1 Clostridium Anaerobic Endospore formers Filename Clostridium ppt

1 Clostridium: Anaerobic Endospore formers Filename: Clostridium. ppt 12/6/2020

2 Clostridial Diseases ä Botulism C. botulinum ä Tetanus C. tetani ä Gas gangrene C. perfringens ä Food poisoning Clostridium spp ä Pseudomembranous colitis C. difficile 12/6/2020

3 Clostridium ä Gram positive ä Rods ä Endospore formers ä asporogenous ä Obligate Anaerobes!!! ä Aerotolerant spp C. perfringens, C. tetani, C. botulinum, C. difficile ä Soil organisms 12/6/2020

4 Botulism ä Intoxication ä Foods ä Meats ä Fish ä low-medium acid canned foods ä Wild birds (limberneck) ä ducks, fish, Inuit -- whale blubber, seal fins 12/6/2020

5 Botulism: symptoms ä Adults ä Nerve paralysis ä ä ä ä shorter nerves first Blurred vision Cardiac failure Respiratory failure Intoxication Infants ä ä ä Failure to Thrive Dehydration Polyneuropathy Infection Cl. Botulinum ä umbilical cord 12/6/2020

6 Botulism: Symptoms 1 st symptoms: weakness and dizziness soon after: blurred vision (double vision), difficulty swallowing, throat pain, constipation, abdominal pain Flaccid paralysis: Bilateral, descending, weakness of the peripheral muscles. Death: respiratory paralysis 12/6/2020
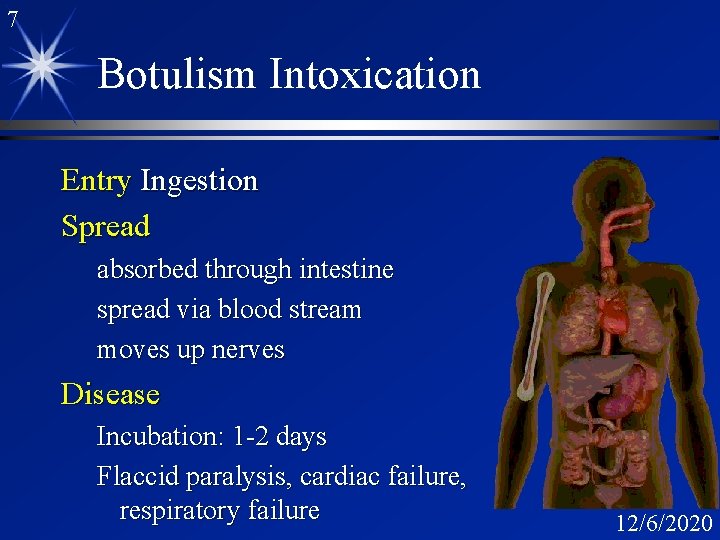
7 Botulism Intoxication Entry Ingestion Spread absorbed through intestine spread via blood stream moves up nerves Disease Incubation: 1 -2 days Flaccid paralysis, cardiac failure, respiratory failure 12/6/2020

8 Botulism: Treatment Disease is progressive may not respond to treatment. -ventilatory support -gastric lavage -penicillin -antitoxin (polyvalent A, B, E) Heat food to 80 C to kill toxin and kill spores. 12/6/2020

9 Infant Botulism ä Infant botulism: Colonizes the GI tract of young infants. Appears as non-specific weakness. ä Flaccid paralysis: respiratory arrest. ä Mortality = 1 -2% ä Some cases of sudden infant death syndrome have proven to be botulism. Eating honey. 12/6/2020

10 Wound botulism: rare -- organisms multiply in the wound. ä Can occur through umbilical cord ä 12/6/2020

11 Botulism: Lab Diagnosis Culture: culture organisms from feces, food. Heat to 80 C. Food, stool and patient’s serum. Toxin Assay: mix one portion of each specimen with antitoxin. Keep one portion antitoxin free. 12/6/2020

12 Botulism Toxin Potent neurotoxin regulated by bacteriophage. Toxins: A -- E, C alpha, C beta, F, G Humans: A, B, E 150 Kd protein -- cleaved 12/6/2020
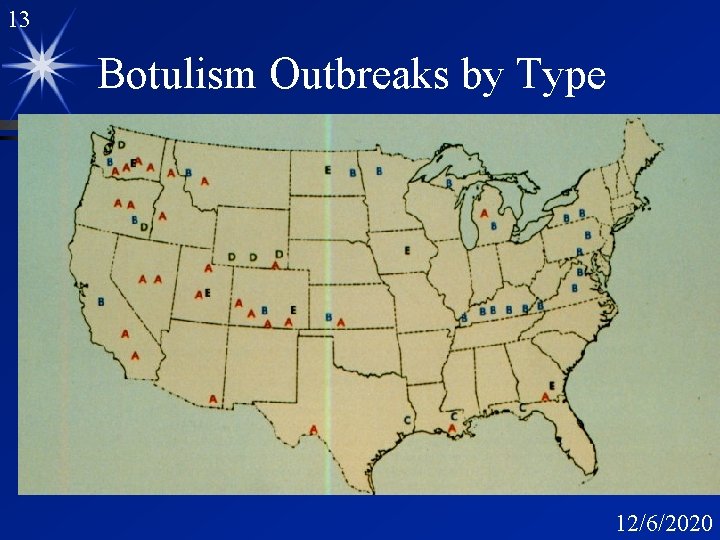
13 Botulism Outbreaks by Type 12/6/2020

14 INCIDENCE Botulism Intoxication in USA YEAR 12/6/2020

15 INCIDENCE Botulism in USA; neonates YEAR 12/6/2020
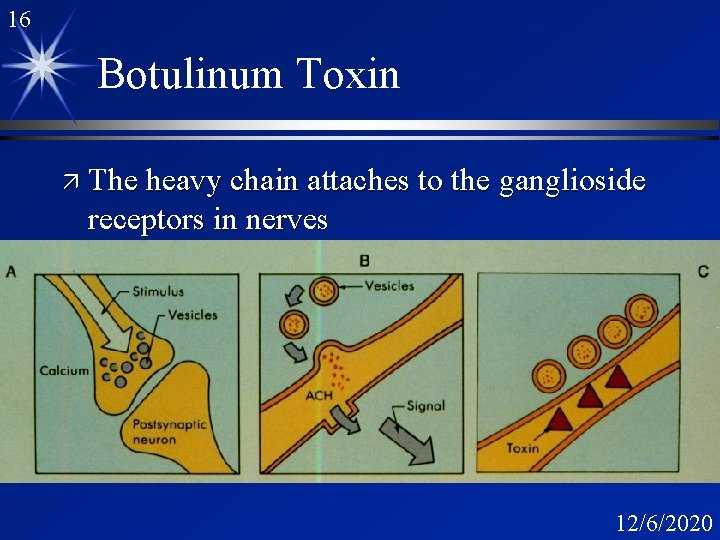
16 Botulinum Toxin ä The heavy chain attaches to the ganglioside receptors in nerves 12/6/2020

17 C. botulinum toxin Synaptic activity at cholinergic synapses is mediated by acetylcholine. Acetylcholine is rapidly hydrolysed by acetylcholine esterase. The result is an electrical stimulus. 12/6/2020

18 Sequence of Events A. Nerve stimulus -- calcium is stimulated B. Acetylcholine release into the synaptic space -moves into post synaptic membrane and acts on specific receptors. C. Botulinum toxin interferes with the release of acetylcholine from the synaptic vesicles. 12/6/2020

19 Tetanus 12/6/2020

20 C. tetani looks like a tennis racket. Found in soil, carried by horses. Toxin: heat labile, 150, 000 d peptide Neurotoxin: splits carboxy terminal to gangliosides on neuronal membranes. Moves to CNS by retrograde axonal transport. 12/6/2020
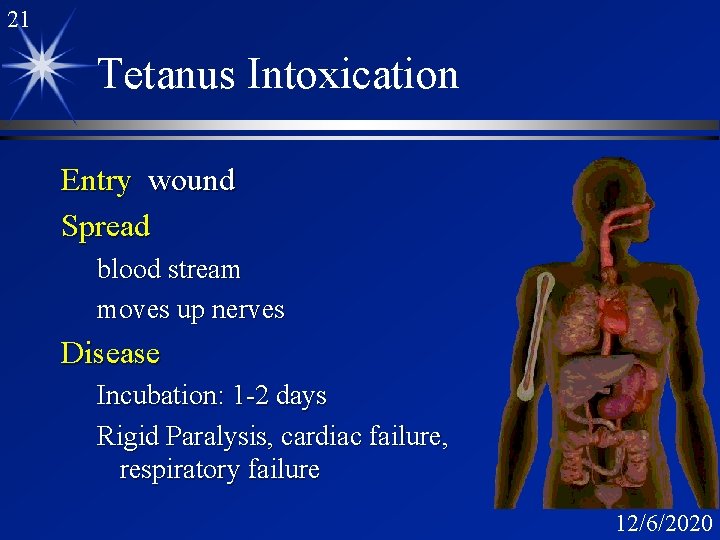
21 Tetanus Intoxication Entry wound Spread blood stream moves up nerves Disease Incubation: 1 -2 days Rigid Paralysis, cardiac failure, respiratory failure 12/6/2020

22 Lockjaw 12/6/2020
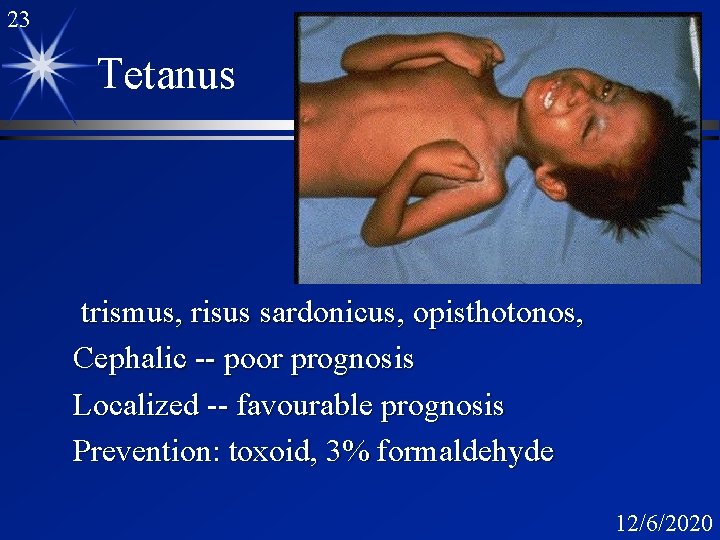
23 Tetanus trismus, risus sardonicus, opisthotonos, Cephalic -- poor prognosis Localized -- favourable prognosis Prevention: toxoid, 3% formaldehyde 12/6/2020

24 Risus sardonicus 12/6/2020
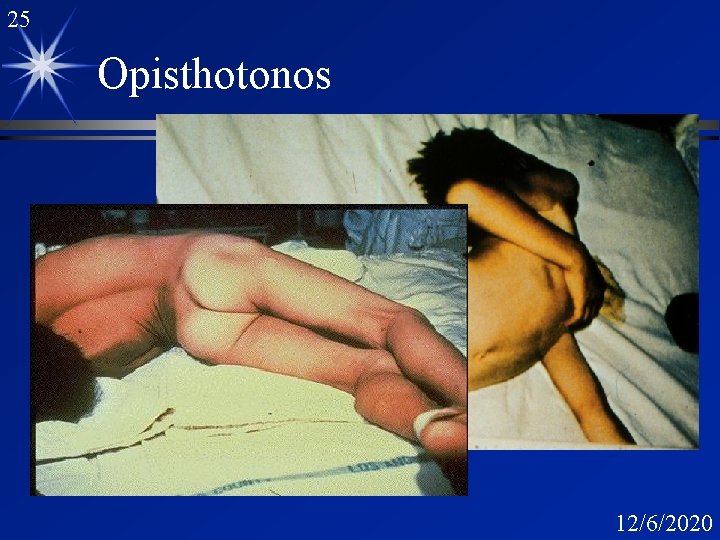
25 Opisthotonos 12/6/2020

26 Tetanus Neonatorum 12/6/2020
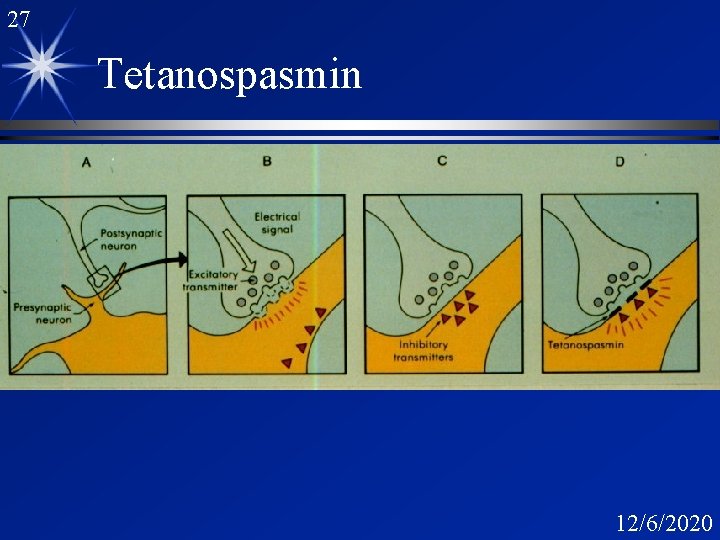
27 Tetanospasmin 12/6/2020

28 Toxin similarity ä Clostridium botulinum and C. tetani are Zn requiring Endopeptidases that cleave a set of proteins. . Synaptobrevins found in synaptic vesicles of neurons Interfere with release of neurotransmitters and the normal inhibitory function. 12/6/2020

29 Binding regions of tetanus toxin and botulinum toxin are different in terms of cell specificity. 12/6/2020

30 Tetanus Distribution 12/6/2020
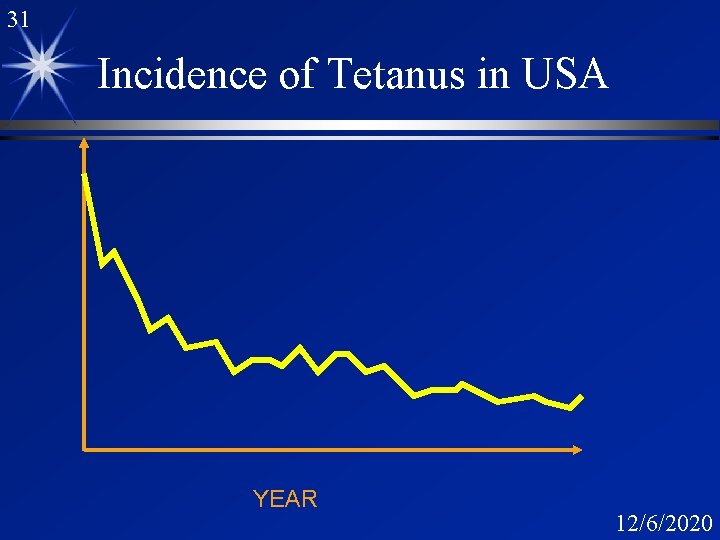
31 Incidence of Tetanus in USA YEAR 12/6/2020

32 C. perfringens: Diseases 4 bacteremia 4 myonecrosis 4 gas gangrene 4 cellulitis 4 fascitis 4 food poisoning: enteritis necroticans 12/6/2020

33 C. perfringens ä large rectangular, hemolytic, very distinctive spreading colonies. ä target hemolysis ä found in soil and intestines, man and animals 12/6/2020

34 C. perfringens toxins ä Alpha toxin is a lecithinase (phospholipase C) ä lyses erythrocytes, platelets, leucocytes, endothelial cells ä Massive hemolysis and tissue destruction ä Theta Toxin- Beta hemolysis- increases permeability-- necrotizing enterocolitis ä Delta -- hemolysis ä Kappa -- collagenase 12/6/2020

35 C. perfringens toxins Mu -- hyaluronidase ä Nu -- DNAase Lambda toxin -- protease Neuraminidase -- hydrolyses serum glycoproteins Enterotoxin -- reverses water, sodium and chloride transport in the intestine (like V. cholerae) Produced by Group A. ä 12/6/2020

36 Nagler Reaction ä Presumptive identification of C. perfringens ä alpha toxin (lecithinase) hydrolyses phospholipids ä egg yolk agar becomes turbid ä specifically blocked by antitoxin 12/6/2020

37 Nagler Reaction blocked by Antibodies 12/6/2020

38 12/6/2020

39 Clinical Syndromes: Bacteremia - usually transient, only diagnostic with other clinical symptoms Myonecrosis - gas gangrene - trauma or surgical contaminant 12/6/2020
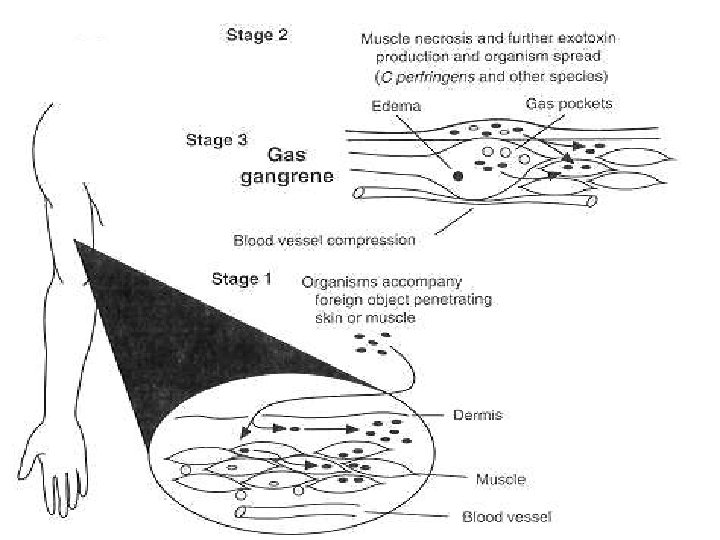
40 Gas Gangrene Entry Penetrating. Wound Multiplication in dead anaerobic tissue Toxin production hemolysin, proteases, lipase, collagenase Disease necrosis, edema, gas 12/6/2020
41 12/6/2020

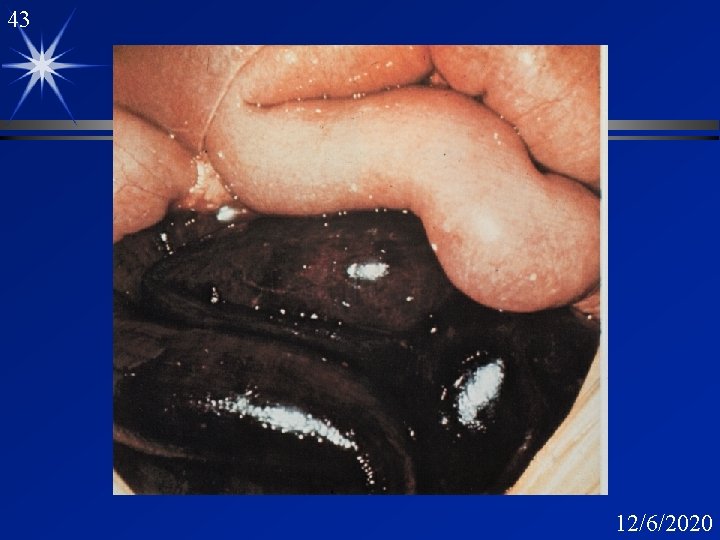
42 C. perfringens Gas gangrene Incubation: <1 week pain severe muscle necrosis shock renal failure death -crepitant -cellulitis & fascitis (no muscle) 12/6/2020
43 12/6/2020

44 C perfringens Food poisoning incubation 8 -24 hrs. Abdominal cramps, watery diarrhea lasts less than 24 hrs. Contaminated meat (left overs) 12/6/2020

45 C. difficile Gram + anaerobic rod. -found in normal flora -ultimate opportunistic pathogen -difficult to determine cause as the organism is ubiquitous -not difficult to culture 12/6/2020

46 C. difficile Diagnosis: cytotoxin - stool culture C. difficile antigen -- latex agglutination 12/6/2020

47 Cytotoxin slurry of stool centrifuged filter through 0. 45 u filter 0. 1 ml - supernatant to buffer at p. H 7. 2 WI-38 tissue cells human diploid lung fibroblasts Add supernatant to tissue culture. Observe for cytotoxicity 24 hrs. 12/6/2020

48 Mechanism of pathogenicity: Toxin A enterotoxin hypersecretion of fluid Toxin B cytotoxin cytopathic to tissue monolayers 12/6/2020

49 C. difficile. Treatment: stop antibiotic causing disease metronidazole, vancomycin Relapses due to resistant spores. retreatment with same antibiotic neutralization with specific antitoxin obtained commercially amount of toxin present can be determined by a dilution series of the stool sample. 12/6/2020

50 C. difficile Culture: standard test for Clostridia include: indole, sugars, lecithinase, catalase (usually neg. ) 12/6/2020

51 C. difficile: Latex agglutination stool buffered and centrifuged drop on slide of stool supernatant add 1 drop latex detection reagent. Latex particles coated with rabbit antibody to C. difficile antigen. In presence of C. difficile clumps can be seen by eye. 12/6/2020

52 Culture: Inoculate anaerobe blood agar -- 2 -3 days egg yolk medium -- 2 -3 days Incubation temp. = 30 C except C. perfringens Inoculate cooked meat medium - (broth with meat particles) 12/6/2020

53 C. difficile: Culture a/ heat to destroy vegetative cells b/ alcohol spore selection for heat labile spores. Clinical syndromes: most serious is (PMC) Pseudomembranous colitis brought about by destruction of the other indigenous intestinal flora. Ranges from mild to serious. PMC self-limiting. 12/6/2020

54 Differential diagnosis: S. aureus, E. coli, shigellosis, acute ulcerative colitis, Campylobacter jejuni 12/6/2020

55 The End 12/6/2020

56 Key Terms ä ä ä ä Obligate anaerobe endospore asporogenous botulism tetanus gangrene pseudomembranous colitis myonecrosis ä ä ä ä Botulism toxin tetanus toxin trismus opisthotonus risus sardonicus C. perfringens enterotoxin aerotolerant Nagler reaction 12/6/2020

57 Key Terms ä ä Enteritis necroticans tetanospasmin 12/6/2020

58 Key Organisms ä ä ä Clostridium C tetani C botulinum C. perfringens C. difficile 12/6/2020

59 Key Concepts 12/6/2020

60 Epidemiology of Botulism ä Disease/bacterial factors ä Transmission ä who is at risk ä geography/ season ä modes of control 12/6/2020

61 Epidemiology of C. difficile infections ä Disease/bacterial factors ä Transmission ä who is at risk ä geography/ season ä modes of control 12/6/2020

62 Epidemiology of C. tetani infections ä Disease/bacterial factors ä Transmission ä who is at risk ä geography/ season ä modes of control 12/6/2020

63 Epidemiology of C. perfringens infections ä Disease/bacterial factors ä Transmission ä who is at risk ä geography/ season ä modes of control 12/6/2020

64 Short Answers ä Construct a table of the virulence factors associated with C. tetani and the biological activity of each ä Use a series of no more than four diagrams to describe the mechanism of tetanospasmin activity ä Describe the clinical manifestions of generalized, cephalic and localized tetanus 12/6/2020

65 Short Answers ä Construct a table listing the common clostridial species and the associated human diseases. ä Construct a table listing 5 virulence factors associated with C. difficile and the biological activity of each ä Construct a table of the virulence factors associated with C. perfringens and the biological activity of each 12/6/2020
- Slides: 65