1 MANAGING GASTROINTESTINAL SYMPTOMS Dr Hattie Roebuck Consultant

1 MANAGING GASTRO-INTESTINAL SYMPTOMS Dr Hattie Roebuck, Consultant in Palliative Medicine E mail: harriet. roebuck@colchesterhospital. nhs. uk Dec 2016

2 Assessing constipation – what does the pt mean?

3 Laxatives, PR intervention (BNF classification) Stimulant Softener • Senna • Na docusate at dose 200 mg tds • Picosulphate or less • Laxido/ movicol • Lactulose • Mg salts • Bisaccodyl • Glycerine supps • Arachis oil enema • Phosphate enemas

4 Other options: Relistor • Indications: opioid induced constipation in terminally ill patients who have failed to respond to other laxatives • Methylnaltrexone -dose dependent on weight • Most pts 8 or 12 mg s/c 2 doses 24 hrs apart • Does not cross Blood brain barrier so analgesic effect of opioids unaffected • Cautions: faecal impaction, diverticular dx, colostomy, peritoneal catheter, liver or renal impairment • C/I: bowel obstruction, perforation • £ 21 per vial

5 Nausea vs Vomiting post chemo is much better controlled than nausea Molassiotis A et al, Support Care Cancer 2008; 16: 201 -8 The evidence for use of anti-emetics is poor ‘A systematic review of the treatment of nausea and/ or vomiting in cancer unrelated to chemotherapy or radiation’ M Davis. JPSM April 2010, Vol 39, no 4, p 756

Common causes of N&V in advanced cancer Drugs Gastric stasis Biochemical Intestinal obstruction Other ICP Lichter, 1993

7 Intractable nausea and vomiting Definition: “Nausea and vomiting that is not adequately controlled after multiple anti-emetics are used in series and/or in combination” Those with the most difficult N&V to manage tend to be those with altered anatomy • eg due to malignant bowel obstruction (dysfunction) or stents/surgical interventions

8 A general approach - 1 Principles: • 1) Initially - identify and treat reversible causes • This may not be appropriate if someone is imminently dying • 2) Assess severity – does the patient need rehydration • 3) Start anti-emetic treatment Prescribe regularly 2. Review control every 24 -48 hours • A second line anti-emetic is required in 1/3 of patients 1.

9 A general approach - 2 4) Consider route of administration Oral route maybe ineffective as frequent vomiting = poor absorption Usually -> Syringe driver Community options: • Rectal route: domperidone supps (true/false? ) • Buccal prochlorperazine • Hysoscine patch • (granisetron patch) • Olanzapine orodispersible melt = 5 mg strength

10 A general approach - 3 • Remember N&V is often multi-factorial • Aim for acceptable control < 3 days • Consider whether dietary/ other factors may help. • • Avoiding triggers Parenteral fluids Limiting oral intake, protein meals, low fat diet Relaxation techniques Acupuncture point P 6 Ginger Surgery (stents, venting g-tubes),

11 PHYSIOLOGY

12 • Stomach – usually has slow wave contractions (3/min) • Rate increases with ‘circular vection’ • Vasopressin release • Nausea perception related to vasopressin release • Primates – VP antagonists stop motion sickness • Humans – ginger reduces nausea, vp rise, reduced tachygastria in motion sickness trials

13 Dietary management • Protein meal – regulates gastrin release, which reduces gastric dysrhythmia & nausea Gastroparesis diet: • Low fat – fat activates stretch receptors in stomach • Fluids • Maintains nutrition & hydration
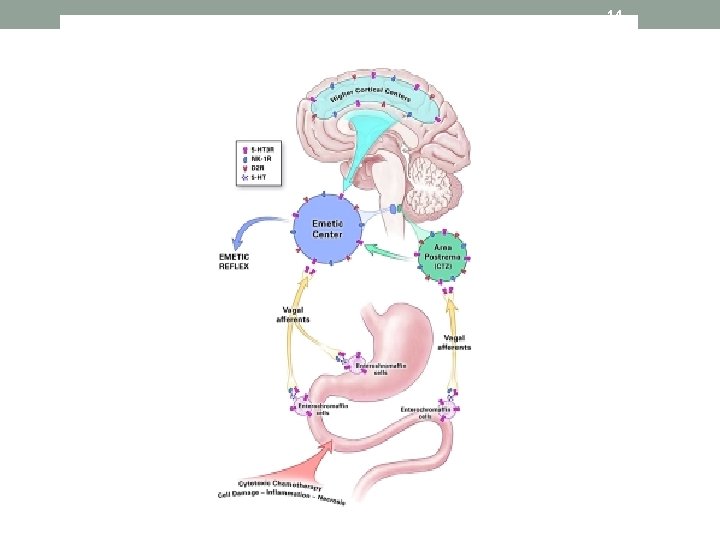
14
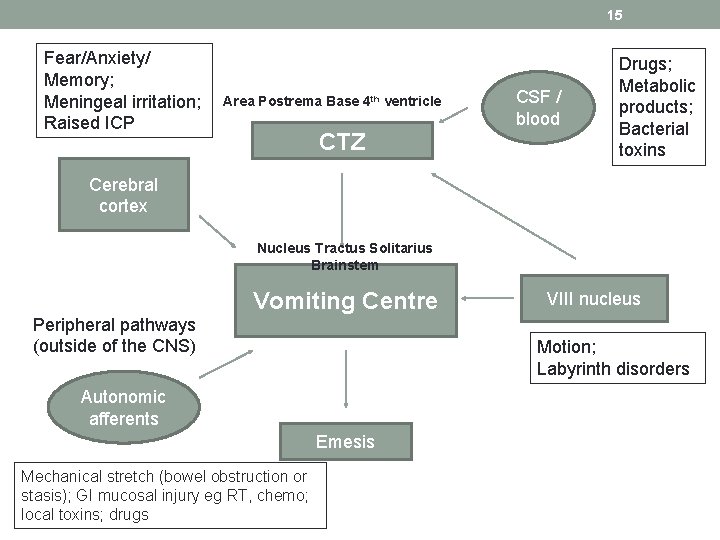
15 Fear/Anxiety/ Memory; Meningeal irritation; Raised ICP Area Postrema Base 4 th ventricle CTZ CSF / blood Drugs; Metabolic products; Bacterial toxins Cerebral cortex Nucleus Tractus Solitarius Brainstem Vomiting Centre Peripheral pathways (outside of the CNS) Motion; Labyrinth disorders Autonomic afferents Emesis Mechanical stretch (bowel obstruction or stasis); GI mucosal injury eg RT, chemo; local toxins; drugs VIII nucleus

16 Metoclopramide • Prokinetic • Dopamine 2 antagonist, 5 HT 4 agonist, 5 HT 3 antagonist • Central (CTZ) and peripheral action (gut mucosa) • Prokinetic effect antagonised by anticholinergic drugs Side effects Extrapyramidal symptoms Drowsiness, restlessness, depression, diarrhoea • (Max 30 mg in 24 hours for up to 5 days – EU review 2013)

17 Domperidone • Prokinetic • Dopamine 2 antagonist • Acts peripherally and at the CTZ • Does not readily cross the blood brain barrier • Oral only • Side effects • Rarely extrapyramidal • Hyperprolactinaemia • Cardiac arrhythmias • Max dose 10 mg TDS (for up to 7 days)

18 Haloperidol • Dopamine 2 antagonist, 5 HT 2 a and α 1 antagonist • Acts predominantly at the CTZ but also peripherally (gut mucosa) • First line for biochemical induced N&V • T½ 13 – 35 hours Side effects Extrapyramidal, hyperprolactinaemia Minimal sedation and hypotension NB - Prolongation of QT interval

19 Cyclizine • H 1 antagonist and cholinergic muscarinic antagonist • Acts at the vestibular apparatus (& vomiting centre) • Plasma T½ 13 hours Side effects Drowsiness, urinary retention, dry mouth, blurred vision, constipation, headache, psychomotor impairment • Caution in severe liver disease, severe heart failure, renal failure, glaucoma

20 Cyclizine • Not advocated for use in heart failure • Increases systemic & pulmonary arterial pressures • Increases right & left ventricular filling pressures • Counteract beneficial haemodynamic effects of opioids in heart failure • ‘Detrimental haemodynamic effects of cyclizine in heart failure’ LB Tan • The Lancet March 1988

21 Hyoscine Hydrobromide / Butylbromide Hyoscine hydrobromide Hyoscine butylbromide • Tertiary amine • Quaternary ammonium deriv • Central AChm antagonist • Peripheral AChm antagonist • anti-emetic • anti-secretory (d of a 1– 9 hrs) • anti-secretory (d of a < 2 hrs) • anti-spasmodic • Side effects Drowsiness, agitation, delirium, bradycardia • Side effects Dry mouth, blurred vision, constipation, urinary retention

22 Ondansetron • 5 HT 3 antagonist • Acts at CTZ and gut mucosa Blocks amplifying effect of excess 5 HT on vagus Bowel wall enterochromaffin cells release 5 HT by various stimuli. >Sensitises the vagal afferent nerves to emetogenic substances via 5 HT 3 receptors • Early N&V post chemo: First 24 hrs after chemo only • Useful where excessive 5 HT released eg chemotherapy or radiotherapy induced damage of gut mucosa, bowel distension, renal failure Side effects Headache, flushing, constipation

23 Aprepitant • Neurokinin-1 receptor antagonist (NK 1) • Substance P found widely in the CNS, including CTZ, VC and GI tract • Chemotherapy increases substance P levels as well as serotonin release • Antiemetic effects of NK 1 antagonism is a central effect • Effective for delayed Chemo Induced N&V (>24 hrs) • Given alongside 5 HT 3 antagonist and Dexamethasone • No evidence that it has much role in Palliative Care

24 Levomepromazine • Dopamine 2 antagonist, Muscarinic cholinergic antagonist, Histamine 1 antagonist, 5 HT 2 A antagonist, alpha-adrenergic antagonist • Acts at vomiting centre • Plasma T½ 15 – 30 hours Side effects Sedation, weakness Dry mouth, hypotension, extrapyramidal symptoms
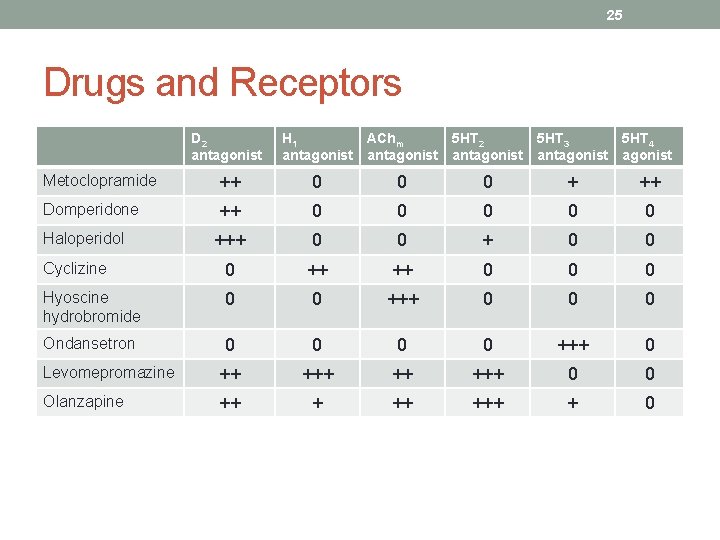
25 Drugs and Receptors D 2 antagonist H 1 antagonist AChm antagonist 5 HT 2 antagonist 5 HT 3 antagonist 5 HT 4 agonist Metoclopramide ++ 0 0 0 + ++ Domperidone ++ 0 0 0 +++ 0 0 Cyclizine 0 ++ ++ 0 0 0 Hyoscine hydrobromide 0 0 +++ 0 0 0 Ondansetron 0 0 +++ 0 Levomepromazine ++ +++ 0 0 Olanzapine ++ +++ + 0 Haloperidol

26 Olanzapine • Atypical antipsychotic • Dopamine 1, 2, 3 and 4 antagonist 5 HT 2 A, 5 HT 2 C, 5 HT 3 and 5 HT 6 antagonist, Alpha-adrenergic antagonist, Histamine-1 antagonist, Muscarinic cholinergic antagonist • Acts at the Vomiting Centre • T½ 34 hours (↑ 52 hours in the elderly) • Side effects Drowsiness, weight gain Dry mouth, constipation, hypotension, peripheral oedema Less movement disorders than with Haloperidol
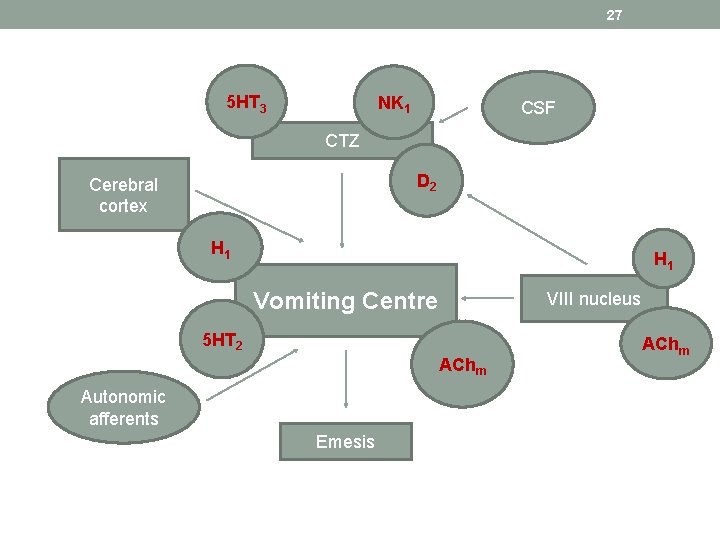
27 5 HT 3 NK 1 CSF CTZ D 2 Cerebral cortex H 1 Vomiting Centre VIII nucleus 5 HT 2 AChm Autonomic afferents Emesis AChm
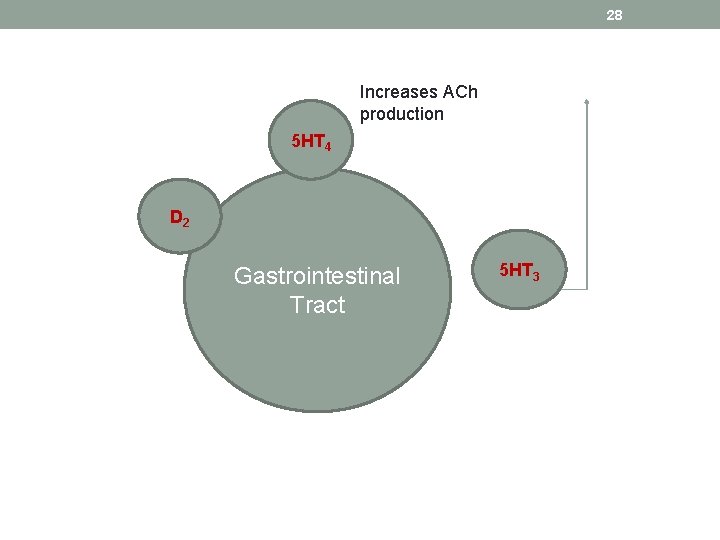
28 Increases ACh production 5 HT 4 D 2 Gastrointestinal Tract 5 HT 3

29 Dexamethasone • Glucocorticoid • Reduces permeability of the CTZ and the blood brain barrier to emetogenic substances • Reduces neuronal content of GABA in the brain stem • Suggested that antagonism of PGs, release of endorphins and depletion of tryptophan may play a role • ? central or peripheral effect

30 Summary • Vomiting is unpleasant and debilitating • There are multiple causes • General measures and drug interventions are usually successful • It is helpful to understand the receptor basis of rational prescribing • But we cannot always control all associated symptoms

31 Medical management of bowel obstruction • Features of bowel obstruction: • Causes of bowel obstruction: 1. 2. 3. 4. Intraluminal Extraluminal Motility disorders (tumour infiltration, neuropathic damage to GIT, drugs such as opioids, anticholinergics etc) Constipation/ faecal impaction

32 Systematic review of surgery for malignant bowel obstruction (D. Feuer et al, Gynaecological Oncology 1999) • Control of symptoms 42 -80% • Re-obstruction rates 10 -50% (most studies did not describe time scales) • Wide range of post op morbidity & mortality Gynaecological Oncology 2003 Pothuri et al: palliative bowel obstruction in ovarian ca • Major surgical mobidity 22% - fistula/ abscess/ PE/ peritonitis/ sepsis • Perioperative mortality 6% • But survival mean 12 months if palliation successful cf 3 months no surgery

33 • How best to manage? • 1. Surgical opinion & document time for audit • Non surgical: colic/ high risk perforation or no colic • 2. Antiemetic: Stimulant antiemetic/ Non stimulant • 3. Laxative (non stimulant) • 4. Steroid s/c or IV (NNT 6) • 5. NG/ antisecretory • 6. Fluids?

34 Prognosticating hard Outcomes: • Subacute bowel obstruction can resolve • Most pts will have a recurrence unless have treatment options such as chemotherapy still available to them • Pts can live with subacute bowel obstruction for some months, equates to gut failure • Psycho-social impact can be profound; inability to eat • US – use of parenteral nutrition>UK • Risk of death, sudden deterioration if perforate • Sudden increased pain

35 Summary • Effect on GIT helpful in determining which laxatives and anti-emetics to use • Adherence to laxative regime can be challenging • Nausea & Vomiting evidence base is poor • Rational prescribing makes sense • Bowel obstruction has significant complications, including death or for chronic subacute bowel obstruction, psycho-social. Equates to gut failure.

36 Further reading ‘Treating nausea & vomiting in palliative care: a review’ P Glare. Clinical Interventions in Aging 2011; 6 p 243 Wood G et al. Management of Intractable Nausea and Vomiting in Patients at the End of Life: “I Was Feeling Nauseous All of the Time…Nothing Was Working” in Mc. Phee S et al (eds) Care at the Close of Life: Evidence and Experience, 2010 www. palliativedrugs. com
- Slides: 36