2 Concepts of Healing Healing Bridge of cells

2 Concepts of Healing

Healing ___________: ______________ Bridge of cells binds ends of wound together _____________: Separation is large-2 nd ° Sprains Tissue must fill space-starting at bottom and sides of wound _______________
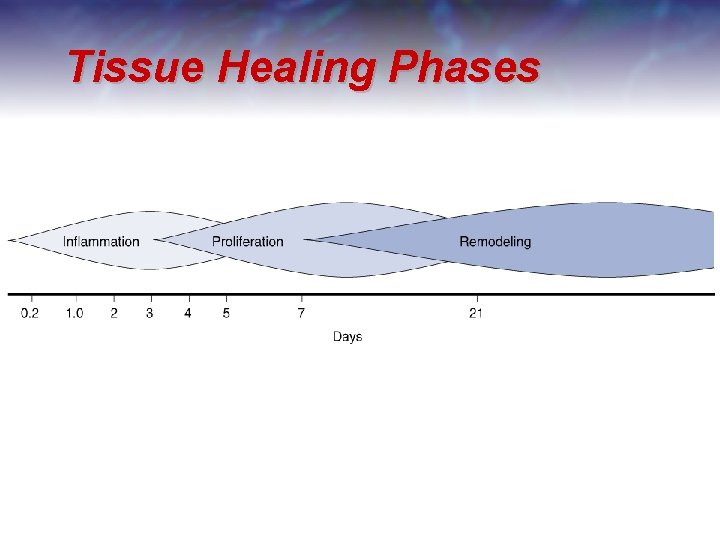
Tissue Healing Phases

Inflammation Phase Necessary phase ____________ Complex cellular and chemical interactions take place Neutrophils/PMN’s abound Macrohages replace PMNs in 24 -48 h to debride area

Signs of Inflammation _______ Temperature increase _______ Pain ________

Causes of Inflammation The signs of inflammation occur because of the increased metabolic activity and fluid in the region and the tissue damage that has occurred. Loss of function is produced by the primary signs of inflammation.
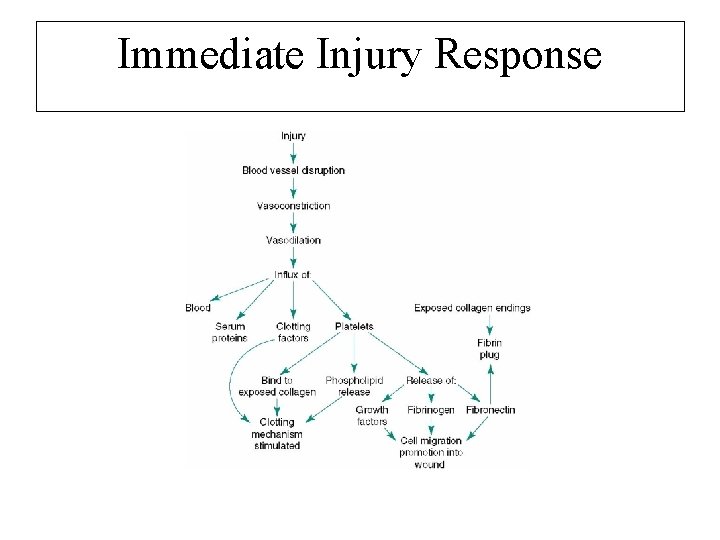
Immediate Injury Response

Proliferation Phase ________ Angiogenesis and granulation tissue formation Increased fibroblasts by day 3 -5 following injury; reduced PMNs ________________________

Signs of Proliferation Redness Swelling Pain Local temperature

Remodeling Phase _______ Myofibroblasts cause wound contraction to minimize scar _____________________________ Tensile strength increases

Signs of Remodeling Reduced redness Reduced edema Reduced pain No local temperature

Growth Factors Proteins Specific growth factors impact specific cells Named for target cells, source, behavior Perform important roles in healing process

Roles of Growth Factors in Healing - p. 42 -43 Control migration and proliferation of cells Affect fibrin-plug formation Control phagocytization Assist capillary endothelial production Stimulate type III collagen removal, type I formation

Ligament Healing ________________ Monocytes and macrophages infiltrate. Fibroblasts appear, increase, produce extracellular matrix. Cellular and matrix structures replace the blood clot. Macrophages, fibroblasts diminish; type I collagen replaces type III. ______________

Tendon Healing Wound gap filled by phagocytes Collagen synthesis Revascularization; synovial sheath rebuilt Fibroblasts revert to tenocytes; type III collagen replaced with type I ______________

Tensile strength -maximal amount of stress or force that a structure is able to withstand before tissue failure occurs—in this case, the amount of outside force that can be applied to a muscle, tendon, ligament, or bone before it tears or breaks
Muscle Healing Fragmentation of muscle fibers; macrophages appear _______________________________ Day 7: scar tissue; near-normal muscle tension can be produced Day 7 -11: near-normal tensile strength Regenerating myotubes; crossstriated muscle fibers _____________________________
Articular Cartilage Healing Fibrin clot is formed Fibroblasts combine with collagen fibers to replace clot 1 month- fibroblasts separate; condrocytes appear 2 months—defect resembles cartilage, but collagen is type I 6 months—type I and II calcified cartilage with normal appearance
Bone Healing ______________ Hematoma forms; fractured edges become necrotic Osteoclasts/Osteoblast proliferate; soft turns hard callus develops External blood supply dominates; then inner bone circulation reestablished ____________________________

Tensile strength -maximal amount of stress or force that a structure is able to withstand before tissue failure occurs—in this case, the amount of outside force that can be applied to a muscle, tendon, ligament, or bone before it tears or breaks

Tensile Strength During Healing Phases Inflammation _______________________________ Proliferation Increase in tensile strength Source of tensile strength: collagen, granulation tissue (continued)

Tensile Strength During Healing Phases Remodeling ______________ Ligament and tendon near normal in 17 -50 weeks ______________

Healing and Tensile Strength For a therapeutic exercise program to be successful, one must have respect for the healing process and a knowledge of tensile strength factors.

Factors That Affect Healing Modalities Medications/Drugs Other modifying factors (age, disease, etc. )

Treatment Modalities Ice Electrical stimulation Superficial heat Deep heat

Influence of Modalities on Healing Relieve pain, spasm, edema Enhance protein synthesis Retard atrophy, facilitate muscle activity Improve circulation Enhance collagen and neovascular production Promote fibroblast production

Factors in Medication Effectiveness – p. 55 half-life: definition and examples steady state of a drug: definition and examples

Effects of NSAIDs on Healing Inhibit prostaglandin production Increase blood clotting time Decrease the effectiveness of other drugs Absorption rate decreased when NSAIDs used with antacids

Drugs That Can Delay Healing Antibiotics Nicotine Corticosteroids

Other Modifying Factors That Can Affect Healing Surgical technique Age Disease Wound size Infection Nutrition Muscle spasm Edema

Role of Therapeutic Exercise in Inflammation Phase Control edema and pain ______________________________

Role of Therapeutic Exercise in Proliferation Phase Tissue is weak but improving in strength with collagen production. Patient can start range-of-motion and limited strengthening activities. Exception is in tendon repairs.

Role of Therapeutic Exercise in Remodeling Phase _____________________________ Stress application must coincide with increase in tensile strength.

Considerations for Appropriate Course Usual healing sequence and timing Individual’s unique response to the injury and treatment

Signs of an Overly Aggressive Program Increased pain, especially postexercise Increased edema, especially if lasts more than 1 day postexercise Diminished function from the previous day’s treatment
- Slides: 35