2015 2016 ATLANTA VAMC HOUSESTAFF ORIENTATION Shahed Brown

2015 -2016 ATLANTA VAMC HOUSESTAFF ORIENTATION Shahed Brown, MD Associate Program Director J. Willis Hurst Internal Medicine Residency, Emory University School of Medicine Andrew Ip, MD Chief Medical Resident 215 -901 -7383

Department of Veterans’ Affairs Mission Statement

Who is a “Veteran”? Drew Carey Ice-T Pat Tillman Chuck Norris Hammer-Time

VA Healthcare • 22 millions veterans in the US – Approximately 9 million receive care within the VA healthcare system • Comprehensive care – Primary care – Specialty care – Mental health – Substance abuse treatment – Home care – Respite care – Palliative care

Veterans are a Unique, Complex, Widely Variable Population

Veterans & Mental Health

Veterans & Mental Health • From 2008: – Prevalence of 36. 9% for mental health diagnoses – 21. 8% diagnosed with PTSD – 17. 4% diagnosed with depression • Active duty veterans < 25 y/o have higher rates of PTSD and alcohol/drug use disorders compared with active duty veterans > 40 J Gen Intern Med. 2012 Sep; 27(9): 1200– 1209 Am J Public Health. 2009; 99: 1651– 8.

THE BASICS
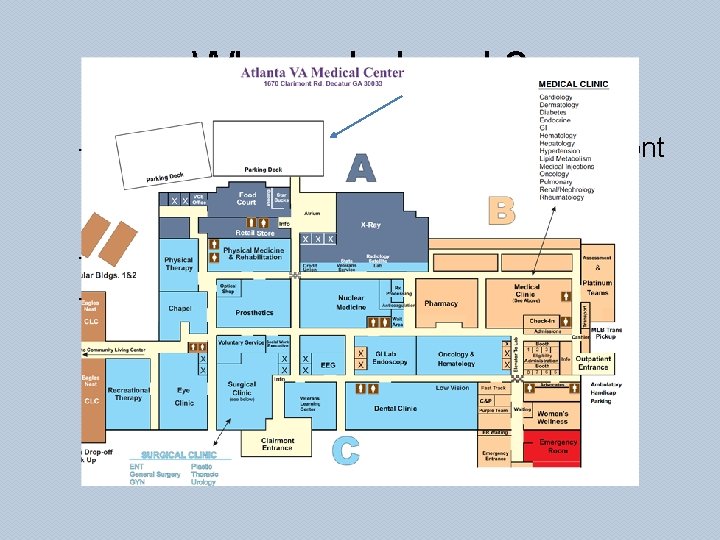
Where do I park? – There are 2 large parking garages in the front & back of the hospital • PLEASE PARK IN THE BACK – Don’t need a special sticker or pass – Obey all traffic & parking rules… this is a federal property, you will have to go to the Richard Russell Federal Building if you want to challenge your parking ticket!!!
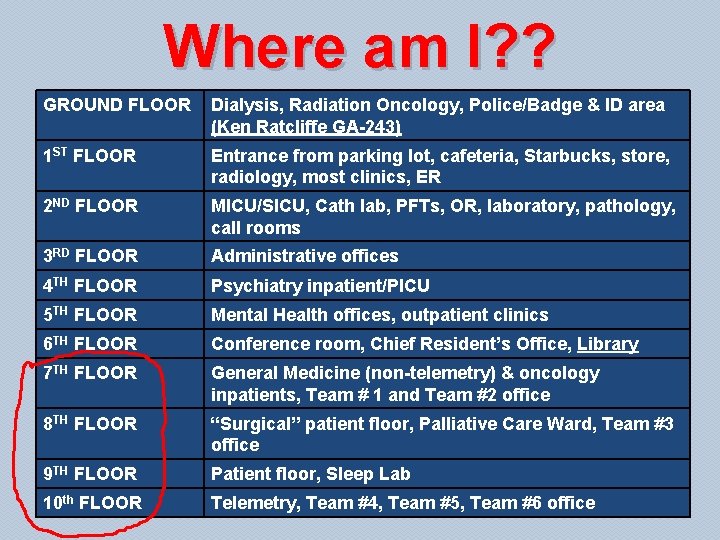
Where am I? ? GROUND FLOOR Dialysis, Radiation Oncology, Police/Badge & ID area (Ken Ratcliffe GA-243) 1 ST FLOOR Entrance from parking lot, cafeteria, Starbucks, store, radiology, most clinics, ER 2 ND FLOOR MICU/SICU, Cath lab, PFTs, OR, laboratory, pathology, call rooms 3 RD FLOOR Administrative offices 4 TH FLOOR Psychiatry inpatient/PICU 5 TH FLOOR Mental Health offices, outpatient clinics 6 TH FLOOR Conference room, Chief Resident’s Office, Library 7 TH FLOOR General Medicine (non-telemetry) & oncology inpatients, Team # 1 and Team #2 office 8 TH FLOOR “Surgical” patient floor, Palliative Care Ward, Team #3 office 9 TH FLOOR Patient floor, Sleep Lab 10 th FLOOR Telemetry, Team #4, Team #5, Team #6 office

Telephone Numbers • Outside of hospital, calling into VA: – (404) 321 -6111, then you press 1 + 4 digit extension • Inside the VA, dial the 4 -digit extension • VA-pager, dial 1590, enter the pager number then your call back number • To call local numbers (Grady, Emory) – need to dial 9 + 404 - then the number • Long Distance - Dial 9 then 1 and the long distance # - use 339960 as PIN

On-Line Training • MUST BE COMPLETED IN ORDER TO RECEIVE COMPUTER ACCESS CODES MUST do the on-line training for privacy & information security EVERY year

Computer Access • Cannot “share” your computer logon information with anyone. • Using someone else’s computer logon will be considered a serious professionalism breach

Computer Access • Codes will expire (deleted from the system) after 3 months of inactivity • After 1 month of inactivity, you can call “HELP” (4357) on a VA-phone & your codes can be reactivated • HOME CPRS Access – see atlvainfo. wikidot. com under general info

VA BADGES • Once you have computer access, you can get a VA-Badge • *Must be fingerprinted as well • See Mr. Ken Ratcliffe in Education – Office is located on Ground Floor – Will give you a document to take over to badge office – Should have your badge within a few days • Ok to use your Grady badge until VA badge is ready

How to get your VA ID Badge • First get fingerprinted! – Go to the ID-badge office on the Ground floor (bottom floor) of the Atlanta VA Medical Center before 2 pm • Approximately 3 days after fingerprinting, contact Mr. Ken Ratcliffe in Education office, also on Ground Floor in Room GA 243 – (404) 321 – 6111, extension 2720 – Ken. Ratcliffe@va. gov • Mr. Ratcliffe will sponsor your badge • Return to the ID office to get your picture taken and ID badge made • Ok to wear Grady badge until VA badge is ready!
This is helpful! Can access this website from any computer! http: //atlvainfo. wikidot. com/
VA ID Badges (“PIV” Badges) http: //atlvainfo. wikidot. com/
Who am I working with? http: //atlvainfo. wikidot. com/

• • We have an electronic on-call schedule for medicine and medicine subspecialties and surgery subspecialties that is accessible via VA-intranet. It is a great way to find out who is covering weekends, or who is on call for urology, etc The link is on the Emory VA info page under “Rosters” and is also accessible from the VISN 7 homepage http: //vaww. visn 7. med. va. gov/intranet/facilities/182247/ http: //atlvainfo. wikidot. com/

Noon Conference - Daily, 12: 00 pm - Tuesday Core conference- INTERNS at noon; residents at 1 pm - Room 6 C-130

EDUCATION & CONFERENCES • Noon conference everyday, unless otherwise noted (12 pm-1 pm) in 6 C-130 Conference Room – Emory Grand Rounds, “Core” Conference Tuesdays • Chief residents work VERY hard on creating and organizing these conferences • Schedule: http: //atlvainfo. wikidot. com/ • Attendance is mandatory, mandatory unless: – Day off – Clinic – Crashing patient • Bring your lunch & enjoy!

EDUCATION & CONFERENCES • INTERN REPORT – THURSDAYS 2: 30 pm to 3: 15 pm on 6 C 130 – COFFEE AND PASTRIES/SNACKS provided!! – Mandatory for all wards interns, optional for subspecialty interns – Goal is to go over intern specific issues such as cross-cover, interesting cases, bread & butter questions

EDUCATION & CONFERENCES • Dr. Jurado Rounds – Occur M-F, 9: 00 am – Usually on pre-call day – Informal discussion of interesting cases – He will come to your team room – Great opportunity to discuss something that you’re stumped on, need advice, or his opinion

CALL ROOMS • Call room in MICU • Call room for Night Float Resident on 8 th floor 164 – Both call rooms are locked, with a bed, computer, TV, telephone and bathroom • Small Conference room on the 6 th floor has a “Snack Fridge” – food for residents who are on call Code for this door: 3 -1 -5; Fridge Code 0 -9 -1 -4
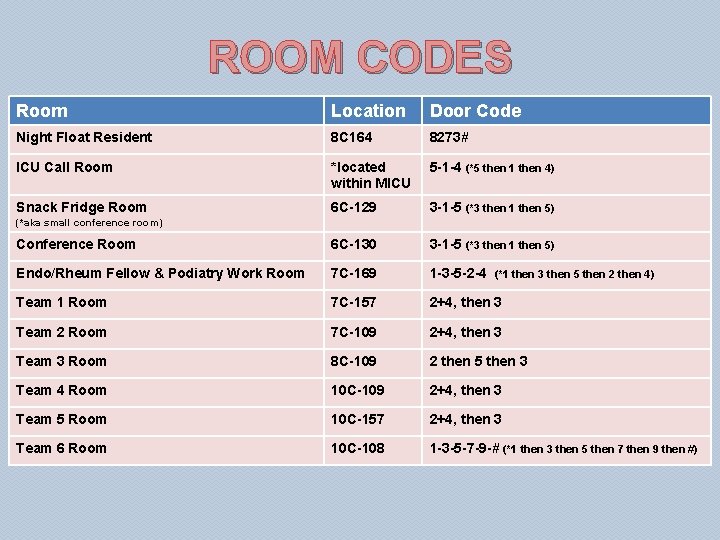
ROOM CODES Room Location Door Code Night Float Resident 8 C 164 8273# ICU Call Room *located within MICU 5 -1 -4 (*5 then 1 then 4) Snack Fridge Room 6 C-129 3 -1 -5 (*3 then 1 then 5) Conference Room 6 C-130 3 -1 -5 (*3 then 1 then 5) Endo/Rheum Fellow & Podiatry Work Room 7 C-169 1 -3 -5 -2 -4 Team 1 Room 7 C-157 2+4, then 3 Team 2 Room 7 C-109 2+4, then 3 Team 3 Room 8 C-109 2 then 5 then 3 Team 4 Room 10 C-109 2+4, then 3 Team 5 Room 10 C-157 2+4, then 3 Team 6 Room 10 C-108 1 -3 -5 -7 -9 -# (*1 then 3 then 5 then 7 then 9 then #) (*aka small conference room) (*1 then 3 then 5 then 2 then 4)

FOOD • You will receive “meal tickets” from your chief resident for each call day – @ 10 tickets/month, $5. 50 per ticket – There is an expiration date!! – Can be redeemed in cafeteria, Starbucks • Team rooms have a mini-fridge if you bring food from home • Several restaurants nearby that deliver

SUMMARY • Use our website!! – atlvainfo. wikidot. com • NOON CONFERENCE – mandatory, bring lunch or use your food vouchers • INTERN REPORT EVERY THURSDAY 2: 30 – free coffee/snacks!

Schedules , your multidisciplinary team

Inpatient Medicine • Each team has a team room – Keypad for entry – Lockers to keep your things secure – Mini-fridge – Computers, printer in each team room • Each team has a mobile computer to facilitate rounds

WORK HOURS • Start time: 7 am – Receive sign out – If you have AM clinic, discuss with resident if you need to come in before clinic (you should not need to unless your resident requests you to). Same with PM clinic – you should not need to return unless on call • On-Call days: – 7 AM to 7 PM

• WE TAKE THE RRC RULES VERY SERIOUSLY – 4 days off per month – <80 hours per week averaged over a 4 week period – LOG DUTY HOURS!!

Schedules • Work with your team to set up the schedule early in the month, including days off • Let your resident and attending know as soon as possible if there are certain days that you need off (no guarantees) • Discuss with your resident expectations for clinic days

Medicine Wards at the VA • 6 Resident Teams – 4 Emory Teams (1 - 4) – 2 Morehouse Teams (5, 6) • 2 Hospitalist (“Direct Care”) Teams – Hospitalist A – Hospitalist B • MICU, CCU rotations – “Closed Unit” • Subspecialists are consultants – Do not have their own inpatient services

Medicine Wards Call Schedule • Every 3 rd day 2 teams are “on-call” – – Team 1, 2 Team 3, 4 Team 5, 6 *Hospitalists admit daily • Care for patients admitted from overnight & admitted during the day – Until 7 PM (7 -days a week) – Total of 10 new patients – Cap of 20 patients total for your team • Night Float resident admits and crosscovers already admitted patients overnight (7 pm-7 am)

Medicine Wards Call Schedule • On your call day, every team member will go to the 6 th floor conference room at 7 am sharp – Night float resident will hand-over their overnight admissions – Hear about your new admissions briefly, discuss what has been done already & what else needs to happen – Admissions are alternated between the 2 “on-call” teams & hospitalists • After morning sign-out, your resident will be contacted by the ER, clinics, etc with admissions until 7 PM

Medicine Wards Call Schedule • On your non-call day, AT LEAST one team member will go to the 6 th floor conference room at 7 am sharp – Night float resident will discuss any crosscover issues that occurred overnight – Good teaching opportunity to hear about the other new patients that were admitted • Be on-time.

Medicine Wards Call: Crosscover • Check the on-call schedule carefully • Every 6 th or so day, you will be on “Crosscover Call”, unless you have PM clinic on a call day – Crosscover already admitted patients for 3 other teams • Teams 1, 3, 5 cover each other • Teams 2, 4, 6 cover each other • When you are not on call & your work is done, you sign-out your patients to the crosscover intern after 5 pm – You are responsible for your patients until 5 pm. • Crosscover intern will cover 3 teams until 9 pm, then sign-out those patients to night float (see schedule on who to page at 9 pm)

Typical Day • • 7 am-9 am – pre-round and work-round 9 -9: 30 – make discharges ready, can call consult 9: 30 or 10: 00 to 11: 30 – attending rounds 11: 30 – 12: 00 – finish up discharges or consults, get lunch • 12: 00 – 1: 00 – Noon conference • Afternoon – pre-call/post-call – finish work/place morning labs and finish signout ; on call admits until 7 pm, cross cover intern stays until 9

“The Book” • Admission log • Hospitalists keep track of admissions • Hospitalist team A/B admit every day, so they typically only take patients from their nocturnist, and then if teaching teams cap they will admit in afternoon

Admissions • MICU/CCU transfers occur from 7 am 2 pm (ICU resident needs to page the book before 2 pm) • Transfers count as “ 1” to team • Transferring service must write “Transfer Summary” note • When ward team accepts the patient: – Write an accept note – Reconcile orders – Change the “Admit To” order to your respective team with the attending, intern and intern pager

Night Float Who is cross-covering my patients? • Before the team leaves the hospital: • Use the “Shift Hand-Off Tool” as your signout sheet • Print it out from CPRS, meet with the crosscover intern and go over your sign-out, from sickest patient to least sick • Must have your cell phone, your resident’s cell phone, and your attending’s cell phone printed on the sheet.

Nurse Practitioners • Each team has a NP – In process of hiring NP for Team #2 – All teams are covered • Integral part of the team – Know the VA system very well & how to get things done – Help you orient to and learn the VA system – Direct patient care – Input and recommendations for patient care – Assistance with care coordination, follow-up

Nurse Practitioners Roles: • Discharge coordination • Liaison between housestaff and nursing • Direct patient care: – Working on system for NP to admit 1 pt each call (will vary team by team) – continued care of acute inpatients – Nurse practitioners can write admission orders, H&P, progress notes, daily orders, discharge instructions, etc – Write orders, place consults, participate in family meetings

Nurse Practitioners Expectations: • Must involve your NP in daily work rounds • NPs must be aware of the care plan & changes in care plan at all times • Beneficial to participate in afternoon “huddle” with your NP, other team members – Discuss potential discharges for next day – Discuss tests, consults, etc that are pending – Make sure everyone is on the same page

Social Workers • Inpatient social workers cover 3 teams each • Office is located on Ground Floor • Communicate daily with your social worker – Keep them updated with new admissions that may have difficult social circumstances – All patients that may need nursing home placement – All patients that may need transportation – Patients that may be in vulnerable situations, potential for abuse – Assist with advanced directives, VA-benefits questions, eligibility • Beneficial to participate in afternoon “huddle” with your SW as well

Pharmacists • Each team has their own dedicated Pharm. D • Medication selection (indications, drug-drug interactions) • Pharmacokinetics • Formulary vs non-formulary medications • Discharge medication counseling • See monthly roster schedule for Pharm. D contact information

Notes, Sign out

History & Physical • Complete H&P, on the day the patient is admitted!!! • HPI: extensive description including location, duration, severity, quality, timing, context, modifying factors and associated signs and symptoms • Include 10 organ systems in ROS • Always document PMHx, Fam Hx and Social Hx • In physical, complete all organ systems; always document “ 4 extremities” in your note

History & Physical Words you should never use in your H&P or progress notes: – “Rule out” : no one pays for ruling out! – “Non-contributory” : use “No heart dz, ” “no DM, ” – “Urosepsis” • Billed as UTI (pays nothing) • Better to use “bacteremia, ” “sepsis of urinary tract origin, ” or just “sepsis”

Sign-Out • Process of talking to the “on-call” intern who will cover your patients from the time you leave until the time you return • Generally a print-out that you update EVERY SINGLE DAY q. Print Your name, your resident’s name, Attending’s name , with the pager for everyone and your cell # q. Include in signout q. IV Access & Do they need it? q. Code status q. Family/Next of kin contact information q. SHORT synopsis of plan for patient

Sign-Out • APPROPRIATE: – “Please check Chem-8 at 10 pm. If K <3. 0, give 40 m. Eq of KCl po x 1” – “Check 10 pm troponin. If > 1. 0, start heparin drip, no bolus” – “Check CBC at 10 pm. If Hgb less than 7. 0, give 2 units PRBCs” Must consent your patients for blood if you are signing this out!!! • INAPPROPRIATE: – “Check CBC” – “Check Chem-8” Discuss the items for follow-up with the on-call intern, as well as any patients that are critically ill

Sign Out Do’s and Don’ts • • • Must have face to face sign-out Students cannot do sign-out Do not sign-out unstable patients Update EVERY SINGLE DAY Make sure your resident has access to your sign out • Use “If… then” statements for all follow-up items

Crosscover Call • When to write a cross-cover note: – Any change in vitals, mental status, or any other pertinent factor that will influence patient’s plan of care – Your follow-up on things signed out to youwhat the value was & what you did with that result: • Repeat Potassium • Troponins – You do not have to write a cross-cover note for writing for prn colace or prn mylanta!

Progress Notes – good example S: No events overnight. Pt reports feeling "okay" this morning. No SOB, CP. No abdominal pain. O: 104/56 (09/27/2008 00: 47) 70 (09/27/2008 00: 47) 20 (09/27/2008 00: 47) 98. 2 F [36. 8 C] (09/27/2008 00: 47) Gen: NAD, resting comfortably, AAOx 2 (person/place) Pulm: Few bibasilar crackles CV: IRRR, s 1 s 2, 2/6 HSM at apex, JVP at 12 cm. Abd: soft, +BS, non-tender, +distension, increased, +shifting dullness. Ext: Warm ext, 2+pitting edema BLE, decub ulcer with dressing in place, no oozing noted. Labs: WBC - 29. 5, 8% bands, 78% segs, PO 4 - 1. 7, K - 3. 6, Mg - 1. 9, BUN – 29, Cr - 0. 7 MEDICATIONS ===================================== 1) ACETAMINOPHEN TAB 650 MG PO Q 6 H PRN PAIN OR HEADACHE ACTIVE 2) ALOH/MGOH/SIMTH REG STRENGTH LIQUID 30 ML PO Q 6 H PRN ACTIVE 3) ASPIRIN (325) TAB 325 MG PO DAILY ACTIVE 4) CHLOROPHYLL/PAPAIN/UREA OINT, TOP SMALL AMOUNT TOP ACTIVE DAILY Apply to coccyx decub. daily. cleanse skin 5) FERROUS SULFATE TAB 325 MG PO DAILY ACTIVE 6) FINASTERIDE (PROSCAR - PROSTATE) TAB 5 MG PO DAILY ACTIVE 7) HEPARIN INJ, SOLN 5000 UNT/0. 5 ML SQ Q 12 H ACTIVE 8) LACTINEX (EQUIV) GRANULES 1 GM/1 PKT PO TID ACTIVE 9) MILK OF MAGNESIA SUSP, ORAL 30 CC PO Q 12 H PRN CONSTIPATION 10) RANITIDINE TAB 150 MG PO DAILY ACTIVE 11) VANCOMYCIN INJ 250 MG PO QID Dilute with 20 cc S. W. 125 mg/2. 5 cc 12) VENLAFAXINE (DOSED DAILY) CAP, SA 75 MG PO DAILY ACTIVE A/P: 90 y/o man c h/o CHF, peritoneal carcinomatosis admitted with SBP, now with severe C-diff colitis. 1. C-diff colitis: - Pt continues to have high stool output. - WBC trending down now, continue with PO vanc with increased dose and dc flagyl per ID recs. Appears stable currently, no signs of tox megacolon. Monitor closely. 2. Acutely decompensated systolic heart failure: - Pt initially diuresed aggresively however diuretics dc'd 2 ndary to concern for volume depletion as pt became hypotensive. - Now appears to be volume overloaded, very delicate balance given CHF and on-going GI losses 2 ndary to c-diff. - Will resume low-dose hydralazine for afterload reduction and schedule lasix IV q 24 hours. - Afib - Heart rate improved - monitor. - Monitor vitals q 4. Strict I/O's. 3. F/E/N- Very poor Po intake currently, likely 2 ndary to multiple acute issues. - Pt started on supplements per nutrition recs. Will likely need to discuss enteral feeding options with family given severity of malnutrition. - Continue to aggresively replete K. Will replete Phos IV. 4. Recent SBP- S/p course of Abx, repeat paracentesis w/o evid of infection. - Monitor. No further Abx at this time, will discuss need for prophylaxis with ID. 5. Peritoneal carcinomatosis: - Unknown etiology at this time. - Urine cytology negative. - Previous peritoneal cytology suspicious for CA, will likely repeat diagnostic paracentesis once more stable. May need U/S marking if ascites improves with diuretics.
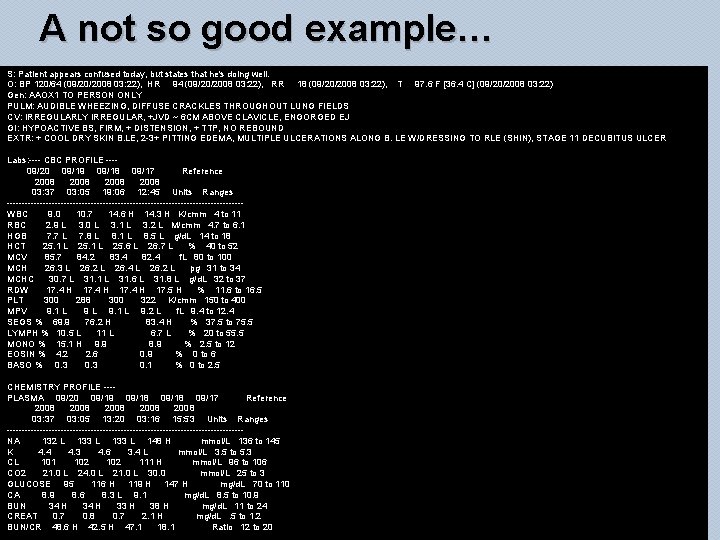
A not so good example… S: Patient appears confused today, but states that he's doing well. O: BP 120/64 (09/20/2008 03: 22), HR 94 (09/20/2008 03: 22), RR 18 (09/20/2008 03: 22), T 97. 6 F [36. 4 C] (09/20/2008 03: 22) Gen: AAOX 1 TO PERSON ONLY PULM: AUDIBLE WHEEZING, DIFFUSE CRACKLES THROUGHOUT LUNG FIELDS CV: IRREGULARLY IRREGULAR, +JVD ~ 6 CM ABOVE CLAVICLE, ENGORGED EJ GI: HYPOACTIVE BS, FIRM, + DISTENSION, + TTP, NO REBOUND EXTR: + COOL DRY SKIN B. LE, 2 -3+ PITTING EDEMA, MULTIPLE ULCERATIONS ALONG B. LE W/DRESSING TO RLE (SHIN), STAGE 11 DECUBITUS ULCER Labs: ---- CBC PROFILE ---09/20 09/19 09/18 09/17 Reference 2008 03: 37 03: 05 19: 06 12: 45 Units Ranges ---------------------------------------WBC 9. 0 10. 7 14. 6 H 14. 3 H K/cmm 4 to 11 RBC 2. 9 L 3. 0 L 3. 1 L 3. 2 L M/cmm 4. 7 to 6. 1 HGB 7. 7 L 7. 8 L 8. 1 L 8. 5 L g/d. L 14 to 18 HCT 25. 1 L 25. 6 L 26. 7 L % 40 to 52 MCV 85. 7 84. 2 83. 4 82. 4 f. L 80 to 100 MCH 26. 3 L 26. 2 L 26. 4 L 26. 2 L pg 31 to 34 MCHC 30. 7 L 31. 1 L 31. 6 L 31. 8 L g/d. L 32 to 37 RDW 17. 4 H 17. 5 H % 11. 6 to 16. 5 PLT 300 288 300 322 K/cmm 150 to 400 MPV 9. 1 L 9. 2 L f. L 9. 4 to 12. 4 SEGS % 69. 9 76. 2 H 83. 4 H % 37. 5 to 75. 5 LYMPH % 10. 5 L 11 L 6. 7 L % 20 to 55. 5 MONO % 15. 1 H 9. 9 8. 9 % 2. 5 to 12 EOSIN % 4. 2 2. 6 0. 9 % 0 to 6 BASO % 0. 3 0. 1 % 0 to 2. 5 CHEMISTRY PROFILE ---PLASMA 09/20 09/19 09/18 09/17 Reference 2008 2008 03: 37 03: 05 13: 20 03: 16 15: 53 Units Ranges ---------------------------------------NA 132 L 133 L 148 H mmol/L 136 to 145 K 4. 4 4. 3 4. 6 3. 4 L mmol/L 3. 5 to 5. 3 CL 101 102 111 H mmol/L 96 to 106 CO 2 21. 0 L 24. 0 L 21. 0 L 30. 0 mmol/L 25 to 3 GLUCOSE 95 116 H 119 H 147 H mg/d. L 70 to 110 CA 8. 9 8. 6 8. 3 L 9. 1 mg/d. L 8. 5 to 10. 9 BUN 34 H 33 H 38 H mg/d. L 11 to 24 CREAT 0. 7 0. 8 0. 7 2. 1 H mg/d. L. 5 to 1. 2 BUN/CR 48. 6 H 42. 5 H 47. 1 18. 1 Ratio 12 to 20
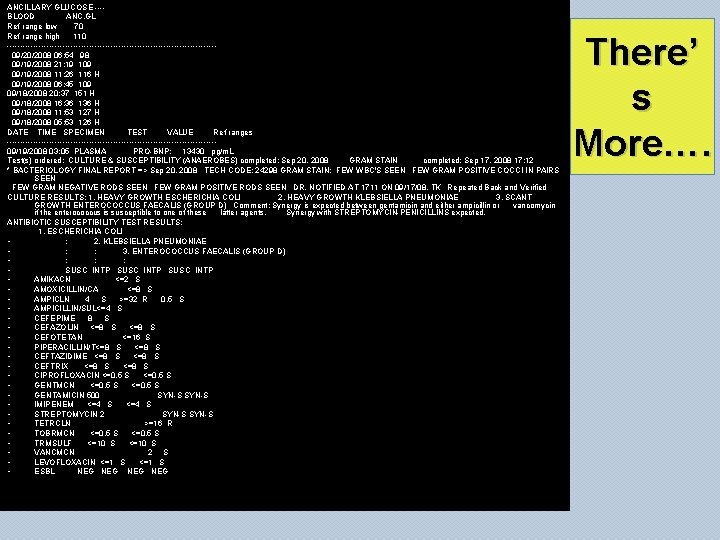
ANCILLARY GLUCOSE ---BLOOD ANC. GL Ref range low 70 Ref range high 110 ---------------------------------------09/20/2008 06: 54 98 09/19/2008 21: 19 109 09/19/2008 11: 26 116 H 09/19/2008 06: 45 109 09/18/2008 20: 37 151 H 09/18/2008 16: 36 136 H 09/18/2008 11: 53 127 H 09/18/2008 05: 53 126 H DATE TIME SPECIMEN TEST VALUE Ref ranges ---------------------------------------09/19/2008 03: 05 PLASMA PRO-BNP: 13430 pg/m. L Test(s) ordered: CULTURE & SUSCEPTIBILITY (ANAEROBES) completed: Sep 20, 2008 GRAM STAIN completed: Sep 17, 2008 17: 12 * BACTERIOLOGY FINAL REPORT => Sep 20, 2008 TECH CODE: 24298 GRAM STAIN: FEW WBC'S SEEN FEW GRAM POSITIVE COCCI IN PAIRS SEEN FEW GRAM NEGATIVE RODS SEEN FEW GRAM POSITIVE RODS SEEN DR. NOTIFIED AT 1711 ON 09/17/08. TK Repeated Back and Verified CULTURE RESULTS: 1. HEAVY GROWTH ESCHERICHIA COLI 2. HEAVY GROWTH KLEBSIELLA PNEUMONIAE 3. SCANT GROWTH ENTEROCOCCUS FAECALIS (GROUP D) Comment: Synergy is expected between gentamicin and either ampicillin or vancomycin if the enterococcus is susceptible to one of these latter agents. Synergy with STREPTOMYCIN-PENICILLINS expected. ANTIBIOTIC SUSCEPTIBILITY TEST RESULTS: 1. ESCHERICHIA COLI • : 2. KLEBSIELLA PNEUMONIAE • : : 3. ENTEROCOCCUS FAECALIS (GROUP D) • : : : • SUSC INTP • AMIKACN <=2 S • AMOXICILLIN/CA <=8 S • AMPICLN 4 S >=32 R 0. 5 S • AMPICILLIN/SUL<=4 S • CEFEPIME 8 S • CEFAZOLIN <=8 S • CEFOTETAN <=16 S • PIPERACILLIN/T<=8 S • CEFTAZIDIME <=8 S • CEFTRIX <=8 S • CIPROFLOXACIN <=0. 5 S • GENTMCN <=0. 5 S • GENTAMICIN 500 SYN-S • IMIPENEM <=4 S • STREPTOMYCIN 2 SYN-S • TETRCLN >=16 R • TOBRMCN <=0. 5 S • TRMSULF <=10 S • VANCMCN 2 S • LEVOFLOXACIN <=1 S • ESBL NEG NEG There’ s More….

ASSESSMENT & PLAN: 90 Y. O. CAUCASIAN MALE WITH SUSPECTED MALIGNANT ASCITES ADMITTED TO THE SERVICE FOR SEPSIS 2/2 SPONTANEOUS BACTERIAL PERITONITIS. 1. SEPSIS: 2/2 SBP E. COLI & E. FAECALIS - Continue Vancomycin 1 G IV Q 12 HRS, Imipenem 500 MG IV Q 6 HRS for now - Hold albumin given elevated BNP levels. 2. PERITONEAL CARCINOMATOSIS (? ): UNKNOWN ETIOLOGY - Diagnostic tap to be done yesterday, patient provided consent; patient's son notified by phone- left a voicemail. However, when we attempted to perform the procedure, the patient appeared confused about our intent and declined the procedure. We did not feel comfortable proceeding with the paracentesis as the patient was insistent upon us not withdrawing fluid from his abdomen and was actively guarding his abdomen with his hands. - Per the cross-cover resident, after we left for the day, the patient's son arrived at the bedside and was very upset about us having not performed the procedure. Dr. has spoken in depth (~1 hour over the phone) with one of the patient's daughters this morning to explain the rationale behind not proceeding with the diagnostic paracentesis at that time. - Will re-attempt diagnostic paracentesis tomorrow with patient's daughter present. 3. ELEVATED BNP: >13, 000 - CXR, diuresis today with Lasix 40 MG IV x 1 now: will monitor Is & Os, reassess and diurese again as needed - All anti-HTN/CHF meds currently being held given HOTN: will re-start once BP normalizes 4. ALTERED MENTAL STATUS: ONGOING SBP VS. DELIRIUM 5. ACUTE RENAL FAILURE: - Cr stable at 0. 7 -0. 8 6. HYPOTENSION: 2/2 SEPSIS- D/C all anti-HTN meds 7. AFIB: STABLE- Not on anticoagulation 2/2 fall risk 8. DEPRESSION: - Continue Effexor 75 MG PO QD 9. ANEMIA: - Continue Fe. SO 4 10. CONSTIPATION: - Continue Colace 100 MG PO BID- Dulcolax 10 MG PRN Active Inpatient Medications (including Supplies): ===================================== • 1) ACETAMINOPHEN TAB 650 MG PO Q 6 H PRN PAIN OR HEADACHE ACTIVE • 2) ALBUTEROL 0. 083% SOLN, INHL 2. 5 MG (3 ML) INH Q 4 H ACTIVE • NEBULIZER • 3) ALOH/MGOH/SIMTH REG STRENGTH LIQUID 30 ML PO Q 6 H PRN ACTIVE • FOR DYSPEPSIA • 4) ASPIRIN (325) TAB 325 MG PO DAILY ACTIVE • 5) DOCUSATE CAP, ORAL 100 MG PO BID FOR STOOL SOFTENER. ACTIVE • 6) FERROUS SULFATE TAB 325 MG PO DAILY ACTIVE • 7) FINASTERIDE (PROSCAR - PROSTATE) TAB 5 MG PO DAILY ACTIVE • 8) FUROSEMIDE INJ, SOLN 40 MG/4 ML IV ONCE ACTIVE • 9) HEPARIN INJ, SOLN 5000 UNT/0. 5 ML SQ Q 12 H ACTIVE • 10) IPRATROPIUM (ATROVENT) 0. 02% SOLN, INHL 0. 5 MG ACTIVE • (2. 5 ML) INH Q 4 H NEBULIZER • 11) MEROPENEM INJ, PWDR MEROPENEM 1000 MG in SOLUTION 100 ACTIVE • ML INFUSE OVER 30 -60 MIN. ASSEMBLED ____ • ACTIVATED _____ IVPB Q 12 H • 12) MILK OF MAGNESIA SUSP, ORAL 30 CC PO Q 12 H PRN ACTIVE • CONSTIPATION • 13) MORPHINE (m. ORPhine)-(MS CONTIN EQUIV) 15 MG PO Q 8 H ACTIVE • 14) VANCOMYCIN INJ VANCOMYCIN 1250 MG in NORMAL ACTIVE • SALINE 500 ML INFUSE OVER 2 HOURS • ASSEMBLED_____ACTIVATED_____ IV DAILY • 15) VENLAFAXINE (DOSED DAILY) CAP, SA 75 MG PO DAILY ACTIVE A/P:

Keeping Track of Patient Data • Have a system for tracking Labs, Radiology, Medications, etc – Cards – Templates • Have a system for a daily checklist – Signout sheets – To-Do list

Helpful Tips for Inpatient Wards • Orders: – Everything is done through CPRS – Enter the orders, and they print where the patient is located (9 th floor, ER) – PAIN MEDS PRN (Tylenol, tramadol, etc), sliding scale insulin, DVT ppx – NEVER assume the nurse will realize you put in orders as soon as you enter them – Best to communicate with nurses what you need done • AM labs: • Don’t forget to order them the day before • “Lab Collect = 3 am” • Medications:

Basic Rules to Remember… n n The patient always comes FIRST Your education and that of others is important, take time to learn and to teach Take care of yourself and your team If you have concerns or problems, bring them up, we are here to help you!

Any questions? Shahed Brown, MD Assistant Chief of Medicine for Education, Atlanta VA Medical Center; Associate Program Director, Emory University Internal Medicine Residency Program Shahed. Brown@va. gov SLewis 6@emory. edu (404) 321 -6111, Ext. 2083 (office) (404) 593 -9923, (cell phone)

The rest of these slides will go into detail about using our charting system. Best way to go about this is to have this powerpoint open while you’re here at the VA getting used to CPRS.

Desktop View • CPRS • VISN 7 Telephone Directory: For VA numbers • Emory Simonweb paging & phonebook • “Clinical Call Back Roster”: Non-medicine services contact info • My computer: takes you to your I: Drive

Computers at the VA • You will receive 2 codes: – Network log-on (to get on a computer) – CPRS log-on (for the charting system) • Cannot log onto a computer unless you have a log-on • Desktop icon for CPRS
CPRS= Computerized Patient Record System

Patient Identifiers • No medical record numbers • Patients are identified by the first letter of last name + last 4 of social security number – Mr. John Doe, SSN: 999 -99 -9999 = D 9999 • This is what you would enter in the first screen once you have logged onto CPRS to pull up a chart
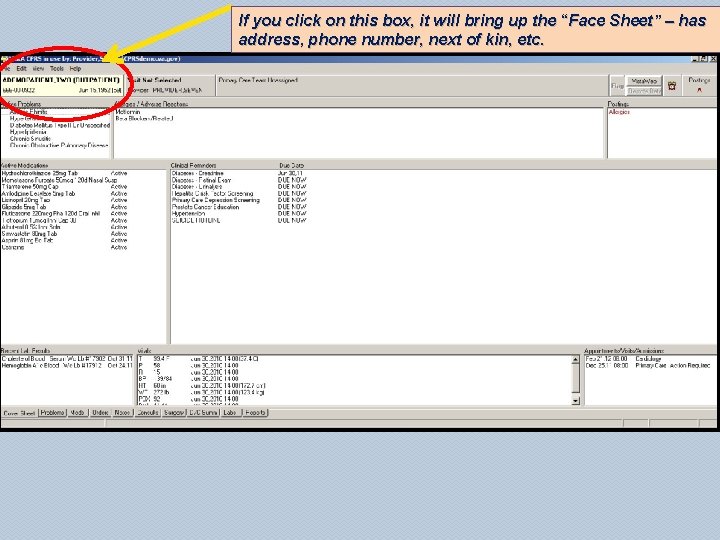
If you click on this box, it will bring up the “Face Sheet” – has address, phone number, next of kin, etc.
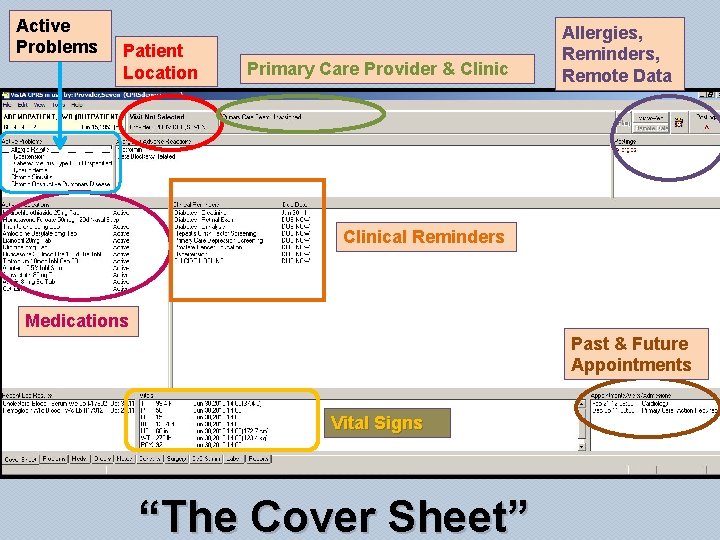
Active Problems Patient Location Primary Care Provider & Clinic Allergies, Reminders, Remote Data Clinical Reminders Medications Past & Future Appointments Vital Signs “The Cover Sheet”
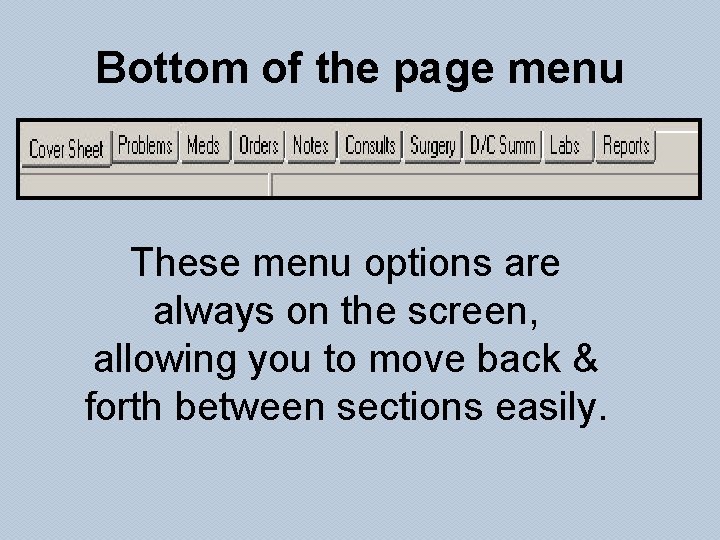
Bottom of the page menu These menu options are always on the screen, allowing you to move back & forth between sections easily.
Problems….
MEDICATIONS

MEDICATIONS When you double click on any medication, it brings up a “History”: - Who prescribed it & when, dosage, frequency, etc. For inpatient: - Tells you the time each dose was given, how it was given, etc
ORDERS

LABS • Must enter lab orders everyday • Phlebotomy (“Lab collect”) – Scheduled daily collections early morning (order for “ 3 am”) – “Immediate Collect” – if you need labs any other time, up until 11 pm – “Ward Collect” - either YOU or the NURSE will obtain specimen (used for Stat/after-hours)

Admit Orders • • Delayed vs. Active orders Easy to use “Admit to Medicine” orders Telemetry orders Medication Reconciliation Hypoglycemia order set Diabetes order bundle Document DVT prophylaxis Text orders
NOTES
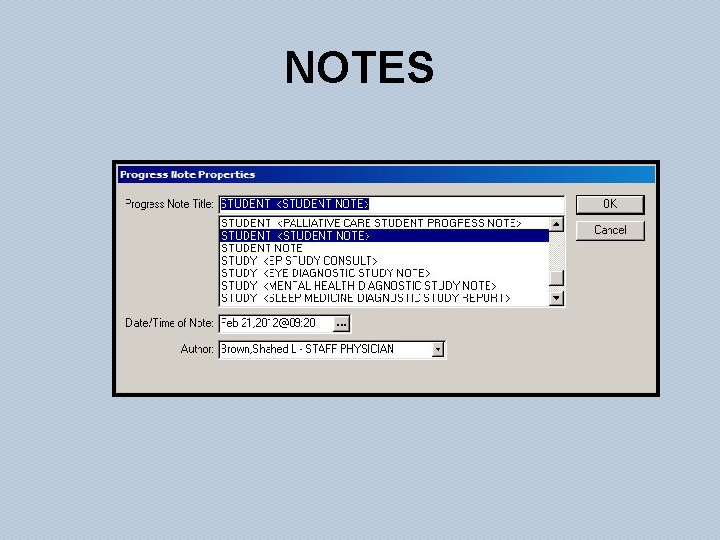
NOTES
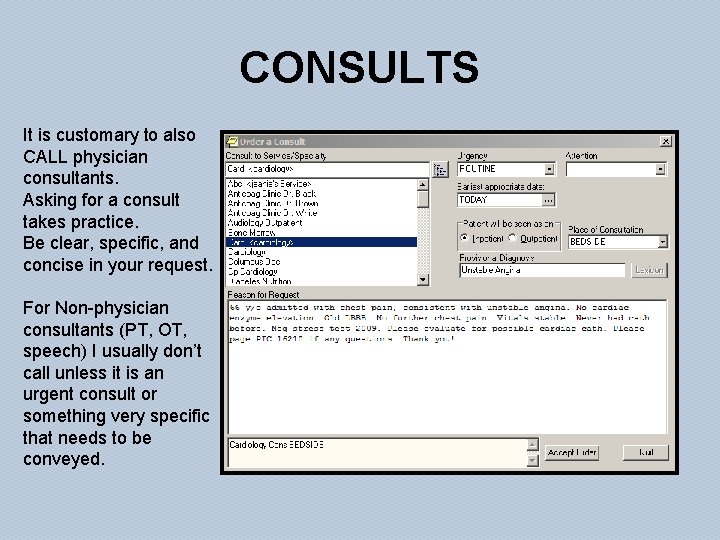
CONSULTS It is customary to also CALL physician consultants. Asking for a consult takes practice. Be clear, specific, and concise in your request. For Non-physician consultants (PT, OT, speech) I usually don’t call unless it is an urgent consult or something very specific that needs to be conveyed.

SURGERY • Lists dictated surgery notes • Detailed description of everything that occurred, from anesthesia, positioning, surgical approach/technique, nursing documentation

DISCHARGE SUMMARIES One of the most valuable places to get information Team Resident is responsible for discharge summaries
LABS
LABS – CUMULATIVE
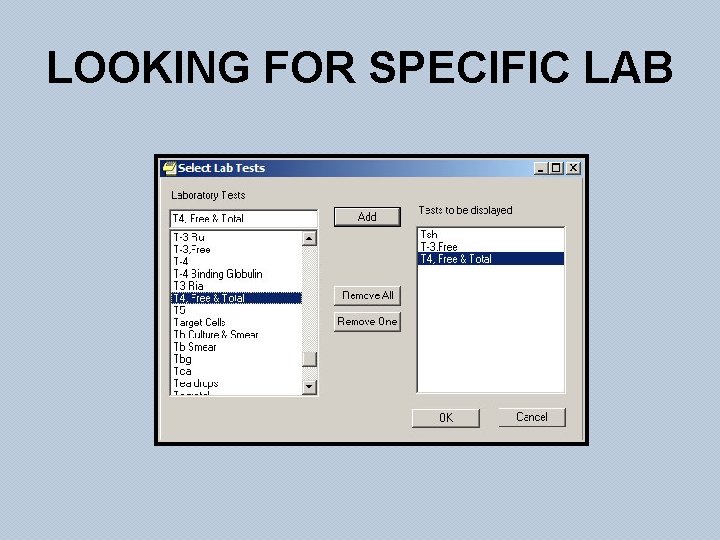
LOOKING FOR SPECIFIC LAB
LAB WORKSHEET
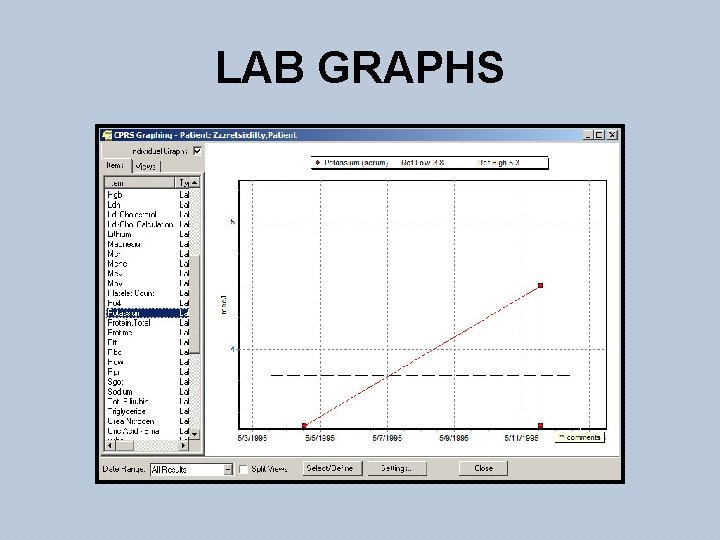
LAB GRAPHS
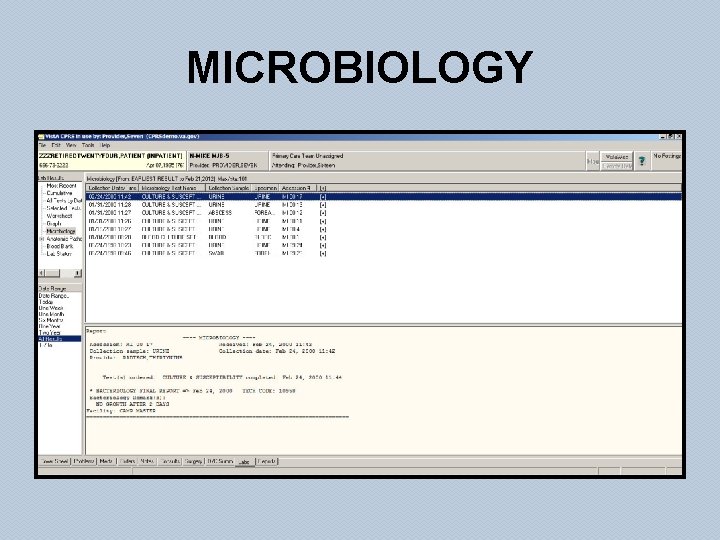
MICROBIOLOGY
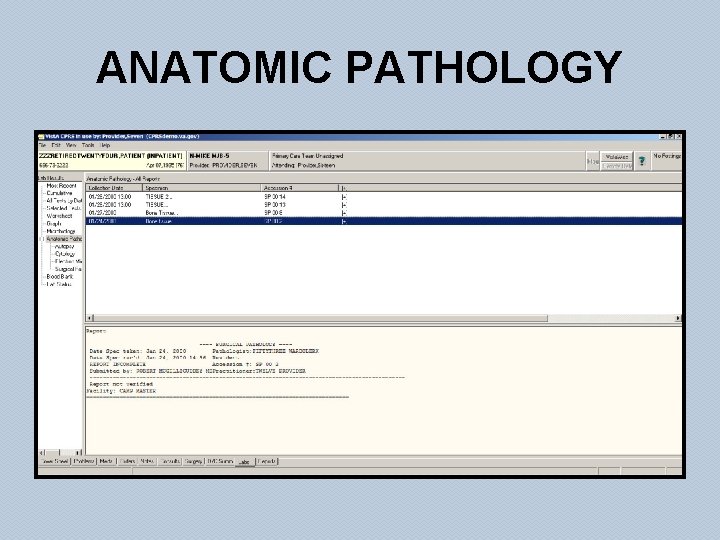
ANATOMIC PATHOLOGY

REPORTS TAB • HEALTH SUMMARY: – Immunization history • IMAGING – Dictated/Transcribed “reads” of imaging • MEDICATION – Charting from nurses
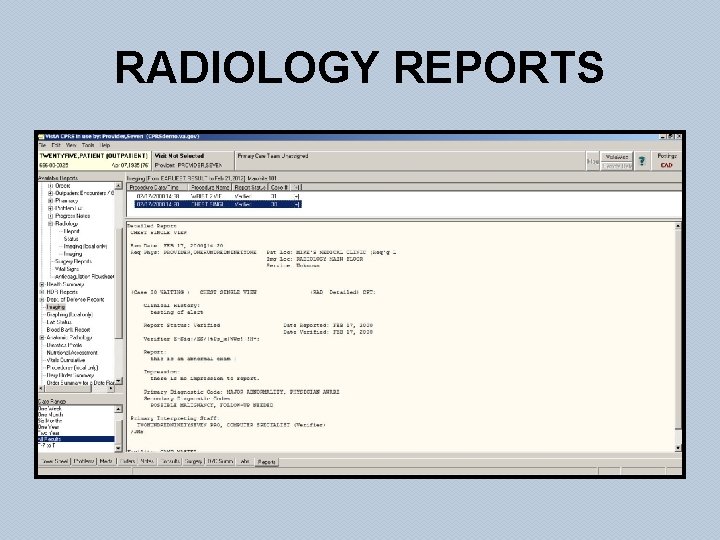
RADIOLOGY REPORTS
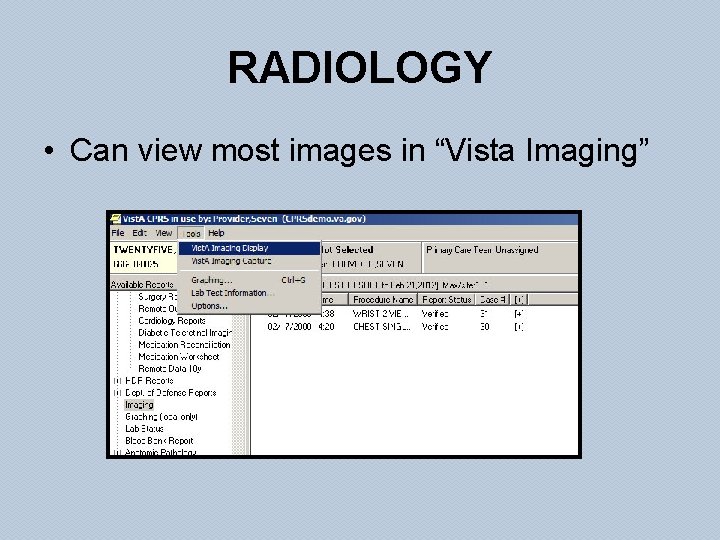
RADIOLOGY • Can view most images in “Vista Imaging”
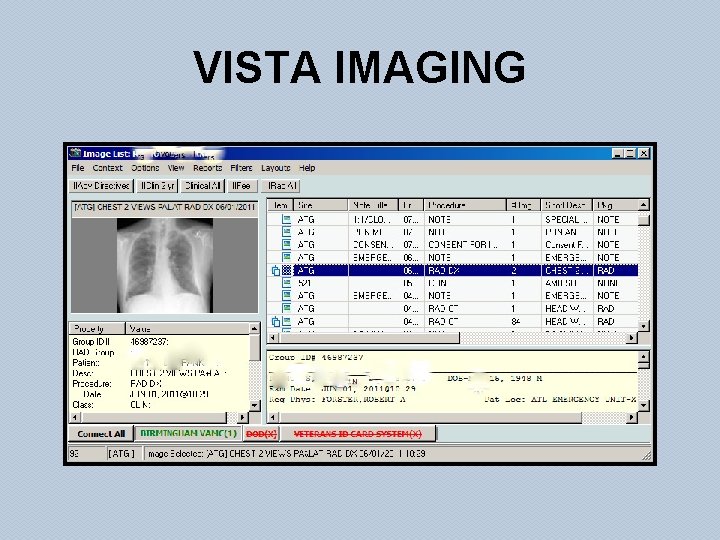
VISTA IMAGING
VISTA IMAGING
VISTA IMAGING

CARDIOLOGY PROCEDURES • Transthoracic & Transesophageal Echocardiograms are located in “Vista Imaging” as PDF files • Cardiac catheterization reports are found in the “Notes” tabs • Nuclear stress test reports are found in the “Reports” tab under imaging
TOOLS TAB
EKGs

Helpful Tools • Atlanta Clinical Resources – UP TO DATE – NEW ENGLAND JOURNAL OF MEDICINE – MICROMEDEX – VISUAL DIAGNOSIS – THERADOC (Log-in: antibiotic, Password: resident) TOOLS tab at top of screen, select “ATLANTA CLINICAL RESOURCES”

ATLANTA CLINICAL RESOURCES
REMOTE DATA
- Slides: 100