3 Generalized Anxiety DisorderGAD Characterized by Excessive anxiety

3 -Generalized Anxiety Disorder(GAD) ** Characterized by: - Excessive anxiety and worry, about some events/activities (work or school performance) - Difficult to control their worry. - May expect the worst even when there is no apparent reason for concern. - They anticipate disaster and may be overly concerned about money, health, family, work, or other issues. Psychiatric and Mental Health Nursing 1

Generalized Anxiety Disorder. . cont. Diagnostic criteria GAD. - Anxiety/worry associated with “ 3 or more” of the following six symptoms: (more days than not for the past 6 months) 1. Restlessness feeling. 2. Being easily fatigued. 3. Difficulty concentrating or mind going blank. 4. Irritability. 5. Muscle tension. 6. Sleep disturbance (difficulty falling, or restless unsatisfying sleep). Psychiatric and Mental Health Nursing 2

3 -Generalized Anxiety Disorder(GAD) diagnostic criteria. . con. Impairment in social, occupational, or other areas of functioning. - The disturbance is not related to other physiological or medical condition. - The disturbance is not better explained by another mental disorder. Typical worries in GAD about everyday routine events like job responsibilities, finances, health of family members and household tasks. - Client may shift from one worry to another. - NB. Medical condition associated with Anxiety disorder is due to pheochromocytoma “ PCC” Psychiatric and Mental Health Nursing 3

3 -Generalized Anxiety Disorder(GAD) diagnostic criteria. . con. Associated Features support the diagnostic criteria of GAD: - Trembling –Twitching – Feeling shaky – Muscle aches – Soreness – Sweating – Nausea – Diarrhea – Exaggerated startle response. Treatment: - Anxiolytics as Buspirone (Bu. Spar) - SSRI “e. g. Prozac” antidepressants are the most effective treatment. - CBT (Cognitive Behavioral Therapy) Psychiatric and Mental Health Nursing 4

4 -Obsessive-Compulsive & Related Disorders I-Obsessive Compulsive Disorder “OCD” II- Body Dysmorphic Disorder “BDD” III- Trichotillomania (Hair-Pulling Disorder) “HPD” I-Obsessive Compulsive Disorder OCD: Diagnostic Criteria OCD: Presence of obsessions, compulsions, or both: * Obsessions are defined by: 1. Recurrent & persistent unwanted thoughts/images experienced causing marked distress. 2. Individual attempts to ignore/suppress or Psychiatric and Mental Health Nursing 5

I-Obsessive Compulsive Disorder OCD. . Cont. * Compulsions are defined by: 1. Repetitive behaviors (e. g. , hand washing, ordering, checking) or mental acts (e. g. , praying, counting, repeating words) “perform in response to obsession”. 2. The behaviors/mental acts aimed at preventing or reducing anxiety/distress; “not realistic & clearly excessive. Psychiatric and Mental Health Nursing 6

I-Obsessive Compulsive Disorder OCD. . Cont. Obsessions or compulsions are time consuming. Impairment in social, occupational, or other important areas of functioning. Not related to physiological or medical condition. Not better explained by the symptoms of another mental disorder. Psychiatric and Mental Health Nursing 7

I-Obsessive Compulsive Disorder OCD. . Cont. Development and Course: OCD o Prevalence of OCD (1%-2%) o Mean age at onset of OCD is 19. 5 years but may occur on 14 years o The onset of symptoms is typically gradual. o Clients with OCD have higher rates of major depression. o Clients with excessive washing may have concurrent dermatitis. Psychiatric and Mental Health Nursing 8

II- Body Dysmorphic Disorder BDD Diagnostic Criteria BDD: * Preoccupation with perceived defects in physical appearance , but not observable to others. * Individual has performed repetitive behaviors (e. g. , mirror checking, excessive grooming, ) Or mental acts (e. g. , comparing his appearance with others). Psychiatric and Mental Health Nursing 9

II- Body Dysmorphic Disorder. . Cont. * Impairment in social, occupational, or other important areas of functioning. • Not related to other disorder e. g. ED Development and Course: Prevalence of body dysmorphic disorder, females 2. 5% and males 2. 2%. The mean age onset is 16 -17 years, gradual onset & chronic. Psychiatric and Mental Health Nursing 10

III- Trichotillomania (Hair Pulling Disorder)HPD Prevalence l-2%, Females more than males Onset coincides with, or follows puberty. HPD- Diagnostic Criteria. - Recurrent pulling out of hair, resulting in hair loss. -Repeated attempts to decrease or stop hair pulling. - Impairment in social, occupational, or other important areas of functioning. - Not related to another medical condition (e. g. dermatological condition). - Not explained by the symptoms of another Psychiatric and Mental Health Nursing 11

III- Trichotillomania (Hair-Pulling Disorder): . . cont. HPD- Diagnostic Features: - Most common hair (scalp, eyebrows, and eyelids) & less common (axillary, facial, pubic) - Hair pulling may occur briefly but may continue for months or years. - Hair loss may not be clearly visible (i. e. , pulling single hairs from all over a site). - May attempt to conceal or camouflage hair loss (e. g. , by using makeup, scarves, or wigs). - Repeated attempts to decrease or stop hair pulling. Psychiatric and Mental Health Nursing 12

Treatment of OCD: 1. Combines medication and behavior therapy. (Behavior therapy includes exposure &response prevention). 2. Exposure (flooding): assisting the client to confront the situations & stimuli that he usually avoids. 3. Response prevention (systemic desensitization) focuses on delaying or avoiding performance of rituals. - Learns to tolerate anxiety and to recognize that it will decrease without disastrous consequences Psychiatric and Mental Health Nursing 13

5 -Trauma & Stressor Related Disorders: I- Posttraumatic Stress Disorder(PTSD): II- Acute Stress Disorder (ASD) : Stress: Relationship between person &environment, appraised by him as exceeding his resources & endangering wellbeing. Trauma: Sever sudden unexpected overwhelming event outside the range of human experience. I- Posttraumatic Stress Disorder PTSD: development of characteristic symptoms following exposure to extreme Psychiatric and Mental Health Nursing 14

Prevalence: PTSD More prevalent among females than males across lifespan Diagnostic Criteria : A. Exposure to actual or threatened death, serious injury, or sexual violence in (one or more) of the following ways: 1. Directly experiencing the traumatic event. 2. Witnessing the events as it occurred to others. 3. Traumatic events to a close family member or friend. 4. Repeated exposure to aversive details of traumatic event e. g. (police officers, firefighters, emergency medical personnel). Psychiatric and Mental Health Nursing 15

PTSD diagnostic criteria. . Cont. NB: “(Criteria B, C, D, E) is more than 1 month” B. Presence of (one or more) of the following intrusion symptoms: 1. Recurrent, involuntary, and intrusive distressing memories of traumatic event 2. Recurrent distressing dreams related to traumatic event. 3. Individual feels or acts as if the traumatic events were recurring. 4. Intense or prolonged distress at exposure to internal or external cues resemble an aspect of traumatic event. Psychiatric and Mental Health Nursing 16

PTSD diagnostic criteria. . Cont. C. Persistent avoidance of associated stimuli with traumatic events by following (one or both) : 1. Avoidance of distressing memories & thoughts. 2. Avoidance of external reminders associated with traumatic events (people, places, conversations, situations. . etc. ) Psychiatric and Mental Health Nursing 17

PTSD diagnostic criteria. . Cont. D. Negative Alterations in cognitions and mood associated with traumatic events as following (two or more) : 1. Inability to remember an important aspect of traumatic events due to dissociative amnesia. 2. Persistent negative beliefs or expectations about oneself, others, or the world (e. g. , “I am bad, ” “No one can be trusted, ” ‘world is completely dangerous, ”) 3. Persistent, distorted cognitions about traumatic events lead to blame himself or others. Psychiatric and Mental Health Nursing 18

PTSD diagnostic criteria. . Cont. 4. Persistent negative emotional state (fear, horror, anger, guilt, shame). 5. Markedly diminished participation in significant activities. 6. Feelings of detachment from others. 7. Persistent inability to experience positive emotions (e. g. , inability to experience happiness, satisfaction, or loving feelings). Psychiatric and Mental Health Nursing 19

PTSD diagnostic criteria. . Cont. E. Marked alterations in reactivity associated with traumatic events, (two or more) as: 1. Irritable and angry with little or no provocation (verbal or physical aggression). 2. Reckless or self-destructive behavior. 3. Hypervigilance. 4. Exaggerated startle response. 5. Poor concentration. Psychiatric and Mental Health Nursing 20

PTSD diagnostic criteria. . Cont. Impairment in social, occupational, or other important functioning areas. Disturbance not related to another physiological/medical condition. PTSD Development and Course: - PTSD can occur at any age. - Symptoms begin within first 3 months posttrauma - May be delay of months, years, before full diagnostic criteria met. (now called "delayed expression). Psychiatric and Mental Health Nursing 21

II- Acute Stress Disorder (ASD) : *Transient response to severe trauma as (accident, natural disaster, crime, torture. . Etc. ) ASD- Diagnostic Criteria: A. Exposure to actual or threatened death, serious injury, or sexual violation in (one or more) of the following ways: 1. Directly experiencing traumatic event. 2. Witnessing, in person, the event as it occurred to others 3. Learning of event occurred to a close family member or friend. Psychiatric and Mental Health Nursing 22

Acute Stress Disorder. . Cont. 4. Repeated or extreme exposure to aversive details of traumatic event ( police officers, firefighters, emergency medical personnel). Note: not include exposure to electronic media or pictures, unless this exposure is event related. B. Presence of (nine or more) of the following: from any of five categories of intrusion, negative mood, dissociation, avoidance, and arousal, (3 days to 1 Psychiatric and Mental Health Nursing 23

Acute Stress Disorder. . Cont. 1. Recurrent, involuntary, and distressing memories of the traumatic event 2. Recurrent distressing dreams related to the event. 3. Individual feels or acts as if traumatic event was recurring (e. g. flashbacks). 4. Intense psychological or physiological response to cues resemble aspect of traumatic event. 5. Persistent inability to experience positive emotions e. g. happiness, satisfaction. Psychiatric and Mental Health Nursing 24

Acute Stress Disorder. . Cont. 6. Altered sense of reality of oneself or surroundings (e. g. , seeing oneself from another’s perspective). 7. Inability to remember an important aspect of traumatic events (dissociative amnesia). 8. Efforts to avoid distressing memories, thoughts, or feelings about traumatic events. 9. Efforts to avoid external reminders (people, places, . . etc. related to traumatic Psychiatric and Mental Health Nursing 25

Acute Stress Disorder. . Cont. 11. Irritable/angry behavior, verbal/nonverbal with little or no provocation. 12. Hypervigilance. 13. Concentration Problems. 14. Exaggerated startle response. D. Impairment in social, occupational, or other important functioning areas. E. Disturbance not related to another physiological or medical condition. Psychiatric and Mental Health Nursing 26
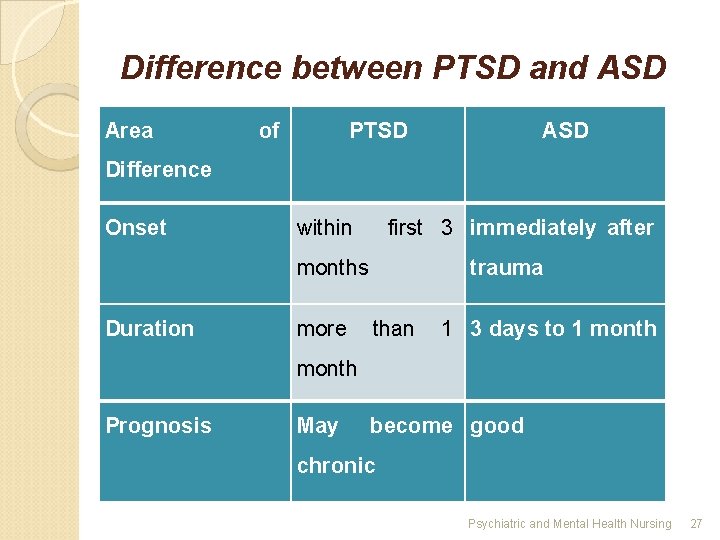
Difference between PTSD and ASD Area of PTSD ASD Difference Onset within first 3 immediately after months Duration more trauma than 1 3 days to 1 month Prognosis May become good chronic Psychiatric and Mental Health Nursing 27

Treatment: (Trauma- and Stressor-Related Disorders) 1 - Debriefing: Helps the individual to gain a clear understanding of trauma, express his thoughts and reactions to trauma & to identify any stress related symptoms. 2 - Cognitive Behavioral Therapy: CBT 3 - In PTSD , client assisted to view self as a survivor rather than a victim. Psychiatric and Mental Health Nursing 28

Drugs used to treat anxiety disorders Anxiolytic drugs: two groups: - Benzodiazepines: may abuse or dependence, as Diazepam (Valium) & Alprazolam (Xanax). - Non-Benzodiazepines: doesn't depress CNS, as Buspirone (Bu. Spar). 2 - Antihistamine drugs: hydroxyzine (Atarax) used to treat anxiety, panic disorder. 3 - Antidepressants: (Prozac), (Tofranil). 4 - Beta-blockers: propranolol (deralin). 5 - Alpha-adrenergic agonist: Clonidine (Catapres). Psychiatric and Mental Health Nursing 29 1.
- Slides: 29