2016 Wearable Cardioverter Defibrillators Susan ODonoghue M D

2016 Wearable Cardioverter Defibrillators Susan O’Donoghue, M. D. Presenter: 1

Approved Indications for Implantable Cardioverter-Defibrillator (ICD) Secondary prevention: post VT/VF no acute MI or other reversible cause Primary Prevention: CAD with prior MI>40 days EF<35% if Class ll or lll EF<30% if Class l CAD pt must be 3 months post CABG or PCI NICM EF<35% must have 3 mos GDMT Familial or inherited condition with high risk VF (channelopathies; HCM)

Indications for ICD Implantation • ICD placement NOT indicated within 40 days AMI or within 3 months post revascularization or new diagnosis NICM because benefit has not been demonstrated in clinical trials, and a significant number of patients have improvement in EF

WCD 3000 Life. Vest System No adhesive, no gel ECG Response buttons 1. 8 lbs 150 joules Self-gelling defibrillation electrodes Stores ECG, daily use, etc.
Wearable Cardioverter-Defibrillator (WCD) Therapy • 4 -electrode 2 lead system • Programmable VT and VF zones • If arrhythmia detected alert tones and vibration allow patient to abort shock • If patient does not abort, gel deployed; shock strength up to 150 J, up to 5 shocks • Shock efficacy 69 -99%

WCD Clinical Experience • Observational studies reported, none randomized • Variety of patient populations and durations of therapy • Incidence of appropriate shocks 0 -3. 1% • Incidence of inappropriate shock 0 -5. 9%

WCD Clinical Experience in Patients with Newly Diagnosed Cardiomyopathy • There is one study in USA reporting WCD data specifically in patients in the “waiting period” after new Dx of low EF • Retrospective review of all patients prescribed WCD from 2004 -2015 at University of Pittsburg • 254 pts with newly Dx NICM and 271 with newly Dx ICM – average time WCD use 66 days
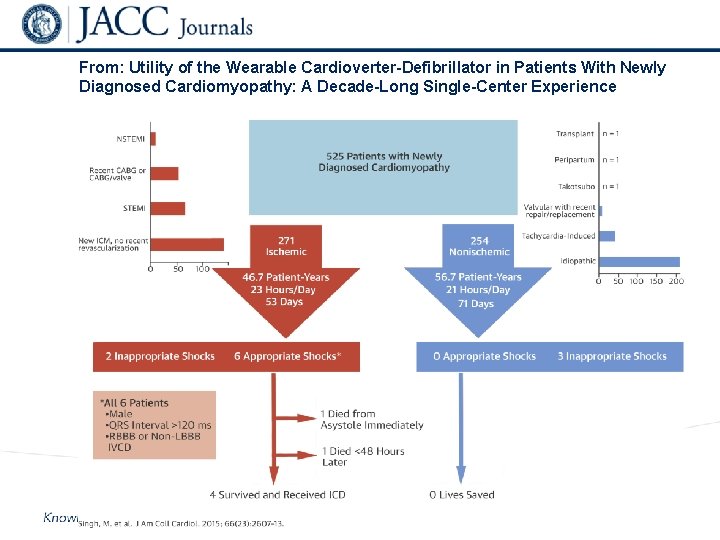
From: Utility of the Wearable Cardioverter-Defibrillator in Patients With Newly Diagnosed Cardiomyopathy: A Decade-Long Single-Center Experience

Conclusions – WCD in Newly Diagnosed Cardiomyopathy • In NICM short term risk is minimal (0/254 pts received an appropriate shock)– routine use of WCD in this group should be prospectively evaluated • In ICM 4/271 pts (1. 5%) survived a WCD shock and received an ICD - all therapies occurred in males with QRS > 120 msec • Lifevest cost during the study $2. 2 million
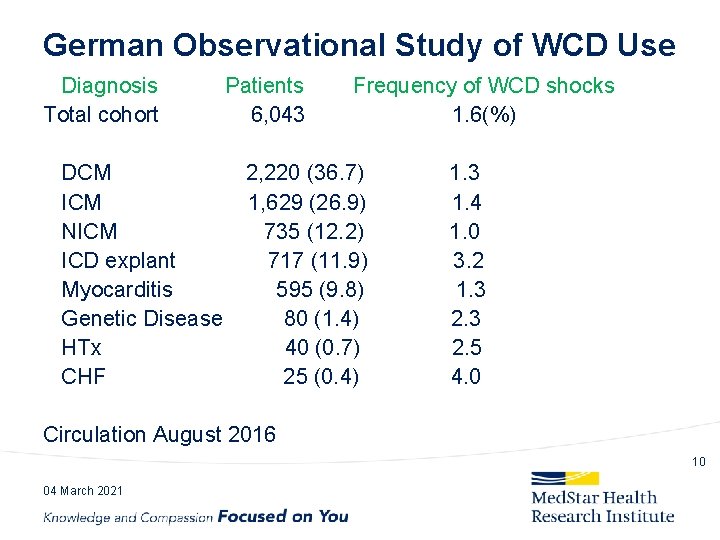
German Observational Study of WCD Use Diagnosis Total cohort DCM ICM NICM ICD explant Myocarditis Genetic Disease HTx CHF Patients 6, 043 Frequency of WCD shocks 1. 6(%) 2, 220 (36. 7) 1, 629 (26. 9) 735 (12. 2) 717 (11. 9) 595 (9. 8) 80 (1. 4) 40 (0. 7) 25 (0. 4) 1. 3 1. 4 1. 0 3. 2 1. 3 2. 5 4. 0 Circulation August 2016 10 04 March 2021

WCD Cost and Cost Efficacy • Lifevest rental approx. $3, 300/month • 2015 cost analysis using $2, 700/month estimated cost <$100, 000/quality-adjusted life year gained as long as the event rate was at least 1. 7% per month J Innov Card Rhythm Management 2015

Applying Classification of Recommendations and Level of Evidence Class IIa Class IIb Class III Benefit >>> Risk Benefit >> Risk Additional studies with focused objectives needed Benefit ≥ Risk Additional studies with broad objectives needed; Additional registry data would be helpful Risk ≥ Benefit No additional studies needed Procedure/ Treatment SHOULD be performed/ administered IT IS REASONABLE to perform procedure/administer treatment Procedure/Treatment MAY BE CONSIDERED Level of Evidence: Level A: Data derived from multiple randomized clinical trials or meta-analyses Multiple populations evaluated; Level B: Data derived from a single randomized trial or nonrandomized studies Limited populations evaluated Level C: Only consensus of experts opinion, case studies, or standard of care Very limited populations evaluated Procedure/Treatment should NOT be performed/administered SINCE IT IS NOT HELPFUL AND MAY BE HARMFUL

AHA Science Advisory on WCD Use • WCD use is reasonable when there is an existing indication for ICD but therapy must be delayed (eg. for infection) (ll. A –level of evidence C) Circulation April 2016

AHA Science Advisory on WCD Use • WCD use may be reaonable when there is concern about heightened risk that may resolve eg newly Dx ICM or NICM (ll. B-level of evidence C) • Caveat : “Blanket use of WCD in this way not appropriate or consistent with clinical evidence, but may be useful in certain patients with high risk features” Circulation April 2016

WCD Contraindications (Class lll) • Nonarrhythmic risk > arrhythmic risk • Life expectancy < 6 months • Patient unable to understand device function or unable to respond to alerts to abort inappropriate shock

WCD – Ongoing Clinical Trials • VEST – randomizing pts within 7 days post MI • SWIFT – observational study evaluating 4 groups: advanced HF, newly Dx CM (ischemic or nonischemic), AMI with Killip class lll-l. V, and pts awaiting ICD reimplant • No randomized studies of new NICM alone are likely because of large number needed given low risk

Medstar Electrophysiologists’ Consensus Recommendations for WCD • Use WCD for those with existing ICD indication when there is need to delay • Patients in the 40 day ICM or 3 month NICM waiting period should be informed of the data (1. 5% risk for ICM, no demonstrated risk for NICM) and the discussion/decision documented – WCD not routinely recommended • In patients with high risk features (eg ICM with QRS>120, large AMI with NSVT ) WCD may be recommended based on physician judgement • Patients presenting with syncope need EP evaluation
- Slides: 17