2017 BLSALS PROTOCOL UPDATE County of San Diego

2017 BLS/ALS PROTOCOL UPDATE County of San Diego Kristi L. Koenig, MD. , Emergency Medical Services Medical Director July 1, 2017 -2018

All EMS providers shall be responsible to read and review each protocol and policy in its entirety 2017 -2018

PURPOSE OF PROTOCOLS AND TRAINING Ø Training is designed to familiarize the EMS provider with the use and content of revised protocols and policies Ø Represents a standardized approach Ø Provides quality improvement standards 2017 -2018

USING THE POWER POINT Identifies a change in a protocol or policy, which appears in a rectangular box. A unidirectional arrow leads to what has been changed, deleted or added. Rationale in italics. Teaching points provide further guidance to keep in mind when assessing a patient. 2017 -2018

PROTOCOLS / EDUCATION INCLUDED Ø S-100 Introduction Ø S-101 Glossary of Terms Ø S-122 Allergic Reaction/ Anaphylaxis (Adult) Ø S-127 Dysrhythmias Ø S-144 Stroke/Transient Ischemic Attack *New Protocol* Ø S-104 Skills List-LEADSD Ø S-104 Skills List- Spinal Motion Restriction (SMR) Ø S-104 Additional Skills List Clarification Ø S-162 Allergic Reaction/ Anaphylaxis (Pediatric) 2017 -2018

POLICY / EDUCATION INCLUDED Ø S-411 Reporting of Suspected Abuse Ø S-412 Consent for Prehospital Treatment and Transport Ø S-415 Base Hospital Contact/Patient Transportation and Report Ø Co. SD LEMSIS – County of San Diego - Local Emergency Medical Services Information System Ø Transfer of Care (TOC) Ø Strangulation Education 2017 -2018

Treatment Protocols 2017 -2018

S-100 INTRODUCTION KEY POINTS Ø Updated verbiage to match elements in S-415 Base Hospital Contact/Patient Transportation and Report Ø Deleted: “All BH orders supersede any standing order expect defibrillation and intubation. ” Ø Deleted: “All subsequent medication orders must be from that Base (S-415)” Ø Field may continue with standing orders after initial base hospital contact and once a complete patient report has been provided to the base hospital unless the base hospital directs otherwise 2017 -2018

S-100 INTRODUCTION Changed: provides clarification standing orders may be continued even after base hospital contact. 2017 -2018

S-122 (adult) and S-162(pediatric) Allergic Reaction/Anaphylaxis 2017 -2018

S-122 AND S-162 ALLERGIC REACTION/ANAPHYLAXIS KEY POINTS Ø Recognition of anaphylaxis Ø Protocol revised to emphasize the importance of timely administration of epinephrine Ø Epinephrine is essential to the effective treatment of anaphylaxis Ø CQI identified recent cases where failure to recognize anaphylaxis led to under treatment Ø Deleted categories of mild and acute and replaced with “hives and anaphylaxis/ angioedema” Ø Adult and pediatric identification of symptoms are identical 2017 -2018

S-122 (ADULT) ALLERGIC REACTION/ANAPHYLAXIS Changed to emphasize recognition of anaphylaxis criteria Changed: Q 10” to Q 5” 2017 -2018

S-122 (ADULT) ALLERGIC REACTION/ANAPHYLAXIS Epinephrine is the drug of choice for anaphylaxis and should be administered promptly. 2017 -2018

S-162 (PEDIATRIC) ALLERGIC REACTION/ANAPHYLAXIS Changed to emphasize recognition of anaphylaxis criteria Changed: Q 10” to Q 5” Added: to maintain perfusion Added: adequate perfusion 2017 -2018

S-162 (PEDIATRIC) ALLERGIC REACTION/ANAPHYLAXIS Epinephrine is the drug of choice for anaphylaxis and should be administered promptly. 2017 -2018

ANAPHYLAXIS CRITERIA Signs and symptoms can occur minutes to several hours after unknown exposure Onset can occur rapidly after exposure to a likely allergen Hypotension can occur within minutes to hours after exposure to a known allergen 2017 -2018

WHAT CAN ANAPHYLAXIS LOOK LIKE? § Angioedema: obstructive swelling (tongue and/or lips) or complaints of difficulty swallowing § Skin: pruritus, flushing, hives, angioedema § Respiratory: shortness of breath, wheezing, repetitive cough, hoarseness, trouble breathing or swallowing, dyspnea, wheezebronchospasm, stridor, hypoxemia § Cardiovascular: pale, blue, faint, weak pulse, dizzy, confused, hypotension § GI: vomiting, crampy abdominal pain, diarrhea 2017 -2018

S-123 Altered Neurologic Function 2017 -2018

S-123 ALTERED NEUROLOGICAL FUNCTION KEY POINTS Ø BLS/ALS CVA/Stroke elements removed from S-123 Ø New S-144 Stroke/Transient Ischemic Attack with BLS/ALS treatment guidelines 2017 -2018

S-123 ALTERED NEUROLOGICAL FUNCTION Deleted CVA/Stroke treatment from BLS and ALS 2017 -2018

S-127 Dysrhythmias 2017 -2018

S-127 DYSRHYTHMIAS WHICH DYSRHYTHMIA PROTOCOLS WERE REVISED? : Ø VF/ Pulseless VT Ø PEA/Asystole now separated § PEA § Asystole o Termination of Resuscitation (TOR) 2017 -2018

S-127 DYSRHYTHMIAS HISTORY BEHIND THE REVISIONS Ø Current research recommends high quality CPR (including continuous compressions) are paramount to improving out of hospital cardiac arrest (OHCA) survival rates Ø Most revisions and teaching points focus on the aspects of High Performance CPR (aka: HP-CPR) 2017 -2018

S-127 DYSRHYTHMIAS NEW ELEMENTS ADDED TO DYSRHYTHMIA PROTOCOLS Ø Feedback for 100% of cardiac arrest calls Ø Include all involved in the call in an After Action Report Ø Review monitor data that is captured during the call (also review at a later time for QA purposes) Ø This feedback is to be used to improve practice and the quality of HPCPR in the field with the goal to improve OHCA rates over time Ø NEW Termination of Resuscitation (TOR) criteria have been added and are included in the Asystole Protocol Ø All 5 criteria must be met in order to terminate resuscitation without base contact 2017 -2018

S-127 DYSRHYTHMIAS ELEMENTS OF HIGH PERFORMANCE CPR (HP-CPR) ü Continuous Compressions ü Rate of 110 – Use metronome ü Adequate Depth - at least 2 inches ü Adequate Recoil- allow the chest to rise after compression ü Minimize time off the chest to < 5 seconds for compressor changes or defibrillation ü Avoid Hyperventilation – 1 breath every 6 seconds ü Rotate compressors every 2 minutes to reduce rescuer fatigue and ensure high quality compressions ü Assign a Team Leader to coordinate rotation of compressors to reduce rescuer fatigue, monitor the rate, quality, depth an recoil of compressions, and optimize compression fraction ü Review and provide feedback of all cardiac arrest calls, including all involved in the call, and including all tools available during the call (e. g. , monitor data) 2017 -2018

DYSRHYTHMIAS S-127 HP-CPR and Continuous Compressions Do NOT stop compressions during other interventions such as: q Intubation q IV starts q Medicine administration q Charging the monitor q Rhythm checks 2017 -2018

S-127 VF/Pulseless VT 2017 -2018 UPDATED SLIDE Consider immediate “hot wash” or “after action report” following each cardiac arrest call. Also review/track/trend data from monitors to evaluate quality of resuscitation and provide feedback to the crews
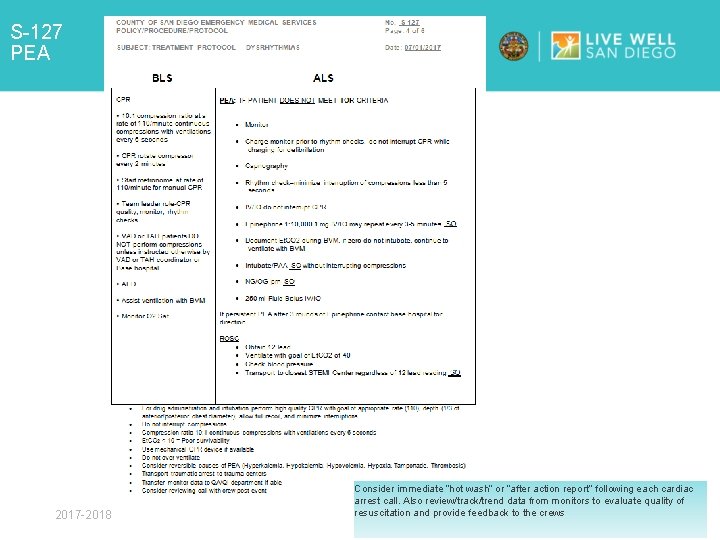

S-127 PEA 2017 -2018 Consider immediate “hot wash” or “after action report” following each cardiac arrest call. Also review/track/trend data from monitors to evaluate quality of resuscitation and provide feedback to the crews

S-127 Asystole w/Termination of Resuscitation (TOR) – See page 3 of 3 for TOR 2017 -2018 Consider immediate “hot wash” or “after action report” following each cardiac arrest call. Also review/track/trend data from monitors to evaluate quality of resuscitation and provide feedback to the crews

S-127 Asystole w/Termination UPDATED SLIDE of Resuscitation (TOR) Termination of Resuscitation aka (TOR) • TOR may only be applied to patients in asystole • All 5 criteria must be met to use the TOR protocol • This protocol only applies to patients of presumed cardiac origin……Drowning, Hypothermia, and Electrocution are excluded • If resuscitation of less than 30 minutes with no improvement, then Base Hospital contact must be made to request the patient pronounced by the BHMD • Asystolic patients of cardiac origin should not be transported unless there are extenuating circumstances (e. g. , family insisting, unsafe scene) 2017 -2018 • If resuscitation of 30 minutes or greater with no improvement then Declaration of Apparent Death can be made with the time documented by the paramedic Consider immediate “hot wash” or “after action report” following each cardiac arrest call. Also review/track/trend data from monitors to evaluate quality of resuscitation and provide feedback to the crews

S-104 Skills List 2017 -2018

Spinal Motion Restriction (SMR) 2017 -2018

S-104 SKILLS LIST SPINAL MOTION RESTRICTION KEY POINTS Ø Formally known as spinal stabilization terminology UPDATED for consistency with current evidence-based data to Spinal Motion Restriction (SMR) Ø Simplified SMR algorithm for prehospital Ø Acronym “NSAIDS” should be used to remember steps in the algorithm Ø Strongly consider SMR in the trauma patient with a mechanism of injury that suggests a risk of spinal injury. This can include but is not limited to ground level falls, motor vehicle collision, motorcycle collision, motor pedestrian collision 2017 -2018
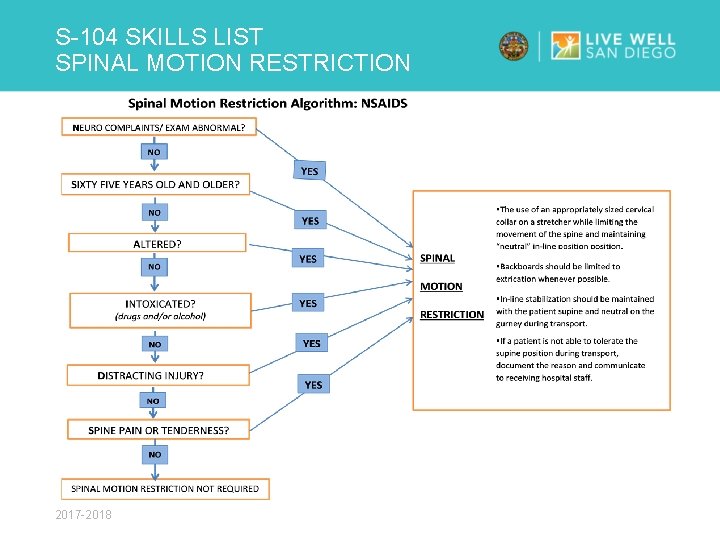
S-104 SKILLS LIST SPINAL MOTION RESTRICTION 2017 -2018

S-104 SKILLS LIST SPINAL MOTION RESTRICTION THE ACRONYM “NSAIDS” SHOULD BE USED TO REMEMBER THE STEPS IN ALGORITHM N-Neurologic exam- Are there any abnormal sensory or motor findings? Weakness/numbness or complaints of paresthesia? Look for focal deficit such as tingling, reduced strength, numbness in an extremity. S-Sixty five- Age greater than or equal to 65 years of age? A-Altered- Is the patient oriented to person, place, time and situation? Is the patient altered in any way? Is there a language barrier? Is the patient cooperative? I-Intoxication- Is there any indication that the person is impaired by drugs or alcohol? D-Distracting injury- Is there any other injury which is capable of producing significant pain in this patient? S-Spine exam- Does the patient complain of neck or back pain? Look for point tenderness in along the entire spine. 2017 -2018

S-104 SKILLS LIST SPINAL MOTION RESTRICTION THE GOALS OF SMR Ø SMR refers to the practice of maintaining the entire spine in a neutral in-line position (anatomic alignment) and minimizing movement of the spine without the use of a backboard Ø However, if the EMS provider determines if it would beneficial to leave the patient restrained on a backboard after extrication due to patient status or short ETA to definitive care, the reason should be clearly documented 2017 -2018

S-104 SKILLS LIST SPINAL MOTION RESTRICTION SMR - PROCEDURE Ø SMR should be accomplished using the most appropriate tool for the specific circumstance Ø Tools useful to minimize movement, compression, or distraction of the spine include: • vacuum splints • straps • scoop stretcher • pneumatic splints • cervical collars • tape and soft materials such as pillows and blankets 2017 -2018

S-104 SKILLS LIST SPINAL MOTION RESTRICTION PATIENTS IN WHOM SPINAL INJURIES CANNOT BE EXCLUDED Ø Language barrier or inability to communicate Ø Lack of cooperation during exam Ø Evidence of alcohol/drug intoxication Ø Painful distracting injury such as a long bone fracture These patients need SMR 2017 -2018

S-104 SKILLS LIST SPINAL MOTION RESTRICTION A MOTOR/SENSORY EXAM INCLUDES A complete patient assessment should be performed before and after application of SMR: Ø Wrist/hand extension and flexion bilaterally Ø Foot plantar/flexion bilaterally Ø Foot dorsiflexion bilaterally Ø Gross sensation in all 4 extremities Ø Check for paresthesia in all 4 extremities 2017 -2018

If you did it, document it. 2017 -2018

S-104 SKILLS LIST SPINAL MOTION RESTRICTION SPECIAL CONSIDERATIONS Ø Patients with severe kyphosis or other anatomical or medical conditions (e. g. , ankylosing spondylitis or rheumatoid arthritis) § Stabilize using a combination of pillow, blanket or other devices Ø Patients with acute or chronic difficulty breathing § Use spinal motion restriction with caution in patients presenting with dyspnea and place patient best suited to protect the airway and ventilation 2017 -2018

LEADSD 2017 -2018

S-104 SKILLS LIST LEADSD KEY POINTS Ø Added LEADSD acronym in comments for reference Ø Revision of LEADSD in Intubation- ET/Stomal Intubation- Perilaryngeal airway adjuncts (ETAD) Ø “D” changed from “Doctor” to “Documentation” “Document presence of Et. CO 2 waveform and Et. CO 2 numeric value at Transfer of Care” Ø Addition of establishment of Et. CO 2 prior to intubation Exception to mandatory use of Et. CO 2 prior to ET Tube/ETAD 2017 -2018
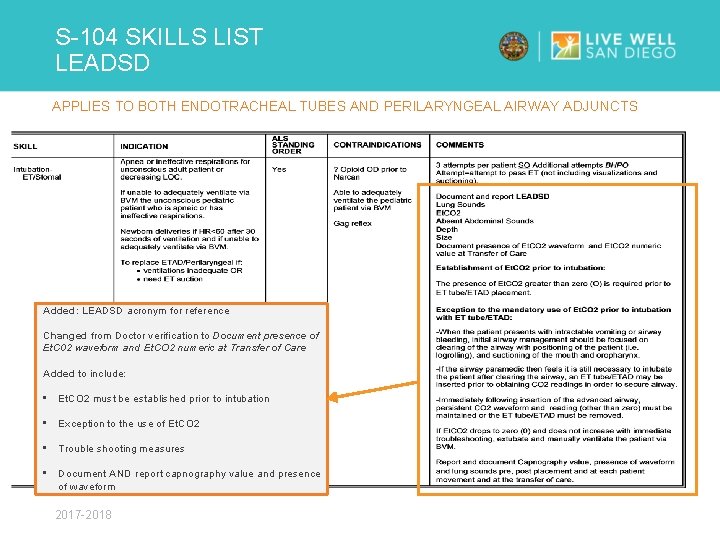
S-104 SKILLS LIST LEADSD APPLIES TO BOTH ENDOTRACHEAL TUBES AND PERILARYNGEAL AIRWAY ADJUNCTS Added: LEADSD acronym for reference Changed from Doctor verification to Document presence of Et. C 02 waveform and Et. CO 2 numeric at Transfer of Care Added to include: • Et. CO 2 must be established prior to intubation • Exception to the use of Et. CO 2 • Trouble shooting measures • Document AND report capnography value and presence of waveform 2017 -2018

Additional Protocol Clarifications 2017 -2018

S-104 SKILLS LIST CLARIFICATIONS TO S-104, NO CHANGES IN PRACTICE • Bougie- Added under indication “vocal cords” • CPAP- Added under contraindication “Non-verbal patients with poor head/neck tone may be too obtunded for CPAP” • Hemostatic gauze-Added under indication “unable to be controlled with direct pressure” • Video Laryngoscopy- Added under Standing Order “yes” and Added under Contraindication “none” 2017 -2018
S-144 Stroke/Transient Ischemic Attack (TIA) 2017 -2018

S-144 STROKE AND TRANSIENT ISCHEMIC ATTACK KEY POINTS Ø Thank you to the San Diego County Stroke Consortium. The following slides teaching points are from: Prehospital Care of Stroke & TIA Patients Update 2016 Ø New protocol for stroke and transient ischemic attack due to evolving time sensitive treatment options Ø Contains elements from S-123 Altered Neurologic Function Ø Importance of correctly identifying patient LAST KNOWN WELL TIME 2017 -2018
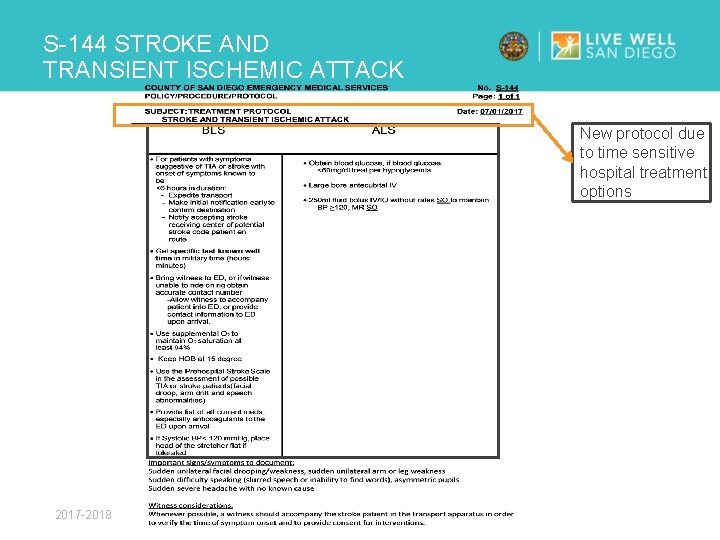

S-144 STROKE AND TRANSIENT ISCHEMIC ATTACK New protocol due to time sensitive hospital treatment options 2017 -2018

S-144 STROKE AND TRANSIENT ISCHEMIC ATTACK OVERVIEW Stroke Sudden and abrupt disruption of blood flow to brain tissue § A blockage of an artery (Ischemic) § A rupture of an artery (Hemorrhagic) TIA Temporary disruption in blood flow to the brain, causing “stroke-like” symptoms TIAs require immediate medical attention Do NOT ignore even if symptoms are improving or have resolved Source: National Stroke Association Explaining Stroke Brochure. Retrieved from: http: //www. stroke. org/sites/default/files/resources/Explaining. Stroke. Brochure. pdfooter 2017 -2018 Mozaffarian, et. Al. Circulation. 2015; e 179 -e 185

S-144 STROKE AND TRANSIENT ISCHEMIC ATTACK GOALS OF PREHOSPITAL THERAPY Ø Early identification of stroke symptoms in the field Ø Prompt transport of patient to nearest stroke receiving center Ø Hospital notification of stroke patient en route Ø Communication (including LAST KNOWN WELL time) Slides courtesy of Prehospital Care of Stroke & TIA Patients Update 2016 2017 -2018

S-144 STROKE AND TRANSIENT ISCHEMIC ATTACK Nurses. Zone, 10/16/2015. Kothari RU, Pancioli A, Liu T, Brott T, Broderick J. “Cincinnati Prehospital Stroke Scale: reproducibility and validity. ” Ann Emerg Med 1999 Apr; 33(4): 373 -8 2017 -2018

S-144 STROKE AND TRANSIENT ISCHEMIC ATTACK RAPIDLY IMPROVING SYMPTOMS Just because a patient is getting better DOES NOT mean the symptoms will completely resolve Ø Stroke symptoms can wax and wane. Even if patients’ symptoms appear to be improving, they can experience rapid neurological decline Ø Err on the side of caution and initiate stroke codes from the field, prior to arrival in the ED Ø Some of these patients will be considered for (and need) immediate IV Alteplase (t. PA) and/or Large Vessel Occlusion (LVO) clot retrieval 2017 -2018

S-144 STROKE AND TRANSIENT ISCHEMIC ATTACK THE STROKE CHAIN OF SURVIVAL Detection: Rapid recognition of stroke symptoms (EMS Involvement) • Dispatch: Early activation and dispatch of emergency medical services (EMS) system by calling 911 (EMS Involvement ) • Delivery: Rapid EMS identification, management, and transport (EMS Involvement ) • Door: Appropriate triage to stroke center (EMS Involvement ) • Data: Rapid triage, evaluation, and management within the emergency department (ED) • Decision: Stroke expertise and therapy selection • Drug: Fibrinolytic therapy, intra-arterial strategies • Disposition: Rapid admission to stroke unit, critical-care unit, Neuro-ICU • HTTP: //CIRC. AHAJOURNALS. ORG/CONTENT/122/18_SUPPL_3/S 818. FULL 2017 -2018 Slides courtesy of: Pre. Hospital Care of Stroke & TIA Patients Update 2016

S-144 STROKE AND TRANSIENT ISCHEMIC ATTACK THE STROKE CHAIN OF SURVIVAL DETECTION Accurate recognition by prehospital personnel is KEY § Obtain Accurate History (Including last known well or last known baseline) § Determine the last time the patient was FREE of acute stroke symptoms and at baseline (use military date/time, not “an hour ago”) § 2017 -2018 • Did someone witness the onset? • Was the patient found with the stroke-like symptoms? • Did patient wake up with symptoms, i. e. last at baseline when went to bed the night before? If there is a witness, bring that person to the ED with you. Obtain a cell phone or contact number if witness is unable to ride along with you Slides courtesy of Pre. Hospital Care of Stroke & TIA Patients Update 2016

S-144 STROKE AND TRANSIENT ISCHEMIC ATTACK Most critical information in stroke patient § Last known well/symptom onset time § Witness (bring in person or obtain direct contact information/cell phone) § Medications Slides courtesy of Pre. Hospital Care of Stroke & TIA Patients Update 2016 2017 -2018

LAST KNOWN WELL TIME IMPORTANT INFORMATION! § Determine the last time the patient was FREE of acute stroke symptoms and at baseline § Important to be precise in gathering information § For patient with “woke up with stroke symptoms, ” time starts when patient was last awake and at baseline, e. g. when went to bed or awake during the night without symptoms § Report and document in military date/time, NOT “an hour ago” Example: “Patient was last known well at 20: 30” NOT “about 45 minutes ago” 2017 -2018

S-144 STROKE AND TRANSIENT ISCHEMIC ATTACK OTHER CONSIDERATIONS-BLOOD GLUCOSE § HYPERglycemia & HYPOglycemia can mimic stroke § Always obtain fingerstick glucose and report values to the ED receiving the patient. If a patient has a low blood glucose, treatment should be given Anyone that EMS providers suspect to be having a stroke or TIA, regardless of symptom resolution, should have a blood glucose checked 2017 -2018 § In the presence of documented hypoglycemia, administer glucose per protocol; otherwise, withhold glucose containing solutions Slides courtesy of Pre. Hospital Care of Stroke & TIA Patients Update 2016

S-144 STROKE AND TRANSIENT ISCHEMIC ATTACK OTHER CONSIDERATIONS-BLOOD PRESSURE § Reduction of BP in the first 24 hours has been associated with poor neurological outcomes 2017 -2018

POLICIES EFFECTIVE JULY 1, 2017 -2018

POLICY UPDATE S-412 Prehospital Treatment and Transportation of Adults - Refusal of Care or Suggested Destination, Release (7/2017) 2017 -2018

S-412 PREHOSPITAL TREATMENT AND TRANSPORTATION OF ADULTS-REFUSAL OR CARE OF SUGGESTED DESTINATION, RELEASE KEY POINTS Ø Updated definition of designated decision maker Ø Updated definition of an emergency patient that is a minor. Made to match S-415 Base Hospital Contact/Patient Transportation and Report 2017 -2018

POLICY UPDATE S-415 Base Hospital Contact/Patient Transportation and Report (7/2017) 2017 -2018

S-415 BASE HOSPITAL CONTACT/ PATIENT TRANSPORTATION AND REPORT KEY POINTS Ø Early base hospital contact is required Ø Field may continue with standing orders after initial base hospital contact and once a complete patient report has been provided to the base hospital unless the base hospital directs otherwise Ø Added: “Shall call Sharp Memorial for pediatric patients who meet trauma center criteria (T-460)” Ø Updated: New radio report requirements for prehospital personnel 2017 -2018

County of San Diego Local Emergency Medical Services Information System (Co. SD LEMSIS) 2017 -2018

Co. SD LEMSIS OBJECTIVES Ø What is Co. SD LEMSIS? Ø Policies related to new Radio Report format Ø New Initial Radio Contact Scripting Ø Policies related to Co. SD LEMSIS patient care documentation 2017 -2018

Co. SD LEMSIS WHAT IS DRIVING THIS CHANGE? Ø Co. SD LEMSIS stands for County of San Diego’s Local Emergency Services Information System Ø Co. SD LEMSIS is the new electronic, cloud based data collection system that meets AB 1129 regulation requirements Ø AB 1129 - state mandate for agencies to submit NEMSIS, CEMSIS and LEMSIS compliant data in real time to the LEMSA (County of San Diego EMS) 2017 -2018

PARADIGM SHIFT KEY CHANGES 1. Early base hospital contact from the field will be necessary 2. Field initiates ALL calls to the base hospital by providing the full CAD incident number 3. No more QCS numbers from MICNs 2017 -2018

Co. SD LEMSIS KEY POINTS Ø QCS Run numbers will no longer be generated by the base hospitals after June 6, 2017, LEMSIS Go-Live Date Ø All radio calls from the field (even those agencies not using LEMSIS Elite) will now be started with the full CAD Incident Number generated at dispatch Ø The CAD Incident Number will be given to the MICN by field providers during the initial base hospital radio contact Ø The MICN needs this to generate a Base Hospital Record (BHR) 2017 -2018

Co. SD LEMSIS INITIAL BASE HOSPITAL RADIO CONTACT Once Base Hospital is available to take call LEMSIS USERS Ø Script “This is medic 10, are you free to take my call? ” If YES, “I am UPLOADing CAD Incident Number XXXXX” Ø The LEMSIS user: data fields transfer to base hospital record. Crew verbally provides pertinent information (per S-415) to the MICN. Ø If no connectivity, the LEMSIS user shall use the Non-LEMSIS script NON-LEMSIS USERS Ø Script “This is medic 11, are you free to take my call? ” If YES, “Our CAD Incident Number is XXXXXXX” Ø The Non-LEMSIS user verbally provides radio report to the MICN with pertinent patient elements per -415 (Base Hospital Contact, Patient Transportation and Report) Ø Early base hospital contact is essential for base and receiving hospitals to prepare to accept the patient; this is one factor that reduces wall time Ø Please provide the entire CAD Incident Number generated by dispatch to the MICN 2017 -2018 S

Co. SD LEMSIS Please take the time to review these new policies posted on EMS Prehospital website Ø NEW patient care documentation policies for all prehospital can be found in § S-601 Documentation Standards and Transferral of Prehospital Care Record (PCR) Info (10/2016) § S-602 EMS Provider Data Submission Process (10/2016) § S-603 System Management and Support During Downtime (10/2016) 2017 -2018

S-601 DOCUMENTATION STANDARDS AND TRANSFER OF PCR INFORMATION IMPORTANT ELEMENTS OF S-601 Ø PCR is made available to receiving hospital staff prior to leaving facility Ø EMS documentation requirements Ø Hospital documentation requirements 2017 -2018

POLICY UPDATE S-411 Reporting of Suspected Child, Dependent Adult, or Elder Abuse/Neglect 2017 -2018

S-411 REPORTING OF SUSPECTED CHILD, DEPENDENT ADULT, OR ELDER ABUSE/NEGLECT KEY POINTS Ø Added: definitions to policy: Abuse, Mandated Reports, Serious Bodily Injury Ø Added: as mandated reporters, it is each agency’s responsibility to ensure a report has been filed Ø Dependent Adult and Elder Abuse/Neglect Ø Added: online reporting website Ø Added: updated contact information for Long Term Care Ombudsman Ø Added: attachment A - Flowsheet for Mandated Reporters Ø Added: general information on - AB 40 - Elder Justice Act (EJA) 2017 -2018

S-411 REPORTING OF SUSPECTED CHILD, DEPENDENT ADULT, OR ELDER ABUSE/NEGLECT Ø Aging & Independent Services (AIS) offers an online referral system for mandated reporters to make referrals. Each mandated report can self-register, reset password and select the agency they are working for when making the referral. https: //www. aiswebreferral. org/ Ø Updated S-411 reflects time sensitive reporting responsibilities (see next slide) Ø Find mandatory reporting links on the Co. SD EMS website 2017 -2018
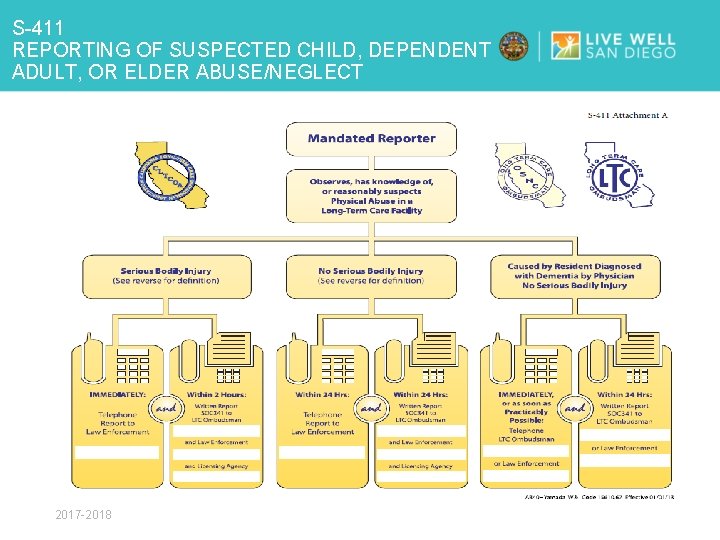
S-411 REPORTING OF SUSPECTED CHILD, DEPENDENT ADULT, OR ELDER ABUSE/NEGLECT 2017 -2018

S-411 REPORTING OF SUSPECTED CHILD, DEPENDENT ADULT, OR ELDER ABUSE/NEGLECT 2017 -2018

Transfer Of Care (TOC) Key Information 2017 -2018

TRANSFER OF CARE (TOC) KEY POINTS Ø Policy related to the transfer of care from paramedics to emergency department personnel Ø S-610 Transfer of Care Guidelines and Procedure & Addendum Ø Policy approved by the Emergency Medical Care Committee on 10/31/2016 2017 -2018

TRANSFER OF CARE (TOC) Transfer of Care (TOC) Ø First. Watch reporting module is live Ø County of San Diego EMS is required to submit quarterly offload time reports to EMSA per AB 1223 Ø Everyone’s responsibility to ensure accurate times Ø TOC completion responsibility is dually owned by prehospital and ED personnel 2017 -2018

TOC AND AB 1223 Health and Safety Code 1797. 120 - EMSA must develop a statewide methodology for the calculation and reporting of ambulance patient offload times by a local EMS agency Health and Safety Code 1797. 225 - Local EMS agency authorized to adopt policies/procedures relating to ambulance patient offload time 2017 -2018

ACCURATE FIRSTWATCH® DATA Current TOC Data (40 -45%) ALS Unit Arrival at ED>>>>>>TOC>>>>>>Crew Completes PCR/Clean Rig/Break/Go Available First. Watch® Data (TBD): ALS Unit Arrival at ED>>>>>>TOC With the initiation of First. Watch® the offload time will stop with TOC time and the pushing of the TOC button within the module 2017 -2018

PRIMARY PROCEDURE FOR TOC S-610 PRIMARY TRANSFER of CARE (TOC) PROCEDURE h The primary process of electronic time-stamped TOC will be via the ALS Transporting Units internet-connected mobile device, signed into the First. Watch® app, at the patient’s bedside (ALS crew to ED Nurse or ALS crew to ED Physician). h Every patient arriving at the ED via an ALS Transporting Unit will require an electronic time-stamped TOC within the First. Watch® app h The patient TOC performance expectation for the County of San Diego Emergency Medical Services System (EMSS) is 30 minutes or less 2017 -2018

DEFAULT PROCEDURE FOR TOC S-610 DEFAULT TRANSFER of CARE (TOC) PROCEDURE h When the ALS Transporting Unit does not provide an internet-connected mobile device to the ED Nurse or Physician for bedside time-stamped TOC, the process will default to using an ED internetconnected desktop or laptop that is signed in to the First. Watch® website h If the ALS Transporting Unit’s mobile device loses internet-connectivity in the ED then the TOC process will default to using an ED internet-connected desktop or laptop that is signed in to the First. Watch® website h If for any reason, an ALS Transporting Unit’s mobile device is unavailable to the ED Nurse or Physician the TOC process will default to using an ED internetconnected desktop or laptop that is signed in to the First. Watch® website h The patient transfer of care performance expectation for the County of San Diego Emergency Medical Services System (EMSS) is 30 minutes or less 2017 -2018
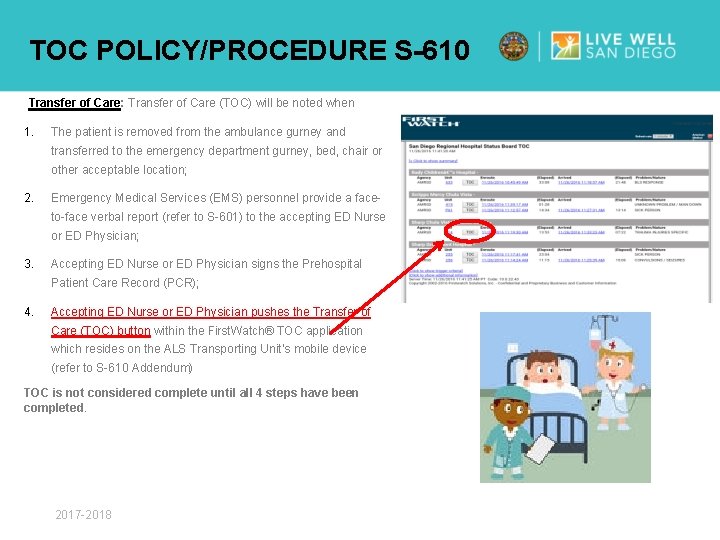
TOC POLICY/PROCEDURE S-610 Transfer of Care: Transfer 1. of Care (TOC) will be noted when The patient is removed from the ambulance gurney and transferred to the emergency department gurney, bed, chair or other acceptable location; 2. Emergency Medical Services (EMS) personnel provide a faceto-face verbal report (refer to S-601) to the accepting ED Nurse or ED Physician; 3. Accepting ED Nurse or ED Physician signs the Prehospital Patient Care Record (PCR); 4. Accepting ED Nurse or ED Physician pushes the Transfer of Care (TOC) button within the First. Watch® TOC application which resides on the ALS Transporting Unit’s mobile device (refer to S-610 Addendum) TOC is not considered complete until all 4 steps have been completed. 2017 -2018

STRANGULATION EDUCATION Strangulation Education 2017 -2018

STRANGULATION EDUCATION Ø San Diego County has a new Strangulation Protocol for law enforcement § Approved on February 1, 2017 by the Chiefs of Police, Sheriff, San Diego District Attorney and San Diego City Attorney § Adopted to increase public safety, promote public health, and to ultimately save lives § Important for prehospital personnel to have knowledge regarding implications of strangulation and current law enforcement protocols Ø In 2012, California Penal Code section 273. 5 was amended to specifically include injuries as a result of strangulation and suffocation as grounds for felony prosecution 2017 -2018

STRANGULATION EDUCATION KEY POINTS Ø Define Choking vs. Strangulation Ø Identify physical and subjective presentation of a victim Ø Identify EMS care priorities 2017 -2018

STRANGULATION EDUCATION CHOKING VS. STRANGULATION Ø Choking is an internal blockage of the airway (e. g. , choking on a piece of food) Ø Strangulation is often an intentional form of abuse due to external pressure applied to the neck. The pressure placed on the neck results in a reduction of blood flow and/or oxygen to the brain, also known as asphyxia. § Loss of consciousness can occur within 5 -10 seconds. Death within minutes § Often even in fatal cases there are no external signs of injury § Only 50% of victims have visible injuries 2017 -2018

STRANGULATION EDUCATION TYPES OF STRANGULATION Ø Manual Strangulation § Use of the fingers or other extremity Ø Ligature Strangulation § Use of some form of cord-like object around the neck without suspension Ø Strangulation by Hanging § Use of some form of cord-like object around the neck with suspension Strangulation injuries are frequently not visible. Domestic Violence professionals must investigate further to gather evidence related to strangulation. 2017 -2018
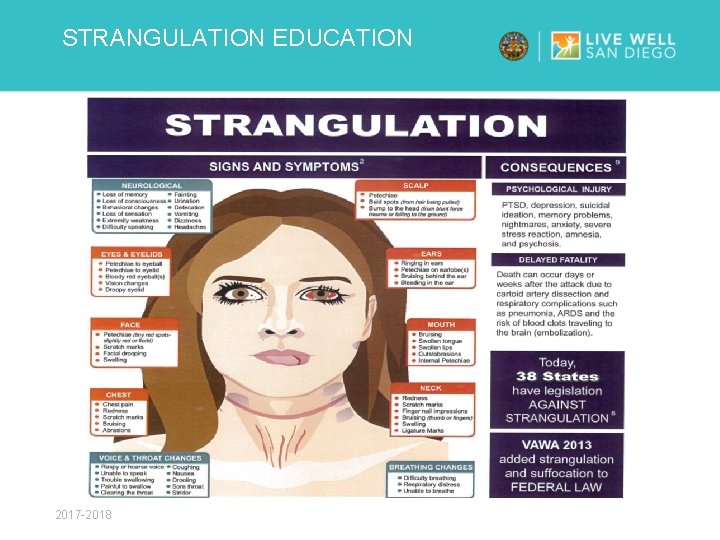
STRANGULATION EDUCATION 2017 -2018

STRANGULATION EDUCATION SIGNS & SYMPTOMS • Red eyes – spots (petechiae) • Neck swelling • Nausea or vomiting • Unsteady • Loss/lapse of memory • Loss of consciousness • Incontinence of bowel or bladder • Droopy eyelid or face • Alt metal status, seizure • Tongue, lip injury • Voice changes 2017 -2018 • Neck or jaw pain • Sore throat • Difficulty breathing • Difficulty swallowing • Voice changes • Headache/lightheaded • Weakness or numbness to arms or legs • Vision changes • Hearing changes • Scalp pain (from hair pulling)

STRANGULATION EDUCATION EMS CARE PRIORITIES Ø Scene safety Ø Assess for immediately life threatening injuries § Difficulty breathing, difficulty swallowing, loss of consciousness, petechial hemorrhage, vision changes, loss of consciousness, urination or defecation Ø Provide privacy for patient to disclose history of event Ø Treat patient and transport to appropriate destination § Strongly consider ED/trauma center if victim is pregnant § Incidence of domestic violence is increased in pregnancy 2017 -2018

STRANGULATION EDUCATION EMS CARE PRIORITIES Ø DOCUMENT: Document patient statement, “quote” patient, visible injuries, observations and physical symptoms. Victims may look fine and say they are fine but may develop delayed complications § Findings may include: swelling, hematomas, vocal cord immobility, displaced laryngeal fracture, hyoid bone fracture, airway obstruction, stroke, carotid dissection, blood clot, respiratory complications or anoxic brain damage 2017 -2018

Thank you for participating in the County of San Diego EMS Protocol Update for July 1, 2017 A special thanks to everyone that participated in protocol review and to the Base Station Physicians Committee for all their hard work and commitment to providing better emergency medical care in San Diego County. Questions? Please contact Quality Assurance Specialist: Meredith Mahoney, RN: Meredith. Mahoney@sdcounty. ca. gov or Diane Ameng, RN: Diane. Ameng@sdcounty. ca. gov Phone: (619)-285 -6429 2017 -2018
- Slides: 95