10222021 ANESTHESIA FOR ORGAN TRANSPLANTATION Dr Abdollahi 1

10/22/2021 ANESTHESIA FOR ORGAN TRANSPLANTATION Dr Abdollahi 1

10/22/2021 Solid organ transplantation has become a well-accepted treatment modality for patients with end-stage organ disease. The role of the anesthesiologist in organ transplantation may involve caring for organ donors, prospective recipients, or patients who have already received transplants but require further surgery. 2

10/22/2021 Organs that are most frequently transplanted are the kidneys and the liver. An extensive preoperative workup with an emphasis on the cardiopulmonary system and conditions related to the failing organ is required for all potential transplant candidates. 3

Organ transplantation unavoidably exposes the anesthesiologist to issues related to biomedical ethics, the diagnosis of death, and transplantation immunology. 10/22/2021 UNIQUE CONSIDERATIONS FOR ORGANTRANSPLANTATION 4

10/22/2021 Criteria for the Diagnosis of Brain Death 5
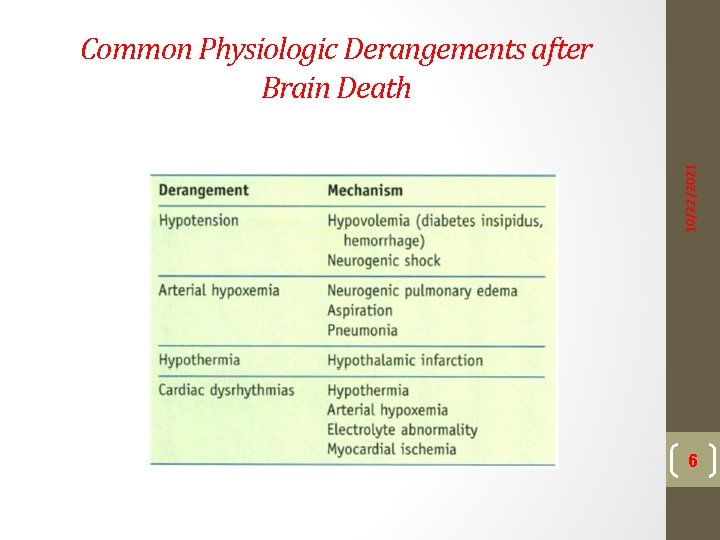
10/22/2021 Common Physiologic Derangements after Brain Death 6

10/22/2021 Death is always certified before the donor procedure. Anestheric care for organ procurement requires a focus on maintenance of donor organ perfusion and oxygenation and recognition of common physiologic derangements associated with brain death. Organ preservarion after removal from the donor includes hypothermia to decrease metabolism with preservative solutions of specific additives to maintain cellular integrity and decrease hypothermia-mediated injury. 7

10/22/2021 Refinement of peri operative care plus improved management of patients after transplantation has resulted in a dramatic improvement in both 1 - and 5 -year graft survival. Postoperative organ function after transplantation depends on multiple factors, including donor demographics, organ ischemia time, mechanism of death of the donor, and medical condition of the recipient. Improvement in immunosuppressive regimens and better tissue typing have contributed to the increasing success of organ transplantation. 8

10/22/2021 Infection (bacterial, fungal, viral) attributable to chronic immunosuppression is the most common cause of death in transplant recipients, thus emphasizing the importance of strict asepsis during the management of anesthesia. The frequency of cancer (especially skin and Iymphoproliferative) is increased in transplant patients, perhaps reflecting loss of the protective effects of an active immune system. 9

Absolute and relative contraindications to solid organ transplantation have diminished over recent years. For instance, candidates for kidney transplantation are increasingly older and have more complex medical problems. Evidence of malignancy is not a contraindication per se. 10/22/2021 CONTRAINDICATIONSTO SOLID ORGAN TRANSPLANTATION 10
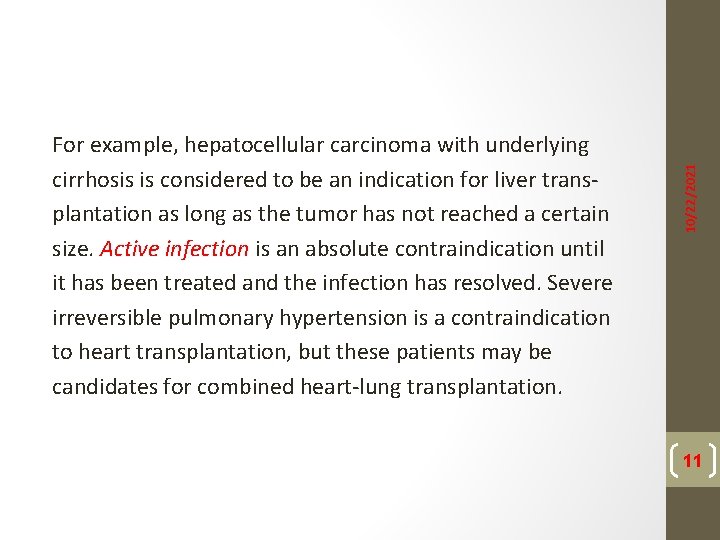
10/22/2021 For example, hepatocellular carcinoma with underlying cirrhosis is considered to be an indication for liver transplantation as long as the tumor has not reached a certain size. Active infection is an absolute contraindication until it has been treated and the infection has resolved. Severe irreversible pulmonary hypertension is a contraindication to heart transplantation, but these patients may be candidates for combined heart-lung transplantation. 11

Approximately 16, 500 kidney transplants are performed in the United States annually. 10/22/2021 KIDNEY TRANSPLANTATION 12

10/22/2021 Major Indications for Kidney Transplantation 13

10/22/2021 The graft survival rate of kidney transplants from deceased donors is approximately 65% at 5 years, whereas it is 80% in recipients who receive a kidney from a living donor. Although transplants involving deceased donor organs are often scheduled as urgent or emergency operations, prolonged cold preservation of the donor kidney is generally well tolerated and provides enough time for transplant candidates to be well prepared for surgery. This time allows for normalization of electrolyte imbalance, volume status, and if necessary, renal dialysis before surgery. 14

10/22/2021 Donor kidneys, whether from a living or a deceased donor, are usually implanted in the iliac fossa. Either side of the abdomen can be used. Although vascular anastomoses can be performed to a variety of recipient vessels, the external iliac artery and vein are most frequently used. The ureter is anastomosed directly to the bladder. 15
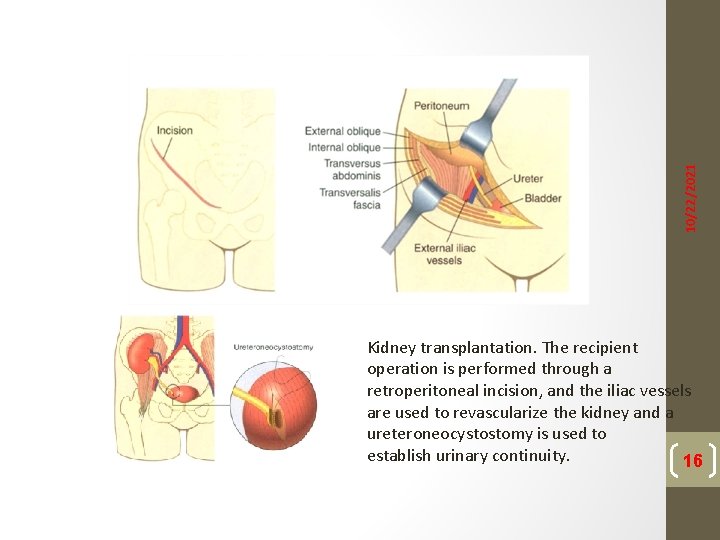
10/22/2021 Kidney transplantation. The recipient operation is performed through a retroperitoneal incision, and the iliac vessels are used to revascularize the kidney and a ureteroneocystostomy is used to establish urinary continuity. 16

The majority of patients with end-stage renal disease have significant comorbid conditions that may influence the anesthetic approach that is chosen for these patients. Management of anesthesia for renal transplantation follows the same principles as described for patients with chronic renal failure, including possible renal dialysis before surgery to optimize fluid, electrolyte, and acid-base status. 10/22/2021 Management of Anesthesia 17

10/22/2021 Physiologic Disturbances Often Present before Renal Transplantation 18

10/22/2021 A variety of anesthetic techniques (most often general anesthesia) have been used successfully for renal transplantation. Selection of monitors may be influenced by the patient's comorbid conditions. For example, patients with longstanding diabetes mellitus may require more extensive monitoring (continuous arterial or central venous pressure [CVP] monitoring, or both) than a young patient with glomerulonephritis and well-controlled systemic hypertension. when CVP monitoring is used, the goal is to maintain CVP in the 10 - to IS-mm Hg range to optimize fluid status and renal perfusion. 19

10/22/2021 Surgical stimulation after dissection of the fascia for placement of the donor kidney is minimal, and systemic hypotension may ensue as a result of the effects of anesthetic drugs. Effort should be made to avoid episodes of hypotension after reperfusion because renal graft function is critically dependent on perfusion pressure. Excessive opioid administration coupled with minimal surgical stimulation may contribute to hypotension. 20

10/22/2021 Intravenous administration of a-adrenergic drugs such as phenylephrine may be avoided in as much as animal models have demonstrated that vessels in the transplanted kidney are sensitive to sympathomimetics, which can compromise blood flow to the transplanted organ. Of note, convincing scientific data in humans are not available. 21

10/22/2021 Mannitol, loop diuretics, and dopamine may be used intraoperatively to improve renal perfusion pressure and enhance urine production. Lowdose mannitol (12. 5 to 25 g IV) and loop diuretics are usually administered before unclamping the vascular supply to the transplanted kidney. The role of dopamine in kidney transplantation remains controversial. 22
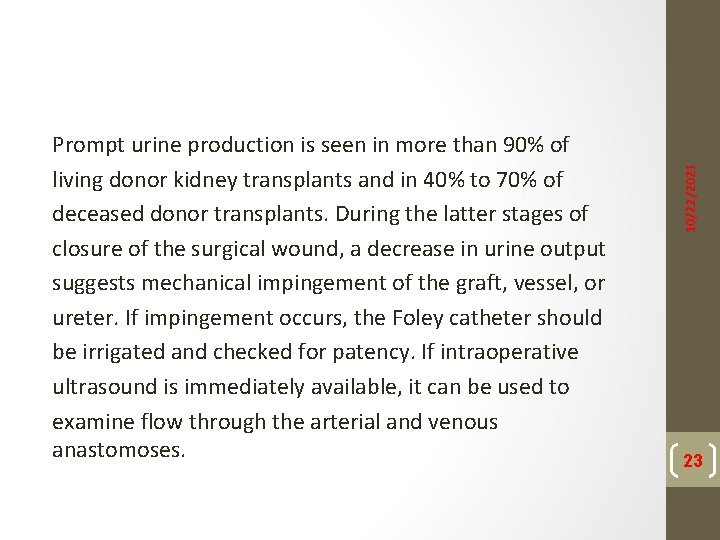
10/22/2021 Prompt urine production is seen in more than 90% of living donor kidney transplants and in 40% to 70% of deceased donor transplants. During the latter stages of closure of the surgical wound, a decrease in urine output suggests mechanical impingement of the graft, vessel, or ureter. If impingement occurs, the Foley catheter should be irrigated and checked for patency. If intraoperative ultrasound is immediately available, it can be used to examine flow through the arterial and venous anastomoses. 23

10/22/2021 Moderate to severe systemic hypertension can accompany emergence from anesthesia after renal transplantation. Antihypertensive therapy may be initiated in the operating room and continued during the recovery period. Postoperative pain is generally mild to moderate and can be well controlled with intravenous opioids. Epidural catheters are not usually placed in this patient population. 24
Approximately 6400 liver transplantations are performed in the United States annually, including a small number with living liver donors. The 3 -year survival rate after transplantation in the United States is greater than 75%. 10/22/2021 Liver transplantation 25

10/22/2021 The most common causes of end-stage liver disease requiring liver transplantation are chronic viral hepatitis C or B and alcoholic and cholestatic cirrhosis (primary sclerosing cholangitis). 26

10/22/2021 Patients are categorized by either the Child- Pugh classification or the Model for End-stage Liver Disease (MELD). The MELD risk score is a mathematical formula that uses creatinine, bilirubin, and INR (international normalized ratio for prothrombin time). 27

10/22/2021 Candidates for liver transplantation have various symptoms ranging from chronic fatigue with mild jaundice to coma with multiple organ failure. The severity of hepatic dysfunction and the urgent nature of the operation often limit the time available to optimize preoperative disturbances before proceeding with liver transplantation surgery. 28
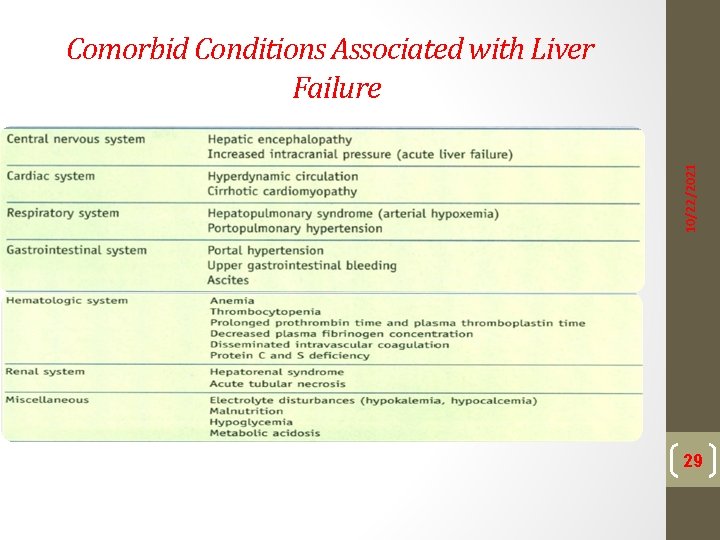
10/22/2021 Comorbid Conditions Associated with Liver Failure 29
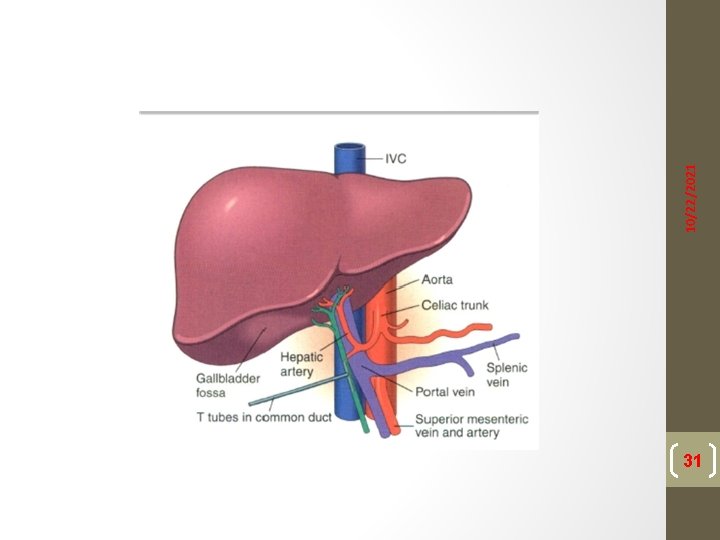
Liver transplant surgery can be divided into three phases. The dissection phase includes lysis of adhesions and mobilization of the liver. The anhepatic phase consists of removal of the native liver and implantation of the donor liver. The reperfusion or neohepatic phase involves surgical completion of the remaining anastomoses, hemostasis, and closure. 10/22/2021 Phases of Liver Transplantation 30
31 10/22/2021

Management of anesthesia during liver transplantation includes invasive monitoring of arterial blood pressure and CVP. The decision to place a pulmonary artery catheter or transesophageal echocardiography (TEE) probe varies between institutions and often depends on the medical condition of the patient. Large-bore intravenous access is mandatory because of the significant blood loss that may be encountered during surgery. 10/22/2021 Management of Anesthesia 32

10/22/2021 Before induction of anesthesia it is important to consider the impact of ascites and its effect on gastric emptying and pulmonary function. Several different anesthetic drugs can be used for induction and maintenance of anesthesia. Although a significant number of anesthetic drugs rely on hepatic metabolism and excretion, titration of their use is generally safe because of the subsequent implantation of a functioning liver. Nitrous oxide, however, is generally avoided. 33

During the dissection phase, cardiovascular instability from hemorrhage, venous pooling as a result of sudden decreases in intra-abdominal pressure, and impaired venous return secondary to surgical retraction may occur. Hypocalcemia, hyperkalemia, and metabolic acidosis may also be encountered. 10/22/2021 DISSECTION PHASE 34

The anhepatic phase begins when the native liver is removed after transection and clamping of the suprahepatic and infrahepatic portions of the inferior vena cava and portal vein. The hepatic artery is usually ligated before the anhepatic phase. A venous bypass system is used in some cases to minimize decreases in preload and cardiac output and to prevent splanchnic congestion. 10/22/2021 ANHEPATIC PHASE 35

10/22/2021 Cardiac output and systemic blood pressure may need to be supported with inotropes and vasoconstrictors during this phase. Citrate intoxication from rapid blood transfusion is more likely during the anhepatic phase because of the complete absence of any liver metabolic function. Calcium may need to be administered rapidly to prevent hypocalcemia. 36

The reperfusion phase begins with release of the clamps on the major vascular structures. The sequence of reperfusion depends on surgical preference. Severe hemodynamic instability may occur during unclamping of the portal vein (reperfusion syndrome); this effect appears to be multifactorial in origin and may require pharmacologic intervention with potent vasopressors such as epinephrine or norepinephrine, or both. 10/22/2021 REPERFUSION PHASE 37

10/22/2021 Once the allograft begins to function, hemodynamic and metabolic stability is gradually restored, and the need for inotropic support decreases. Indirect signs of a functioning graft include intraoperative bile production, correction of the negative base excess, and improvement in coagulation. 38

Continued intubation of the patient's trachea may not be required in the postoperative period, especially in patients with active protective airway reflexes and no preexisting respiratory compromise. Blood loss per se should not be considered an indication for postoperative intubation. Most often patients are admitted directly to the intensive care unit for monitoring. Ultrasound is warranted if there is any doubt about hepatic artery or portal vein patency. Thrombosis of the hepatic artery usually requires retransplantation. 10/22/2021 Postoperative Care 39

Approximately 1000 to 1200 lung transplants are performed annually in the United States, whereas fewer than 40 heart-lung transplants are performed annually. s Lung transplantation for adults generally refers to (1) single-lung transplantation (SLT), (2) bilateral sequential lung transplantation (BSLT), and (3) heartlung transplantation (HLT). Patients with primary lung pathology typically undergo SLT or BSLT. 10/22/2021 LUNG TRANSPLANTATION 40

10/22/2021 Most Frequent Indications for Lung Transplantation 41

10/22/2021 When significant left ventricular dysfunction is present as a result of underlying coronary artery disease or dilated cardiomyopathy, patients may instead undergo HLT 42

The derangement in pulmonary mechanics assumes central importance in the intraoperative management of patients with end-stage lung disease. Lung transplant patients have varying degrees of impaired gas exchange, altered pulmonary mechanics, and impaired right ventricular function that are largely determined by the underlying cause of the pulmonary failure. 10/22/2021 Management of Anesthesia 43

10/22/2021 Lung transplantation begins with a pneumonectomy performed through either a standard posterolateral thoracotomy incision or a bilateral thoracosternotomy incision. With the assistance of one-lung ventilation, the lung is dissected and the hilar structures are identified, clamped, and divided. After the native lung is removed, the lung graft is placed in the patient's hemithorax, and anastomosis of the hilar structures is performed (bronchial and arterial anastomoses). 44

10/22/2021 Cardiopulmonary bypass (CBP) may or may not be used, depending on the exact surgical procedure performed and the patient's medical condition. In select cases (severe pulmonary hypertension), cannulation of the femoral vessels may be indicated before induction of anesthesia in preparation for emergency institution of CPB. 45

10/22/2021 If postoperative neuraxial analgesia is planned, the best time for injection of subarachnoid opioids or placement of an epidural catheter is before induction of anesthesia, although some have preferred to postpone this until the postoperative period. In addition to standard monitors and intravenous access, appropriate adjuncts include arterial, central, and pulmonary arterial pressure monitoring. 46

The decision whether to place invasive monitors before or immediately after induction of anesthesia is made after considering the individual patient's degree of cardiovascular impairment or instability. TEE assists in the intraoperative assessment of right ventricular function, pulmonary hypertension, intracardiac air, and unexplained hypotension. 10/22/2021 Monitoring 47

The anesthetic induction technique should preserve ventricular contractility and avoid elevation of pulmonary vascular resistance. Consideration should be given to temporary placement of a single-lumen endotracheal tube to facilitate fiberoptic bronchoscopic assessment of the tracheobronchial tree and allow thorough suctioning, especially in patients with cystic fibrosis. Ultimately, however, provision will need to be made for single lung ventilation. 10/22/2021 INDUCTION OF ANESTHESIA 48

Volatile anesthetics are generally well tolerated, especially when combined with intravenous drugs to lower dose requirements for the inhaled drugs. Nitrous oxide is not recommended because of its potential to increase pulmonary vascular resistance, aggravate intravascular air by expansion, and substantially limit FI 02 when administered at clinically relevant doses. 10/22/2021 MAINTENANCE OF ANESTHESIA 49

10/22/2021 After implantation of the graft or grafts, ventilation is reestablished to both lungs. FI 02 is titrated to maintain acceptable systemic oxygen saturation while keeping in mind the concern for pulmonary toxicity with sustained administration of high concentrations of oxygen. The use of positive end-expiratory pressure (5 cm H 20) and inhaled nitric oxide may facilitate this goal. Bronchoscopy is useful for the evaluation of anastomosis integrity, whereas TEE may reveal pulmonary venous obstruction. 50

10/22/2021 Before leaving the operating room, the double-lumen tube is removed from the patient's trachea and replaced with a single-lumen tube. The single-lumen tube is necessary to facilitate bronchoscopic inspection of the anastomoses, allow tracheobronchial suctioning, and assist in postoperative ventilatory care. 51

10/22/2021 Mechanical ventilation is typically provided for 1 or more days in the absence of complications. It may be prolonged in the presence of early graft dysfunction, acute rejection episodes, bronchial anastomosis stricture or failure, pneumonia, and complications related to bleeding. 52

Between 2000 and 2200 heart transplantation procedures are performed each year in the United States. Significant number of patients who undergo heart transplantation have end-stage cardiac failure as a result of ischemic or idiopathic dilated cardiomyopathy. Most of the remainder suffer from congenital defects, valvular heart disease, or increasingly, dysfunction of a previously placed cardiac graft (retransplantation). 10/22/2021 HEART TRANSPLANTATION 53

10/22/2021 In a small minority of patients without heart failure per se, a heart transplant is indicated to treat uncontrolled ventricular dysrhythmias, idiopathic hypertrophic cardiomyopathy, intracardiac tumors, or life-threatening myocardial ischemia that is not amenable to revascularization. 54

10/22/2021 Significant comorbid conditions (renal and hepatic dysfunction) are common sequelae of severe cardiac disease. Transplantation is generally considered appropriate in patients with mild organ system dysfunction that is deemed likely to normalize with the improved cardiac output after transplantation. Many patients awaiting transplantation are stabilized with intravenous inotropes, intra-aortic balloon pumps, ventricular assist devices, or mechanical ventilation (or any combination of these measures). 55

10/22/2021 Preoperative measurement of pulmonary vascular resistance is of major importance because engraftment of a normal donor heart into a patient with high, fixed pulmonary vascular resistance may cause acute right ventricular failure. In these patients, pulmonary vascular resistance may be normalized by treating with intravenous or inhaled pulmonary vasodilators. Those who show significant improvement with this treatment may safely undergo cardiac transplantation. 56

During the operation the patient is placed on CPB, and the operative technique consists of anastomosis of the aorta, pulmonary artery, and left and right atria. Anesthetic induction should be conducted by following principles similar to those for any patient with end-stage cardiac failure. Standard anesthetic monitoring is supplemented by invasive hemodynamic monitoring, including peripheral arterial, central venous TEE, and pulmonary artery pressure lines (RV assist device support may preclude pulmonary artery catheterization until weaning from CPB). 10/22/2021 Management of Anesthesia 57

10/22/2021 It will be necessary to withdraw a central venous catheter or pulmonary artery catheter back into the internal jugular vein when the recipient's heart is removed. The catheter can then be repositioned when the donor heart is in place. 58

10/22/2021 Vasopressors or inotropes may be instituted in the operating room before induction of anesthesia. For patients who are at the limit of their hemodynamic compensatory mechanisms, subsequent institution of extracorporeal membrane oxygenation or CPB support may be necessary. 59

10/22/2021 Anesthetic induction drugs that do not cause significant myocardial depression are a consideration. Many variations of anesthetic technique have been used with success. Balanced anesthesia with continuous infusion or intermittent bolus administration of opioids, benzodiazepines, and neuromuscular blocking drugs is typical and may be supplemented with low doses of volatile anesthetics. 60

Once all anastomoses are completed, anesthetic goals include the provision of optimal conditions for separation from CPB and the anticipation of probable hemodynamic derangements. In patients with bradycardia or atrioventricular conduction heart block, an adequate heart rate and cardiac rhythm may be achieved by the intravenous infusion of a chronotropic drug (isoproterenol or dobutamine) or the use of a temporary artificial cardiac pacemaker. 10/22/2021 Separation from Cardiopulmonary Bypass 61

10/22/2021 An appropriate target heart rate for weaning from CPB is in the range of 90 to 110 beats/min. Because of the absence of autonomic nervous system innervation to the transplanted heart, only direct-acting sympathomimetics such as catecholamines or phosphodiesterase inhibitors are effective for inotropic or chronotropic effect. Drugs that increase the heart rate with a vagolytic effect (atropine) are ineffective. 62

10/22/2021 Separation from CPB may also be complicated by myocardial dysfunction, which is often attributable to incomplete or prolonged cardiac preservation (cold ischemia time) or circumstances of the critical illness of the donor. Although left ventricular function is generally adequate, right ventricular function is also important after heart transplantation for adequate cardiac output, hemodynamic stability, and end-organ perfusion. 63

10/22/2021 The persistence of significant pulmonary hypertension or right ventricular failure despite pharmacologic interventions may warrant the administration of other drugs with pulmonary vasodilating properties. 64

10/22/2021 Nonpharmacologic measures to minimize pulmonary vascular resistance include the avoidance of hypercapnia, delivery of high FIo 2 concentrations, and maintenance of normothermia. Refractory right ventricular failure may be treated with a right ventricular assist device in an attempt to restore acceptable hemodynamics and systemic perfusion during the postoperative period. Cardiac dysrhythmias, hypovolemia, left ventricular dysfunction, and even anastomotic obstruction can contribute to hemodynamic compromise during reperfusion. 65

Tracheal extubation most often occurs in an intensive care unit setting in the absence of significant hemodynamic instability or other complications. Although normal or near-normal biventricular function is expected in most cases, right ventricular dysfunction may develop postoperatively and persist because of increased pulmonary vascular resistance. 10/22/2021 Postoperative Management 66
- Slides: 66