Problem Issues Treatment Options Metabolic Syndrome (1) Glucose is high at 134. (2) Increased risk (2 x) for CVD and diabetes (5 x); (3) Once impaired fasting glucose or impaired glucose tolerance has occurred, there has already been a loss of 60 -65% beta cell function. (4) In early stages of metabolic syndrome hyperinsulinemia occurs to compensate for insulin resistance which causes blood sugar to drop at times as insulin is being secreted erratically. At this point, it is not uncommon to see normal or even low glucose. Hb. A 1 c is 5. 4. Lifestyle: (1) Treatment with lifestyle changes and medications are important to reduce the progression to diabetes. Initially treat with diet modification and increased exercise. (2) Exercise a minimum of 30 min/day. (3) Avoid alcohol as alcohol raises triglycerides. (4) Reduce intake of simple sugars and refined carbs. Chose whole grains and foods high in Omega 3 instead of saturated fats. Medications: Medications need to control insulin resistance and improve metabolism but not produce hyperglycemia. In his case, he is also using off label to help address triglycerides and one root cause of elevation (Insulin resistance). Start Glumetza (metformin ER 500 mg) 2 -3 tablets daily with slow titration as tolerated. Some experience GI side effects such as diarrhea or nausea. When used in combination with diet and exercise most patients lose weight. If Glumetza does not work, other options are Actos or Cycloset which both benefit triglycerides. Vitamin D Deficiency (1) Vitamin D levels are low at 22. (2) Deficiency is associated with increased risk for CVD, fatigue, depression, muscle aching, and cancer. (1) Start vitamin D 3 5000 IU for 8 weeks and Vitamin D 2 50000 IU/week. Take D 3, not D 2. Choose an oil based capsule rather than a tablet for better absorption.

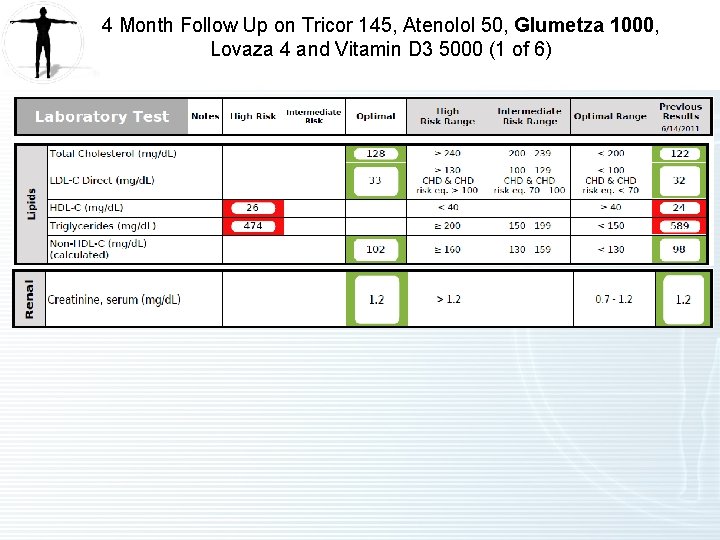
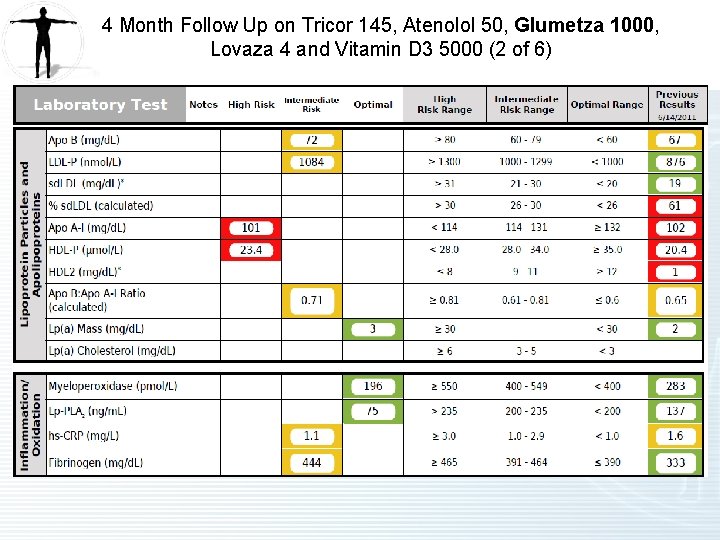
4 Month Follow Up on Tricor 145, Atenolol 50, Glumetza 1000, Lovaza 4 and Vitamin D 3 5000 (1 of 6)

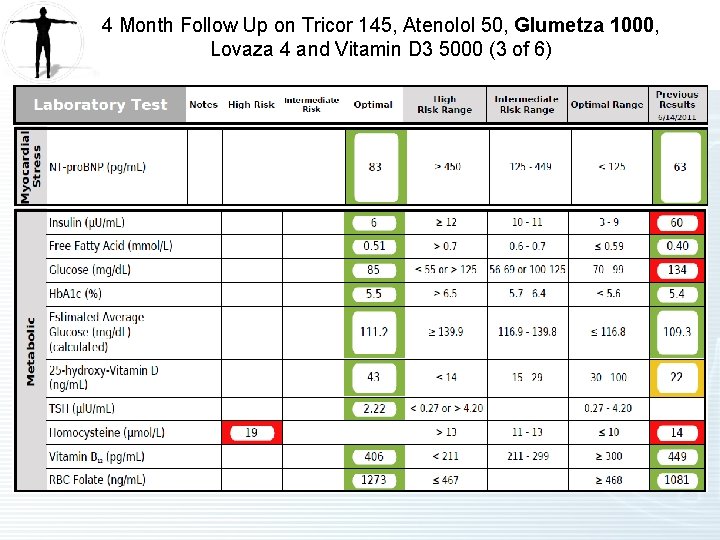
4 Month Follow Up on Tricor 145, Atenolol 50, Glumetza 1000, Lovaza 4 and Vitamin D 3 5000 (2 of 6)

4 Month Follow Up on Tricor 145, Atenolol 50, Glumetza 1000, Lovaza 4 and Vitamin D 3 5000 (3 of 6)

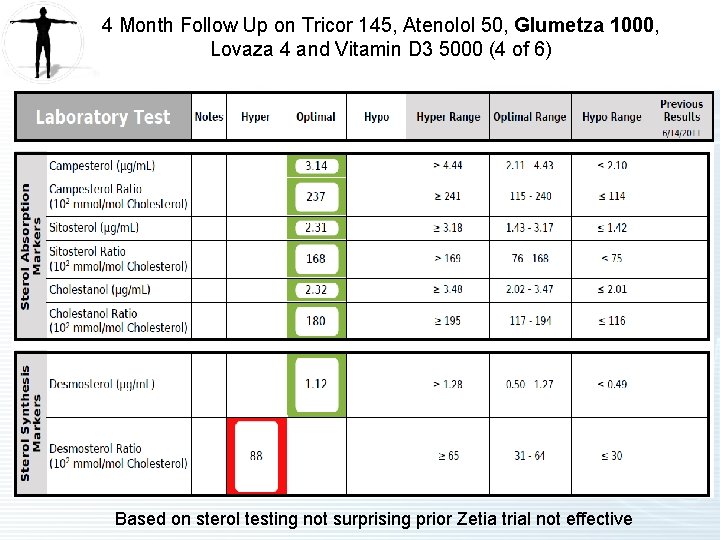
4 Month Follow Up on Tricor 145, Atenolol 50, Glumetza 1000, Lovaza 4 and Vitamin D 3 5000 (4 of 6) Based on sterol testing not surprising prior Zetia trial not effective

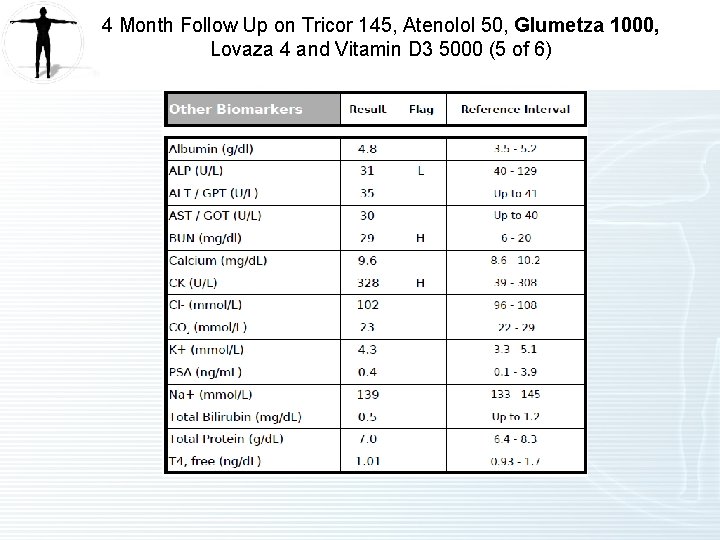
4 Month Follow Up on Tricor 145, Atenolol 50, Glumetza 1000, Lovaza 4 and Vitamin D 3 5000 (5 of 6)

4 Month Follow Up on Tricor 145, Atenolol 50, Glumetza 1000, Lovaza 4 and Vitamin D 3 5000 (6 of 6)

NMR Lipo. Profile • Insert NMR Lipoprofile 09272011 MC 54 Insert

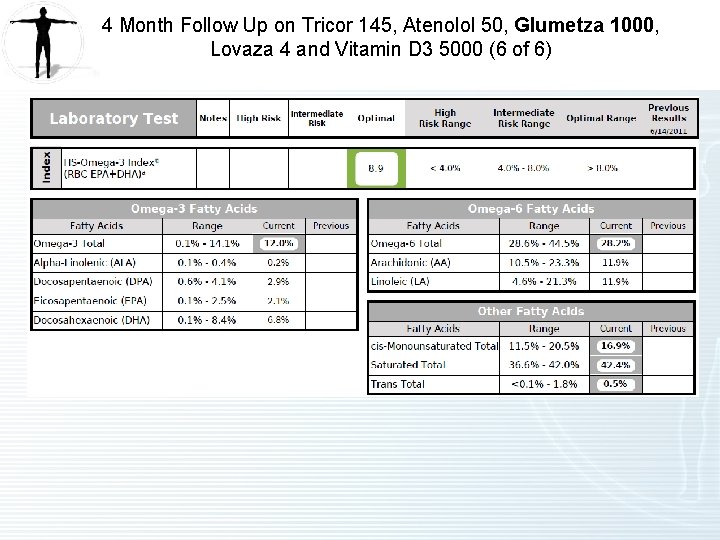
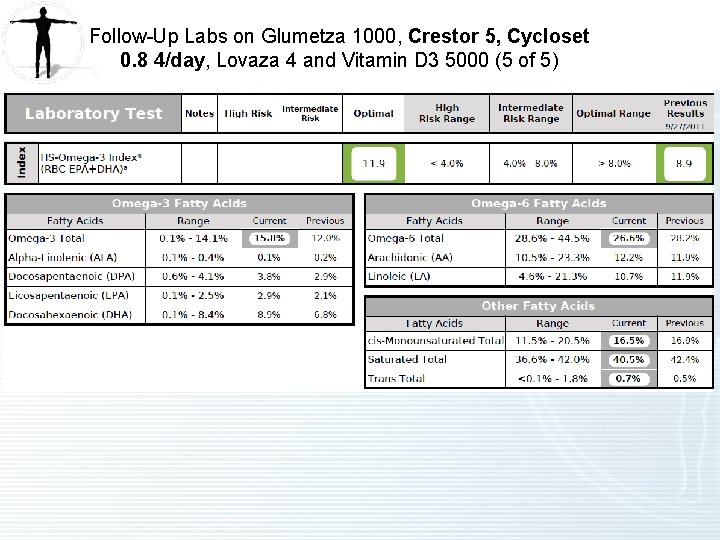
4 Month Follow Up on Tricor 145, Atenolol 50, Glumetza 1000, Lovaza 4 and Vitamin D 3 5000 (1 of 2) • Hypertriglyceridemia – Improved. – On Tricor 145, Lovaza 4 and Glumetza (metformin ER) 1000 mg. Only taking 1000 mg due to tolerance issues. Higher doses needed to impact triglycerides Triglycerides have lowered to 474 from 589, but still too high. – HDL is too low at 26. Apo A 1 is also low possibly due to genetic inability to make HDL protein. HDL cholesterol may decrease with fenofibrate. – Advise stopping Tricor due to ineffectiveness. – Stain therapy may be an option. He has experienced muscles aches during past taking statins. He tried CO Q 10, but did not experience much benefit. There is also no evidence of hyperabsorbing on sterol testing(normal campesterol/sitosterol). Bottom line Zetia or intestinally acting agents unlikely to be of benefit. Statin more appropriate – Start Crestor 5 mg to lower triglycerides and raise HDL. Crestor is better tolerated. It is better metabolized than other alternative statins. Patients experience less muscle aches. The JUPITER clinical trial has shown 47% reduction in cardiac events in those who take Crestor. It is acceptable to take ½ a tablet if necessary. – Modify diet. Patient is still consuming too many carbs and more sugar than optimal. – Continue Lovaza 4 as omega 3 index is currently optimal >8%

4 Month Follow Up on Tricor 145, Atenolol 50, Glumetza 1000, Lovaza 4 and Vitamin D 3 5000 (2 of 2) • Hypertension – Deteriorated. – BP is high at 160/92. – Advise switching from Atenolol to Carvedilol due to triglyceride impact and avoid HCTZ. • Metabolic Syndrome – Unchanged. – Only taking Glumetza 1000 mg due to tolerance issues which does not impact triglycerides as much as higher doses. – Try increasing Glumetza to 1500 mg. – Start Cycloset can be used safely in prediabetic patients as it does not lower glucose to the extent that would cause hypoglycemia and works well to treat insulin resistance. Cycloset has beneficial effects on lipids and shown to reduce CVD events and may lower BP as well as triglycerides up to 30%. Another study showed Cycloset to reduce CVD events by 55%. – Take Cycloset 0. 8 mg. Take with food within 2 hours of waking. Start with 1 tablet and gradually increase to 4 -6 per day all at once and in the morning. Taking with food will minimize nausea. – Reduce carb and sugar intake.

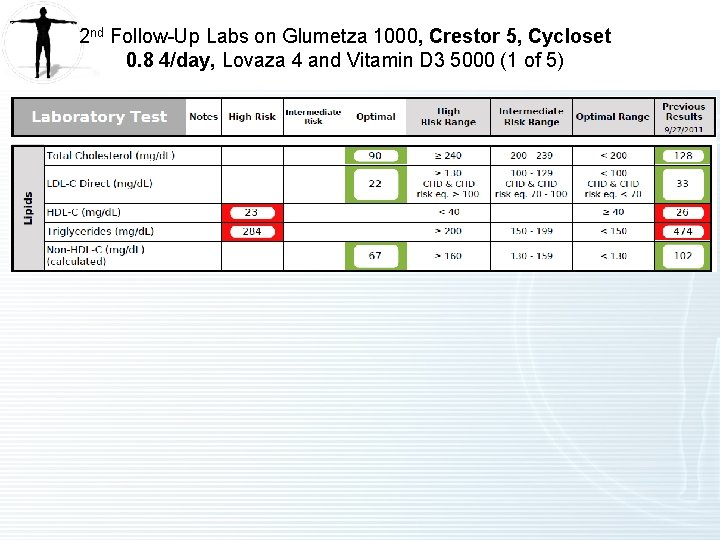
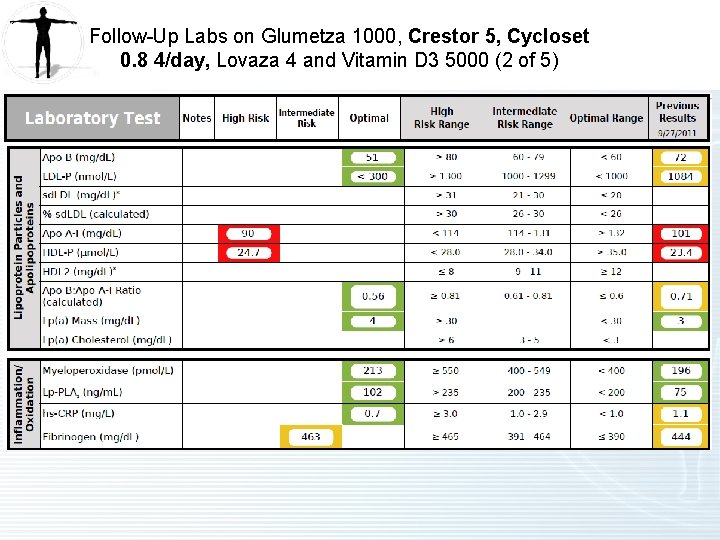
2 nd Follow Up on Glumetza 1000, Crestor 5, Cycloset 0. 8 4/day, Lovaza 4 and Vitamin D 3 5000 (1 of 2) • Hypertriglyceridemia – Improved. – Stopped Tricor last visit. – Started Crestor 5 mg, history of prior intolerance to other statins. Tolerating well and NOT taking CO Q 10. Also had a recent steroid injection. Try Crestor 10 mg. – Started Cycloset 0. 8 mg 4/day. Tolerating well. – Taking Glumetza 1000 and Lovaza 4. – Triglycerides lowered from 474 to 284. LDL-C lowered to 22. LDL-P lowered to < 300 from 1084. – Insulin resistance improved with the addition of Cycloset. – Inflammatory markers are normal (MPO, Lp. PLA 2, CRP). • Hypertension – Improved. – Stopped Atenolol last visit and switched to Losartan. Atenolol may have affected triglycerides. • Myalgia – Improved. – Consider CO Q 10 300 -600.

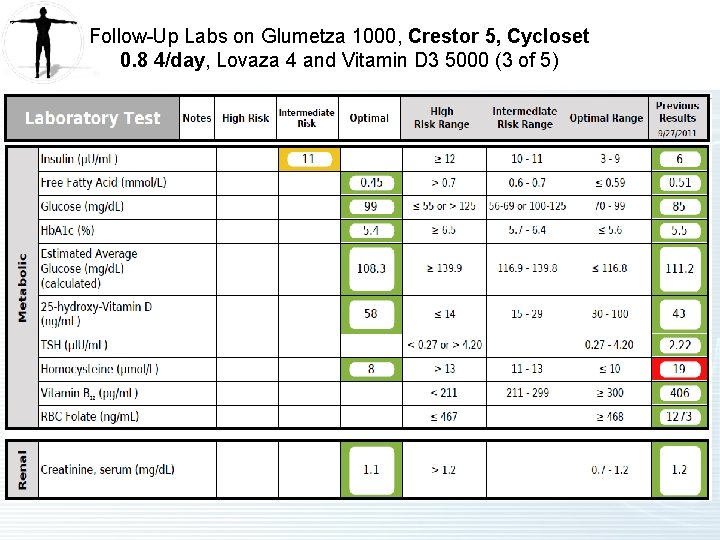
2 nd Follow Up on Glumetza 1000, Crestor 5, Cycloset 0. 8 4/day, Lovaza 4 and Vitamin D 3 5000 (2 of 2) • Metabolic Syndrome – Improved. – Hb. A 1 c is down to 5. 4 from 5. 5. – Glumetza 1000 mg is tolerated. – Cycloset 0. 8 mg 4/day is well tolerated. • Vitamin D Deficiency – Improved. – Taking Vitamin D 3 5000 mg/day. – Levels are up to 58 compared to 43 last visit and originally 22. • Homocystinemia – Improved. – Homocysteine levels decreased to 8 from 19 last visit. – Tricor can increase levels and Tricor was stopped last visit. Level is now normal.

2 nd Follow-Up Labs on Glumetza 1000, Crestor 5, Cycloset 0. 8 4/day, Lovaza 4 and Vitamin D 3 5000 (1 of 5)

Follow-Up Labs on Glumetza 1000, Crestor 5, Cycloset 0. 8 4/day, Lovaza 4 and Vitamin D 3 5000 (2 of 5)

Follow-Up Labs on Glumetza 1000, Crestor 5, Cycloset 0. 8 4/day, Lovaza 4 and Vitamin D 3 5000 (3 of 5)

Follow-Up Labs on Glumetza 1000, Crestor 5, Cycloset 0. 8 4/day, Lovaza 4 and Vitamin D 3 5000 (4 of 5)

Follow-Up Labs on Glumetza 1000, Crestor 5, Cycloset 0. 8 4/day, Lovaza 4 and Vitamin D 3 5000 (5 of 5)

NMR Lipo. Profile • Insert NMR Lipoprofile 01122012 MC 54 Insert

Clinical Pearls • Treating insulin resistance is always an option to consider as an alternative approach to a hard to treat patient with history of many drug intolerances. Pioglitazone, Metformin, Cycloset, and GLP 1 agonists all improve lipids and will not cause hypoglycemia so can be used safely in prediabetes. • Homocysteine elevations may be due to other medications (fenofibrate >>> Niacin).

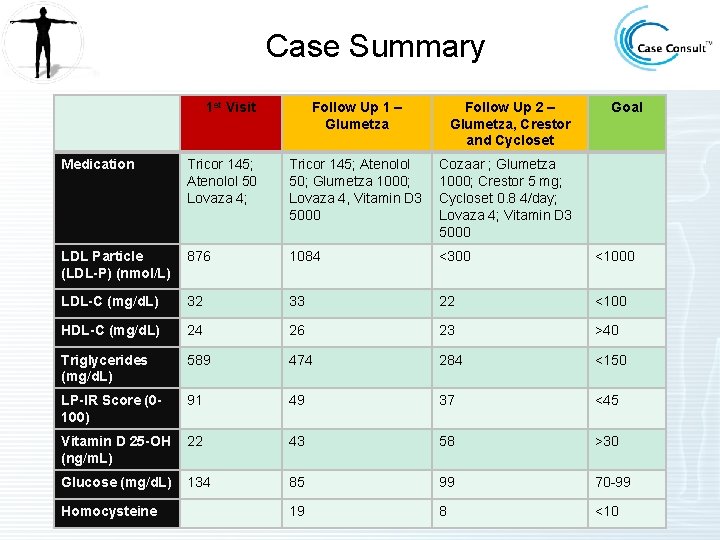
Case Summary 1 st Visit Follow Up 1 – Glumetza Follow Up 2 – Glumetza, Crestor and Cycloset Goal Medication Tricor 145; Atenolol 50 Lovaza 4; Tricor 145; Atenolol 50; Glumetza 1000; Lovaza 4, Vitamin D 3 5000 Cozaar ; Glumetza 1000; Crestor 5 mg; Cycloset 0. 8 4/day; Lovaza 4; Vitamin D 3 5000 LDL Particle (LDL-P) (nmol/L) 876 1084 <300 <1000 LDL-C (mg/d. L) 32 33 22 <100 HDL-C (mg/d. L) 24 26 23 >40 Triglycerides (mg/d. L) 589 474 284 <150 LP-IR Score (0100) 91 49 37 <45 Vitamin D 25 -OH (ng/m. L) 22 43 58 >30 Glucose (mg/d. L) 134 85 99 70 -99 19 8 <10 Homocysteine

References (1 of 2) • • Cromwell WC, Otvos JD, Keyes MJ, et al. LDL particle number and risk of future cardiovascular disease in the Framingham offspring study – implications for LDL management. J Clin Lipidol 2007 Dec; 1(6): 583 -92. . Grundy SM, Cleeman JI, Merz CN, et al. Implications of recent clinical trials for the National Cholesterol Education Program Adult Treatment Panel III guidelines. Circulation. Jul 13 2004; 110(2): 227 -39. Kolovou GD, Anagnostopoulou KK, Kostakou PM, et al. Primary and secondary hypertriglyceridaemia. Curr Drug Targets. Apr 2009; 10(4): 336 -43. Mc. Kenney JM, Mc. Cormick LS, Weiss S. A randomized trial of the effects of atorvastatin and niacin in patients with combined hyperlipidemia or isolated hypertriglyceridemia. Collaborative Atorvastatin Study Group. Am J Med. Feb 1998; 104(2): 137 -43. National Cholesterol Education Program. Executive Summary of The Third Report of The National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, And Treatment of High Blood Cholesterol In Adults (Adult Treatment Panel III). JAMA. May 16 2001; 285(19): 2486 -97. Roth EM, Bays HE, Forker AD, et al. Prescription omega-3 fatty acid as an adjunct to fenofibrate therapy in hypertriglyceridemic subjects. J Cardiovasc Pharmacol. Jul 10 2009. Triglycerides and Cardiovascular Disease: A Scientific Statement form the American Heart Association Circulation published online Apr 18, 2011 DOI: 10. 1161/CIR. 0 b 013 e 3182160726 Circulation published online Apr 18, 2011;

References (2 of 2) • • • Goldstein LB, Bushnell CD, Adams RJ, Appel LJ, Braun LT, Chaturvedi S, et al. Guidelines for the primary prevention of stroke: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 2011 Feb; 42: 517 -84. Kaplan NM. Systemic hypertension: Treatment. In: Bonow RO, Mann DL, Zipes DP, Libby P, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 9 th ed. Philadelphia, Pa: Saunders Elsevier; 2011: chap 46. Victor, RG. Systemic hypertension: Mechanisms and diagnosis. In: Bonow RO, Mann DL, Zipes DP, Libby P, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 9 th ed. Philadelphia, Pa: Saunders Elsevier; 2011: chap 45. Gaziano JM, Cincotta AH, O’Connor CM, et al. Randomized clinical trial of quick-release bromocriptine among patients with type 2 diabetes on overall safety and cardiovascular outcomes. Diabetes Care. 2010 Jul; 33(7): 1503 -8. Pili H, Ohashi S, Matsuda M, et al. Bromocriptine: a novel approach to the treatment of type 2 diabetes. Diabetes Care 2000 Aug; 23(8): 1154 -61.