1 Prtesis Hbrida Maxilar Superior Generalidades Anatoma Estticafontica

1 Prótesis Híbrida Maxilar Superior • Generalidades • Anatomía • Estética-fonética INICIO CLASE

2 Prótesis Híbrida Maxilar Superior • Generalidades Prótesis híbrida Es una prótesis fija sobre implantes (implanto retenida y soportada), pero que reproduce tejidos blandos y duros, como una prótesis removible.

3 Prótesis Híbrida Maxilar Superior • Generalidades No requiere que los implantes coincidan con el eje de emergencia estética de las piezas a restaurar, pues la relación con la encía se genera artificialmente.

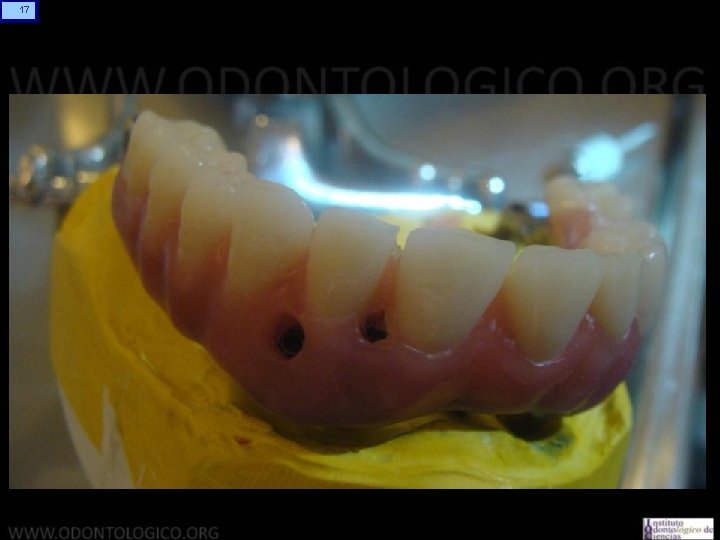
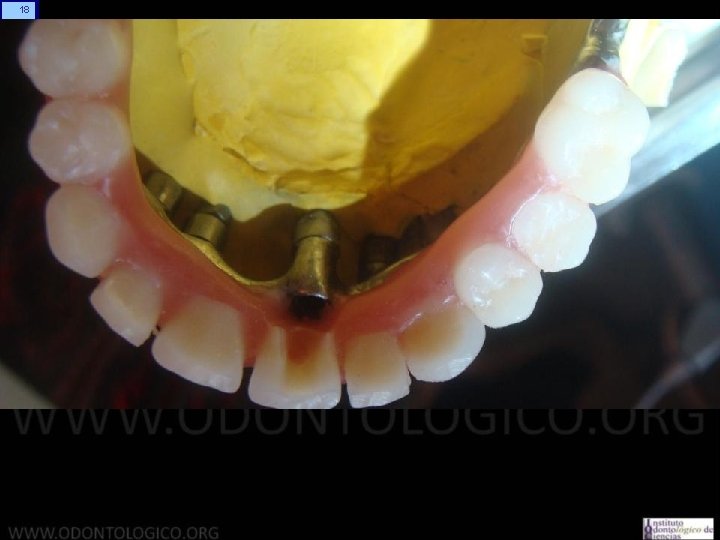
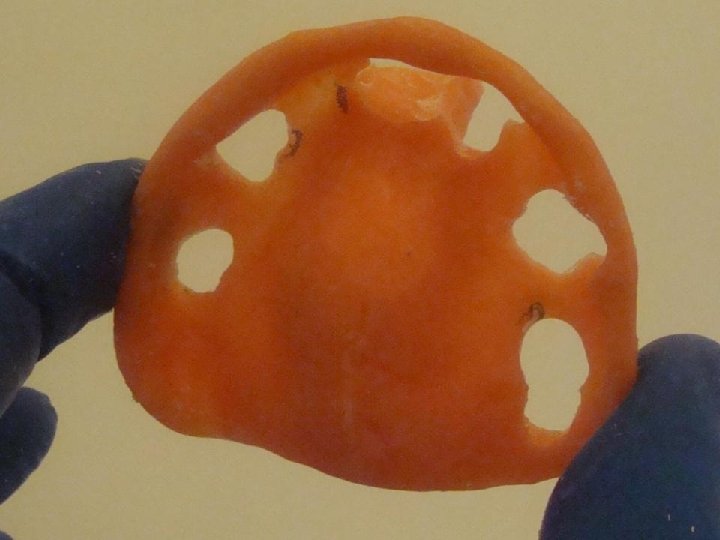
4 Prótesis Híbrida Maxilar Superior • Generalidades Sobre los implantes se confecciona una barra con retenciones para el acrílico y orificios que dan acceso a los tornillos que la fijan a estos implantes

5 Prótesis Híbrida Maxilar Superior • Generalidades Se debe contar con una altura suficiente para dar cabida a estructura metálica, por lo que esta indicada en rebordes con cierto grado de reabsorción. En caso contrario estaría indicada una prótesis fija plural.

6 Prótesis Híbrida Maxilar Superior • Generalidades No tiene flancos, y no debe tener flancos, para permitir acceso a la higiene, pues el paciente no se la puede retirar, como en una sobredentadura.

7 Prótesis Hibrida Maxilar Superior Procedimiento básico por sesiones: 1. Impresión preliminar en alginato para construir cubeta individual, medir altura encía, angulación implantes y seleccionar multiunits. 2. Impresión cubeta abierta ferulizando transfers. 3. Placa de altura, toma de relaciones, toma de color 4. Enfilado en cera, confección y prueba estructura metálica. 5. ¿Nueva toma de relaciones? , Prueba de enfilado sobre estructura metálica 6. Terminación, ajuste oclusal.

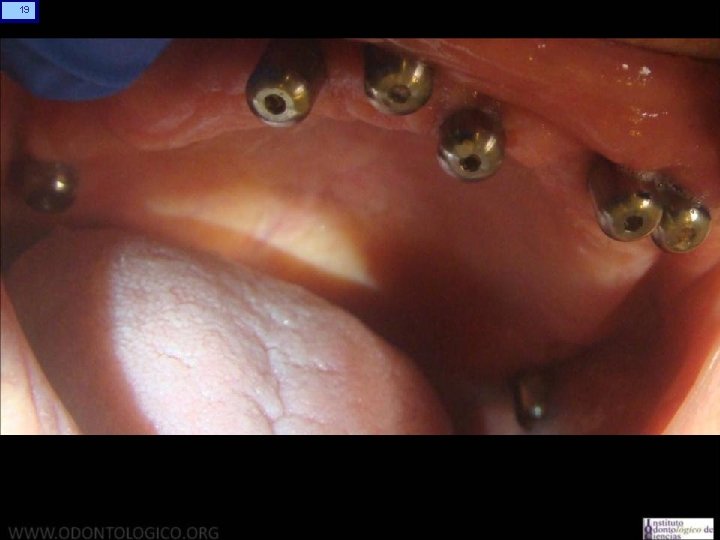
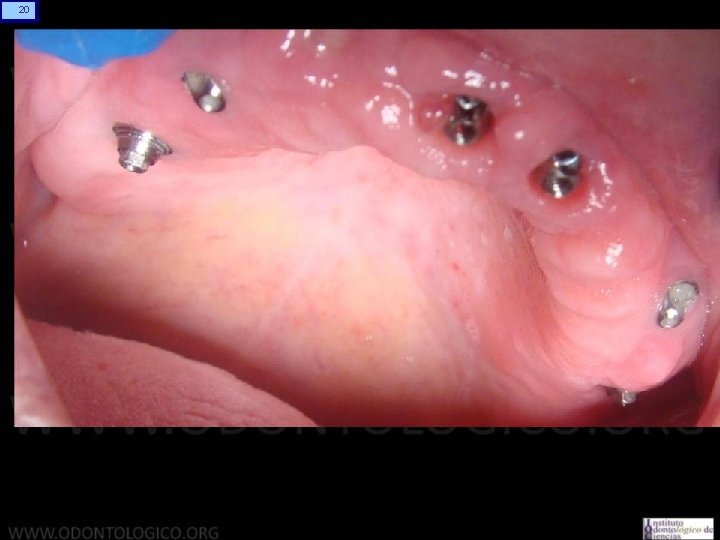
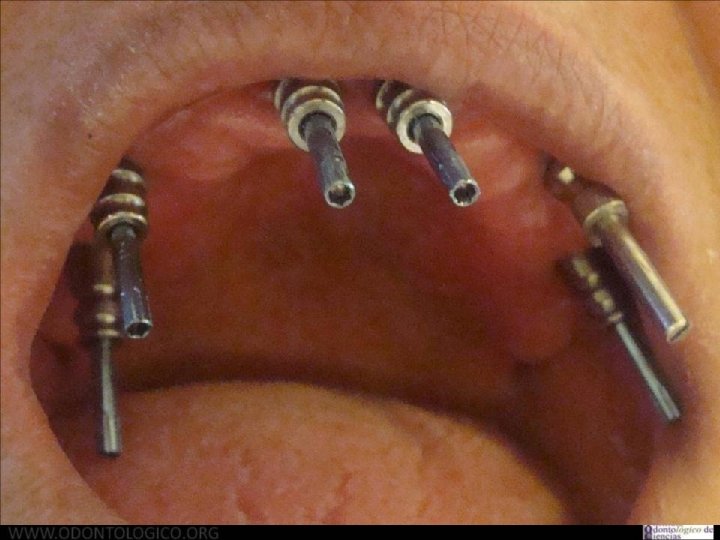
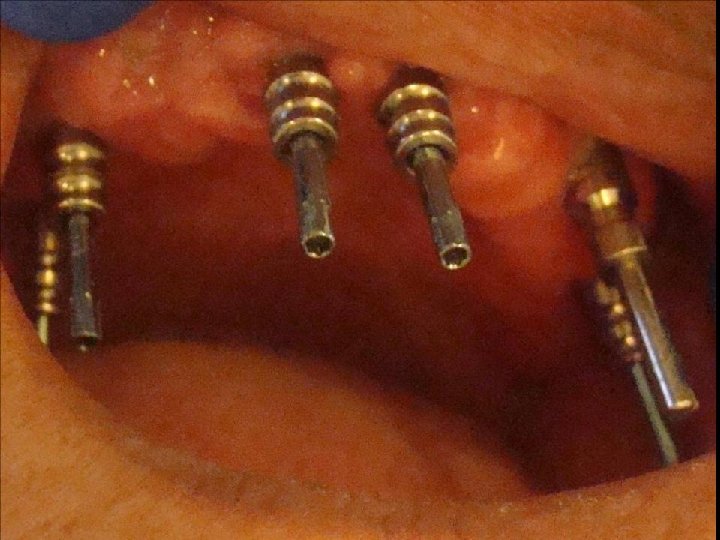
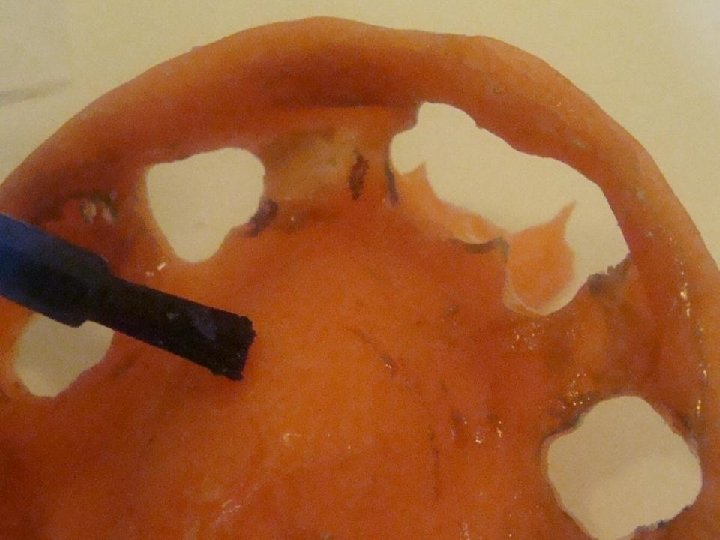
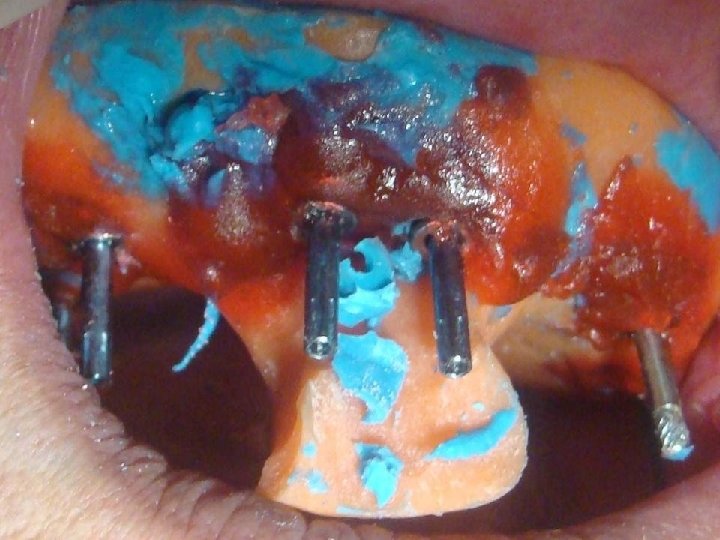
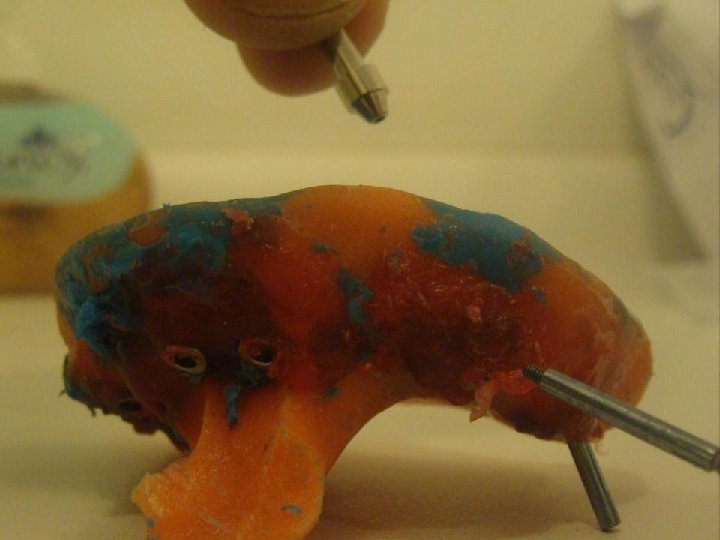
8 Prótesis Hibrida Maxilar Superior • Anatomía: A diferencia del maxilar inferior, acá la reabsorción se genera principalmente a expensas de la tabla vestibular y de forma que usualmente los implantes quedan angulados de vestibular a palatino. Esto provoca que los tornillos tiendan a salir por vestibular. La neumatizacion del seno maxilar obliga a colocar implantes muy distalados y angulados, o bien por mesial del seno angulados hacia distal para evitar perforarlo y disminuir los cantilevers.

9 Prótesis Híbrida Maxilar Superior • Anatomía: Esto determina que los implantes usualmente quedan muy angulad entre sí, mucho mas que en el maxilar inferior, lo que representa u desafía para lograr el eje de inserción pasivo que debe tener la estructura sobre ellos.

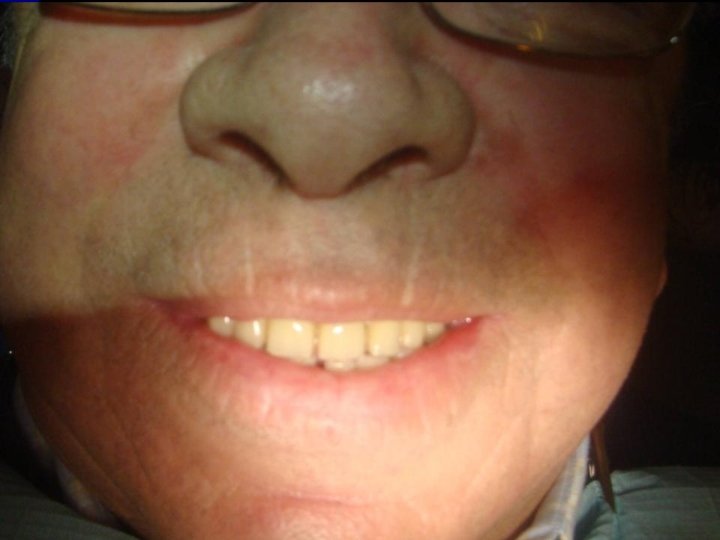
10 Prótesis Híbrida Maxilar Superior • Estética-fonética: A diferencia del maxilar inferior estas prótesis requieren restaurar las piezas más exigentes en términos estéticos (las anterosuperiores), y además cumple un rol importante en el relleno labial. Pero por el hecho de no poder tener flancos se genera a veces disconformidad de los pacientes en ese ámbito. Además a diferencia de las prótesis totales que cubren totalmente el paladar, estas no sellan totalmente el paso del aire por lo que pudieran presentar problemas fonéticos. -

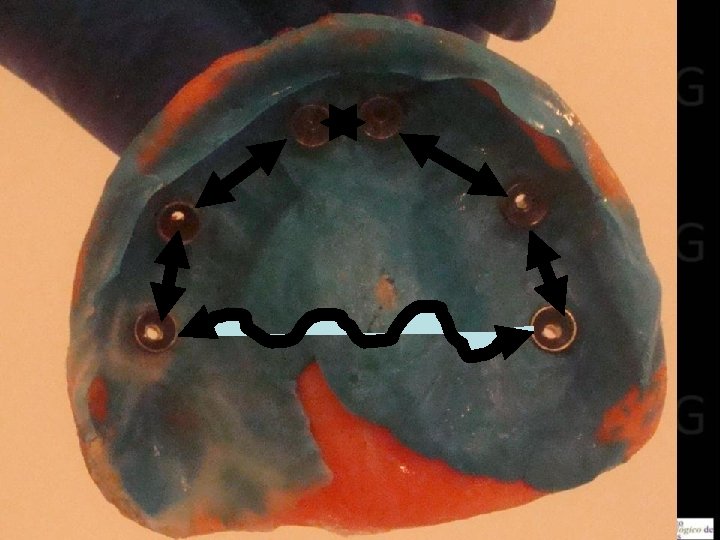
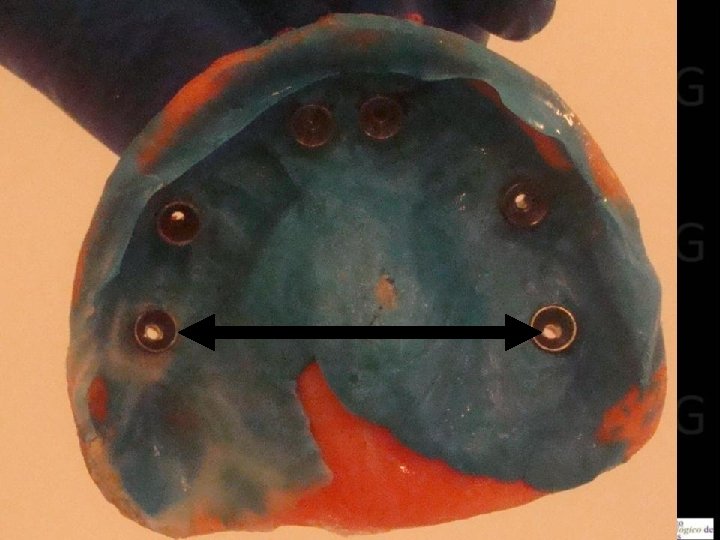
11 Protesis Híbrida Maxilar Superior • Protocolo protésico Impresiones: Al haber mucha angulación entre los implantes, no es aconsejable desde ninguna perspectiva tomar la impresión directamente a las plataformas de los mismos, menos aun si son implantes de conexión interna, pues difícilmente el material de impresión podrá dar la flexibilidad suficiente como par sortear las retenciones generadas por los hexágonos, internos o externos, o bien se puede llegar a fracturar la ferulización. Por otro lado siempre es mejor no trabajar directamente sobre la plataforma del implante, evitando así el restablecimiento del ancho biológico desde ahí.

12 Prótesis Híbrida Maxilar Superior • Protocolo protésico. Impresiones: Por ello se deben instalar primero pilares cónicos tipo multiunnit para dar más tolerancia a las angulaciones, o definitivamente corregirlas utilizando multiunits angulados. Después se hace recomendable ferulizar los transfers no entre sí, si no mas bien a la cubeta individual, pues los implantes distales terminan quedando muy separados en esta herradura, lo que se puede soslayar si se ferulizan a través del paladar usando la cubeta individual, asegurando la precisión de la impresión.

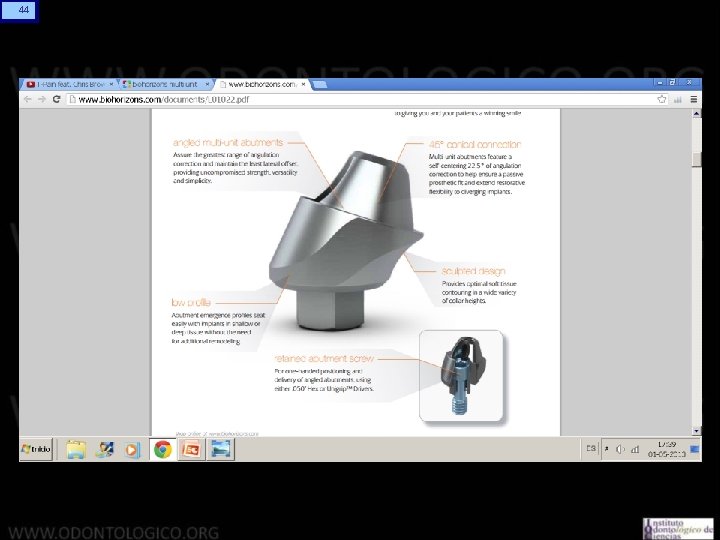
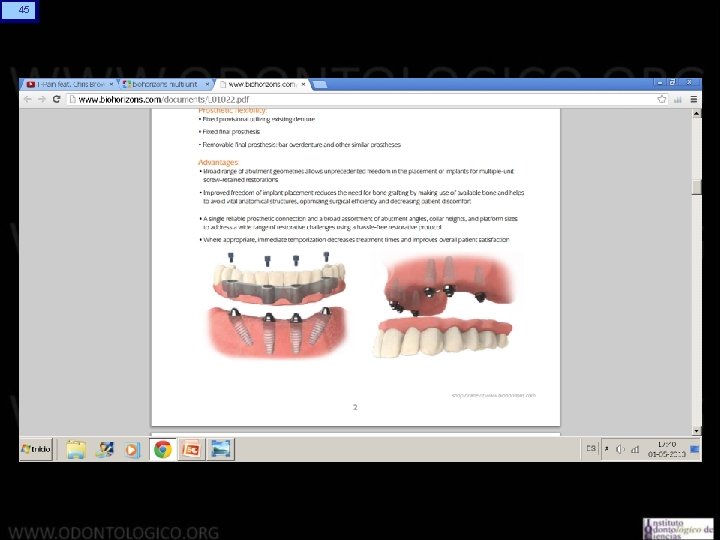
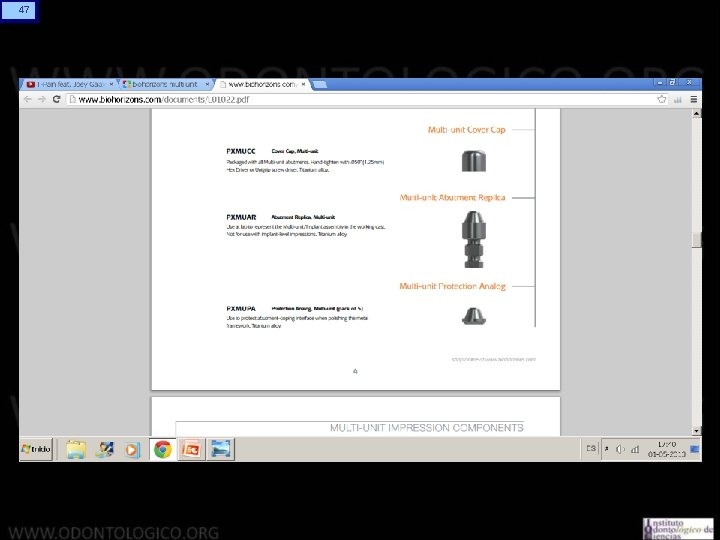
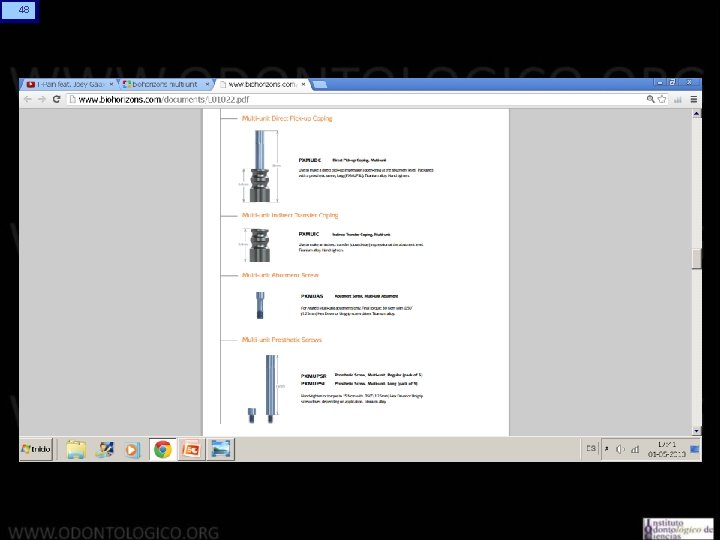
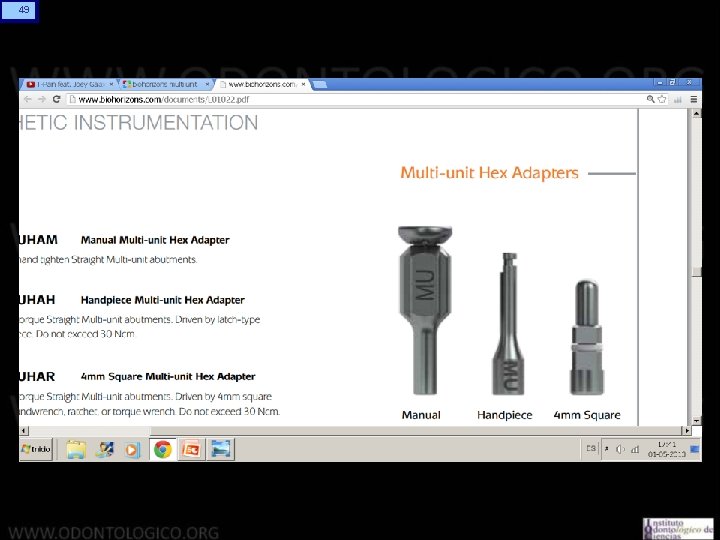
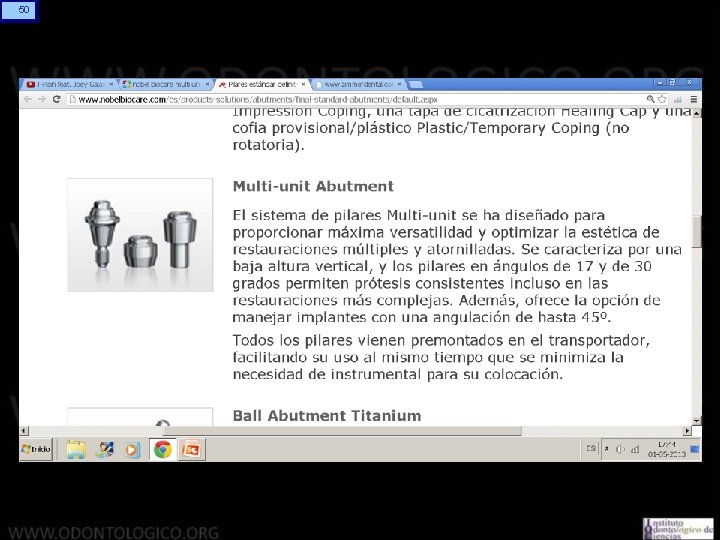
13 Sistema Multiunit • Se ha establecido como el estándar en rehabilitación en prótesis híbridas. • Consiste en un abutment cónico que se atornilla al implante. • La conicidad del abutment permite dar tolerancia al eje de inserción , lo que es particularmente útil en el maxilar superior. • Cuenta con versiones recta y anguladas, hasta en 30°, lo que da aun más posibilidades de paralelizar ejes en implantes muy angulados entre sí. • Transforma diferentes plataformas de implantes en solo una estándar, lo que simplifica la rehabilitación. • Tienen una rosca interna que permite atornillar la estructura protésica, por lo tanto cuando hay que desmontarla no es necesario agredir la plataforma del implante.

14 Sistema Multiunit Indicaciones: • Permite paralelizar eje de inserción de prótesis. • En el maxilar superior permite evitar que tornillo de fijación salga por vestibular. • Aleja superficie de trabajo protésico del implante. • Además simplifica los procedimientos protésicos al transformar distintos tipos de plataformas de implantes en una sola universal.

15 Sistema Multiunit Selección: Plataforma del implante: Un Implante restore 3, 3 o un Tapered Internal Biohorizons de 4, 6 se transforman en multiunits idénticos. Se debe pedir los multiunits que adapten a las diferentes plataformas de los implantes colocados.
16
17
18
19
20
21
22
23
24
25
26
27
28

29
30
31
32
33

34
35
36
37
38
39
40

41
42
43
44
45
46
47
48
49
50
51
52
53
54
55
56
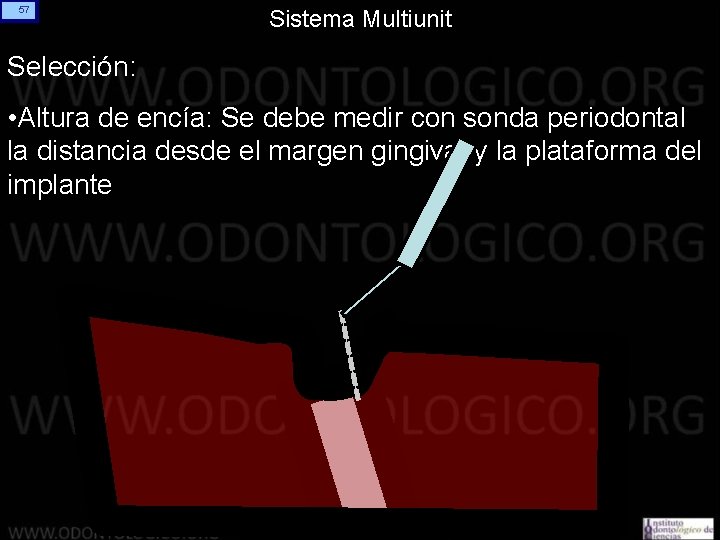
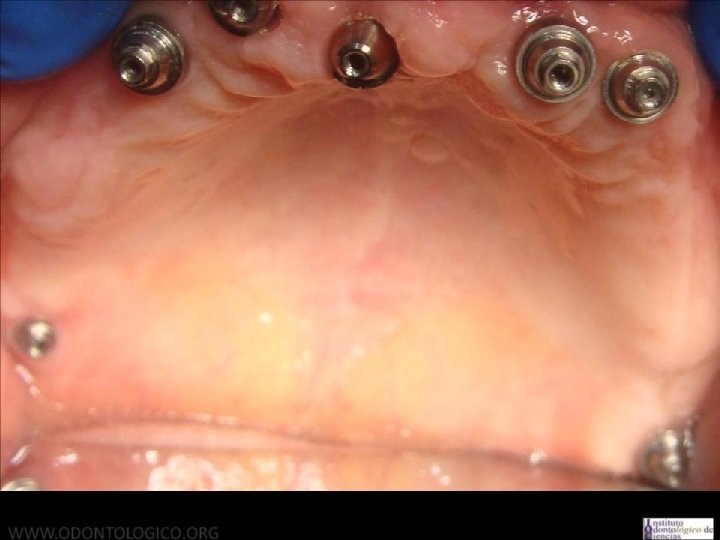
57 Sistema Multiunit Selección: • Altura de encía: Se debe medir con sonda periodontal la distancia desde el margen gingival y la plataforma del implante

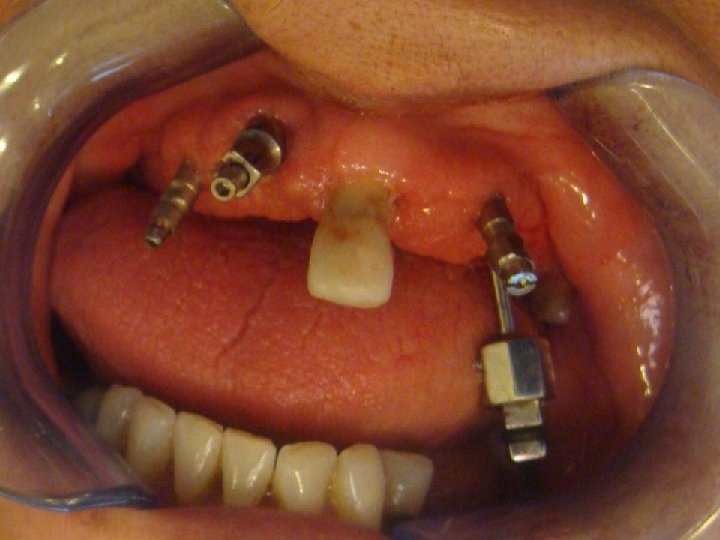
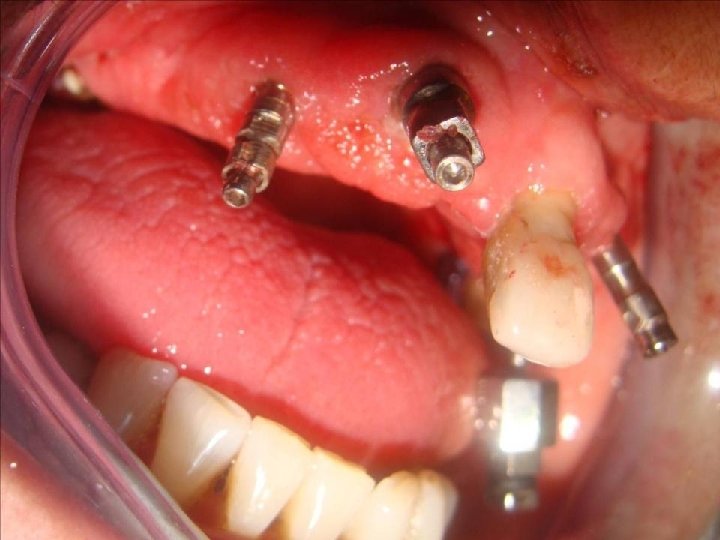
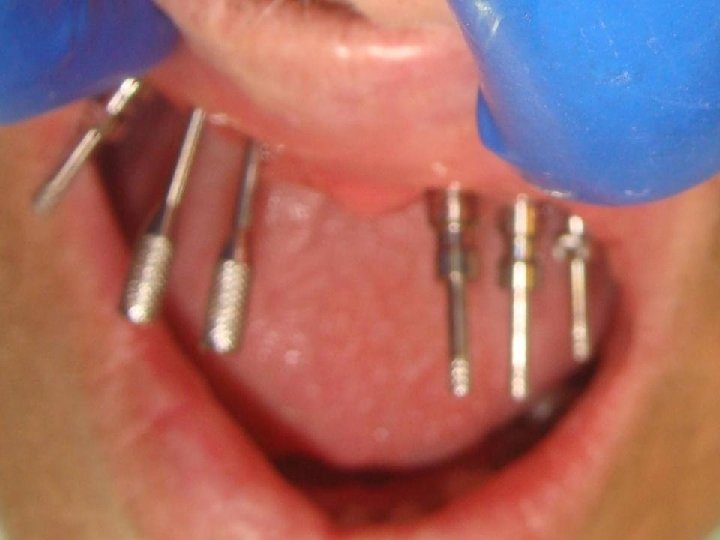
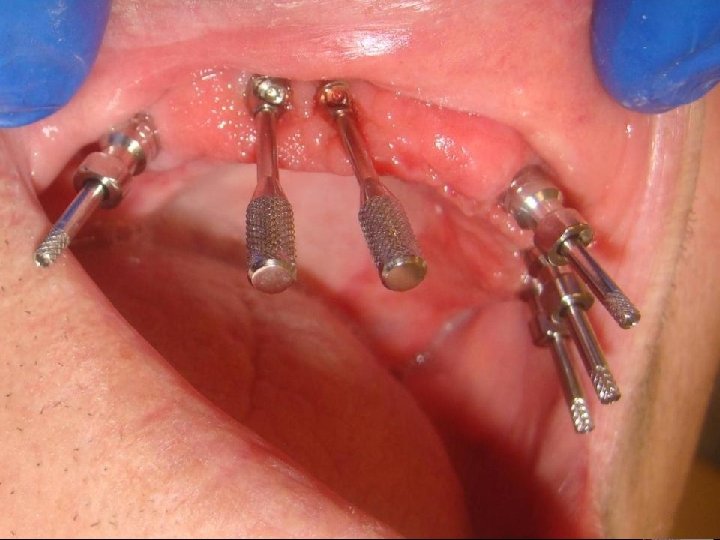
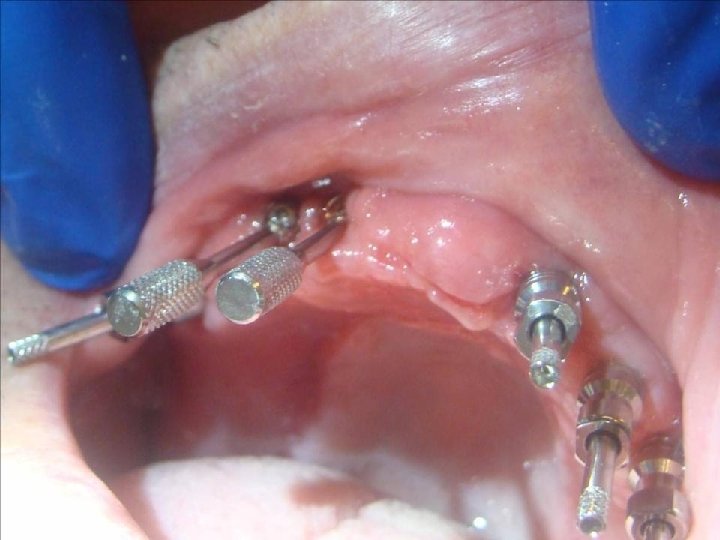
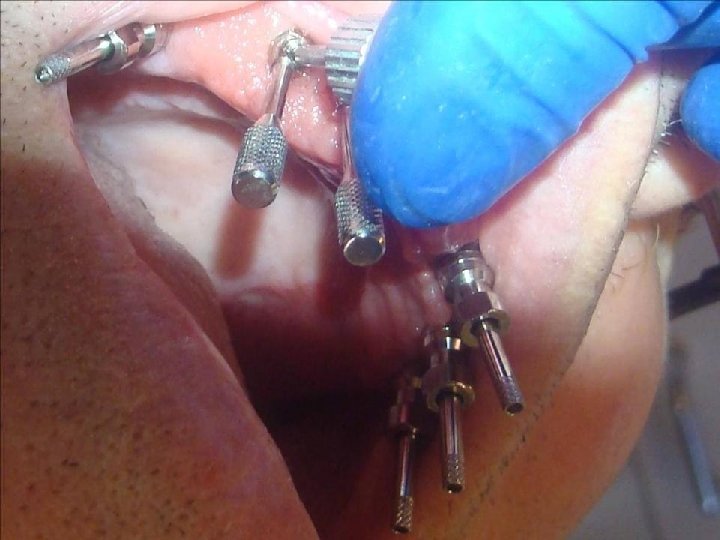
58 Sistema Multiunit Selección: • Angulación: Se pueden atornillar a los implantes transfers o tornillos de transfers para evaluar mejor la angulación entre ellos. Recomiendo contar con un transportador o una guía preformada. Evaluar: Eje e inseción-emergencia del tornilo protésico (o sale por palatino o bien por la encia vestibulo-cervical, pero nunca por la cara vestibular del diente)

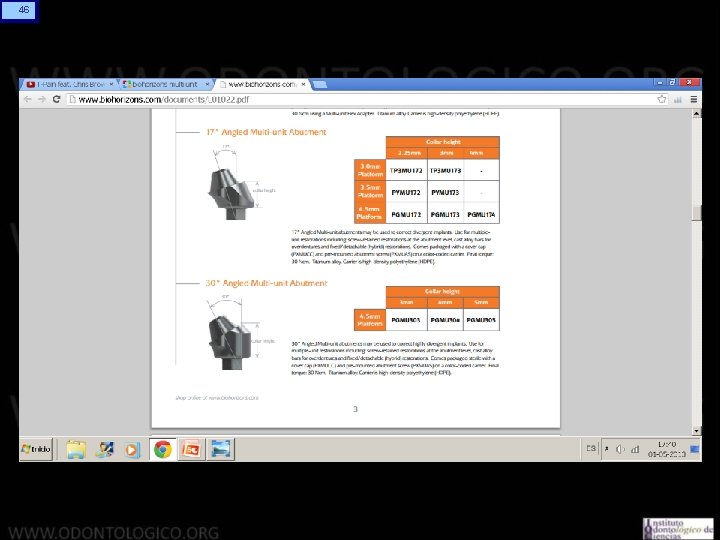
59 Sistema Multiunit Selección: • Angulación: • Multiunit recto: Convergencia de 22, 5 por cara, es decir pueden dar tolerancia hasta 45° de divergencia entre dos implantes. • Multiunit angulado 17°: Suma 17° de tolerancia (entre uno de 17° y uno recto aumenta a 62°, entre dos de 17° aumenta a 79°). • Multiunit angulado 30°: Suma 30° de tolerancia (entre un 30° y uno recto aumenta a 75°, entre dos 30° aumenta a 104°).

60 EVIDENCIA

61 J Oral Maxillofac Surg. 2009 Nov; 67(11 Suppl): 60 -73. doi: 10. 1016/j. joms. 2009. 07. 007. Fixed rehabilitation of the edentulous maxilla: possibilities and clinical outcome. Att W 1, Bernhart J, Strub JR. Abstract PURPOSE: The aim of the present report was to describe the different treatment approaches available for fixed rehabilitation of the edentulous maxilla in the presence of varying hard and soft tissue conditions and to review the clinical outcome of each treatment approach. MATERIALS AND METHODS: A review of the published data published from 1980 through 2009 was conducted using electronic databases and manual searching to identify the treatment possibilities for the fixed rehabilitation of the edentulous maxilla and report their clinical outcomes. The search terms used, in simple or multiple conjunctions, were "fixed rehabilitation, " "implants, " "edentulous, " "fixed dental prosthesis, " "implant-supported, " and "maxilla. " RESULTS: Several treatment modalities were identified for the fixed rehabilitation of the edentulous maxilla, with and without bone augmentation procedures. Regular, tilted, and zygoma implants were identified for treatment modalities that do not require bone augmentation. Sinus floor elevation with the lateral window technique or Le Fort I osteotomy with interpositional bone grafts was identified as a treatment possibility that required bone augmentation procedures. The database initially yielded 230 titles. Of the 230 studies, 42 were finally selected. Although all studies reported the survival rates of the implants, only 20 provided information about the prosthetic outcome. Because of the limited number of studies, at least for the specific treatment modalities, and the heterogeneity in the design of the different studies identified, it was not possible to perform a statistical analysis of the data. Except for regular implants placed in native bone, no sufficient long-term clinical studies were found for the other procedures. CONCLUSIONS: Except for regular implants placed in non augmented native bone, the published data provide insufficient evidence about the outcome of other procedures. Until long-term data are available, such procedures should not be considered reliable treatment modalities.

62 Dent. 2014 Oct; 42(10): 1228 -41. doi: 10. 1016/j. jdent. 2014. 05. 016. Epub 2014 Jun 26. Systematic review of short- (5 -10 years) and long-term (10 years or more) survival and success of full-arch fixed dental hybrid prostheses and supporting implants. Kwon T 1, Bain PA 2, Levin L 3. Author information Abstract OBJECTIVES: The aim of this systematic review was to investigate the short-term (5 -10 year mean follow-up) and long-term (10 year or more) survival and success of fixed full arch dental hybrid prosthesis and supporting dentalimplants. METHODS: Studies reporting interventions with full-arch fixed dental hybrid prostheses were identified by searching Pub. Med/Medline (NCBI), Web of Science (Thomson Reuters), the Cochrane Register of Controlled Clinical Trials (EBSCO), and Dentistry and Oral Sciences Source (DOSS; EBSCO) from the earliest available dates through July 17, 2013. Through a series of review process by two examiners, potentially qualifying studies were identified and assessed with respect to the inclusion criteria. RESULTS: A total of 18 studies were included for the quality assessment and the systematic review. Within the limitation of available studies, high short-term survival rates of full arch fixed dental hybrid prostheses (93. 3 -100%) and supporting implants (87. 89 -100%) were found. However, the availability of studies investigating long-term outcomes seemed scarce. Furthermore, the included studies were subjected to potential sources of bias (i. e. publication, reporting, attrition bias). CONCLUSIONS: Despite seemingly high short-term survival, long-term survival of implant supported full arch fixed dental hybrid prosthesis could not be determined due to limited availability of true long-term studies. Although it may be a valuable option for a patient with a completely edentulous ridge(s), the strategic removal of teeth with satisfactory prognosis for the sake of delivering an implant supported full-arch dental hybrid prosthesis should be avoided.

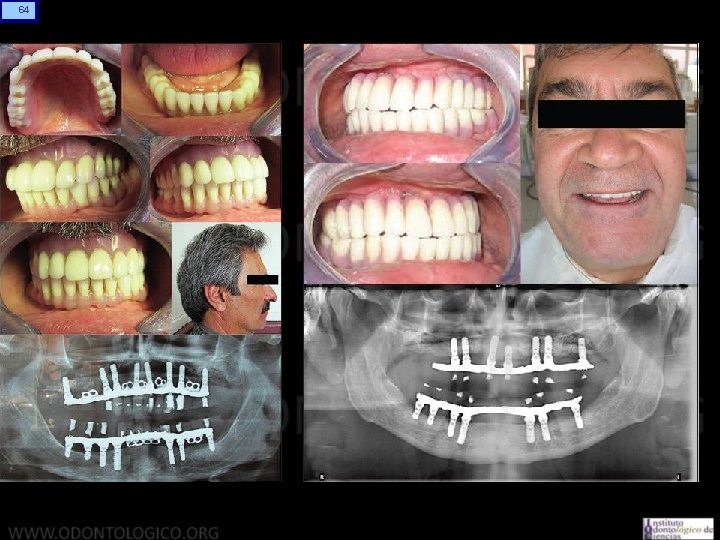
63 Eur J Dent. 2015 Jul-Sep; 9(3): 442– 448. doi: 10. 4103/1305 -7456. 163324 PMCID: PMC 4570001 Implant-supported hybrid prosthesis: Conventional treatment method for borderline cases Ferhan Egilmez, 1 Gulfem Ergun, 1 Isil Cekic-Nagas, 1 and Suleyman Bozkaya 2 Author information ► Copyright and License information ► Go to: Abstract An implant-supported hybrid prosthesis is an acrylic resin complete fixed dental prosthesis and supported by implants might be a solution in extreme cases that the need of the restoration for esthetics, function, lip support, and speech. This clinical report aims to present the esthetic and functional prosthetic rehabilitation of three borderline cases with implant-supported hybrid prostheses. Patient 1 (62 -year-old man) and Patient 2 (61 -year-old man) presented a chief complaint of a compromised esthetic. After clinical evaluations, in Patient 1, 8 implants in the maxilla and 7 implants in mandibula were observed. Patient 2 had 7 implants in the maxilla and 7 implants in mandibula, which were previously placed. The intra-arch dimension of both patients was excessive and an insufficient peri-oral soft tissue support was observed. Patient 3 was a 61 -yearold man had 2 implants with a history of previously implanted graft infection and implant loss on his maxillary posterior jaw. An excessive intra-arch dimension was observed in clinical examination. In addition, massive bone defect and insufficient soft tissue support were examined. In all patients, implant-supported hybrid prostheses were successfully performed. The clinical and radiologic findings were satisfactory. After 3 years of follow-up, no functional, phonetic, or esthetic problems with the restorations were noted. These case reports suggest that implant-supported hybrid prostheses can be a reliable alternative treatment procedure when a porcelain-fused metal fixed restoration does not satisfy a patient's requirements for esthetics, phonetics, oral hygiene, and oral comfort.
64
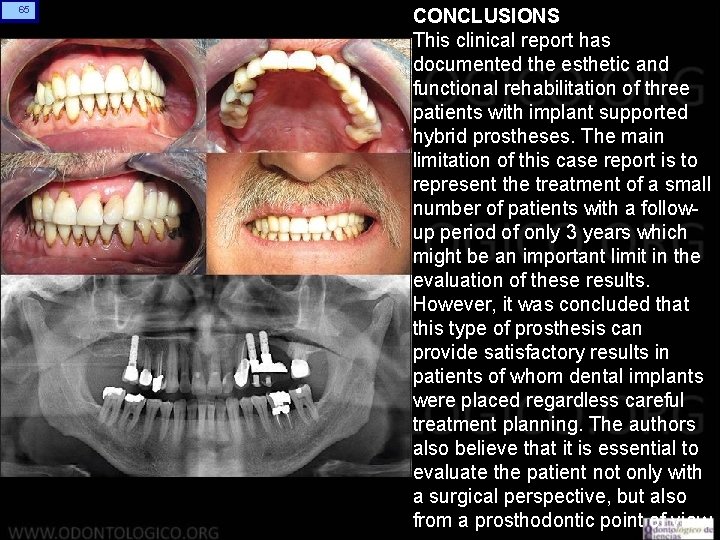
65 CONCLUSIONS This clinical report has documented the esthetic and functional rehabilitation of three patients with implant supported hybrid prostheses. The main limitation of this case report is to represent the treatment of a small number of patients with a followup period of only 3 years which might be an important limit in the evaluation of these results. However, it was concluded that this type of prosthesis can provide satisfactory results in patients of whom dental implants were placed regardless careful treatment planning. The authors also believe that it is essential to evaluate the patient not only with a surgical perspective, but also from a prosthodontic point of view

66 Int J Oral Maxillofac Implants. 2015 Mar-Apr; 30(2): 419 -26. doi: 10. 11607/jomi. 3767. Biomechanical in vitro evaluation of two full-arch rehabilitations supported by four or five implants. Francetti L, Cavalli N, Villa T, La Barbera L, Taschieri S, Corbella S, Del Fabbro M. Abstract PURPOSE: The aim of this in vitro study was to evaluate the stress pattern on the abutments in two different full-arch implantsupported clinically equivalent prosthetic rehabilitations. MATERIALS AND METHODS: Two steel master casts were created and titanium implants were inserted in two different configurations. One configuration used four implants, with the distal implants tilted 30 degrees (4 IMP configuration), and the other used five axially inclined implants (5 IMP configuration). A straight multiunit abutment (MUA) was connected to every axial implant and a 30 -degree angulated MUA was connected to each tilted implant. One titanium framework was fabricated for each configuration, with a 5 -mm (4 IMP configuration) or a 15 -mm (5 IMP configuration) distal cantilever length. Six cycles of vertical loading between 20 and 200 N were applied unilaterally at the most distal point of the frameworks on both sides. Readings of the deformations at the abutment level were obtained with the use of linear strain gauges. RESULTS: A similar pattern of deformation was seen in both configurations. The greatest compressive stress was measured by the strain gauge on the abutment closest to load application and was similar for the 4 IMP and 5 IMP configurations. The tensile stress measured on the same abutment was higher in the 5 IMP configuration than in the 4 IMP configuration. In terms of the distribution of stresses, the deformation measured on the central abutment in the 5 IMP configuration was less than 10% of the overall stress in all the tested conditions. CONCLUSION: There was no difference in strain between the two different designs, so the use of tilted implantswith angulated abutments to reduce cantilever length could be considered a viable clinical option.
- Slides: 66