1 Anemia 2 Iron metabolism 3 Iron deficiency


순서 1. Anemia 2. Iron metabolism 3. Iron deficiency anemia • Clinical features • Laboratory features • Differential diagnosis • Management

Anemia Below lower limit of 95% reference interval for Hb or Hct Reference values below which anemia is considered to exist at sea level Age (years) Hb (g/d. L) Both sexes 1 -2 11 3 -5 11. 2 6 -11 11. 8 Females 12 -15 11. 9 16 -69 12 ≥ 70 11. 8 Males 12 -15 12. 6 16 -19 13. 6 20 -49 13. 7 50 -69 13. 3 ≥ 70 12. 4 2. 5% of normal individuals Significantly below his or her own reference values

Anemia • Absolute – decreased RBC mass impaired production increased destruction / loss • Relative – higher plasma volume (pregnancy) • Morphology Macrocytic Normocytic Microcytic

Clinical signs and symptoms of anemia • resulting from diminished delivery of oxygen to tissues (Hb conc, blood vol, rate of changes) • pt who is not severely ill : Hb 6 g/d. L not develop any discomfort • Easy fatigability, dyspnea on exertion, faintness, vertigo, Palpitation, headache • Pallor, rapid bounding pulse, low BP, slight fever, dependent edema, systolic murmurs
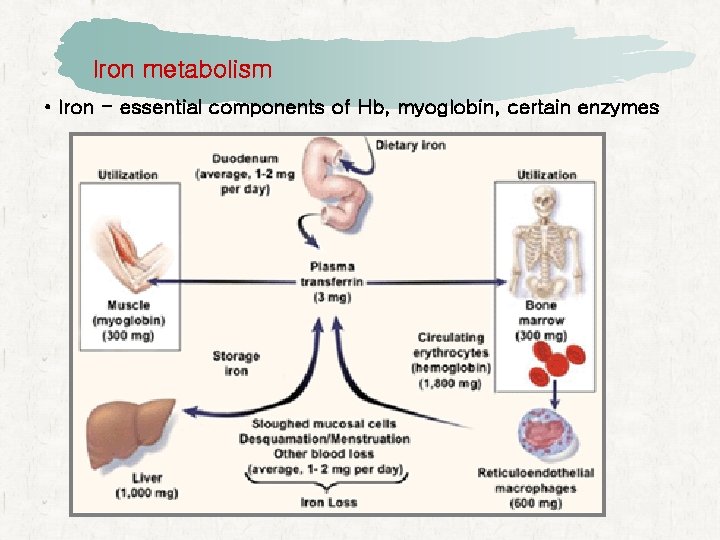
Iron metabolism • Iron - essential components of Hb, myoglobin, certain enzymes
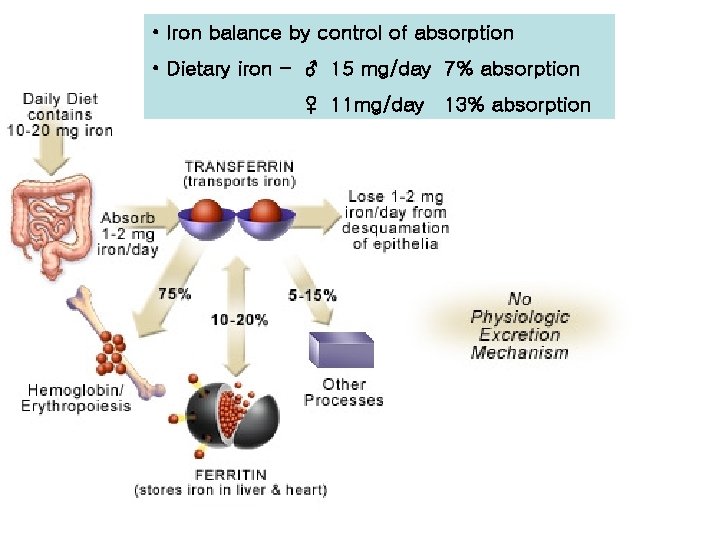
• Iron balance by control of absorption • Dietary iron - ♂ 15 mg/day 7% absorption ♀ 11 mg/day 13% absorption
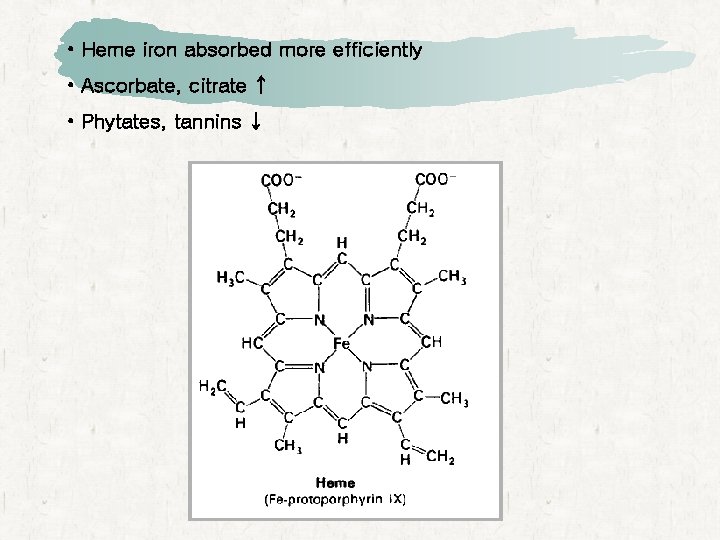
• Heme iron absorbed more efficiently • Ascorbate, citrate ↑ • Phytates, tannins ↓
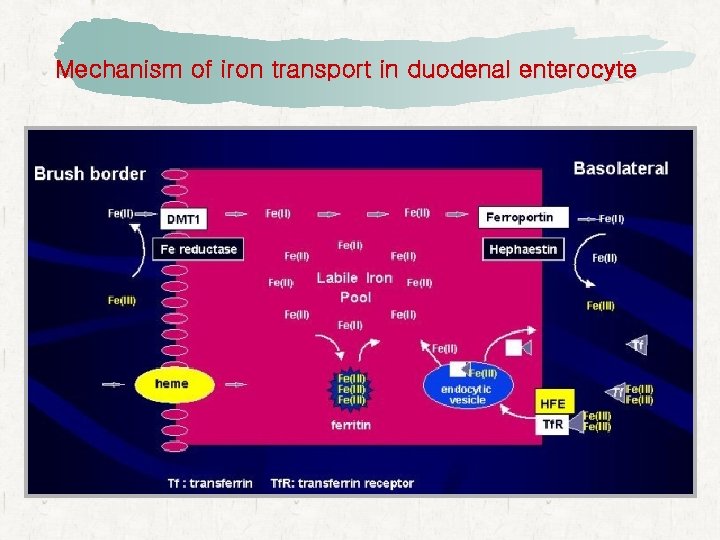
Mechanism of iron transport in duodenal enterocyte

Other proteins that regulate the iron • Ceruloplasmin (cupper containing protein) - ferroxidase activity, release of iron form cells • Hepcidin - iron homeostasis - control GI iron absorption & release of iron form MØ • In plasma total iron 110 μg/d. L bound to transferrin (capacity to bind 330 μg of iron /d. L) plasma ferritin 100 μg/L

Iron deficiency anemia Overall • Iron loss > intake • Depletion of body’s iron stores • Increased need for iron (during rapid growth in infancy & childhood or preg) • Excessive loss of blood (following repeated hemorrhages, excessive mens, multiple preg)

Iron deficiency anemia Overall • M/C cause of anemia, affecting 1/3 of world’s population • 6 -24 months children – “ milk anemia” of infancy 3% of toddlers aged 1 -2 yrs & 2 -5% of adolescent girls and women of childbearing age in US • Defective absorption of iron – total or subtotal gastrectomy H 2 blockers & acid pump blockers

Iron deficiency anemia • Absolutely no iron intake or absorption in adult male -> 1000 mg last 3 -4 yrs -> almost all cases of IDA in adult males d/t chronic blood loss • Sequence of events in developing IDA 1> iron depletion 2> iron deficient erythropoiesis 3> iron deficiency anemia

Clinical features of IDA • d/t underlying cause of blood loss • General manifestation of anemia • Iron deficiency – lack of tissue iron numbness, tingling tongue atrophy angular stomatitis Pica spoon-shaped nails (koilonychia) webs of tissue at esophagopharyngeal junction
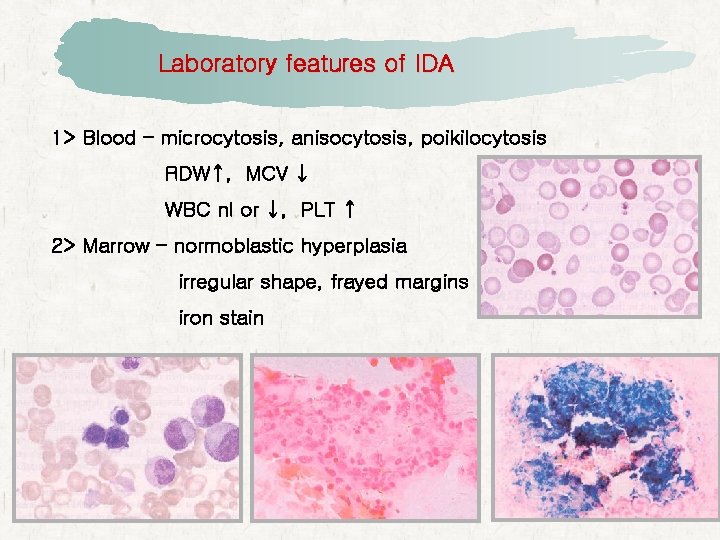
Laboratory features of IDA 1> Blood – microcytosis, anisocytosis, poikilocytosis RDW↑, MCV ↓ WBC nl or ↓, PLT ↑ 2> Marrow – normoblastic hyperplasia irregular shape, frayed margins iron stain

Laboratory features of IDA 3> serum iron ↓ – reference interval (50 -160 μg/d. L) 4> serum iron-binding capacity – reference interval (250 -400 μg/d. L) TIBC ↑ 5> percent saturation of TIBC – ratio of serum iron to TIBC (20 -55%) values below 15% -> IDA marked diurnal variation in serum iron fasting morning blood specimens 6> serum ferritin – reference values (12 -300 μg/d. L) 1 μg/d. L ⇔ 8 -10 mg storage iron acute phase reactant
Laboratory features of IDA 7> erythrocyte porphyrins ↑ 8> serum transferrin receptors (TRs) produced by shedding of memb TRs ↑ TRs ← memb TRs ↑, iron starvation 9> serum transferrin to serum ferritin ratio (R/F ratio) 10> reticulocyte hemoglobin content

DDx of IDA other microcytic hypochromic anemias thalassemia anemia of chronic disease sideroblastic anemia

Management of IDA • underlying cause be identified & corrected • Ferrous iron given orally 200 mg/day three doses between meals • reticulocyte count ↑ maximum at 5 -10 days • monitoring Hb 0. 1 -0. 2 g/d. L/day after 5 th day 2 g/d. L for 3 wks • after Hb to normal : iron therapy continued for 2 Mo

- Slides: 20