1 Hyperhidrosis Dr Abbas Pardakhty 2011 Kerman Faculty

1

Hyperhidrosis Dr Abbas Pardakhty 2011 Kerman Faculty of Pharmacy 2

Sweat Glands The human body has 2 -5 million sweat glands Two main types: ECCRINE APOCRINE Source: www. sweathelp. org 3

Eccrine Sweat Glands Ø Approximately 3 million eccrine sweat glands Ø Secrete a clear, odorless fluid Ø Aid in regulating body temperature Ø Areas of concentration: l Facial, plantar, and axillae Source: www. sweathelp. org 4

Apocrine Sweat Glands Inactive until puberty Produce thick fluid Secretions come in contact with bacteria on the skin and produce characteristic “body odor” Found in axillary and genital areas Source: www. sweathelp. org 5

Sweating The hypothalamus serves as thermoregulatory center It controls both blood flow and sweat output to the skin’s surface Source: www. sweathelp. org 6

Sweating Ø The hypothalamus can be triggered by: EXERCISE STRESS TEMPERATURE CHANGE HORMONES Source: www. sweathelp. org 7
Sweating Once triggered, the hypothalamus sends messages down the spinal cord via neurotransmitters. Source: www. sweathelp. org 8

Sweating The neurostransmitters travel down the spine via ganglion or sympathetic nerves These ganglion travel to nerves, which reach the skin’s surface Source: www. sweathelp. org Photo used with permission: The Whiteley Clinic, 2007 9
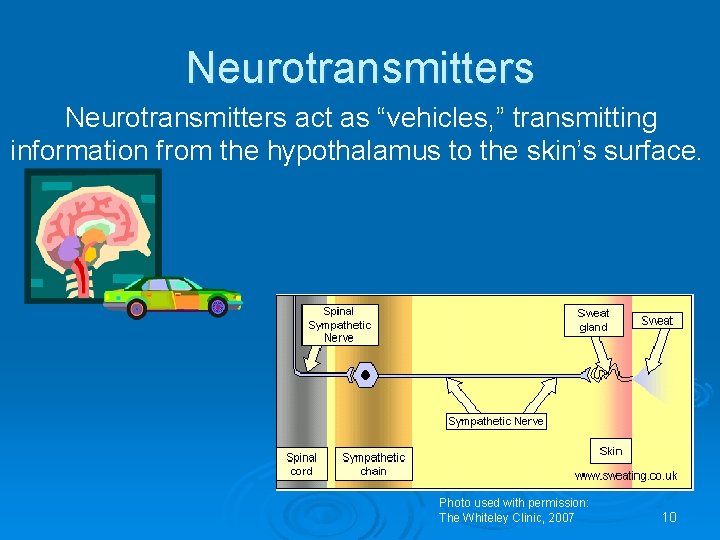
Neurotransmitters act as “vehicles, ” transmitting information from the hypothalamus to the skin’s surface. Photo used with permission: The Whiteley Clinic, 2007 10

Neurotransmitters The neurotransmitters can “exit” at various places along the spinal cord. The “exit” determines the location of skin innervation. 11
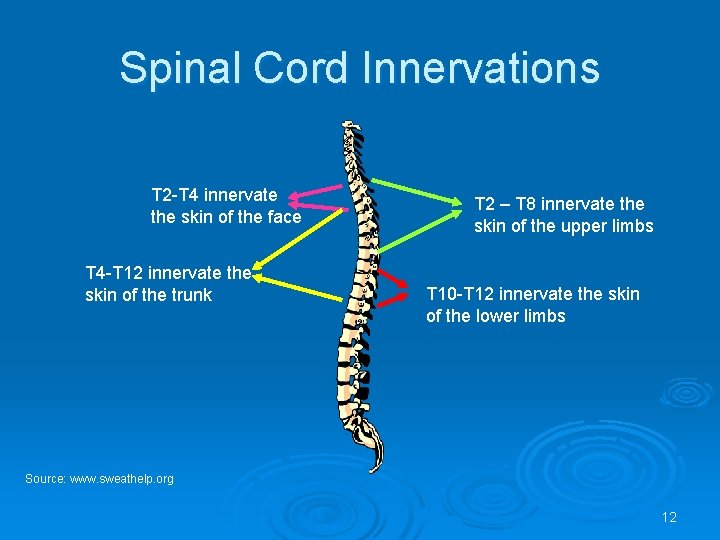
Spinal Cord Innervations T 2 -T 4 innervate the skin of the face T 4 -T 12 innervate the skin of the trunk T 2 – T 8 innervate the skin of the upper limbs T 10 -T 12 innervate the skin of the lower limbs Source: www. sweathelp. org 12
Neurotransmitters Acetylcholine innervates Eccrine Sweat Glands Catecholamines innervate Apocrine Sweat Glands Source: www. sweathelp. org 13

Sweating Once innervated, the apocrine and eccrine glands will produce …. Source: www. sweathelp. org SWEAT! 14

What is Hyperhidrosis? w Sweating that is more than required to maintain normal thermal regulation 15

Sweating Nomenclature w Areas: Focal, regional, generalized w Symmetry: Symmetric or asymmetric w Classification: Primary vs. secondary w Type of sweating: Anhidrosis, euhydrosis, hyperhidrosis Multi-specialty Working Group on Recognition, Diagnosis, and Treatment of Primary Focal Hyperhidrosis, 2003. 16

Hyperhidrosis 17

Causes of Generalized Hyperhidrosis Usually secondary in nature w Drugs (Venlafaxine, . . . ), toxins, substance abuse w Cardiovascular disorders w Respiratory failure w Infections w Malignancies w Hodgkin’s, myleoproliferative disorders, cancers with increased catabolism w Endocrine/metabolic disorders w Thyrotoxicosis, pheochromocytoma, acromegaly, carcinoid tumor, hypoglycemia, menopause w Rarely Idiopathic / Primary HH 18

Causes of Localized Hyperhidrosis w Usually Idiopathic / Primary w Social anxiety disorder w Eccrine nevus w Gustatory sweating w Frey syndrome w Impaired evaporation w Stump hyperhidrosis after amputation 19
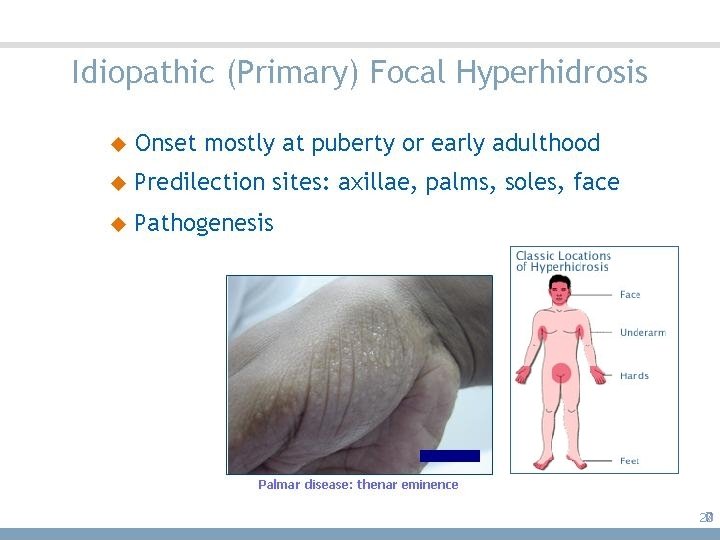
Idiopathic (Primary) Focal Hyperhidrosis 20
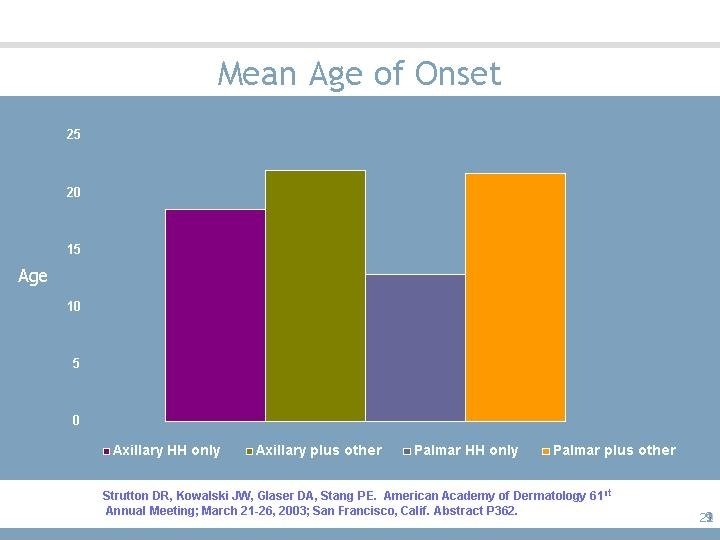
Mean Age of Onset 21

Diagnosis of Primary Focal Hyperhidrosis w Focal, visible, excessive sweating of at least 6 months duration without apparent cause with at least 2 of the following characteristics: • • • Bilateral and relatively symmetric Impairs daily activities Frequency of at least one episode per week Age of onset less than 25 years Positive family history Cessation of focal sweating during sleep Multi-specialty Working Group on Recognition, Diagnosis, and Treatment of Primary Focal Hyperhidrosis, 2003. 22
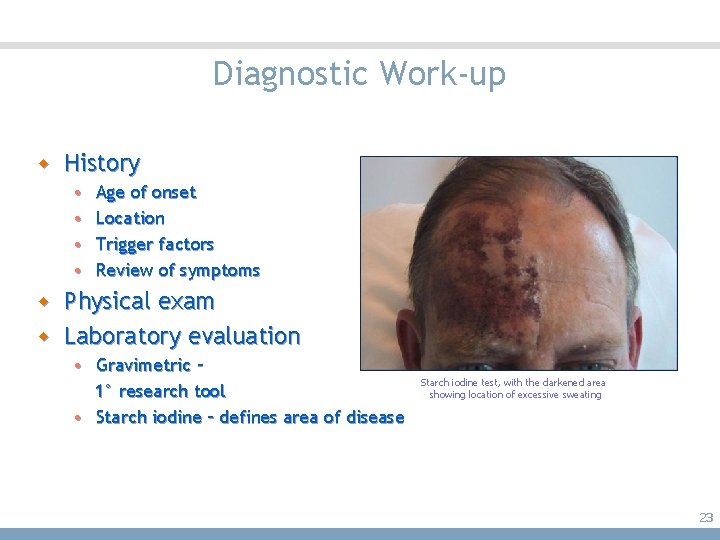
Diagnostic Work-up w History • • Age of onset Location Trigger factors Review of symptoms w Physical exam w Laboratory evaluation • Gravimetric – 1° research tool • Starch iodine – defines area of disease Starch iodine test, with the darkened area showing location of excessive sweating 23
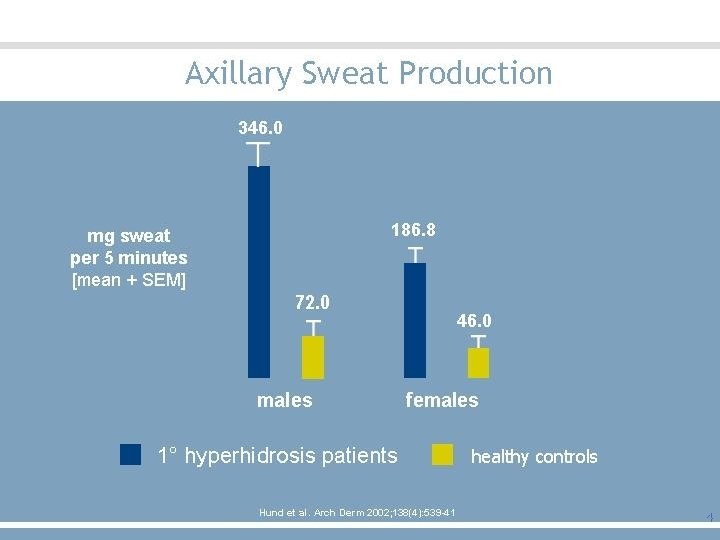
Axillary Sweat Production 346. 0 1° hyperhidrosis patients Hund et al. Arch Derm 2002; 138(4): 539 -41 healthy controls 24
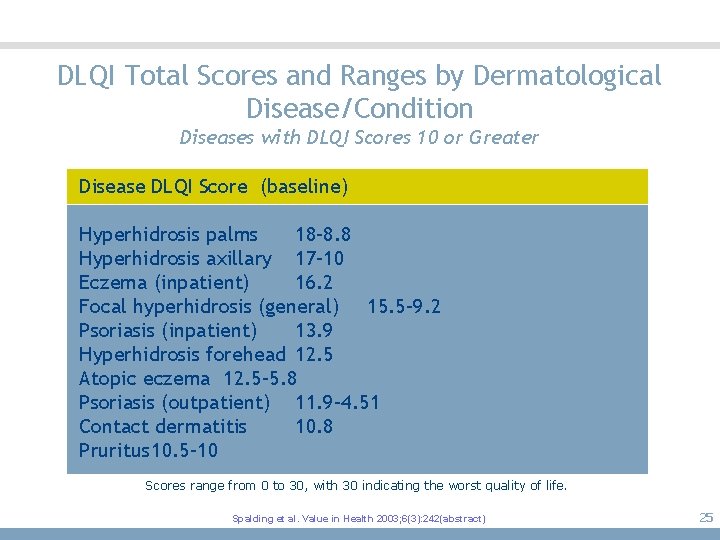
DLQI Total Scores and Ranges by Dermatological Disease/Condition Diseases with DLQI Scores 10 or Greater Disease DLQI Score (baseline) Hyperhidrosis palms 18– 8. 8 Hyperhidrosis axillary 17– 10 Eczema (inpatient) 16. 2 Focal hyperhidrosis (general) 15. 5– 9. 2 Psoriasis (inpatient) 13. 9 Hyperhidrosis forehead 12. 5 Atopic eczema 12. 5– 5. 8 Psoriasis (outpatient) 11. 9– 4. 51 Contact dermatitis 10. 8 Pruritus 10. 5– 10 Scores range from 0 to 30, with 30 indicating the worst quality of life. Spalding et al. Value in Health 2003; 6(3): 242(abstract) 25

Summary Primary Focal Hyperhidrosis is a separate and unique disease • Bilateral & symmetric • Axilla, palms, soles, craniofacial • Onset in childhood and adolescence • Significant impact on quality of life • Effective therapies 26

Treatment 27

Available Treatments Topical agents w Iontopheresis w Systemic agents w • anticholnergic Botulinum toxin w Surgery w • • Local excision/currettage Thoracic sympathectomy 28
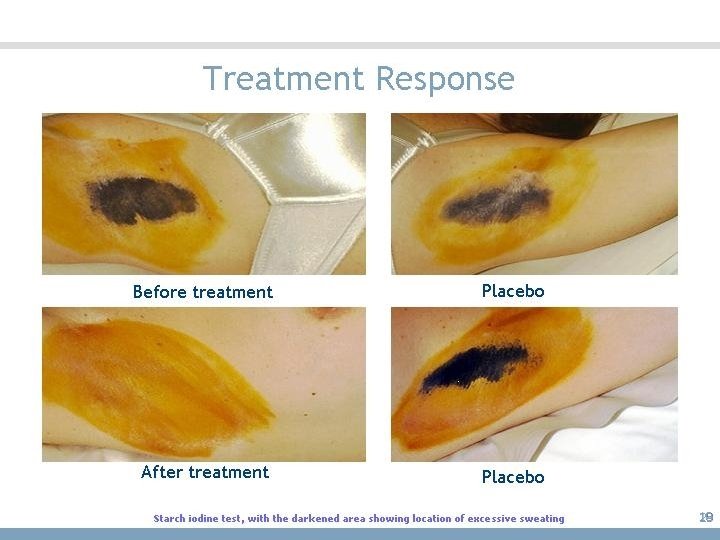
Treatment Response 29
Topical Treatment Options Click on the first treatment option to begin! Systemic Iontophoresis Botox Local Excision Thorascopic Sympathectomy 30

Topical Treatment First line treatment Aluminum Chloride Hexahydrate antiperspirant of choice Photos used with permission: www. feelbest. com Most beneficial for axillary hyperhidrosis Can be used for plantar and palmar Hornberger, 2004 31

Topical Treatment: How Does it Work? The metal ions in the topical antiperspirant damage the lining of the sweat gland. As damage continues, a PLUG is formed over the sweat gland. www. sweathelp. org 32

Topical Treatment Sweat production never ceases, the gland is simply plugged Sweating will return as the skin undergoes regeneration or shedding Photo used with permission: Neurosurgical Medical Clinic, Inc Therefore…topical treatment is NOT a cure! Hornberger, 2004 33

Topical Treatment: How to Use Best to apply before bedtime Allow to remain on skin for 6 – 8 hours Apply every 24 – 48 hours until sweating diminishes Maintenance applications needed every 13 weeks Hornberger, 2004 34
Topical Treatment: Pros and Cons – n No Hornberger, 2004 a v in e v i s Itch ing and at a bur ppl icat ning o f sk ion Tim in site & e-c ons um Tem ing & por ary reli ef 35
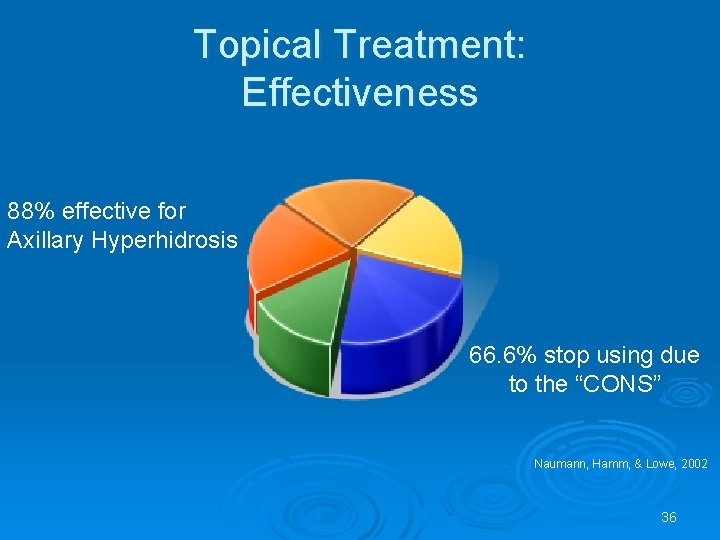
Topical Treatment: Effectiveness 88% effective for Axillary Hyperhidrosis 66. 6% stop using due to the “CONS” Naumann, Hamm, & Lowe, 2002 36

Topical Treatment Options Click on the second treatment option! Systemic Iontophoresis Botox Local Excision Thorascopic Sympathectomy 37

Systemic Treatment Anticholinergics can be used in treating hyperhidrosis Most effective for cranio-facial hyerhidrosis Robinul – drug of choice Haider & Solish, 2004 38

Oral Glycopyrrolate (Glycopyrronium bromide) 39

How Does it Work? Anticholinergic Blocks Acetylcholine transmission Eccrine sweat glands no longer stimulated Sweat production ceases! Haider & Solish, 2004 40

Anticholinergics Ø Long term therapy is required Ø Major side effects: l l l Dry mouth Dry eyes Constipation Blurred vision Difficulty with urination Thomas, Brown, & Vafaie, 2004 41

Anticholinergics Ø Limited use in treating hyperhidrosis Ø Only 21% effective Ø 69. 7% stop using due to side effects Hamm, Naumann, & Kowalski, 2006 42

Topical anticholinergics glycopyrronium bromide as 1 and 2% cream or roll-on solution Ø Topical hyoscine as 0. 25, 1, or 3% solution or cream also gave control of sweating, but was associated with a much higher incidence of sideeffects. Ø Patients with diabetic gustatory sweating have also noted a reduction in the frequency and severity of episodes after applying glycopyrronium 0. 5% cream Ø 43

Topical Treatment Options Click on the third treatment option! Systemic Iontophoresis Botox Local Excision Thorascopic Sympathectomy 44

Iontophoresis Ø Used for palmar and plantar hyperhidrosis Ø Passage of direct electrical current onto skin’s surface Ø Device can be purchased for home use Photo used with permission: Beast Psoriasis, 2006 Thomas, Brown, & Vafaie, 200 4 45
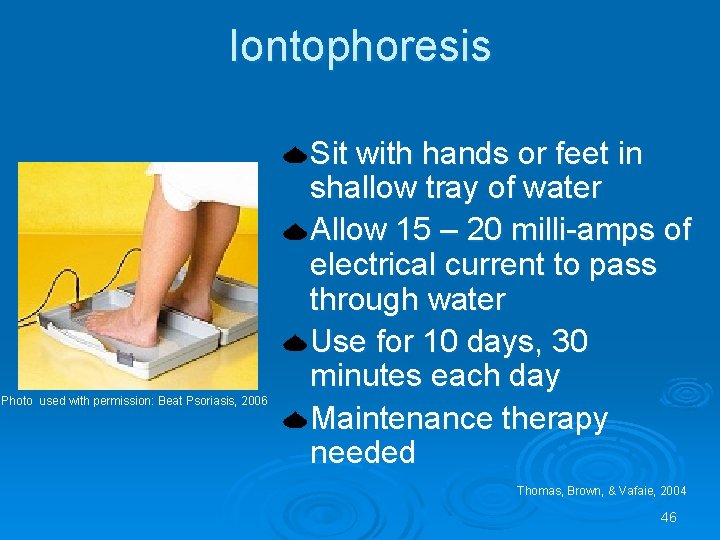
Iontophoresis Photo used with permission: Beat Psoriasis, 2006 Sit with hands or feet in shallow tray of water Allow 15 – 20 milli-amps of electrical current to pass through water Use for 10 days, 30 minutes each day Maintenance therapy needed Thomas, Brown, & Vafaie, 2004 46

Iontophoresis: Mechanism of Action + WATER = ELECTRICTY Thickening of skin And Blocked sweat flow www. sweathelp. org 47

Iontophoresis Side effects: Skin irritation Skin burns Vesicle formation Photo used with permission: Beat Psoriasis, 2006 Time consuming treatment 80% effective for palmar and/or plantar hyperidrosis Thomas, Brown, and Vafaie, 2004 48
Topical Treatment Options Click on the fourth treatment option! Systemic Iontophoresis Botox Local Excision Thorascopic Sympathectomy 49
50
Botox Ø Botox injections can be used to treat axillary, palmar, and plantar hyperhidrosis Ø Analgesic applied prior to injection Ø Nerve block applied to ulnar or radial nerve prior to palmar injection Haider & Solish, 2004 51

Botox blocks the release of acetylcholine at the site of the neuromuscular junction. Sweat glands are not stimulated, and sweat production ceases Photo used with permission: Whiteley Clinic, 2007 Site of blockage Haider & Solish, 2004 52
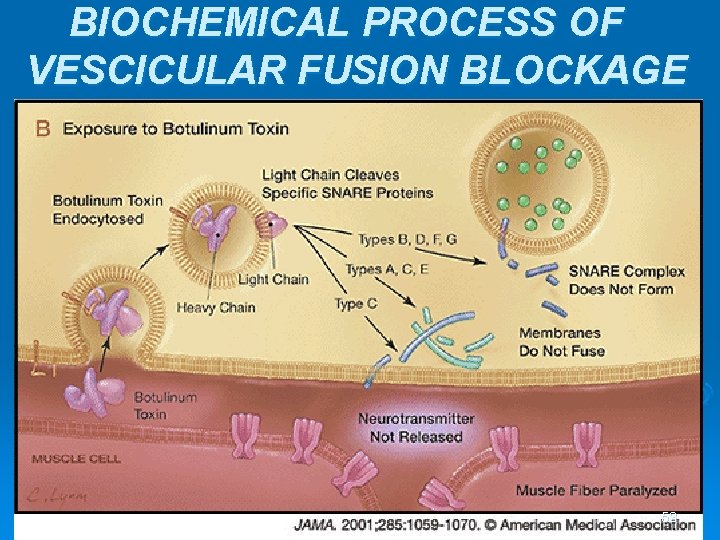
BIOCHEMICAL PROCESS OF VESCICULAR FUSION BLOCKAGE 53
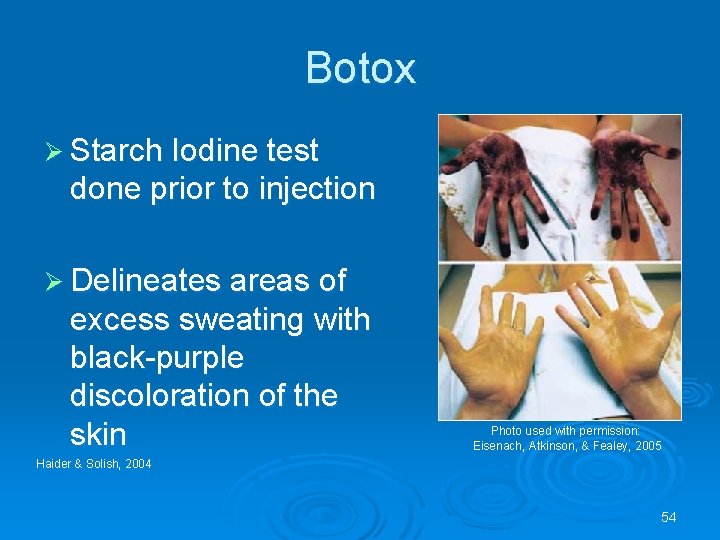
Botox Ø Starch Iodine test done prior to injection Ø Delineates areas of excess sweating with black-purple discoloration of the skin Photo used with permission: Eisenach, Atkinson, & Fealey, 2005 Haider & Solish, 2004 54

Botox Pros: Lasts 6 -7 months 90% effective Cons: Very painful to the palms and soles of feet Ø Expensive: $1400$1600 per treatment Ø Thomas, Brown, & Vafaie, 2004 55
Topical Treatment Options Click on the fourth treatment option! Systemic Iontophoresis Botox Local Excision Thorascopic Sympathectomy 56
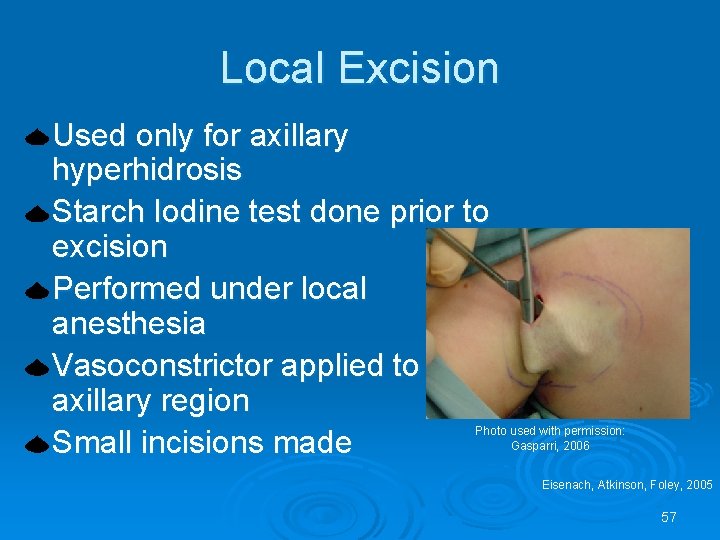
Local Excision Used only for axillary hyperhidrosis Starch Iodine test done prior to excision Performed under local anesthesia Vasoconstrictor applied to axillary region Small incisions made Photo used with permission: Gasparri, 2006 Eisenach, Atkinson, Foley, 2005 57

Local Excision Ø Eccrine sweat glands removed through: l l l Liposuction – suctioned out Curettage – scraped out Excision – cut out Ø Incisions sutured Ø Pain and bruising to excision site Photo used with permission: Gasparri, 2006 Eisenach, Atkinson, & Fealey, 2005 58

Local Excision Ø Starch Iodine tests done post excision show 80% - 90% decrease in sweating Ø Has a potential for scarring Eisenach, Atkinson, & Fealey, 2005 59
Topical Treatment Options Click on the fourth treatment option! Systemic Iontophoresis Botox Local Excision Thorascopic Sympathectomy 60
Endoscopic Thoracic Sympathectomy (ETS) Ø Last treatment option Ø PERMANENT Ø Surgery performed under general anesthesia Haider & Solish, 2004 61

ETS Ø Goal of surgery is to excise or ablate the ganglion that innervate the sweat glands Ø Performed most frequently for palmar hyperhidrosis Ø Performed through thorascope or video Ø Minimally invasive Han, Oren, & Gottfried, 2002 Photo used with permission: Neurosurgical Medical Clinic, Inc 62

ETS Ø Small incision made laterally under each axilla Ø Incision made through intercostal space Ø Surgery can be performed on outpatient basis Ø However, some patients remain in hospital for one night Han, Oren, & Gottfried, 2002 63
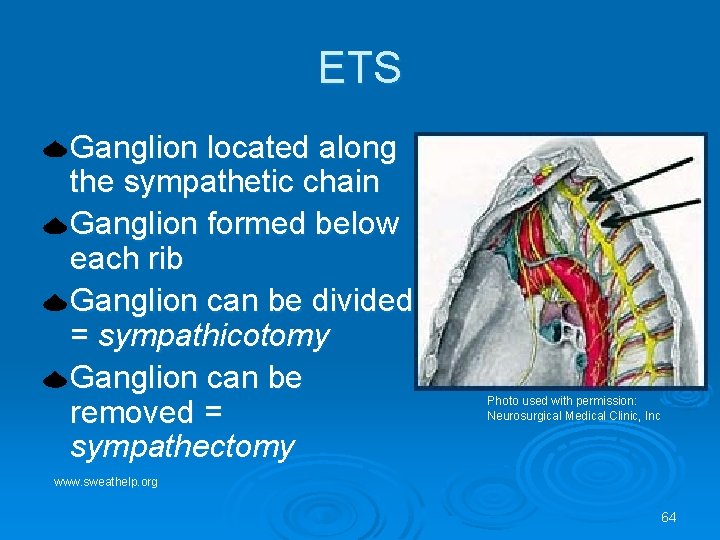
ETS Ganglion located along the sympathetic chain Ganglion formed below each rib Ganglion can be divided = sympathicotomy Ganglion can be removed = sympathectomy Photo used with permission: Neurosurgical Medical Clinic, Inc www. sweathelp. org 64
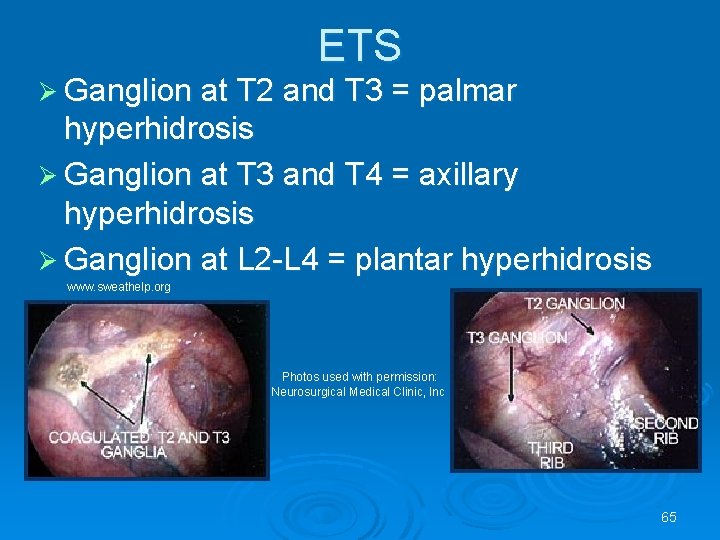
ETS Ø Ganglion at T 2 and T 3 = palmar hyperhidrosis Ø Ganglion at T 3 and T 4 = axillary hyperhidrosis Ø Ganglion at L 2 -L 4 = plantar hyperhidrosis www. sweathelp. org Photos used with permission: Neurosurgical Medical Clinic, Inc 65

ETS Cannot surgically excise or ablate L 2 -L 4 for plantar hyperhidrosis due to sexual side effects 95% success rate in curing palmar hyperhidrosis Success rates slightly lower for axillary hyperhidrosis Eisenach, Atkinson, & Fealey, 2005 66

ETS Ø Plantar hyperhidrosis resolves in 50% - 75% of cases when T 2 and T 3 are excised, though L 2 -L 4 ganglion are never surgically treated Ø Mechanism is unknown! Eisenach, Atkinson & Fealey, 2005 67

ETS: Side Effects Ø Surgical complications: l l l Hemo-pneumothorax requiring chest tube placement – 1% Atelectasis (collapse of the lung) Intercostal neuralgia – 1% Horner’s Syndrome – 1% Compensatory Sweating – 60% Eisenach, Atkinson, & Fealey, 2005 68

Horner’s Syndrome Ø Stellate ganglion – fusion of C 8 and T 1 l Innervates the face Ø If Stellate ganglion is damaged, Horner’s Syndrome will occur l l May be mistaken for T 2 and T 3 May receive electrical current from cautery of T 2 and T 3 www. sweathelp. org 69

Horner’s Syndrome Ø Signs and Symptoms l l l Unilateral upper eyelid ptosis Pupil constriction Facial anhidrosis www. sweathelp. org 70
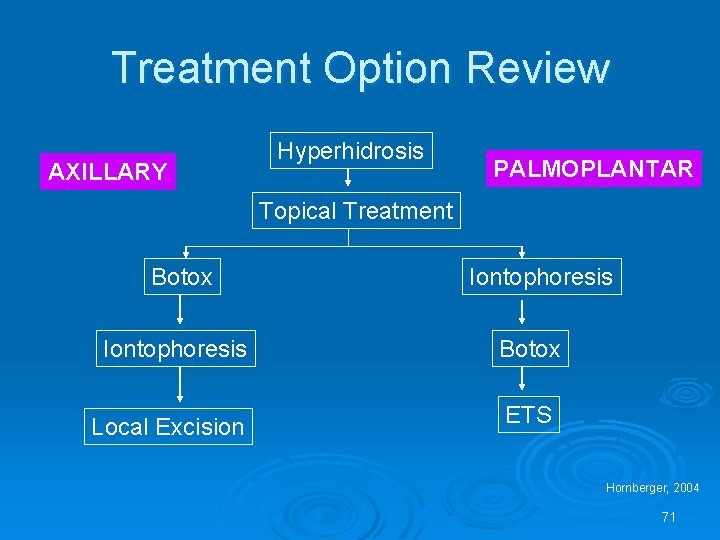
Treatment Option Review AXILLARY Hyperhidrosis PALMOPLANTAR Topical Treatment Botox Iontophoresis Local Excision Iontophoresis Botox ETS Hornberger, 2004 71
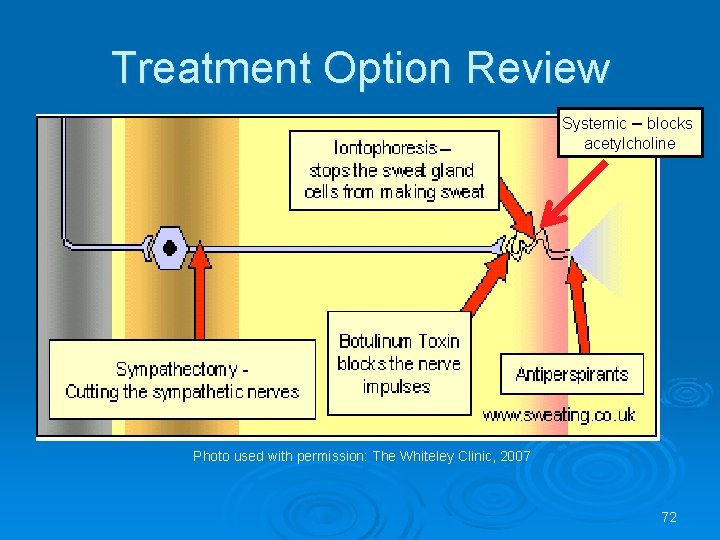
Treatment Option Review Systemic – blocks acetylcholine Photo used with permission: The Whiteley Clinic, 2007 72
- Slides: 72