1 Conduction Disturbances 2 SINUS BRADYCARDIA SINUS TACHYCARDIA

1

Conduction Disturbances 2

SINUS BRADYCARDIA SINUS TACHYCARDIA… SINUS DYSRHYTHMIA (ARHYTHMIA) SINUS PAUSE (ARREST) SINOATRIAL BLOCK Only single shape P 3

SINUS DYSRHYTHMIA u Some variation in the sinus node discharge rate is common, but if the variation exceeds 0. 12 s between the longest and shortest intervals, sinus dysrhythmia is present. u The ECG: u (1) normal sinus P waves and P-R intervals, (2) 1: 1 AV conduction, and u (3) variation of at least 0. 12 s between the shortest and longest P-P interval 4
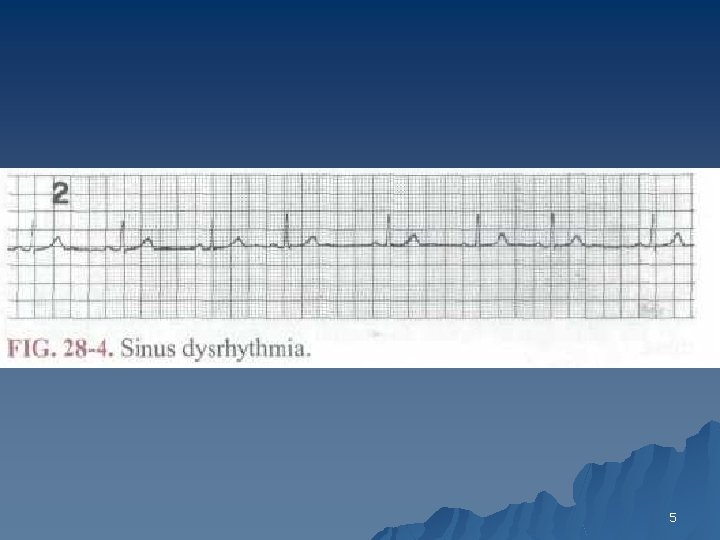
5
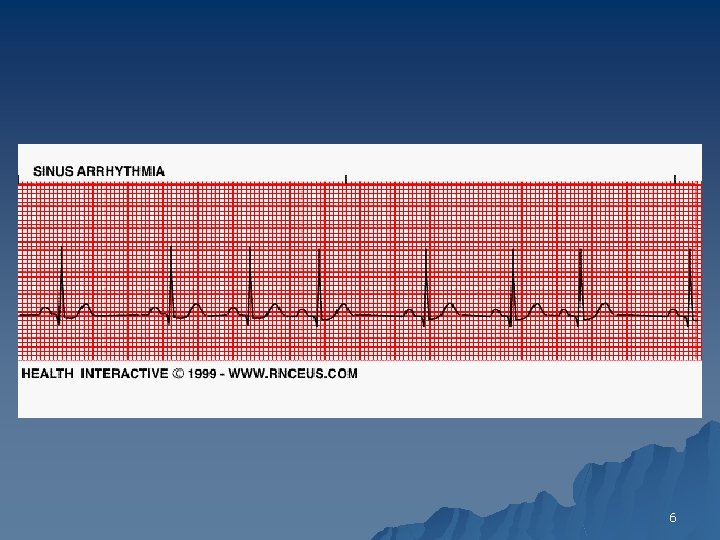
6
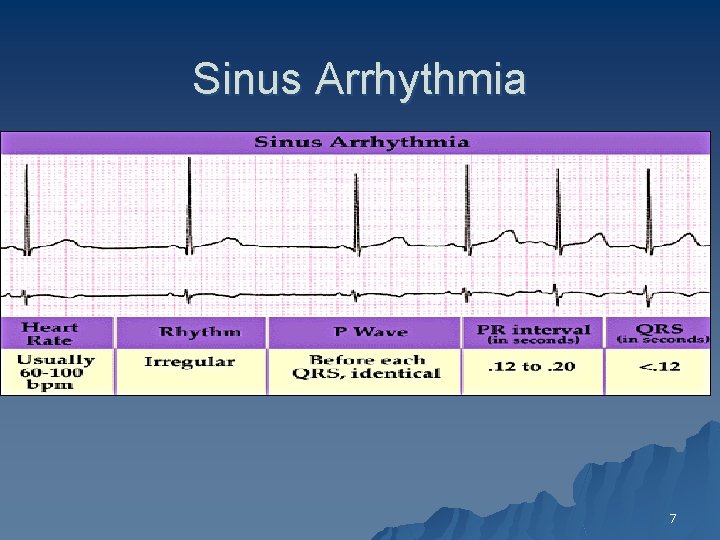
Sinus Arrhythmia 7
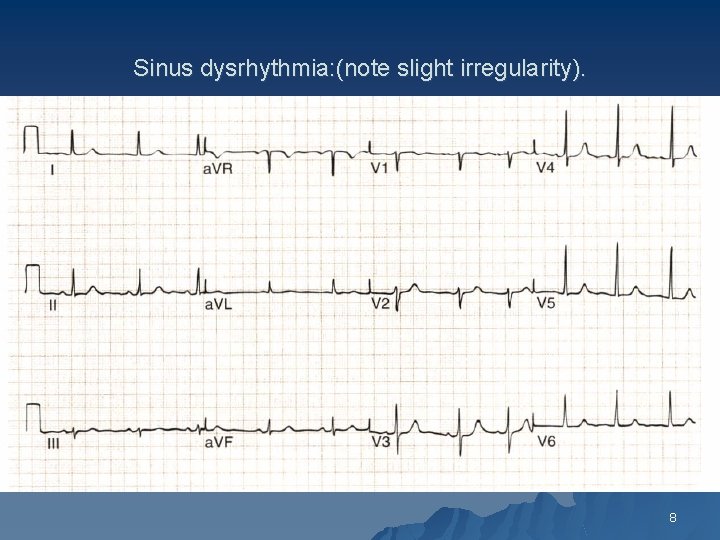
Sinus dysrhythmia: (note slight irregularity). 8

Sinus Arrest (Pause) u Sinus pause is a failure of impulse formation within the sinus node. u In sinus arrest, the P-P interval has no mathematical relation to the basic sinus node discharge rate 9
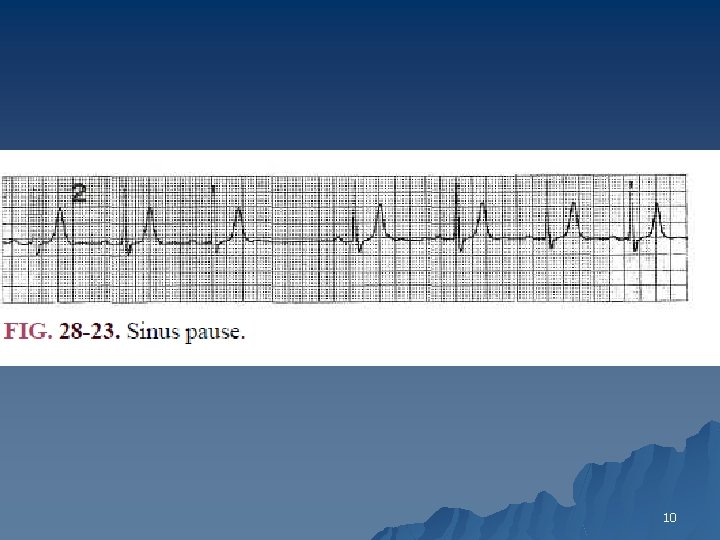
10

u s. dysrhythmia vs s. arrest? u Sinus dysrhythmia : irregular-irregular u Sinus Arrest (Pause): regular-irregular 11

The pause is not equal to exactly two or more(3, 4, …) cardiac cycles of the underlying rhythm. 12

u. Sinoatrial Block 13

pause In a sinus exit block the pause is equal to ex two or more cardiac cycles of the underlying rhythm. The electrical impulse from the SA node is bl and not conducted to the atria. 14

Sino Atrial Exit Block • • Implies that there is delay or failure of a normally generated sinus impulse to exit the nodal region. First degree SA block: slowed conduction Second degree SA block: intermittent conduction 1. Type 1 (Mobitz 1) 2. Type 2 (Mobitz 2) • • Third degree SA block: complete conduction failure 15

First Degree Sino Atrial Exit Block u Implies that the conduction time where each impulse leaving the node is prolonged u This problem cannot be observed on surface EKG u Electro physiology study needed to measure the sino atrial conduction time 16

Second Degree Sino Atrial Exit Block u Type I (SA Wenckebach) 1. PP intervals gradually shorten until a pause occurs (i. e. , the blocked sinus impulse fails to reach the atria) 2. The pause duration is less than the two preceding PP intervals 3. The PP interval following the pause is greater than the PP interval just before the pause 17
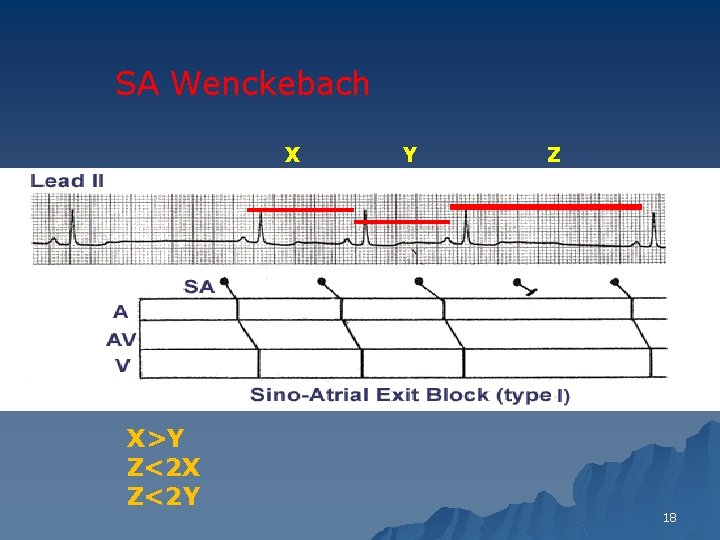
SA Wenckebach X X>Y Z<2 X Z<2 Y Y Z 18

SA Block type 1 vs S. Pause? u Both irregular-irregular u SA Block type 1: 1. PP intervals gradually shorten until a pause occurs 2. The pause duration is <2 PP 3. The PP interval following the pause > PP interval just before the pause 19
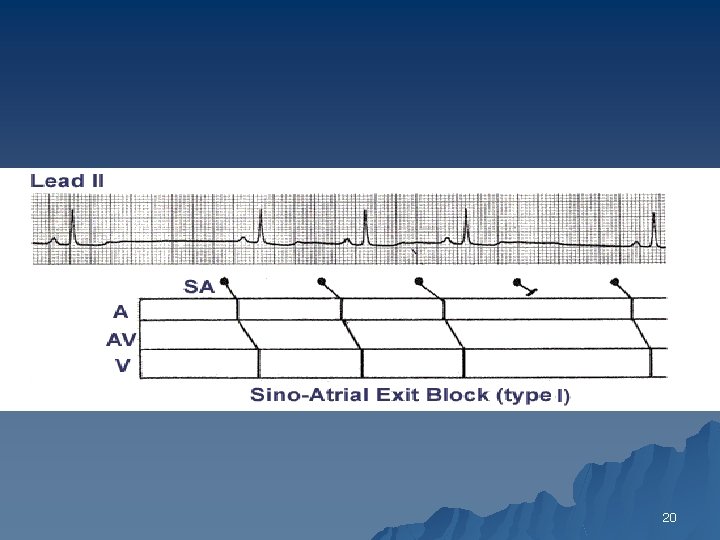
20

Second Degree Type II SA Block u PP intervals fairly constant (unless sinus arrhythmia present) until conduction failure occurs. u The pause is approximately twice the basic PP interval 21
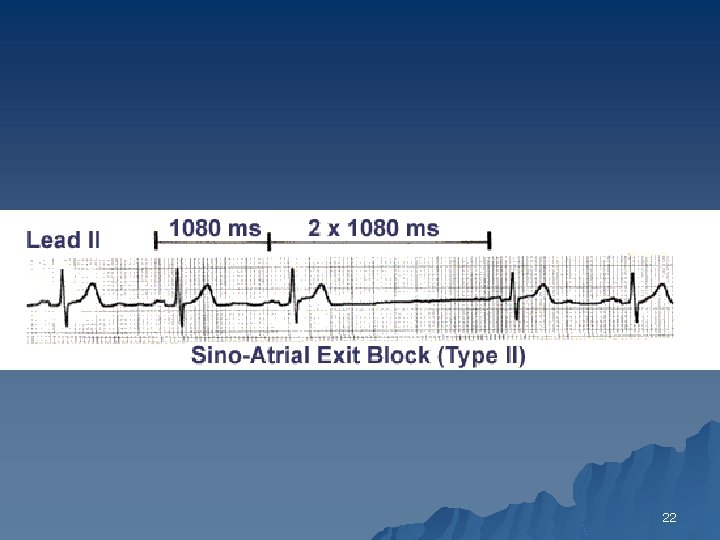
22

Third Degree Or Complete Sino Atrial Exit Block u May Cannot be distinguished from a prolonged sinus pause or arrest u According to below foci or escape rhythm ECG is variable! u Can be identified from direct recording of sinus node pacemaker activity during an EP study 23

Rosen Sinoatrial Block and Escape Rhythms u Incomplete SA block is diagnosed when an occasional P wave is dropped from the normal P-QRS-T sequence on the ECG. There are no P waves on the ECG complete SA block (sinus arrest). Usually, a lower pacemaker emerges in complete SA block; if this pacemaker is within the AV node, the QRS complex is narrow and results in an "idiojunctional“escape rhythm at a rate of 45 to 60 beats/min. u 24
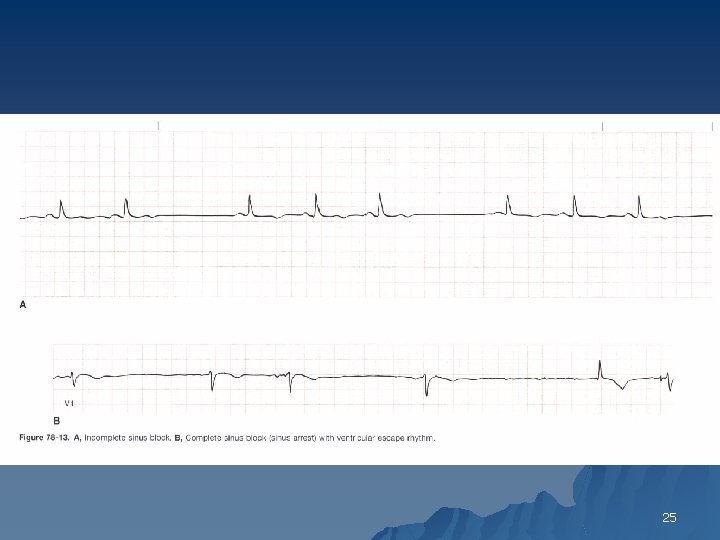
25

SA Block type 2 vs SA arrest? u Both u PP’ regular-irregular = 2 x PP >>> SA Block type 2 26

The pause is not equal to exactly two or more(3, 4, …) cardiac cycles of the underlying rhythm. 27
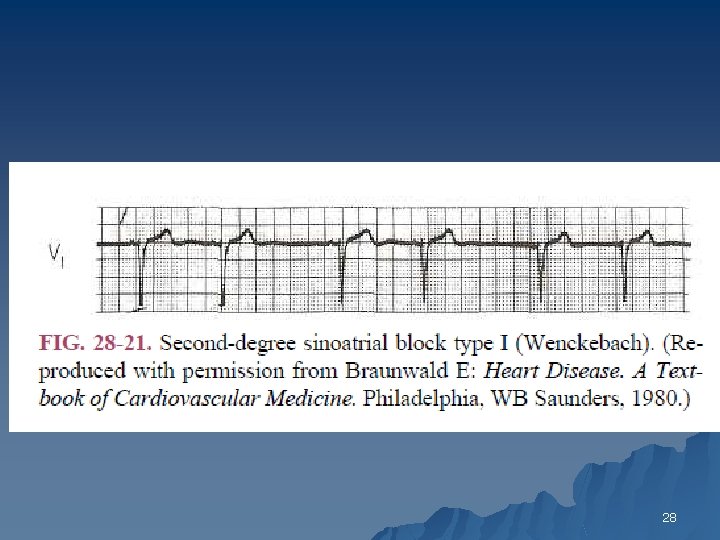
28
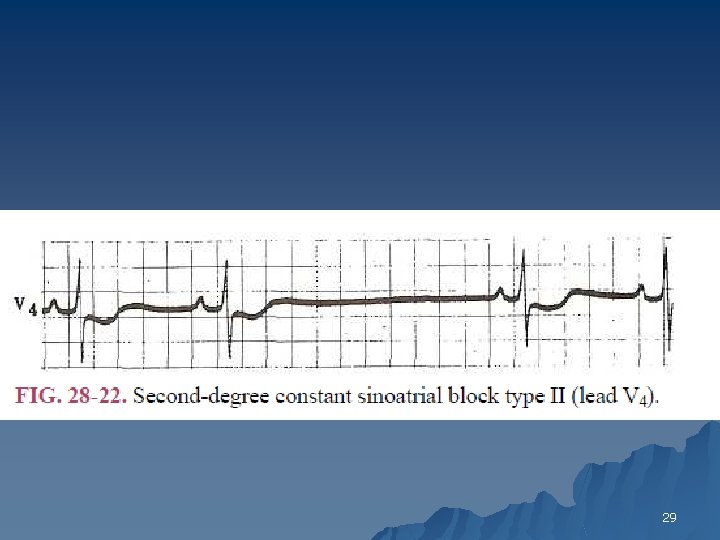
29

Dx u Regular-Irregular Or Irregular-Irregular u Regular-Irregular: SA Block type 2 or SA arrest PP’ = 2 x PP >>> SA Block type 2 u Irregular-Irregular: SA Block type 1 vs S. arrhythmia u 30
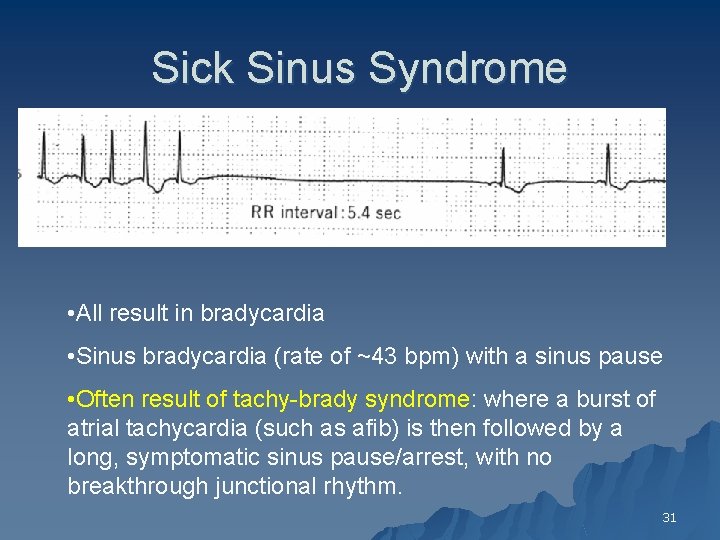
Sick Sinus Syndrome • All result in bradycardia • Sinus bradycardia (rate of ~43 bpm) with a sinus pause • Often result of tachy-brady syndrome: where a burst of atrial tachycardia (such as afib) is then followed by a long, symptomatic sinus pause/arrest, with no breakthrough junctional rhythm. 31
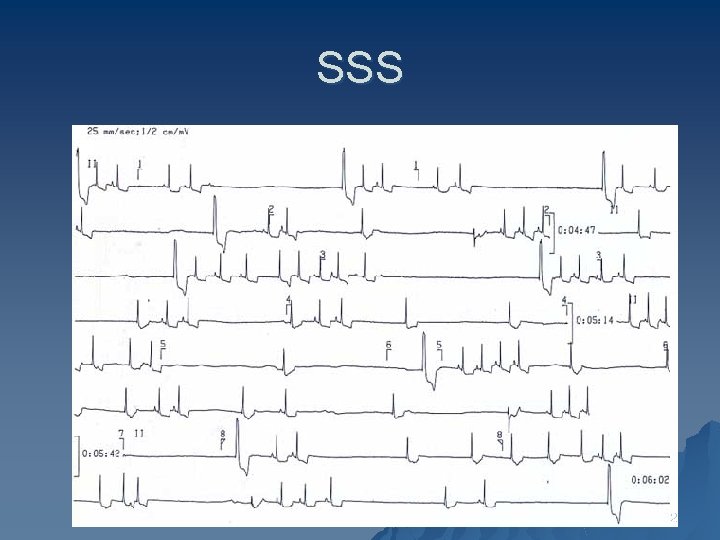
SSS 32

u Sick sinus syndrome is an indication for a permanent pacemaker. Pharmacologic treatment of atrial tachyarrhythmias carries the risk of aggravating preexisting AV block or sinus arrest. u Therefore, most patients should have pacemaker implantation before drug therapy is begun. 33
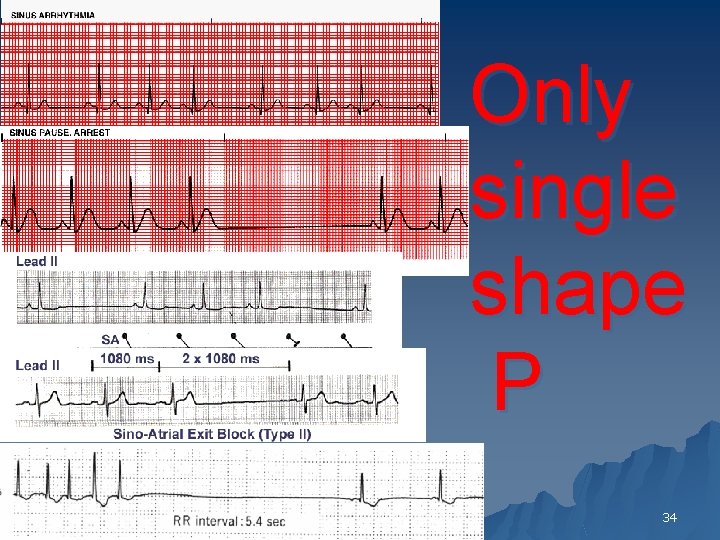
Only single shape P 34

Atrial Dysrhythmias Atrial dysrhythmias have ECG features similar to those of sinus dysrhythmias, u except u an atrial source serves as the pacemaker, producing P' waves that are different from the sinus P waves. u The P'R interval may also vary from the normal sinus PR interval, which distinguishes these rhythms. u 35
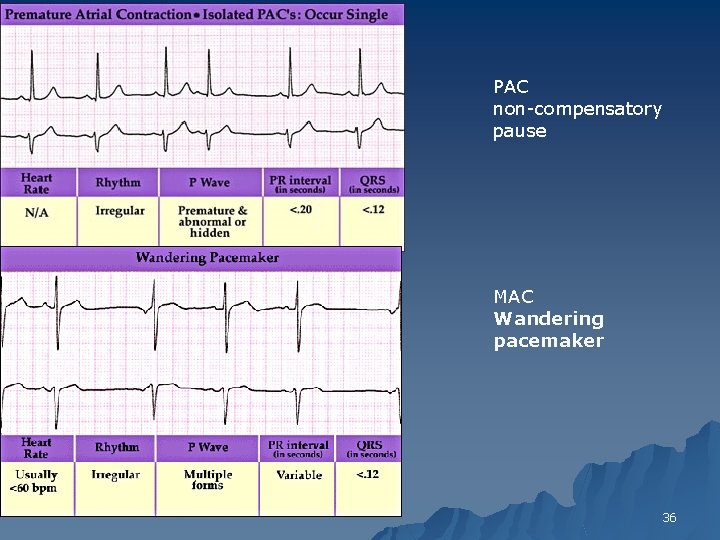
PAC non-compensatory pause MAC Wandering pacemaker 36
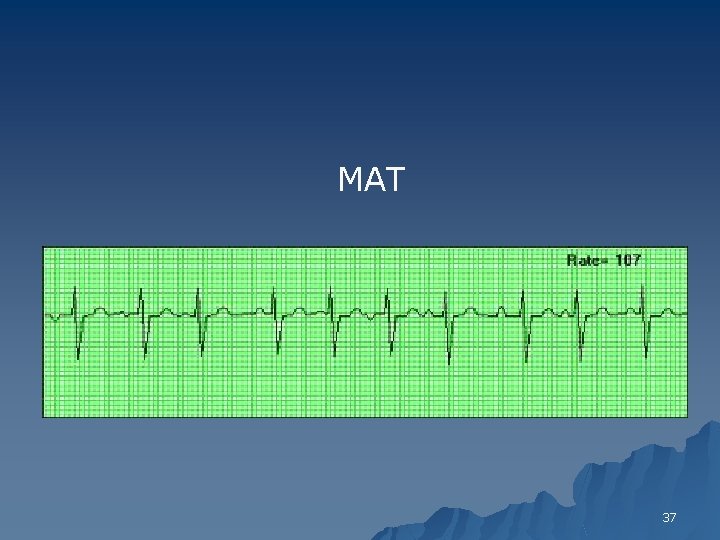
MAT 37

AV Blocks: Divided in to incomplete and complete block u Incomplete AV block includes a. first-degree AV block b. second degree AV block c. advanced AV block u Complete AV block, also known as third degree AV block 38

Location of the Block u Proximal to, in, or distal to the His bundle in the atrium or AV node u All degrees of AV blocks may be intermittent or persistent 39

First Degree AV Block u PR interval is prolonged 0. 210. 40 seconds, but no R-R interval change u Normal=0. 10”-0, 20” 40
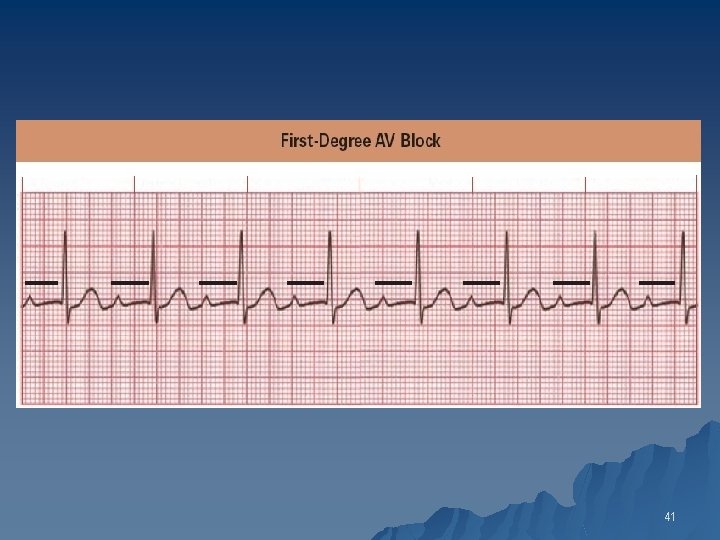
41
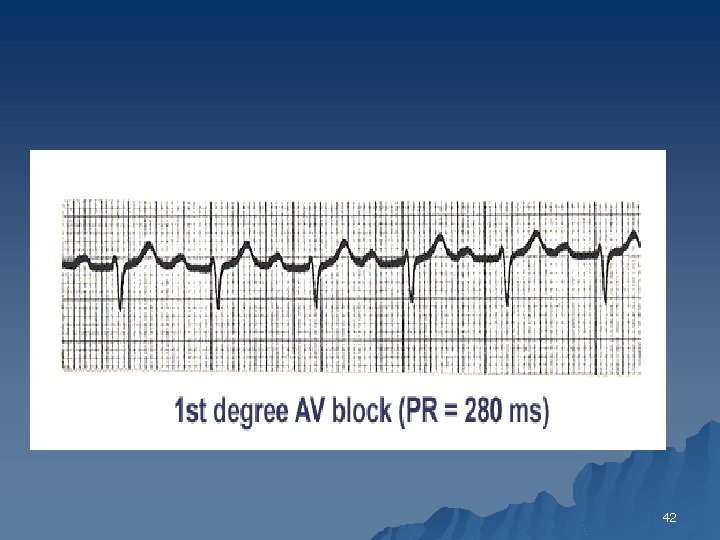
42

Second-Degree AV Block u u There is intermittent failure of the supraventricular impulse to be conducted to the ventricles Some of the P waves are not followed by a QRS complex. The conduction ratio (P/QRS ratio) may be set at 2: 1, 3: 2, 4: 3, and so forth 43

Types Of Second-Degree AV Block: I and II u Type I also is called Wenckebach phenomenon or Mobitz type I and represents the more common type u Type II is also called Mobitz type II 44

Type I Second-Degree AV Block: Wenckebach Phenomenon u ECG findings 1. Progressive lengthening of the PR interval until a P wave is blocked 2. Progressive shortening of the RR interval until a P wave is blocked 3. RR interval containing the blocked P wave is shorter than the sum of two PP intervals 45
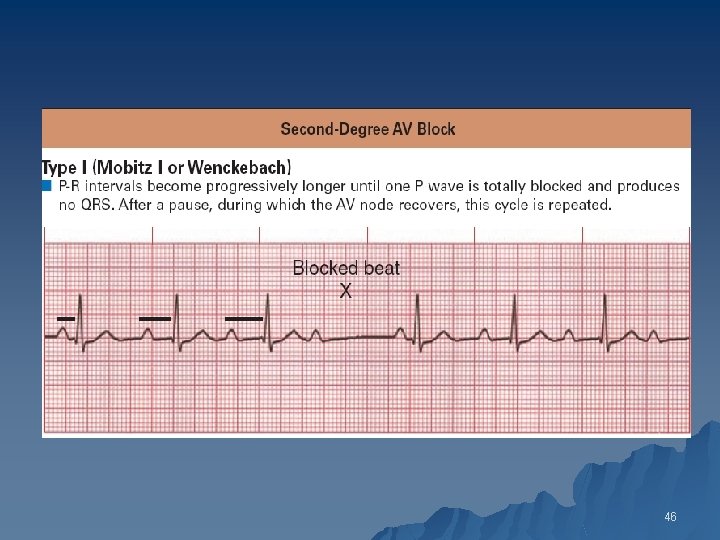
46

Type II Second-Degree AV Block: Mobitz Type II u ECG findings 1. Intermittent blocked P waves 2. PR intervals may be normal or prolonged, but they remain constant 3. When the AV conduction ratio is 2: 1, it is often impossible to determine whether the second-degree AV block is type I or II 4. A long rhythm strip may help 47
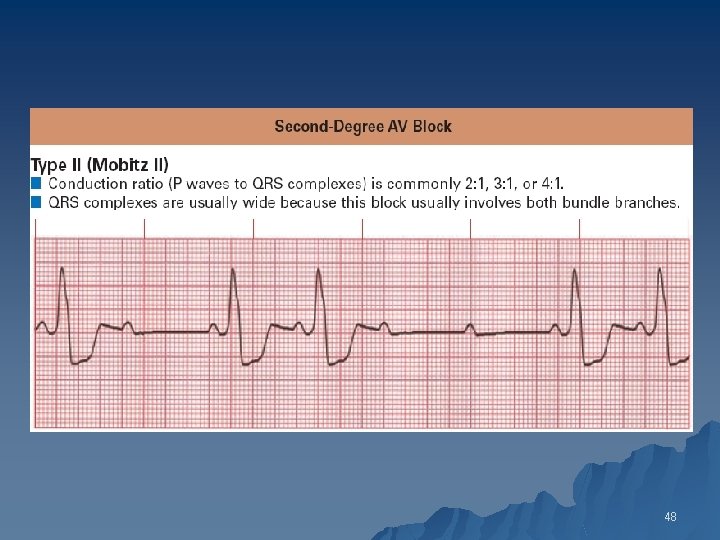
48
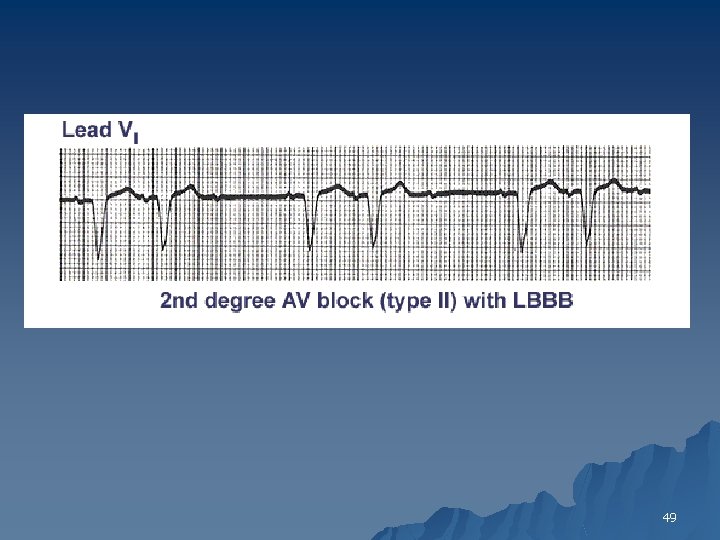
49

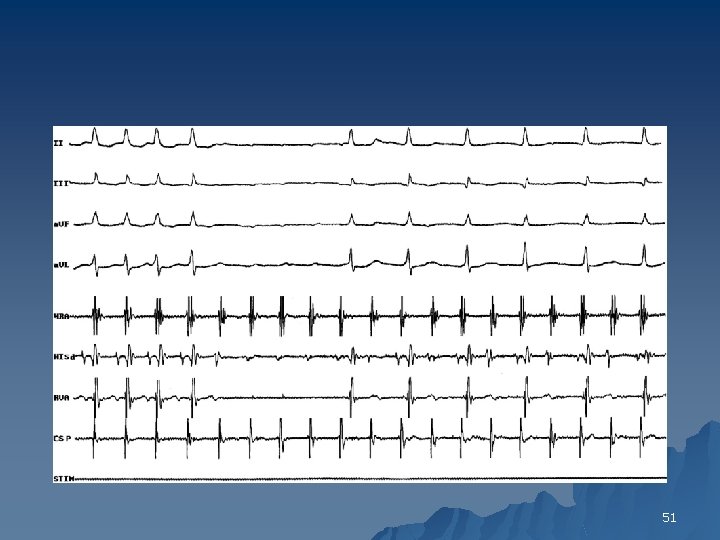
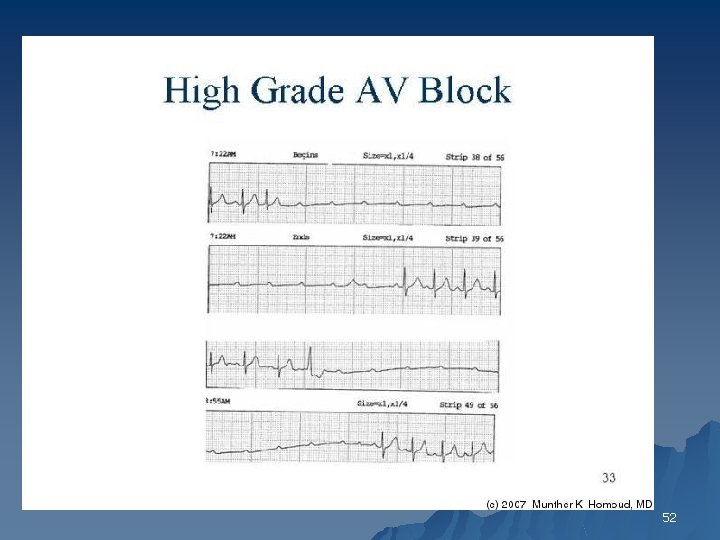
High-Grade or Advanced AV Block When the AV conduction ratio is 3: 1 or higher, the rhythm is called advanced AV blocked u A comparison of the PR intervals of the occasional captured complexes may provide a clue u If the PR interval varies and its duration is inversely related to the interval between the P wave and its preceding R wave (RP), type I block is likely u A constant PR interval in all captured complexes suggests type II block u 50
51
52

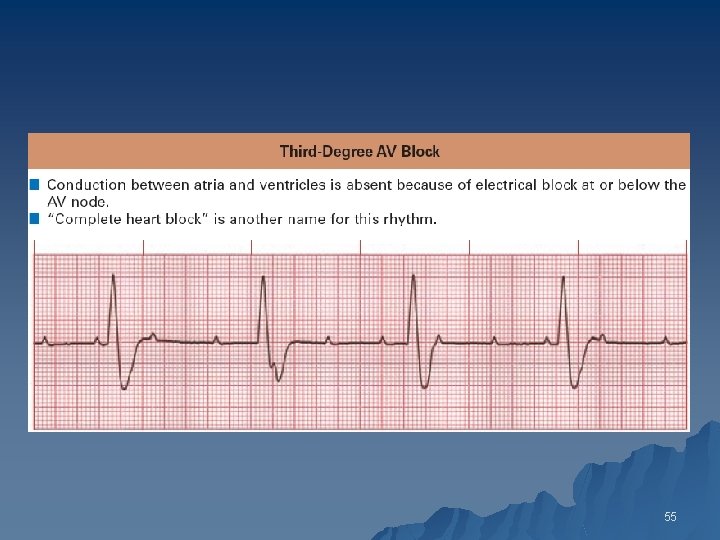
Complete (Third-Degree) AV Block u u There is complete failure of the supraventricular impulses to reach the ventricles The atrial and ventricular activities are independent of each other 53

ECG Findings u In patients with sinus rhythm and complete AV block, the PP and RR intervals are regular, but the P waves bear no constant relation to the QRS complexes 54
55
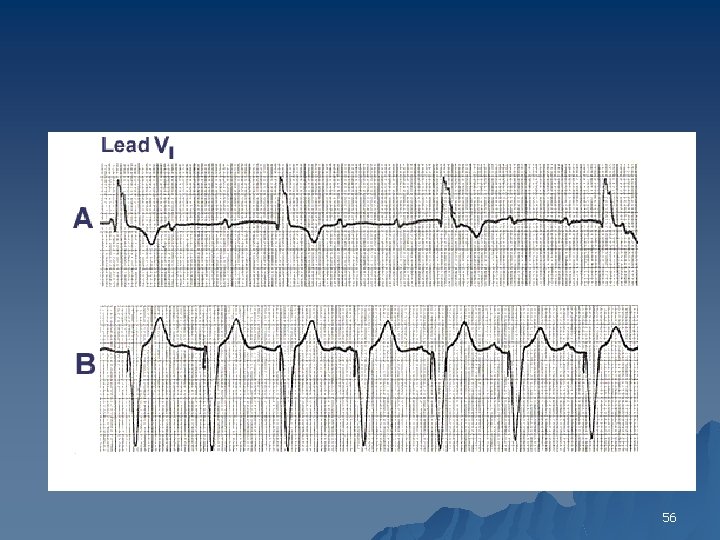
56

Bundle Branch Block Left Bundle Branch Block 1. Complete LBBB 2. Incomplete LBBB • Rigt Bundle Branch Block 1. Complete RBBB 2. Incomplete RBBB • 57

Left Bundle Branch Block Criteria 1. The QRS duration is > 120 ms 2. Leads V 5, V 6 and AVL show broad and notched or slurred R waves 3. With the possible exception of lead AVL, the Q wave is absent in left-sided leads 4. Reciprocal changes in V 1 and V 2 5. Left axis deviation may be present Deep S in V 1 no R in. V 1 & R in V 6 no S in V 6 58
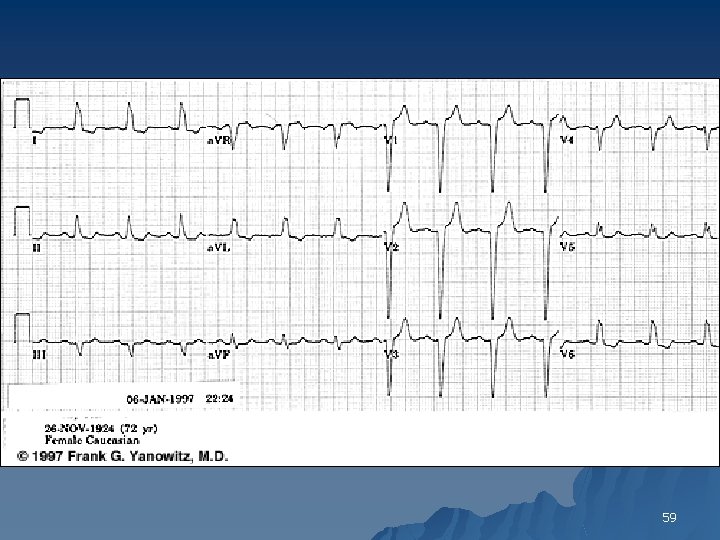
59
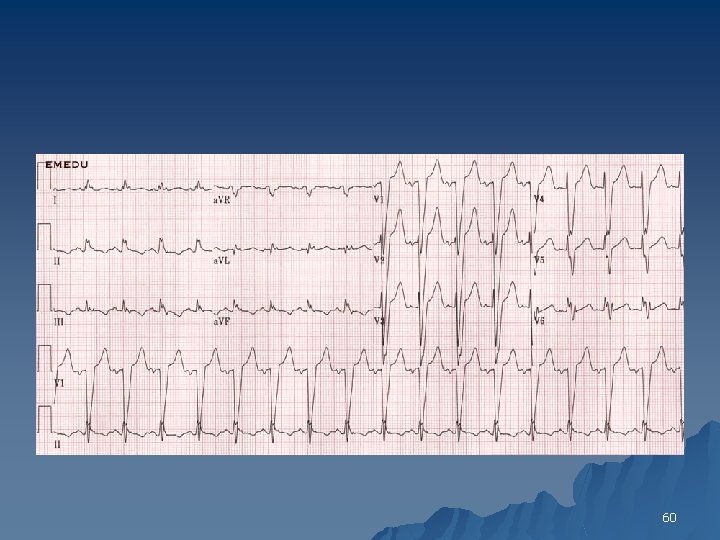
60
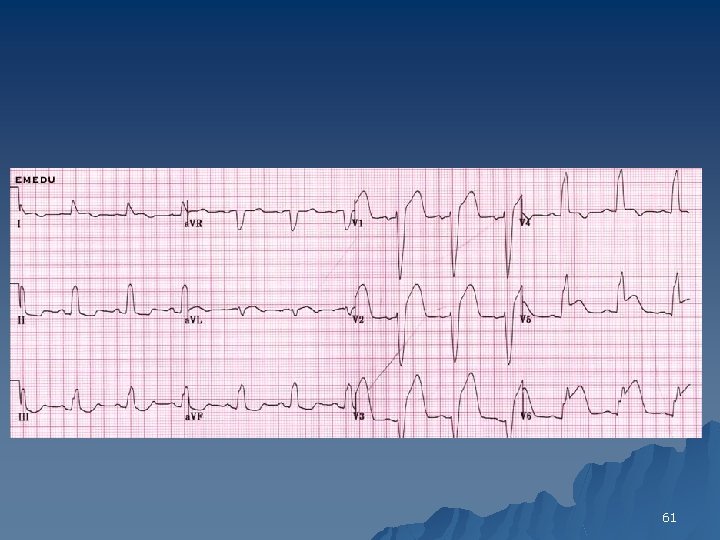
61

Right Bundle Branch Block u The diagnostic criteria include 1. QRS duration is >120 ms 2. An rsr’, rs. R’ or r. SR’ pattern in lead V 1 or V 2 and occasionally a wide and notched R wave. 3. Reciprocal changes in V 5, V 6, I and AVL 62
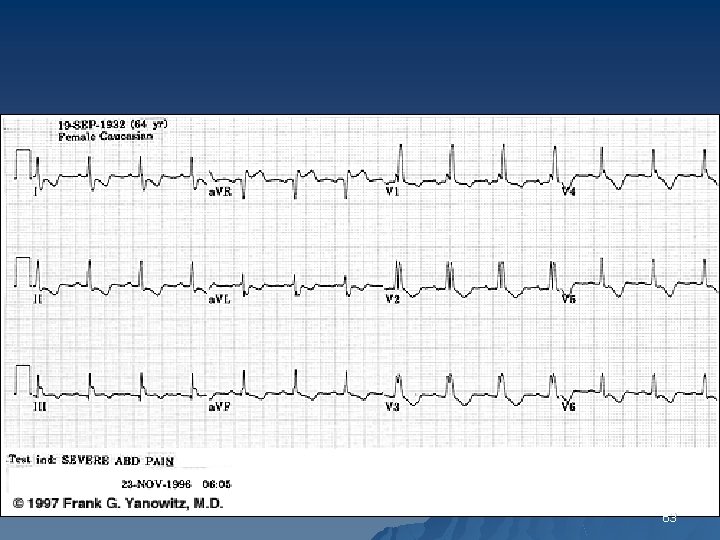
63
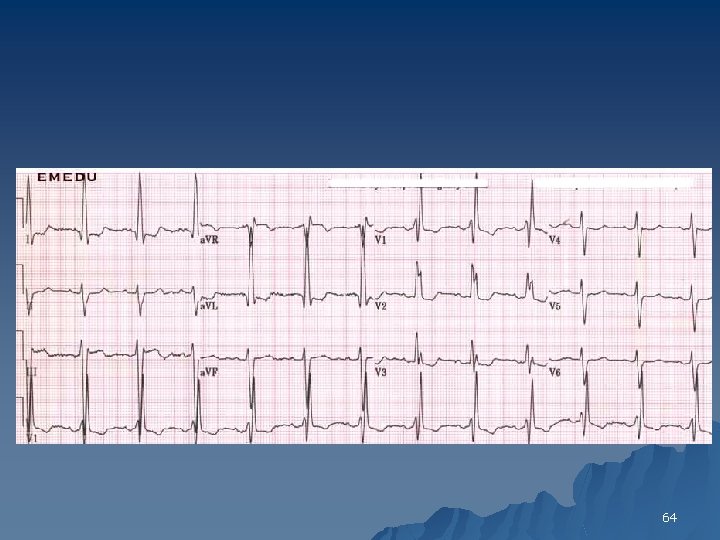
64
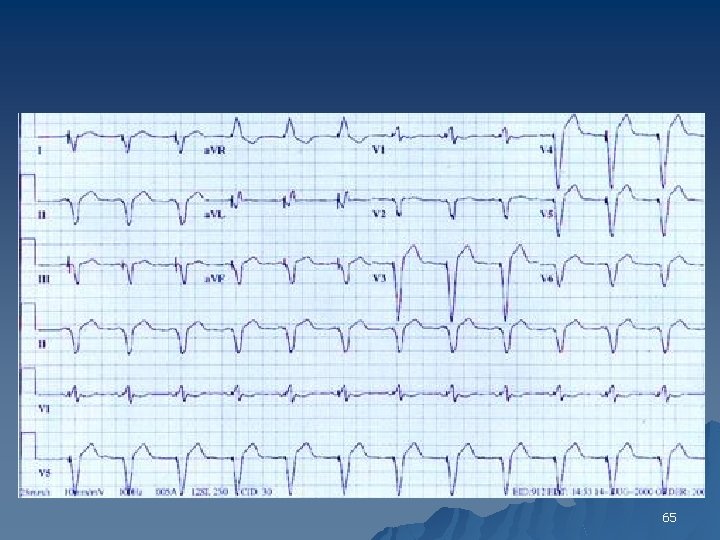
65

Incomplete RBBB u Criteria for incomplete RBBB are the same as for complete RBBB except that the QRS duration is < 120 ms 66
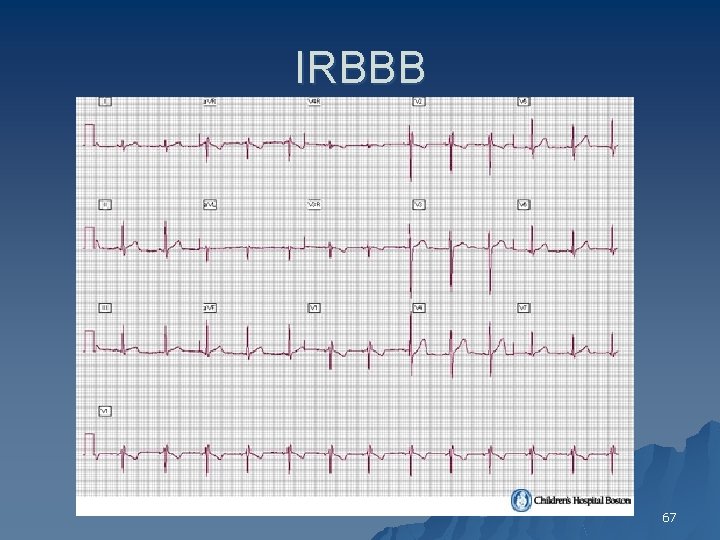
IRBBB 67

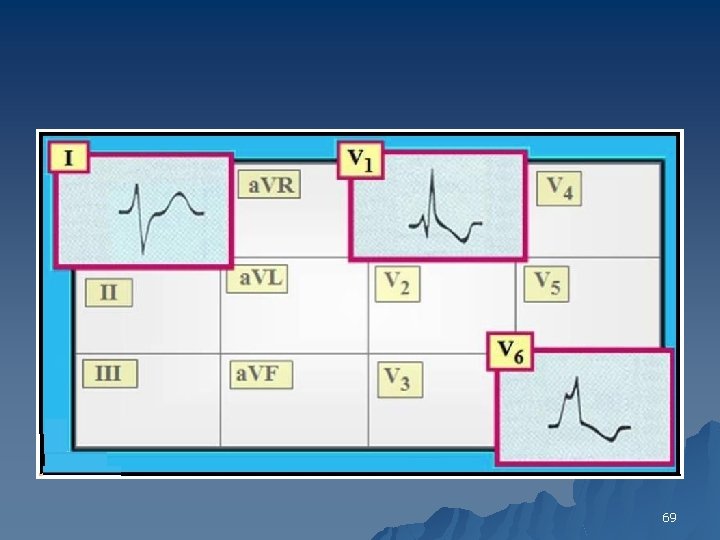
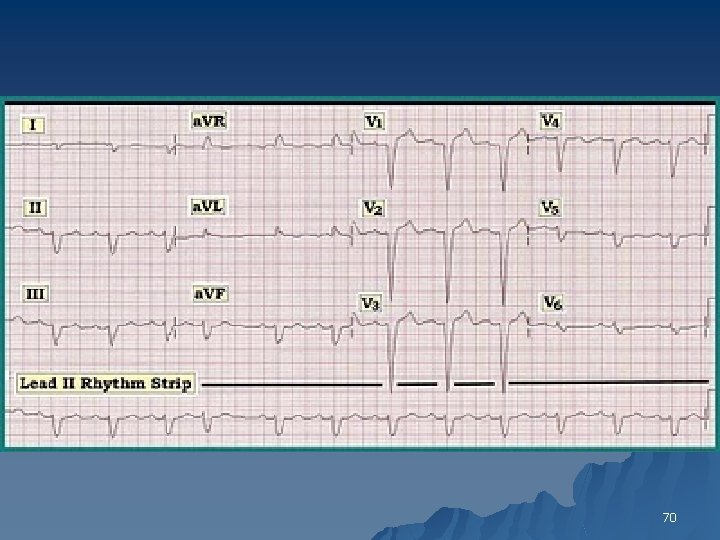
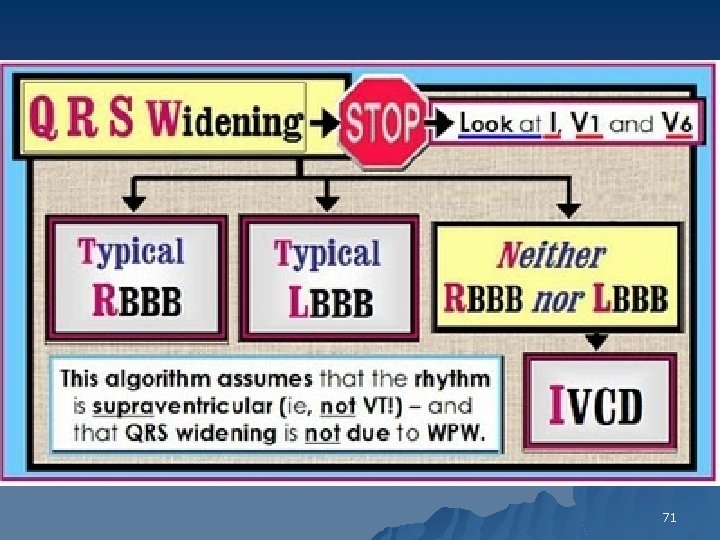
interventricular conduction delay IVCD u Nonspecific Intraventricular Conduction Defects (IVCD) QRS duration >0. 10 s indicating slowed conduction in the ventricles Criteria for specific bundle branch or fascicular blocks not met 68
69
70
71

u bilateral bundle branch block (BBBB) interruption of cardiac impulses through both bundle branches, clinically indistinguishable from third degree (complete) heart block. 72

Fascicular Blocks u The left bundle branch divides into two fascicles 1. Superior and anterior 2. Inferior and posterior 73

Types Of Fascicular Block Left anterior fascicular block u Left posterior fascicular block u Bifascicular Block u Trifascicular Block u 74
Left Anterior Fascicular Block u Left axis deviation , usually -45 to -90 degrees u QRS duration usually <0. 12 s unless coexisting RBBB u Poor R wave progression in leads V 1 -V 3 and deeper S waves in leads V 5 and V 6 u There is RS pattern with R wave in lead II > III S wave in lead III > lead II u u u QR pattern in lead I and AVL, with small Q wave No other causes of left axis deviation 76
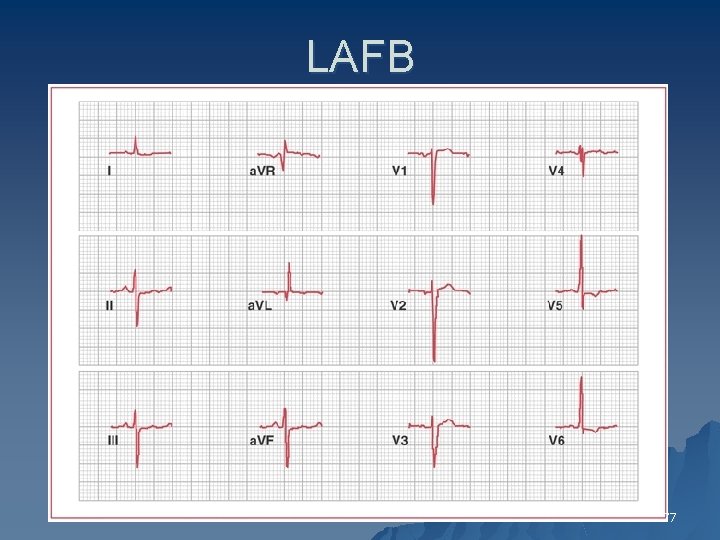
LAFB 77
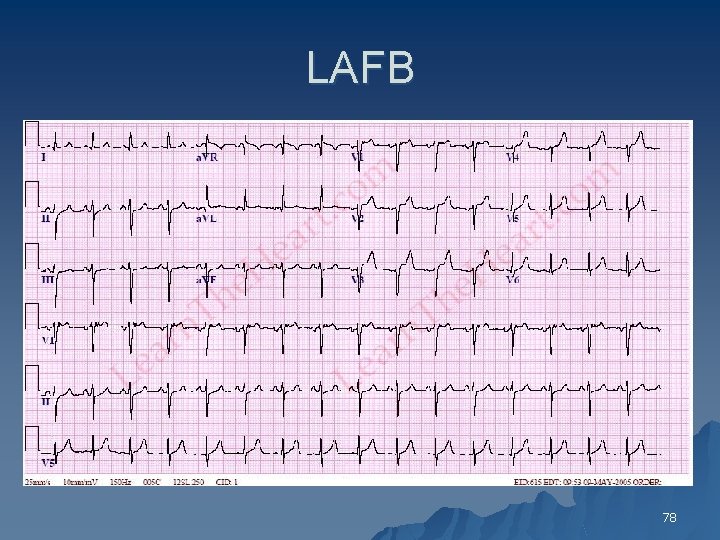
LAFB 78
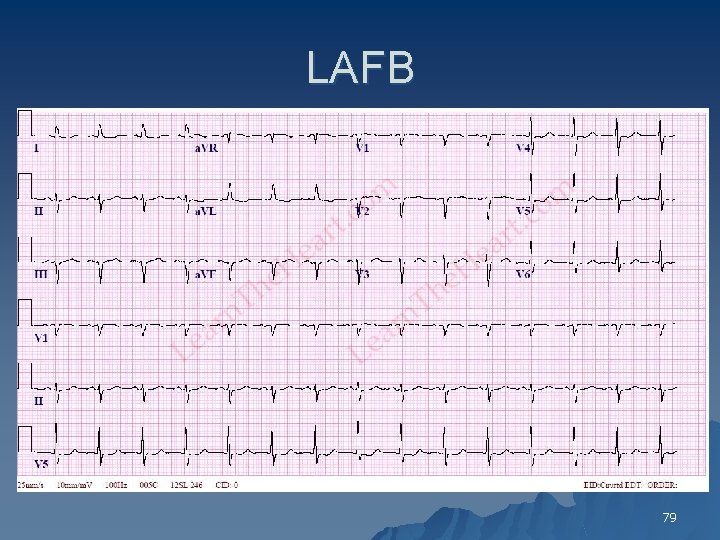
LAFB 79

Left Posterior Fascicular Block u Diagnostic Criteria include 1. QRS duration <120 ms 2. No ST segment or T wave changes 3. Right axis deviation (100 degree) 4. QR pattern in inferior leads (II, III, AVF) small q wave 5. RS patter in lead I and AVL(small R with deep S) 6. No other causes of right axis deviation 80
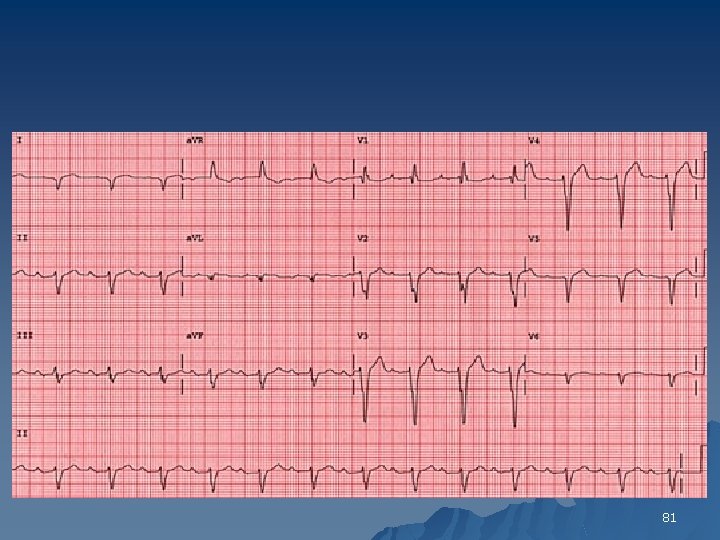
81
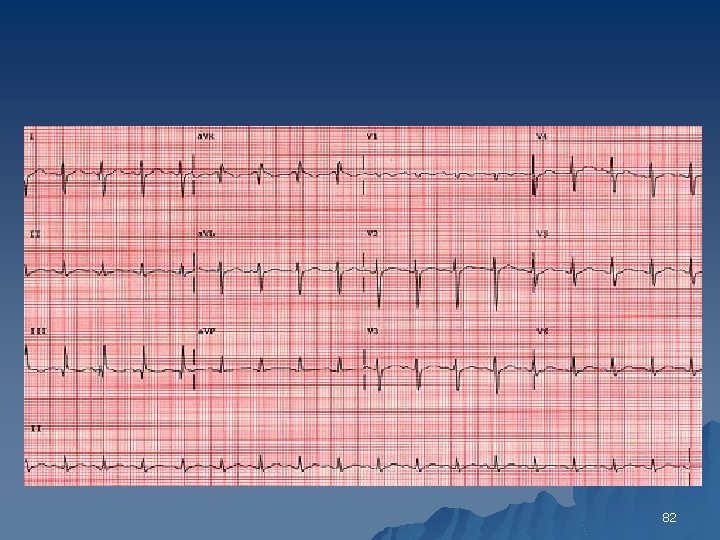
82
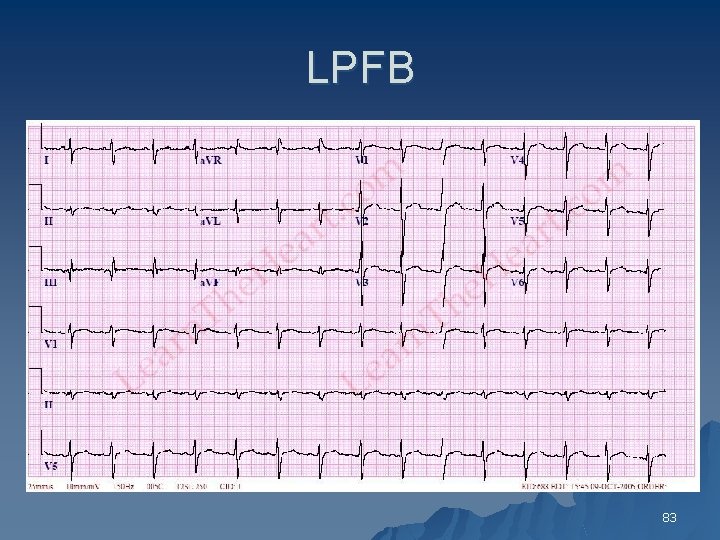
LPFB 83

Bifascicular Bundle Branch Block RBBB + LAFB RBBB + LPFB LBBB LAFB + 1 st degree AV LPFB + 1 st degree AV 84
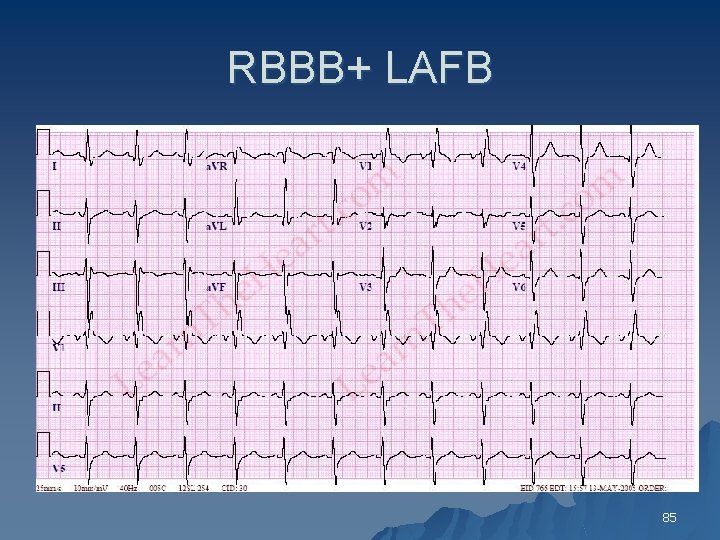
RBBB+ LAFB 85
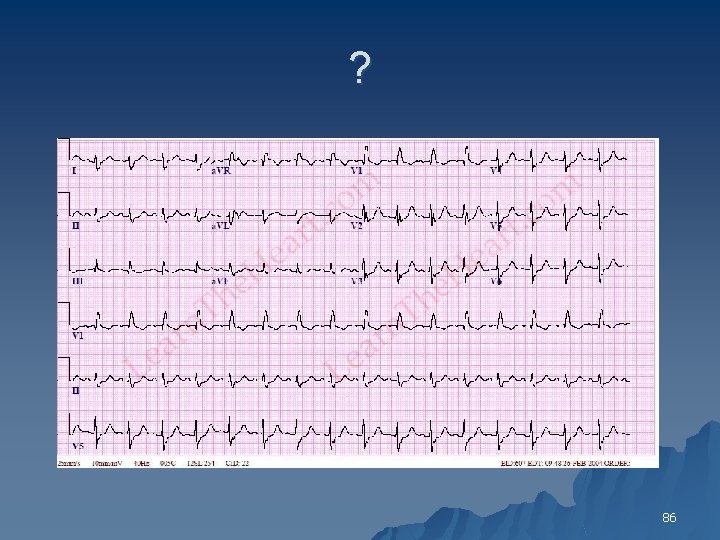
? 86
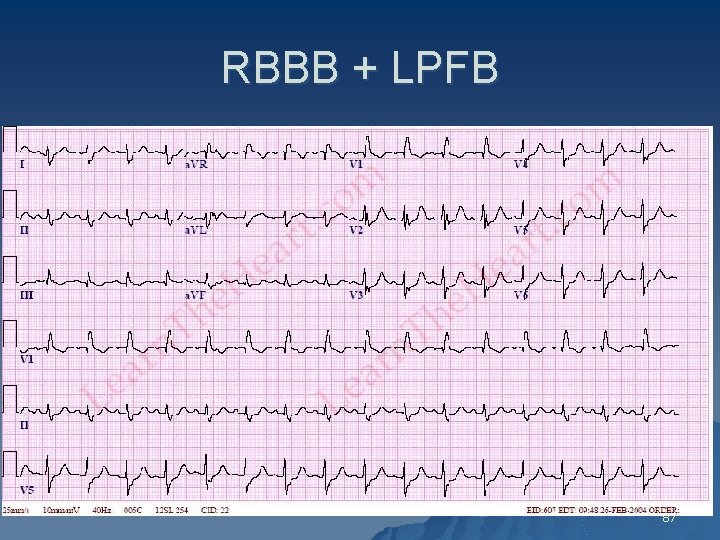
RBBB + LPFB 87
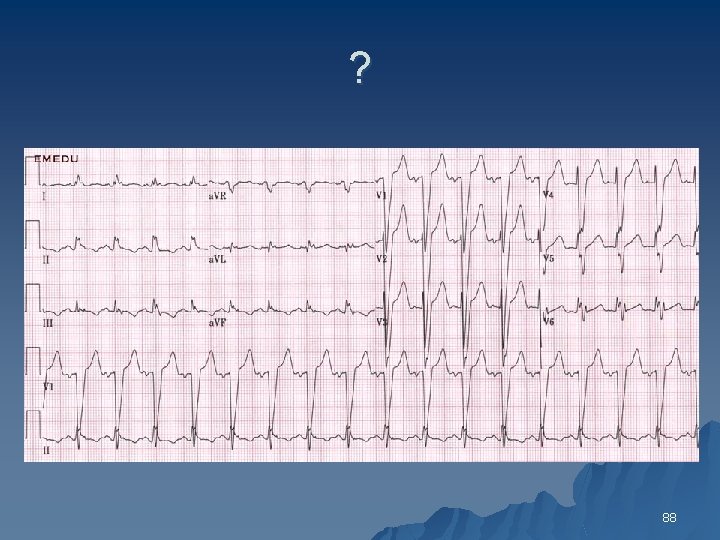
? 88

Trifascicular Block LBBB + 1 st degree AV RBBB + LAFB/LPBF +1 st degree AV 89
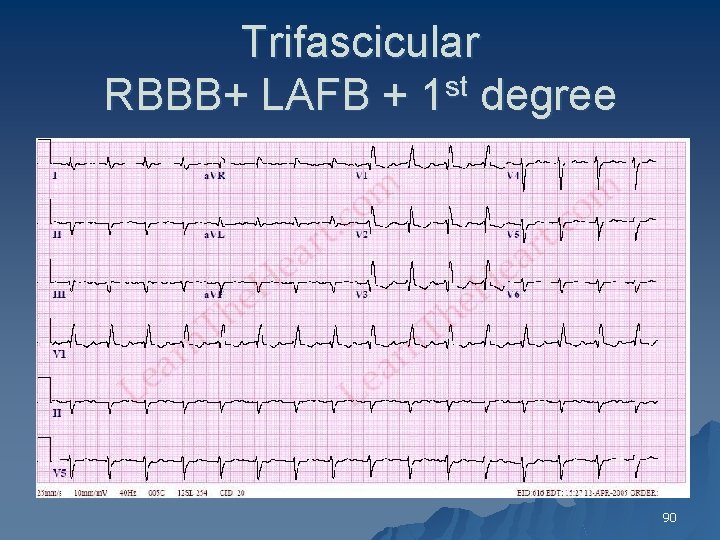
Trifascicular RBBB+ LAFB + 1 st degree 90
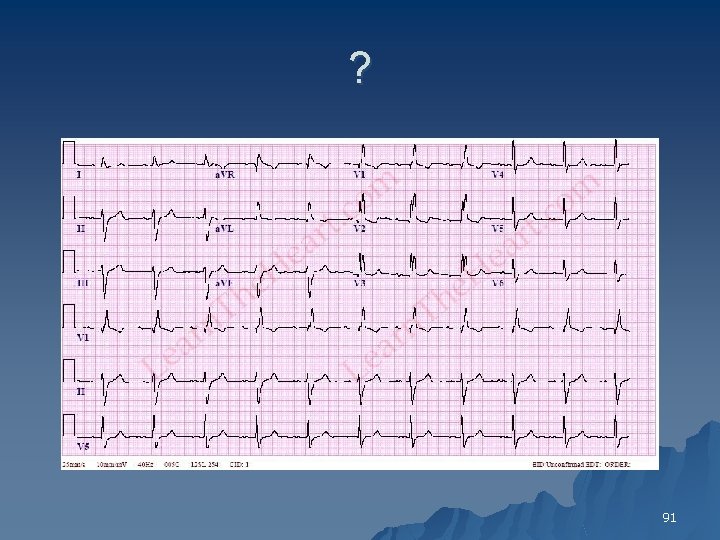
? 91
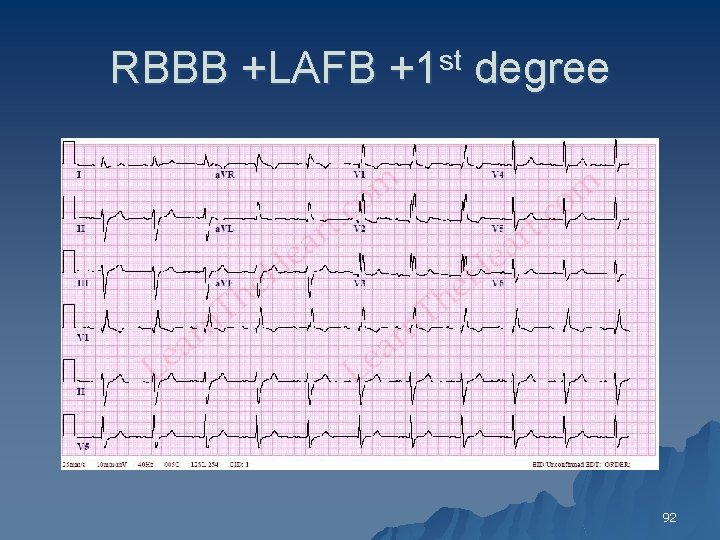
RBBB +LAFB +1 st degree 92

Indications for Permanent Pacing in Chronic Bifascicular and Trifascicular Block 1. Class I u Intermittent third-degree AV block. (B) u Type II second-degree AV block. (B) 2. Class IIa u Syncope not proved to be due to AV block when other likely causes have been excluded, specifically ventricular tachycardia (VT). (B) 3. Class III u Fascicular block without AV block or symptoms. (B) u Fascicular block with first-degree AV block without symptoms. (B) 97
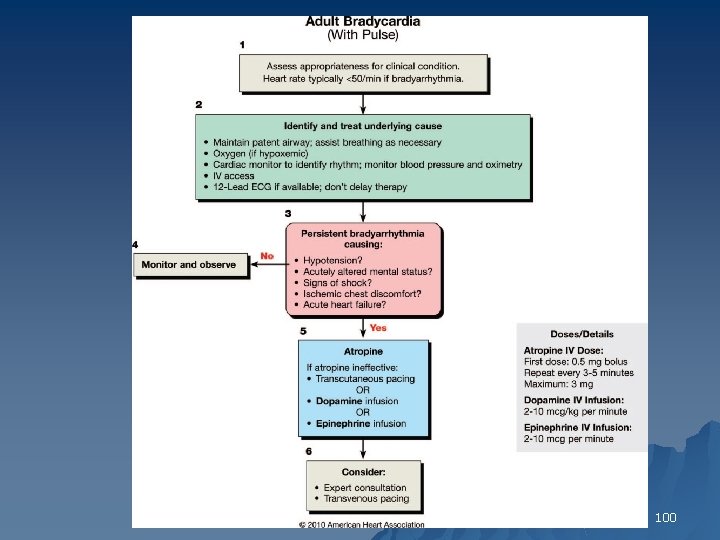
100

101

102

Atropine will likely be ineffective in patients who have undergone cardiac transplantation because the transplanted heart lacks vagal innervation. 103

104

Tintinalli u As patients with atrial fibrillation can have a physiologic rate response to trauma, sepsis, and other disease process, other causes of hypotension should be investigated before concluding that the rate is causing the hemodynamic deterioration. 105
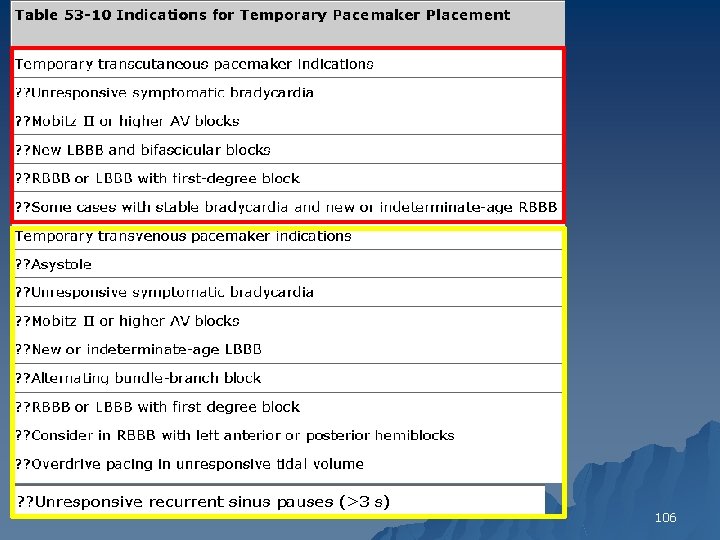

106

107
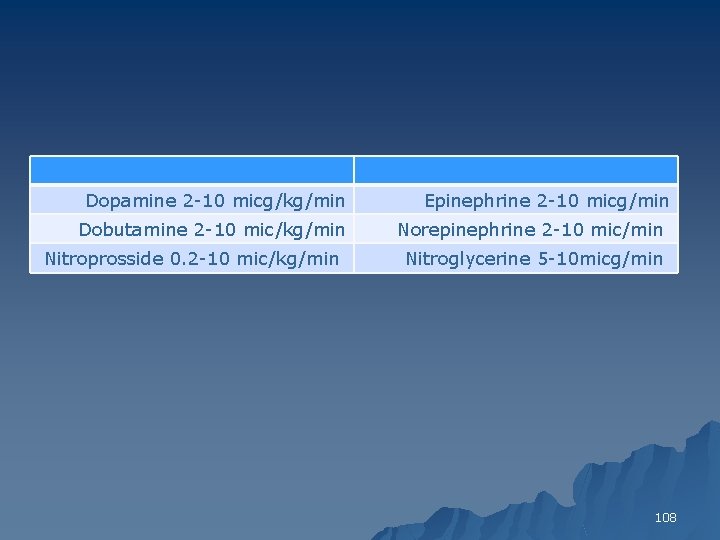

Dopamine 2 -10 micg/kg/min Dobutamine 2 -10 mic/kg/min Nitroprosside 0. 2 -10 mic/kg/min Epinephrine 2 -10 micg/min Norepinephrine 2 -10 mic/min Nitroglycerine 5 -10 micg/min 108
- Slides: 101