1 B 260 FUNDAMENTALS OF NURSING PRACTICE Gas

1 B 260: FUNDAMENTALS OF NURSING PRACTICE Gas Exchange

2 Gas exchange/Oxygenation • Oxygenation can be defined as the mechanisms that facilitate or impair the body’s ability to supply oxygen to all cells of the body. The function of the respiratory system is to obtain oxygen from atmospheric air, to transport this air through the respiratory tract into the alveoli, and ultimately to diffuse oxygen into the body that carries oxygen to all the cells of the body.
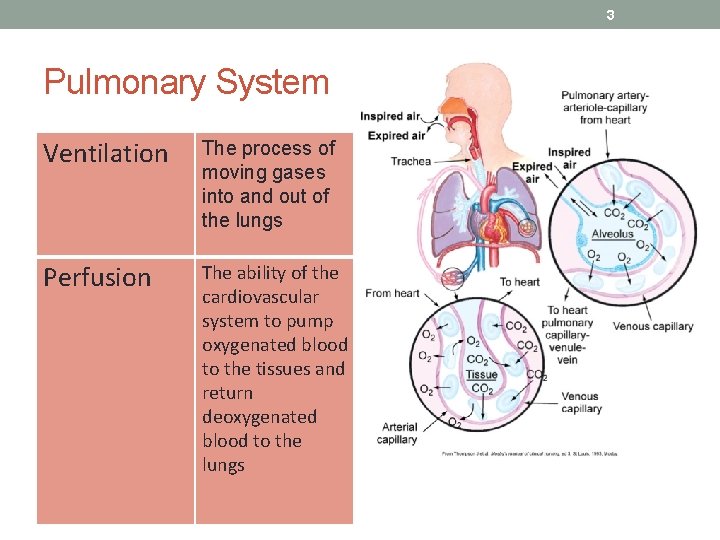
3 Pulmonary System Ventilation The process of moving gases into and out of the lungs Perfusion The ability of the cardiovascular system to pump oxygenated blood to the tissues and return deoxygenated blood to the lungs
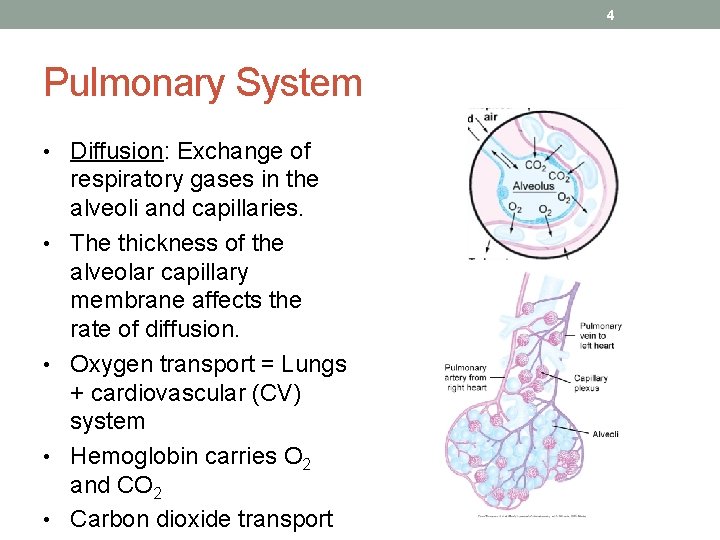
4 Pulmonary System • Diffusion: Exchange of • • respiratory gases in the alveoli and capillaries. The thickness of the alveolar capillary membrane affects the rate of diffusion. Oxygen transport = Lungs + cardiovascular (CV) system Hemoglobin carries O 2 and CO 2 Carbon dioxide transport
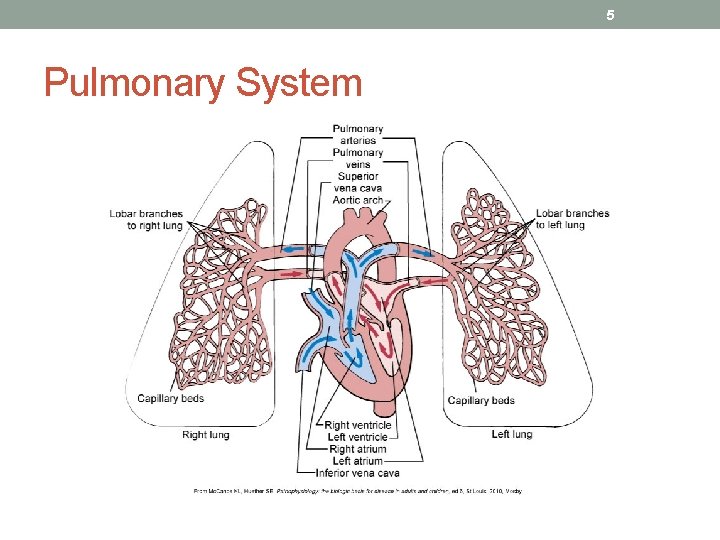
5 Pulmonary System

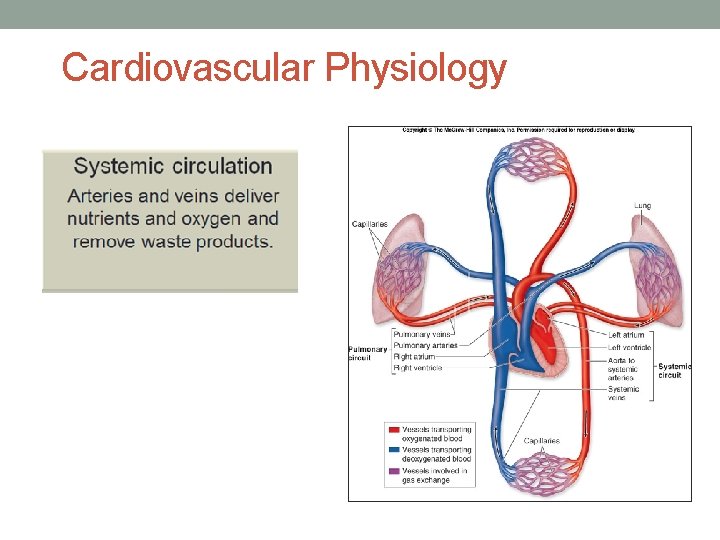
Cardiovascular Physiology • Cardiopulmonary physiology involves delivery of deoxygenated blood (blood high in carbon dioxide and low in oxygen) to the right side of the heart and then to the lungs, where it is oxygenated. • Oxygenated blood (blood high in oxygen and low in carbon dioxide) then travels from the lungs to the left side of the heart and the tissues.
Cardiovascular Physiology
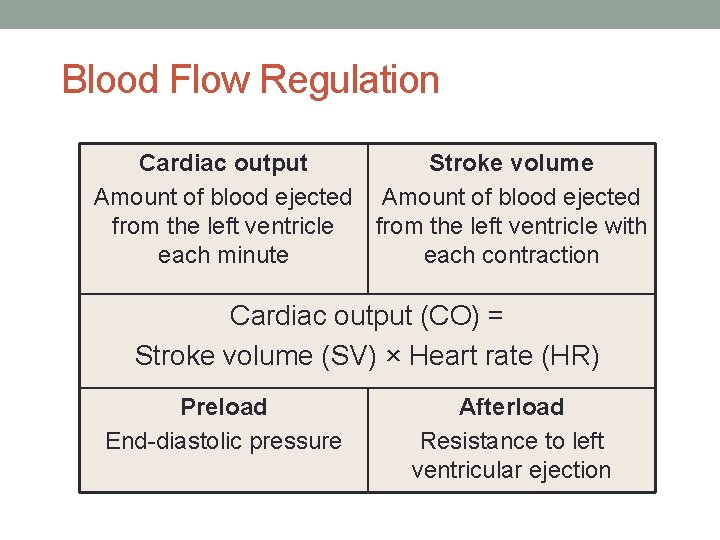
Blood Flow Regulation Cardiac output Stroke volume Amount of blood ejected from the left ventricle with each minute each contraction Cardiac output (CO) = Stroke volume (SV) × Heart rate (HR) Preload End-diastolic pressure Afterload Resistance to left ventricular ejection

9 Factors Affecting Oxygenation • Physiological factors • Decreased oxygen-carrying capacity • Anemia • Hypovolemia • Dehydration and hemorrhage • Decreased inspired oxygen concentration • High altitudes • Increased metabolic rate • Fever
10 Factors Affecting Oxygenation Factors Affecting Chest Wall Movement • • Pregnancy • Obesity • Musculoskeletal abnormalities Kyphosis Pectus Excavatum
11 Factors Affecting Oxygenation Factors Affecting Chest Wall Movement • Trauma • Neuromuscular disease • CNS alterations • Chronic disease
12 Alterations in Respiratory Functioning Respiratory Alterations • Hypoventilation: alveolar ventilation inadequate to meet the body’s oxygen demand; respiratory rate and depth is low • Hyperventilation: ventilation in excess of that required; rate and depth of respirations increase • Hypoxia: Inadequate tissue oxygenation at the cellular level, late sign cyanosis
13 Hypoventilation • Causes • Signs and Symptoms
14 Hypoventilation • Causes • Atelectasis • Signs and Symptoms
15 Hypoventilation • Causes • Atelectasis • Signs and Symptoms • Mental status changes • Dysrhythmias • Convulsions • Unconscious • Death

16 Hyperventilation • Causes • Signs and symptoms

17 Hyperventilation • Causes • Severe anxiety • Infection • Drugs • Acid-base imbalance • Fever • Signs and symptoms

18 Hyperventilation • Causes • Severe anxiety • Infection • Drugs • Acid-base imbalance • Fever • Signs and symptoms • Rapid respirations • Sighing breaths • Numbness and tingling of hands/feet • Light-headedness • Loss of consciousness

19 Hypoxia • Causes • Signs and Symptoms

20 Hypoxia • Causes • A ↓in Hgb and lowered O 2 -carrying capacity of blood. • A diminished inspired O 2 • A ↓ in diffusion of O 2 from the alveoli to the blood • Impaired ventilation • Signs and symptoms

21 Hypoxia • Causes • A ↓in Hgb and lowered O 2 carrying capacity of blood. • A diminished inspired O 2 • A ↓ in diffusion of O 2 from the alveoli to the blood • Impaired ventilation • Signs and symptoms • Apprehensive • Restlessness, inability to concentrate • ↓ LOC • Dizziness • Behavioral changes • Agitated • ↑ RR • ↑ HR • Late signs: ↓ RR, ↓ HR and cynosis

22 Lifestyle Factors Nutrition Cardioprotective nutrition = Diets rich in fiber; whole grains; fresh fruits and vegetables; nuts; antioxidants; lean meats; and omega-3 fatty acids. Exercise People who exercise for 30 to 60 minutes daily have a lower pulse rate and blood pressure, decreased cholesterol level, increased blood flow, and greater oxygen extraction by working muscles.

23 Lifestyle Risk Factors • Smoking • Associated with heart disease, COPD, and lung cancer • The risk of lung cancer is 10 times greater for a person who smokes than for a nonsmoker. • Substance abuse • Excessive use of alcohol and other drugs impairs tissue oxygenation. • Stress • A continuous state of stress or severe anxiety increases the metabolic rate and oxygen demand of the body.

24 Environmental Factors • The incidence of pulmonary disease is higher in smoggy, urban areas than in rural areas. • A patient’s workplace sometimes increases the risk for pulmonary disease. • Asbestosis

25 Case Study: Mr. William Smith

26 Case Study: Mr. William Smith • Mr. Smith is a 65 -year-old man who developed shortness of breath while on a family vacation in the mountains. When he returned home from vacation he presented to the emergency department alert and feeling ill with an elevated temperature of 101. 5 F and chills. • Mr. Smith has a 1 -pack per week history of smoking and no history of alcohol or illicit drug abuse. Recent history includes dry hacking cough, low-grade fever, fatigue, loss of appetite, and feeling terrible.

27 Case Study: Mr. William Smith • Ben Adams is the nursing student assigned to his first hospital-based clinical experience. He has some experience in health assessment and patient teaching related to health promotion activities from a recent rotation at a clinic. In the previous experience, patients were encouraged to adjust their at-risk health behaviors, such as smoking or poor diet. • Ben feels confident when he arrives in the clinical area this morning because Mr. Smith has similar health needs to the clinical experiences he has had.

28 Nursing Process: Assessment Collaborative Learning With your neighbor, discuss what questions Ben would have asked Mr. Smith if he had been at the hospital when Mr. Smith was being admitted.

29 While Ben is completing his morning physical assessment, what observations would he focus on to determine if Mr. Smith’s oxygen needs were being met? • Presents of: • Inspection • Palpation • Percussion • Auscultation

30 While Ben is completing his morning physical assessment, what observations would he focus on to determine if Mr. Smith’s oxygen needs were being met? • Presents of: • Pain • Fatigue • Dyspnea • Cough • Breath sounds • Respiratory rate • Inspection • Color of skin and mucous membranes, LOC, breathing patterns, chest wall movement, cap refill, • Palpation • Chest, feet, legs, Pulses • Percussion • Abnormal fluid or air in lungs • Auscultation • Breath sounds and lung sounds

31 Diagnostic Tests • CBC • WBC: 5 -10, 000 • RBC: Male: 4 -6, 000 Female 4 -5, 000 • Hgb: Male: 14 -18 g/d. L Female 12 -16 g/d. L • Hct: Male 42%-52% Female 37%- 47% • Chest x-ray • Sputum specimens for C & S • Pulse oximetry

32 Case Study: William Smith • Ben’s morning assessment included the following findings: • BP 110/70 mm Hg • HR 102 beats/min • Temp 101. 5 • RR 36 breaths/min • Breath sounds: Expiratory wheezing, crackles and diminished breath sounds over the right lower lobe are audible. • O 2 Sats at 88% with O 2 per NC at 2 L/NC • Sputum is thick and discolored (yellow-green). • Wt 190 lbs

33 Case Study: William Smith • Ben’s morning assessment included the following findings: • Alert and oriented • Pupils PEARL • Bowel sounds positive in all 4 quadrants • Heart sounds regular • Radial and pedal pulses equal • No edema • Able to move all 4 extremities • Weak from being SOB • Saline lock in left forearm - patent, dry, intact

34 Case Study: William Smith • Ben reviewed the recent HCP’s orders and results. • Admitting Diagnosis: Pneumonia • Chest x-ray: revealed upper and middle lobe opacities on the right side and some atelectasis in the lower lobe • WBC 12. 9 • Blood Cultures pending • IV fluids: D 5. 45 normal saline at 100 ml/hr • Cefepime 1 g every 8 hours over 30 min. Mix in 50 ml of NS • O 2/NC at 2 L. Call if O 2 sats are below 94% • Encourage rest for 24 hours then up ad lib • Incentive spirometer 10 time/hour while awake
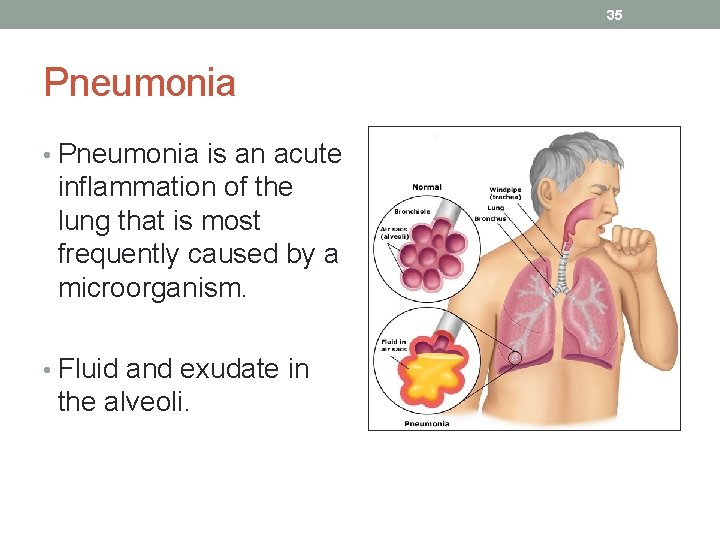
35 Pneumonia • Pneumonia is an acute inflammation of the lung that is most frequently caused by a microorganism. • Fluid and exudate in the alveoli.

36 Interventions • Positioning: HOB up semi Fowlers • Helps to drain secretions from specific segments of the lungs and bronchi into the trachea
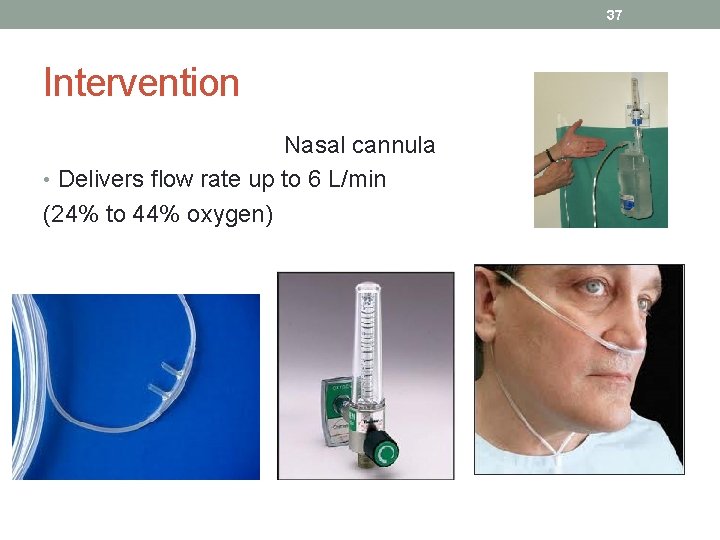
37 Intervention Nasal cannula • Delivers flow rate up to 6 L/min (24% to 44% oxygen)

• Concentrating on nasal cannulas • Starting at 1 L/min, increasing the oxygen flow by 1 L/min will increase the inspired oxygen concentration about four percentage points: • • 1 L/min = 24% • • 2 L/min = 28% • • 3 L/min = 32% • • 4 L/min = 36% • • 5 L/min = 40% • • 6 L/min = 44%
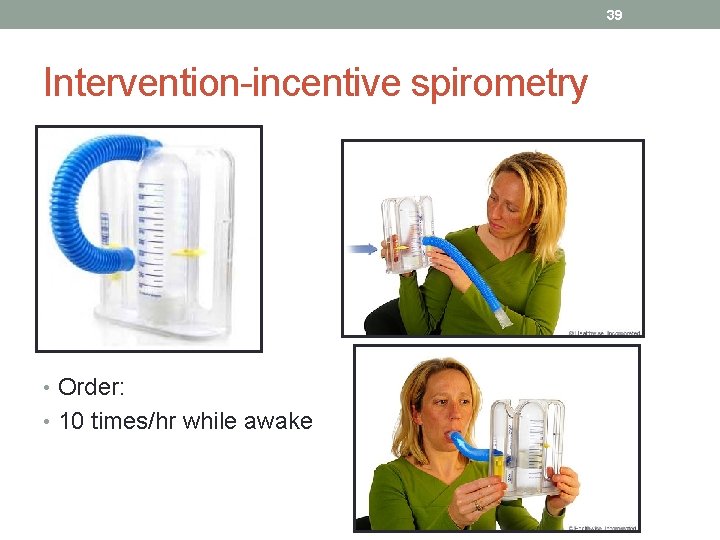
39 Intervention-incentive spirometry • Order: • 10 times/hr while awake

40 Interventions Deep breathing and coughing Encourage fluids • Diaphragmatic • Hydration breathing/belly breathing • Cascade cough • Huff cough • Humidification • Nebulization • Oral and IV

41 Case Study • At the end of his 8 hours shift, Ben reported off to his primary nurse. He reported: • Mr. Smith: • Used his IS 10 time every hour while awake. He had a productive cough at the beginning of the morning, but by mid afternoon, he no longer had a productive cough. • Received his antibiotic per order • Remained on bed rest per order. He did go to the BR and Ben noticed Mr. Smith was SOB when he returned to bed. Mr. Smith did have his HOB up at all time. After the change of O 2 to 3 liter (per order change) his O 2 sats stayed at 95%. • IV fluids are infusing without difficulty and he is taking oral fluids independently (800 ml)
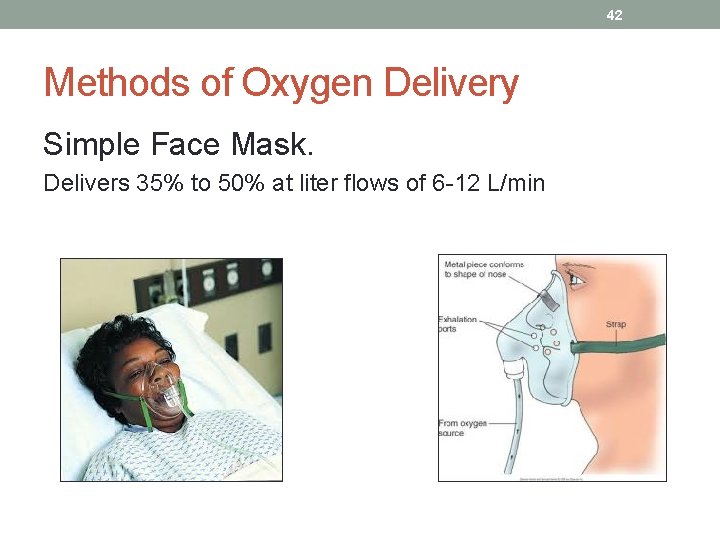
42 Methods of Oxygen Delivery Simple Face Mask. Delivers 35% to 50% at liter flows of 6 -12 L/min

43 Methods of Oxygen Delivery • A plastic face mask with a reservoir bag is capable of delivering higher concentrations of oxygen. A partial rebreather mask is a simple mask with a reservoir bag that should be at least one third to one half full on inspiration and delivers from 60% to 90% with a flow rate of 10 -15 L/min

44 Methods of Oxygen Delivery • Venturi mask delivers higher oxygen concentrations of 24% to 50% with oxygen flow rates of 4 to 12 L/min, depending on the flow-control meter selected.

45 Oxygenation Safety • Oxygen must be prescribed and adjusted only with a HCP’s order. • Determine that all electrical equipment in the room is functioning correctly and properly grounded. An electrical spark in the presence of oxygen can result in a serious fire. • Check the oxygen level of portable tanks before transporting a patient to ensure there is enough oxygen in the tank.

46 Oxygenation Safety • Secure oxygen cylinders so they do not fall over. Store them upright and either chained or secured in appropriate holders.
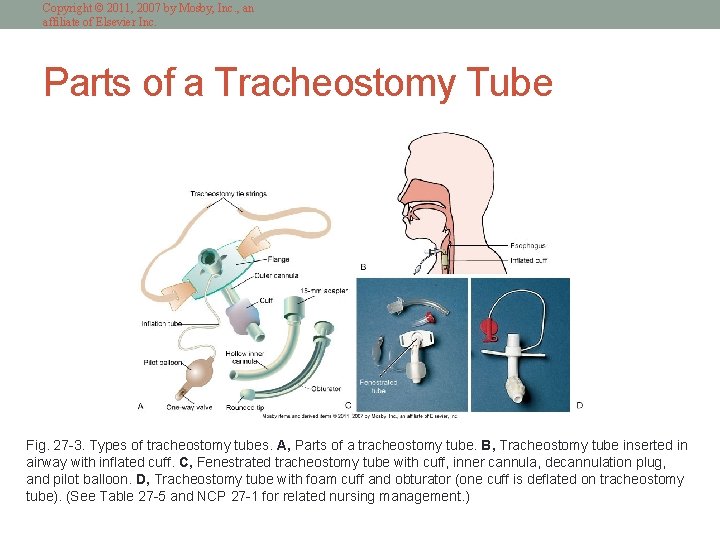
Copyright © 2011, 2007 by Mosby, Inc. , an affiliate of Elsevier Inc. Parts of a Tracheostomy Tube Fig. 27 -3. Types of tracheostomy tubes. A, Parts of a tracheostomy tube. B, Tracheostomy tube inserted in airway with inflated cuff. C, Fenestrated tracheostomy tube with cuff, inner cannula, decannulation plug, and pilot balloon. D, Tracheostomy tube with foam cuff and obturator (one cuff is deflated on tracheostomy tube). (See Table 27 -5 and NCP 27 -1 for related nursing management. )
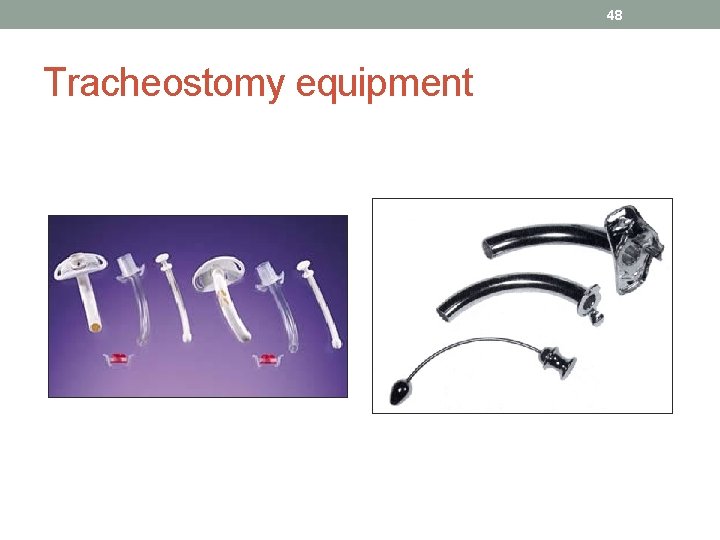
48 Tracheostomy equipment
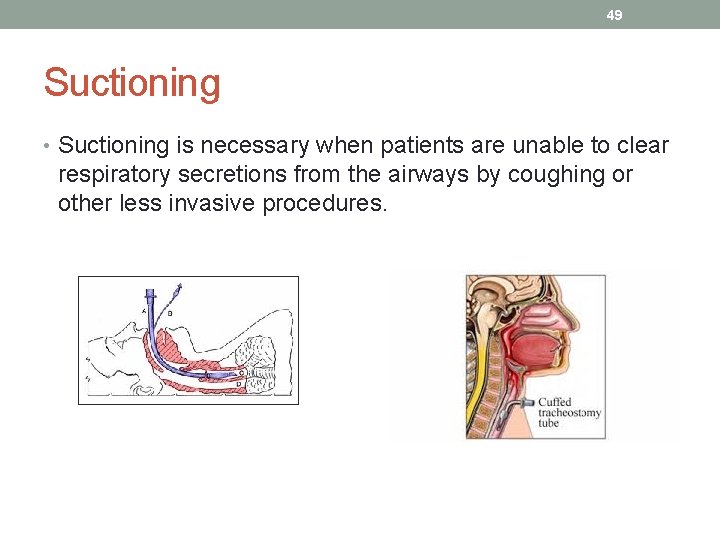
49 Suctioning • Suctioning is necessary when patients are unable to clear respiratory secretions from the airways by coughing or other less invasive procedures.
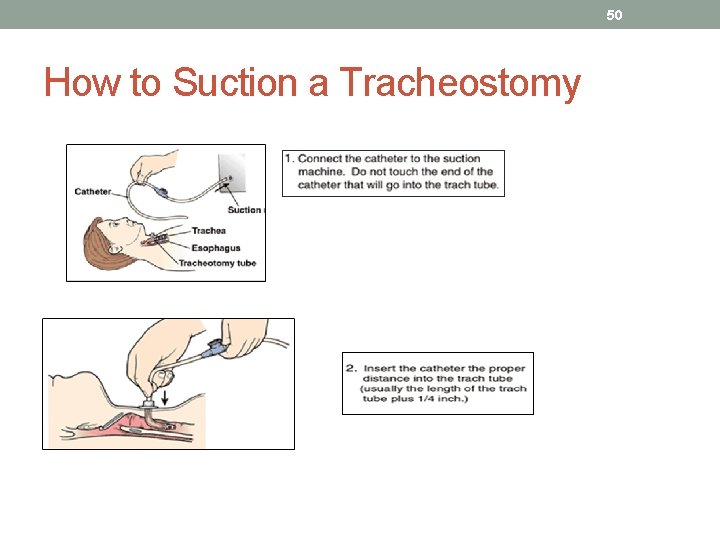
50 How to Suction a Tracheostomy
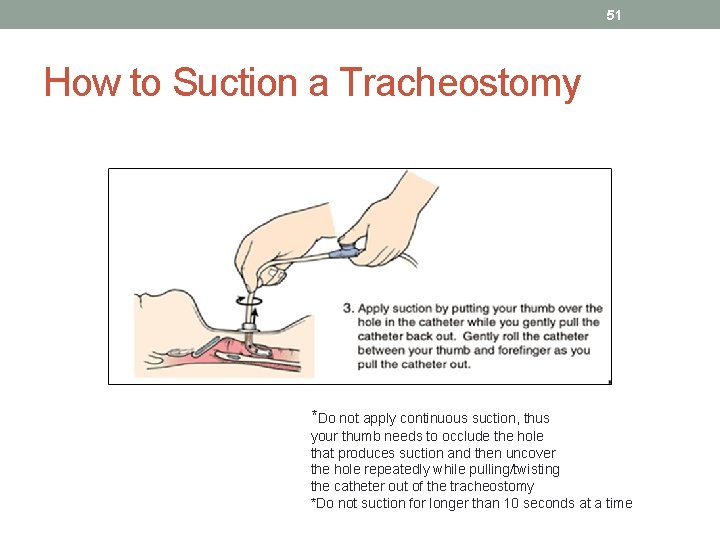
51 How to Suction a Tracheostomy *Do not apply continuous suction, thus your thumb needs to occlude the hole that produces suction and then uncover the hole repeatedly while pulling/twisting the catheter out of the tracheostomy *Do not suction for longer than 10 seconds at a time

52 Emergency Patient is having Acute Dyspnea • Acute dyspnea for patient with tracheostomy is most commonly caused by partial or complete blockage of the tracheostomy tube retained secretions. To unblock the tracheostomy tube: • 1. ASK THE PATIENT TO COUGH: A strong cough may be all that is needed to expectorate secretions. • 2. REMOVE THE INNER CANNULA: If there are secretions stuck in the tube, they will automatically be removed when you take out the inner cannula. The outer tube – which does not have secretions in it – will allow the patient to breath freely. Clean and replace the inner cannula. • 3. SUCTION: If coughing or removing the inner cannula do not work, it may be that secretions are lower down the patients airway. Use the suction machine to remove secretions. • 4. If these measures fail – commence low concentration oxygen therapy via a tracheostomy mask, and call for medical assistance.

53 Suctioning • Key points: • Use sterile procedure • Suction set on continuous suction up to 120 mm Hg for open suctioning • Suction set on continuous suction up to 160 mm Hg for closed suctioning. • Insert catheter, suction intermittently 10 seconds and slowly rotate and withdraw • Allow 20 -30 seconds between passes • Monitor patient: • Risk for hypoxia • Hypotension • Arrhythmias • Trauma • Irritation • Vagal stimulation
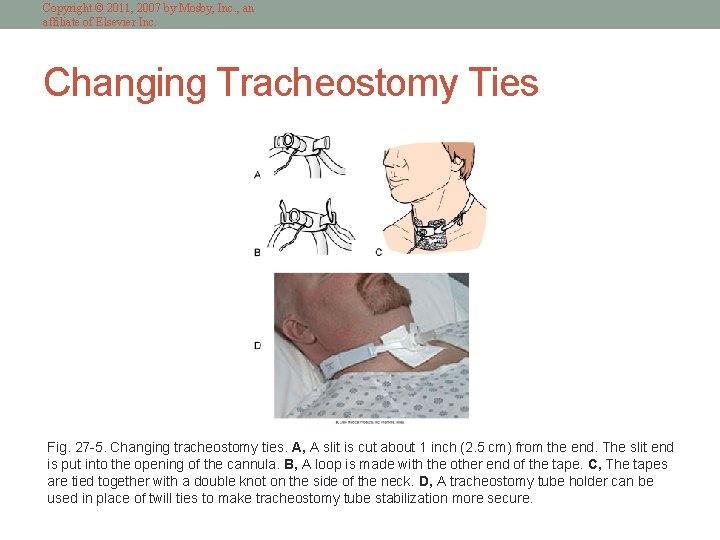
Copyright © 2011, 2007 by Mosby, Inc. , an affiliate of Elsevier Inc. Changing Tracheostomy Ties Fig. 27 -5. Changing tracheostomy ties. A, A slit is cut about 1 inch (2. 5 cm) from the end. The slit end is put into the opening of the cannula. B, A loop is made with the other end of the tape. C, The tapes are tied together with a double knot on the side of the neck. D, A tracheostomy tube holder can be used in place of twill ties to make tracheostomy tube stabilization more secure.
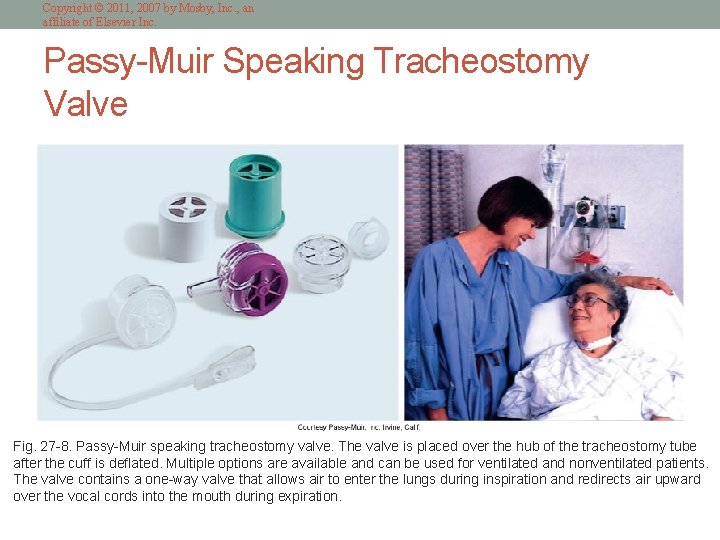
Copyright © 2011, 2007 by Mosby, Inc. , an affiliate of Elsevier Inc. Passy-Muir Speaking Tracheostomy Valve Fig. 27 -8. Passy-Muir speaking tracheostomy valve. The valve is placed over the hub of the tracheostomy tube after the cuff is deflated. Multiple options are available and can be used for ventilated and nonventilated patients. The valve contains a one-way valve that allows air to enter the lungs during inspiration and redirects air upward over the vocal cords into the mouth during expiration.

56 Oxygenation: Chest Tubes Chest tubes • A catheter placed through the thorax to remove air and fluids from the pleural space Purpose • To remove air and fluids from the pleural space • To prevent air or fluid from reentering the pleural space • To re-establish normal intra-pleural and intrapulmonary pressures

57 Case Study: Mr. Scott • Mr. Scott a 73 -year-old man fell from a ladder while cleaning his gutters. He presented to the emergency department with c/o sudden onset of acute chest pain on the right side and labored breathing and dyspnea. • Assessment • BP 170/88, HR 110, RR 40, O 2 Sat 80% • Uneven chest wall movement • Very anxious
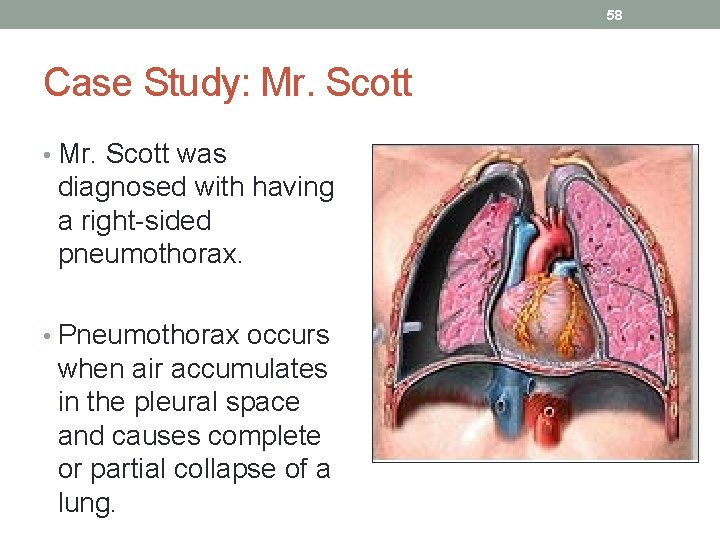
58 Case Study: Mr. Scott • Mr. Scott was diagnosed with having a right-sided pneumothorax. • Pneumothorax occurs when air accumulates in the pleural space and causes complete or partial collapse of a lung.
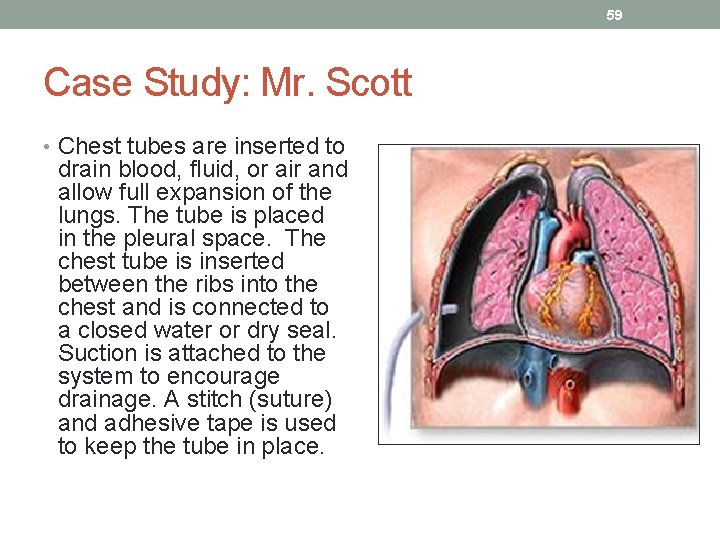
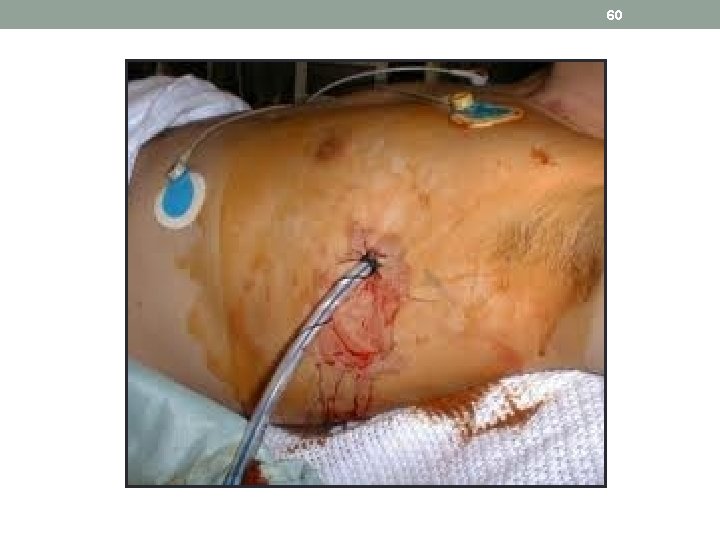
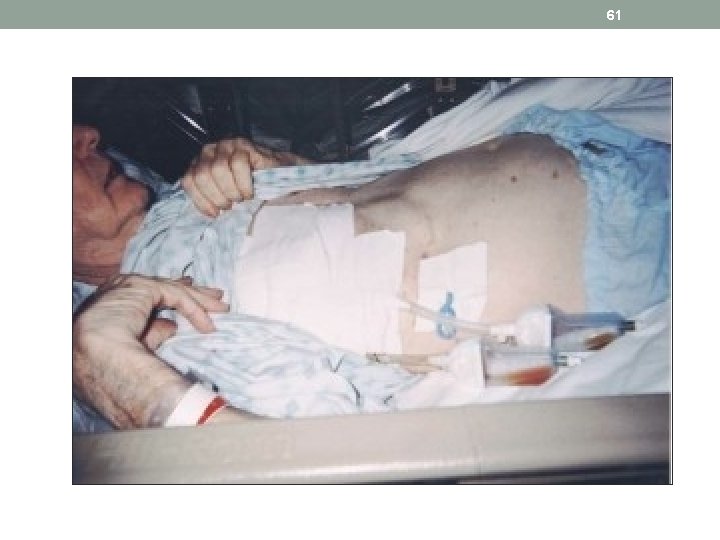
59 Case Study: Mr. Scott • Chest tubes are inserted to drain blood, fluid, or air and allow full expansion of the lungs. The tube is placed in the pleural space. The chest tube is inserted between the ribs into the chest and is connected to a closed water or dry seal. Suction is attached to the system to encourage drainage. A stitch (suture) and adhesive tape is used to keep the tube in place.
60
61


63

64 Chest Tube Interventions • Maintain secure, airtight dressing • Maintain underwater seal • Monitor and secure all connections • Observe for bubbling • Monitor tubing for patency • Record output (quantity, characteristics) • Monitor patient • Dressing changes per agency
65 Case Study: Mr. Scott Day 5 • Patient received a chest x-ray to monitor the status of the chest tube placement and pneumothorax. Results showed that the right lung remained fully expanded.
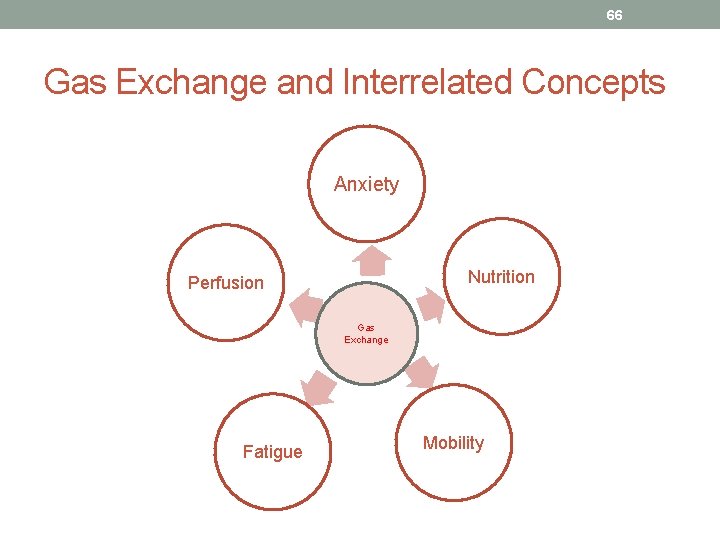
66 Gas Exchange and Interrelated Concepts Anxiety Nutrition Perfusion Gas Exchange Fatigue Mobility
- Slides: 66