1 Background Local Process Changes 6 Patient experience

1


Background

Local Process Changes

6
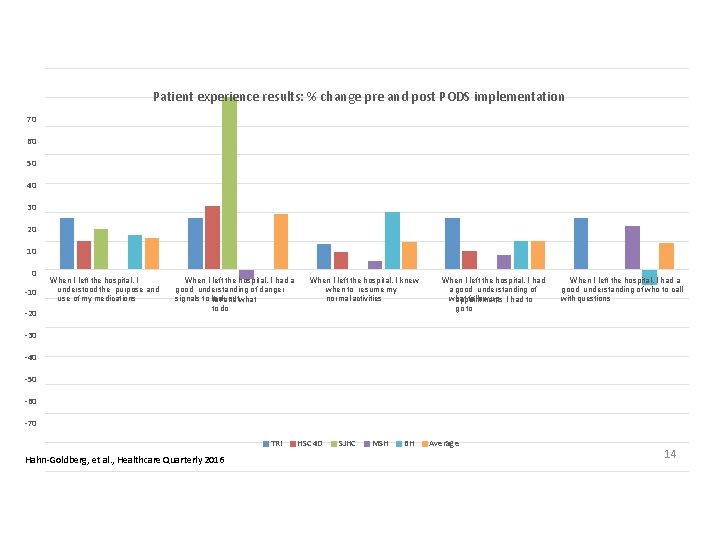
Patient experience results: % change pre and post PODS implementation 70 60 50 40 30 20 10 0 -10 -20 When I left the hospital, I understood the purpose and use of my medications When I left the hospital, I had a good understanding of danger signals to look outwhat for and to do When I left the hospital, I knew when to resume my normal activities When I left the hospital, I had a good understanding of what follow up I had to appointments go to When I left the hospital, I had a good understanding of who to call with questions -30 -40 -50 -60 -70 TRI Hahn-Goldberg, et al. , Healthcare Quarterly 2016 HSC 4 D SJHC MSH BH Average 14
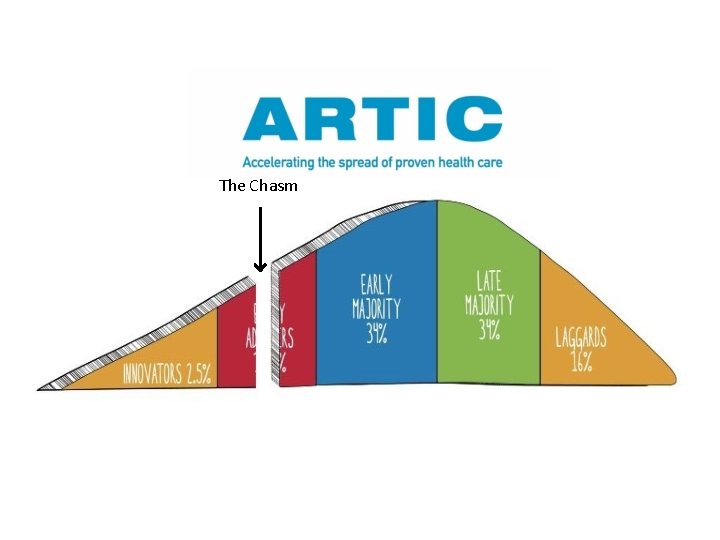
The Chasm
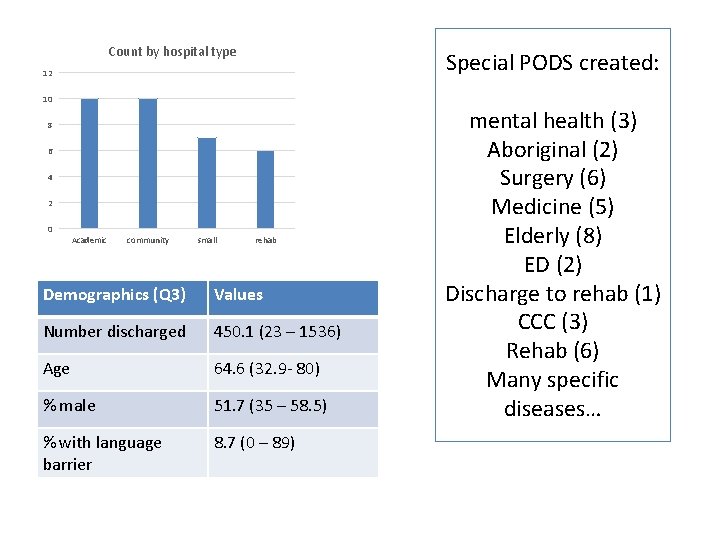
Count by hospital type Special PODS created: 12 10 8 6 4 2 0 Academic community small rehab Demographics (Q 3) Values Number discharged 450. 1 (23 – 1536) Age 64. 6 (32. 9 - 80) % male 51. 7 (35 – 58. 5) % with language barrier 8. 7 (0 – 89) mental health (3) Aboriginal (2) Surgery (6) Medicine (5) Elderly (8) ED (2) Discharge to rehab (1) CCC (3) Rehab (6) Many specific diseases…
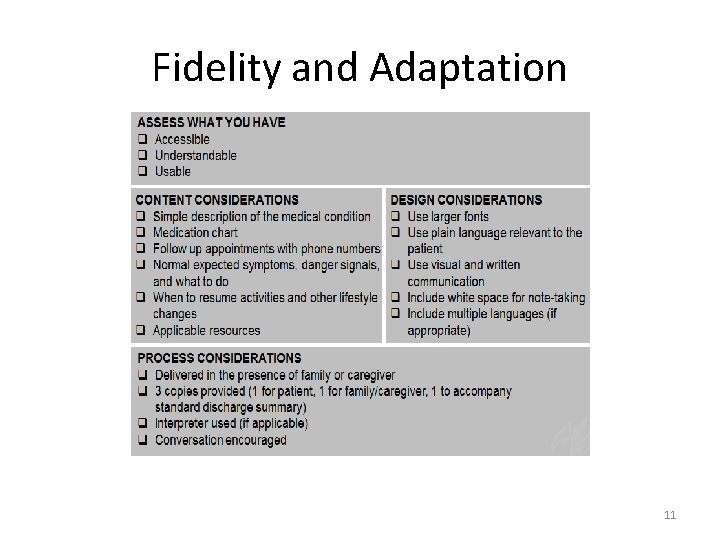
Fidelity and Adaptation 11

Primary Care • Co-creation of best practice guidelines • 7 sites reported engaging primary care in the co-design process • Handout 12

13

PODS at Toronto Rehab • Lyndhurst Centre (spinal cord rehab) – 2015 • University Centre Inpatient Stroke rehab - 2017 • Outpatient stroke and spread to ABI units in 2018

What is Teach Back? • It is a research-based health literacy intervention that promotes adherence, quality, and patient safety. • It is technique where you ask patients to repeat back in their own words or demonstrate what they understand from what they’ve been taught. • It is NOT a test of the patient's knowledge but an indication of how well information was taught and what needs to be clarified or reviewed.

Teach-Back Spinal Cord Injury Patient Oriented Discharge Strategy Lyndhurst Rehabilitation - UHN For more information please contact: Heather Flett – Advanced Practice Leader Heather. Flett@uhn. ca Sandra Mills - Patient and Family Educator Sandra. Mills@uhn. ca

What is Teach-Back SCI PODS? 1. Teach-back style PODS meeting that uses self-management best practices led by a neutral clinician facilitator 2. An SCI-focused document Medications Care Plan Signs, Symptoms and What to do’s Appointments Individualized Contact List In patient’s own words 3. When: 1 week prior to discharge ( 45 min-1 hr) 4. Who: patient/family, facilitator, team member 17

What are the benefits of Teach-Back SCI? • Consolidate rehab learning • Identify outstanding needs before discharge • Reduce anxiety prior to discharge • Enhance self-efficacy 18
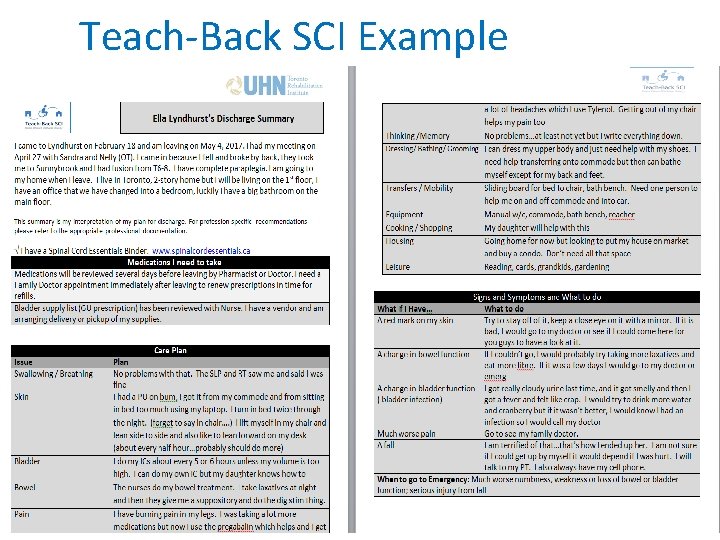
Teach-Back SCI Example 19

PODS on Inpatient Stroke at TR • • Evaluation Development & Implementation Data tracking Next steps
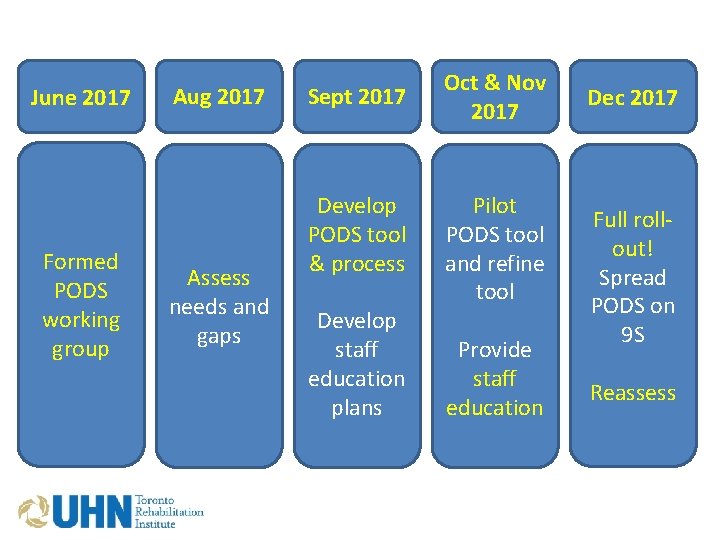
June 2017 Formed PODS working group Aug 2017 Assess needs and gaps Sept 2017 Develop PODS tool & process Develop staff education plans Oct & Nov 2017 Pilot PODS tool and refine tool Provide staff education Dec 2017 Full rollout! Spread PODS on 9 S Reassess

In the beginning … Our Discharge Process Profession / team-based assessment, intervention, & discharge teaching / preparation throughout rehab stay Care Conference Discharge Binder & discussion on day of discharge

What did our evaluation tell us? • Patients, caregivers and staff valued the discharge education being provided, including the discharge binder. • Content was meaningful, easy to understand, easy to use and comprehensive. • Opportunity to look at the timing at which we provide discharge education and more consistent use of teach back methodology.

What does PODS look like on 9 S? ü Discharge binder being introduced sooner ü Teach-back meeting 3 -4 days prior to discharge facilitated by a Rehab Therapist : – check-in with patients to ensure all necessary discharge teaching has been completed and identify any gaps so they can be addressed prior to discharge. – Family encouraged to attend if involved. ü Team members prepare earlier for discharge ü Minor changes to discharge binder
Current Discharge Process Profession / team -based assessment, intervention, & discharge teaching / preparation throughout rehab stay Care Conference Discharge Teaching (PODS) Meeting 3 -4 days before discharge Review Discharge Binder and discharge information Provide Discharge Binder on day of discharge
PODS Teach-back Guide

Impact on Patient Safety and Patient Experience 1) identifying gaps earlier will allow team time to address education needs prior to discharge. 2) reduces feelings of being overwhelmed with information on day of discharge. 3) provides time for patient to process information. 4) doing teach-back promotes self-management and self-efficacy. 5) flags outpatient team of any concerns raised at discharge and patient’s plan for managing at home.

Implementation • Pilot: 9 patients in early November • Roll out to unit in mid December • Rehab therapist completes data tracking tool

Data Tracking to date Total PODS completed 63 Avg time to complete (min) 45 Avg no. (calendar) days PODS mtg completed prior to discharge 4 % PODS meetings where learning needs were identified 59% • Gaps identified are often patient-specific • Most common gaps: outpatient schedule, CCAC, transportation, medications.

Learnings • Flexibility with timing to meet patient, team and family needs. • Patients are retaining most information needed for discharge. • Provides an opportunity for the team to address patient-specific concerns pre-discharge. • Patients/families feel teach-back meeting is valuable and helps them to feel more confident with transition home.

Post-PODS Evaluation • • Patient/caregiver interviews completed Patient/caregiver surveys (ongoing) Staff surveys to be completed in March Focus group with rehab therapists to be completed in March

Patient/Caregiver interviews • Was the discharge meeting useful in preparing you for discharge home? “Yes it was useful; it was useful because I had the sections explained to me and I knew where to find what. ” “It was pretty straightforward and the information was easy to understand. I already knew most of the information” “It was certainly useful; everything in the binder was valuable. There were questions that were answered. ”

Patient/Caregiver Interviews • Did you receive the information you needed to feel prepared for discharge? “Yes, I felt prepared. Only thing that would have been helpful is e-mail addresses for therapists so you can reach them more easily. They are busy and not at the phone. ” “Yes, apart from the meeting you had with me, all the other staff took time out to explain their role in preparation for discharge. They remembered pages that they had forgotten but got them in there before I left. ”

Patient/Caregiver Interviews • How did you feel about the timing of the meeting (a few days before discharge)? “Good timing for the meeting because I had a couple of questions which he was able to get me answers for (before I left). ”

Next Steps • Focusing on outpatient stroke programs to address: – 1) how can inpatient PODS be used on intake for outpatient programs? – 2) development of outpatient PODS – 3) link to outpatient physiatry rehab appointments • Spread to ABI programs

Contact info Lucy Kilby, OT Reg. (Ont. ) Occupational Therapist Inpatient Stroke Rehab Program Toronto Rehab, UHN lucy. kilby@uhn. ca
- Slides: 36