2003 CDA Clinical Practice Guidelines Diabetes Office Mgmt

2003 CDA Clinical Practice Guidelines Diabetes Office Mgmt Toronto May 6 2004 J. Robin Conway M. D. Diabetes Clinic - Smiths Falls, ON www. diabetesclinic. ca
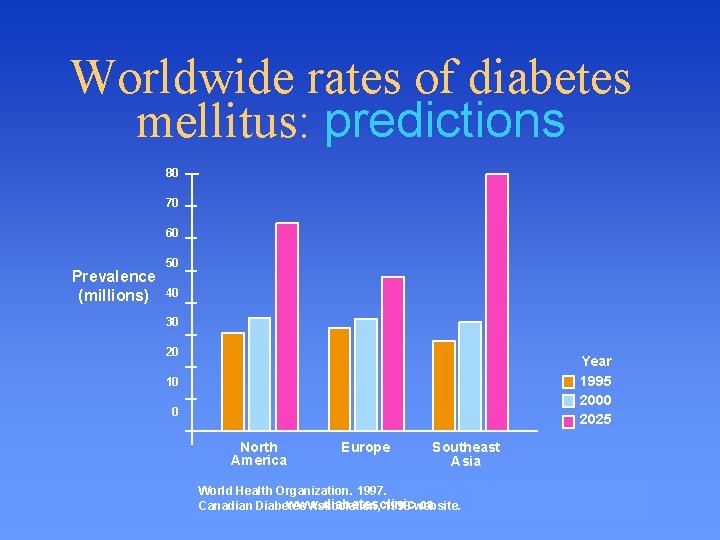
Worldwide rates of diabetes mellitus: predictions 80 70 60 Prevalence (millions) 50 40 30 20 Year 1995 2000 2025 10 0 North America Europe Southeast Asia World Health Organization. 1997. www. diabetesclinic. ca Canadian Diabetes Association, 1998 website.
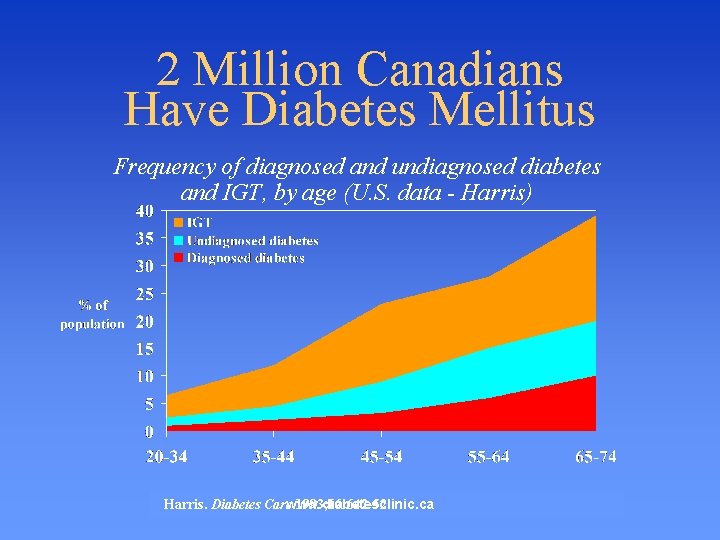
2 Million Canadians Have Diabetes Mellitus Frequency of diagnosed and undiagnosed diabetes and IGT, by age (U. S. data - Harris) Harris. Diabetes Carewww. diabetesclinic. ca 1993; 16: 642 -52.
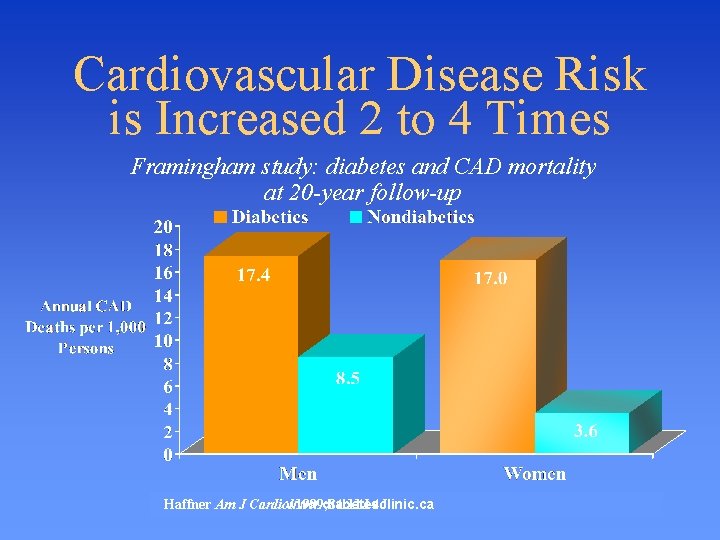
Cardiovascular Disease Risk is Increased 2 to 4 Times Framingham study: diabetes and CAD mortality at 20 -year follow-up Haffner Am J Cardiol 1999; 84: 11 J-4 J. www. diabetesclinic. ca

What proportion of your office visits involve Diabetics? 1. 2. 3. 4. 5. <10% 10 -20% 20 -30% 30 -50% >50% www. diabetesclinic. ca

The burden of Diabetes • 87% of Type 2 Diabetes is managed in Primary Care • Diascan Study: 23. 5% of patients in our office have diabetes Leiter et al. Diabetes Care 2000 • Quebec screening >2 Risk Factors 79% tested 7% Diabetes 13% IGT or IFG 74% No Treatment Advice Strychar I et al. Cdn J Diab 2003(abs) www. diabetesclinic. ca

Glucose Monitoring • Do you do A 1 c to follow glycemic control 1= YES 2= NO www. diabetesclinic. ca

Microvascular Complications • Do you order urine microalbumen test 1= YES 2= NO www. diabetesclinic. ca

Microvascular Complications • Do you use a 10 gm filament for testing sensation in the feet? 1= YES 2= NO www. diabetesclinic. ca

T 2 DM in Family Practice • • • 84% of patients had A 1 c in past year Average A 1 c 7. 9% (goal<7%) 88% had BP check 48% had lipid profiles 28% tested for microalbuminuria 15% had foot exams Harris S et al. Cdn Fam Phys 2003 www. diabetesclinic. ca

Organization and Delivery of Care • Diabetes should be organized using a DHC (Diabetes Healthcare) team approach • People with diabetes should be offered initial and ongoing needs-based diabetes education • The role of diabetes nurse educators and other DHC team members should be enhanced in cooperation with the physician www. diabetesclinic. ca

Structured care • • ACLS ATLS Seattle Defibrillator Experience GREACE Study www. diabetesclinic. ca

Structured Care: • Patients received atorvastatin 10 mg/d (titrated up to 80 mg/d) to reach the NCEP LDL-C goal • Specialist care unit with a strict protocol to achieve NCEP LDL-C target Usual Care: Structured Care VS Usual Care • Treatment from a physician of pt’s choice • All patients had access to any necessary medications, including statins • Included lifestyle modifications (diet and exercise) as well as lipid-lowering medications Αthyros VG et al. Curr Med Res Opin. 2002; 18: 220 -228. www. diabetesclinic. ca
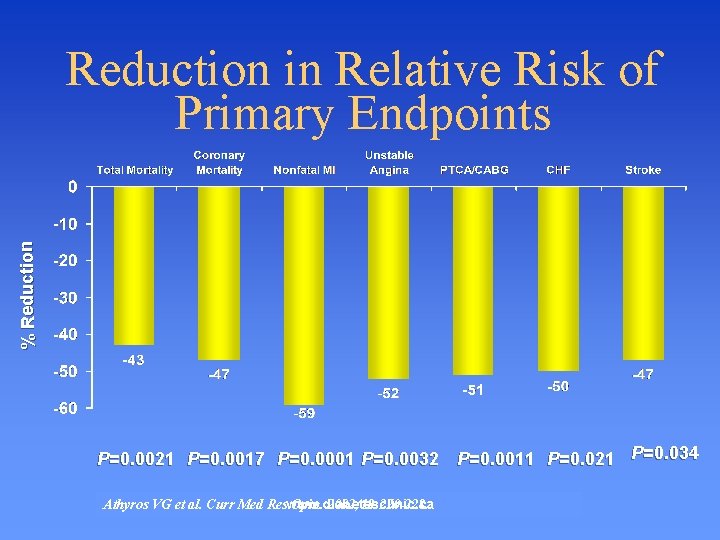
% Reduction in Relative Risk of Primary Endpoints P=0. 0021 P=0. 0017 P=0. 0001 P=0. 0032 P=0. 0011 P=0. 021 P=0. 034 Αthyros VG et al. Curr Med Reswww. diabetesclinic. ca Opin. 2002; 18: 220 -228.

Type 2 Diabetes • • Increasing Prevalence Primary Care Based Forms a large part of a practice Needs structured care approach Team Approach Multiple comorbidities Limited Time & Funding www. diabetesclinic. ca

How can we deal with this? • • Refer all Diabetic Patients? Community Education Programs? Guidelines Based Structured Care? Identify the Diabetics in the practice? Diabetes Day in Office? Get some Diabetes CME? Team Approach in Office? Office Tools? www. diabetesclinic. ca

Diabetes Day in the Office • • Book Diabetic Patients for one day Get office support staff to follow formula Office staff do Wt, BMI, BP, Glucose, lab Have educational material, consider 1 room Follow Guideline Algorithms Use Tools & Flowsheet Extra Staff? Follow up Appt & Lab www. diabetesclinic. ca

Educational Material • • • Canadian Diabetes Assoc: www. diabetes. ca Pharma Companies; Lilly, Novo, Bayer Web Site list www. diabetesclinic. ca Hospital Diabetes Education Program Community Diabetes Education Program www. diabetesclinic. ca
www. diabetesclinic. ca
www. diabetesclinic. ca

www. diabetesclinic. ca
www. diabetesclinic. ca
www. diabetesclinic. ca
www. diabetesclinic. ca
www. diabetesclinic. ca

Screening and Prevention - Type 2 Diabetes • Screen all persons >40 years for type 2 diabetes, with a fasting blood glucose (FPG), every 3 years. • For people with risk factors, screen earlier and /or more frequently, with either FPG or Oral Glucose Tolerance test (OGTT). www. diabetesclinic. ca
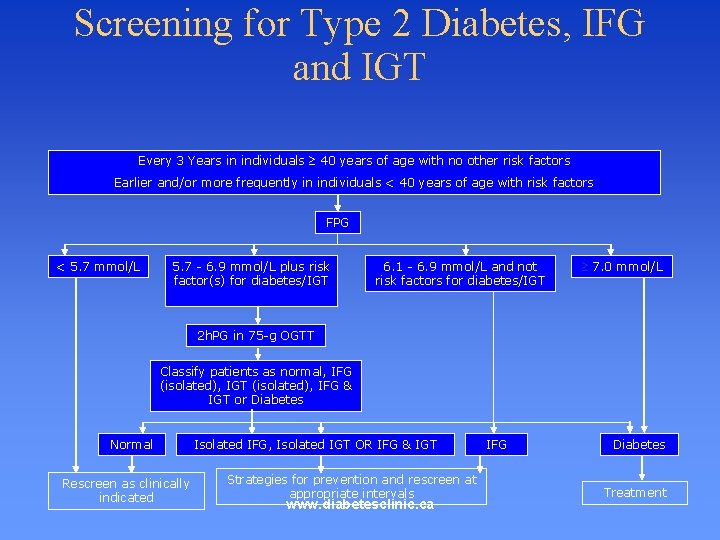
Screening for Type 2 Diabetes, IFG and IGT Every 3 Years in individuals 40 years of age with no other risk factors Earlier and/or more frequently in individuals < 40 years of age with risk factors FPG < 5. 7 mmol/L 5. 7 - 6. 9 mmol/L plus risk factor(s) for diabetes/IGT 6. 1 - 6. 9 mmol/L and not risk factors for diabetes/IGT 7. 0 mmol/L 2 h. PG in 75 -g OGTT Classify patients as normal, IFG (isolated), IGT (isolated), IFG & IGT or Diabetes Normal Rescreen as clinically indicated Isolated IFG, Isolated IGT OR IFG & IGT Strategies for prevention and rescreen at appropriate intervals www. diabetesclinic. ca IFG Diabetes Treatment

Diagnostic Criteria Diagnosis of diabetes FPG 7. 0 mmol/L or Casual PG 11. 1 mmol/L + symptoms of diabetes or 2 h. PG in a 75 g OGTT 11. 1 mmol/L • FPG = fasting plasma glucose, no caloric intake for at least 8 hours • OGTT = oral glucose tolerance test • 2 h. PG = 2 -hour plasma glucose • Casual PG = any time of the day, without regard to the interval since the last meal • Classic symptoms of diabetes = polyuria, polydipsia and unexplained weight loss • A confirmatory laboratory glucose test must be done on another day unless there is unequivocal hyperglycemia and acute metabolic decompensation www. diabetesclinic. ca
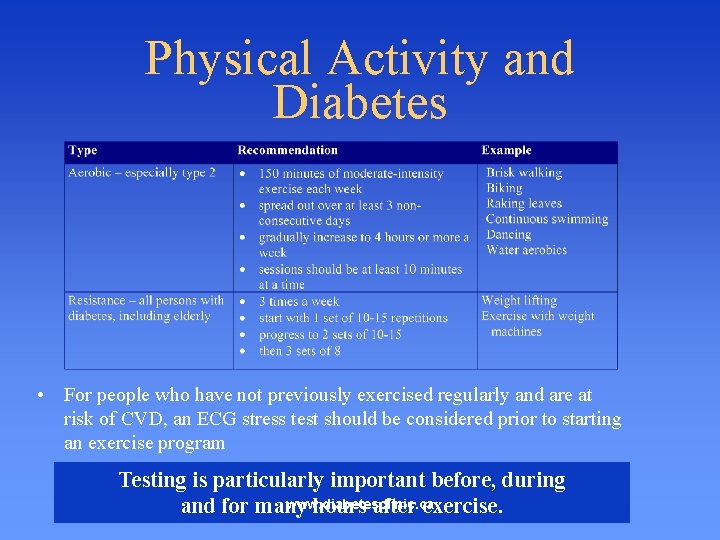

Physical Activity and Diabetes • For people who have not previously exercised regularly and are at risk of CVD, an ECG stress test should be considered prior to starting an exercise program Testing is particularly important before, during www. diabetesclinic. ca and for many hours after exercise.

Nutrition Therapy People with diabetes should: • Receive nutrition counseling by a registered dietitian • Receive individualized meal planning • Follow Canada’s Guidelines for Healthy Eating • People on intensive insulin should also be taught to adjust the insulin for the amount of carbohydrate consumed www. diabetesclinic. ca
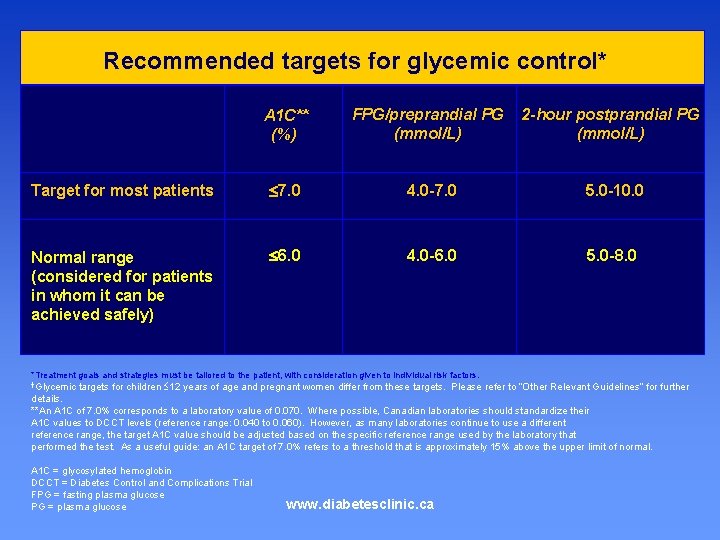
Recommended targets for glycemic control* A 1 C** (%) FPG/preprandial PG (mmol/L) 2 -hour postprandial PG (mmol/L) Target for most patients 7. 0 4. 0 -7. 0 5. 0 -10. 0 Normal range (considered for patients in whom it can be achieved safely) 6. 0 4. 0 -6. 0 5. 0 -8. 0 *Treatment goals and strategies must be tailored to the patient, with consideration given to individual risk factors. targets for children 12 years of age and pregnant women differ from these targets. Please refer to “Other Relevant Guidelines” for further details. **An A 1 C of 7. 0% corresponds to a laboratory value of 0. 070. Where possible, Canadian laboratories should standardize their A 1 C values to DCCT levels (reference range: 0. 040 to 0. 060). However, as many laboratories continue to use a different reference range, the target A 1 C value should be adjusted based on the specific reference range used by the laboratory that performed the test. As a useful guide: an A 1 C target of 7. 0% refers to a threshold that is approximately 15% above the upper limit of normal. †Glycemic A 1 C = glycosylated hemoglobin DCCT = Diabetes Control and Complications Trial FPG = fasting plasma glucose PG = plasma glucose www. diabetesclinic. ca
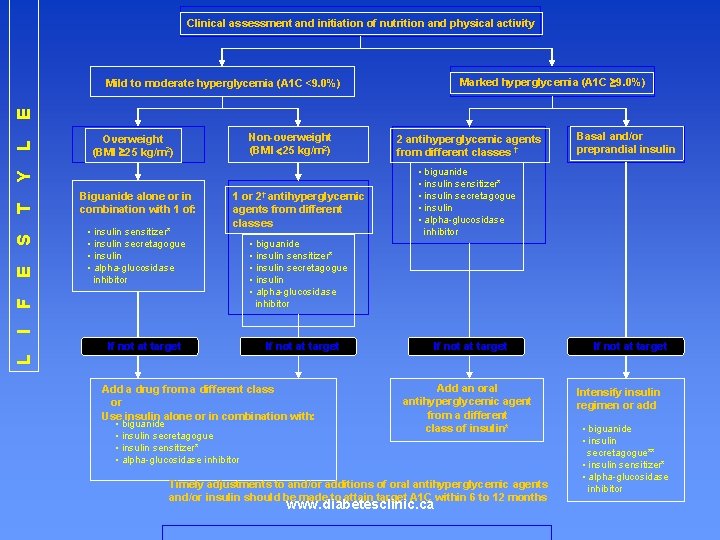
Clinical assessment and initiation of nutrition and physical activity Marked hyperglycemia (A 1 C 9. 0%) Overweight (BMI 25 kg/m 2) Non-overweight (BMI 25 kg/m 2) Biguanide alone or in combination with 1 of: • insulin sensitizer* • insulin secretagogue • insulin • alpha-glucosidase inhibitor 1 or 2† antihyperglycemic agents from different classes 2 antihyperglycemic agents from different classes † Basal and/or preprandial insulin • biguanide • insulin sensitizer* • insulin secretagogue • insulin • alpha-glucosidase inhibitor I F E S T Y L E Mild to moderate hyperglycemia (A 1 C <9. 0%) If not at target L If not at target Add a drug from a different class or Use insulin alone or in combination with: • biguanide • insulin secretagogue • insulin sensitizer* • alpha-glucosidase inhibitor Add an oral antihyperglycemic agent from a different class of insulin* Timely adjustments to and/or additions of oral antihyperglycemic agents and/or insulin should be made to attain target A 1 C within 6 to 12 months www. diabetesclinic. ca Intensify insulin regimen or add • biguanide • insulin secretagogue** • insulin sensitizer* • alpha-glucosidase inhibitor

Economics • • Gen Ass Int Ass Counselling Insulin Rx Type 2 Flow Glucose Urine Venipuncture A 003 A 007 K 013 K 029 K 030 G 002 G 009 G 489 $54. 10 $28. 50 $50. 45 $30. 00 $ 1. 97 $ 4. 20 $ 2. 27 www. diabetesclinic. ca 4 x/yr 6 x/yr 3 x/yr
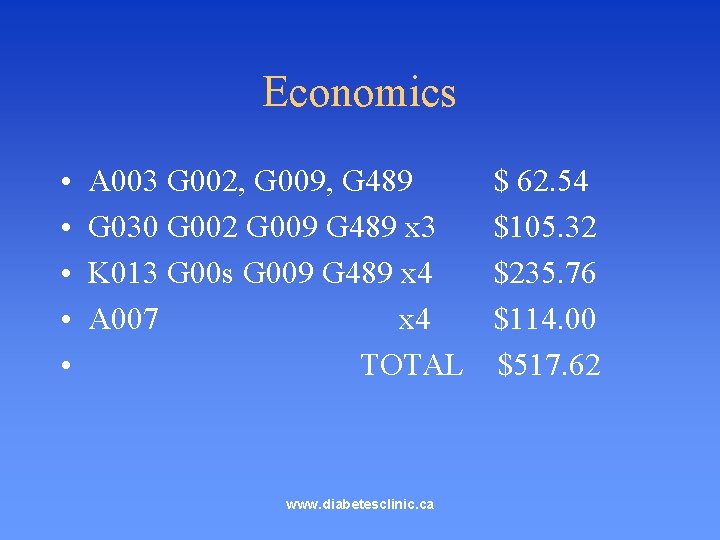
Economics • • • A 003 G 002, G 009, G 489 G 030 G 002 G 009 G 489 x 3 K 013 G 00 s G 009 G 489 x 4 A 007 x 4 TOTAL www. diabetesclinic. ca $ 62. 54 $105. 32 $235. 76 $114. 00 $517. 62

FLOWSHEETS www. diabetesclinic. ca
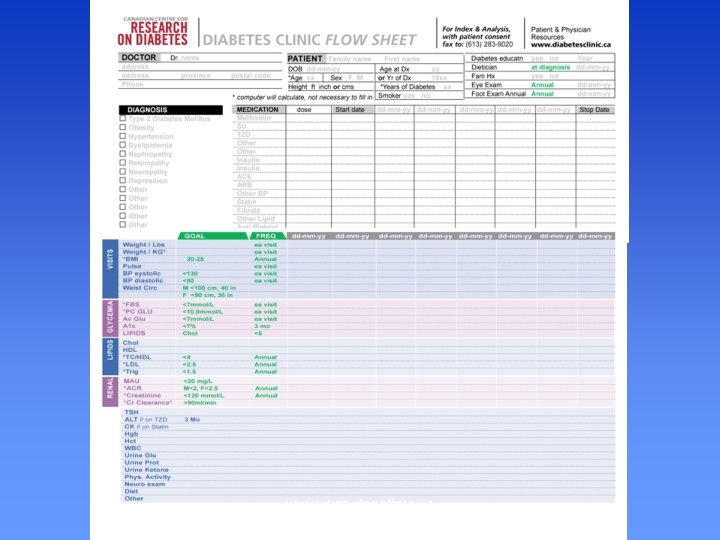
www. diabetesclinic. ca
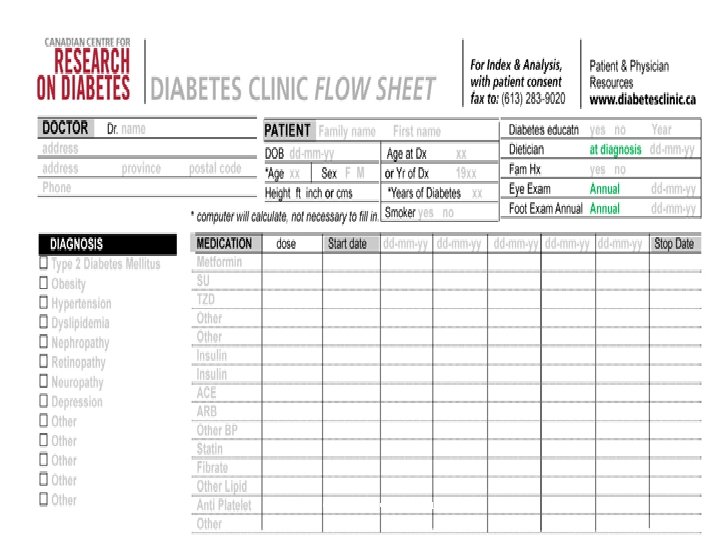

www. diabetesclinic. ca
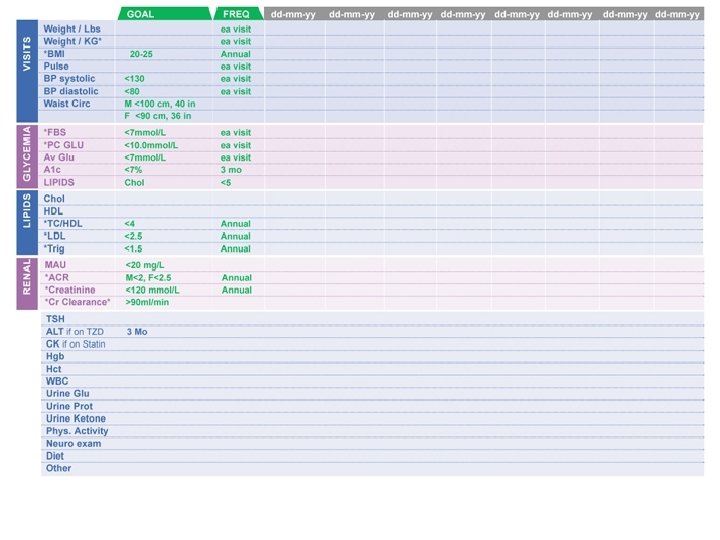
www. diabetesclinic. ca

ABC of Diabetes • A 1 c <7 • Blood Pressure <130/80 • Chol/HDL <4, LDL <2. 5, Trig <1. 5 • ACR <2 men, <2. 5 women • ACE • ASA www. diabetesclinic. ca

INVOLVE THE PATIENT www. diabetesclinic. ca
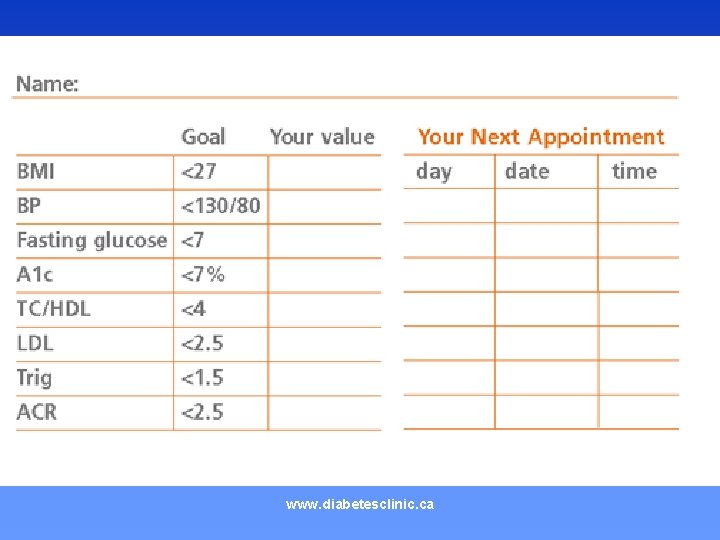
www. diabetesclinic. ca

www. diabetesclinic. ca

In Conclusion • Prevalence of type 2 diabetes is increasing dramatically • Majority of patients are diagnosed and treated by the family physician • New paradigm: need to be much more aggressive early in the treatment of these patients utilizing dual therapies • Hypoglycemia can be managed through proper treatment choices and lifestyle management • Glucose is a continuous progressive risk factor for cardiovascular disease www. diabetesclinic. ca

Questions? www. diabetesclinic. ca
- Slides: 44