43 Year Old Female with Familial Hypercholesterolemia Metabolic

43 Year Old Female with Familial Hypercholesterolemia, Metabolic Syndrome and PCOS Case Category: Familial Hypercholesterolemia, Metabolic Syndrome, PCOS History of present illness: 43 year old female with dyslipidemia, metabolic syndrome, hypertension, elevated CRP, vitamin D deficiency, and PCOS. Has a family history of diabetes and has had elevated insulin levels for over 10 years. Has taken metformin and Byetta in the past. Hypertension is well controlled with medications. Taking a low dose of vitamin D but in caplet form. Not taking omega 3 or aspirin due to previous bruising on these supplements. No history of thyroid disease. Patient is very interested in being aggressive with medication for prevention. No plans for childbearing as she has had uterine ablation for PCOS/fibroids.
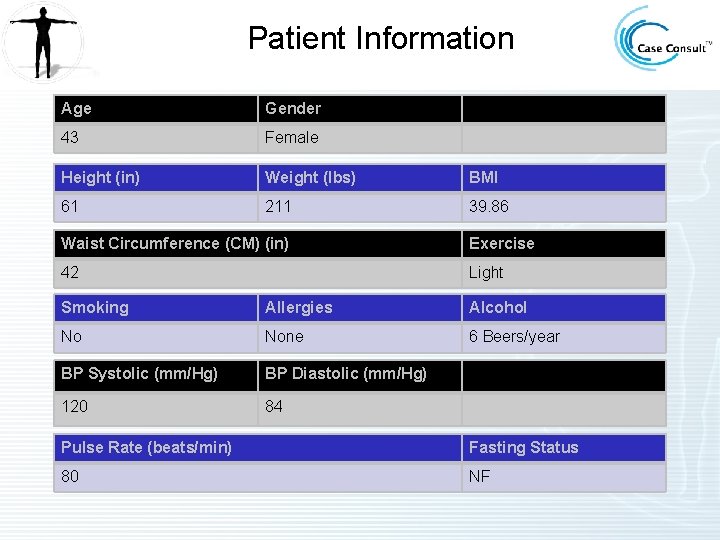
Patient Information Age Gender 43 Female Height (in) Weight (lbs) BMI 61 211 39. 86 Waist Circumference (CM) (in) Exercise 42 Light Smoking Allergies Alcohol No None 6 Beers/year BP Systolic (mm/Hg) BP Diastolic (mm/Hg) 120 84 Pulse Rate (beats/min) Fasting Status 80 NF
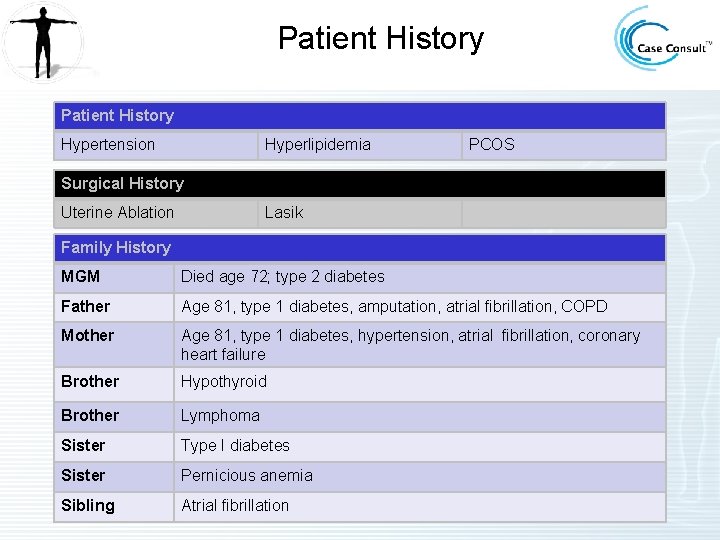
Patient History Hypertension Hyperlipidemia PCOS Surgical History Uterine Ablation Lasik Family History MGM Died age 72; type 2 diabetes Father Age 81, type 1 diabetes, amputation, atrial fibrillation, COPD Mother Age 81, type 1 diabetes, hypertension, atrial fibrillation, coronary heart failure Brother Hypothyroid Brother Lymphoma Sister Type I diabetes Sister Pernicious anemia Sibling Atrial fibrillation
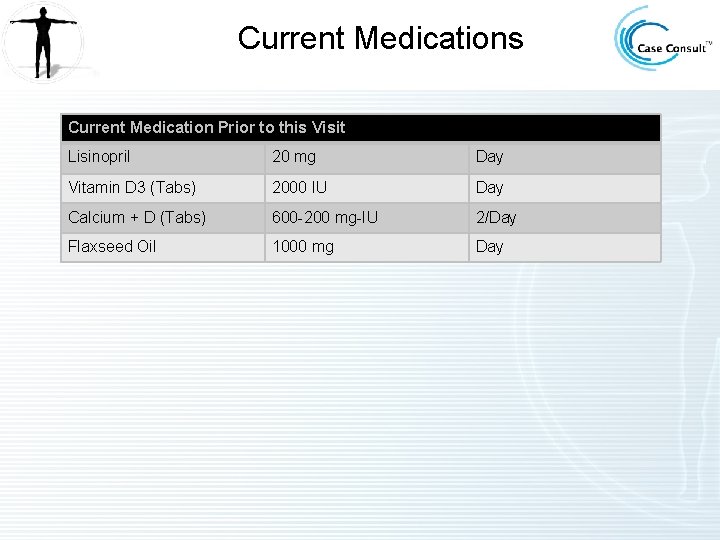
Current Medications Current Medication Prior to this Visit Lisinopril 20 mg Day Vitamin D 3 (Tabs) 2000 IU Day Calcium + D (Tabs) 600 -200 mg-IU 2/Day Flaxseed Oil 1000 mg Day
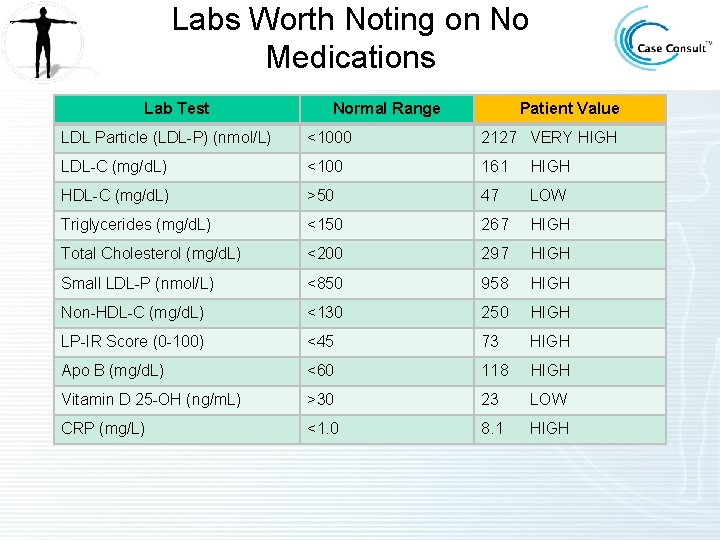
Labs Worth Noting on No Medications Lab Test Normal Range Patient Value LDL Particle (LDL-P) (nmol/L) <1000 2127 VERY HIGH LDL-C (mg/d. L) <100 161 HIGH HDL-C (mg/d. L) >50 47 LOW Triglycerides (mg/d. L) <150 267 HIGH Total Cholesterol (mg/d. L) <200 297 HIGH Small LDL-P (nmol/L) <850 958 HIGH Non-HDL-C (mg/d. L) <130 250 HIGH LP-IR Score (0 -100) <45 73 HIGH Apo B (mg/d. L) <60 118 HIGH Vitamin D 25 -OH (ng/m. L) >30 23 LOW CRP (mg/L) <1. 0 8. 1 HIGH

Questions to Consider • Question 1: Assess diet. Labs suggest she may be eating too many carbs and simple sugars? Alcohol intake? Exercise? • Question 2: In past on metformin and Byetta for PCOS/metabolic syndrome. Did she feel better on medications? Is carb craving or “hypoglycemia” an issue for her? Abdominal weight gain? Fatigue and depression? Sleep disturbances? • Question 3: How is she managing stress? • Question 4: What type of Vitamin D 3 is she taking? Oil based gel cap or tablet/combo with calcium? (Currently taking in tablet form which is not well absorbed and very low vitamin D reflects this)
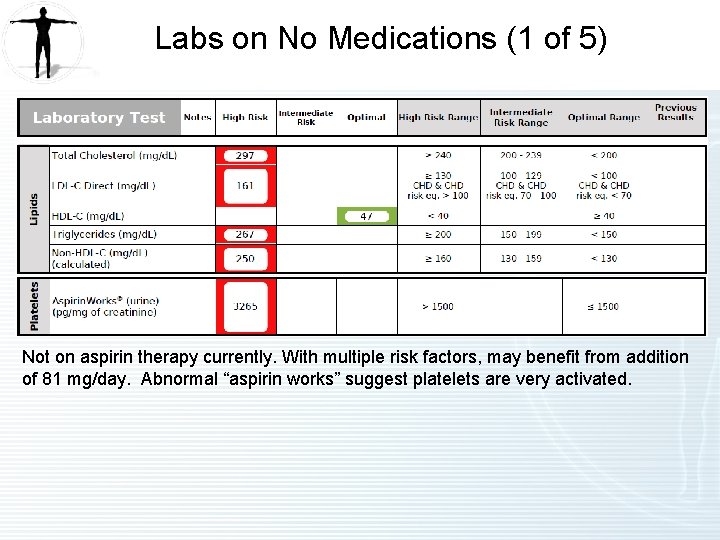
Labs on No Medications (1 of 5) Not on aspirin therapy currently. With multiple risk factors, may benefit from addition of 81 mg/day. Abnormal “aspirin works” suggest platelets are very activated.
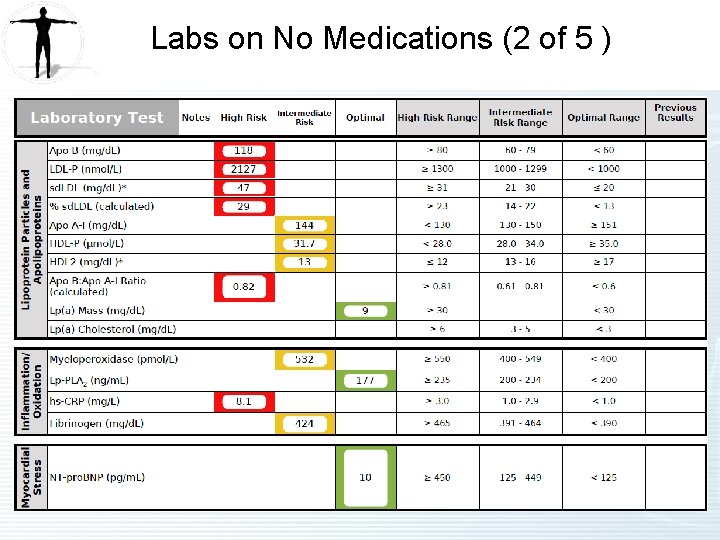
Labs on No Medications (2 of 5 )
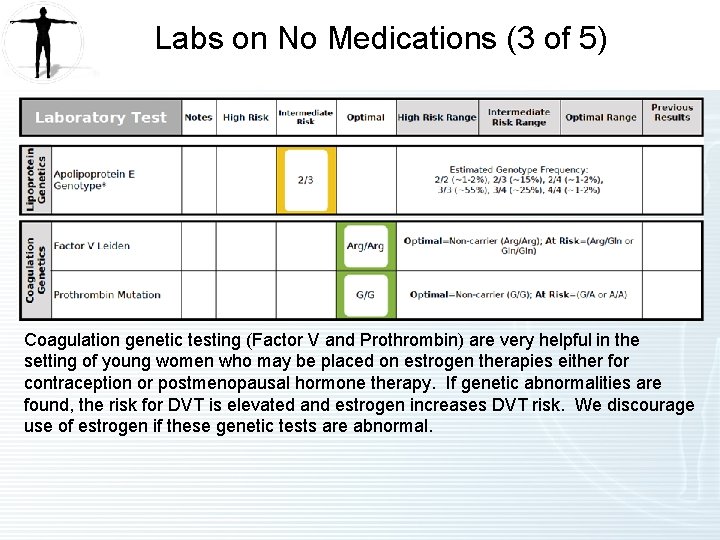
Labs on No Medications (3 of 5) Coagulation genetic testing (Factor V and Prothrombin) are very helpful in the setting of young women who may be placed on estrogen therapies either for contraception or postmenopausal hormone therapy. If genetic abnormalities are found, the risk for DVT is elevated and estrogen increases DVT risk. We discourage use of estrogen if these genetic tests are abnormal.
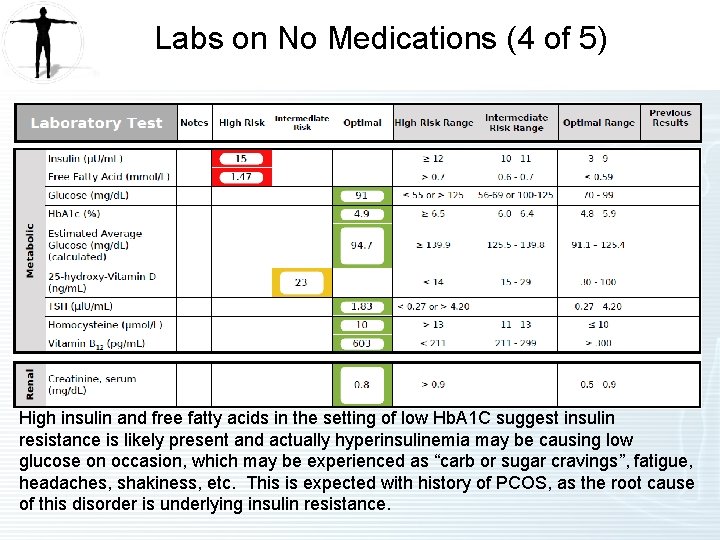
Labs on No Medications (4 of 5) High insulin and free fatty acids in the setting of low Hb. A 1 C suggest insulin resistance is likely present and actually hyperinsulinemia may be causing low glucose on occasion, which may be experienced as “carb or sugar cravings”, fatigue, headaches, shakiness, etc. This is expected with history of PCOS, as the root cause of this disorder is underlying insulin resistance.
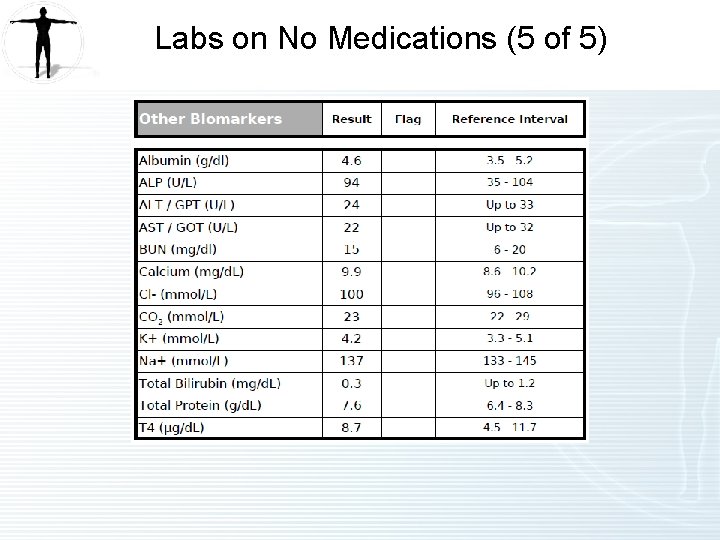
Labs on No Medications (5 of 5)

Initial Treatment & Management PCOS, FCH • Advise diet modifications (low carb, anti-inflammatory) and increased exercise. • For familial combined hyperlipidemia (FCH), start Crestor 20 mg/day to lower triglycerides and LDL-P. • Continue Lisinopril for hypertension. • Start metformin ER 500 mg 2 -3 tablets daily with slow titration as tolerated for metabolic syndrome and PCOS. • Start Lovaza 4 g/day and anti-inflammatory diet for elevated CRP and arthritis. Should also help triglycerides. • Start vitamin D 3 5000 IU/day in gel cap not tablet form (which she is currently taking).
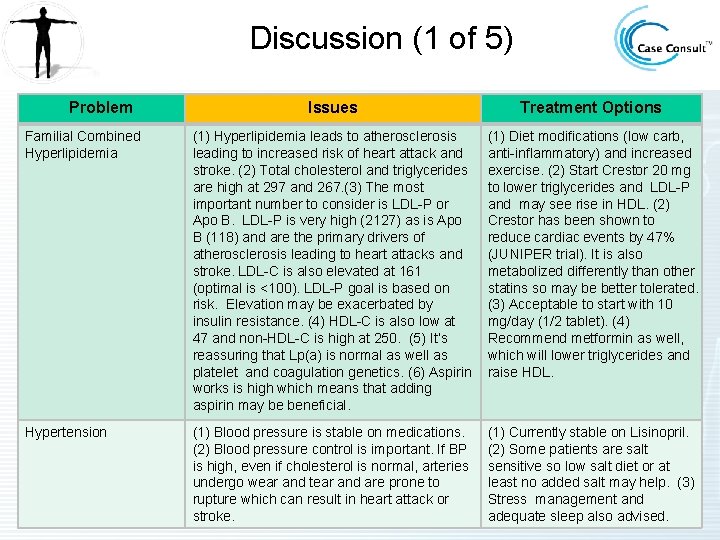
Discussion (1 of 5) Problem Issues Treatment Options Familial Combined Hyperlipidemia (1) Hyperlipidemia leads to atherosclerosis leading to increased risk of heart attack and stroke. (2) Total cholesterol and triglycerides are high at 297 and 267. (3) The most important number to consider is LDL-P or Apo B. LDL-P is very high (2127) as is Apo B (118) and are the primary drivers of atherosclerosis leading to heart attacks and stroke. LDL-C is also elevated at 161 (optimal is <100). LDL-P goal is based on risk. Elevation may be exacerbated by insulin resistance. (4) HDL-C is also low at 47 and non-HDL-C is high at 250. (5) It’s reassuring that Lp(a) is normal as well as platelet and coagulation genetics. (6) Aspirin works is high which means that adding aspirin may be beneficial. (1) Diet modifications (low carb, anti-inflammatory) and increased exercise. (2) Start Crestor 20 mg to lower triglycerides and LDL-P and may see rise in HDL. (2) Crestor has been shown to reduce cardiac events by 47% (JUNIPER trial). It is also metabolized differently than other statins so may be better tolerated. (3) Acceptable to start with 10 mg/day (1/2 tablet). (4) Recommend metformin as well, which will lower triglycerides and raise HDL. Hypertension (1) Blood pressure is stable on medications. (2) Blood pressure control is important. If BP is high, even if cholesterol is normal, arteries undergo wear and tear and are prone to rupture which can result in heart attack or stroke. (1) Currently stable on Lisinopril. (2) Some patients are salt sensitive so low salt diet or at least no added salt may help. (3) Stress management and adequate sleep also advised.
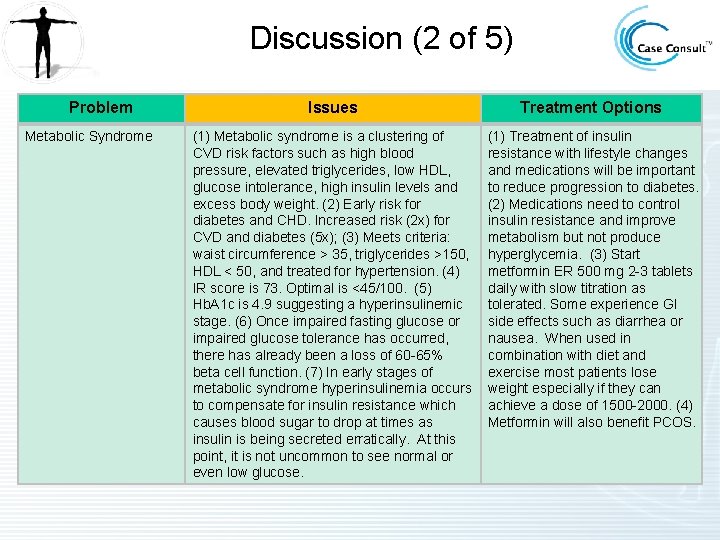
Discussion (2 of 5) Problem Metabolic Syndrome Issues Treatment Options (1) Metabolic syndrome is a clustering of CVD risk factors such as high blood pressure, elevated triglycerides, low HDL, glucose intolerance, high insulin levels and excess body weight. (2) Early risk for diabetes and CHD. Increased risk (2 x) for CVD and diabetes (5 x); (3) Meets criteria: waist circumference > 35, triglycerides >150, HDL < 50, and treated for hypertension. (4) IR score is 73. Optimal is <45/100. (5) Hb. A 1 c is 4. 9 suggesting a hyperinsulinemic stage. (6) Once impaired fasting glucose or impaired glucose tolerance has occurred, there has already been a loss of 60 -65% beta cell function. (7) In early stages of metabolic syndrome hyperinsulinemia occurs to compensate for insulin resistance which causes blood sugar to drop at times as insulin is being secreted erratically. At this point, it is not uncommon to see normal or even low glucose. (1) Treatment of insulin resistance with lifestyle changes and medications will be important to reduce progression to diabetes. (2) Medications need to control insulin resistance and improve metabolism but not produce hyperglycemia. (3) Start metformin ER 500 mg 2 -3 tablets daily with slow titration as tolerated. Some experience GI side effects such as diarrhea or nausea. When used in combination with diet and exercise most patients lose weight especially if they can achieve a dose of 1500 -2000. (4) Metformin will also benefit PCOS.
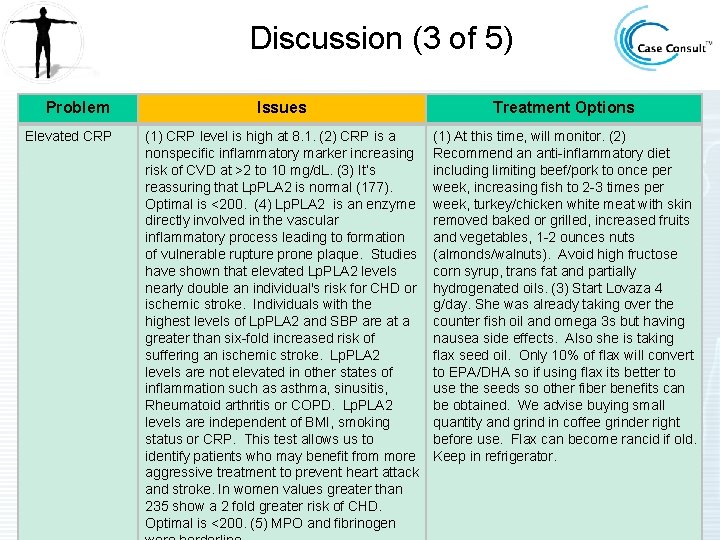
Discussion (3 of 5) Problem Elevated CRP Issues Treatment Options (1) CRP level is high at 8. 1. (2) CRP is a nonspecific inflammatory marker increasing risk of CVD at >2 to 10 mg/d. L. (3) It’s reassuring that Lp. PLA 2 is normal (177). Optimal is <200. (4) Lp. PLA 2 is an enzyme directly involved in the vascular inflammatory process leading to formation of vulnerable rupture prone plaque. Studies have shown that elevated Lp. PLA 2 levels nearly double an individual's risk for CHD or ischemic stroke. Individuals with the highest levels of Lp. PLA 2 and SBP are at a greater than six-fold increased risk of suffering an ischemic stroke. Lp. PLA 2 levels are not elevated in other states of inflammation such as asthma, sinusitis, Rheumatoid arthritis or COPD. Lp. PLA 2 levels are independent of BMI, smoking status or CRP. This test allows us to identify patients who may benefit from more aggressive treatment to prevent heart attack and stroke. In women values greater than 235 show a 2 fold greater risk of CHD. Optimal is <200. (5) MPO and fibrinogen (1) At this time, will monitor. (2) Recommend an anti-inflammatory diet including limiting beef/pork to once per week, increasing fish to 2 -3 times per week, turkey/chicken white meat with skin removed baked or grilled, increased fruits and vegetables, 1 -2 ounces nuts (almonds/walnuts). Avoid high fructose corn syrup, trans fat and partially hydrogenated oils. (3) Start Lovaza 4 g/day. She was already taking over the counter fish oil and omega 3 s but having nausea side effects. Also she is taking flax seed oil. Only 10% of flax will convert to EPA/DHA so if using flax its better to use the seeds so other fiber benefits can be obtained. We advise buying small quantity and grind in coffee grinder right before use. Flax can become rancid if old. Keep in refrigerator.
Discussion (4 of 5) Problem Issues Treatment Options Vitamin D Deficiency (1) Vitamin D is low at 23. Optimal is >6090. (2) Deficiency is associated with increased risk for CVD, hypertension, obesity, fatigue, glucose intolerance, metabolic syndrome, depression, muscle aching, and cancer. 1) Severe vitamin D deficiency needs treatment, as this can cause worsening muscle aches and make statin treatment more difficult. (2) Start vitamin D 3 5000 IU/day for 8 -12 weeks. Take D 3, not D 2. Choose an oil based capsule rather than a tablet for better absorption. She is on vitamin D 2 in tablet form and level was very low. Tablets are not well absorbed. (3) Will consider starting vitamin D 2 50000 IU/week after recheck of vitamin D levels. Alternative would be to increase dose of over the counter Vitamin D 3 if level not optimal on 5000 IU, 700010, 000. Arthritis (1) Recommend taking high dose omega 3 fatty acids which may help reduce inflammation. (2) Starting Lovaza 4 g/day is an option or potent diet supplement with at least 4 grams of EPA/DHA.
Discussion (5 of 5) Problem Issues Treatment Options Polycystic ovarian syndrome (1) Increased risk for diabetes and cardiovascular disease. (2) Diagnosis based on any evidence of excess androgens (hirsuitism, acne, hair loss, elevated testosterone) and menstrual irregularity and/or cysts on ovaries. (3) Diagnosis is clinical and does not require additional lab testing although testosterone may be elevated. (4) LH/FSH ratio may be >2: 1. (5) Lab abnormalities not necessary to make diagnosis. (1) Standard of care is use of Metformin especially if also overweight. (2) There are several studies showing benefit with TZDs (both Avandia and Actos) and a small study with use of Byetta to help restore ovulation. Note: Oral contraceptives may help with menstrual irregularities but do not treat root cause of this disorder which is insulin resistance. In this patient she has had uterine ablation so contraception not a concern.

Follow-Up on Crestor 20 and Vitamin D 3 5000 (1 of 2) • Familial Combined Hyperlipidemia – Improved. – Excellent response to Crestor 20 monotherapy (Did not take Lovaza or metformin prescribed last visit). LDL-P dropped from 2127 to 1182. Apo B reduced to 75 from 118. Total cholesterol lowered to 176 from 297. LDL-C dropped to 85 from 161. Triglycerides lowered to 181 from 267. HDL at 49. – Very high aspirin test suggests very active platelets and may benefit from aspirin 81. – Sterol testing normal on Crestor. No overabsorption in stomach or oversecretion in liver. – Continue therapy. • Hypertension – Deteriorated. – Blood pressure is 130/96. – Taking Lisinopril. – Advise monitoring BP with a home BP meter. Goal is to be below <120/80. • PCOS/Metabolic Syndrome – Discontinued metformin due to severe nausea. – Recommend starting Glumetza 500 2/day as tolerated. Glumetza will help with insulin resistance, lipids, and PCOS. – Insulin is improved. IR score down to 68 from 73. – Continue efforts at diet and exercise.

Follow-Up on Crestor 20 and Vitamin D 3 5000 (2 of 2) • Elevated CRP – Unchanged. – Discontinued Lovaza due to severe nausea. Patient would like to try Krill Mega Red. She has already failed other over the counter omega 3 due to nausea and GI side effects – CRP lowered from 8. 1 to 4. 0. – Omega 3 index is low at 4%. Optimal is >8 -10%. – Highest sources of omega 3 come from Atlantic salmon, herring, mackerel, or bluefin tuna. – MPO normalized. – Fibrinogen improved. • Vitamin D Deficiency – Improved with switch to gel caps vs tablets. – Taking Vitamin D 3 5000/day. – Levels increased from 23 to 45. Optimal is >60 -90. – Continue therapy. • Arthritis – Unchanged. – Patient reports arthritis much better when taking Lovaza 4/day, but discontinued due to nausea.
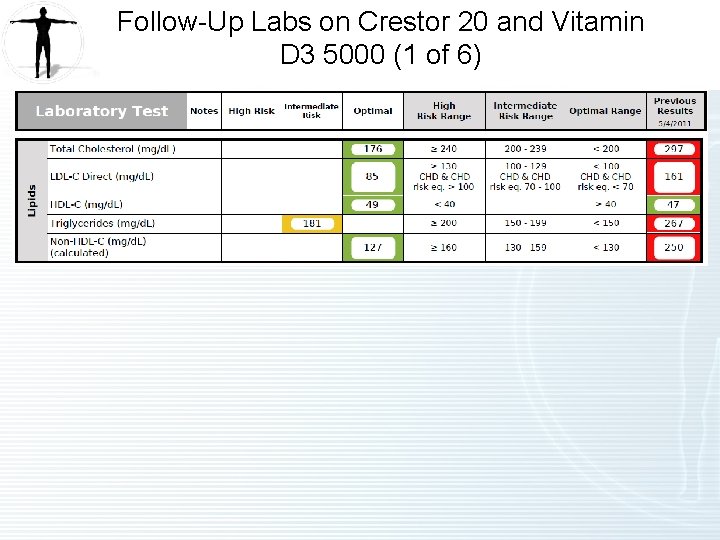
Follow-Up Labs on Crestor 20 and Vitamin D 3 5000 (1 of 6)
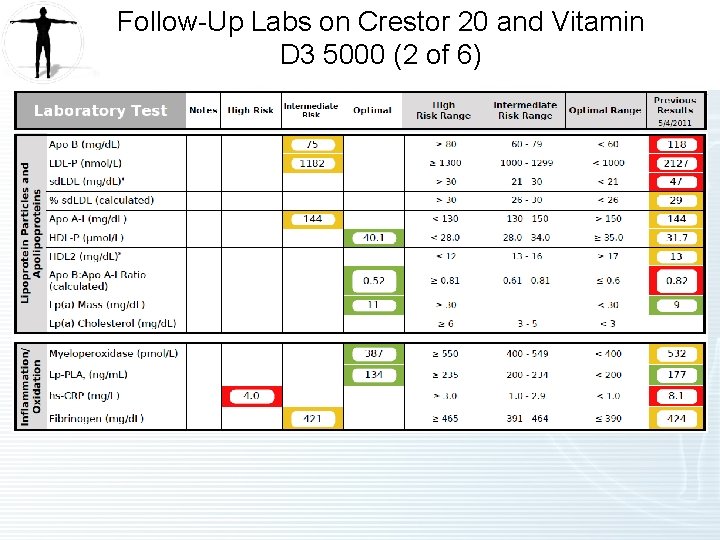
Follow-Up Labs on Crestor 20 and Vitamin D 3 5000 (2 of 6)
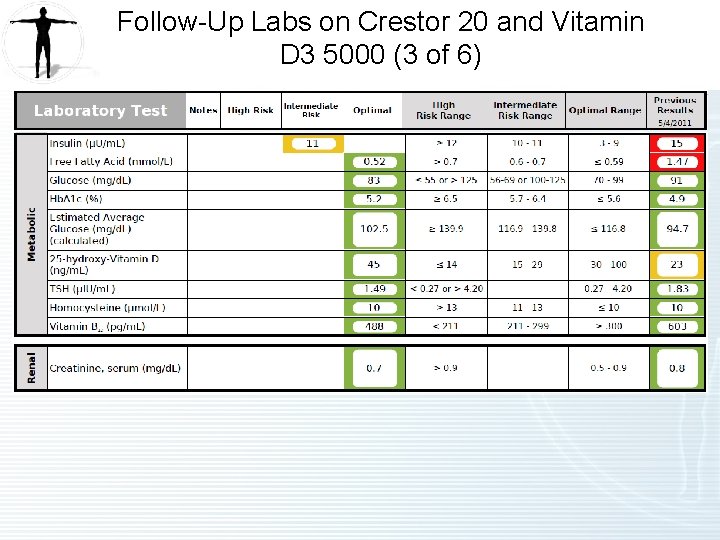
Follow-Up Labs on Crestor 20 and Vitamin D 3 5000 (3 of 6)
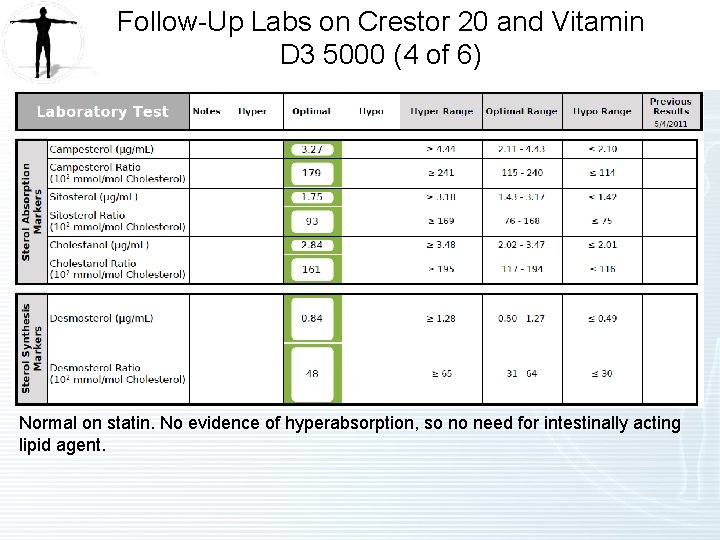
Follow-Up Labs on Crestor 20 and Vitamin D 3 5000 (4 of 6) Normal on statin. No evidence of hyperabsorption, so no need for intestinally acting lipid agent.
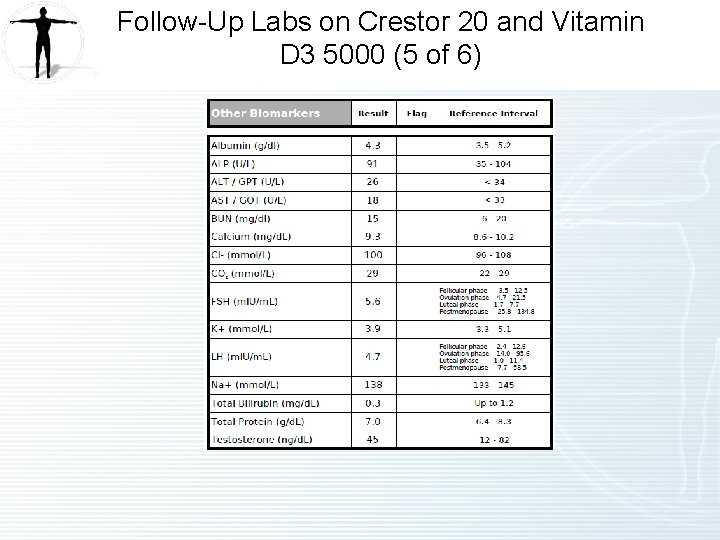

Follow-Up Labs on Crestor 20 and Vitamin D 3 5000 (5 of 6)
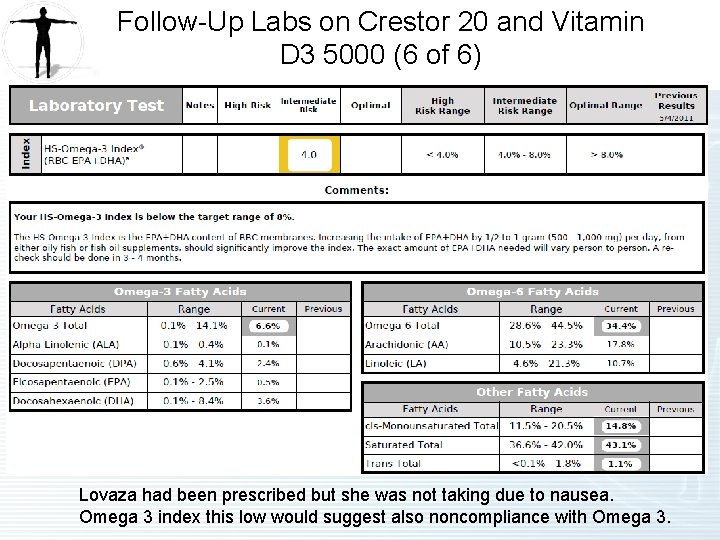
Follow-Up Labs on Crestor 20 and Vitamin D 3 5000 (6 of 6) Lovaza had been prescribed but she was not taking due to nausea. Omega 3 index this low would suggest also noncompliance with Omega 3.

NMR Lipo. Profile • Insert NMR Lipoprofile 02162012 KW 67 Insert
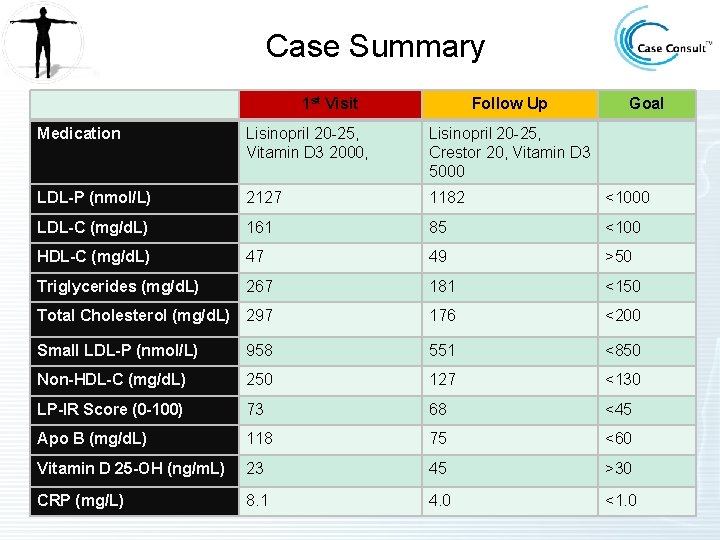
Case Summary 1 st Visit Follow Up Goal Medication Lisinopril 20 -25, Vitamin D 3 2000, Lisinopril 20 -25, Crestor 20, Vitamin D 3 5000 LDL-P (nmol/L) 2127 1182 <1000 LDL-C (mg/d. L) 161 85 <100 HDL-C (mg/d. L) 47 49 >50 Triglycerides (mg/d. L) 267 181 <150 Total Cholesterol (mg/d. L) 297 176 <200 Small LDL-P (nmol/L) 958 551 <850 Non-HDL-C (mg/d. L) 250 127 <130 LP-IR Score (0 -100) 73 68 <45 Apo B (mg/d. L) 118 75 <60 Vitamin D 25 -OH (ng/m. L) 23 45 >30 CRP (mg/L) 8. 1 4. 0 <1. 0
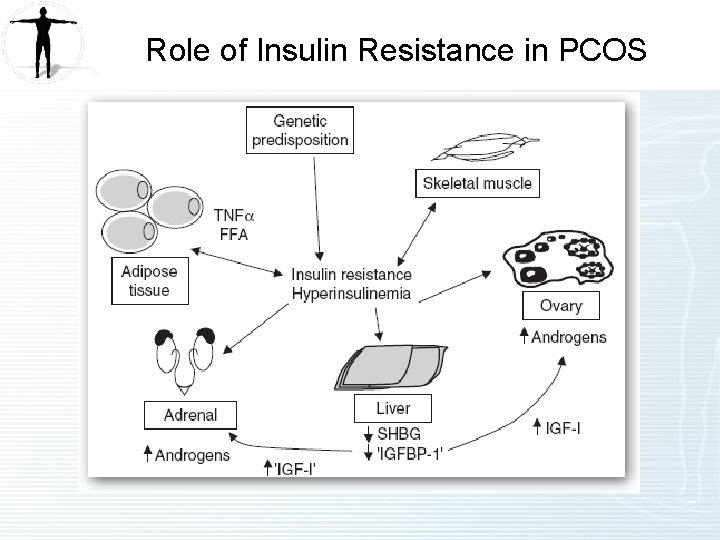
Role of Insulin Resistance in PCOS
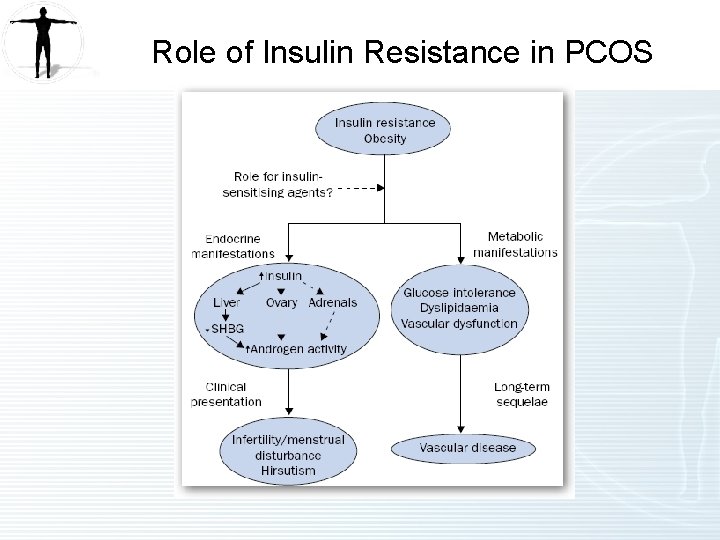
Role of Insulin Resistance in PCOS
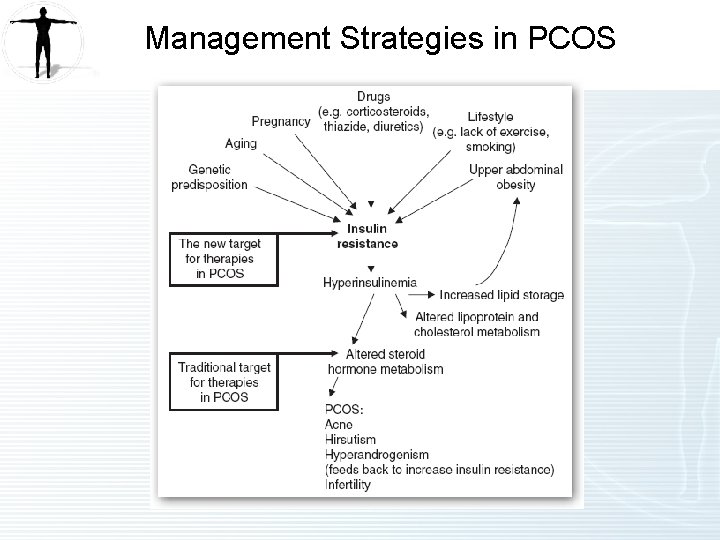
Management Strategies in PCOS

Thiazolidinedione – (Actos) Pioglitazone • • Improves ovulatory dysfunction and hyperandrogenism Lowers triglycerides and raises HDL- C Recommend dose of pioglitazone - 15 -30 mg/day Well tolerated Brettenthaler N, De Geyter C, Huber PR, et al. Effect of the insulin sensitizer pioglitazone on insulin resistance, hyperandrogenism, and ovulatory dysfunction in women with polycystic ovary syndrome. J Clin Endrocrinol Metab. 2004 Aug; 89(8): 3835 -40.

Byetta (Exenatide GLP-1 Agonist) and Metformin in PCOS • Comparison of single and combined treatment with exenatide and metformin on menstrual cyclicity in overweigh women with PCOS. • 60 overweight women with PCOS randomized to metformin, exenatide or both. Measured effects on menstrual cyclicity, hormonal parameters, metabolic profiles, and inflammatory markers. 42 women completed study. • Combination therapy was superior to exenatide or metformin monotherapy in improving menstrual cyclicity, ovulation rate, free androgen index, and insulin sensitivity measures and reducing weight and abdominal fat. Both exenatide arms were more effective in promoting weight loss than metformin (p=0. 003). Eikelboom JW, Hirsh J, Weitz JI, et al. Aspirin-resistant Thromboxane biosynthesis and the risk of myocardial infarction, stroke, or cardiovascular death in patients at high risk for cardiovascular events. Circulation. 2002; 105: 1650 -1655.

Clinical Pearls • Aspirin Works – Not everyone benefits from the same dose of aspirin. – Aspirin therapy is not without risk and test values may be utilized to identify patients most likely to benefit from antiplatelet therapy. – In aspirin-treated patients, high levels of 11 dh. TXB 2 are associated with increased risk of heart attack and cardiac death. – Patients classified as aspirin-resistant are at about a fourfold increased risk of cardiovascular events. – Elevations of 11 -d. TXB 2 in patients already receiving antiplatelet therapy suggest a continued hypercoagulable state. Increased aspirin dose or alternative antithrombotic or antiplatelet therapies should be considered in such patients. – Hyperlipidemia is associated with diminished response to aspirin. – 11 dh. TXB 2 levels demonstrate a dose-related effect of aspirin treatment. – Diabetes may contribute to a diminished response to aspirin. – 11 dh. TXB 2 levels have been shown to correlate with a Framingham Risk Score.
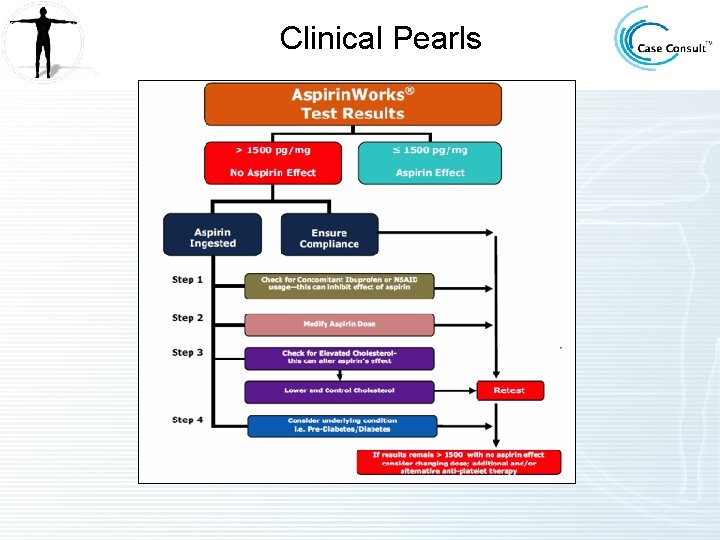
Clinical Pearls

References (1 of 3) • • Cromwell WC, Otvos JD, Keyes MJ, et al. LDL particle number and risk of future cardiovascular disease in the Framingham offspring study – implications for LDL management. J Clin Lipidol. 2007 Dec; 1(6): 583 -92. Rosenson RS, Otvos JD and Hsia J. Effects of rosuvastatin and atovastatin on LDL and HDL particle concentrations in patients with metabolic syndrome: a randomized, doubleblind, controlled study. Diabetes Care. 2009 Jun; 32(6): 1087 -91. ADA Standards of Medical Care in Diabetes - 2012. Diabetes Care. Jan 2012 35(1)11 -63. Knowler WC, Barrett-Connor E, Fowler SE, et al. Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. N Engl J Med. 2002 Feb 7; 346(6): 393 -403. Nathan DM, Davidson M, De. Fronzo RA, et al. Impaired fasting glucose and impaired glucose tolerance: implications for care. A consensus statement from the American Diabetes Association. Diabetes Care. 2007; 30: 753 -759. Nicholls SJ, Ballantyne CM, Barter PJ, et al. Effect of two intensive statin regimens on progression of coronary disease. N Engl J Med. 2011 Dec 1; 365(22): 2078 -87. Ridker PM, Danielson E, Fonseca FA, et al. Rosuvastatin to prevent vascular events in men and women with elevated C-reactive protein. N Engl J Med. 2008 Nov 20; 359(21): 2195 -207. Ballantyne CM, Hoogeveen RC, Bang H, et al. Lipoprotein-associated phospholipase A 2, high-sensitivity C-reactive protein, and risk for incident ischemic stroke in middle-aged men and women in the Arthrosclerosis Risk in Communities (ARIC) study. Arch Intern Med. 2005; 165: 2479 -2484.

References (2 of 3) • • Koenig W, Khuseyinova N, Löwel H, et al. Lipoprotein-associated phospholipase A 2 adds to risk prediction of incident coronary events by C-reactive protein in apparently healthy middle -aged men from the general population. Results from the 14 -year follow-up of a large cohort from southern Germany. Circulation. 2004; 110: 1903 -1908 Koenig W, Twardella D, Brenner H, et al. Lipoprotein-associated phospholipase A 2 predicts future cardiovascular events in patients with coronary heart disease independently of traditional risk factors, markers of inflammation, renal function, and hemodynamic stress. Arterioscler Thromb Vasc Biol. 2006; 26: 1586 -1593. Persson M, Hedblad B, Nelson JJ, et al. Elevated Lp-PLA 2 levels add prognostic information to the metabolic syndrome on incidence of cardiovascular events among middleaged nondiabetic subjects. Arterioscler Thromb Vasc Biol. 2007; 27: 1411 -1416. Davidson MH, Corson MA, Alberts MJ, et al. Consensus panel recommendation for incorporating lipoprotein-associated phospholipase A 2 testing into cardiovascular disease risk assessment guidelines. Am J Cardiol. 2008; 101 suppl: 51 F-57 F. Dobnig H, Pilz S, Scharnagl H, et al. Independent association of low serum 25 hydroxyvitamin d and 1, 25 -dihydroxyvitamin d levels with all-cause and cardiovascular mortality. Arch Intern Med. 2008; 168(12): 1340 -1349. Michos E and Blumenthal R. Vitamin D Supplementation and Cardiovascular Disease Risk. Circulation. 2007; 115(7): 827 -828. Elkind-Hirsch K, Marrioneaux O, Bhushan M, et al. Comparison of single and combined treatment with exenatide and metformin on menstrual cyclicity in overweight women with polycyctic ovary syndrome. J Clin Endocrinol Metab. 2008 Jul; 93(7): 2670 -8.

References (3 of 3) • • • Harborne L, Fleming R, Lyall H, et al. Descriptive review of the evidence for the use of metformin in polycystic ovary syndrome. Lancet. 2003 May 31; 361(9372): 1849 -901. Brettenthaler N, De Geyter C, Huber PR, et al. Effect of the insulin sensitizer pioglitazone on insulin resistance, hyperandrogenism, and ovulatory dysfunction in women with polycystic ovary syndrome. J Clin Endrocrinol Metab. 2004 Aug; 89(8): 3835 -40. Eikelboom JW, Hirsh J, Weitz JI, et al. Aspirin-resistant Thromboxane biosynthesis and the risk of myocardial infarction, stroke, or cardiovascular death in patients at high risk for cardiovascular events. Circulation. 2002; 105: 1650 -1655. Di. Chiara J, Bliden KP, Tantry US, et al. The effect of aspirin dosing on platelet function in diabetic and nondiabetic patients: an analysis from the aspirin-induced platelet effect (ASPECT) study. Diabetes. 2007 Dec; 56(12): 3014 -9. Faraday N, Becker DM, Yanek LR, et al. Relation between atherosclerosis risk factors and aspirin resistance in a primary prevention population. Am J Cardiol. 2006 Sep 15; 98(6): 7749. Markuszewski L, Rosiak M, Golanski J, et al. Reduced blood platelet sensitivity to aspirin in coronary artery disease: are dyslipidemia and inflammatory states possible factors predisposing to sub-optimal platelet response to aspirin? Basic & Clin Pharmacol Toxicol. 2006 May; 98: 503 -9.
- Slides: 37