4 Access Incision Flap design Incision Sharp blade

4) Access • Incision • Flap design

Incision • Sharp blade (change if necessary) • Continuous stroke (reduce tissue tearing). • Protect the vital structures. • Surgeon must focus on the blade while cutting. • Blade must be perpendicular on the surface. • Incision line must be on health gingiva and bone (never place the incision over the defect area).
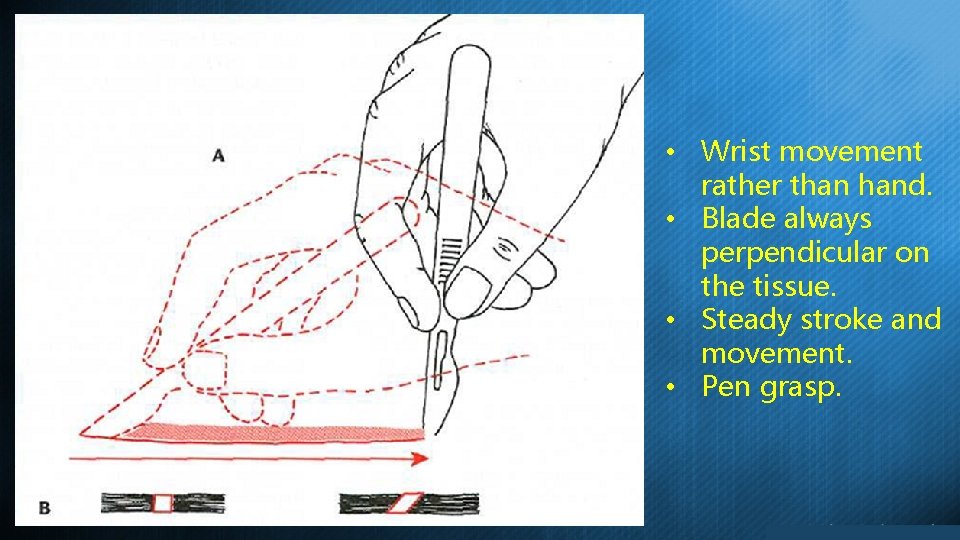
• Wrist movement rather than hand. • Blade always perpendicular on the tissue. • Steady stroke and movement. • Pen grasp.

• Flaps • Full thickness mucoperiosteal flap • Partial thickness flaps.
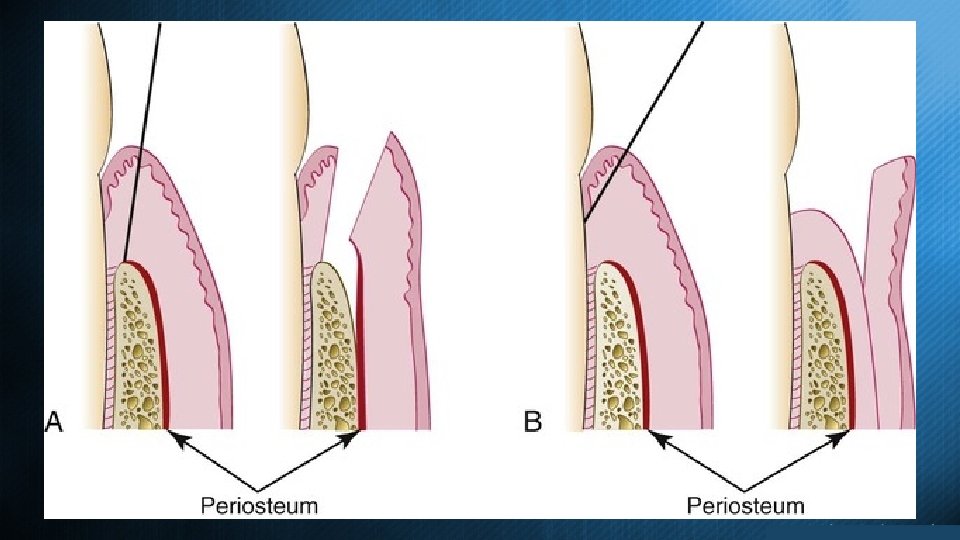

Flap Tissue reflected to provide access to surgical site. Three major point with flap design: • Design to prevent flap necrosis. • Design to prevent flap dehiscence. • Design to prevent flap tearing.

Prevention of flap necrosis: 4 basic principles must be followed • Apex (tip) never wider than the base. • If 3 sided flap the releasing should be parallel or converged from the base to apex. • Length should be no more than twice the width of the base. Preferably the width is greater. • Base of the flap should never be twisted or grasped excessively.
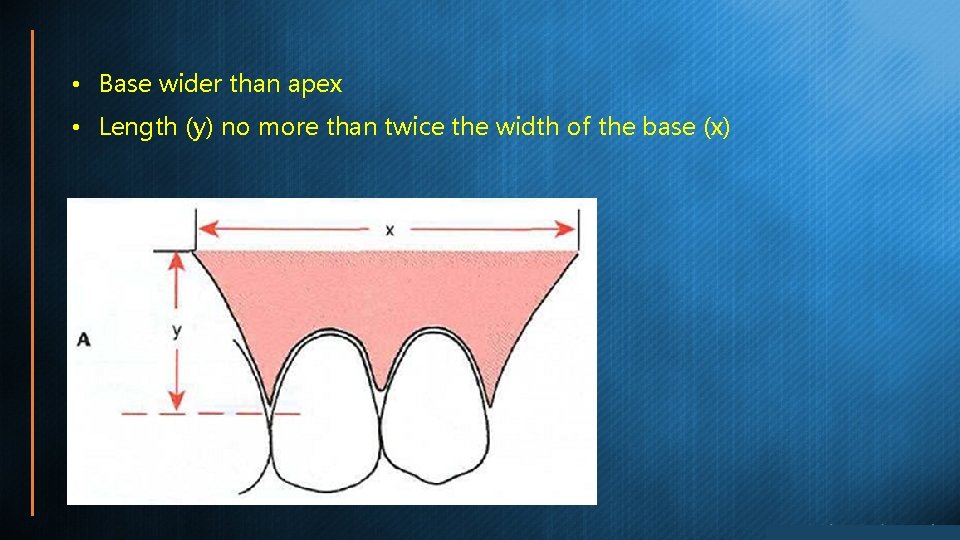
• Base wider than apex • Length (y) no more than twice the width of the base (x)
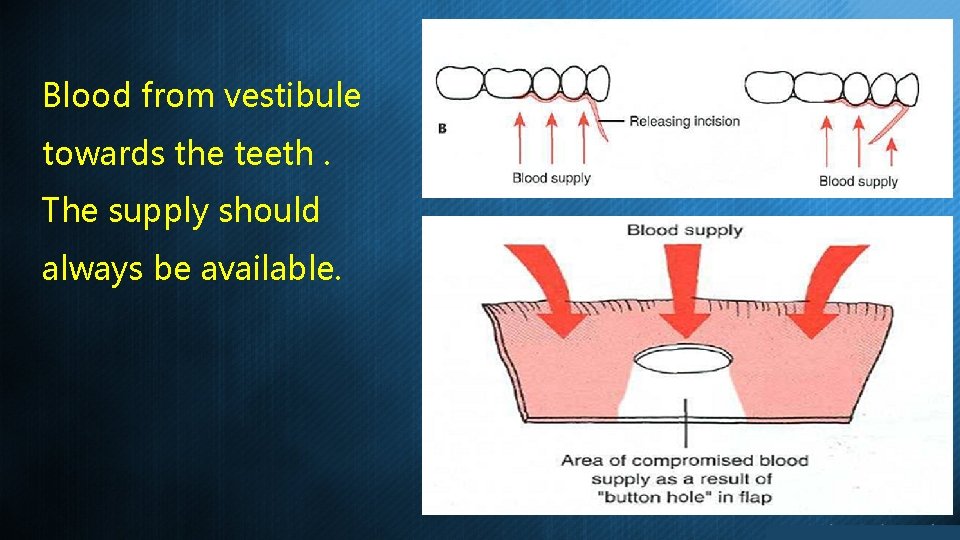
Blood from vestibule towards the teeth. The supply should always be available.

Prevention of flap dehiscence. • Usually achieved by approximation of flap on healthy bone. • Do not place the flap under tension. • Dehiscence will prevent healing by primary intention (which we want to achieve), healing will be by secondary intention (will include bone exposure, pain) healing will by time with granulation tissue which will create scarring.

Prevention of Flap tearing • Long flap heal the same as short flap (do not attempt to make short flap if you need more access). • Well designed flap according to the surgical procedure will reduce the risk of tearing. (choose your flap wisely; envelop, 2 sided, 3 sided) • Gentle handling.

5) Hemostasis Control bleeding during surgery • Good visualization. • Too much bleeding increase the risk of hematoma. Hematoma • Place pressure on the wound. • Decrease vascularity. • Potential space for micro-organisms and infection.

Hemostasis Pressure • Small vessels can be controlled by applying pressure for about 20 -30 seconds • Large vessels require pressure 5 -10 mins continuous • DO NOT WIPE [that will remove the clot]. Dab the bleeder do not wipe it.

• Hemostasis – Heat (thermo-coagulation) • Electrical current (electro-cautery) – Must be applied to the bleeder vessel OTHERWISE it will cause burn. – Clean field with controlled fluid accumulation such as saliva and blood.

• Hemostasis – Ligation • Ligate the bleeding vessel by using suture.

• Hemostasis – Pressure dressing (with hemostatic material or without). • Periodontal pack • Hemostatic agents (bone wax, surgicel®). • The most effective is – Tranexamic acid (5% mouth rinse)

• Dead space: any area that remains devoid of tissue after closure of the wound. • Created (usually due to blood accumulation within space created by the surgery; that will create hematoma which is potential risk for infection) – Remove too much tissue in depth of the wound. – Poor re-approximation of wound planes and edges.

• Elimination of dead space. – Suture all the planes of the wound. – Apply pressure [depending on the size of the space]. – Packing the wound with dressing material which will provide pressure and antibacterial properties. – Drain; if large space is created a drain should be place into the space to prevent fluids and blood accumulation.

Edema • is an accumulation of fluid in the interstitial space because of transudation from damaged vessels and lymphatic obstruction by fibrin • Degree of edema depends on 2 variables: – The amount of tissue injury – The looser the connective tissue.

How to manage edema • Reduce tissue damage and better tissue handling. • Corticosteroids (especially if given before tissue damage (preop)) [4 -8 mg dexamethasone I. M. or I. V. ] • Ask the patient to keep his head above the level of the body in the post-op period. • Post-op Ice application (debatable: no control study to confirm its effectiveness)

6) Prevention of wound infection • Before closure good irrigation to the surgical site will decrease the bacterial count. • Gentle tissue handling and good suturing will decrease the risk of contamination. • Remove all debris and sharp bone to ensure good closure. • Wound debridement; remove any necrotic tissue. All necrotic tissue must be removed before closure. If large space and suture not possible then closure must be achieved with a surgical pack.

7) Patient support • Good medical history • Depending on the operation; we can decide the type of antibiotics and pain killers that we must use.

- Slides: 24